Abstract
Various adverse events resulting from, or associated with, benzodiazepine and/or Z-drug use have been extensively reported on and discussed in great detail within the biomedical literature. It is widely accepted that motor vehicle accidents and falls leading to fractures in older adults are major adverse events that have been shown to occur more frequently in users of sedative-hypnotic medication, especially of the benzodiazepine and related Z-drug variety. However, the last few years have seen increasing reports in the literature raising the issue of benzodiazepine and Z-drug exposure in the development of other serious medical issues including dementia, infections, respiratory disease exacerbation, pancreatitis, and cancer. This article provides an overview and interpretation on the current state of evidence regarding each of these associations and proposes what gaps in the evidence for drug-exposure–harm associations need to be addressed in the future for the purpose of evaluating causality of harm as it relates to these drugs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
There is sufficient, converging evidence from epidemiologic and experimental studies to establish a strong causal connection between benzodiazepine/Z-drug use to motor vehicle accidents, falls and fractures as a consequence of psycho-motor impairment. |
A strong causal connection between benzodiazepine/Z-drug use and the other reviewed harm associations (i.e., dementia, infections, cancer etc.) cannot be soundly concluded at this time due to insufficient and conflicting evidence from both epidemiologic and experimental studies. |
As doubt and controversy persists regarding many of these adverse harm associations, further research is required to reconcile the evidence base for the sake of optimizing medication safety in the population. |
1 Introduction
Benzodiazepines are prescription sedative-hypnotic medications that have been used for decades in the treatment of anxiety, epilepsy, insomnia, and other conditions [1]. Zopiclone, eszopiclone, zaleplon and zolpidem are the ‘Z-drugs’; introduced into the market in the 1990s, they have only been approved for insomnia. Though these medications are widely recognized as being effective, like any class of drugs, they are not without potential harms. This review serves as a comprehensive summary of the available literature on major adverse events associated with benzodiazepine and Z-drug use. Discussions of pharmacology and other clinical topics relating to these drugs will not be taken up here. Over the past few years, literature has emerged raising a tentative link between benzodiazepine and/or Z-drug exposure with adverse outcomes such as respiratory disease exacerbation, infections, dementia, pancreatitis, and cancer. To our knowledge, this will be the first review of its kind that summarizes the available literature on each of these outcomes for these drug classes. For the sake of completeness, harms proposed/identified much earlier in the literature such as motor vehicle accidents, falls leading to fracture, and drug overdose will be reviewed as well.
2 Methodology
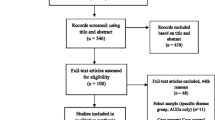
In this narrative, non-systematic review, a repeated search strategy involving the terms ‘benzodiazepine’ OR ‘Z-drug’ (and individual drugs) in conjunction with combinations of the terms ‘traffic’, ‘vehicle’, ‘falls’, ‘fractures’, ‘dementia’, ‘Alzheimer’s’, ‘infections’, ‘cancer’, ‘carcinogenic’, ‘pneumonia’, ‘mortality’, ‘overdose’, ‘COPD’, ‘respiratory’, and ‘pancreatitis’ to the databases of PubMed, SCOPUS, and EMBASE. English language references were selectively retrieved with this search strategy and also yielded additional citations of interest in the bibliography sections. When necessary, authoritative organizational reports and related data sources were used. Articles reported on are preferentially systematic reviews, meta-analyses, narrative reviews, and single studies (experimental, observational or randomized controlled trial) deemed of significant value for the review where compilation-level evidence (i.e., meta-analyses and systematic reviews) was unavailable. There was no restriction on the date range of references collected, though newer literature from 2000 to 2017 (134/143 references used herein) was preferentially selected when it was deemed to be representative of the current state of research.
3 Motor Vehicle Accidents
According to the World Health Organization, road injury was the ninth leading cause of death globally between 2002–2012 [2].The prevalence of prescription-drug–positive fatal motor vehicle accidents has increased by an estimated 49% in the US over the past 20 years, with benzodiazepines in particular more than doubling their rate of involvement in such accidents [3]. In Canada, 11.2% of drivers killed in vehicle accidents between 2000 and 2010 tested positive for sedative-hypnotic prescription drugs post-mortem [4]. For the past decades, benzodiazepines and Z-drugs have been the focus of much public safety research, both epidemiological and experimental, on motor vehicle driving performance and outcomes.
3.1 Pharmacological Basis and Experimental Studies
Experimental studies have involved administration of a sedative-hypnotic medication to individuals prior to a measured test of driving performance, be it simulated or in an actual vehicle. Though experimental study designs may differ, many studies have utilized a common, validated measure of safe driving performance called the standardized deviation of lateral position (SDLP); an index of maintaining vehicle positioning while driving on a stretch of road (usually straight) at a constant speed [5]. A 2009 meta-analysis by Rapoport et al. carefully selected five on-road experimental studies of similar methodology to determine differences in SDLP between benzodiazepine users and controls with a reported pooled estimate of standardized mean difference (SMD) between groups of 0.80 (p = 0.0004) at a ≤5-mg dose equivalent of diazepam [6]. The SMD further increased to 3.07 standard deviations at a ≥10-mg diazepam dose equivalent, thus implying a dose-dependent loss of vehicle control in users compared with controls [6]. Another meta-analysis of 14 randomized controlled trials by Roth et al. in 2014 concluded that driving performance diminished significantly with longer half-life agents, higher doses, and when time between single dosing and driving was reduced [7]. Furthermore, based on some studies, blood plasma concentrations of benzodiazepines in impaired drivers has been shown to correlate, with some degree of reliability, with risk of potential accidents [8, 9]. For instance, the presence of benzodiazepine in blood samples from 818 drivers (159 not impaired, 659 impaired) yielded an adjusted odds ratio for determination of driving impairment of 1.60 for mildly elevated concentrations and 3.75 for highly elevated concentrations [9].
Z-drugs in particular have also been the subject of experimental studies, although less so than benzodiazepines. A pooled analysis of four studies on zopiclone’s potential for residual sedation contributing to driving risk demonstrated that impairment lasted for up to 11 hours after dosing, was not significantly dependent on sex or age, and was comparable in magnitude to a blood alcohol concentration of up to 0.8 mg/L, which, in turn, corresponds to at least twice the risk of motor-vehicle accidents [10]. Perhaps because of this, zopiclone has been used as a positive control for studies on other drugs in driving because of its reliability in causing significant impairment [11]. Studies on zolpidem and zaleplon in healthy subjects have not been shown to cause significant residual impairment leading to traffic accident risk with early or middle-of-the-night dosing [12,13,14,15]. Zolpidem has been shown to cause significant changes in SDLP, standard deviation in speed, and alertness in healthy drivers between the ages of 55–65 years [16]. A literature review by Gunja also ranks zopiclone over the other Z-drugs in terms of potential for residual impairment, but also places rightful emphasis on safety concerns arising from sleep behaviors (including sleep driving) reported more frequently in zolpidem users [17]. A simplified, summative, evidence-based categorization guide produced by the International Council on Alcohol, Drugs and Traffic Safety (ICADTS) has ranked various medications based on their potential for causing impaired driving (I = presumed safe, II = minor to moderate impairment, III = severe impairment), with 22 benzodiazepines and zopiclone ranked at III and nine benzodiazepines, zolpidem, and zaleplon ranked at II [18, 19].
3.2 Epidemiologic Studies
Epidemiological studies examining real-world accident outcomes, as opposed to experimental surrogate outcomes (SDLP and others), are perhaps easier to place into relevant context for clinicians and those in public health. Twenty-five of 28 epidemiological studies examined in a review by Gjerde et al. found positive associations between road traffic accidents and benzodiazepine/Z-drugs [20]. Smink et al., in a 2010 systematic review, examined 66 studies published between 1960 and 2009 of varying methodologies [21]. However, interpretation of the studies was partially hampered due to the extremely divergent study designs, populations, exposure measurement methods, and outcome measures assessed for the included studies. Nonetheless, the authors concluded that risk is greatest with higher dosages, longer half-life agents, and within the first few weeks of drug initiation [21].
In terms of quantifying this association, the meta-analysis by Rapoport et al. also provided pooled odds ratio estimates for case–control studies (n = 6) and cohort studies (n = 3) on accident risk with benzodiazepine exposure, reporting a 60% higher odds of accident in benzodiazepine users [6]. Another 2011 meta-analysis by Dassanayake et al. also included an assessment of benzodiazepine association with motor vehicle accidents via three distinct pooled odds ratio estimates based on case–control studies (n = 6, OR = 1.59), cohort studies (n = 3, OR = 1.81), and accident culpability studies (n = 5, OR = 1.41), all of which significantly indicated an association [22]. The last estimate, on accident culpability, when considered in conjunction with the experimental studies, strengthens the causal argument by showing that those involved in vehicle accidents who consumed benzodiazepine medication were ~40% more likely to be at fault than the other parties involved. The latest 2013 meta-analysis by Elvik separated pooled risk estimates by outcome (fatal, injury, or property damage) rather than by study type for benzodiazepines [23]. For benzodiazepines, after adjusting for publication bias, these estimates remained significant for fatal accidents (n = 10, OR = 2.30), injury accidents (n = 51, OR = 1.17), and property damage (n = 4, OR = 1.35) [23].
