Abstract
Introduction
The currently licensed quadrivalent MenACWY-CRM conjugate vaccine presentation consists of two vials (lyophilized MenA and liquid MenCWY) to be reconstituted before injection. A new fully liquid, single-vial formulation has been developed to simplify administration and prevent reconstitution errors. We present pooled safety data from two randomized, controlled, observer-blind phase 2b clinical trials, in which the fully liquid presentation was compared with the licensed presentation.
Methods
This is a post hoc analysis of two studies, in which safety data from participants aged 10–40 years who received one dose of either liquid MenACWY-CRM (1337 participants; MenACWY liquid group) or licensed MenACWY-CRM (1332 participants; MenACWY licensed group) were pooled. Frequencies were calculated for solicited adverse events (AEs) during 7 days post-vaccination and unsolicited AEs, including medically attended AEs and serious AEs (SAEs), during the 6-month safety follow-up period. Analysis results are presented by vaccine group, overall and by age category (10–17 and 18–40 years).
Results
Overall, AEs solicited for collection during the first 7 days after vaccination were reported by similar percentages of participants (69.2%, MenACWY liquid; 68.2%, MenACWY licensed), and were generally mild/moderate in intensity. Solicited local AEs were reported by 46.0% of the MenACWY liquid group and 43.5% of the MenACWY licensed group and solicited systemic AEs by 55.2 and 54.1%, respectively. During the 6-month post-vaccination period, unsolicited AEs were reported by 32.2 and 31.2% of the MenACWY liquid group and MenACWY licensed group, respectively, and medically attended AEs by 18.6 and 17.3%, respectively. Overall, 14 participants in each group (1.0 and 1.1%, respectively) reported SAEs, none of which was considered vaccine-related by the investigator. The safety profiles of both MenACWY-CRM presentations were similar for each age group and overall.
Conclusions
This pooled analysis shows the safety profile of fully liquid MenACWY-CRM is comparable with that of the currently licensed vaccine presentation.
Clinical Trial Registration
ClinicalTrials.gov Identifiers: NCT03652610 (August 29, 2018), NCT03433482 (14 February 2018).
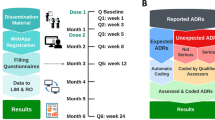
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
The currently licensed presentation of the MenACWY-CRM vaccine, which is used to immunize against meningococcal disease caused by four meningococcal serogroups, is marketed as a lyophilized serogroup A component and a liquid serogroups C, W, and Y component, for reconstitution before injection. |
To simplify vaccine administration and prevent reconstitution errors, a fully liquid, single-vial presentation of the MenACWY-CRM vaccine has been developed containing the same amount of each antigen. |
Two studies compared the new fully liquid MenACWY-CRM presentation with the licensed presentation. Pooled safety data from these studies confirm that the safety profiles of the two vaccine presentations are similar, supporting the introduction of the fully liquid MenACWY-CRM vaccine, once approved. |
1 Introduction
Invasive meningococcal disease (IMD), caused by Neisseria meningitidis, has an unpredictable onset with rapid progression, is life-threatening, and is associated with a broad range of persisting physical, neurological, and psychological sequelae in survivors [1, 2]. Six of the 12 meningococcal serogroups (MenA, B, C, W, Y, and X) are responsible for almost all IMD cases [3]. Among the available meningococcal vaccines, monovalent MenC and quadrivalent MenACWY glycoconjugate vaccines and protein-based MenB vaccines are commonly used [4, 5].
The quadrivalent glycoconjugate vaccine MenACWY-CRM (Menveo, GSK) was first licensed in 2010 and has a well-established safety and immunogenicity profile [6, 7]. The vaccine uses non-toxic diphtheria cross-reacting material 197 (CRM197) as carrier protein, conjugated to MenA, MenC, MenW, and MenY polysaccharides. The licensed vaccine consists of two vials; before administration, the MenA component, which is lyophilized, is reconstituted using the liquid MenCWY component [8]. The structure of MenA conjugated polysaccharide is labile in aqueous solution in terms of the glycosidic linkage and susceptibility to hydrolytic degradation [9, 10].
