Abstract
Introduction
In 2020, the restrictions adopted to control the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) pandemic led to an unprecedented reduction in influenza-related burden. As such, the reduced chance to characterize the circulating virus strains might have increased the risk of vaccine mismatch for the forthcoming winter seasons. The role of an effective influenza vaccination campaign might therefore assume even more value, especially for frail and multimorbid older individuals. Methodological concerns on confounding by indication are always debated in vaccine effectiveness studies and it might be instrumental to give a pragmatic message on an individual’s responsibility to receive the influenza vaccine. We therefore investigated the role of specific confounders to explain the association between influenza vaccine and mortality among older adults.
Methods
Using a primary care database, we formed a cohort of patients aged 65 years or older who were actively registered with their general practitioner (GP) at the beginning of each of nine influenza seasons through to the 2018/2019 season. The study index date was the related seasons’ starting date. Exposure to the influenza vaccine was operationally defined in the 2 months preceding the index date up to 2 weeks before the exit date. Cox regression models were estimated to calculate hazard ratios (HRs) and their 95% confidence intervals (CI) of death between vaccinated and unvaccinated patients in a time-dependent fashion. The potential confounders sequentially entered the model based on their increasing effect size observed in univariate analyses.
Results
Over the 10 years under study, the influenza vaccine showed a significant protective effect in terms of mortality, reaching 13% reduction (HR 0.87, 95% CI 0.80–0.95) in the 2018/2019 influenza season. When we estimated the multivariate model by sequentially adding the potential confounders, there was an inversion of HR (below the unit) that was significantly explained by the covariates coding for a prior history of lower respiratory tract infections and the presence of the pneumococcal vaccine.
Conclusion
In the current pandemic scenario, we cannot divert attention to proper use of face masks, social distancing, and hand hygiene, which are important measures to prevent influenza and other respiratory viral infections. Nonetheless, their effectiveness might be negligible without acceptable coverage for influenza vaccine, especially in older patients with a history of lower respiratory tract infections, which appears to be the main source of confounding by indication.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
High vaccine coverage in older adults is the main strategy to prevent influenza-related burden and mortality, especially during the current pandemic scenario. |
To investigate the role of confounding by indication in observational studies on influenza vaccine effectiveness is instrumental to channel a public health message. |
Older patients with a history of lower respiratory tract infection, which is the main source of confounding by indication, are those who majorly benefit from influenza vaccination. |
1 Introduction
The influenza lethality rate is higher in older adults than in the general population. Nielsen et al. reported an excess mortality attributable to influenza of 24.4 per 100,000 individuals in the general population, with figures peaking at up to 118.2 per 100,000 among those aged 65 years or older [1]. A recent review showed that excess death rates due to influenza are more than sixfold higher in older people compared with the rest of the population [2].
To date, immunization is the most effective strategy to reduce the circulation of influenza viruses and limit their burdensome consequences on health. To note, several influenza vaccines are effective and have been approved for their utilization in older adults [3, 4]. In real-world evidence (RWE) studies using comparable methodologies [5, 6], older adults undergoing influenza vaccination were reported to experience a 20–35% risk reduction of all-cause mortality. The effectiveness of influenza vaccines was also confirmed by studies showing that millions of influenza infections can be prevented through vaccination, even in seasons that see a wider mismatch between the currently recommended vaccine and the circulating virus strain [7].
On average, during influenza seasons, from 10 to 30% of the global population is usually exposed to the infection. However, in 2020 the restrictions adopted to control the SARS-CoV-2 pandemic have led to an unprecedented reduction in influenza-related burden in the 2020/2021 season. In this scenario, it is possible to hypothesize that the drastic reduction in the circulation of influenza virus might have decreased herd immunity at the population level, especially in frail and multimorbid groups, subsequently promoting the rise of more serious influenza epidemics [7]. In this context, the role of an effective influenza vaccination campaign might assume even more value, given that vaccine coverage is still far from optimal. In Italy, despite the health and social threats due to the coronavirus disease 2019 (COVID-19) pandemic, the minimum coverage target of 75% for flu vaccine among those aged 65 years or older, as well as other individuals at risk for influenza complications, is far to be reached [8]. Some methodological aspects of RWE studies might be instrumental in giving a pragmatic message on the individual’s responsibility to receive the influenza vaccine, especially for frail and multimorbid older individuals [9]. The morbidity and frailty-related variables are indeed the main source of confounding by indication in epidemiological studies, along with the fact that clinicians’ behavior and patients’ acceptance of vaccination might influence the vaccine uptake, provision or coverage, which lead to under- or overestimates of influenza vaccine effectiveness [10]. In essence, patients’ and physicians’ perception of risk might contribute to channeling vaccination towards people more prone to develop influenza-related complications, including fatal events. As such, vaccine effectiveness might be artificially reduced by individuals’ baseline risk of influenza-related complications in vaccinated versus unvaccinated subjects. Moreover, the resistance to infectious disease decreases with advancing age [11] and immunosenescence undoubtedly affects the response to vaccines in older people [12,13,14].
To our knowledge, several studies adopted sound methods, such as test-negative case-control [5, 9] and/or propensity score matching design [6, 9], through which confounding by indication was fairly controlled. Nevertheless, they did not aim to uncover the role of each potential confounder in the association between vaccination and mortality risk across different epidemic seasons. We therefore investigated the role of specific confounders to explain the association between influenza vaccine and mortality among older adults.