The epidemiologic association made between Z-drugs and motor vehicle accidents is less robust than with the benzodiazepines yet is still significant enough to warrant concern among clinicians, public health researchers, and policy makers. Studies of differing methodologies and sample populations have reported overall risk/odds ratios ranging from a 38% increased risk/odds to over double the risk/odds of traffic accidents in zolpidem users over non-users [24,25,26,27]. Despite the compelling experimental evidence for driving impairment, the epidemiological evidence for zopiclone in vehicle accidents is less clear, as some studies have found an association [28, 29] and others have not [27]. An exhaustive 2016 systematic review of epidemiologic studies on numerous medications and motor vehicle collisions by Rudisill et al. found four of five studies to be statistically significant for zolpidem and two of six studies to be statistically significant for zopiclone [30].
Although sedative-hypnotic drugs undoubtedly seem to pose a hazard in driving safety, increased risk has been tentatively identified in certain users or medication-related behaviors, albeit with much uncertainty. Younger age [22, 28] and new use of benzodiazepines [26] have been reported as additional risk factors in users of these medications. A literature review on gender risk difference in drugged driving has found that, with the exception of zolpidem and flurazepam, no differences in impairment have been noted between the sexes, but this has been foremost due to a lack of study data differentiating the magnitude of impairment between men and women [31]. An observational study finding suggests that drug impaired driving, in some jurisdictions, may be primarily among a younger population using these medications non-medically with or without the concurrent use of illicit street drugs [32]. This raises the question as to what proportion of vehicle crashes associated with sedative-hypnotics is from irresponsible or non-medical use as opposed to use as prescribed. Driving and drug-taking behavior among younger drivers is likely sufficiently different enough for confounding to have played some role in these associations. Further to this, others have speculated that the increased risk observed among younger drivers is partially owed to a combination of factors including reduced life experience with these drugs leading to an underestimation of impairment effect, higher doses routinely received, and a relative absence of competing risk factors (poorer health status etc.) making modest risk differences attributable to benzodiazepines more easily detectible in comparison [22, 33].
Despite the general consensus among the literature, some other overall limitations warrant mention regarding many of the epidemiological studies on this association. Foremost, is confounding by indication, whereby sleep deprivation increases accident risk independent of drug use [34]. This is especially the case for studies defining exposure by only receipt of prescription rather than toxicologic confirmation of drug use or patient testimony. Furthermore, many retrospective designs are incapable of reliably establishing a sufficient causal context for each recorded traffic accident in no small part due to biases (patient or investigator) or lack of pertinent information relating to driving incidents. For example, a particular traffic accident may have taken place long after the cessation of a drug’s sedative effect, making exposure purely coincidental but nevertheless resulting in a false-positive accident captured within study results.
3.3 Summary
There is an overwhelming degree of evidence, both experimental and epidemiological, implicating benzodiazepines in particular, but Z-drugs as well, with fatal and non-fatal motor vehicle accidents. Though some limitations and discrepancies persist, both streams of evidence (experimental and epidemiological), when considered together, support a strong causal argument for exposure of these drugs resulting in motor vehicle accidents. It seems more research is necessary to elucidate with certainty which medications, at what doses, and in which patients increases risk beyond an acceptable degree so as to enable effective targeted interventions to reduce motor vehicle harm.
4 Falls and Bone Fractures
Osteoporosis, a state of bone mineral density deterioration, is a medical condition in which the health burden increases with advancing age, particularly in females after menopause [35]. This higher incidence of osteoporosis in elderly females corresponds to the higher sedative-hypnotic medication usage incidence and prevalence witnessed in this same portion of the general population. Importantly, fractures, being the main devastating outcome to be prevented in osteoporosis, are linked directly to increases in mortality rates [36]. This is especially true for hip fractures with an estimated excess mortality ranging from 8 to 36% over a 1-year period [37].
4.1 Pharmacological Basis and Experimental Studies
In terms of a speculative causal association between fractures and the GABAA receptor-modulating benzodiazepines and Z-drugs, a direct effect on bone mineral metabolism seems untenable and so the association has instead been attributed to their adverse pharmacodynamic effect on cognition, gait, and balance leading to falls in susceptible patients such as the elderly or those with mobility issues [38, 39]. Furthermore, prior literature reviews conclusively show that benzodiazepines and Z-drugs exhibit a dose-dependent deleterious effect on postural stability and balance, thus implying an inextricable link to fractures, with falling as the critical intermediary event [40, 41].
4.2 Epidemiologic Studies
A multitude of individual studies, summarized by comparative systematic reviews and meta-analyses, have consistently demonstrated various psychotropic medication classes, including antidepressants, antipsychotics, opioids, benzodiazepines, and Z-drugs, to be linked to falls [42,43,44] and fractures [45]. Fall-related harm from benzodiazepine use was estimated to cost 1.8 billion Euro in the European Union in the year 2000 [46]. This is one of the few cost estimates of benzodiazepine fracture-related harm but nonetheless shows the negative expenses of such drug use in the population.
Attempts to quantify the overall risk of fractures associated with benzodiazepine use has been carried out by careful compilation of existing study data. A meta-analysis published by Khong et al. in 2012, consisting of data from 14 studies, used an ecological study design to examine hip fracture rates in association with benzodiazepine consumption in the US and five European countries [47]. They concluded a pooled relative increased risk of 24–58% in benzodiazepine users over non-users for hip fracture [47]. Another, more recent meta-analysis from 2014 by Xing et al. included 25 distinct studies (19 case–control and 6 cohort) and determined a conservative adjusted overall estimate indicating a 13–30% increased risk of fractures attributable to benzodiazepine use [48].
When it comes to discerning differences in falls and fracture risk among benzodiazepines, there have been some discrepancies in the findings of individual studies. For example, a few studies demonstrated a seemingly greater risk with long-acting benzodiazepines supposedly explained by their pharmacokinetic profile in the elderly [49,50,51]. Another study, hypothesizing increased rates of fractures with oxidative benzodiazepines (i.e., requiring phase 1 hepatic metabolism for elimination) found no difference to support the hypothesis that non-oxidative benzodiazepines are of lesser risk in causing fractures among elderly persons [52]. Other studies, including the aforementioned 2014 meta-analysis, have attributed a higher risk to short-acting agents [48, 53,54,55,56,57].
These discordant pharmacokinetic findings on population drug safety have been partially explained by selection bias and confounding by indication. For instance, prescribers may select shorter-acting or non-oxidative agents on a frequent basis for higher risk patients, thus making lower risk drugs appear higher in risk when fractures and falls do occur [38, 55]. However, evidence has shown, with limited conflicting results and adherence to expected pharmacological principles, that the risk of falls and fractures increases with higher doses [51, 55, 58,59,60], use of interacting medications [55], and after treatment initiation, particularly during the first 1–2 weeks of drug exposure [55, 58, 59, 61]. New data from three studies suggests variant CYP 2C9 allele expression plays a significant role in fall risk among benzodiazepine users, thus suggesting a future clinical role for pharmacogenetic screening [62]. Lastly, of particular concern is that some limited evidence indicates that elderly individuals at a higher baseline risk for falls (pre-existing risk factors) may be more likely to receive new benzodiazepine prescriptions than a lower-risk elderly cohort [63].
Despite the fact that, in comparison with the benzodiazepine class, there is substantially less study data elucidating the degree of association between Z-drugs and fractures, a meta-analysis of the available studies on zolpidem by Park et al. was published recently in 2016 [64]. This meta-analysis comprised nine studies (four cohort, four case–control and one case–crossover) and reported a pooled estimate of 92% excess risk of fractures in zolpidem users. Given the comparably lower meta-analytic risk estimates attributed to benzodiazepines, this estimate may be inflated due to heterogeneity, confounding, and the reduced sample size of the included studies. Nonetheless, three of the studies included in the meta-analysis had reported event rate comparisons with benzodiazepines, yet the relative risk of fracture with zolpidem still exceeded that of benzodiazepines [65,66,67]. Predictably, a trend towards greater risk in the early treatment period and with increasing doses has been shown to hold true for Z-drugs in the same way as for benzodiazepines [51, 64].
4.3 Summary
It is unclear what further studies (non-intervention based) on this topic will accomplish considering the overall weight of the current evidence establishing an association between these drugs and falls leading to fractures. Though much work has already been done on fall prevention [68], interventional studies with an aim to reduce fall-related harm from sedative-hypnotics should perhaps be the continued focus of future research. For now, clinicians should keep in mind that higher doses, psychotropic poly-pharmacy, and the early treatment period with these drugs probably pose a greater hazard, within the context of benzodiazepine/Z-drug use. This is especially true for patients with history of fractures and poor mobility (i.e., frail elderly).
5 Drug Overdose
The risk of fatality from benzodiazepine overdose alone via respiratory or nervous system depression is seemingly non-existent [69]. In rare instances of mono-drug overdose, benzodiazepines may produce an idiosyncratic, potentially fatal atrioventricular heart block [70]. More importantly, involvement of benzodiazepines with other agents known to cause central nervous system (CNS) and respiratory depression, such as alcohol, opioids, or muscle relaxants, substantially increases risk of harm [69, 71]. Concurrent use of benzodiazepines and opioids, in particular, is a complex topic reviewed in detail elsewhere [72, 73]. Co-administration of these drug classes simultaneously, purportedly enhances the euphoric ‘high’ as per synergistic pharmacologic CNS mechanisms [74]. This likely reinforces dangerous medication taking behavior among those with a substance-use disorder, thus increasing risk of overdose. Issues surrounding combination benzodiazepine–opioid use remain highly relevant for clinical practice as studies from various jurisdictions have shown co-prescription use of these drug classes to be frequent or increasing [75,76,77,78,79].
