Abstract
Objective
The aim of this study was to assess the budget impact of introducing the proprotein convertase subtilisin/kexin type 9 inhibitors (PCSK9i) alirocumab and evolocumab to market for the treatment of adults with heterozygous familial hypercholesterolemia or clinical atherosclerotic cardiovascular (CV) disease requiring additional lowering of low-density lipoprotein cholesterol (LDL-C).
Methods
A 3-year model estimated the costs of lipid-modifying therapy (LMT) and CV events to a hypothetical US health plan of 1 million members, comparing two scenarios—with and without the availability of PCSK9i as add-on therapy to statins. Proportions of patients with uncontrolled LDL-C despite receiving statins, and at risk of CV events, were estimated from real-world data. Total undiscounted annual LMT costs (2017 prices, including PCSK9i costs of $14,563.50), dispensing and healthcare costs, including the costs of CV events, were estimated for all prevalent patients in the target population, based on baseline risk factors. Maximum PCSK9i utilization of 1–5% over 3 years according to risk group (following the same pattern as current ezetimibe use), and 5–10% as a secondary scenario, were assumed.
Results
Total healthcare budget impacts per target patient (and per member) per month for years 1, 2 and 3 were $3.62($0.10), $7.22($0.20) and $10.79($0.30), respectively, assuming 1–5% maximum PCSK9i utilization, and $15.81($0.44), $31.52($0.88) and $47.12($1.31), respectively, assuming 5–10% utilization. Results were sensitive to changes in model timeframe, years to maximum PCSK9i utilization and PCSK9i costs.
Conclusions
The budget impact of PCSK9i as add-on therapy to statins for patients with hypercholesterolemia is relatively low compared with published estimates for other specialty biologics. Drug cost rebates and discounts are likely to further reduce budget impact.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Assuming utilization rates of 1–5 for the proprotein convertase subtilisin/kexin type 9 inhibitors (PCSK9i) alirocumab and evolocumab in patients with clinical atherosclerotic cardiovascular disease or heterozygous familial hypercholesterolemia receiving statins and with uncontrolled LDL-C, the introduction of these treatments was estimated to increase total healthcare costs per target patient (and per member) per month by $3.62 ($0.10), $7.22 ($0.20) and $10.79 ($0.30) for years 1, 2 and 3, respectively. |
These findings suggest that the PCSK9i alirocumab and evolocumab, at wholesale acquisition cost, are likely to have a smaller impact on US healthcare plans compared with prior estimates. |
To the extent that the manufacturers offer rebates and discounts to the wholesale acquisition cost, the budget impact would be even lower than the results presented herein. |
1 Introduction
Cardiovascular disease (CVD) is considered one of the leading causes of mortality in the US and worldwide [1]. The American Heart Association estimated that the combined direct and indirect costs of CVD and stroke in the US in 2012 was $316.6 billion [2]. Hypercholesterolemia, particularly elevated low-density lipoprotein cholesterol (LDL-C) levels, constitutes a major risk factor for the development of atherosclerotic CVD (ASCVD) and an increased risk of cardiovascular (CV) events [3, 4]. A positive relationship has been established between the lowering of blood cholesterol and LDL-C levels and the reduction of CV event rates [3, 5,6,7,8,9,10]. Statins are endorsed in current treatment guidelines to reduce LDL-C in both the primary and secondary prevention setting [4, 11,12,13,14]; however, as many as 8.1 million patients with clinical ASCVD in the US fail to achieve the recommended reduction of lipid levels necessary to optimally reduce the risk of CV events despite treatment with a statin [15,16,17].
Non-statin lipid-modification therapy (LMT) may be added to statin therapy for patients who continue to have high LDL-C despite treatment with maximally tolerated doses of statins or who are intolerant to statin therapy [4, 13]. Inhibitors of proprotein convertase subtilisin/kexin type 9 (PCSK9), which is involved in the control of LDL-C receptor degradation, represent a new class of non-statin LMT for use as an adjunct treatment with statins in patients with elevated LDL-C [18]. In phase II and III studies, treatment with the PCSK9 inhibitors (PCSK9i) alirocumab and evolocumab has been shown to be an efficacious and well-tolerated approach to lower LDL-C levels [19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36]. Both alirocumab and evolocumab were approved by the US FDA in 2015 as an adjunct to diet and maximally tolerated statin therapy for the treatment of adults with heterozygous familial hypercholesterolemia (HeFH) or clinical ASCVD who require additional lowering of LDL-C levels [18, 37], and the treatments are now included in European and US guidelines for these specific patient groups [38, 39].
The efficacy and long-term safety of PCSK9i for the treatment of individuals with hypercholesterolemia, clinical ASCVD, HeFH and/or homozygous familial hypercholesterolemia (HoFH) have been evaluated in the phase III ODYSSEY programme for alirocumab, and the PROFICIO programme for evolocumab. Data from the ODYSSEY and PROFICIO clinical programmes suggest sustained LDL-C reductions of up to 61% after 12 weeks associated with alirocumab [29] and evolocumab [34]. Despite endorsements of their clinical value, the perceived costs and budgetary concerns of treatment-eligible patients [40] are likely to have had a role in the limited uptake of PCSK9i in resource-constrained health systems [41]. Therefore, further evidence of their economic impact to healthcare budgets, with particular consideration of eligible patient groups, is warranted to support formulary adoption and treatment decision making [42]. This evaluation examined the pharmacy and total healthcare budget impacts of introducing alirocumab and evolocumab to a US health plan as a treatment modality for adult patients with HeFH or clinical ASCVD who are treated with statins and require additional LDL-C lowering.
2 Methods
2.1 Model Overview
The budget impact model estimated pharmacy (i.e. LMT) costs and total healthcare costs (i.e. costs of LMT and CV events) for a US health plan over a 3-year period. Two scenarios were evaluated with respect to the utilization of PCSK9i among patients with HeFH and ASVCD receiving statins and with uncontrolled LDL-C: (1) the reference case, in which PCSK9i was not an option for add-on LMT; and (2) the new case, with PCSK9i as an option for these patients, based on real-world data and modelling assumptions. The expected budget impact of PCSK9i was calculated as the difference in pharmacy and total healthcare costs for the target population between these two scenarios (electronic supplementary Fig. 1).
