Abstract
Introduction
The serotonin 5-HT4 receptor agonist prucalopride is approved in the European Union for the treatment of chronic constipation. This offered the unique opportunity to include real-world observational data on cardiovascular safety in the new drug application for approval of prucalopride in the USA.
Methods
This observational population-based cohort study (EUPAS9200) conducted in five data sources (three in the UK, one in Sweden, and one in Germany [which was subsequently excluded from the pooled analyses]) aimed to estimate the pooled adjusted incidence rate ratio for major adverse cardiovascular events (defined as hospitalization for non-fatal acute myocardial infarction or stroke, and in-hospital cardiovascular death) in adult initiators of prucalopride compared with initiators of polyethylene glycol 3350 (PEG) following a common protocol. Standardized incidence rates and incidence rate ratios of major adverse cardiovascular events were derived using propensity score stratification. Sensitivity analyses explored the impact of exposure definition, outcome categories, interim cancer, and unmeasured confounding.
Results
The pooled analyses included 5715 initiators of prucalopride and 29,372 initiators of PEG. Average duration of use was 175 days for prucalopride and 82 days for PEG. The pooled standardized incidence rate per 1000 person-years (95% confidence interval) of major adverse cardiovascular events was 6.57 (3.90–10.39) for patients initiating prucalopride and 10.24 (6.97–14.13) for PEG. The pooled adjusted incidence rate ratio for major adverse cardiovascular events was 0.64 (95% confidence interval 0.36–1.14). Results remained consistent in various sensitivity analyses.
Conclusions
The pooled incidence rate ratio estimate was consistent with no indication of an increased risk above the pre-specified safety threshold of 3.00 for major adverse cardiovascular events in patients with chronic constipation using prucalopride as compared with PEG.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Among patients with chronic constipation using prucalopride or polyethylene glycol 3350, the pooled adjusted incidence rate ratio of major adverse cardiovascular events comparing new use of prucalopride with new use of polyethylene glycol 3350 was 0.64 (95% confidence interval 0.36–1.14). |
The upper limit of the 95% confidence interval for this estimate was below the pre-specified safety threshold of 3.00. |
These results were robust to the use of an alternative definition of the study endpoint and to bias analyses for hypothetical unmeasured confounders, as well as in most subgroup analyses. |
1 Introduction
Chronic constipation is a common and often debilitating medical problem, with an impact on quality of life [1, 2]. The 5-hydroxytryptamine (serotonin) receptor type 4 (5-HT4) receptor agonists have the potential to treat disorders of gastrointestinal motility, including delayed gastric emptying and colonic dysmotility [3]. The first-generation 5-HT4 receptor agonists cisapride and tegaserod were withdrawn from the US market because of serious concerns about associated cardiovascular risk, arrythmias thought to be associated with QTc prolongation with cisapride, and ischemic events of uncertain origin with tegaserod [4].
Prucalopride, a selective 5-HT4 agonist with high affinity and selectivity for the 5-HT4 receptors [5], has been licensed in the European Union since 2009 for adult women and since 2015 for adult men for the treatment of chronic constipation and is currently approved in 82 countries [6, 7]. No signal for an increased risk of adverse cardiovascular events or QTc prolongation has been observed for prucalopride during non-clinical and clinical cardiovascular investigations or as a result of safety monitoring [5]. Nevertheless, given the prior serious concern experienced with other 5-HT4 receptor agonists, the US Food and Drug Administration (FDA) requested additional information about cardiovascular safety outcomes in the new drug application submitted for prucalopride [5].
The primary objective of this study was to estimate, in real-world usual care settings, the adjusted incidence rate ratio (IRR) and 95% confidence interval (CI) for major adverse cardiovascular events (MACE) in initiators of prucalopride compared with initiators of polyethylene glycol 3350 (PEG), two treatments indicated for chronic constipation. We defined MACE as the composite of hospitalization for non-fatal acute myocardial infarction, hospitalization for non-fatal stroke, and in-hospital cardiovascular death. For the adjusted IRR of MACE among prucalopride initiators relative to PEG initiators, the pre-specified safety threshold was defined as having an upper bound of the two-sided 95% CI of less than 3.00. Secondary objectives were to estimate the incidence rates for MACE and its individual components in the prucalopride and PEG cohorts, and to estimate their adjusted IRRs comparing prucalopride and PEG. This article focuses on the results of the primary and secondary study outcomes; the study design, general methods, and a detailed description of the study cohorts are presented in Fortuny et al. [8].