5.1 Epidemiologic Studies
Drug overdose fatality data, made available by the US National Institute for Drug Abuse (NIDA), reveals that death involving benzodiazepine overdose has been steadily on the rise since 2002 (2022 deaths) to the present (8791 deaths in 2015), with ~75% of these overdoses involving opioids [80]. These government-reported statistics are generally in alignment with a 2016 study analyzing trends in benzodiazepine prescription and overdose deaths in the US for 1996–2013, which found that the dispensed benzodiazepine prescription drug volume more than tripled during this period and overdose deaths involving benzodiazepines became five times more frequent [81].
Remaining in the US, from 2004 to 2011, emergency department visits involving non-medical combined use of benzodiazepines and opioids increased threefold (from 11 to 34.2 per 100,000 persons) and increases in death from co-overdose was nearly proportional to this (0.6 to 1.7 per 100,000) [82]. In terms of poisoning leading to hospitalization (i.e., beyond the emergency department) in the US, from 1999 to 2006, benzodiazepines were involved in more poisoning events and had the largest increase in rate of poisoning among all drug classes studied (39% increase from 26,321 in 1999 to 36,700 in 2006) [83]. In terms of which benzodiazepines may present greater risk, an observational study of 2063 single benzodiazepine overdose admissions showed markedly higher frequencies for ICU admission, ventilation, flumazenil administration, and length of stay for alprazolam over other benzodiazepines [84]. A case–control study in a US veterans population concluded a ‘dose-dependent’ relationship between benzodiazepine prescription issuance with overdose mortality (overall adjusted hazard ratios of 2.33 and 3.86 for previous prescription and current prescription of benzodiazepines, respectively) [85]. As with dose response, as duration of use increases, the odds of overdose seem to increase as well according to results from a retrospective cohort study of prescription opioid users [86]. Despite the logic underlying dose-duration relationships with mortality at the population level, these findings require confirmation by result replication in other populations and study designs. More importantly, continued drug studies examining overdose measures for this drug class will determine if overall utilization is improving over time in terms of drug safety in overdose.
Recent, easily findable, large observational studies specifically on benzodiazepine overdose in countries other than the US appear to be lacking and this is even more true for the Z-drugs. It is currently difficult to determine with accuracy the extent of Z-drug overdose morbidity and mortality in general populations (national, regional, or otherwise) as they are frequently grouped with benzodiazepines. Nevertheless, a comparative epidemiologic study of single drug overdose fatalities from the UK from 1983 to 1999 found a reduced frequency of fatalities for Z-drugs in overdose compared with benzodiazepines (~2 deaths vs ~5.6 deaths/million prescriptions) [87]. However, these findings warrant caution in concluding that Z-drugs are generally safer in overdose as the death rates amongst individual benzodiazepines differed tremendously (flurazepam being the highest and medazepam the lowest at 20.5 and 0.0 deaths/million prescriptions, respectively) and user populations for particular agents may be inherently different [87].
5.2 Summary
Given their relative safety in mono-drug overdose, benzodiazepines have seldom been studied on an epidemiologic basis in this context unless other co-intoxicants, such as opioids, are also involved. However, it is only sensible that opioids are afforded research priority over benzodiazepines in the pharmacoepidemiology of prescription drug overdose because of their comparably greater toxicity. Future studies examining benzodiazepine and Z-drug overdose outcomes, similar in design to studies by Buckley and McManus [87] or Isbister et al. [84] would be invaluable.
6 Infections
6.1 Pharmacological Basis and Experimental Research
Speculation linking benzodiazepines to infections originally began when multiple in vivo pharmacology studies demonstrated immune dysfunction and bacterial infections of greater frequency among rodents exposed to diazepam [88,89,90]. Despite these results, the immunopharmacology of peripheral and central benzodiazepine GABAA receptors remains complex as other in vitro studies have shown potentiation of immune response from triazolo-benzodiazepines such as alprazolam and triazolam [91,92,93]. This begs the question as to whether there is a true ‘class effect’ of these agents or if there are indeed indisputable immunopharmacological differences between them.
6.2 Epidemiologic Studies
Scaling back focus to an epidemiologic level, evidence is conflicting as some observational studies have detected associations between mortality from community-acquired pneumonia and benzodiazepine/Z-drug use [94,95,96,97], and others have not [98, 99]. The largest and most recent observational study by Nakafero et al. (2016) employed a survival analysis methodology on a retrospective cohort study of >800,000 patients with ‘influenza-like illness’ (ILI). They reported resultant adjusted hazard ratios of 4.24 (95% CI 2.27–7.95) and 20.69 (95% CI 15.54–27.54) for ILI and ILI-related mortality, respectively, in current benzodiazepine/zopiclone users [94]. This team of researchers and another independent group, Obiora et al., not only found strong statistical significance for an association but also observed a dose-response trend for many benzodiazepines and Z-drugs under study as the hazard ratios generally trended higher from ‘non-users’ to ‘past-users’ to ‘current-users’, albeit with many instances reflecting a J-curve [94, 95]. Discrepant findings in an elderly population (those not found to be at greater risk from exposure) [99] have been explained by both Nakafero et al. and Obiora et al. by the higher comorbidity burden in older patients which independently increases pneumonia and mortality risk by a magnitude substantially greater than benzodiazepine exposure, thus limiting statistical detection in this sub-population [94, 95]. Considering Z-drugs separately from benzodiazepines, a meta-analysis of published studies and FDA randomized clinical trial data by Joya et al. found a 25–64% increased risk of infection (various types) in those exposed to Z-drugs (and oddly, ramelteon) over placebo [100]. There was enough data only for sub-analysis of eszopiclone and zolpidem, both of which were statistically significant with adjusted hazard ratios at 1.48 (95% CI 1.25–1.74) and 1.99 (95% CI 1.21–3.26), respectively [100]. Despite the fact that the association was significant and that this meta-analysis is composed of randomized trial data (thus obviating the dilemma of confounding and temporality seen with some observational study designs), the absolute event rates were low at 6.86% in the hypnotics group and 4.56% in the placebo group, thus yielding an absolute risk difference of only 2.30%. Lastly, no single type of infection was driving the association and 34% of the infections were not even clinically recorded by subtype [100].
6.3 Summary
Infection risk with benzodiazepines and Z-drugs has yet to be widely recognized by clinicians as a concern deserving of attention as the population-based evidence supporting this association is rather recent and not yet confirmed by the scientific rigor required of causal associations. With a proposed mechanism derived from lab-based pharmacologic experiments in place to explain infection risk from this class of drugs, the concerning results from some observational studies are granted a limited degree of plausibility for a causal association. Unlike the literature on falls, fractures, and motor vehicle accidents, however, there is a scarcity of pharmacoepidemiologic research on this association. It may also be argued that the pharmacological plausibility for infection is made less tenable given the basic pharmacology, as commonly understood, for this class of sedative-hypnotics. Therefore, confirmation of this tentative adverse drug event should be sought from high-quality prospective study designs along with the pharmacological basis being more clearly defined.
7 Pancreatitis
Less reported on in the literature is the possible association between benzodiazepines and/or Z-drugs with acute episodes of pancreatitis. Thus far, one Taiwanese retrospective cohort study has raised the association for benzodiazepines [101] and two Taiwanese case–control studies have raised the issue with zopiclone [102] and zolpidem [103].
After adjusting for potential confounders, Liaw et al. observed a 5.33-fold (95% CI 2.26–12.60) increased risk of pancreatitis within 1 month of benzodiazepine poisoning over controls [101]. Lai et al. reported a confounding adjusted odds ratio of 2.36 (95% CI 1.70–3.28) for those with receipt of zopiclone prescription within 30 days of pancreatitis compared with never-users of this drug [102]. Of note is that the association remained significant even when a prescription was dispensed ≥31 days prior to the episode of pancreatitis (95% CI 1.60–2.66), thus suggesting a possible spurious association. The authors address this by claiming possible ‘as needed’ use of the drug prior to the episode, however this is not verifiable with the database study design. The same group of researchers, in an almost identical study design, reported an adjusted odds ratio for pancreatitis of 7.20 (95% CI 5.81–9.82) in those who received a prescription for zolpidem within 7 days of pancreatitis diagnosis compared with those who never received zolpidem [103]. Unlike the study with zopiclone, the authors examined and discovered a dose-response trend where the association was greater for doses >10 mg (OR 8.70) compared with ≤10 mg (OR 6.76) [103].
A precise mechanism behind benzodiazepine- or Z-drug-induced pancreatitis remains elusive, though the authors of the previous studies have proposed direct noxious effects on pancreatic tissue from these drugs [101,102,103]. However, a pharmacological mouse-model study of cerulein-induced pancreatitis yielded anti-thetical results wherein pre-treatment diazepam 5 mg/kg (intra-peritoneal) was observed to produce anti-inflammatory effects; reducing pancreatic edema along with lipase and amylase serum levels compared with a negative control [104]. Recent review articles also make no mention of either benzodiazepines or Z-drugs as agents being associated with drug-induced pancreatitis [105, 106].
7.1 Summary
Few original research studies exist that investigate the presence or absence of an association between benzodiazepines and Z-drugs with pancreatitis. The three population-level observational studies that do exist are all of a retrospective design in the Taiwanese population. Despite this, all of these studies are in concordance with each other in presenting odds ratios of sufficient magnitude to raise an alert for this serious association. There is a dearth of experimental studies specifically determining the effects of benzodiazepines and Z-drugs on pancreatic tissues. At least one published experiment offers contradictory evidence. As of yet, there is no sound, well recognized, molecular pharmacological basis for clinically relevant tissue inflammation from benzodiazepines or Z-drugs. Further high-quality research, both observational and experimental, from multiple countries would be invaluable towards determining whether there is any causal truth behind this drug exposure–adverse outcome association.
