Abstract
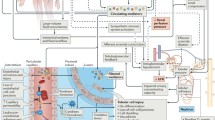
The care of patients with acute kidney injury (AKI) has been limited due to the lack of effective therapeutics that can either prevent AKI during high-risk situations or treat AKI once established. A revolution in the scientific understanding of the pathogenesis of AKI has led to the identification of potential therapeutic targets. These targets include pathways involved in inflammation, cellular repair and fibrosis, cellular metabolism and mitochondrial function, oxidative stress, apoptosis, and hemodynamics and oxygen delivery. Many compounds are entering early-phase clinical trials. In addition, efforts to better describe sub-categories of AKI (through endo-phenotyping) hold promise to target therapies more effectively based upon pathways that are operative in the pathogenesis. These advances bring optimism that the care of patients with AKI will be transformed with the hope of better outcomes.




Similar content being viewed by others
References
KDIGO clinical practice guideline for acute kidney injury. Kidney Int Suppl 2012;2:1–139.
United States Renal Data System (USRDS). https://www.usrds.org/2017/view/v1_05.aspx Accessed 14 Jan 2019.
Heung M, Steffick DE, Zivin K, Gillespie BW, et al. Acute kidney injury recovery pattern and subsequent risk of CKD: an analysis of Veterans Health Administration Data. Am J Kidney Dis. 2016;67:742–52.
Chawla LS. Acute kidney injury leading to chronic kidney disease and long-term outcomes of acute kidney injury: the best opportunity to mitigate acute kidney injury. Contrib Nephrol. 2011;174:182–90.
Collister D, Pannu N, Ye F, James M, et al. Health care costs associated with AKI. Clin J Am Soc Nephrol. 2017;12:1733–43.
Kerr M, Bedford M, Matthews B, O’Donoghue D. The economic impact of acute kidney injury in England. Nephrol Dial Transpl. 2014;29:1362–8.
Hobson C, Ozrazgat-Baslanti T, Kuxhausen A, Thottakkara P, et al. Cost and mortality associated with postoperative acute kidney injury. Ann Surg. 2015;261:1207–14.
de Caestecker M, Harris R. Translating knowledge into therapy for acute kidney injury. Semin Nephrol. 2018;38:88–97.
Jo SK, Rosner MH, Okusa MD. Pharmacologic treatment of acute kidney injury: why drugs haven’t worked and what is on the horizon. Clin J Am Soc Nephrol. 2007;2:356–65.
Zuk A, Palevsky PM, Fried L, Harrell FE Jr, et al. Overcoming translational barriers in acute kidney injury: a report from an NIDDK workshop. Clin J Am Soc Nephrol. 2018;13:1113–23.
Zuk A, Bonventre JV. Acute kidney injury. Annu Rev Med. 2016;67:293–307.
Ostermann M, Liu K. Pathophysiology of AKI. Best Pract Res Clin Anesthesiol. 2017;31:305–14.
Prowle JR, Bellomo R. Sepsis-associated acute kidney injury: macrohemodynamic and microhemodynamic alterations in the renal circulation. Semin Nephrol. 2015;35:64–74.
AtoxBio. Atox Bio Announces Enrollment of First Patient in Phase 2 Study of Acute Kidney Injury. http://www.atoxbio.com/clinical-data-7. Accessed 12 Feb 2019.
Kaempfer R, Arad G, Levy R, Hillman D, Nasie I, Rotfogel Z. CD28: direct and critical receptor for superantigen toxins. Toxins. 2013;5:1531–42.
Bulger EM, Maier RV, Sperry J, et al. A novel drug for treatment of necrotizing soft-tissue infections: a randomized clinical trial. JAMA Surg. 2014;149:528–36.
Arad G, Levy R, Nasie I, Hillman D, Rotfogel Z, Barash U, et al. Binding of superantigen toxins into the CD28 homodimer interface is essential for induction of cytokine genes that mediate lethal shock. PLoS Biol. 2011;9(9):e1001149. https://doi.org/10.1371/journal.pbio.1001149.
Arad G, Levy R, Hillman D, Kaempfer R. Superantigen antagonist protects against lethal shock and defines a new domain for T-cell activation. Nat Med. 2000;6:414–21.
Arad G, Hillman D, Levy R, Kaempfer R. Superantigen antagonist blocks Th1 cytokine gene induction and lethal shock. J Leukoc Biol. 2001;69:921–7.
Arad G, Hillman D, Levy R, Kaempfer R. Broad-spectrum immunity against superantigens is elicited in mice protected from lethal shock by a superantigen antagonist peptide. Immunol Lett. 2004;91:141–5.
