Abstract
Introduction
Antimicrobial prophylaxis before a surgical procedure can reduce the risk of surgical site infections (SSI). The literature suggests that the greater the lag period between the first dose of antimicrobial administration and surgical incision, the greater the chances of developing an SSI. Hence, appropriate timing of the administration of prophylactic antimicrobials is critical to maximize the benefits of prophylaxis.
Objective
To examine the association between the timing of prophylactic antimicrobial administration and SSI rate in a tertiary-care hospital.
Methodology
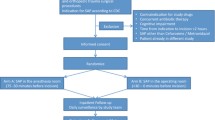
A total of 200 patients undergoing elective surgery from different surgical wards were included. Their detailed history, drug use especially that of antimicrobials, and surgical site were observed daily till discharge from the hospital. Odds ratios were calculated to examine the association between the timing of prophylactic antimicrobial use and the rate of SSIs.
Results
In the total population of 200 patients, 63 patients (31.5 %) received their first prophylactic antimicrobial dose within 30 min before incision, with SSIs occurring in 6 of these patients (9.5 %); 133 patients (66.5 %) received a prophylactic antimicrobial >30 min before incision, with SSIs occurring in 29 (21.8 %); and the remaining 4 (2 %) patients did not receive preoperative antimicrobials prior to incision, with SSIs occurring in 3 patients (75 %). The odds ratio of developing an SSI in patients receiving their first dose of preoperative antimicrobial >30 min before incision relative to those receiving their first dose of preoperative antimicrobial within 30 min before incision is 2.65.
Conclusion
This study examines the association between the timing of antimicrobial administration before surgery and the development of SSIs. Patients who received the antimicrobial dose too early before the procedure, including cases where the surgical procedure was delayed after the antimicrobial was administered, had an increased likelihood of an SSI. Efforts to improve the timing of antimicrobial administration are needed to decrease the SSI rate.
Similar content being viewed by others
References
Mangram AJ, Horan TC, Pearson ML, et al. Guideline for prevention of surgical site infection, 1999. Hospital Infection Control Practices Advisory Committee. Infect Control Hosp Epidemiol. 1999;1999(20):250–78.
Dale BW, Peter HM. Antimicrobial prophylaxis for surgery: an advisory statement from the National Surgical Infection Prevention Project. Clin Infect Dis. 2004;38:1706–15.
Hardman JG, Limbird LE, Gilman AG. Goodman and Gilman’s the pharmacological basis of therapeutics. 11th ed. New York: McGraw-Hill; 2006.
Dellinger EP, Hausmann S, Bratzler D, et al. Hospitals collaborate to decrease surgical site infections. Am J Surg. 2005;190:9–15.
Dettenkofer M, Forster DH, Ebner W, et al. The practice of perioperative antibiotic prophylaxis in eight German hospitals. Infection. 2002;30:164–7.
Shah A, Gajjar B, Shankar R. Antibiotic utilization for surgical prophylaxis in a tertiary care teaching rural hospital. Int J User Driven Healthcare. 2011;1(4):1–14.
Nestor MS. Perioperative use of antibiotics: preventing and treating perioperative infections. J Drugs Dermatol. 2005;4(6):34–6.
Yalcin AN, Serin S, Gurses E, et al. Surgical antibiotic prophylaxis in Turkish University Hospital. J Chemother. 2002;14:373–7.
Finkelstein R, Reinhertz G, Embom A. Surveillance of use of antibiotic prophylaxis in surgery. Isr J Med Science. 1996;32:1093–7.
Tourmousoglou CE, Yiannakopoulou EC, Kalapothaki V, et al. Adherence to guidelines for antibiotic prophylaxis in general surgery: a critical appraisal. J Antimicrob Chemother. 2008;61(1):214–8.
Shethwala MH, Gajjar BM. Study of pattern of antibiotic use for surgical prophylaxis in surgical departments of tertiary care urban hospital. PhD [dissertation], Vallabh Vidyanagar, Gujarat, India: Sardar Patel University; 2008.
Scottish Intercollegiate Guidelines Network (SIGN). Antibiotic prophylaxis in surgery (SIGN publication no. 104). Edinburgh: SIGN; 2008 (updated 2014).
Kulkarni RA, Kochhar PH, Dargude VA, et al. Patterns of antimicrobial use by surgeons in India. Ind J Surg. 2005;67:308–15.
Rehan HS, Kakkar A, Goel S. Surgical antibiotic prophylaxis in a tertiary care teaching hospital in India. Int J Infect Control. 2010;6(2):1–6.
Andrajati R, Vlcek J, Kolar M, et al. Survey of surgical antimicrobial prophylaxis in Czech Republic. Pharm World Sci. 2005;27:436–41.
Munckhof W. Antibiotics for surgical prophylaxis. Aust Prescr. 2005;28:38–40.
Classen DC, Evans RS, Pestotnik SL, et al. The timing of prophylactic administration of antibiotics and the risk of surgical-wound infection. N Engl J Med. 1992;326(5):281–6.
McDonald M, Grabsch E, Marshall C, et al. Single-versus multiple-dose antimicrobial prophylaxis for major surgery: a systematic review. Aust NZ J Surg. 1998;68:388–96.
Acknowledgments
Authors would like to thank Dr. G. V. Shah, the dean of the Institute for granting the permission to carry out the study in the premises and also sincere thanks to staff members of the surgical departments for their help in facilitation of data collection.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical clearance
This study was conducted in compliance with Ethical Standards of India as mentioned under Good Clinical Practices guidelines in Schedule Y. The study protocol was approved by the institutional ethics committee and written informed consent was obtained from all the participants before enrolling them in the study.
Funding source
None.
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Khakhkhar, T., Shah, R. & Hemavathi, K.G. Relationship between timing of surgical antimicrobial prophylaxis and surgical site infection in a tertiary-care hospital. Drugs Ther Perspect 32, 539–544 (2016). https://doi.org/10.1007/s40267-016-0347-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40267-016-0347-9