In field usage, as for other vaccines requiring reconstitution, some administration errors have been reported for the MenACWY-CRM vaccine, with only the liquid MenCWY component administered or the lyophilized MenA component reconstituted in sterile water, saline, a different liquid vaccine, or an unspecified diluent [11]. A fully liquid presentation of MenACWY-CRM vaccine, containing in a single vial the same amounts of antigen as the licensed presentation, has been developed to ease administration and avoid potential reconstitution and administration errors. Excipients that were necessary for lyophilization of the MenA component of MenACWY-CRM licensed vaccine (i.e., potassium dihydrogen phosphate and sucrose) are not required in the liquid presentation. In two randomized controlled phase 2b studies, the immunogenicity, reactogenicity, and safety profiles of the new fully liquid presentation were similar to those of the licensed presentation [12, 13]. In both studies, the fully liquid presentation was aged via either a controlled artificial process [12] or storage up to the end of the intended shelf-life [13] to test its immunogenicity under stress conditions.
In this article, we present a comprehensive overview of the safety profile of the fully liquid MenACWY presentation, using pooled tolerability and safety data from over 2600 participants in the two phase 2b studies [12, 13]. We also present, for the first time, safety data by age group (10–17 years and 18–40 years).
2 Methods
2.1 Study Design and Participants
This was a post hoc analysis, pooling safety data from two multicenter, randomized, controlled, observer-blind, phase 2b clinical studies in which participants received a single dose of either the fully liquid investigational presentation or the licensed presentation of MenACWY-CRM vaccine. The methods and results of each individual study have been published [12, 13] and study summaries are available at www.gsk-studyregister.com (study identifiers: 205343 and 207467). The first study (study #1; ClinicalTrials.gov Identifier: NCT03652610) recruited 979 healthy adults (age 18–40 years) between September 2018 and June 2019 in Australia, Belgium, Canada, Germany, and Italy, and the second study (study #2; NCT03433482) recruited 1690 adolescents and young adults (age 10–40 years) between August 2018 and December 2019 in Brazil, Estonia, Finland, France, Mexico, Russia, South Africa, Spain, and Turkey. The primary objective in both studies was demonstration of the non-inferiority of fully liquid MenACWY-CRM to the licensed presentation, as measured by human serum bactericidal assay geometric mean titers against MenA, the only component modified from lyophilized to liquid in the new presentation, 1 month post-vaccination. Immunological non-inferiority against MenA was fully demonstrated in both studies, based on the between-groups ratio of geometric mean antibody titers elicited at 1 month from vaccination [12, 13].
Clinical tolerability (solicited reactions within 7 days after vaccination) and safety (unsolicited adverse events [AEs] for the full study duration of 6 months) data were assessed as secondary objectives and were pooled for this post hoc integrated safety analysis of more than 2600 enrolled participants, half of whom were exposed to the new fully liquid presentation of MenACWY-CRM vaccine. The publications of the individual study results [12, 13] presented safety data for the overall study population in each of the two clinical trials; here, we report an integrated safety analysis of the two studies for all participants and also safety data by age group (10–17 years and 18–40 years).
2.2 Study Vaccines
In both studies, participants received in the deltoid region of the non-dominant arm a single 0.5 mL intramuscular dose of either the investigational fully liquid MenACWY-CRM presentation (MenACWY liquid group) or the licensed MenACWY-CRM presentation (MenACWY licensed group). The investigational fully liquid presentation and the licensed presentation of the vaccine contained the same CRM-conjugated meningococcal active components (10 µg MenA-CRM197 and 5 µg each of MenC-, MenW-, and MenY-CRM197). The fully liquid presentation did not include the excipients sucrose and potassium dihydrogen phosphate needed for the MenA lyophilized component in the licensed presentation. Fully liquid MenACWY was tested under stress conditions induced by an artificial, accelerated, controlled ageing process, involving storage at around 22.5 °C (± 2 °C) for approximately 2 months during the usual 2–8 °C storage period (study #1 [12]) or storage up to the intended shelf-life, approximately 24 or 30 months, at 2–8 °C in normal conditions (study #2 [13]). The aim was to assess if, even under these stress conditions, the MenA component, more labile in its liquid presentation, was still able to elicit immune responses non-inferior to those induced by the licensed vaccine. Further technical details are published elsewhere [12, 13].