8 Respiratory Disease Exacerbation
8.1 Pharmacological Basis and Experimental Studies
It is rational to hypothesize that patients with significant respiratory dysfunction are more susceptible to the otherwise minor respiratory depressive effects of benzodiazepines at approved doses. A review by Roth reported that benzodiazepines diminish respiratory function by reducing airway smooth muscle tone and/or increasing the threshold for arousal by desensitizing neurons in airway obstructed sleep states [107]. In contrast, Roth further observed that Z-drugs, unlike benzodiazepines, were absent of any significant effect on either ventilation or CNS control of breathing in normal subjects and patients with mild to moderate chronic obstructive pulmonary disease (COPD) [107]. Another review by Stege et al. assessed the results of drug-effect studies on oxygen saturation, inspiratory flow rate, and a variety of other objectively determined respiratory parameters on COPD patients with insomnia receiving benzodiazepines and Z-drugs. However, the overall verdict was inconclusive as some experiments showed deleterious changes in these domains and others did not [108]. In terms of a difference in safety between benzodiazepines and Z-drugs in COPD, Stege et al., unlike Roth, refrain from declaring either sub-class as being safer in this context given that four of six studies found no difference in respiratory changes between these classes [108]. In the context of obstructive sleep apnea (OSA), the results of two meta-analyses largely found an absence of any worsening of sleep-disordered breathing parameters [109, 110].
8.2 Epidemiologic Studies
Contrary to much of the experimental literature just discussed, mounting evidence from observational studies over the past number of years has raised the suspicion that use of benzodiazepines or Z-drugs in those with COPD increases risk of respiratory exacerbations and mortality beyond that expected from the course of the disease state alone [111,112,113,114]. For the first time, an association with asthma exacerbation has also been raised from the results of a large observational study in the UK [115]. The results for a few of these studies have been subject to extensive reviewer discussion with criticism, but will not be reiterated in extensive detail here [116, 117].
Despite the similar findings and model adjustments by the authors of these studies, issues of confounding, bias, and other methodological limitations can probably be raised as usual [111,112,113,114,115]. Of special potential confounding interest is the common usage of benzodiazepines for dyspnea in palliation [118]. Despite the fact that palliative drug usage is poorly captured in most pharmacoepidemiologic study designs (databases typically limited to outpatients), it is reasonable to speculate that even later-stage ambulatory COPD patients with poor survival prognoses may be granted prescriptions for benzodiazepines and Z-drugs more frequently than those with milder disease severity to assuage breathlessness, anxiety, or insomnia related to their illness (i.e., confounding by indication). Nonetheless, this was anticipated in one study by Vozoris et al. who stratified their Canadian patient cohort by severity and still discovered that the highest hospitalization or pneumonia rate ratio was in the healthiest sub-group of the COPD patients initiating benzodiazepines [111].
8.3 Summary
The effect of benzodiazepines and Z-drugs on respiratory disease states is not yet perfectly clear due to the disparity of results between acute respiratory effects as measured in smaller experimental studies and longer term clinical outcomes in observational studies. Given that population-based studies examining outcomes from exposure to these drugs have been predominantly case–control and retrospective cohort designs, prospective evidence, or even a meta-analysis of the available studies would be useful to persuade researchers and clinicians of any causal truth behind these associations. This is yet another example where findings from one discipline are not clearly in accord with those of another for these drugs and efforts should be made to reconcile this discrepant mistranslation in findings between pharmacology and epidemiology.
9 Dementia
Dementia, comprising Alzheimer’s disease, vascular, Lewy body and other sub-types, remains among the most feared disease states associated with aging because of its poor prognosis, lack of effective treatment modalities, and increasing global prevalence in the aging population [119]. It is long-standing basic knowledge that benzodiazepines and Z-drugs cause acute, reversible cognitive dysfunction (slurred speech, transient amnesia, etc.) in many patients. It is also well known that older individuals are more sensitive to the psychotropic adverse effects of benzodiazepines. Beyond acute drug effect, an association extending to progressive, neurodegenerative disease has been raised on numerous occasions by independent researchers.
9.1 Pharmacological Basis and Experimental Studies
Barker et al. published a 2006 meta-analysis of 13 experimental studies, all of which employed a battery of various neuropsychological tests, finding overall statistically significant reductions for 12 of 12 cognitive domains, thus strongly affirming the cognitive decline associated with long-term use of benzodiazepines [120]. However, these findings, though compelling in establishing the range of cognitive deficits that may occur from benzodiazepine use, do not confer direct knowledge on whether these drugs lead to neurodegenerative changes in neural tissue. Pariente et al., in a recent review article, speculate on a few potential drug-induced disease mechanisms but settle on favoring the hypothesis whereby exposed subjects are less likely to resort to a ‘cognitive reserve’; that is, alternative neural signaling pathways unaffected by undetected pre-clinical lesions that may have otherwise been protective of cognitive faculties [121]. Ultimately, the true mechanism, if there even is one, remains unknown and so these authors call for more experimental research to clarify this.
9.2 Epidemiologic Studies
Pariente et al. also reviewed the pharmacoepidemiologic body of evidence for this association and critically appraised the methodology of ten observational studies as per the Newcastle-Ottawa scale for non-randomized studies [122]. Of the studies, nine reported an increased risk of dementia from benzodiazepines [122]. A systematic review of ten studies and meta-analysis of eight studies, many of which overlapped with the prior review, used a random-effects model and found an overall 78% increased odds of dementia in benzodiazepine users over non-users [123]. A slightly older meta-analysis included six studies and reported a 49% increased odds in those ever having used benzodiazepines [124]. The association is strengthened considerably in those using benzodiazepines chronically for long periods, with a potentially further increased risk with higher doses and use of long-acting agents [121,122,123]. The meta-analyses, though quite recent themselves, may already warrant an updated estimate given three recent publications, two of which reported increased risk of dementia from benzodiazepine use [125,126,127]. Notably, Takada et al. conducted various analyses on Canadian, American, and Japanese data sources (adverse event databases, claims databases) and found that data from all three countries supported an association between long-term and long-acting benzodiazepine use and dementia [125]. The majority of studies on this association have been retrospective but a recent prospective study by Gray et al. reported discordant findings. Despite having shown ‘any use’ of benzodiazepines to be significantly associated with dementia, they failed to find higher dementia incidence in those individuals with the highest level of exposure to these drugs [128].
In terms of evidence regarding any association of Z-drugs specifically to dementia, the evidence is primarily restricted to a few sub-analyses in benzodiazepine studies previously alluded to, which suggest a similar risk of dementia as was seen with benzodiazepines [129]. A single Taiwanese case–control study reported an increased risk of dementia with zolpidem compared with for non-users, but other than this there appears to be a lack of studies solely on Z-drugs and dementia with benzodiazepines excluded [130].
There has been general consensus among researchers in this area that methodological limitations and differences giving rise to bias or confounding have been the primary challenge that remains to be overcome in order to conclude judgment on this association with high-level confidence. The most popular alternative explanations and criticisms for the reported association is founded upon protopathic bias (reverse-causality) whereby early-onset symptoms of clinically undetected dementia are first treated with benzodiazepines prior to a formal dementia diagnosis [122, 131,132,133]. Similarly, the association is further confused through the common clinical use of benzodiazepines to treat behavioral and psychological symptoms of dementia [134]. In this case, confounding by indication is a danger for proper interpretation and, with reverse-causality, represents a temporal continuum of potential bias in pharmacoepidemiologic studies on this topic.
9.3 Summary
Clear evidence of a drug-induced neuropathological mechanism as well as a large, well designed prospective study with a sufficiently long follow-up period (30+ years) are current gaps in the research that have already been called to be filled by previous authors who have examined the body of evidence [121,122,123,124]. Nevertheless, the truth behind this association carries potentially major public health implications for prevention of an, as of yet, incurable but always devastating neurodegenerative disease. Despite the large proportion of studies concluding an association between benzodiazepines and dementia, the criteria required to strongly substantiate a causal relationship remains only partially fulfilled [122].
10 Cancer
10.1 Pharmacological Basis and Experimental Studies on Carcinogenicity
With the burden of cancer having increased substantially over the past decades, the medico-scientific community, in response, has been ever more vigilant in identifying potential causal exposures leading to cancers (i.e., environmental hormone disruptors, dietary red meat, etc.). Mechanisms underlying benzodiazepine- and Z-drug-induced tumorigenesis remain tentative and unclear based on a review by Brambilla et al. of carcinogenicity and genotoxicity study results [135]. These authors reviewed study data for 51 benzodiazepines and the related Z-drugs and, at the very least, it is clear that there does not appear to be a consistent class effect for these agents in causing neoplasms in various animal tissue types. However, at the time of reporting, the authors state that only eight of 41 marketed molecules had all the necessary data needed for fulfillment of the FDA guidelines for carcinogenicity testing of pharmaceuticals [135].
