Abstract
Objective
The objective of this article was to conduct a systematic review of published research on the use of discrete event simulation (DES) for resource modelling (RM) in health technology assessment (HTA). RM is broadly defined as incorporating and measuring effects of constraints on physical resources (e.g. beds, doctors, nurses) in HTA models.
Methods
Systematic literature searches were conducted in academic databases (JSTOR, SAGE, SPRINGER, SCOPUS, IEEE, Science Direct, PubMed, EMBASE) and grey literature (Google Scholar, NHS journal library), enhanced by manual searchers (i.e. reference list checking, citation searching and hand-searching techniques).
Results
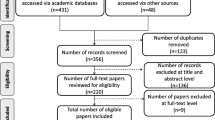
The search strategy yielded 4117 potentially relevant citations. Following the screening and manual searches, ten articles were included. Reviewing these articles provided insights into the applications of RM: firstly, different types of economic analyses, model settings, RM and cost-effectiveness analysis (CEA) outcomes were identified. Secondly, variation in the characteristics of the constraints such as types and nature of constraints and sources of data for the constraints were identified. Thirdly, it was found that including the effects of constraints caused the CEA results to change in these articles.
Conclusion
The review found that DES proved to be an effective technique for RM but there were only a small number of studies applied in HTA. However, these studies showed the important consequences of modelling physical constraints and point to the need for a framework to be developed to guide future applications of this approach.

Similar content being viewed by others
References
Weinstein M. Recommendations of the panel on cost-effectiveness in health and medicine. JAMA. 1996;276(15):1253–8.
Thokala P, Dixon S, Jahn B. Resource modelling: the missing piece of the HTA jigsaw? Pharmacoeconomics. 2015;33(3):193–203.
Marshall D, Burgos-Liz L, Ijzerman M, Osgood N, Padula W, Higashi M, et al. Applying dynamic simulation modeling methods in health care delivery research—the SIMULATE checklist: report of the ISPOR Simulation Modeling Emerging Good Practices Task Force. Value Health. 2015;18(1):5–16.
Marshall D, Burgos-Liz L, Ijzerman M, Crown W, Padula W, Wong P, et al. Selecting a dynamic simulation modeling method for health care delivery research—part 2: report of the ISPOR Dynamic Simulation Modeling Emerging Good Practices Task Force. Value Health. 2015;18(2):147–60.
Karnon J, Stahl J, Brennan A, Caro J, Mar J, Moller J. Modeling using discrete event simulation: a report of the ISPOR-SMDM Modeling Good Research Practices Task Force-4. Med Decis Mak. 2012;32(5):701–11.
Caro J, Briggs A, Siebert U, Kuntz K. Modeling good research practices—overview: a report of the ISPOR-SMDM Modeling Good Research Practices Task Force-1. Med Decis Mak. 2012;32(5):667–77.
Standfield L, Comans T, Scuffham P. Markov modeling and discrete event simulation in health care: a systematic comparison. Int J Technol Assess Health Care. 2014;30(02):165–72.
Gunal M, Pidd M. Discrete event simulation for performance modelling in health care: a review of the literature. J Simul. 2010;4(1):42–51.
Konig M, Beibert U, Steinhauer D, Bargstadt H. Constraint-based simulation of outfitting processes in shipbuilding and civil engineering. In: Eurosim Congress on Modelling and Simulation. 2007:1–11. http://citeseerx.ist.psu.edu/viewdoc/summary?doi=10.1.1.462.6589. Accessed 10 Aug 2016.
Cardoen B, Demeulemeester E, Belien J. Operating room planning and scheduling: a literature review. Eur J Oper Res. 2010;201(3):921–32.
Salleh S, Thokala P, Brennan A, Hughes R, Booth A. Simulation modelling in healthcare: an umbrella review of systematic literature reviews. Pharmacoeconomics. 2017. doi:10.1007/s40273-017-0523-3 (Epub 2017 May 30).
Caro J, Moller J, Getsios D. Discrete event simulation: the preferred technique for health economic evaluations? Value Health. 2010;13(8):1056–60.