2 Methods
2.1 Data Source
We used data from the Health Search Database (HSD) of the Italian College of General Practitioners and Primary Care. This data source is a general practice research database and covers data from computer-based patient records covering a total of 1.5 million patients. The HSD was established in 1998 by the Italian College of General Practitioners and Primary Care. The database contains clinical (diagnoses, patient referrals, hospital admissions, clinical investigation results and date of death) and lifestyle records (body mass index [BMI], smoking and alcohol use) as well as prescription data (drug name, prescription date, number of days’ supply) for the drugs that are reimbursed by the National Health System (NHS). All prescription data were coded with Anatomical Therapeutic Classification (ATC) codes, while the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) was used for all medical records. The GPs included in this study had to meet ‘up to standard’ quality criteria for epidemiological studies, particularly levels of coding, prevalence of well-known diseases, and mortality rates. Furthermore, only GPs who provided data for at least 1 year were included in the analysis. The HSD is a valid data source for scientific research and is aligned with the European Union guidelines on the use of medical data for research. Representativeness of the HSD has been previously demonstrated by comparing distributions of patient categories in age and sex with the National Institute of Statistics (https://www.healthsearch.it/). For these reasons, the HSD has been used as a data source in many studies and publications [15,16,17].
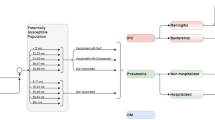
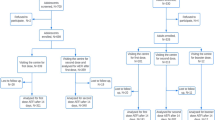
2.2 Study Population and Data Analyses
We formed a cohort of patients aged 65 years or older who were actively registered with their general practitioner (GP) at the beginning of 10 influenza seasons from 2009/2010 to 2018/2019. The 2016/2017 season was excluded because of the reduced quality of registration for vaccination as well as mortality. The study index dates were the starting dates for the specific seasons in keeping with the official observatories for influenza epidemics [8] (see Appendix 1). We excluded patients with < 1 year of medical history in the HSD. Eligible patients were followed until occurrence of the following events, whichever came first: all cause of death (event date), end of the epidemic period, end of data availability with the patient’s GP, or end of the study period (31 December 2019). A patient might be followed up in one or more influenza seasons. Exposure to the influenza vaccine was operationally defined in the 2 months preceding the index date up to 2 weeks before the exit date. This approach allowed us to ensure the biological plausibility of vaccine effectiveness according to the expected time for seroconversion [18]. Cox regression models were estimated to calculate hazard ratios (HRs) and related 95% confidence intervals (CI) of death between vaccinated and unvaccinated patients. The person-times of each individual could be counted in both the exposed and unexposed groups to avoid immortal time bias [19]. The potential confounders entered the model based on their increasing effect size observed in univariate analyses according to clinical (i.e., expected growing association between vaccine injection and mortality) and statistical (i.e., increasing p values) criteria. Besides age and sex, they included use of polypharmacy (more than four drugs), cardiovascular risk profile (moderate [< 5%], high [≥ 5 and < 10%], very high [≥ 10%] as per the European Society of Cardiology score) [20], diagnosis of other cardio/cerebral cardiovascular diseases (angina and other chronic ischemic cardiomyopathies), gastrointestinal disorders (gastritis, esophagitis, duodenitis, gastric/duodenal/esophagus hemorrhages), heart failure, atrial fibrillation, depression, asthma/chronic obstructive pulmonary disease (COPD), prior history of bronchitis and/or pneumonia, and presence of pneumococcal vaccination.
We conducted two sensitivity analyses to verify the robustness of the results. First, we evaluated the burden of vaccine under-registration (i.e. false-negative exposures) on the results as well as the influence of clinicians’ behavior and patients’ acceptance of vaccination as part of confounding by indication [10]. This is mainly due to the fact that GPs have the mandate to register vaccinations twice, in a public regional registry and in their own electronic health records. Such an increase in GPs’ workload might therefore reduce completeness of data collection. The primary analysis was therefore rerun by limiting GPs to those reporting a vaccine coverage of at least 55%, which is consistent with the coverage reported by official reports by the Italian public health authorities [8]. Second, the order with which the confounders entered the multivariate model was tested using backward stepwise regression (p = 0.15 and 0.10 for entering and exiting variables, respectively) [21]. By doing so, we were able to compare the clinical/biological and statistical basis with which the confounders entered the regression analysis.
Regarding analysis of the roles of specific confounders in explaining the results, both primary and sensitivity analyses were focused on the last influenza season (2017/2018) given its proximity to the incoming seasons. However, the same analyses were repeated over the other eight seasons and are reported in a dedicated Appendix (see Appendix 2).
3 Results
Over the nine seasons, the eligible population ranged from 285,244 (2018/2019 season) to 313,763 (2015/2016 season) patients aged 65 years or older (mean age 75.7 years, 57.32%). We reported a median incidence rate of 9.13 and 6.1 fatal cases per 100,000 person-weeks in vaccinated and unvaccinated elderly patients, respectively.
In Table 1, we report patient characteristics by vaccine exposure during the 2018/2019 epidemic season. Vaccinated patients were older than their counterparts, and those presenting with a ‘high’ or ‘very high’ cardiovascular risk were more likely to be vaccinated (43.6% vs. 41.1%; 37.8% vs. 28.6%). Several other comorbidities showed a higher prevalence in vaccinated than unvaccinated patients. Pneumococcal vaccination (25.5% vs. 8.6%) showed the greatest difference between vaccinated and unvaccinated individuals.