Kaempfer R, Arad G, Levy R, Hillman D. Defense against biologic warfare with superantigen toxins. Isr Med Assoc J. 2002;4:520–3.
ClinicalTrials.gov. Identifier NCT02469857, phase III efficacy and safety study of AB103 in the treatment of patients with necrotizing soft tissue infections (ACCUTE). Bethesda: National Library of Medicine; 2015. Accessed 12 Feb 2019.
ClinicalTrials.gov. Identifier NCT03403751, phase 2 study of reltecimod vs placebo in patients with sepsis-associated acute kidney injury. Bethesda: National Library of Medicine; 2018 Accessed 12 Feb 2019.
Zhang Y, Darssan D, Pascoe E, Johnson D, Pi H, Dong J. Vitamin D status and mortality risk among patients on dialysis: a systematic review and meta-analysis of observational studies. Nephrol Dial Transpl. 2018;33:1742–51.
Sahay M, Kalra S, Bandgar T. Renal endocrinology: the new frontier. Indian J Endocrinol Metab. 2012;16(2):154–5.
Dusso AS. Kidney disease and vitamin D levels: 25-hydroxyvitamin D, 1,25-dihydroxyvitamin D, and VDR activation. Kidney Int Suppl. 2011;1:136–41.
Levin A, Bakris GL, Molitch M, et al. Prevalence of abnormal serum vitamin D, PTH, calcium, and phosphorus in patients with chronic kidney disease: results of the study to evaluate early kidney disease. Kidney Int. 2007;71:31–8.
Wolf M, Shah A, Gutierrez O, et al. Vitamin D levels and early mortality among incident hemodialysis patients. Kidney Int. 2007;72:1004–13.
Teng M, Wolf M, Lowrie E, Ofsthun N, Lazarus JM, Thadhani R. Survival of patients undergoing hemodialysis with paricalcitol or calcitriol therapy. N Engl J Med. 2003;349:446–56.
Wolf M, Betancourt J, Chang Y, et al. Impact of activated vitamin D and race on survival among hemodialysis patients. J Am Soc Nephrol. 2008;19:1379–88.
Teng M, Wolf M, Ofsthun MN, et al. Activated injectable vitamin D and hemodialysis survival: a historical cohort study. J Am Soc Nephrol JASN. 2005;16:1115–25.
Vijayan A, Li T, Dusso A, Jain S, Coyne DW. Relationship of 1,25 dihydroxy vitamin D levels to clinical outcomes in critically ill patients with acute kidney injury. J Nephrol Ther. 2015;5:190.
Lai L, Qian J, Yang Y, et al. Is the serum vitamin D level at the time of hospital-acquired acute kidney injury diagnosis associated with prognosis? PLoS One. 2013;8:e64964.
Leaf DE, Wolf M, Waikar SS, et al. FGF-23 levels in patients with AKI and risk of adverse outcomes. Clin J Am Soc Nephrol. 2012;7:1217–23.
Zhang M, Hsu R, Hsu CY, et al. FGF-23 and PTH levels in patients with acute kidney injury: a cross-sectional case series study. Ann Intensive Care. 2011;1:21.
Thadhani R, Pascual M, Bonventre JV. Acute renal failure. N Engl J Med. 1996;334:1448–60.
Banerjee M. Antiproliferative role of vitamin d and its analogs—a brief overview. Pubmed NCBI. http://www.ncbi.nlm.nih.gov. N.p., 2019. Web. Accessed 5 Feb 2019.
Cameron LK, Lei K, Smith S, et al. Vitamin D levels in critically ill patients with acute kidney injury: a protocol for a prospective cohort study (VID-AKI). BMJ Open. 2017;7:e016486. https://doi.org/10.1136/bmjopen-2017-016486.
ClinicalTrials.gov. Identifier NCT02962102, activated vitamin D for the prevention and treatment of acute kidney injury (ACTIVATE-AKI). Bethesda: National Library of Medicine; 2016. Accessed 12 Feb 2019.
Peters E, Heemskerk S, Masereeuw R, Pickkers P. Alkaline phosphatase: a possible treatment for sepsis-associated acute kidney injury in critically ill patients. Am J Kidney Dis. 2014;63:1038–48.
Peters E, Masereeuw R, Pickkers P. The potential of alkaline phosphatase as a treatment for sepsis-associated acute kidney injury. Nephron Clin Pract. 2014;127:144–8.