For each scenario and each year of the 3-year projection period, total undiscounted annual LMT medication, dispensing and healthcare costs, including the costs of CV events, were estimated for all prevalent patients in the target population. The model was developed in Microsoft Excel 2007 (Microsoft Corporation, Redmond, WA, USA) and complied with recommendations of the Academy of Managed Care Pharmacy Format for Formulary Submissions [43] and the International Society for Pharmacoeconomics and Outcomes Research Principles of Good Practice for Budget Impact Analysis [42].
2.2 Target Population
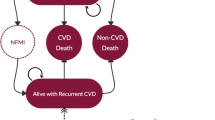
The target population in the model included all adults (≥ 18 years) with HeFH or clinical ASCVD who were treated with statins and had uncontrolled LDL-C, defined as LDL-C > 70 mg/dL. Patients were stratified into two age groups: 18–64 and ≥ 65 years. Patients were then assigned to two mutually exclusive subgroups hierarchically ranked (highest first) by presumed CV risk [44] (electronic supplementary Tables 1a and b): (1) HeFH (with or without clinical ASCVD); or (2) clinical ASCVD (without HeFH). The clinical ASCVD subgroup included (a) acute coronary syndrome, (b) history of ischemic stroke, (c) history of myocardial infarction (MI), (d) history of other coronary heart disease, and (e) peripheral artery disease (Fig. 1).
The base-case estimates of the percentage of patients in each age and risk group, as well as the percentages of patients within each group with uncontrolled LDL-C, including those with uncontrolled LDL-C receiving statins (electronic supplementary Table 2), were estimated from real-world data derived from the Truven Health MarketScan® Research Databases of a large US commercial managed care database representing an employer-sponsored health plan population in 2013 (Truven Health Analytics, Ann Arbor, MI, USA; and data on file, Regeneron Pharmaceuticals, Inc., and Sanofi US). The prevalence of ASCVD, adjusted for age, sex and high CV risk conditions, was then extrapolated to the US population (electronic supplementary Table 1b) [16, 45,46,47]. The proportion of these patients receiving LMT, and, of those receiving LMT, the proportion achieving LDL-C thresholds of < 100 and < 70 mg/dL [16, 45,46,47], was then estimated. The target patient population and growth trends in the hypothetical health plan assumed that the 1 million members followed the US Census Bureau general population age distribution and population growth rate (0.74%) [48].
2.3 Treatment Combination and Cost
Data on the combinations of LMTs received by the target population under the reference scenario were derived from the Truven MarketScan data and extrapolated to the US population as above (Table 1) (data on file, Regeneron Pharmaceuticals, Inc., and Sanofi US) [16, 45,46,47,48,49].
LMTs were classified into the following four categories: (1) statin monotherapy; (2) statin and ezetimibe; (3) statin and other LMT (including niacin and bile acid sequestrants); (4) statin and PCSK9i. The model did not consider any triple therapy in its calculation given the already low utilization rate of ezetimibe.
For PCSK9i, it was assumed that 3-year utilization would follow the same pattern as current ezetimibe use, although in a secondary analysis a higher rate was applied based on the uptake rates for statins after the first 5 years on the market [50, 51]. Therefore, the percentage of patients in the target population who would receive PCSK9i was assumed to increase linearly each year to maximum rates at year 3, while the use of statins and other LMT were proportionally reduced. In the base case, PCSK9i utilization started at 0.33% in year 1 and increased 0.33% each year, reaching a maximum of 1% for all risk groups, except HeFH, which started at 1.67% in year 1 and increased by 1.67% each year to a maximum of 5% (Table 2). The higher 5% utilization rate for HeFH was applied since treatments for this condition are limited and based on real-world uptake for alirocumab through September 2016 (data on file, Regeneron Pharmaceuticals, Inc., and Sanofi US). In the secondary analysis, the maximum PCSK9i utilization rate was increased to 5% for all risk groups, except HeFH, which reached 10% at year 3. Utilization rates across all risk groups were assumed to be equivalent between age groups.
The 2017 wholesale acquisition costs (WACs) were applied for alirocumab, evolocumab and all other LMTs (Truven Health Analytics, Ann Arbor, MI, USA) (Table 3). Alirocumab and evolocumab were both assumed to be self-administered as subcutaneous injection once every 2 weeks, with the cost of PCSK9i treatments based on their average ($558.58 per injection, $39.90 per day, or $14,563.50 per year), given that the present analysis evaluates the budgetary impact of the treatment class based on their equivalent efficacy [38]. The cost of dispensing for all drugs was estimated to be $10.50 per prescription, based on a study of the costs of dispensing drugs in community pharmacies in the US [52]. It was assumed that PCSK9i would be dispensed as a 1-month supply (two injections) every 4 weeks.
Because data on adherence with a combination of a statin and PCSK9i in a real-world setting are unavailable, estimates were based on median adherence to subcutaneous exenatide (78%) administered once every 7 days, which was the nearest analogue given its similar method of administration (subcutaneous injection) [53]. Adherence with other LMTs was assumed to equal 58%, as estimated in a retrospective claims-based study of statin utilization in high CV-risk patients [49]. The analyses assumed no discounts, rebates, co-payments, or co-insurances on the cost of medications. Estimates of total LMT costs for the reference case and for the scenario with PCSK9i, including its budget impact, were made in terms of per-patient per-month (PPPM) and per-member per-month (PMPM).
2.4 Costs of Cardiovascular Events
For the estimation of the total healthcare budget impact of introducing PCSK9i to a health plan, the model also considered the potential cost-offsets resulting from expected reductions in CV events associated with reductions in LDL-C. The estimated incremental mean percentage LDL-C reductions for PCSK9i + statin were 57.0% versus statin monotherapy [54], 36.10% versus statin + ezetimibe [54], and 36.10% versus statin + other LMT. Adherence to PCSK9i (78%) was also taken into account in the estimation of CV events.