In Fig. 1, we depicted the HRs of mortality between vaccinated and unvaccinated patients over the influenza seasons. For the raw models, HRs showed a constant positive association between vaccine exposure and higher mortality rate. The estimates were almost fully reversed in multivariate analyses, showing a protective association between vaccine exposure and mortality. In the 2018/2019 winter season, the influenza vaccine showed a significant protective effect, in terms of mortality, as high as 13% (HR 0.87, 95% CI 0.80–0.95). As shown in Table 2, when we estimated the multivariate model for the 2018/2019 season by sequentially adding the covariates, there was an inversion of HRs triggered by the inclusion of polypharmacy (use of more than four drugs) in the model. Statistical significance was reached when the covariates coding for prior history of lower respiratory tract infections and the presence of pneumococcal vaccination were added to the model.
These findings were confirmed, even with a stronger effect size (HR 0.57, 95% CI 0.44–0.74 for the 2018/2019 season) (Fig. 2), when the analyses were restricted to those GPs reporting a vaccine coverage of at least 55%, which is consistent with the coverage reported by official reports from the Italian public health authorities [8]. Along this line, when the confounders entered the model using a stepwise backward regression (i.e. software-based approach), the results were consistent with those obtained for the primary model (Table 3).
Unadjusted and adjusted hazard ratios of mortality of patients exposed or unexposed to the influenza vaccine, restricting the sample population to GPs reporting a minimum vaccination coverage of 55%. Caption: Reference category = no vaccine. GPs general practitioners, HR hazard ratio, CI confidence interval
When the same analyses were repeated over the nine influenza seasons, the results were generally consistent with those observed during the 2018/2019 season, with the exception of the 2013/2014 and 2015/2016 seasons, in keeping with Figs. 1 and 2. However, especially when the analysis was limited to GPs with an influenza vaccine coverage of 55% or greater among elderly patients, inversion of the point estimate was statistically significant when covariates coding for polypharmacy and cardiovascular risk entered the model. The effect size showed a small increase when pneumococcal vaccination and history of lower respiratory tract infections were reached. Similar results were also obtained for the 2018/2019 season (Appendix 2).
4 Discussion
This retrospective study shows that among older primary care patients, the influenza vaccine presented a clear protective effect by reducing the risk of all-cause death by 13% during the 2018/2019 winter season. This effect was likely underestimated by exposure misclassification, as we have demonstrated by limiting the analyses to those GPs with a vaccine coverage of 55% or greater among elderly patients. These results were indeed consistent with the 20–30% risk reduction reported in previous studies [3, 5, 6]. Of note, these findings look to be strongly influenced by patients’ comorbidities. In this respect, while the raw model showed an artificial increased risk (36% higher) of death for vaccinated versus unvaccinated individuals, when the use of polypharmacy entered the model the HR moved below the unit and remained stable for the following seven covariates with no significant associations. After adjusting for the last two covariates, we found that a prior history of lower respiratory tract infections and/or pneumococcal vaccinations were the main confounders explaining the statistically significant reduction in mortality among vaccinated patients. Similar results were obtained for six of the other influenza seasons, although the inversion of point estimates was statistically significant before pneumococcal vaccination and a prior history of pneumonia entered the multivariate model. Confounding by indication might be viewed as a vector of covariates, including other comorbidities in addition to the respiratory conditions. The latter were therefore the main source of confounding for the 2018/2019 season, whose particular relevance is due to its proximity to the incoming influenza season. The fact that the 2013/2014 and 2015/2016 seasons did not show a significant protection for older vaccinees was likely due to vaccine mismatch [7, 22].
This methodological issue, which pertains to confounding by indication [10], has been tackled in prior investigations using a test-negative [5] study design and/or propensity score matching [6], but it also embeds a pragmatic message as to whether the relative weight of the individual confounder is examined. From a clinical and public health perspective, these findings may ease the identification of those individuals who can majorly benefit from influenza-related immunization. The role of the pneumococcal vaccine is indeed suggestive of conditions predisposing to pneumonia, therefore confirming that respiratory complications are likely the most burdening sequelae of influenza infection. Along this line, there is also public health relevance for the results on pneumococcal immunization. The acceptance and administration of the pneumococcal vaccine was indeed unsurprisingly related to the acceptance and administration of the influenza vaccine. In Italy, the fact that these vaccines are usually co-injected by GPs offers a clear advantage, which has not yet been homogeneously adopted across Italian regions. Such a strategy might therefore be universalized in primary care to foster the related vaccine coverage in older adults [3, 17].
This analysis suffers from some limitations to account for when interpreting the results. First, given the large underutilization of laboratory diagnostics, it was not possible to use laboratory-confirmed diagnoses of influenza, therefore assuming a causal relationship with death. However, our analyses were extended to several influenza seasons, therefore covering many temporal patterns of proportions of potential influenza cases, and consistent results were provided over the ten seasons. Second, some unmeasured confounding characteristics might explain part of the results. Specifically, the lack of variable coding for a holistic health status or frailty measure might be an unmeasured confounder with which a systematic prevention strategy could be properly planned. Third, we cannot exclude the burden of missing data on the operational definition of cardiovascular risk score, which includes information on BMI and smoking, which are generally featured by missing data. Nevertheless, this bias would be expectedly minimized, given that the distribution of older patients with unrecorded values is unlikely to be differential between exposure groups, given the higher propensity for this patient category to receive GP care [23, 24].