10.2 Epidemiologic Studies
Despite the lack of conclusive experimental data, alarm signals for cancer risk have been raised by researchers for benzodiazepines and the Z-drugs based on observational study findings [136,137,138,139]. In attempts to get a clear answer to this quandary, Kim et al. published a 2016 meta-analysis of 22 observational studies (18 case–control and 4 cohort) which concluded an overall estimate of 19% increased cancer risk, with a significant dose-response trend, among benzodiazepine users over non-users [140]. There does exist a fine degree of granularity when it comes to the determination of cancer risk from benzodiazepines/Z-drugs as certain types of cancer (i.e., esophageal, brain, pancreatic) and certain agents (lorazepam, clonazepam, zopiclone) carry greater statistical weight, driving the overall association [137, 140]. Given that most of the studies included in the meta-analysis are retrospective, the authors address the limitations fairly by reminding us of confounding by indication (cancer patients more likely to use anxiolytic medication) and unmeasured confounding (alcohol and smoking) [140].
Perhaps most strikingly and of special interest is the odds/risk ratio of 2.08 (CI 1.77–2.44) for brain tumors which was of considerably greater magnitude than other types of cancer in the above-cited meta-analysis. Harnod et al., in the only study solely devoted to this cancer sub-type, found a >3-fold greater incidence of benign brain tumors in those exposed to benzodiazepines [141]. However, the benzodiazepine users in this study were significantly confounded as they were more likely to have had histories of dementia, epilepsy, head injuries, and brain scan imaging. The authors claim to have adequately adjusted for confounding but also rightfully mention the potential for unmeasured confounding as well as protopathic bias (undiagnosed brain tumors giving rise to insomnia, seizures, and psychiatric symptomatology) which may have skewed the results [141]. Nevertheless, an alarming finding of this magnitude may be viewed as hypothesis generating, which should require either confirmation or refutation from further study. Can it be more than coincidence that the anatomical location of highest neoplasm risk and the primary site of action for these agents is one and the same?
10.3 Summary
There is currently a lack of complete, high-quality experimental and epidemiologic evidence to confirm an association between benzodiazepine/Z-drug use and cancer. Ultimately, if these drugs are later proven to be carcinogenic it seems reasonable to question why this association was not detected with certainty many years earlier given their widespread usage. Malignancy caused by any regulated prescription medication is almost always rare and slow to develop. Even after diagnosis, it is not likely to be frequently identified in the minds of clinicians in terms of a causal association. Further to this, confounding by indication and unmeasured confounding are real limitations which place doubt on the association as it currently stands according to the observational study data. For these reasons, as with the dementia association, a prospective study of sound methodology and sufficient sample size is needed to address the seriousness of the claims raised recently in the literature.
11 Conclusion
Standard considerations for the causality of harm associations have been discussed and implied throughout this review. A concise summary assessing each adverse outcome association (excluding overdose for obvious reasons) for causality has been provided in Table 1 based on the well recognized Bradford Hill criteria [142], which has been operationalized in pharmacoepidemiology in the past [143]. However, the reader is cautioned that a systematic objective process to determine whether a criterion was fulfilled was not undertaken in this narrative review. Therefore, Table 1 simply serves as a summative, visual display of the authors’ interpretation, which may be vulnerable to bias.
It is clear that, despite the voluminous body of biomedical literature on benzodiazepines and Z-drugs, there is still a research need to answer vital questions relevant to the optimization of their effectiveness and safety in society. As with legal matters (i.e., innocent until proven guilty), doubt persists in the biomedical community regarding the relatively new safety accusations (dementia, infections, pancreatitis, and cancer) levelled against these drugs by pharmacoepidemiologic researchers (i.e., association until proven causation). Although serious clinical doubt persists, if even one of these newer associations stands the rigorous test of scientific scrutiny and is practically proven, it will have potentially tremendous public health implications given the already existent controversy surrounding certain patterns of use. Furthermore, serious negative health outcomes that are known to be associated with these agents such as falls, hip fractures, overdose, and motor vehicle accidents still need to be continually addressed in policies and clinical practice.
References
Trevor AJ. Chapter 22: sedative–hypnotic drugs. In: Katzung BG, Trevor AJ, editors. Basic and clinical pharmacology, 13e. New York: McGraw-Hill Medical; 2015. http://mhmedical.com/content.aspx?aid=1104844214.
World Health Organization. WHO | The top 10 causes of death. WHO. 2014. http://www.who.int/mediacentre/factsheets/fs310/en/. Accessed 26 Jan 2017.
Rudisill TM, Zhao S, Abate MA, Coben JH, Zhu M. Trends in drug use among drivers killed in US traffic crashes, 1999–2010. Accid Anal Prev. 2014;70:178–87. doi:10.1016/j.aap.2014.04.003.
Facts about drug-impaired driving. Canadian Centre on Substance Abuse, Ottawa, CAN. 2016.
Verster JC, Roth T. Standard operation procedures for conducting the on-the-road driving test, and measurement of the standard deviation of lateral position (SDLP). Int J Gen Med. 2011;4:359–71. doi:10.2147/IJGM.S19639.
Rapoport MJ, Lanctot KL, Streiner DL, et al. Benzodiazepine use and driving: a meta-analysis. J Clin Psychiatry. 2009;70(5):663–73. doi:10.4088/JCP.08m04325.
Roth T, Eklov SD, Drake CL, Verster JC. Meta-analysis of on-the-road experimental studies of hypnotics: effects of time after intake, dose, and half-life. Traffic Inj Prev. 2014;15(5):439–45. doi:10.1080/15389588.2013.830211.
Smink BE, Lusthof KJ, de Gier JJ, Uges DRA, Egberts ACG. The relation between the blood benzodiazepine concentration and performance in suspected impaired drivers. J Forensic Leg Med. 2008;15(8):483–8. doi:10.1016/j.jflm.2008.04.002.
Bramness JG, Skurtveit S, Mørland J. Clinical impairment of benzodiazepines—relation between benzodiazepine concentrations and impairment in apprehended drivers. Drug Alcohol Depend. 2002;68(2):131–41. doi:10.1016/S0376-8716(02)00188-6.
Leufkens TRM, Vermeeren A. Zopiclone’s residual effects on actual driving performance in a standardized test: a pooled analysis of age and sex effects in 4 placebo-controlled studies. Clin Ther. 2014;36(1):141–50. doi:10.1016/j.clinthera.2013.11.005.
Verster JC, Spence DW, Shahid A, Pandi-Perumal SR, Roth T. Zopiclone as positive control in studies examining the residual effects of hypnotic drugs on driving ability. Curr Drug Saf. 2011;6(4):209–18.
Hindmarch I, Patat A, Stanley N, Paty I, Rigney U. Residual effects of zaleplon and zolpidem following middle of the night administration five hours to one hour before awakening. Hum Psychopharmacol. 2001;16(2):159–67. doi:10.1002/hup.282.
Verster JC, Volkerts ER, Schreuder AHCML, et al. Residual effects of middle-of-the-night administration of zaleplon and zolpidem on driving ability, memory functions, and psychomotor performance. J Clin Psychopharmacol. 2002;22(6):576–83.
Verster JC, van de Loo AJAE, Moline ML, Roth T. Middle-of-the-night administration of sleep medication: a critical review of the effects on next morning driving ability. Curr Drug Saf. 2014;9(3):205–11.
Vermeeren A, Vuurman EFPM, Leufkens TRM, et al. Residual effects of low-dose sublingual zolpidem on highway driving performance the morning after middle-of-the-night use. Sleep. 2014;37(3):489–96. doi:10.5665/sleep.3482.
Bocca M-L, Marie S, Lelong-Boulouard V, et al. Zolpidem and zopiclone impair similarly monotonous driving performance after a single nighttime intake in aged subjects. Psychopharmacology (Berl). 2011;214(3):699–706. doi:10.1007/s00213-010-2075-5.
Gunja N. In the Zzz zone: the effects of Z-drugs on human performance and driving. J Med Toxicol. 2013;9(2):163–71. doi:10.1007/s13181-013-0294-y.
ICADTS Working Group. Categorization system for medicinal drugs affecting driving performance. 2007.
ICADTS. ICADTS drug list—July 2007. 2007:1–15. http://www.icadts.nl/reports/medicinaldrugs2.pdf.
Gjerde H, Strand MC, Morland J. Driving under the influence of non-alcohol drugs–an update part I: epidemiological studies. Forensic Sci Rev. 2015;27(2):89–113.
Smink BE, Egberts ACG, Lusthof KJ, Uges DRA, De Gier JJ. The relationship between benzodiazepine use and traffic accidents a systematic literature review. CNS Drugs. 2010;24(8):639–53.
Dassanayake T, Michie P, Carter G, Jones A. Effects of benzodiazepines, antidepressants and opoids on driving: a systematic review and meta-analysis of epidemiological and experimental evidence. Drug Saf. 2011;34(2):125–56.
Elvik R. Risk of road accident associated with the use of drugs: a systematic review and meta-analysis of evidence from epidemiological studies. Accid Anal Prev. 2013;60:254–67. doi:10.1016/j.aap.2012.06.017.
Booth JN 3rd, Behring M, Cantor RS, et al. Zolpidem use and motor vehicle collisions in older drivers. Sleep Med. 2016;20:98–102. doi:10.1016/j.sleep.2015.12.004.
Yang Y-H, Lai J-N, Lee C-H, Wang J-D, Chen P-C. Increased risk of hospitalization related to motor vehicle accidents among people taking zolpidem: a case–crossover study. J Epidemiol. 2011;21(1):37–43.
Hansen RN, Boudreau DM, Ebel BE, Grossman DC, Sullivan SD. Sedative hypnotic medication use and the risk of motor vehicle crash. Am J Public Health. 2015;105(8):e64–9. doi:10.2105/AJPH.2015.302723.