2 Methods
2.1 Study Design
This was an observational population-based cohort study of patients initiating prucalopride or PEG from five data sources across Germany, Sweden, and the UK (including England, Wales, Scotland, and Northern Ireland) following a common protocol (EUPAS9200) [9]. Data from Germany were excluded from the pooled analyses because the patient population was markedly different compared with the other countries in terms of comorbidities, likely owing to differences in prescribing and reimbursement practices for laxatives in Germany as compared with the other countries, as well as specifically between prucalopride and PEG within Germany [8].
2.2 Setting
The study was originally conducted in five administrative healthcare databases across Germany, Sweden, and the UK. In the UK, two data sources derived from electronic medical records from general practices—the Clinical Practice Research Datalink (CPRD) and The Health Improvement Network (THIN)—and the Information Services Division (ISD) of Scotland, an administrative healthcare data source, were used. In Sweden, data from the Swedish National Registers (SNR) were used, including health data from the National Patient Register, the Prescribed Drug Register, the Swedish Cancer Register, the Causes of Death Register, and information from the Total Population Register. In Germany, the German Pharmacoepidemiological Research Database, a claims database of four statutory healthcare insurance providers, was used. Based on the results of an interim analysis assessing the characteristics of the study cohorts [8], the final pooled analysis presented in this article combined the three databases from the UK and the SNR; data from Germany were not included because of marked differences between prucalopride and PEG initiators, as well as differences in both cohorts compared with the data sources in the UK and Sweden. Patients and practices that overlapped in the UK data sources were retained in only one data source (see Electronic Supplementary Material 1 of Fortuny et al. [8] for more details on each data source).
2.3 Population
Details regarding the inclusion and exclusion criteria are presented elsewhere by Fortuny et al. [8]. The prucalopride cohort consisted of adult patients who had a dispensing (for claims data sources and the Prescribed Drug Register in Sweden) or prescription (as recorded in electronic medical record data sources) for prucalopride within the study period with at least 12 months of data coverage in the data source before this first dispensing or prescription, no evidence in the data source of prior use of prucalopride, and no evidence of short use of PEG (i.e., < 5 days) within 12 months before this first prucalopride prescription/dispensing. The first prescription of prucalopride was the index prescription, which determined the index date.
The PEG cohort consisted of patients who had a dispensing or prescription for PEG of at least 5 days within the study period, who had at least 12 months of data coverage in the data source before this first dispensing or prescription, and who had no evidence of prior use of PEG for chronic constipation in the data source. The first prescription for PEG was the index prescription, prescribed or dispensed on the index date. Up to five PEG initiators were selected for each prucalopride initiator, matched by age, sex, and calendar year of first prescription of prucalopride or PEG. (The SNR also matched patients by recent hospitalization and specialty of the prescribing physician to increase comparability between PEG and prucalopride initiators.) At the time of study initiation, PEG was the most commonly prescribed reimbursable medication for chronic constipation in Europe. Individuals who switched from PEG to prucalopride entered the prucalopride cohort. Individuals who switched from prucalopride to PEG were eligible for the PEG cohort.
2.4 Variables
2.4.1 Exposure
Prucalopride or PEG exposure was ascertained from general practitioner prescriptions in the CPRD and THIN data and by outpatient dispensings in the ISD and SNR data. A patient was considered exposed to a study drug if he/she met all inclusion and exclusion criteria and had at least 1 day of exposure to that study drug alone (i.e., not the whole time at risk on overlap exposure time).
A treatment episode was defined as consecutive prescriptions of the index medication separated by gaps of 7 days or less, including a 7-day extension period after the drug was discontinued. Overlapping time of two prescriptions of the same drug was counted only once in the three data sources from the UK, while stockpiling was used in Sweden and Germany. Identification of drug use was carried out using the conventional drug coding schemes at each data source. All prucalopride use within the study period was accounted for as exposed time (i.e., regardless of the duration of the prescription/dispensing). Short episodes of PEG (lasting < 12 days) during follow-up were considered proxies of indications other than chronic constipation (e.g., acute constipation or preparation for a colonoscopy) and were ignored, as the comparison cohort was intended to have chronic constipation and PEG is assumed to be neutral in terms of the risk of MACE (see Fig. 1).