2.3 Collection of Tolerability and Safety Data
Tolerability and safety data were collected using the same procedures in both studies. Reactions immediately after vaccination were monitored in participants through 30-min observation periods at the study centers. Solicited local AEs included erythema, induration, and pain at the injection site; solicited systemic AEs included arthralgia, chills, fatigue, headache, loss of appetite, myalgia, and nausea. Solicited AEs and body temperature were reported by participants for 7 days post-vaccination via electronic diaries. Solicited AEs were categorized as mild, moderate, or severe, with “severe” defined as preventing normal activity or, for loss of appetite, not eating at all. Severe erythema and induration were defined as diameter over 100 mm. Fever was indicated by a body temperature of 38 °C or higher.
During the 29-day post-vaccination period, unsolicited AEs were recorded; an unsolicited AE was defined as any AE that was not solicited using the electronic diaries during the first 7 days post-vaccination and, after that period, any AE spontaneously reported by a participant or parent/legally acceptable representative. Serious AEs (SAEs), medically attended AEs, and AEs leading to withdrawal were reported over the entire study period of 6 months via study visits at day of vaccination and 29 days afterwards, and three telephone calls to each participant approximately 2 weeks, 3 months, and 6 months after vaccination. An SAE was defined as any untoward medical occurrence that resulted in death or disability/incapacity, was life-threatening, or required hospitalization or prolongation of existing hospitalization, or a congenital anomaly or birth defect in the offspring of a study participant.
Study investigators assessed the causal relationship of all AEs to vaccination.
2.4 Statistical Analysis
The pooled set of participants who had received vaccination in each study and had provided safety data were included in the integrated safety analysis, which is descriptive in nature. Percentages of participants with at least one AE were calculated with exact 95% confidence intervals (CIs). Data are presented overall and by the age groups 10–17 years and 18–40 years. Data for the 10–17 years age group are not pooled since this age group was included in study #2 only.
Statistical analyses were performed using SAS version 9.4 (SAS Institute Inc., Cary, NC, USA).
3 Results
3.1 Study Population
A total of 2669 participants aged 10–40 years received one dose of either fully liquid MenACWY-CRM (1337 participants) or licensed MenACWY-CRM (1332 participants), of which 25.6% (overall 683 participants: 342 in MenACWY liquid group; 341 in MenACWY licensed group) were aged 10–17 years. Main demographic characteristics were comparable between vaccine groups for the overall population and for the analysis by age group (Fig. 1).
Demographic characteristics of participants included in the pooled analysis of safety using data from two phase 2b clinical studies in which participants received a single dose of either the fully liquid investigational presentation (MenACWY liquid) or the licensed presentation (MenACWY licensed) of MenACWY-CRM vaccine. aOne participant was aged 44 years at enrolment and was excluded from the per-protocol immunogenicity analysis [12] but was included in the analysis of safety. N = number of participants who received either MenACWY liquid or MenACWY licensed vaccine; SD = standard deviation
3.2 Solicited Adverse Events
Overall, solicited AEs were reported in the 7-day post-vaccination period by similar proportions of participants in each vaccine group (69.2% in MenACWY liquid group; 68.2% in MenACWY licensed group). The proportion of participants reporting solicited local AEs was 46.0% in the MenACWY liquid group and 43.5% in the MenACWY licensed group, with injection site pain being most frequently reported (44.4 and 41.8%, respectively) (Table 1). Solicited systemic AEs were reported by 55.2% of participants in the MenACWY liquid group and 54.1% in the MenACWY licensed group, and the most frequent were headache (36.9 and 35.6%, respectively) and fatigue (36.2%, both groups) (Table 1).
In the age group analyses, any solicited AEs were reported by 72.4% of participants aged 10–17 years in the MenACWY liquid group and 72.1% in the MenACWY licensed group, and by 68.1 and 66.9%, respectively, of participants aged 18–40 years. Within each age group, the proportion of participants reporting each solicited local AE was similar between vaccine groups, with injection site pain most frequently reported (Table 2). Erythema and induration at the injection site tended to be reported more frequently in participants aged 10–17 years than in adults (Table 2).