Orriols L, Philip P, Moore N, et al. Benzodiazepine-like hypnotics and the associated risk of road traffic accidents. Clin Pharmacol Ther. 2011;89(4):595–601. doi:10.1038/clpt.2011.3.
Gustavsen I, Bramness JG, Skurtveit S, Engeland A, Neutel I, Mørland J. Road traffic accident risk related to prescriptions of the hypnotics zopiclone, zolpidem, flunitrazepam and nitrazepam. Sleep Med. 2008;9(8):818–22. doi:10.1016/j.sleep.2007.11.011.
Barbone F, McMahon AD, Davey PG, et al. Association of road-traffic accidents with benzodiazepine use. Lancet. 1998;352(9137):1331–6.
Rudisill TM, Zhu M, Kelley GA, Pilkerton C, Rudisill BR. Medication use and the risk of motor vehicle collisions among licensed drivers: a systematic review. Accid Anal Prev. 2016;96:255–70. doi:10.1016/j.aap.2016.08.001.
Verster JC, Roth T. Gender differences in highway driving performance after administration of sleep medication: a review of the literature. Traffic Inj Prev. 2012;13(3):286–92. doi:10.1080/15389588.2011.652751.
Kriikku P, Hurme H, Wilhelm L, et al. Sedative-hypnotics are widely abused by drivers apprehended for driving under the influence of drugs. Ther Drug Monit. 2015;37(3):339–46. doi:10.1097/FTD.0000000000000138.
Hetland A, Carr D. Medications and impaired driving: a review of the literature. Ann Pharmacother. 2014;48(4):494–506. doi:10.1016/j.pestbp.2011.02.012.Investigations.
Greenblatt DJ. Sleep-promoting medications: weighing the hazards of use versus non-use. Clin Pharmacol Drug Dev. 2014;3(3):167–9. doi:10.1002/cpdd.127.
Leslie WD, Morin SN. Osteoporosis epidemiology 2013: implications for diagnosis, risk assessment, and treatment. Curr Opin Rheumatol. 2014;26(4):440–6. doi:10.1097/BOR.0000000000000064.
Sattui SE, Saag KG. Fracture mortality: associations with epidemiology and osteoporosis treatment. Nat Rev Endocrinol. 2014;10(10):592–602. doi:10.1038/nrendo.2014.125.
Abrahamsen B, van Staa T, Ariely R, Olson M, Cooper C. Excess mortality following hip fracture: a systematic epidemiological review. Osteoporos Int. 2009;20(10):1633–50. doi:10.1007/s00198-009-0920-3.
Cumming R, Le Couteur D. Benzodiazepines and risk of hip fractures in older people—a review of the evidence. CNS Drugs. 2003;17(11):825–37.
Aronson J. Hypnosedatives. In: Meyler’s side effects of psychiatric drugs. Elsevier; 2009. p. 375–450. https://www-clinicalkey-com.uml.idm.oclc.org/#!/browse/book/3-s2.0-C20090017863.
Mets MAJ, Volkerts ER, Olivier B, Verster JC. Effect of hypnotic drugs on body balance and standing steadiness. Sleep Med Rev. 2010;14(4):259–67. doi:10.1016/j.smrv.2009.10.008.
Allain H, Bentué-Ferrer D, Polard E, Akwa Y, Patat A. Postural instability and consequent falls and hip fractures associated with use of hypnotics in the elderly: a comparative review. Drugs Aging. 2005;22(9):749–65. doi:10.2165/00002512-200522090-00004.
Hartikainen S, Lonnroos E, Louhivuori K. Medication as a risk factor for falls: critical systematic review. J Gerontol A Biol Sci Med Sci. 2007;62(10):1172–81.
Woolcott JC, Richardson KJ, Wiens MO, et al. Meta-analysis of the impact of 9 medication classes on falls in elderly persons. Arch Intern Med. 2009;169(21):1952–60. doi:10.1001/archinternmed.2009.357.
Park H, Satoh H, Miki A, Urushihara H, Sawada Y. Medications associated with falls in older people: systematic review of publications from a recent 5-year period. Eur J Clin Pharmacol. 2015;71(12):1429–40. doi:10.1007/s00228-015-1955-3.
Takkouche B, Montes-Martinez A, Gill SS, Etminan M. Psychotropic medications and the risk of fracture: a meta-analysis. Drug Saf. 2007;30(2):171–84.
Panneman MJM, Goettsch WG, Kramarz P, Herings RMC. The costs of benzodiazepine-associated hospital-treated fall Injuries in the EU: a Pharmo study. Drugs Aging. 2003;20(11):833–9.
Khong TP, De Vries F, Goldenberg JSB, et al. Potential impact of benzodiazepine use on the rate of hip fractures in five large European countries and the United States. Calcif Tissue Int. 2012;91(1):24–31. doi:10.1007/s00223-012-9603-8.
Xing D, Ma XL, Ma JX, Wang J, Yang Y, Chen Y. Association between use of benzodiazepines and risk of fractures: a meta-analysis. Osteoporos Int. 2014;25(1):105–20. doi:10.1007/s00198-013-2446-y.
Ray WA, Griffin MR, Downey W. Benzodiazepines of long and short elimination half-life and the risk of hip fracture. JAMA. 1989;262(23):3303–7.
Cummings SR, Nevitt MC, Browner WS, et al. Risk factors for hip fracture in white women. Study of Osteoporotic Fractures Research Group. N Engl J Med. 1995;332(12):767–73. doi:10.1056/NEJM199503233321202.
Vestergaard P, Rejnmark L, Mosekilde L. Anxiolytics and sedatives and risk of fractures: effects of half-life. Calcif Tissue Int. 2008;82(1):34–43. doi:10.1007/s00223-007-9095-0.
Sgadari A, Lapane KL, Mor V, Landi F, Bernabei R, Gambassi G. Oxidative and nonoxidative benzodiazepines and the risk of femur fracture. The Systematic Assessment of Geriatric Drug Use Via Epidemiology Study Group. J Clin Psychopharmacol. 2000;20(2):234–9.
Wagner AK, Zhang F, Soumerai SB, et al. Benzodiazepine use and hip fractures in the elderly: who is at greatest risk? Arch Intern Med. 2004;164(14):1567–72. doi:10.1001/archinte.164.14.1567.
Chang C-M, Wu EC-H, Chang I-S, Lin K-M. Benzodiazepine and risk of hip fractures in older people: a nested case–control study in Taiwan. Am J Geriatr Psychiatry. 2008;16(8):686–92. doi:10.1097/JGP.0b013e31817c6a99.
Zint K, Haefeli W, Glynn R, Al E. Impact of drug interactions, dosage, duration of therapy on the risk of hip fracture associated with benzodiazepine use in older adults. Pharmacoepidemiol Drug Saf. 2010;19(12):1248–55. doi:10.1002/pds.2031.Impact.
de Vries OJ, Peeters G, Elders P, et al. The elimination half-life of benzodiazepines and fall risk: two prospective observational studies. Age Ageing. 2013;42(6):764–70. doi:10.1093/ageing/aft089.
Passaro A, Volpato S, Romagnoni F, Manzoli N, Zuliani G, Fellin R. Benzodiazepines with different half-life and falling in a hospitalized population: The GIFA study. Gruppo Italiano di Farmacovigilanza nell’Anziano. J Clin Epidemiol. 2000;53(12):1222–9.
Skinner BW, Johnston EV, Saum LM. Benzodiazepine initiation and dose escalation: a risk factor for inpatient falls. Ann Pharmacother. 2016;. doi:10.1177/1060028016682530.
Ray WA, Thapa PB, Gideon P. Benzodiazepines and the risk of falls in nursing home residents. J Am Geriatr Soc. 2000;48(6):682–5.
Herings RM, Stricker BH, de Boer A, Bakker A, Sturmans F. Benzodiazepines and the risk of falling leading to femur fractures. Dosage more important than elimination half-life. Arch Intern Med. 1995;155(16):1801–7.
Neutel CI, Hirdes JP, Maxwell CJ, Patten SB. New evidence on benzodiazepine use and falls: the time factor. Age Ageing. 1996;25(4):273–8. doi:10.1093/ageing/25.4.273.
Ham AC, Ziere G, Broer L, et al. CYP2C9 genotypes modify benzodiazepine-related fall risk: original results from three studies with meta-analysis. J Am Med Dir Assoc. 2016;18(1):88.e1–88.e15. doi:10.1016/j.jamda.2016.09.021.
Bartlett G, Abrahamowicz M, Grad R, Sylvestre M-P, Tamblyn R. Association between risk factors for injurious falls and new benzodiazepine prescribing in elderly persons. BMC Fam Pract. 2009;10:1. doi:10.1186/1471-2296-10-1.
Park SM, Ryu J, Lee DR, Shin D, Yun JM, Lee J. Zolpidem use and risk of fractures: a systematic review and meta-analysis. Osteoporos Int. 2016;27(10):2935–44. doi:10.1007/s00198-016-3605-8.
Finkle WD, Der JS, Greenland S, et al. Risk of fractures requiring hospitalization after an initial prescription for zolpidem, alprazolam, lorazepam, or diazepam in older adults. J Am Geriatr Soc. 2011;59(10):1883–90. doi:10.1111/j.1532.
Wang PS, Bohn RL, Glynn RJ, Mogun H, Avorn J. Zolpidem use and hip fractures in older people. J Am Geriatr Soc. 2001;49(12):1685–90. doi:10.1046/j.1532-5415.2001.49280.x.
Kang D-Y, Park S, Rhee C-W, et al. Zolpidem use and risk of fracture in elderly insomnia patients. J Prev Med Public Health. 2012;45(4):219–26. doi:10.3961/jpmph.2012.45.4.219.