CV events considered were MI, unstable angina, revascularization, ischemic stroke and CV death. As CV event data have only recently become available for evolocumab [55], with results for alirocumab expected in 2018, the annual CV event incidence was calculated using CV-risk functions derived from estimates of the relative risk reduction associated with lowering LDL-C. Relative risks were obtained from the Cholesterol Treatment Trialists’ (CTT) Collaboration meta-analysis [11]; baseline risk estimates were derived from the Truven MarketScan Research Database in which patients were assigned to two mutually exclusive CV risk-based subgroups (Regeneron Pharmaceuticals, Inc., and Sanofi US) (electronic supplementary Table 1c) [44]. The CTT meta-analysis was based on statin trials and the data were assumed to be generalizable to other cholesterol-lowering therapies.
Costs of CV events were based on estimates from a study by O’Sullivan and colleagues [56] that used data from a variety of sources for event costs and costs in the first, second and third year after the event. Drug costs were based on WACs, and costs for CV events were based on administrative claims data from a large US health for enrolees aged ≥ 35 years making a claim for a CV event any time during 2003. Generalized linear models were fitted to develop cost prediction equations for selected CV events, including ischemic stroke, MI, unstable angina, revascularization procedures and CV-related death. Separate equations were used for patients with events and for their propensity score-matched controls. Acute costs were equal to the sum of event costs and first-year costs. Long-term costs were equal to the average of year 2 and year 3 costs. For patients in whom multiple events occurred simultaneously (e.g. hospitalization for MI in which revascularization took place), the event was included as a case for the procedure (e.g. revascularization) rather than the diagnosis (MI). Costs were adjusted to 2015 price levels using the Consumer Price Index (CPI) for medical care (Table 4). The per event, annual costs of CV events for the target population were assumed to be equivalent for risk and age groups, and for both scenarios.
2.5 Sensitivity Analyses
Sensitivity analyses were conducted around PPPM total healthcare costs. Key parameters, including costs of CV events and percentages of plan members in different age and population groups, were varied between plausible ranges. The PCSK9i utilization rate and costs of alirocumab and evolocumab injections varied by ± 50%, while the percentage of plan members with uncontrolled LDL-C varied by ± 25%.
2.6 Payer Perspective Analysis
As a separate scenario, the budget impact of PCSK9i was calculated from the perspective of commercial and Medicare Advantage health plans. In these analyses, the age distribution of the population was set to match the age distribution of a typical health plan of each type, which was derived from data from the US Census Bureau and America’s Health Insurance Plans [57,58,59,60].
3 Results
3.1 Target Population and Treatment Costs
For the hypothetical health plan of 1 million members, 62.6% were assumed to be between 18 and 64 years of age, and 14.1% were aged ≥ 65 years (23.3% were under 18 years of age). Depending on the age group, 0.1–0.2% of plan members were estimated to have HeFH, and 0.4–8.5% were estimated to have clinical ASCVD [16] (Table 1) [16]. All patients with HeFH were estimated to have uncontrolled LDL-C, and most (90.3–96.7%) received statin therapy. Similarly, most of the patients who had clinical ASCVD were estimated to have uncontrolled LDL-C (58.2–78.9%). Depending on the age and risk group, between 35.9 and 67.4% of these patients were estimated to have received a statin. The number of patients in the target population who would receive PCSK9i was projected to increase from 112 in year 1 to 340 in year 3 (Table 2), for a total of 676 person-years of treatment over years 1–3.
LMT costs for the reference scenario were estimated to increase from $6.66 million in year 1 to $6.76 million in year 3 due to population growth. With the introduction of PCSK9i, assuming 1–5% utilization in the base case, LMT costs in the target population were projected to be $7.94 million, $9.29 million and $10.66 million for years 1, 2 and 3, respectively (electronic supplementary Fig. 2a). This would result in a 3-year pharmacy budget increase of $7.76 million.
On the basis of PPPM (and PMPM), LMT costs were estimated to be $19.94 ($0.56) for each year of the reference scenario. With the introduction of PCSK9i, PPPM (PMPM) LMT costs were projected to increase to $23.78 ($0.66), $27.61 ($0.77) and $31.44 ($0.88) for years 1, 2 and 3, respectively (electronic supplementary Fig. 2b).
For the reference scenario, it was estimated that a total of 5667 CV events (1875, 1889 and 1903 for years 1, 2 and 3, respectively) would occur in the target population (i.e. adults in a plan with ASCVD or HeFH and uncontrolled LDL-C receiving statins). In the new scenario, the introduction of PCSK9i was projected to reduce the number of CV events by 10.2, to a total of 5656 events over 3 years. As a consequence of the CV events avoided with the introduction of PCSK9i, a cost offset of $0.46 million would be realized ($0.07, $0.15 and $0.24 million for years 1, 2 and 3, respectively) (electronic supplementary Fig. 2c).
By incorporating these cost offsets, the introduction of PCSK9i would yield a net total healthcare budget increase of $1.21 million, $2.43 million and $3.66 million for each of years 1, 2 and 3, respectively ($7.30 million over 3 years). On a PPPM (PMPM) basis, total healthcare costs would range from $1652 ($45.99), $1675 ($46.65) to $1699 ($47.30) for each of the years 1, 2 and 3, respectively, for the reference scenario, and from $1655 ($46.09), $1683 ($46.85) to $1709 ($47.60) for years 1, 2 and 3, respectively, after the introduction of PCSK9i (electronic supplementary Fig. 2d), resulting in a PPPM (PMPM) total healthcare budget impact of $7.23 ($0.20) for the 3-year period.