Solicited systemic AEs were reported by 60.0% of participants aged 10–17 years in the MenACWY liquid group and 57.8% in the MenACWY licensed group, and by 53.5 and 52.9%, respectively, of those aged 18–40 years. The most frequently reported systemic AEs in each age group were headache (10–17 years: 42.9% in MenACWY liquid group and 36.7% in MenACWY licensed group; 18–40 years: 34.8 and 35.3%, respectively) and fatigue (10–17 years: 34.1 and 36.4%, respectively; 18–40 years: 36.9 and 36.2%, respectively) (Table 2). Comparison of the MenACWY liquid group and MenACWY licensed group within each age group showed similar proportions of participants reporting each solicited systemic AE between vaccine groups for both the 10–17 years and 18–40 years age groups. Several of the systemic AEs (chills, fever, and loss of appetite) tended to be reported by a lower proportion of adult participants than adolescents in the MenACWY licensed group (Table 2).
Solicited local and systemic AEs were generally mild to moderate in intensity, with few reports of severe solicited AEs (Tables 1, 2). There were only two reports of fever with temperature ≥ 40 °C, one in the MenACWY liquid group (18–40 years age group) and the other in the MenACWY licensed group (10–17 years age group), occurring within 3 days of vaccination.
3.3 Unsolicited Adverse Events
Proportions of participants reporting unsolicited AEs within 30 days of vaccination were similar between the two vaccine groups overall and by age group (Table 3). Overall, the three most frequently reported unsolicited AEs in the 29-day post-vaccination period were the same in each vaccine group: headache (3.6% in MenACWY liquid group and 3.8% in MenACWY licensed group), nasopharyngitis (1.8 and 2.3%, respectively), and upper respiratory tract infection (1.9 and 1.4%, respectively). Injection site pain was reported by 1.4 and 1.0%, respectively, injection site erythema by 1.2 and 0.9%, and rhinitis by 0.7 and 1.3%, respectively.
In the 10–17 years age group, injection site pain was reported by 11 participants (3.2%) in the MenACWY liquid group and seven (2.1%) in the MenACWY licensed group, injection site erythema by eight (2.3%) and five (1.5%) participants, respectively, and headache by seven (2.0%) and five (1.5%) participants, respectively. In the 18–40 years age group, injection site pain was reported by eight participants (0.8%) in the MenACWY liquid group and six (0.6%) in the MenACWY licensed group, injection site erythema by eight (0.8%) and seven (0.7%) participants, respectively, and headache by eight (0.8%) and 11 (1.1%) participants, respectively.
At least one unsolicited AE considered related to vaccination was reported in the 29-day post-vaccination period by 6.2% of participants in the MenACWY liquid group and 5.0% in the MenACWY licensed group. In the age group analyses, vaccine-related unsolicited AEs were reported by 7.3% of participants aged 10–17 years in the MenACWY liquid group and 5.0% of the MenACWY licensed group, and by 5.8 and 5.0%, respectively, of those aged 18–40 years. Overall, the three most frequently reported related unsolicited AEs were the same in each vaccine group: injection site pain (1.4% in MenACWY liquid group and 1.0% in MenACWY licensed group), injection site erythema (1.2 and 0.9%, respectively), and headache (1.1 and 1.2%, respectively).
During the entire safety follow-up period of 6 months, unsolicited AEs were reported by 32.2% of participants in the MenACWY liquid group and 31.2% in the MenACWY licensed group overall; by age group, these percentages were 36.3 and 28.4% for the 10–17 years group and 30.8 and 32.2% for the 18–40 years group (Table 3). Medically attended AEs were reported by 18.6 and 17.3% of participants in the MenACWY liquid group and MenACWY licensed group, respectively. Medically attended AEs assessed as related to vaccination were reported by few participants: 14 (1.0%) in the MenACWY liquid group and 11 (0.8%) in the MenACWY licensed group; nine were aged 10–17 years in each vaccine group. In adolescents, the most frequent vaccine-related medically attended AEs were, irrespective of vaccine group, injection site pain, reported by five participants (1.5%) in the MenACWY liquid group and four (1.2%) in the MenACWY licensed group, injection site induration, reported by four (1.2%) and three (0.9%) participants, respectively, and injection site erythema, reported by four (1.2%) and five (1.5%) participants, respectively. In the 18–40 years group, each medically attended AE considered related to vaccination was reported by one participant only (0.1%).