Gillespie LD, Robertson MC, Gillespie WJ, et al. Interventions for preventing falls in older people living in the community. Cochrane database Syst Rev. 2012;. doi:10.1002/14651858.CD007146.pub3.
Ben Tsutaoka P. Chapter 31. Benzodiazepines. In: Olson KR, editor. Poisoning and drug overdose, 6e. New York: The McGraw-Hill Companies; 2012. http://mhmedical.com/content.aspx?aid=55975250.
Arroyo Plasencia AM, Ballentine LM, Mowry JB, Kao LW. Benzodiazepine-associated atrioventricular block. Am J Ther. 2012;19(1):e48–52. doi:10.1097/MJT.0b013e3181dcf572.
Day C. Benzodiazepines in combination with opioid pain relievers or alcohol: greater risk of more serious ED visit outcomes. The CBHSQ Report: December 18, 2014. Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration, Rockville, MD.
Jones JD, Mogali S, Comer SD. Polydrug abuse: a review of opioid and benzodiazepine combination use. Drug Alcohol Depend. 2012;125(1–2):8–18. doi:10.1016/j.drugalcdep.2012.07.004.
Jann M, Kennedy WK, Lopez G. Benzodiazepines: a major component in unintentional prescription drug overdoses with opioid analgesics. J Pharm Pract. 2014;27(1):5–16. doi:10.1177/0897190013515001.
Horsfall JT, Sprague JE. The pharmacology and toxicology of the “Holy Trinity”. Basic Clin Pharmacol Toxicol. 2016;. doi:10.1111/bcpt.12655.
Hwang CS, Kang EM, Kornegay CJ, Staffa JA, Jones CM, McAninch JK. Trends in the concomitant prescribing of opioids and benzodiazepines, 2002–2014. Am J Prev Med. 2016;51(2):1–10. doi:10.1016/j.amepre.2016.02.014.
Saunders KW, Von Korff M, Campbell CI, et al. Concurrent use of alcohol and sedatives among persons prescribed chronic opioid therapy: prevalence and risk factors. J Pain. 2012;13(3):266–75. doi:10.1016/j.jpain.2011.11.004.
Mellbye A, Svendsen K, Borchgrevink PC, Skurtveit S, Fredheim OMS. Concomitant medication among persistent opioid users with chronic non-malignant pain. Acta Anaesthesiol Scand. 2012;56(10):1267–76. doi:10.1111/j.1399-6576.2012.02766.x.
Skurtveit S, Furu K, Bramness J, Selmer R, Tverdal A. Benzodiazepines predict use of opioids—a follow-up study of 17,074 men and women. Pain Med. 2010;11(6):805–14. doi:10.1111/j.1526-4637.2010.00870.x.
Bramness JG, Kornor H. Benzodiazepine prescription for patients in opioid maintenance treatment in Norway. Drug Alcohol Depend. 2007;90(2–3):203–9. doi:10.1016/j.drugalcdep.2007.03.008.
National Institute on Drug Abuse (NIDA). Overdose death rates. 2017. https://www.drugabuse.gov/related-topics/trends-statistics/overdose-death-rates. Accessed 2 Feb 2017.
Bachhuber MA, Hennessy S, Cunningham CO, Starrels JL. Increasing benzodiazepine prescriptions and overdose mortality in the United States, 1996–2013. Am J Public Health. 2016;106(4):686–8. doi:10.2105/AJPH.2016.303061.
Jones CM, McAninch JK. Emergency department visits and overdose deaths from combined use of opioids and benzodiazepines. Am J Prev Med. 2015;49(4):493–501. doi:10.1016/j.amepre.2015.03.040.
Coben JH, Davis SM, Furbee PM, Sikora RD, Tillotson RD, Bossarte RM. Hospitalizations for poisoning by prescription opioids, sedatives, and tranquilizers. Am J Prev Med. 2010;38(5):517–24. doi:10.1016/j.amepre.2010.01.022.
Isbister GK, O’Regan L, Sibbritt D, Whyte IM. Alprazolam is relatively more toxic than other benzodiazepines in overdose. Br J Clin Pharmacol. 2004;58(1):88–95. doi:10.1111/j.1365-2125.2004.02089.x.
Park TW, Saitz R, Ganoczy D, Ilgen MA, Bohnert ASB. Benzodiazepine prescribing patterns and deaths from drug overdose among US veterans receiving opioid analgesics: case–cohort study. BMJ. 2015;350:h2698.
Turner BJ, Liang Y. Drug overdose in a retrospective cohort with non-cancer pain treated with opioids, antidepressants, and/or sedative–hypnotics: interactions with mental health disorders. J Gen Intern Med. 2015;30(8):1081–96. doi:10.1007/s11606-015-3199-4.
Buckley NA, McManus PR. Changes in fatalities due to overdose of anxiolytic and sedative drugs in the UK (1983–1999). Drug Saf. 2004;27(2):135–41. doi:10.2165/00002018-200427020-00004.
Sanders RD, Godlee A, Fujimori T, et al. Benzodiazepine augmented gamma-amino-butyric acid signaling increases mortality from pneumonia in mice. Crit Care Med. 2013;41(7):1627–36. doi:10.1097/CCM.0b013e31827c0c8d.
Sanders RD, Grover V, Goulding J, et al. Immune cell expression of GABAA receptors and the effects of diazepam on influenza infection. J Neuroimmunol. 2015;282:97–103. doi:10.1016/j.jneuroim.2015.04.001.
Galdiero F, Bentivoglio C, Nuzzo I, et al. Effects of benzodiazepines on immunodeficiency and resistance in mice. Life Sci. 1995;57(26):2413–23.
Jirillo E, Maffione AB, Greco B, Cannuscio B, Calvello R, Covelli V. Triazolobenzodiazepines exert immunopotentiating activities on normal human peripheral blood lymphocytes. Immunopharmacol Immunotoxicol. 1993;15(2–3):307–19. doi:10.3109/08923979309026001.
Covelli V, Munno I, Decandia P, et al. Effects of benzodiazepines on the immune system. Acta Neurol (Napoli). 1991;13(5):418–23.
Covelli V, Maffione AB, Nacci C, Tato E, Jirillo E. Stress, neuropsychiatric disorders and immunological effects exerted by benzodiazepines. Immunopharmacol Immunotoxicol. 1998;20(2):199–209. doi:10.3109/08923979809038539.
Nakafero G, Sanders RD, Nguyen-Van-Tam JS, Myles PR. The association between benzodiazepines and influenza-like illness-related pneumonia and mortality: a survival analysis using UK Primary Care data. Pharmacoepidemiol Drug Saf. 2016;25:1263–73. doi:10.1002/pds.
Obiora E, Hubbard R, Sanders R. The impact of benzodiazepines on occurrence of pneumonia and mortality from pneumonia: a nested case–control and survival analysis in a population-based cohort. Thorax. 2013;68:163–70. doi:10.1016/j.jemermed.2013.03.009.
Hak E, Bont J, Hoes AW, Verheij TJM. Prognostic factors for serious morbidity and mortality from community-acquired lower respiratory tract infections among the elderly in primary care. Fam Pract. 2005;22(4):375–80. doi:10.1093/fampra/cmi020.
Vergis EN, Brennen C, Wagener M, Muder R. Pneumonia in long-term care: a prospective case–control study of risk factors and impact on survival. Arch Intern Med. 2001;161:2378–81.
Dublin S, Walker RL, Jackson ML, et al. Use of opioids or benzodiazepines and risk of pneumonia in older adults: a population-based case–control study. J Am Geriatr Soc. 2011;59(10):1899–907. doi:10.1111/j.1532-5415.2011.03586.x.Use.
van de Nadort C, Smeets HM, Bont J, Zuithoff NPA, Hak E, Verheij TJM. Prognosis of primary care patients aged 80 years and older with lower respiratory tract infection. Br J Gen Pract. 2009;59(561):e110–5. doi:10.3399/bjgp09X420239.
Joya FL, Kripke DF, Loving RT, Dawson A, Kline LE. Meta-analyses of hypnotics and infections: eszopiclone, ramelteon, zaleplon, and zolpidem. J Clin Sleep Med. 2009;5(4):377–83.
Liaw G-W, Hung D-Z, Chen W-K, Lin C-L, Lin I-C, Kao C-H. Relationship between acute benzodiazepine poisoning and acute pancreatitis risk. Medicine (Baltimore). 2015;94(52):e2376. doi:10.1097/MD.0000000000002376.
Lai SW, Lai HC, Lin CL, Liao KF. Zopiclone use associated with increased risk of acute pancreatitis: a case–control study in Taiwan. Int J Clin Pract. 2015;69(11):1275–80. doi:10.1111/ijcp.12689.
Lai SW, Lin CL, Liao KF. Increased relative risk of acute pancreatitis in zolpidem users. Psychopharmacology (Berl). 2015;232(12):2043–8. doi:10.1007/s00213-014-3833-6.
Abed A, Minaiyan M, Safaei A, Taheri D. Effect of diazepam on severity of acute pancreatitis: possible involvement of peripheral benzodiazepine receptors. ISRN Gastroenterol. 2013;2013:484128. doi:10.1155/2013/484128.
Jones MR, Hall OM, Kaye AM, Kaye AD. Drug-induced acute pancreatitis: a review. Ochsner J. 2015;15(1):45–51. http://www.ncbi.nlm.nih.gov/pubmed/25829880%5Cn. http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=PMC4365846.