Inclusion of polyethylene glycol 335 (PEG) initiators regarding duration of the first episode. If a potential new initiator of PEG had an episode of prior use of PEG lasting less than 12 days that included the date that marked the beginning of the 12-month period before the index date (i.e., 12-month cut-off date, for short), the patient was excluded, as per general exclusion criteria, because a colonoscopy (or other non-chronic constipation indication of PEG) could have taken place at the end of the short episode of use, that is, during the 12-month period before the index date. RX prescription/dispensing
2.4.2 Follow-Up
For the primary analysis, time at risk from current use for prucalopride initiators and PEG initiators started on the day of index prescription. Time at risk from current use was cumulative across all episodes of current use (as described above) of the index medication, not including gaps. Accrual of time at risk of current use for a study medication was terminated if there was a prescription or dispensing for the other study medication. Time at risk did not accrue beyond 7 days after the end of the last prescription/dispensing for the index medication, date of death, date of first occurrence of the endpoint under evaluation during the time at risk, termination of enrolment in the health plan or system, or end of the study period.
2.4.3 Outcomes
The main composite cardiovascular endpoint of interest for this study was based on the classical MACE endpoint ascertained in randomized clinical studies. Definition of this endpoint followed FDA recommendations for clinical studies summarized in the Standardized Definitions for Endpoint Events in Cardiovascular Trials [10] but was adapted to the observational setting and the availability of information in each data source selected for study implementation, following harmonization criteria to achieve similarity across databases. This composite cardiovascular endpoint included hospitalization for non-fatal acute myocardial infarction, hospitalization for non-fatal stroke, and in-hospital cardiovascular death. Individual components of this endpoint were also evaluated separately for the secondary objectives. For any individual who experienced more than one cardiovascular endpoint (e.g., stroke and myocardial infarction), both endpoints would count in the individual component analyses. The individual components of MACE were considered secondary endpoints.
Because of the anticipated lack of information on causes of out-of-hospital death and the lack of information on outpatient diagnoses in some of the selected data sources, the MACE endpoint for the main analyses included in-hospital but not out-of-hospital cardiovascular deaths. This approach followed the FDA recommendations for consistent classification (i.e., the ascertainment of homogeneous events across all selected data sources is preferable to defining endpoints based on the maximum available information in each data source).
A sensitivity analysis included a composite endpoint comprising MACE plus out-of-hospital cardiovascular deaths. For the sensitivity analysis that included out-of-hospital cardiovascular deaths as part of the composite MACE study endpoint, out-of-hospital cardiovascular death was defined as a death occurring out of a hospital setting and with evidence of a coronary heart disease, sudden cardiac death, or cerebrovascular cause.
In all data sources, potential study endpoints were identified by electronic algorithms that used operational definitions and lists of diagnostic and procedural codes (using International Classification of Diseases codes and/or local dictionaries). Potential study endpoints from the UK data sources were validated per a common validation plan, which included (1) direct confirmation via linkage to hospital records (CPRD only); (2) requests for additional clinical information through questionnaires (CPRD), free-text comments (THIN), or original hospital case records (ISD); (3) patient profile review by study investigators (CPRD/THIN) to rule out non-cases; and (4) independent review by two clinicians, blinded to exposure. If there were discrepancies in the decision between the two reviewers, the full committee (all three clinicians, blinded to exposure) met to review the case and come to consensus. Cases were assigned final status of definite, probable, possible, or non-cases. Cases included in Sweden were identified using modifications of electronic algorithms previously validated in the Swedish registers and were not further validated. No validation occurred for cases identified in Germany.
2.4.4 Covariates
Cardiovascular risk factors, including previous history of cardiovascular disease, history of diabetes mellitus, hypertension, dyslipidemia, body mass index (BMI) (or obesity) in CPRD, THIN, and SNR, and history of smoking and alcohol use in CPRD and THIN, as well as other covariates related to gastrointestinal diseases, were identified from the available healthcare utilization codes before the index date. Table 1 lists the cardiovascular risk factors evaluated.
2.5 Study Size
To estimate the expected statistical power for the final study analysis, we used an expected incidence for MACE of 2 per 1000 person-years. The study size was driven by the number of prucalopride initiators and associated duration of exposure that was available in the selected data sources during the study period. The number of prucalopride initiators was based on an average current-use follow-up time for prucalopride initiators of 130 days. Calculations were made using the formulas in Episheet [11]. The pre-specified safety threshold was defined as having an upper bound of the two-sided 95% CI for the adjusted IRR of MACE comparing prucalopride to PEG initiators of < 3.00. A cohort size of 10,950 prucalopride initiators was initially targeted to provide 80% power to reject the hypothesis that the risk ratio (RR) is > 3.0 assuming that the true RR is actually 1.0. With these assumptions, a total of 47 patients were expected to experience MACE in this study.