Caro J, Moller J. Advantages and disadvantages of discrete-event simulation for health economic analyses. Expert Rev Pharmacoecon Outcomes Res. 2016;16(3):327–9.
Caro J, Moller J, Karnon J, Stahl J, Ishak J. Discrete event simulation for health technology assessment. Boca Raton: CRC Press; 2016. p. 227.
Karnon J, Haji Ali Afzali H. When to use discrete event simulation (DES) for the economic evaluation of health technologies? A review and critique of the costs and benefits of DES. Pharmacoeconomics. 2014;32(6):547–58.
Booth A. Unpacking your literature search toolbox: on search styles and tactics. Health Info Libr J. 2008;25(4):313–7.
Gough D, Oliver S, Thomas J. An introduction to systematic reviews. London: SAGE; 2012. p. 125–6.
Booth A, Papaioannou D, Sutton A. Systematic approaches to a successful literature review. London: SAGE; 2012. p. 78–9.
Stahl J. Reorganizing the system of care surrounding laparoscopic surgery: a cost-effectiveness analysis using discrete-event simulation. Med Decis Mak. 2004;24(5):461–71.
Stahl J, Sandberg W, Daily B, Wiklund R, Egan M, Goldman J, et al. Reorganizing patient care and workflow in the operating room: a cost-effectiveness study. Surgery. 2006;139(6):717–28.
Jahn B, Pfeiffer K, Theurl E, Tarride J, Goeree R. Capacity constraints and cost-effectiveness: a discrete event simulation for drug-eluting stents. Med Decis Mak. 2009;30(1):16–28.
Crane G, Kymes S, Hiller J, Casson R, Martin A, Karnon J. Accounting for costs, QALYs, and capacity constraints: using discrete-event simulation to evaluate alternative service delivery and organizational scenarios for hospital-based glaucoma services. Med Decis Mak. 2013;33(8):986–97.
Standfield L, Comans T, Raymer M, O’Leary S, Moretto N, Scuffham P. The efficiency of increasing the capacity of physiotherapy screening clinics or traditional medical services to address unmet demand in orthopaedic outpatients: a practical application of discrete event simulation with dynamic queuing. Appl Health Econ Health Policy. 2016;14(4):479–91.
Cooper K, Davies R, Raftery J, Roderick P. Use of a coronary heart disease simulation model to evaluate the costs and effectiveness of drugs for the prevention of heart disease. J Oper Res Soc. 2007;59(9):1173–81.
Cooper K, Davies R, Roderick P, Chase D, Raftery J. The development of a simulation model of the treatment of coronary heart disease. Health Care Manag Sci. 2002;5(4):259–67.
Ramwadhdoebe S. Screening for developmental dysplasia of the hip in primary care. Implementation by simulation [PhD dissertation]. Utrecht: Utrecht University; 2010. p. 77–100.
Ramsay C, Pickard R, Robertson C, Close A, Vale L, Armstrong N, et al. Systematic review and economic modelling of the relative clinical benefit and cost-effectiveness of laparoscopic surgery and robotic surgery for removal of the prostate in men with localised prostate cancer. Health Technol Assess. 2012;16(41):1–313.
Alfonso E, Xie X, Augusto V, Garraud O. Modelling and simulation of blood collection systems: improvement of human resources allocation for better cost-effectiveness and reduction of candidate donor abandonment. Vox Sang. 2012;104(3):225–33.
Standfield L, Comans T, Scuffham P. An empirical comparison of Markov cohort modeling and discrete event simulation in a capacity-constrained health care setting. Eur J Health Econ. 2015;18(1):33–47.
Robberstad B. QALYs vs DALYs vs LYs gained: what are the differences, and what difference do they make for health care priority setting? Glob Health Res. 2005;15(2):183–91.
De Luca G, Suryapranata H, Ottervanger J, Antman E. Time delay to treatment and mortality in primary angioplasty for acute myocardial infarction: every minute of delay counts. Circulation. 2004;109(10):1223–5.
Siciliani L, Borowitz M, Moran V. Waiting time policies in the health sector. Paris: OECD; 2013. p. 238.