5 Conclusions
The SARS-CoV-2 pandemic led to an unprecedented reduction in influenza burden for the 2020/2021 winter season due to restrictions and preventive behavior posed by several countries. With the current relaxation of restrictions, the influenza virus has returned, along with other respiratory infections, and we could pay the reduction of herd immunity due to be almost exposed to the virus in the prior season. In this context, we cannot divert attention to the proper use of face masks, social distancing, and hand hygiene, which are important measures against several respiratory viral diseases. Nonetheless, their effectiveness might be negligible without acceptable influenza vaccine coverage, especially in older patients with a history of lower respiratory tract infections, which is the main source of confounding by indication.
References
Nielsen J, Krause TG, Mølbak K. Influenza-associated mortality determined from all-cause mortality, Denmark 2010/11-2016/17: The FluMOMO model. Influenza Other Respir Viruses. 2018;12(5):591–604.
Yedlapati SH, Khan SU, Talluri S, Lone AN, Khan MZ, Khan MS, et al. Effects of influenza vaccine on mortality and cardiovascular outcomes in patients with cardiovascular disease: A systematic review and meta-analysis. J Am Heart Assoc. 2021;10(6): e019636.
Domnich A, Arata L, Amicizia D, Puig-Barberà J, Gasparini R, Panatto D. Effectiveness of MF59-adjuvanted seasonal influenza vaccine in the elderly: A systematic review and meta-analysis. Vaccine. 2017;35:513–20.
DiazGranados CA, Dunning AJ, Kimmel M, Kirby D, Treanor J, Collins A, et al. Efficacy of high-dose versus standard-dose influenza vaccine in older adults. N Engl J Med. N Engl J Med. 2014;371:635–45.
Chung H, Buchan SA, Campigotto A, Campitelli MA, Crowcroft NS, Dubey V, et al. Influenza Vaccine Effectiveness against All-Cause Mortality following Laboratory-Confirmed Influenza in Older Adults, 2010–2011 to 2015–2016 Seasons in Ontario. Canada Clin Infect Dis. 2021;73:E1191–9.
Walzer P, Estève C, Barben J, Menu D, Cuenot C, Manckoundia P, et al. Impact of Influenza Vaccination on Mortality in the Oldest Old: A Propensity Score-Matched Cohort Study. Vaccines. Vaccines (Basel); 2020;8:356.
Marill MC. After flu vaccine mismatch, calls for delayed selection intensify. Nat Med. 2015;21:297–8.
Ministry of Health. Influenza. Available at: https://www.salute.gov.it/portale/influenza/dettaglioContenutiInfluenza.jsp?lingua=italiano&id=679&area=influenza&menu=vuoto
Andrew MK, Bowles SK, Pawelec G, Haynes L, Kuchel GA, McNeil SA, et al. Influenza Vaccination in Older Adults: Recent Innovations and Practical Applications. Drugs Aging. 2019;36(1):29–37.
Psaty BM, Koepsell TD, Lin D, Weiss NS, Siscovick DS, Rosendaal FR, et al. Assessment and control for confounding by indication in observational studies. J Am Geriatr Soc. 1999;47:749–54.
Pawelec G, Bronikowski A, Cunnane SC, Ferrucci L, Franceschi C, Fülöp T, et al. The conundrum of human immune system “senescence.” Mech Ageing Dev. 2020;192: 111357.
McElhaney JE, Verschoor CP, Andrew MK, Haynes L, Kuchel GA, Pawelec G. The immune response to influenza in older humans: Beyond immune senescence. Immun Ageing. 2020;17:1–10.
Andrew MK, Shinde V, Ye L, Hatchette T, Haguinet F, Dos SG, et al. The Importance of Frailty in the Assessment of Influenza Vaccine Effectiveness Against Influenza-Related Hospitalization in Elderly People. J Infect Dis J Infect Dis. 2017;216:405–14.
Vetrano DL, Triolo F, Maggi S, Malley R, Jackson TA, Poscia A, et al. Fostering healthy aging: The interdependency of infections, immunity and frailty. Ageing Res Rev. 2021;69: 101351.
Filippi A, Vanuzzo D, Bignamini AA, Mazzaglia G, Cricelli C, Catapano AL. The database of Italian general practitioners allows a reliable determination of the prevalence of myocardial infarction. Ital Heart J. 2005;6:311–4.
Dentali F, Fontanella A, Cohen AT, Simonetti M, Parretti L, Marconi E, et al. Derivation and Validation of a Prediction Model for Venous Thromboembolism in Primary Care. Thromb Haemost. 2020;120:692–701.
Lapi F, Marconi E, Simonetti M, Baldo V, Rossi A, Sessa A, et al. Adjuvanted versus nonadjuvanted influenza vaccines and risk of hospitalizations for pneumonia and cerebro/cardiovascular events in the elderly. Expert Rev Vaccines. 2019;18(6):663–70.
Rastogi S, Gross PA, Bonelli J, Dran S, Levandowski RA, Russo C, et al. Time to peak serum antibody response to influenza vaccine. Clin Diagn Lab Immunol. 1995;2(1):120–1.