2.6 Statistical Analyses
The incidence rate of MACE for prucalopride and PEG initiators and the adjusted IRRs and incidence rate differences (IRDs) of MACE comparing prucalopride to PEG use were calculated individually for each data source and after pooling the aggregated results from UK and Sweden. Crude and adjusted incidence rates of each outcome of interest were calculated for the prucalopride and PEG cohorts by categories of each covariate of interest, and corresponding crude and standardized IRRs and IRDs were estimated. Adjusted IRRs and IRDs were calculated using standardization by the deciles of the propensity score (PS), derived as explained in Fortuny et al. [8]. Pooled analyses of aggregate data were conducted by the coordinating center (RTI Health Solutions) and involved standardization of the source-specific PS deciles and data source as stratification variables.
2.6.1 Crude Estimates
Person-time at risk, number of events, and crude incidence rates with the corresponding lower bound and upper bounds of the exact 95% CI were computed using methods described in Dobson et al. [12] for each endpoint overall and stratified individually by each covariate of interest for each cohort within each data source. Crude IRRs were estimated with corresponding exact lower bound and upper bound of the 95% CIs calculated using a Poisson distribution and test-based methods defined in Sahai and Khurshid [13]. The crude IRDs with approximate 95% CIs [14] were estimated.
2.6.2 Standardized Estimates
Within each data source, the incidence rate, IRR, and their 95% CIs were standardized by age, sex, and risk factors. Within each data source, PSs were developed using logistic regression with prucalopride vs. PEG as the outcome and included variables shown to be potential confounders for the relationship of the study drugs with MACE, including cardiovascular risk factors [8]. Within each data source, incidence rates, IRRs, and IRDs were standardized against person-years in the prucalopride cohort and stratified by data source and PS decile.
The standardized incidence rate (SIR) and exact 95% CIs were calculated based on exact methods presented in Dobson et al. [12]. The standardized IRRs (SIRRs) with the 95% CIs were calculated using a normal approximation as described in Rothman et al. [14]. The standardized IRD with 95% CI was calculated as shown in Rothman et al. [14].
2.6.3 Pooled Analyses of Aggregate Data
For the pooled results of aggregate data from each included data source, the incidence rate, IRR, and IRD were standardized to the distribution of person-years among each data source-specific PS decile in the prucalopride group. For each of the endpoints of interest, the results were generated and combined across data sources. Specifically, number of patients, patients with study endpoints, and person-years were added across data sources. Incidence rates and 95% CIs standardized for data source and PS decile within each of the cohorts were calculated. Incidence rate ratios and IRDs per 1000 person-years and their 95% CIs for the prucalopride cohort compared with the PEG cohort, standardized for data source and PS decile, were calculated as in Rothman et al. [14]. The data source was retained as a stratification variable, and the effect within each PS category within each database was estimated.
2.6.4 Missing Values
The frequency of missing information was shown in the descriptive analyses. When presenting results stratified on a single variable, subjects missing information for that variable were reported in a separate category.
2.6.5 Sensitivity Analyses
Sensitivity analyses explored the impact of exposure definition (including the impacts of extending risk to 30 days, evaluating the first episode of use only, including past use, and removing periods of time hospitalized), the impact of outcome categories (including considering probable cases and adding out-of-hospital coronary heart disease and cerebrovascular death to the MACE endpoint), the impact of cancer, and the potential for channeling bias. The impact of unmeasured confounding was assessed by the bias analysis proposed by Lash et al. [15]; this analysis required an a priori specification of the prevalence of the unmeasured confounder in the prucalopride and PEG initiators, respectively, and of the effect of the unmeasured confounder on the outcome. Finally, post hoc subgroup analyses by sex, age, sex by age, and history of cardiovascular disease were conducted for the primary pooled analysis.
2.7 Research Ethics
All relevant authorities reviewed and approved the study on ethical grounds in the UK (Independent Scientific Advisory Committee for CPRD, Scientific Review Committee for THIN, and East of Scotland Research Ethics Services/Public Benefit and Privacy Panel for Health and Social Care for ISD), Germany (all involved health insurance providers, as well as the German Federal [Social] Insurance Office and the Senator for Science, Health, and Consumer Protection in Bremen), and Sweden (Regional Ethical Review Board, Stockholm).