When PCSK9i utilization rates were increased to 5–10% over the 3 years, the number of patients receiving PCSK9i in the target population increased from 487 in year 1 to 1484 in year 3 (Table 2), for a total of 2953 person-years of treatment over the 3-year period. Compared with the reference scenario, 3-year LMT costs increased by $33.89 million (increments of $5.59 million in year 1 to $17.03 million in year 3) (electronic supplementary Fig. 2a). At higher utilization of PCSK9i, PPPM (PMPM) LMT costs were $36.68 ($1.02), $53.43 ($1.49) and $70.17 ($1.95) in years 1, 2 and 3, respectively (electronic supplementary Fig. 2b), resulting in a 3-year pharmacy budget impact of $33.56 ($0.93) and total healthcare budget impact of $31.56 ($0.88).
With the increased utilization of PCSK9i, compared with the reference scenario, a total of 45.5 fewer CV events for the new scenario were projected (decreasing by 7.5, 15.1 and 22.8 for years 1, 2 and 3, respectively) over 3 years. This would result in 3-year CV event-related cost savings of $2.02 million ($0.31, $0.66 and $1.05 million for years 1, 2 and 3, respectively) (electronic supplementary Fig. 2c). Total healthcare costs PPPM (PMPM) would range from $1668 ($46.43), $1707 ($47.52) to $1746 ($48.61) for years 1, 2 and 3, respectively (electronic supplementary Fig. 2d), resulting in a PPPM (PMPM) total healthcare budget impact of $31.56 ($0.88) for the 3-year period.
3.2 Sensitivity Analyses
Model results were most sensitive to model timeframe and years to maximum utilization of PCSK9i for ages 18–64 years (each varied from 1 to 5 years); low and high parameter values for these variables ranged from $3.62 to $8.62, and $9.32 to $5.53, respectively. Alirocumab and evolocumab injection costs, which varied from $280.00 to $840.00, and $279.29 to $837.87, respectively, produced PPPMs ranging from $5.70 to $8.75, and $5.70 to $8.74 (Fig. 2, electronic supplementary Table 3).
Tornado diagram of sensitivity analysis (per-member per-month). ACS acute coronary syndrome, ASCVD atherosclerotic cardiovascular disease, CHD coronary heart disease, HeFH heterozygous familial hypercholesterolemia, IS ischemic stroke, LDL-C low-density lipoprotein cholesterol, LMT lipid-modifying therapy, MI myocardial infarction, PAD peripheral artery disease, PCSK9i proprotein convertase subtilisin/kexin type 9 inhibitors. †A parameter where the high value returned a larger budgetary impact. *A parameter where the low value returned a larger budgetary impact
3.3 Payer Perspective
From the perspective of different healthcare payers (Table 5), assuming 1–5% utilization rates for PCSK9i, the projected number of eligible patients in the base case of 1 million members ranged from a 3-year total of 494 for a commercial health plan, to 1831 for a Medicare Advantage health plan. The incremental cost of LMT over the 3-year period was lower for a commercial health plan ($5.7 million higher than in the reference scenario) than for a typical Medicare Advantage health plan ($21.1 million higher than in the reference scenario). For a commercial health plan, 3-year PPPM (PMPM) total healthcare costs increased by $8.08 ($0.15) compared with the reference scenario, whereas for a Medicare Advantage health plan, PPPM (PMPM) total healthcare costs increased by $6.26 ($0.58). Similar trends were observed assuming 5–10% PCSK9i utilization rates (Table 5).
4 Discussion
This budget impact analysis demonstrated that, assuming the percentage of patients receiving PCSK9i would increase linearly over time to 1–5% of the eligible population in 3 years, adding PCSK9i to the formulary at the list price would result in incremental PPPM (PMPM) total healthcare costs of $3.62 ($0.10) in the first year, up to $10.79 ($0.30) in the third year of the projection compared with the reference scenario without the availability of PCSK9i. However, the model did not include rebates or discounts that drug manufacturers may offer to payers. For example, the Medicaid Drug Rebate Program requires a drug manufacturer to have a national rebate agreement with the Secretary of the Department of Health and Human Services in exchange for state Medicaid coverage [61]. If the Medicaid rebate of at least 23.1% for innovator drugs was applied to PCSK9i for a health plan, the PPPM (PMPM) total healthcare impact would be $2.74 ($0.08), $5.46 ($0.15) and $8.16 ($0.22) in years 1, 2 and 3, respectively, in the base case, and $11.98 ($0.33), $23.85 ($0.66) and $35.62 ($0.99) in years 1, 2 and 3, respectively, with 5–10% utilization.
In addition, the increase in PMPM LMT costs associated with the addition of PCSK9i compared with the reference scenario is substantially less than the PMPM costs reported for the most commonly used specialty therapy drugs. In year 3, the increased LMT cost with the addition of PCSK9i ($0.32 PMPM at a maximum utilization rate of 1–5% over 3 years) is lower than the year 1 PMPM cost (including discounts and rebates) for the top three specialty therapy drugs, which range from $2.80 for adalimumab to $1.78 for the ledipasvir and sofosbuvir combination [62]. With a maximum utilization rate of 5–10% over 3 years, the incremental LMT cost of adding PCSK9i ($0.93 PMPM) remains lower than the PMPM cost for other biologics such as adalimumab.
On a population level, our analysis estimated that the availability of PCSK9i will increase the cost of LMT therapy in a hypothetical plan of 1 million members by $7.76 million over 3 years, assuming a maximum utilization rate of 5% within 3 years. When adjusted to the US population, this reflects a cost increase of approximately $1.7 billion.
A comparison of our results with other recent economic evaluations of PCSK9i is warranted. Kazi et al. estimated the budget impact of alirocumab and evolocumab combined use in all eligible patients in the US, and obtained increased net healthcare costs of $120 billion over 5 years [63]. However, their estimate was likely to be driven by the substantially higher estimates of uptake of the anti-PCSK9 antibodies in the analysis compared with the estimates used in the analysis reported in this study. Their assumption that 61% of patients with familial hypercholesterolemia and 65% of patients with ASCVD would initiate therapy with the two currently available PCSK9i at 5 years (corresponding to an uptake of 37% and 39% after 3 years, respectively) appear to significantly exceed those reported for the current use of ezetimibe and other LMT (not including PCSK9i) [51], and for statins in the first 5 years on the market [50], whereas in the current analysis, it was presumed that PCSK9i would be utilized at a maximum rate of 1–5 or 5–10% in the third year of the projection.