Suissa S. Immeasurable time bias in observational studies of drug effects on mortality. Am J Epidemiol. 2008;168:329–35.
Piepoli MF, Hoes AW, Agewall S, Albus C, Brotons C, Catapano AL, et al. 2016 European Guidelines on cardiovascular disease prevention in clinical practice. Eur Heart J. 2016;37:2315–81.
Wang Q, Koval JJ, Mills CA, Lee KID. Determination of the Selection Statistics and Best Significance Level in Backward Stepwise Logistic Regression. Taylor & Francis Group. 2008;37:62–72. https://doi.org/10.1080/03610910701723625.
Systematic review of the efficacy, effectiveness and safety of newer and enhanced seasonal influenza vaccines [cited 2022 Apr 27]. Available at: https://www.ecdc.europa.eu/en/publications-data/seasonal-influenza-systematic-review-efficacy-vaccines
Delaney JA, Daskalopoulou SS, Brophy JM, Steele RJ, Opatrny L, Suissa S. Lifestyle variables and the risk of myocardial infarction in the general practice research database. BMC Cardiovasc Disord. 2007;7:38.
Delaney JAC, Moodie EEM, Suissa S. Validating the effects of drug treatment on blood pressure in the General Practice Research Database. Pharmacoepidemiol Drug Saf. 2008;17:535–45.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This article was supported by the Italian College of General Practitioners and Primary Care.
Conflicts of interest/competing interests
The authors declare the following financial interests/personal relationships which may be considered as potential competing interests: FL. and EM provided consultancies in protocol preparation for epidemiological studies and data analyses for Seqirus, GSK and Sanofi; IG, AR and CC provided clinical consultancies for Seqirus, GSK and Sanofi; MRG and DV have no conflict of interest to disclose.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent to publication
All authors approve the communication of the results included in this paper.
Availability of data and material
Not applicable.
Code availability
Not applicable.
Authors contribution
FL, EM, CC and AR designed and developed the study. FL extracted data and did the statistical analysis. FL, EM, CC, AR, MRG, and DV interpreted the data. FL drafted the manuscript and discussion with input from all other authors. All authors have seen and approved the final report.
Appendices
Appendix 1
Season | Epidemic period [8] | (Sub)type distribution, % | |||||||
|---|---|---|---|---|---|---|---|---|---|
Start | End | Duration, weeks | Peak | H1N1 | H1N1 pdm09 | H3N2 | A nt | B | |
1999/2000 | 1999–50 (13/12/99–19/12/99) | 2000–09 (28/02/00–5/03/00) | 12 | 2000–02 (10/01/00–16/01/00) | 2 | – | 80 | 17 | 1 |
2000/2001 | 2001–03 (15/01/01–21/01/01) | 2001–10 (5/03/01–11/03/01) | 8 | 2001–06 (5/02/01–11/02/01) | 72 | – | 0 | 20 | 8 |
2001/2002 | 2002–01 (31/12/01–6/01/02) | 2002–12 (18/03/02–24/03/02) | 12 | 2002–05 (28/01/02–3/02/02) | 0 | – | 25 | 1 | 74 |
2002/2003 | 2003–02 (6/01/03–13/01/03) | 2003–14 (31/03/03–6/04/03 | 13 | 2003–09 (24/02/03–2/03/03) | 5 | – | 89 | 1 | 5 |
2003/2004 | 2004–02 (5/01/04–11/01/04) | 2004–13 (22/03/04–28/03/04) | 12 | 2004–06 (2/02/04–8/02/04) | 2 | – | 71 | 19 | 8 |
2004/2005 | 2004–53 (27/12/04–2/01/05) | 2005–12 (21/03/05–27/03/05) | 13 | 2005–06 (7/02/05–13/02/05) | 10 | – | 49 | 24 | 17 |
2005/2006 | 2006–04 (23/01/06–29/01/06) | 2006–13 (27/03/06–2/04/06) | 10 | 2006–12 (20/03/06–26/03/06) | 37 | – | 14 | 26 | 23 |