3 Results
3.1 Study Population
The pooled analyses of aggregate data included 5715 patients treated with prucalopride and 29,372 patients treated with PEG, including 866 prucalopride patients and 4254 matched PEG patients (1:5 ratio) from the CPRD, 501 prucalopride patients and 2543 PEG patients from THIN, 1154 prucalopride patients and 5806 PEG patients from the ISD, and 3194 prucalopride patients and 16,769 PEG patients from the SNR. The average durations of cumulative prucalopride use and cumulative PEG use after the index date were approximately 175 days and 82 days, respectively.
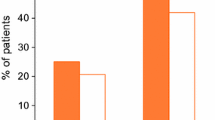
In the final pooled trimmed data, the vast majority of participants were women (93%), and the proportion of patients aged 55 years was 43% for prucalopride and 42% for PEG (Table 2). In general, prucalopride and PEG patients had similar baseline comorbidities, although prucalopride patients had more baseline gastrointestinal comorbidities (Table 3). However, after adjusting for the shorter duration of use in PEG patients compared with prucalopride patients and based on person-years at risk, PEG patients tended to have a higher proportion of comorbidities, including prior hospitalization for cardiovascular disease, presence of at least one cardiovascular risk factor, and cancer in all data sources (data not shown). Additional details regarding baseline comorbidities can be found in Fortuny et al. [8].
3.2 Incidence Rates, Incidence Rate Ratios, and Incidence Rate Differences of Major Adverse Cardiovascular Events in Prucalopride and Polyethylene Glycol 3350 Initiators
In the primary analysis, the pooled PS SIR (95% CI) for the UK and SNR data sources of MACE among patients initiating prucalopride per 1000 person-years was 6.57 (3.90–10.39) and among patients initiating PEG was 10.24 (6.97–14.13) (Table 4). The overall pooled adjusted IRR was 0.64 (95% CI 0.36–1.14). The pooled adjusted IRD for MACE combining the three UK data sources and the SNR was − 3.66 per 1000 person-years (95% CI − 8.27 to 0.95). The upper limit of the 95% CI of the pooled adjusted IRR was below the pre-specified safety threshold of 3.00.
3.3 Secondary Endpoints
In the secondary analyses, the pooled adjusted IRRs for individual components of MACE were 0.95 (95% CI 0.38–2.39) for hospitalization for non-fatal acute myocardial infarction, 0.54 (95% CI 0.23–1.29) for hospitalization for non-fatal stroke, and 0.47 (95% CI 0.13–1.67) for in-hospital cardiovascular death.
3.4 Sensitivity Analyses
Sensitivity analyses revealed the pooled adjusted IRR and IRD results to be generally robust to the alternative definitions of exposure and outcome categories, to the impact of cancer, and to bias analyses that considered the hypothetical impact of unmeasured confounding in different scenarios of confounder prevalence and associations with the outcomes. Specifically, the analyses of first episode of use only, extension to 30 days of risk, and past use yielded similar pooled adjusted IRRs (0.69 [95% CI 0.34–1.42], 0.65 [95% CI 0.38–1.09], and 0.65 [95% CI 0.45–0.92], respectively) to that from the main analysis (0.64 [95% CI 0.36–1.14]) (Table 5). The analysis including out-of-hospital cardiovascular deaths in the MACE definition yielded a pooled adjusted IRR (0.43 [95% CI 0.25–0.73]), lower than that of the main analysis, whereas the pooled adjusted IRR when probable cases were included was higher than in the main analysis: 0.75 (95% CI 0.27–2.05).
In the analysis evaluating the potential impact of a hypothetical unmeasured confounding factor on the overall IRR for each data source, a range of hypothetical values for the prevalence of an unknown confounder among the two cohorts and for the IRR of the unknown confounder and the outcome of interest was used to assess the hypothetical potential impact of an unknown confounder on the overall IRR for each individual data source. The bias analyses showed that adjustment for hypothetical additional confounding factors under various assumptions did not change the direction of the associations observed in the main analyses, even in unlikely scenarios of an extremely different prevalence of the unmeasured confounder between the two exposure groups (e.g., over 70% in one group and nearly absent in the other group) and of a strong association with the MACE outcome.
3.5 Subgroup Analyses
In all subgroup analyses, the 95% CIs for the pooled adjusted IRR were wide and included the null value. In general, all post hoc subgroup analyses were consistent with the overall results, except in the subgroup of men older than 55 years of age, where a pooled adjusted IRR of 2.57 (95% CI 0.71–9.26) was observed (Fig. 2).