Pickkers P, Mehta RL, Murray PT, et al. Effect of human recombinant alkaline phosphatase on 7-day creatinine clearance in patients with sepsis-associated acute kidney injury: a randomized clinical trial. JAMA. 2018;320:1998–2009.
Kelly KJ, Plotkin Z, Vulgamott SL, Dagher PC. P53 mediates the apoptotic response to GTP depletion after renal ischemia-reperfusion: protective role of a p53 inhibitor. J Am Soc Nephrol. 2003;14:128–38.
Wei Q, Dong G, Yang T, Megyesi J, Price PM, Dong Z. Activation and involvement of p53 in cisplatin-induced nephrotoxicity. Am J Physiol Ren Physiol. 2007;293:F1282–91.
Thompson JD, Kornbrust DJ, Foy JW-D, Solano ECR, Schneider DJ, Feinstein E, Molitoris BA, Erlich S. Toxicological and pharmacokinetic properties of chemically modified siRNAs targeting p53 RNA following intravenous administration. Nucleic Acid Ther. 2012;22:255–64.
Molitoris BA, Dagher PC, Sandoval RM, Campos SB, et al. siRNA targeted to p53 attenuates ischemic and cisplatin-induced acute kidney injury. J Am Soc Nephrol. 2009;20:1754–64.
Demirjian S, Ailawadi G, Polinsky M, Bitran D, et al. Safety and tolerability study of an intravenously administered small interfering ribonucleic acid (siRNA) post on-pump cardiothoracic surgery in patients at risk of acute kidney injury. Kidney Int Rep. 2017;2:836–43.
ClinicalTrials.gov. Identifier NCT02610283. A study to evaluate efficacy and safety of QPI-1002 for prevention of acute kidney injury following cardiac surgery. Bethesda: National Library of Medicine; 2015. Accessed 12 Feb 2019.
Quark Pharmaceuticals, Inc. Quark Pharmaceuticals, Inc announces first patient dosed in phase 3 clinical trial of QPI-1002 for prevention of acute kidney injury following cardiac surgery. http://quarkpharma.com/?p=12506. Accessed 12 Feb 2019.
Jiang WG, Hiscox S. Hepatocyte growth factor/scatter factor, a cytokine playing multiple and converse roles. Histol Histopathol. 1997;1997(12):537–55.
Matsumoto K, Nakamura T. Roles of HGF as a pleiotropic factor in organ regeneration. EXS. 1993;65:225–49.
Weidner KM, Sachs M, Birchmeier W. The Met receptor tyrosine kinase transduces motility, proliferation, and morphogenic signals of scatter factor/hepatocyte growth factor in epithelial cells. J Cell Biol. 1993;121:145–54.
Organ SL, Tsao M-S. An overview of the c-MET signaling pathway. Ther Adv Med Oncol. 2011;3(1 Suppl):S7–19.
Ono K, Matsumori A, Shioi T, Furukawa Y, Sasayama S. Enhanced expression of hepatocyte growth factor/c-met by myocardial ischemia and reperfusion in a rat model. Circulation. 1997;95:2552–8.
Zhou D, Tan RJ, Lin L, Zhou L, Liu Y. Activation of hepatocyte growth factor receptor, c-met, in renal tubules is required for renoprotection after acute kidney injury. Kidney Int. 2013;84:509–20.
Gong R, Rifai A, Tolbert EM, Biswas P, Centracchio JN, Dworkin LD. Hepatocyte growth factor ameliorates renal interstitial inflammation in rat remnant kidney by modulating tubular expression of macrophage chemoattractant protein-1 and RANTES. J Am Soc Nephrol. 2004;15:2868–81.
Dai C, Yang J, Liu Y. Single injection of naked plasmid encoding hepatocyte growth factor prevents cell death and ameliorates acute renal failure in mice. J Am Soc Nephrol. 2002;13:411–22.
Fiaschi-Taesch NM, Santos S, Reddy V, Van Why SK, et al. Prevention of acute ischemic renal failure by targeted delivery of growth factors to the proximal tubule in transgenic mice: the efficacy of parathyroid hormone-related protein and hepatocyte growth factor. J Am Soc Nephrol. 2004;15:112–25.
Kamimoto M, Mizuno S, Matsumoto K, Nakamura T. Hepatocyte growth factor prevents multiple organ injuries in endotoxemic mice through a heme oxygenase-1-dependent mechanism. Biochem Biophys Res Commun. 2009;380:333–7.