2006/2007 | 2007–02 (8/01/07–14/01/07) | 2007–11 (12/03/07–18/03/07) | 10 | 2007–07 (12/02/07–18/02/07) | 24 | – | 52 | 18 | 6 |
2007/2008 | 2007–52 (24/12/07–30/12/07) | 2008–11 (10/03/08–16/03/08) | 12 | 2008–05 (28/01/08–3/02/08) | 38 | – | 6 | 48 | 8 |
2008/2009 | 2008–52 (22/12/08–28/12/08) | 2009–11 (9/03/09–15/03/09) | 12 | 2009–04 (19/01/09–25/01/09) | 82 | – | 4 | 9 | 6 |
2009/2010 | 2009–43 (19/10/09–25/10/09) | 2010–07 (15/02/10–21/02/10) | 11 | 2009–46 (15/11/10–21/11/10) | – | 96 | 2 | 1 | 1 |
2010/2011 | 2010–50 (13/12/10–19/12/10) | 2011–11 (14/03/11–20/03/11) | 14 | 2011–05 (31/01/11–6/02–11) | – | 62 | 2 | 8 | 28 |
2011/2012 | 2011–51 (19/12/11–25/12/11) | 2012–11 (12/03/12–18/03/12) | 13 | 2012–05 (30/01/12–5/02/12) | – | 0 | 89 | 7 | 4 |
2012/2013 | 2012–51 (17/12/12–23/12/12) | 2013–13 (25/03/13–31/03/13) | 15 | 2013–06 (4/02/13–10/02/13) | – | 34 | 5 | 3 | 58 |
2013/2014 | 2013–52 (23/12/13–29/13/13) | 2014–13 (24/03/14–30/03/14) | 14 | 2014–06 (3/02/14–9/03/14) | – | 34 | 56 | 7 | 3 |
2014/2015 | 2014–51 (15/12/14–21/12/14) | 2015–13 (23/03/15–29/03/15) | 15 | 2014–04 (19/01/15–25/01/15) | – | 44 | 34 | 6 | 16 |
2015/2016 | 2016–01 (4/01/16–10/01/16) | 2016–14 (4/04/16–10/04/16) | 14 | 2016–08 (22/02/16–28/02/16) | – | 24 | 15 | 4 | 57 |
2016/2017 | 2016–48 (28/11/16–4/12/16) | 2017–09 (27/02/17–5/03/17) | 14 | 2016–52 (26/12/16–1/01/17) | – | 1 | 88 | 6 | 5 |
2017/2018 | 2017–48 (27/11/17–3/12/17) | 2018–11 (12/03/18–18/03/18) | 17 | 2018–02 (8/01/18–14/01/18) | – | 38 | 1 | 1 | 60 |
2018/2019 | 2018–47 (19/11/18–25/11/18) | 2019–13 (25/03/19–31/03/19) | 19 | 2019–05 (28/01/19–3/02/19) | – | 46 | 46 | 8 | 0 |
Appendix 2. Sequential adjunct of confounders in the multivariate model estimating the risk of mortality between vaccinated or unvaccinated patients (from 2009/2010 to 2018/2019 influenza seasons; 2016/2017 season is excluded)
Full cohort | At least 55% vaccine coverage | |
|---|---|---|
HR (95% CI) | HR (95% CI) | |
Season 2009/2010 | ||
Raw model | 1.12 (1.03–1.22) | 0.68 (0.42–1.09) |
+ Gender | 1.12 (1.02–1.22) | 0.68 (0.42–1.09) |
+ Age | 0.99 (0.91–1.08) | 0.52 (0.32–0.84) |
+ Presence of polypharmacy | 0.74 (0.68–0.81) | 0.37 (0.22–0.61) |
+ Cardiovascular risk | 0.77 (0.7–0.84) | 0.37 (0.22–0.61) |
+ Other cerebrovascular disease | 0.76 (0.7–0.83) | 0.37 (0.22–0.61) |
+ Other cardiovascular disease | 0.76 (0.7–0.83) | 0.37 (0.22–0.61) |
+ Gastroinestinal disorders | 0.76 (0.69–0.83) | 0.36 (0.22–0.6) |
+ Hearth failure | 0.75 (0.69–0.82) | 0.36 (0.21–0.6) |
+ Atrial fibrillation | 0.75 (0.69–0.82) | 0.35 (0.21–0.59) |
+ Depression | 0.75 (0.68–0.81) | 0.36 (0.21–0.59) |
+ Asthma/COPD | 0.74 (0.68–0.81) | 0.35 (0.21–0.59) |
+ Presence of pneumococcal vaccination | 0.7 (0.64–0.77) | 0.34 (0.2–0.57) |
+ Prior history of bronchitis and/or pneumonia | 0.7 (0.64–0.77) | 0.34 (0.2–0.56) |
Season 2010/2011 | ||
Raw model | 1.5 (1.37–1.64) | 1.15 (0.98–1.35) |
+ Gender | 1.5 (1.37–1.64) | 1.14 (0.97–1.34) |
+ Age | 1.28 (1.17–1.4) | 0.86 (0.73–1.01) |
+ Presence of polypharmacy | 0.98 (0.89–1.07) | 0.58 (0.49–0.68) |
+ Cardiovascular risk | 0.98 (0.89–1.08) | 0.58 (0.49–0.69) |
+ Other cerebrovascular disease | 0.97 (0.88–1.06) | 0.58 (0.49–0.69) |
+ Other cardiovascular disease | 0.97 (0.88–1.06) | 0.58 (0.48–0.68) |
+ Gastroinestinal disorders | 0.96 (0.88–1.06) | 0.57 (0.48–0.68) |
+ Hearth failure | 0.95 (0.86–1.04) | 0.57 (0.48–0.67) |
+ Atrial fibrillation | 0.94 (0.86–1.04) | 0.57 (0.48–0.67) |