Pooled adjusted incidence rate ratio (IRR) [95% confidence interval (CI)] by sex, age, sex-age strata, and by history of cardiovascular (CV) disease at baseline. The IRR was standardized against the person-years in the prucalopride cohort. Calendar Period #1 corresponds to 2010–2012, and Calendar Period #2 corresponds to 2013–2016 for the three UK databases and 2013–2014 for the German Pharmacoepidemiological Research Database. For the Swedish National Registers, Calendar Period #1 corresponds to year 2012 and Calendar Period #2 corresponds to 2013–2015. aHospitalization for CV disease = history of hospitalization for acute myocardial infarction, stroke, transient ischemic attack, ischemic heart disease, or peripheral vascular disease. bHistory of CV disease = history of acute myocardial infarction, stroke, hypertension, smoking, hyperlipidemia, diabetes mellitus, aged more than 55 years, or a body mass index greater than 30 kg/m2. PEG polyethylene glycol
3.6 Results in Germany
Although Germany was not included in the pooled main analyses, results for the primary study endpoint are presented for transparency. In the German Pharmacoepidemiological Research Database, 30,714 prucalopride and matched PEG initiators were identified after trimming (88% female patients and 66% of patients aged 55 years and older). In general, the proportion of history of comorbid conditions at baseline was lower in prucalopride patients than in PEG patients. The PS deciles SIR of MACE per 1000 person-years was 11.05 (95% CI 8.03–14.69) for prucalopride and 21.53 (95% CI 18.52–24.78) for PEG. The adjusted IRR for MACE was 0.51 (95% CI 0.37–0.71), and the adjusted IRD for MACE was −10.48 (95% CI − 14.99 to − 5.98).
4 Discussion
This study aimed to investigate whether there was evidence of an increased risk of cardiovascular events in patients treated with prucalopride compared with patients treated with PEG. The estimated IRR was 0.64 (95% CI 0.36–1.14), with a 95% CI that included the null value and an upper limit below 3.00, the pre-specified safety threshold. In the post hoc subgroup analysis for men over the age of 55 years, a pooled adjusted IRR of 2.57 (95% CI 0.71–9.26) was observed, based on four cases exposed to prucalopride and 11 cases exposed to PEG. This observation should be interpreted with caution given the small size of this subgroup analysis (as expected, given prucalopride is mostly used in women). In sensitivity analyses conducted to explore the impact of alternative definitions of exposure, outcome categories, and of cancer, the results were consistent with those from the main pooled analysis. The main results were also robust to potential unmeasured confounders.
4.1 Interpretation
The first-generation 5-HT4 receptor agonists cisapride and tegaserod were withdrawn from the US market because of concerns about their associations with cardiovascular risks. In comparison, prucalopride is a more selective 5-HT4 agonist showing greater differential affinity and selectivity for the 5-HT4 receptors, with low affinity for other receptors [5]. We did not detect an increase in cardiovascular risk in patients treated with prucalopride in this study. Prior non-clinical studies, clinical trials, and safety extension studies have found no evidence of increased cardiovascular risk with prucalopride [5].
Some differences in prucalopride usage patterns were noted in this study. Although the proportion of patients aged 55 years and older was similar across the UK data sources (34% in the CPRD, 31% in THIN, and 21% in ISD), the proportion of such patients was higher in Sweden (53%). Moreover, the usage differences in Germany precluded pooling with the other data sources. In this context, the incidence rates in this study were higher than anticipated, driven primarily by an older population in Sweden. Importantly, the FDA accepted evidence from this study in place of a cardiovascular outcomes trial for the prucalopride new drug application in the USA [5].
4.2 Study Limitations
Some limitations of this study must be acknowledged. First, determining exposure duration accurately is challenging when using secondary healthcare data, and exposure misclassification in this study was possible. Additionally, although the results are subject to confounding (as with effect estimates derived from healthcare database studies), confounding by the main variables related to cardiovascular risk was controlled through matching during specification of the PEG cohort and the use of exposure PSs in the analyses. The SNR did not have information on BMI or smoking or alcohol use, all important risk factors for MACE. However, the bias analysis showed that unreasonable scenarios of confounder association with exposure and outcome should occur to change the direction of the association detected.
No direct measure of patient adherence was available, and it was assumed that patients were administered the product as prescribed or dispensed. Efforts were made to harmonize the definitions of exposure periods and key study variables, including endpoints and key covariates, across data sources using a common protocol. Still, nuances were allowed for endpoint definitions, such as the definition of sudden cardiac death in the SNR, to adapt the core definitions to the local coding practices and thus avoid outcome misclassification. Similarly, minor adaptations were also allowed for some covariates included in the analyses.