Separately, a recent commentary by Schulman and colleagues projected that the addition of PCSK9i to the hyperlipidemia treatment armamentarium would increase costs across the insurance pool by $10.33 PMPM if 5% of adults aged 40–64 years who had elevated LDL-C levels were eligible for treatment with PCSK9i [64]. The time frame and analysis details are not specified in the commentary, making direct comparisons difficult. The increased cost after the addition of PCSK9i reported by Schulman et al. is greater than the estimates described in this study ($1.36 PMPM at 3 years, assuming a utilization rate of 5% after 3 years). This may in part be due to the pool of eligible patients considered in the commentary, which appears to be much more broadly defined and therefore larger than that used in the model described herein. The population utilized in the present analysis closely corresponds to the alirocumab and evolocumab product labelling (i.e. eligible patients had HeFH or clinical ASCVD and were receiving statin treatment and had uncontrolled LDL-C (≥ 70 mg/dL)).
This study has several limitations. First, data on the actual utilization of PCSK9i were not available at the time this analysis was conducted and were therefore assumed to be either 1–5 or 5–10% of the target population, reflecting the historical uptake of ezetimibe and statins and the usage patterns of PCSK9i in the HeFH population. Furthermore, the alirocumab ODYSSEY OUTCOMES trial is still ongoing and the early results of the evolocumab FOURIER trial have only just become available [55]; these studies will indicate the effect of treatment with PCSK9i on long-term CV-related mortality and morbidity [65, 66]. Therefore, estimates of the potential savings associated with a potential reduction in CV morbidity and mortality resulting from the introduction of PCSK9i to the market were based on data on reductions in LDL-C with PCSK9i and information on the effect of changes in LDL-C on CV risk for statins. Analyses accounting for these potential benefits will be performed when the results and analyses of both these trials are available. The model also does not include the cost of treatment for adverse events, nor other related healthcare events that may be associated with the PCSK9i treatment. However, it appears unlikely that substantial costs related to adverse events will be incurred, given that pooled analysis of recently completed ODYSSEY and PROFICIO phase III programmes indicated that treatment-emergent adverse events were generally transient and similar between the alirocumab, evolocumab and control groups [67]. Additionally, the costs of CV events were based on resource use data published in 2011 (2007 values) [56]. Given that healthcare costs in the US increased by 3.6–4.0% yearly between 2010 and 2013 [68], it is possible that the costs may have been slightly underrepresented. However, comparisons of results based on costs in the MarketScan data were similar to those based on recently published WACs [50]. Finally, further extrapolation to non-commercial Medicare and Medicaid populations is warranted but would require additional data to account for factors that could predispose these cohorts to treatment, e.g. comorbid conditions and socioeconomic status, and other factors as likely predictors of PCSK9i use in these populations.
5 Conclusions
Assuming that the maximum utilization rate of PCSK9i among patients with clinical ASCVD or HeFH receiving statins and with uncontrolled LDL-C would be 1–5% after 3 years, the introduction of PCSK9i was estimated to increase total healthcare costs in a hypothetical US health plan by $3.62 PPPM ($0.10 PMPM) at year 1, to $10.79 PPPM ($0.30 PMPM) at year 3. If the manufacturers offer rebates and discounts to the list price, the budget impact would be lower than the results presented herein. The budget impact analysis of PCSK9i introduction will be updated when the mortality and morbidity data from both ongoing long-term outcomes trials and real-world data on alirocumab and evolocumab uptake are available.
Data Availability Statement
The datasets generated and/or analysed during the current study are available upon reasonable request to the corresponding author.
References
Pagidipati NJ, Gaziano TA. Estimating deaths from cardiovascular disease: a review of global methodologies of mortality measurement. Circulation. 2013;127(6):749–56.
Mozaffarian D, Benjamin EJ, Go AS, Arnett DK, Blaha MJ, Cushman M, et al. Heart disease and stroke statistics—2016 update: a report from the American Heart Association. Circulation. 2016;133(4):e38–360.
Sharrett AR, Ballantyne CM, Coady SA, Heiss G, Sorlie PD, Catellier D, et al. Coronary heart disease prediction from lipoprotein cholesterol levels, triglycerides, lipoprotein(a), apolipoproteins A-I and B, and HDL density subfractions: the Atherosclerosis Risk in Communities (ARIC) study. Circulation. 2001;104(10):1108–13.
Jacobson TA, Ito MK, Maki KC, Orringer CE, Bays HE, Jones PH, et al. National Lipid Association recommendations for patient-centered management of dyslipidemia: part 1—full report. J Clin Lipidol. 2015;9(2):129–69.
Cohen JC, Boerwinkle E, Mosley THJ, Hobbs HH. Sequence variations in PCSK9, low LDL, and protection against coronary heart disease. N Engl J Med. 2006;354(12):1264–72.
Ference BA, Yoo W, Alesh I, Mahajan N, Mirowska KK, Mewada A, et al. Effect of long-term exposure to lower low-density lipoprotein cholesterol beginning early in life on the risk of coronary heart disease: a Mendelian randomization analysis. J Am Coll Cardiol. 2012;60(25):2631–9.
Hubert HB, Feinleib M, McNamara PM, Castelli WP. Obesity as an independent risk factor for cardiovascular disease: a 26-year follow-up of participants in the Framingham Heart Study. Circulation. 1983;67(5):968–77.
Humphries SE, Whittall RA, Hubbart CS, Maplebeck S, Cooper JA, Soutar AK, et al. Genetic causes of familial hypercholesterolaemia in patients in the UK: relation to plasma lipid levels and coronary heart disease risk. J Med Genet. 2006;43(12):943–9.