There were no reports of AEs leading to participant withdrawal from the two studies.
3.4 Serious Adverse Events
Fourteen participants in each group (1.0%, MenACWY liquid group; 1.1%, MenACWY licensed group) reported SAEs in the 6-month safety follow-up study period (Table 3). Fifteen SAEs were reported by 14 participants in the MenACWY liquid group: non-infective appendicitis, dengue fever, tooth abscess, post-procedural hemorrhage, soft tissue injury, tibia fracture, hemiplegic migraine, incomplete spontaneous abortion, spontaneous abortion (two participants), ruptured ovarian cyst, depression, attempted suicide, and (both in a single participant) ruptured ovarian cyst and pleural effusion. There were 14 SAEs reported by 14 participants in the MenACWY licensed group: atrial flutter, phimosis, hyperthyroidism, hernia, biliary colic, dengue fever, otitis externa, jaw fracture, wrist fracture, malignant melanoma, uterine cancer, tension headache, ectopic pregnancy, and adnexa uteri pain. Of the 14 participants in each group reporting SAEs, three were aged 10–17 years in the MenACWY liquid group (SAEs: post-procedural hemorrhage, depression, and ruptured ovarian cyst) and two were aged 10–17 years in the MenACWY licensed group (phimosis and otitis externa).
No SAE was considered to be related to the study vaccines and there were no deaths reported.
4 Discussion
Results from two phase 2b studies, which involved over 2600 participants, demonstrated that, even when the investigational vaccine was tested under stress conditions, induced by a controlled process or after storage in normal conditions up to the intended shelf-life, the fully liquid MenACWY-CRM presentation was as immunogenic as the unaged licensed presentation [12, 13]. Here we confirmed, using pooled data from two randomized, controlled clinical studies, that the safety profiles of the fully liquid MenACWY-CRM presentation and the currently licensed presentation are comparable, with no concerns identified with the new presentation. The single-vial liquid MenACWY-CRM presentation contains the same amount of antigen as the licensed presentation, the main difference being the absence of sucrose and potassium dihydrogen phosphate in the fully liquid presentation, which is included as lyophilization matrix for the MenA component of the licensed vaccine and is therefore not needed for the new liquid presentation.
Numerous clinical trials have demonstrated the robust immunogenicity of MenACWY-CRM in various age groups and its clinical tolerability and safety profile was shown to be similar to that of a plain polysaccharide vaccine [7, 14]. Additionally, the acceptable safety profile of MenACWY-CRM has been confirmed in large post-marketing safety studies [6]. The most frequent solicited AEs overall in older children, adolescents, and adults in the clinical trials were injection site pain, headache, and myalgia [6, 7]. In our integrated safety analysis, the most frequent solicited AEs in both vaccine groups were injection site pain, headache, and fatigue in the overall population and in the two age groups analyzed, with similar frequencies of each solicited AE between vaccine groups.
In the analysis of unsolicited AEs in the 29-day post-vaccination period, percentages were similar between the two vaccine groups overall and by age group, and the most frequent unsolicited AEs assessed as related to vaccination (injection site pain, erythema, and headache) were the same in the group analyses. In the 6-month follow-up period, SAEs were reported by 14 participants in each group. None of the SAEs were considered related to vaccination and there were no study withdrawals due to an AE. Altogether, the data from this large pooled analysis are consistent with the documented safety profile of the licensed MenACWY-CRM vaccine [6, 7, 15]. Moreover, while the aim of this safety analysis was only to compare two presentations of the same vaccine, indirect comparisons show that, overall, the clinical tolerability and safety profile of the fully liquid MenACWY-CRM vaccine evaluated in the two phase 2b clinical studies also appears comparable with that reported for fully liquid presentations of other licensed MenACWY conjugated vaccines (including as carrier diphtheria toxoid or tetanus toxoid) [16, 17].
Although interpretation of these results is descriptive in nature, a key strength is that the same safety monitoring procedures were used in the two phase 2b studies. We therefore consider this analysis of pooled data from 2,669 adolescents and adults who received fully liquid MenACWY-CRM or licensed MenACWY-CRM as providing a valuable overview of the clinical tolerability and safety profile of the new liquid MenACWY-CRM presentation in the participants evaluated.