The primary objective was aimed at examining the risk of cardiovascular events in the overall population of patients taking prucalopride compared with PEG and was not designed to examine risk in subgroups. Although older men had an IRR of 2.57, the confidence interval was wide and based on a low number of events. Older men are at a higher risk for cardiovascular events than younger men or women. When examining patients who had at least one risk factor for a cardiovascular event or had been hospitalized, there was no indication of an increased risk in patients taking prucalopride compared with PEG.
Note that arrhythmias and symptomatic palpitations were not the subject of the present study, as observational studies are not well suited to capture such outcomes. However, previous studies have not shown an effect of prucalopride on QT prolongation [5]. Instead, the present study focused on the putative objective adverse cardiovascular outcomes of prucalopride exposure, as these outcomes are the important potential toxicities of concern. Finally, the German data from the German Pharmacoepidemiological Research Database could not be used as originally planned because of unadjustable differences in the patient profiles between PEG and prucalopride patients and different baseline characteristics of the population compared with other data sources.
Polyethylene glycol 3350 was selected as a comparator because of its extensive use in chronic constipation and its presumed lack of any cardiovascular effect. The fact that we observed a slightly higher incidence of MACE events in PEG patients most likely reflects the unexpectedly higher baseline cardiovascular risk in the PEG population after adjusting for duration of use that could not be completely controlled through our analytic methods.
5 Conclusion
In this study of patients with chronic constipation using prucalopride or PEG (> 90% women), the pooled adjusted IRR of MACE comparing new use of prucalopride with new use of PEG was 0.64 (95% CI 0.36–1.14). Of note, the upper limit of the 95% CI for this estimate was below the pre-specified threshold of 3, which was the threshold set by regulatory authorities to define safety in this study. These results were robust to the use of an alternative definition of the study endpoint (i.e., including out-of-hospital cardiovascular death), as well as to bias analyses for hypothetical unmeasured confounders. Results were also consistent in post-hoc subgroup analyses, except for the small subgroup of men older than 55 years of age where additional analyses are warranted.
References
Dennison C, Prasad M, Lloyd A, Bhattacharyya SK, Dhawan R, Coyne K. The health-related quality of life and economic burden of constipation. Pharmacoeconomics. 2005;23(5):461–76.
Wald A, Scarpignato C, Kamm MA, Mueller-Lissner S, Helfrich I, Schuijt C, et al. The burden of constipation on quality of life: results of a multinational survey. Aliment Pharmacol Ther. 2007;26(2):227–36.
Gershon MD, Tack J. The serotonin signaling system: from basic understanding to drug development for functional GI disorders. Gastroenterology. 2007;132(1):397–414.
Tack J, Camilleri M, Chang L, Chey WD, Galligan JJ, Lacy BE, et al. Systematic review: cardiovascular safety profile of 5-HT(4) agonists developed for gastrointestinal disorders. Aliment Pharmacol Ther. 2012;35(7):745–67.
FDA. FDA briefing document, New Drug Application 210166 for prucalopride: Gastrointestinal Drug Advisory Committee meeting. 18 October 2018. Available from: https://www.fda.gov/downloads/AdvisoryCommittees/CommitteesMeetingMaterials/Drugs/GastrointestinalDrugsAdvisoryCommittee/UCM623493.pdf. Accessed 26 Oct 2018.
EMA. Assessment report: Resolor (prucalopride). European Medicines Agency; April 23, 2015. Available from: http://www.ema.europa.eu/docs/en_GB/document_library/EPAR_-_Assessment_Report_-_Variation/human/001012/WC500190380.pdf. Accessed 8 May 2018.
EMA. Resolor (prucalopride). European Medicines Agency; November 1, 2016. Available from: http://www.ema.europa.eu/ema/index.jsp?curl=pages/medicines/human/medicines/001012/human_med_001030.jsp&mid=WC0b01ac058001d124. Accessed 3 Nov 2017.
Fortuny J, Gilsenan A, Cainzos-Achirica M, Cantero AF, Flynn RWV, Garcia-Rodriguez L, et al. Study design and cohort comparability in a study of major cardiovascular events in new users of prucalopride versus polyethylene glycol 3350. Drug Saf. 2019. https://doi.org/10.1007/s40264-019-00836-z.
ENCePP. Cohort study of the relative incidence of major cardiovascular events among patients initiating prucalopride versus a matched comparator cohort (EUPAS9200). European Network of Centres for Pharmacoepidemiology and Pharmacovigilance; July 2018. Available from: http://www.encepp.eu/encepp/viewResource.htm?id=22643. Accessed 18 Dec 2018.