+ Depression | 0.94 (0.85–1.03) | 0.56 (0.47–0.67) |
+ Asthma/COPD | 0.93 (0.85–1.02) | 0.56 (0.47–0.67) |
+ Presence of pneumococcal vaccination | 0.9 (0.82–0.99) | 0.55 (0.46–0.66) |
+ Prior history of bronchitis and/or pneumonia | 0.89 (0.81–0.99) | 0.55 (0.46–0.65) |
Season 2011/2012 | ||
Raw model | 1.42 (1.3–1.56) | 1.29 (1.08–1.53) |
+ Gender | 1.42 (1.3–1.56) | 1.29 (1.08–1.53) |
+ Age | 1.22 (1.11–1.33) | 0.95 (0.8–1.13) |
+ Presence of polypharmacy | 0.95 (0.87–1.05) | 0.66 (0.55–0.79) |
+ Cardiovascular risk | 0.97 (0.88–1.06) | 0.66 (0.55–0.8) |
+ Other cerebrovascular disease | 0.96 (0.87–1.05) | 0.66 (0.55–0.79) |
+ Other cardiovascular disease | 0.96 (0.87–1.05) | 0.66 (0.55–0.79) |
+ Gastroinestinal disorders | 0.96 (0.87–1.05) | 0.66 (0.55–0.79) |
+ Hearth failure | 0.94 (0.86–1.04) | 0.65 (0.54–0.78) |
+ Atrial fibrillation | 0.94 (0.86–1.04) | 0.65 (0.54–0.78) |
+ Depression | 0.94 (0.86–1.03) | 0.65 (0.54–0.78) |
+ Asthma/COPD | 0.93 (0.85–1.03) | 0.65 (0.54–0.78) |
+ Presence of pneumococcal vaccination | 0.9 (0.82–0.99) | 0.64 (0.53–0.77) |
+ Prior history of bronchitis and/or pneumonia | 0.9 (0.82–0.99) | 0.63 (0.53–0.76) |
Season 2012/2013 | ||
Raw model | 1.51 (1.38–1.65) | 1.2 (0.96–1.49) |
+ Gender | 1.5 (1.38–1.65) | 1.2 (0.96–1.49) |
+ Age | 1.23 (1.13–1.35) | 0.83 (0.66–1.04) |
+ Presence of polypharmacy | 0.98 (0.9–1.08) | 0.59 (0.47–0.74) |
+ Cardiovascular risk | 0.98 (0.9–1.08) | 0.6 (0.47–0.76) |
+ Other cerebrovascular disease | 0.98 (0.89–1.07) | 0.6 (0.47–0.76) |
+ Other cardiovascular disease | 0.98 (0.89–1.07) | 0.59 (0.47–0.75) |
+ Gastroinestinal disorders | 0.97 (0.89–1.07) | 0.59 (0.47–0.75) |
+ Hearth failure | 0.96 (0.87–1.05) | 0.59 (0.47–0.75) |
+ Atrial fibrillation | 0.96 (0.87–1.05) | 0.59 (0.47–0.75) |
+ Depression | 0.96 (0.87–1.05) | 0.6 (0.47–0.76) |
+ Asthma/COPD | 0.95 (0.87–1.04) | 0.6 (0.47–0.75) |
+ Presence of pneumococcal vaccination | 0.91 (0.83–1.01) | 0.59 (0.47–0.75) |
+ Prior history of bronchitis and/or pneumonia | 0.91 (0.83–1.01) | 0.59 (0.46–0.75) |
Season 2013/2014 | ||
Raw model | 1.8 (1.64–1.99) | 1.8 (1.45–2.24) |
+ Gender | 1.8 (1.64–1.99) | 1.8 (1.45–2.23) |
+ Age | 1.46 (1.32–1.61) | 1.22 (0.98–1.51) |
+ Presence of polypharmacy | 1.18 (1.07–1.3) | 0.89 (0.71–1.12) |
+ Cardiovascular risk | 1.17 (1.05–1.29) | 0.89 (0.71–1.12) |
+ Other cerebrovascular disease | 1.16 (1.05–1.28) | 0.88 (0.7–1.11) |
+ Other cardiovascular disease | 1.16 (1.05–1.28) | 0.88 (0.7–1.1) |
+ Gastroinestinal disorders | 1.16 (1.05–1.28) | 0.88 (0.7–1.11) |
+ Hearth failure | 1.15 (1.04–1.27) | 0.88 (0.7–1.11) |
+ Atrial fibrillation | 1.14 (1.04–1.27) | 0.88 (0.7–1.11) |
+ Depression | 1.14 (1.03–1.26) | 0.88 (0.7–1.11) |
+ Asthma/COPD | 1.13 (1.02–1.25) | 0.88 (0.7–1.1) |
+ Presence of pneumococcal vaccination | 1.09 (0.98–1.21) | 0.88 (0.7–1.12) |
+ Prior history of bronchitis and/or pneumonia | 1.09 (0.99–1.21) | 0.88 (0.7–1.11) |
Season 2014/2015 | ||
Raw model | 1.64 (1.5–1.79) | 1.54 (1.21–1.96) |
+ Gender | 1.63 (1.49–1.79) | 1.54 (1.21–1.95) |
+ Age | 1.31 (1.2–1.43) | 1.03 (0.81–1.31) |
+ Presence of polypharmacy | 1.09 (0.99–1.19) | 0.79 (0.61–1.02) |
+ Cardiovascular risk | 1.08 (0.98–1.18) | 0.78 (0.61–1.01) |
+ Other cerebrovascular disease | 1.07 (0.98–1.18) | 0.78 (0.6–1) |
+ Other cardiovascular disease | 1.07 (0.97–1.17) | 0.77 (0.6–0.99) |
+ Gastroinestinal disorders | 1.07 (0.97–1.17) | 0.77 (0.6–0.99) |