Prospective Studies Collaboration. Blood cholesterol and vascular mortality by age, sex, and blood pressure: a meta-analysis of individual data from 61 prospective studies with 55,000 vascular deaths. Lancet. 2007;370(9602):1829–39.
Stamler J, Wentworth D, Neaton JD. The Multiple Risk Factor Intervention Trial (MRFIT)—importance then and now. JAMA. 2008;300(11):1343–5.
Cholesterol Treatment Trialists’ (CTT) Collaboration. Efficacy and safety of LDL-lowering therapy among men and women: meta-analysis of individual data from 174,000 participants in 27 randomised trials. Lancet. 2015;385(9976):1397–405.
Cannon CP, Blazing MA, Giugliano RP, McCagg A, White JA, Theroux P, et al. Ezetimibe added to statin therapy after acute coronary syndromes. N Engl J Med. 2015;372(25):2387–97.
Stone NJ, Robinson JG, Lichtenstein AH, Bairey Merz CN, Blum CB, Eckel RH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol. 2014;63(25 Pt B):2889–934.
Reiner Ž, Catapano AL, De Backer G, Graham I, Taskinen M-R, Wiklund O, et al. ESC/EAS guidelines for the management of dyslipidaemias. Eur Heart J. 2011;32(14):1769–818.
Cohen JD, Brinton EA, Ito MK, Jacobson TA. Understanding Statin Use in America and Gaps in Patient Education (USAGE): an internet-based survey of 10,138 current and former statin users. J Clin Lipidol. 2012;6(3):208–15.
Gorcyca K, Khan I, Wadhera R, Klimchak A, Song X, Sanchez R, et al. Prevalence of atherosclerotic cardiovascular disease (ASCVD) and diabetes populations in the United States [abstract]. J Clin Lipidol. 2015;9(3):424.
Wong ND, Young D, Zhao Y, Nguyen H, Caballes J, Khan I, et al. Prevalence of the American College of Cardiology/American Heart Association statin eligibility groups, statin use, and low-density lipoprotein cholesterol control in US adults using the National Health and Nutrition Examination Survey 2011–2012. J Clin Lipidol. 2016;10(5):1109–18.
US Food and Drug Administration. Drugs@FDA. Drugs@FDA 2015. http://www.accessdata.fda.gov/scripts/cder/drugsatfda/index.cfm. Accessed February 15 2017.
Roth EM, McKenney JM, Hanotin C, Asset G, Stein EA. Atorvastatin with or without an antibody to PCSK9 in primary hypercholesterolemia. N Engl J Med. 2012;367(20):1891–900.
McKenney JM, Koren MJ, Kereiakes DJ, Hanotin C, Ferrand AC, Stein EA. Safety and efficacy of a monoclonal antibody to proprotein convertase subtilisin/kexin type 9 serine protease, SAR236553/REGN727, in patients with primary hypercholesterolemia receiving ongoing stable atorvastatin therapy. J Am Coll Cardiol. 2012;59(25):2344–53.
Stein EA, Gipe D, Bergeron J, Gaudet D, Weiss R, Dufour R, et al. Effect of a monoclonal antibody to PCSK9, REGN727/SAR236553, to reduce low-density lipoprotein cholesterol in patients with heterozygous familial hypercholesterolaemia on stable statin dose with or without ezetimibe therapy: a phase 2 randomised controlled trial. Lancet. 2012;380(9836):29–36.
Ginsberg HN, Rader DJ, Raal FJ, Guyton JR, Baccara-Dinet MT, Lorenzato C, et al. Efficacy and safety of alirocumab in patients with heterozygous familial hypercholesterolemia and LDL-C of 160 mg/dl or higher. Cardiovasc Drugs Ther. 2016;30(5):473–83.
Cannon CP, Cariou B, Blom D, McKenney JM, Lorenzato C, Pordy R, et al. Efficacy and safety of alirocumab in high cardiovascular risk patients with inadequately controlled hypercholesterolaemia on maximally tolerated doses of statins: the ODYSSEY COMBO II randomized controlled trial. Eur Heart J. 2015;36(19):1186–94.
Kereiakes DJ, Robinson JG, Cannon CP, Lorenzato C, Pordy R, Chaudhari U, et al. Efficacy and safety of the proprotein convertase subtilisin/kexin type 9 inhibitor alirocumab among high cardiovascular risk patients on maximally tolerated statin therapy: the ODYSSEY COMBO I study. Am Heart J. 2015;169(6):906–915 e13.
Robinson JG, Farnier M, Krempf M, Bergeron J, Luc G, Averna M, et al. Efficacy and safety of alirocumab in reducing lipids and cardiovascular events. N Engl J Med. 2015;372(16):1489–99.
Kastelein JJ, Ginsberg HN, Langslet G, Hovingh GK, Ceska R, Dufour R, et al. ODYSSEY FH I and FH II: 78 week results with alirocumab treatment in 735 patients with heterozygous familial hypercholesterolaemia. Eur Heart J. 2015;36(43):2996–3003.
Bays H, Gaudet D, Weiss R, Ruiz JL, Watts GF, Gouni-Berthold I, et al. Alirocumab as add-on to atorvastatin versus other lipid treatment strategies: ODYSSEY OPTIONS I randomized trial. J Clin Endocrinol Metab. 2015;100(8):3140–8.
Moriarty PM, Thompson PD, Cannon CP, Guyton JR, Bergeron J, Zieve FJ, et al. Efficacy and safety of alirocumab vs ezetimibe in statin-intolerant patients, with a statin rechallenge arm: the ODYSSEY ALTERNATIVE randomized trial. J Clin Lipidol. 2015;9(6):758–69.
Farnier M, Gaudet D, Valcheva V, Minini P, Miller K, Cariou B. Efficacy of alirocumab in high cardiovascular risk populations with or without heterozygous familial hypercholesterolemia: pooled analysis of eight ODYSSEY Phase 3 clinical program trials. Int J Cardiol. 2016;223:750–7.