Liu Y, Tolbert EM, Lin L, Thursby MA, Sun AM, Nakamura T, Dworkin LD. Up-regulation of hepatocyte growth factor receptor: an amplification and targeting mechanism for hepatocyte growth factor action in acute renal failure. Kidney Int. 1999;55:442–53.
Nakatani T, Kim T, Uchida J, Kumata N, Kawashima H, Sugimura K. Hepatocyte growth factor ameliorates renal hemodynamic disorder after ischemia/reperfusion. Int J Mol Med. 2002;10:217–9.
Narayan P, Duan B, Jiang K, et al. Late intervention with the small molecule BB3 mitigates postischemic kidney injury. Am J Physiol Renal Physiol. 2016;311:F352–61.
ClinicalTrials.gov. Identifier NCT01286727. Study to improve renal function after kidney transplantation. Bethesda: National Library of Medicine; 2011. Accessed 12 Feb 2019.
ClinicalTrials.gov. Identifier NCT02474667. Reduce the severity of DGF in recipients of a deceased donor kidney. Bethesda: National Library of Medicine; 2015. Accessed 12 Feb 2019.
ClinicalTrials.gov. Identifier NCT02771509. Study to prevent acute kidney injury after cardiac surgery involving cardiopulmonary bypass. Bethesda: National Library of Medicine; 2016. Accessed 12 Feb 2019.
Murphy PG, Myers DS, Davies MJ, et al. The antioxidant potential of propofol (2,6-diisopropylphenol). Br J Anaesth. 1992;68:613–8.
Rodriguez-Lopez JM, Sanchez-Conde P, Lozano FS. Laboratory investigation: effects of propofol on the systemic inflammatory response during aortic surgery. Can J Anaesth. 2006;53:701–10.
Sanchez-Conde P, Rodriguez-Lopez JM, Nicolas JL, et al. The comparative abilities of propofol and sevoflurane to modulate inflammation and oxidative stress in the kidney after aortic cross-clamping. Anesth Analg. 2008;106:371–8.
Wang HH, Zhou HY, Chen CC, Zhang XL, Cheng G. Propofol attenuation of renal ischemia/reperfusion injury involves heme oxygenase-1. Acta Pharmacol Sin. 2007;28:1175–80.
Feng Y, Bai T, Ma H, Wang JK. Propofol attenuates human proximal renal tubular epithelial cell injury induced by anoxia-reoxygenation. Lab Med. 2008;39:356–60.
Assad AR, Delou JM, Fonseca LM, Villela NR, Nascimento JH, Verçosa N, et al. The role of KATP channels on propofol preconditioning in a cellular model of renal ischemia-reperfusion. Anesth Analg. 2009;109:1486–92.
Obal D, Dettwiler S, Favoccia C, Rascher K, Preckel B, Schlack W. Effect of sevoflurane preconditioning on ischaemia/reperfusion injury in the rat kidney in vivo. Eur J Anesthesiol. 2006;23:319–26.
Higuchi H, Sumita S, Wada H, Ura T, Ikemoto T, Nakai T, et al. Effects of sevoflurane and isoflurane on renal function and on possible markers of nephrotoxicity. Anesthesiology. 1998;89:307–22.
Bang JY, Lee J, Oh J, Song JG, Hwang GS. The influence of propofol and sevoflurane on acute kidney injury after colorectal surgery: a retrospective cohort study. Anesth Analg. 2016;123:363–70.
Yoo Y-C, Shim J-K, Song Y, et al. Anesthetics influence the incidence of acute kidney injury following valvular heart surgery. Kidney Int. 2014;86:414–522.
Ammar AS, Mahmoud KM. Comparative effect of propofol versus sevoflurane on renal ischemia/reperfusion injury after elective open abdominal aortic aneurysm repair. Saudi J Anaesth. 2016;10:301–7.
Leite TT, Macedo E, Martins Ida S, Neves FM, Liborio AB. Renal outcomes in critically ill patients receiving propofol or midazolam. Clin J Am Soc Nephrol. 2015;10:1937–45.
Kim N, Lee JG, Lee SH, Nam KS, et al. A comparison of propofol based total intravenous anesthesia and sevoflurane based balanced anesthesia on renal protection during lung transplantation under extracorporeal membrane oxygenation—a prospective, randomized trial. J Heart Lung Transplant. 2017;36:S116–7.
Nieuwenhuijs-Moeke GJ, et al. Propofol-based anaesthesia versus sevoflurane-based anaesthesia for living donor kidney transplantation: results of the VAPOR-1 randomized controlled trial. Br J Anaesth. 2017;118:720–32.