Trivedi C, Pitchumoni C. Drug-induced pancreatitis: an update. J Clin Gastroenterol. 2005;39(8):709–16.
Roth T. Hypnotic use for insomnia management in chronic obstructive pulmonary disease. Sleep Med. 2009;10(1):19–25. doi:10.1016/j.sleep.2008.06.005.
Stege G, Vos PJE, van den Elshout FJJ, Richard Dekhuijzen PN, van de Ven MJT, Heijdra YF. Sleep, hypnotics and chronic obstructive pulmonary disease. Respir Med. 2008;102(6):801–14. doi:10.1016/j.rmed.2007.12.026.
Zhang XJ, Li QY, Wang Y, Xu HJ, Lin YN. The effect of non-benzodiazepine hypnotics on sleep quality and severity in patients with OSA: a meta-analysis. Sleep Breath. 2014;. doi:10.1007/s11325-014-0943-7.
Mason M, Cates CJ, Smith I. Effects of opioid, hypnotic and sedating medications on sleep-disordered breathing in adults with obstructive sleep apnoea. Cochrane database Syst Rev. 2015;. doi:10.1002/14651858.CD011090.pub2.
Vozoris NT, Wang X, Fischer HD, et al. Benzodiazepine drug use and adverse respiratory outcomes among older adults with COPD. Eur Respir J. 2014;44:332–40. doi:10.1183/13993003.01967-2015.
Ekström MP, Bornefalk-Hermansson A, Abernethy AP, Currow DC. Safety of benzodiazepines and opioids in very severe respiratory disease: national prospective study. BMJ. 2014;348:g445. doi:10.1136/bmj.g445.
Chen S-J, Yeh C-M, Chao T-F, et al. The use of benzodiazepine receptor agonists and risk of respiratory failure in patients with chronic obstructive pulmonary disease: a nationwide population-based case–control study. Sleep. 2015;38(7):1045–50. doi:10.5665/sleep.4808.
Chung W-S, Lai C-Y, Lin C-L, Kao C-H. Adverse respiratory events associated with hypnotics use in patients of chronic obstructive pulmonary disease. Medicine (Baltimore). 2015;94(27):e1110. doi:10.1097/MD.0000000000001110.
Nakafero G, Sanders RD, Nguyen-Van-Tam JS, Myles PR. Association between benzodiazepine use and exacerbations and mortality in patients with asthma: a matched case–control and survival analysis using the United Kingdom Clinical Practice Research Datalink. Pharmacoepidemiol Drug Saf. 2015;24(8):793–802. doi:10.1002/pds.3799.
Rodriguez-Roisin R, Garcia-Aymerich J. Should we exercise caution with benzodiazepine use in patients with COPD? Eur Respir J. 2014;44(2):284–6. doi:10.1183/09031936.00071014.
Battaglia S, Bezzi M, Sferrazza Papa GF. Are benzodiazepines and opioids really safe in patients with severe COPD? Minerva Med. 2014;105(6):1–7.
Simon ST, Higginson IJ, Booth S, Harding R, Weingartner V, Bausewein C. Benzodiazepines for the relief of breathlessness in advanced malignant and non-malignant diseases in adults. Cochrane database Syst Rev. 2016;10:7354. doi:10.1002/14651858.CD007354.pub3.
Rizzi L, Rosset I, Roriz-Cruz M. Global epidemiology of dementia: Alzheimer’s and vascular types. Biomed Res Int. 2014;. doi:10.1155/2014/908915.
Barker MJ, Greenwood KM, Jackson M, Crowe SF. Cognitive effects of long-term benzodiazepine use: a meta-analysis. CNS Drugs. 2004;18(1):37–48. doi:10.2165/00023210-200418010-00004.
Pariente A, De Gage SB, Moore N, Bégaud B. The benzodiazepine-dementia disorders link: current state of knowledge. CNS Drugs. 2016;30(1):1–7. doi:10.1007/s40263-015-0305-4.
Billioti de Gage S, Pariente A, Bégaud B. Is there really a link between benzodiazepine use and the risk of dementia? Expert Opin Drug Saf. 2015;. doi:10.1517/14740338.2015.1014796.
Islam MM, Iqbal U, Walther B, et al. Benzodiazepine use and risk of dementia in the elderly population: a systematic review and meta-analysis. Neuroepidemiology. 2016;. doi:10.1159/000454881.
Zhong G, Wang Y, Zhang Y, Zhao Y. Association between benzodiazepine use and dementia: a meta-analysis. PLoS One. 2015;10(5):1–16. doi:10.1371/journal.pone.0127836.
Takada M, Fujimoto M, Hosomi K. Association between benzodiazepine use and dementia: data mining of different medical databases. Int J Med Sci. 2016;13(11):825–34. doi:10.7150/ijms.16185.
Chan T-T, Leung WC-Y, Li V, et al. Association between high cumulative dose of benzodiazepine in Chinese patients and risk of dementia: a preliminary retrospective case–control study. Psychogeriatrics. 2017;. doi:10.1111/psyg.12239.
Bietry FA, Pfeil AM, Reich O, Schwenkglenks M, Meier CR. Benzodiazepine use and risk of developing Alzheimer’s disease: a case–control study based on swiss claims data. CNS Drugs. 2017;. doi:10.1007/s40263-016-0404-x.
Gray SL, Dublin S, Yu O, et al. Benzodiazepine use and risk of incident dementia or cognitive decline: prospective population based study. BMJ. 2016;352:i90. doi:10.1136/bmj.i90.
Chen PL, Lee WJ, Sun WZ, Oyang YJ, Fuh JL. Risk of dementia in patients with insomnia and long-term use of hypnotics: a population-based retrospective cohort study. PLoS One. 2012;. doi:10.1371/journal.pone.0049113.
Shih H-I, Lin C-C, Tu Y-F, et al. An increased risk of reversible dementia may occur after zolpidem derivative use in the elderly population: a population-based case–control study. Medicine (Baltimore). 2015;94(17):e809. doi:10.1097/MD.0000000000000809.
Bocti C, Roy-Desruisseaux J, Hudon C, Roberge P. Benzodiazepine and dementia: a time for reflection. Maturitas. 2013;75(2):105–6. doi:10.1016/j.maturitas.2013.03.001.
Barbui C, Gastaldon C, Cipriani A, Barbui C. Benzodiazepines and risk of dementia: true association or reverse causation? Epidemiol Psychiatr Sci. 2013;22(4):307–8. doi:10.1017/S2045796013000358.
Defrancesco M, Marksteiner J, Wolfgang Fleischhacker W, Blasko I. Use of benzodiazepines in Alzheimer’s disease: a systematic review of literature. Int J Neuropsychopharmacol. 2015;18(10):1–11. doi:10.1093/ijnp/pyv055.
Tampi RR, Tampi DJ. Efficacy and tolerability of benzodiazepines for the treatment of behavioral and psychological symptoms of dementia: a systematic review of randomized controlled trials. Am J Alzheimers Dis Other Dement. 2014;29(7):565–74. doi:10.1177/1533317514524813.
Brambilla G, Carrozzino R, Martelli A. Genotoxicity and carcinogenicity studies of benzodiazepines. Pharmacol Res. 2007;56(6):443–58. doi:10.1016/j.phrs.2007.08.006.
Kao CH, Sun LM, Su KP, et al. Benzodiazepine use possibly increases cancer risk: a population-based retrospective cohort study in Taiwan. J Clin Psychiatry. 2012;73(4):555–60. doi:10.4088/JCP.11m07333.
Iqbal U, Nguyen P-A, Syed-Abdul S, et al. Is long-term use of benzodiazepine a risk for cancer? Medicine (Baltimore). 2015;94(6):e483. doi:10.1097/MD.0000000000000483.
Kao CH, Sun LM, Liang JA, Chang SN, Sung FC, Muo CH. Relationship of zolpidem and cancer risk: a Taiwanese population-based cohort study. Mayo Clin Proc. 2012;87(5):430–6. doi:10.1016/j.mayocp.2012.02.012.
Kripke DF, Langer RD, Kline LE. Hypnotics’ association with mortality or cancer: a matched cohort study—with comments. BMJ Open. 2012;2(1):e000850. doi:10.1136/bmjopen-2012-000850.
Kim H-B, Myung S-K, Park YC, Park B. Use of benzodiazepine and risk of cancer: a meta-analysis of observational studies. Int J Cancer. 2016;. doi:10.1002/ijc.30443.
Harnod T, Lin CL, Sung FC, Kao CH. An association between benzodiazepine use and occurrence of benign brain tumors. J Neurol Sci. 2014;336(1–2):8–12. doi:10.1016/j.jns.2013.11.009.
Bradford-Hill A. The environment and disease: association or causation? Proc R Soc Med. 1965;58:295–300. doi:10.1016/j.tourman.2009.12.005.
Shakir SAW, Layton D. Causal association in pharmacovigilance and pharmacoepidemiology: thoughts on the application of the Austin Bradford-Hill criteria. Drug Saf. 2002;25(6):467–71. doi:10.2165/00002018-200225060-00012.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No sources of funding were used to assist in preparing this manuscript.
Conflict of interest
JB and CL have no conflicts of interest to disclose that are relevant to the contents of this manuscript.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Brandt, J., Leong, C. Benzodiazepines and Z-Drugs: An Updated Review of Major Adverse Outcomes Reported on in Epidemiologic Research. Drugs R D 17, 493–507 (2017). https://doi.org/10.1007/s40268-017-0207-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40268-017-0207-7