5 Conclusions
The integrated safety analysis of two randomized, multicenter, controlled clinical studies shows the tolerability and safety profile of the single-vial fully liquid MenACWY-CRM presentation is comparable with that of the currently licensed MenACWY-CRM presentation, marketed since 2010. This, combined with its immunological non-inferiority to the licensed presentation, provides support for adopting the fully liquid MenACWY-CRM presentation, upon approval.
References
Wang B, Santoreneos R, Giles L, Haji Ali Afzali H, Marshall H. Case fatality rates of invasive meningococcal disease by serogroup and age: a systematic review and meta-analysis. Vaccine. 2019;37(21):2768–82. https://doi.org/10.1016/j.vaccine.2019.04.020.
Olbrich KJ, Müller D, Schumacher S, Beck E, Meszaros K, Koerber F. Systematic review of invasive meningococcal disease: sequelae and quality of life impact on patients and their caregivers. Infect Dis Ther. 2018;7(4):421–38. https://doi.org/10.1007/s40121-018-0213-2.
Parikh S, Campbell H, Bettinger JA, Harrison LH, Marshall HS, Martinon-Torres F, et al. The everchanging epidemiology of meningococcal disease worldwide and the potential for prevention through vaccination. J Infect. 2020;81:483–98. https://doi.org/10.1016/j.jinf.2020.05.079.
Pizza M, Bekkat-Berkani R, Rappuoli R. Vaccines against meningococcal diseases. Microorganisms. 2020. https://doi.org/10.3390/microorganisms8101521.
Martinón-Torres F, Taha MK, Knuf M, Abbing-Karahagopian V, Pellegrini M, Bekkat-Berkani R, et al. Evolving strategies for meningococcal vaccination in Europe: overview and key determinants for current and future considerations. Pathog Glob Health. 2021. https://doi.org/10.1080/20477724.2021.1972663.
Keshavan P, Pellegrini M, Vadivelu-Pechai K, Nissen M. An update of clinical experience with the quadrivalent meningococcal ACWY-CRM conjugate vaccine. Expert Rev Vaccines. 2018;17(10):865–80. https://doi.org/10.1080/14760584.2018.1521280.
Ruiz Garcia Y, Abitbol V, Pellegrini M, Bekkat-Berkani R, Soumahoro L. A decade of fighting invasive meningococcal disease: a narrative review of clinical and real-world experience with the MenACWY-CRM conjugate vaccine. Infect Dis Ther. 2021. https://doi.org/10.1007/s40121-021-00519-2.
Bröker M, Dull PM, Rappuoli R, Costantino P. Chemistry of a new investigational quadrivalent meningococcal conjugate vaccine that is immunogenic at all ages. Vaccine. 2009;27(41):5574–80. https://doi.org/10.1016/j.vaccine.2009.07.036.
Berti F, Romano MR, Micoli F, Pinto V, Cappelletti E, Gavini M, et al. Relative stability of meningococcal serogroup A and X polysaccharides. Vaccine. 2012;30(45):6409–15. https://doi.org/10.1016/j.vaccine.2012.08.021.
Beresford NJ, Martino A, Feavers IM, Corbel MJ, Bai X, Borrow R, et al. Quality, immunogenicity and stability of meningococcal serogroup ACWY-CRM197, DT and TT glycoconjugate vaccines. Vaccine. 2017;35(28):3598–606. https://doi.org/10.1016/j.vaccine.2017.03.066.
Su JR, Miller ER, Duffy J, Baer BM, Cano MV. Notes from the field: administration error involving a meningococcal conjugate vaccine–United States, March 1, 2010–September 22. MMWR Morb Mortal Wkly Rep. 2016;65(6):161–2. https://doi.org/10.15585/mmwr.mm6506a4.
Vandermeulen C, Leroux-Roels I, Vandeleur J, Staniscia T, Girard G, Ferguson M, et al. A new fully liquid presentation of MenACWY-CRM conjugate vaccine: results from a multicentre, randomised, controlled, observer-blind study. Vaccine. 2021;39(45):6628–36. https://doi.org/10.1016/j.vaccine.2021.09.068.