Koren MJ, Scott R, Kim JB, Knusel B, Liu T, Lei L, et al. Efficacy, safety, and tolerability of a monoclonal antibody to proprotein convertase subtilisin/kexin type 9 as monotherapy in patients with hypercholesterolaemia (MENDEL): a randomised, double-blind, placebo-controlled, phase 2 study. Lancet. 2012;380(9858):1995–2006.
Giugliano RP, Desai NR, Kohli P, Rogers WJ, Somaratne R, Huang F, et al. Efficacy, safety, and tolerability of a monoclonal antibody to proprotein convertase subtilisin/kexin type 9 in combination with a statin in patients with hypercholesterolaemia (LAPLACE-TIMI 57): a randomised, placebo-controlled, dose-ranging, phase 2 study. Lancet. 2012;380(9858):2007–17.
Sullivan D, Olsson AG, Scott R, Kim JB, Xue A, Gebski V, et al. Effect of a monoclonal antibody to PCSK9 on low-density lipoprotein cholesterol levels in statin-intolerant patients: the GAUSS randomized trial. JAMA. 2012;308(23):2497–506.
Raal F, Scott R, Somaratne R, Bridges I, Li G, Wasserman SM, et al. Low-density lipoprotein cholesterol-lowering effects of AMG 145, a monoclonal antibody to proprotein convertase subtilisin/kexin type 9 serine protease in patients with heterozygous familial hypercholesterolemia: the Reduction of LDL-C with PCSK9 Inhibition in Heterozygous Familial Hypercholesterolemia Disorder (RUTHERFORD) randomized trial. Circulation. 2012;126(20):2408–17.
Sabatine MS, Giugliano RP, Wiviott SD, Raal FJ, Blom DJ, Robinson J, et al. Efficacy and safety of evolocumab in reducing lipids and cardiovascular events. N Engl J Med. 2015;372(16):1500–9.
Blom DJ, Hala T, Bolognese M, Lillestol MJ, Toth PD, Burgess L, et al. A 52-week placebo-controlled trial of evolocumab in hyperlipidemia. N Engl J Med. 2014;370(19):1809–19.
Kiyosue A, Honarpour N, Kurtz C, Xue A, Wasserman SM, Hirayama A. A phase 3 study of evolocumab (AMG 145) in statin-treated japanese patients at high cardiovascular risk. Am J Cardiol. 2016;117(1):40–7.
Repatha [package insert]. Thousand Oaks: Amgen Inc; 2015.
Writing Committee, Lloyd-Jones DM, Morris PB, Ballantyne CM, Birtcher KK, Daly DD Jr, et al. 2016 ACC expert consensus decision pathway on the role of non-statin therapies for LDL-cholesterol lowering in the management of atherosclerotic cardiovascular disease risk: a report of the American College of Cardiology Task Force on Clinical Expert Consensus Documents. J Am Coll Cardiol. 2016;68(1):92–125.
Landmesser U, Chapman MJ, Farnier M, Gencer B, Gielen S, Hovingh GK, et al. European Society of Cardiology/European Atherosclerosis Society Task Force consensus statement on proprotein convertase subtilisin/kexin type 9 inhibitors: practical guidance for use in patients at very high cardiovascular risk. Eur Heart J. 2017;38(29):2245–55.
Tice JA, Ollendorf DA, Cunningham C, Pearson SD, Kazi DS, Coxson PG, et al. PCSK9 inhibitors for treatment of high cholesterol: effectiveness, value, and value-based price benchmarks. Final report. Institute for Clinical and Economic Review; 2015. https://icerreview.org/wp-content/uploads/2016/01/Final-Report-for-Posting-11-24-15-1.pdf. Accessed August 20 2017.
Sabatine MS. Proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibitors: comparing and contrasting guidance across the Atlantic. Eur Heart J. 2017;38(29):2256–8.
Sullivan SD, Mauskopf JA, Augustovski F, Jaime Caro J, Lee KM, Minchin M, et al. Budget impact analysis—principles of good practice: report of the ISPOR 2012 Budget Impact Analysis Good Practice II Task Force. Value Health. 2014;17(1):5–14.
FMCP Format Executive Committee. The AMCP format for formulary submissions version 3.0. J Manag Care Pharm. 2010;16(1 Suppl A):1–30.
Steen DL, Khan I, Song X, Sanchez R, Gorcyca K, Hollenbeak C, et al. Cardiovascular event rates in a high-risk managed care population in the United States [abstract A1647]. J Am Coll Cardiol. 2015;65(10_S).
Allison MA, Ho E, Denenberg JO, Langer RD, Newman AB, Fabsitz RR, et al. Ethnic-specific prevalence of peripheral arterial disease in the United States. Am J Prev Med. 2007;32(4):328–33.
Blackwell DL, Lucas JW, Clarke TC. Summary health statistics for US adults: National Health Interview Survey, 2012. Vital Health Stat. 2014;10(260):1–161.
Goldberg AC, Hopkins PN, Toth PP, Ballantyne CM, Rader DJ, Robinson JG, et al. Familial hypercholesterolemia: screening, diagnosis and management of pediatric and adult patients: clinical guidance from the National Lipid Association Expert Panel on Familial Hypercholesterolemia. J Clin Lipidol. 2011;5(3 Suppl):S1–8.
US Census Bureau. Annual estimates of the resident population for selected age groups by sex for the United States, states, counties, and Puerto Rico Commonwealth and municipios: April 1, 2010 to July 1, 2013. 2013. http://factfinder.census.gov/faces/tableservices/jsf/pages/productview.xhtml?src=bkmk. Accessed February 15 2017.
Lin I, Sung J, Sanchez RJ, Mallya UG, Friedman M, Panaccio M, et al. Patterns of statin use in a real-world population of patients at high cardiovascular risk. J Manag Care Spec Pharm. 2016;22:685–98.