Ryter SW, Alam J, Choi AMK. Heme oxygenase-1/carbon monoxide: from basic science to therapeutic applications. Physiol Rev. 2006;86:583–650.
Ferenbach DA, Nkejabega NC, McKay J, Choudhary AK, Vernon MA, Beesley MF, et al. The induction of macrophage hemeoxygenase-1 is protective during acute kidney injury in aging mice. Kidney Int. 2011;79(9):966–76.
Thomas RA, Czopek A, Bellamy CO, McNally SJ, Kluth DC, Marson LP. Hemin preconditioning upregulates Heme oxygenase-1 in deceased donor renal transplant recipients: a randomized, controlled, phase IIB trial. Transplantation. 2016;100:176–83.
Guerci P, Ergin B, Ince C. The macro- and microcirculation of the kidney. Best Pract Res Clin Anesthesiol. 2017;31:315–29.
Chawla LS, Busse L, Brasha-Mitchell E. Intravenous angiotensin II for the treatment of high-output shock (ATHOS trial): a pilot study. Crit Care. 2014;18:534.
Brown NJ, Vaughan DE. Angiotensin-converting enzyme inhibitors. Circulation. 1998;97:1411–20.
Correa TD, Jeger V, Pereira AJ, Takala J, Djafarzadeh S, Jakob SM. Angiotensin II in septic shock: effects on tissue perfusion, organ function, and mitochondrial respiration in a porcine model of fecal peritonitis. Crit Care Med. 2014;42:e550–9.
Correa TD, Takala J, Jakob SM. Angiotensin II in septic shock. Crit Care. 2015;19:98.
Wan L, Langenberg C, Bellomo R, May CN. Angiotensin II in experimental hyperdynamic sepsis. Crit Care. 2009;13:R190.
Khanna A, English SW, Wang XS, et al. ATHOS-3 Investigators: angiotensin II for the treatment of vasodilatory shock. N Engl J Med. 2017;337:419–30.
Tumlin JA, Murughan R, Deane AM, Ostermann M, et al. Outcomes in patients with vasodilatory shock and renal replacement therapy treated with intravenous angiotensin II. Crit Care Med. 2018;46:949–57.
Nieminen MS, Pollesello P, Vajda G, et al. Effects of levosimendan on the energy balance: preclinical and clinical evidence. J Cardiovasc Pharmacol. 2009;53:302–10.
Faisal SA, Apatov DA, Ramakrishna H, Weiner MM. Levosimendan in cardiac surgery: evaluating the evidence. J Cardiovasc Vasc Anesth. 2018. https://doi.org/10.1053/j.jvca.2018.05.035.
Zhou C, Gong J, Chen D, Wang W, et al. Levosimendan for prevention of acute kidney injury after cardiac surgery: a meta-analysis of randomized controlled trials. Am J Kidney Dis. 2016;67:408–16.
Mouchiroud L, Houtkooper RH, Auwerx J. NAD (+) metabolism: a therapeutic target for age-related metabolic disease. Crit Rev Biochem Mol Biol. 2013;48:397–408.
Mehr AP, Tran MT, Ralto KM, Leaf DE, et al. De novo NAD+ biosynthetic impairment in acute kidney injury in humans. Nat Med. 2018;24:1351–9.
Mount PF, Power DA. Balancing the energy equation for healthy kidneys. J Pathol. 2015;237:407–10.
Paradies G, Petrosillo G, Paradies V, Ruggiero FM. Role of cardiolipin peroxidation and Ca2+ in mitochondrial dysfunction and disease. Cell Calcium. 2009;45:643–50.
Szeto H. Pharmacologic approaches to improve mitochondrial function in AKI and CKD. J Am Soc Nephrol. 2017;28:2856–65.
Choi YM, Kim HK, Shim W, Anwar MA, et al. Mechanism of cisplatin-induced cytotoxicity is correlated to impaired metabolism due to mitochondrial ROS generation. PLoS One. 2015;10:e0135083 (pmid:26247588).
Palevsky PM. Endpoints for clinical trials of acute kidney injury. Nephron. 2018;140:111–5.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
MHR: member of data safety-monitoring board for clinical studies funded by: Reata, Retrophin; consultant for Baxter Healthcare; editoral board for Clinical Journal of the American Society of Nephrology. MH: none.
Funding
No funding was received for the preparation of this manuscript.
Rights and permissions
About this article
Cite this article
Hulse, M., Rosner, M.H. Drugs in Development for Acute Kidney Injury. Drugs 79, 811–821 (2019). https://doi.org/10.1007/s40265-019-01119-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40265-019-01119-8