Díez-Domingo J, Tinoco JC, Poder A, Dinleyici EC, Nell H, Salamanca de la Cueva I, et al. Immunological non-inferiority of a new fully liquid presentation of the MenACWY-CRM vaccine to the licensed vaccine: results from a randomized, controlled, observer-blind study in adolescents and young adults. Hum Vaccin Immunother. 2022;18(1):1981085. https://doi.org/10.1080/21645515.2021.1981085.
Bröker M, Cooper B, Detora LM, Stoddard JJ. Critical appraisal of a quadrivalent CRM197 conjugate vaccine against meningococcal serogroups A, C W-135 and Y (Menveo) in the context of treatment and prevention of invasive disease. Infect Drug Resist. 2011;4:137–47. https://doi.org/10.2147/idr.s12716.
Lalwani S, Agarkhedkar S, Gogtay N, Palkar S, Agarkhedkar S, Thatte U, et al. Safety and immunogenicity of an investigational meningococcal ACWY conjugate vaccine (MenACWY-CRM) in healthy Indian subjects aged 2 to 75 years. Int J Infect Dis. 2015;38:36–42. https://doi.org/10.1016/j.ijid.2015.07.003.
Jackson LA, Baxter R, Reisinger K, Karsten A, Shah J, Bedell L, et al. Phase III comparison of an investigational quadrivalent meningococcal conjugate vaccine with the licensed meningococcal ACWY conjugate vaccine in adolescents. Clin Infect Dis. 2009;49(1):e1-10. https://doi.org/10.1086/599117.
Chang LJ, Hedrick J, Christensen S, Pan J, Jordanov E, Dhingra MS. A Phase II, randomized, immunogenicity and safety study of a quadrivalent meningococcal conjugate vaccine, MenACYW-TT, in healthy adolescents in the United States. Vaccine. 2020;38(19):3560–9. https://doi.org/10.1016/j.vaccine.2020.03.017.
Acknowledgements
The authors thank all participants, parents, and the clinical teams and investigators involved in the studies, particularly the principal investigators, Dr. Corinne Vandermeulen and Dr. Javier Díez-Domingo, for their roles in coordinating the conduct of the studies. We thank the GSK study teams for their contributions to the studies, as well as Lamine Soumahoro and Fabien François Gerard for critical review of this manuscript. The authors also thank Business & Decision Life Sciences platform for editorial assistance and manuscript coordination, on behalf of GSK. Joanne Knowles (independent medical writer, on behalf of Business & Decision Life Sciences) provided medical writing support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
GlaxoSmithKline Biologicals SA funded this study/research and was involved in all stages of study conduct, including analysis of the data. GlaxoSmithKline Biologicals SA also took in charge all costs associated with the development and publication of this article.
Conflict of interest
PVS, PT, GFDD, VR, TM, MC, VB, ML, and MP are employed by GSK. TA was employed by GSK when the analyses were conducted. PVS, TA, VB, ML, and MP hold shares in GSK. PVS, PT, GFDD, VR, TM, MC, TA, VB, ML, and MP declare no other financial and non-financial relationships and activities.
Availability of data
Anonymized individual participant data and study documents can be requested for further research from http://www.clinicalstudydatarequest.com.
Code availability
Not applicable.
Ethics approval
Studies #1 and #2 (NCT03652610 and NCT03433482) were conducted in accordance with the Declaration of Helsinki and Good Clinical Practice and approved by the appropriate ethics committees.
Consent to participate
Before enrolment in the studies, all individual participants aged at least 18 years provided written informed consent and parents/legally acceptable representatives provided written informed consent for individual participants younger than 18 years.
Consent to publish
Not applicable.
Author contributions
All authors contributed to the concept and design of the post hoc analysis. PVS, PT, GFDD, VR, TM, MC, and VB contributed to data generation and collection. All authors contributed to the analysis of data. All authors contributed to the writing or review of the manuscript and approved the final version for submission.
Trademark statement
Menveo is a trademark owned by or licensed to GSK.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Vir Singh, P., Tiberi, P., Di Domenico, G.F. et al. Fully Liquid MenACWY-CRM Vaccine: Results from an Integrated Safety Analysis. Drug Saf 46, 99–108 (2023). https://doi.org/10.1007/s40264-022-01242-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40264-022-01242-8