Davidson MH, Maki KC, Pearson TA, Pasternak RC, Deedwania PC, McKenney JM, et al. Results of the National Cholesterol Education (NCEP) Program Evaluation ProjecT Utilizing Novel E-Technology (NEPTUNE) II survey and implications for treatment under the recent NCEP Writing Group recommendations. Am J Cardiol. 2005;96(4):556–63.
Leerink Partners LLC. MEDACorp survey: use of anti-PCSK9s in hypercholesterolemia 2014. http://mpi-group.com/wp-content/uploads/2012/05/CostofDispensingStudy_GT.pdf. Accessed February 11 2016.
Grant Thornton LLP. National cost of dispensing study: final report. Coalition for Community Pharmacy Action; 2007.
Johnston SS, Nguyen H, Felber E, Cappell K, Nelson JK, Chu B-C, et al. Retrospective study of adherence to glucagon-like peptide-1 receptor agonist therapy in patients with type 2 diabetes mellitus in the United States. Adv Ther. 2014;31(11):1119–33.
Sanofi-aventis US LLC Regeneron Pharmaceuticals Inc. FDA Advisory Committee Briefing Document Praluent (alirocumab) BLA 125559 Endocrinologic and Metabolic Drugs Advisory Committee Metting Date: June 9, 2015. 2015; http://www.fda.gov/downloads/AdvisoryCommittees/CommitteesMeetingMaterials/Drugs/EndocrinologicandMetabolicDrugsAdvisoryCommittee/UCM449867.pdf. Accessed February 15 2017.
Sabatine MS, Giugliano RP, Keech AC, Honarpour N, Wiviott SD, Murphy SA, et al. Evolocumab and clinical outcomes in patients with cardiovascular disease. N Engl J Med (Epub 17 Mar 2017).
O’Sullivan AK, Rubin J, Nyambose J, Kuznik A, Cohen DJ, Thompson D. Cost estimation of cardiovascular disease events in the US. Pharmacoeconomics. 2011;29(8):693–704.
America’s Health Insurance Plans. Medicare advantage demographics report; 2015. https://www.ahip.org/wp-content/uploads/2017/05/Medigap_Report_5.1.17.pdf. Accessed February 11 2016.
US Census Bureau. Table HI01. Health insurance coverage status and type of coverage by selected characteristics: 2013. US Census Bureau; 2014. https://www.census.gov/data/tables/time-series/demo/income-poverty/cps-hi/hi-01.2014.html. Accessed February 15 2017.
Smith JC, Medalia C. Health Insurance Coverage in the United States: 2014; 2015. https://www.census.gov/content/dam/Census/library/publications/2015/demo/p60-253.pdf. Accessed February 11 2016.
US Census Bureau Population Division. Table 9. Projections of the Population by Sex and Age for the United States: 2015 to 2060 (NP2014-T9). US Census Bureau; 2014.
Medicaid Drug Rebate Program. Medicaid website. 2016 February 5, 2015; https://www.medicaid.gov/Medicaid-CHIP-Program-Information/By-Topics/Benefits/Prescription-Drugs/Medicaid-Drug-Rebate-Program.html. Accessed February 15 2017.
The Express Scripts Lab. The 2015 Drug Tend Report. March 2016. http://lab.express-scripts.com/lab/drug-trend-report. Accessed February 15 2017.
Kazi DS, Moran AE, Coxson PG, Penko J, Ollendorf DA, Pearson SD, et al. Cost-effectiveness of PCSK9 inhibitor therapy in patients with heterozygous familial hypercholesterolemia or atherosclerotic cardiovascular disease. JAMA. 2016;316(7):743–53.
Schulman KA, Balu S, Reed SD. Specialty pharmaceuticals for hyperlipidemia—impact on insurance premiums [editorial]. N Engl J Med. 2015;373(17):1591–3.
Schwartz GG, Bessac L, Berdan LG, Bhatt DL, Bittner V, Diaz R, et al. Effect of alirocumab, a monoclonal antibody to PCSK9, on long-term cardiovascular outcomes following acute coronary syndromes: rationale and design of the ODYSSEY Outcomes trial. Am Heart J. 2014;168(5):682–9.
Sabatine MS, Giugliano RP, Keech A, Honarpour N, Wang H, Liu T, et al. Rationale and design of the Further cardiovascular OUtcomes Research with PCSK9 Inhibition in subjects with Elevated Risk trial. Am Heart J. 2016;173:94–101.
Bays HE, Leiter LA, Colhoun HM, Thompson D, Bessac L, Pordy R, et al. Alirocumab treatment effect on non-HDL-C: pooled analyses of 10 phase 3 trials in the ODYSSEY program [abstract A183]. J Clin Lipidol. 2015;9(3):471.
National Center for Health Statistics. Health, United States, 2014: with special feature on adults aged 55–64. Hyattsville: National Center for Health Statistics; 2015. https://www.cdc.gov/nchs/data/hus/hus14.pdf. Accessed February 11 2016.
Acknowledgements
The authors would like to thank Sean Sullivan for contributing to the initial study concept and data analysis, and Emilie Duchesneau for her assistance conducting the analysis. Medical writing assistance and editorial support, under the direction of the authors, were respectively provided by Gauri Saal, MA Economics, and Elke Sims of Prime (Knutsford, UK), funded by Sanofi/Regeneron according to Good Publication Practice guidelines (http://annals.org/aim/article/2424869). The sponsor was involved in the study design, collection, analysis and interpretation of data, as well as data checking of information provided in the article. The authors had unrestricted access to study data, were responsible for all content and editorial decisions, and received no honoraria related to the development of this publication.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Mallya, U.G., Boklage, S.H., Koren, A. et al. Budget Impact Analysis of PCSK9 Inhibitors for the Management of Adult Patients with Heterozygous Familial Hypercholesterolemia or Clinical Atherosclerotic Cardiovascular Disease. PharmacoEconomics 36, 115–126 (2018). https://doi.org/10.1007/s40273-017-0590-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40273-017-0590-5