Kate S, Richard L, Helen B, Richard S, Paul W. Reducing waiting times in the NHS: is lack of capacity the problem? Clin Manag. 2004;12(3):105–9.
Briggs A. Handling uncertainty in cost-effectiveness models. Pharmacoeconomics. 2000;17(5):479–500.
Briggs A, Gray A. Handling uncertainty when performing economic evaluation of healthcare interventions. Health Technol Assess. 1999;3(2):1–134.
Andronis L, Barton P, Bryan S. Sensitivity analysis in economic evaluation: an audit of NICE current practice and a review of its use and value in decision-making. Health Technol Assess. 2009;13(29):1–61.
Briggs A, Weinstein M, Fenwick E, Karnon J, Sculpher M, Paltiel A. Model parameter estimation and uncertainty analysis: a report of the ISPOR-SMDM Modeling Good Research Practices Task Force Working Group-6. Med Decis Mak. 2012;32(5):722–32.
Bojke L, Claxton K, Sculpher M, Palmer S. Characterizing structural uncertainty in decision analytic models: a review and application of methods. Value Health. 2009;12(5):739–49.
Davis S, Stevenson M, Tappenden P, Wailoo A. Cost-effectiveness modeling using patient-level simulation. NICE DSU technical support document 15. Sheffield: The Decision Support Unit (DSU); 2014:7. https://www.ncbi.nlm.nih.gov/pubmed/27466644. Accessed 11 May 2015.
Mathes T, Jacobs E, Morfeld J, Pieper D. Methods of international health technology assessment agencies for economic evaluations- a comparative analysis. BMC Health Serv Res. 2013;13(1):371.
Sharp L, Tilson L, Whyte S, Ceilleachair A, Walsh C, Usher C, et al. Using resource modelling to inform decision making and service planning: the case of colorectal cancer screening in Ireland. BMC Health Serv Res. 2013;13:105.
Miquel-Cases A, Steuten L, Rigter L, van Harten W. Cost-effectiveness and resource use of implementing MRI-guided NACT in ER-positive/HER2-negative breast cancers in The Netherlands. BMC Cancer. 2016;16:712.
Chhatwal J, He T. Economic evaluations with agent-based modelling: an introduction. Pharmacoeconomics. 2015;33(5):423–33.
Briggs A, Sculpher M. An introduction to Markov modelling for economic evaluation. Pharmacoeconomics. 1998;13(4):397–409.
Fenwick E, Claxton K, Sculpher M. The value of implementation and the value of information: combined and uneven development. Med Decis Mak. 2007;28(1):21–32.
Whyte S, Dixon S, Faria R, Walker S, Palmer S, Sculpher M, Radford S. Estimating the cost-effectiveness of implementation: is sufficient evidence available? Value Health. 2016;19(2):138–44.
Faria R, Walker S, Whyte S, Dixon S, Palmer S, Sculpher M. How to invest in getting cost-effective technologies into practice? A framework for value of implementation analysis applied to novel oral anticoagulants. Med Decis Mak. 2016;37(2):148–61.
Acknowledgements
We thank all of those who contributed to this work. In addition, the corresponding author (SS) would like to thank Majlis Amanah Rakyat (MARA) for sponsoring this project.
Author information
Authors and Affiliations
Contributions
The study idea originated from PT and SD, which was further developed in discussions with SS, and finalised in communication with all authors. SS coordinated the data collection and interpretation, which was agreed among all authors. SS and PT wrote the initial draft, with all authors contributing to the submitted version and also revising the manuscript based on reviewers’ comments. SS is the overall guarantor for the manuscript.
Corresponding author
Ethics declarations
Funding
This work was supported by the Majlis Amanah Rakyat (MARA).
Conflict of interest
Syed Salleh, Praveen Thokala, Alan Brennan, Ruby Hughes and Simon Dixon declare that they have no conflicts of interest.
Appendix 1
Rights and permissions
About this article
Cite this article
Salleh, S., Thokala, P., Brennan, A. et al. Discrete Event Simulation-Based Resource Modelling in Health Technology Assessment. PharmacoEconomics 35, 989–1006 (2017). https://doi.org/10.1007/s40273-017-0533-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40273-017-0533-1