+ Hearth failure | 1.06 (0.96–1.16) | 0.77 (0.59–0.99) |
+ Atrial fibrillation | 1.05 (0.96–1.16) | 0.76 (0.59–0.98) |
+ Depression | 1.05 (0.96–1.15) | 0.76 (0.59–0.98) |
+ Asthma/COPD | 1.04 (0.95–1.14) | 0.75 (0.58–0.97) |
+ Presence of pneumococcal vaccination | 0.99 (0.9–1.09) | 0.75 (0.57–0.97) |
+ Prior history of bronchitis and/or pneumonia | 0.99 (0.9–1.09) | 0.74 (0.57–0.97) |
Season 2015/2016 | ||
Raw model | 1.81 (1.63–2) | 1.65 (1.24–2.19) |
+ Gender | 1.8 (1.62–2) | 1.65 (1.24–2.19) |
+ Age | 1.41 (1.27–1.57) | 1.05 (0.79–1.41) |
+ Presence of polypharmacy | 1.16 (1.05–1.29) | 0.81 (0.6–1.09) |
+ Cardiovascular risk | 1.15 (1.04–1.28) | 0.79 (0.58–1.07) |
+ Other cerebrovascular disease | 1.15 (1.03–1.28) | 0.78 (0.58–1.06) |
+ Other cardiovascular disease | 1.15 (1.03–1.28) | 0.78 (0.58–1.06) |
+ Gastroinestinal disorders | 1.15 (1.03–1.28) | 0.78 (0.58–1.05) |
+ Hearth failure | 1.13 (1.02–1.26) | 0.78 (0.57–1.05) |
+ Atrial fibrillation | 1.13 (1.01–1.25) | 0.77 (0.57–1.04) |
+ Depression | 1.12 (1.01–1.25) | 0.77 (0.57–1.04) |
+ Asthma/COPD | 1.12 (1–1.24) | 0.76 (0.56–1.03) |
+ Presence of pneumococcal vaccination | 1.06 (0.95–1.19) | 0.76 (0.56–1.04) |
+ Prior history on bronchitis and/or pneumonia | 1.07 (0.96–1.2) | 0.76 (0.56–1.04) |
Season 2017/2018 | ||
Raw model | 1.32 (1.21–1.44) | 1.15 (0.91–1.47) |
+ Gender | 1.32 (1.21–1.43) | 1.15 (0.91–1.47) |
+ Age | 1.08 (0.99–1.18) | 0.84 (0.66–1.08) |
+ Presence of polypharmacy | 0.93 (0.85–1.01) | 0.64 (0.5–0.82) |
+ Cardiovascular risk | 0.9 (0.83–0.99) | 0.62 (0.48–0.8) |
+ Other cerebrovascular disease | 0.9 (0.82–0.98) | 0.62 (0.48–0.8) |
+ Other cardiovascular disease | 0.9 (0.82–0.98) | 0.62 (0.48–0.8) |
+ Gastroinestinal disorders | 0.9 (0.82–0.98) | 0.62 (0.48–0.8) |
+ Hearth failure | 0.88 (0.81–0.97) | 0.62 (0.48–0.8) |
+ Atrial fibrillation | 0.88 (0.81–0.96) | 0.62 (0.48–0.8) |
+ Depression | 0.88 (0.81–0.96) | 0.62 (0.48–0.79) |
+ Asthma/COPD | 0.87 (0.8–0.95) | 0.62 (0.48–0.79) |
+ Presence of pneumococcal vaccination | 0.8 (0.73–0.88) | 0.6 (0.46–0.78) |
+ Prior history on bronchitis and/or pneumonia | 0.8 (0.73–0.88) | 0.6 (0.46–0.77) |
Season 2018/2019 | ||
No Covariate | 1.36 (1.26–1.47) | 1.17 (0.91–1.49) |
+ Gender | 1.36 (1.26–1.47) | 1.16 (0.91–1.49) |
+ Age | 1.09 (1.01–1.18) | 0.79 (0.62–1.02) |
+ Presence of polypharmacy | 0.96 (0.89–1.04) | 0.59 (0.46–0.76) |
+ Cardiovascular risk | 0.95 (0.87–1.02) | 0.59 (0.46–0.76) |
+ Other cerebrovascular disease | 0.94 (0.87–1.02) | 0.59 (0.46–0.76) |
+ Other cardiovascular disease | 0.94 (0.87–1.02) | 0.59 (0.46–0.76) |
+ Gastroinestinal disorders | 0.94 (0.87–1.02) | 0.59 (0.46–0.76) |
+ Hearth failure | 0.93 (0.86–1.01) | 0.58 (0.45–0.75) |
+ Atrial fibrillation | 0.93 (0.86–1.01) | 0.58 (0.45–0.75) |
+ Depression | 0.93 (0.86–1.01) | 0.58 (0.45–0.75) |
+ Asthma/COPD | 0.92 (0.85–1.00) | 0.57 (0.44–0.74) |
+ Presence of pneumococcal vaccination | 0.87 (0.80–0.95) | 0.57 (0.44–0.74) |
+ Prior history on bronchitis and/or pneumonia | 0.87 (0.80–0.95) | 0.57 (0.44–0.74) |
Rights and permissions
About this article
Cite this article
Lapi, F., Marconi, E., Gualano, M.R. et al. A Cohort Study on Influenza Vaccine and All-Cause Mortality in Older Adults: Methodological Concerns and Public Health Implications. Drugs Aging 39, 645–656 (2022). https://doi.org/10.1007/s40266-022-00958-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40266-022-00958-7