Hicks KA, Hung HMJ, Mahaffey KW, Mehran R, Nissen SE, Stockbridge NL, et al. Standardized definitions for cardiovascular and stroke endpoint events in clinical trials. Clinical Data Interchange Standards Consortium (Standardized Data Collection for Cardiovascular Trials Initiative); August 20, 2014. Available from: https://www.cdisc.org/system/files/all/standard/Draft%20Definitions%20for%20CDISC%20August%2020%2C%202014.pdf. Accessed 3 Nov 2017.
Rothman KJ. Episheet: spreadsheets for the analysis of epidemiologic data. October 4, 2012. Available from: http://krothman.hostbyet2.com/Episheet.xls. Accessed 19 Dec 2018.
Dobson AJ, Kuulasmaa K, Eberle E, Scherer J. Confidence intervals for weighted sums of Poisson parameters. Stat Med. 1991;10(3):457–62.
Sahai H, Khurshid A. Statistics and epidemiology: methods, techniques, and applications. Boca Raton: CRC Press LLC; 1996.
Rothman KJ, Greenland S, Lash TL, editors. Modern epidemiology. 3rd ed. Philadelphia: Lippincott Williams & Wilkins; 2008.
Lash T, Fox MP, Fink AK. Applying quantitative bias analysis to epidemiologic data. New York: Springer Science + Business Media, LLC; 2009.
Acknowledgements
The authors thank Antonio Gonzalez (CEIFE), who contributed to the statistical analyses of THIN data and report preparation, and Jennifer Bartsch (RTI-HS), who contributed to the statistical programming for the CPRD data. The authors are also grateful for input on the design from Patricia Tennis, Kenneth Rothman, and Eileen Ming. Helle Kieler contributed to the study as a primary investigator in Sweden. Alison McGinnis, a research nurse, toured Scottish hospitals to gather original hospital case records for the purposes of endpoint adjudication. Amy Rogers and Kerr Grieve provided assistance with event validation. Kate Lothman of RTI Health Solutions provided medical writing services, which were funded by Shire Pharmaceuticals, now part of the Takeda group of companies. This study is based in part on data from the CPRD obtained under license from the UK Medicines and Healthcare products Regulatory Agency. The data are provided by patients and collected by the National Health Service as part of their care and support. The interpretation and conclusions contained in this study are those of the authors alone. We thank the statutory health insurance providers in Germany, AOK Bremen/Bremerhaven, DAK-Gesundheit, and Die Techniker (TK), for contributing the data for this analysis. We acknowledge the Electronic Data Research and Innovation Service (eDRIS) of ISD Scotland for providing the ISD data. We also acknowledge Quintiles IMS (now IQVIA) for providing access to THIN data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was performed under a research contract between RTI Health Solutions and Shire Pharmaceuticals, now part of the Takeda group of companies, and was funded by Shire. The research contract granted independent publication rights to the research team, and the content of the publications was developed independently from the study sponsor.
Conflict of interest
Alicia Gilsenan, Abenah Harding, Joan Fortuny, Estel Plana, Ryan Ziemiecki, and Elizabeth B. Andrews are salaried employees of RTI Health Solutions. Miguel Cainzos-Achirica was a salaried employee of RTI Health Solutions when this research was conducted and is currently affiliated with the Hospital Universitari de Bellvitge Department of Cardiology, Feixa Llarga, Hospitalet de Llobregat, Barcelona, Spain. Luis-Alberto Garcia-Rodriguez, Oscar F. Cantero, and Ana Ruigómez are employed at the Spanish Centre for Pharmacoepidemiologic Research (CEIFE Madrid, Spain), which has received research funding from RTI Health Solutions. Robert W.V. Flynn is an employee of the University of Dundee and has received research grants from Novartis and GlaxoSmithKline. Thomas M. MacDonald is an employee of the University of Dundee, an academic organization that received financial support under the research contract between RTI Health Solutions and Shire, now part of the Takeda group of companies, to carry out the study. Thomas M. MacDonald is also the director of MEMO Research at the University of Dundee, an organization that has received research funding from Pfizer, Novartis, Amgen, Ipsen, GlaxoSmithKline, Teijin, and Menarini, mostly for post-licensing studies requested by regulatory authorities, and has personally received honoraria from for educational lectures from Takeda. He has been the principal investigator on trials paid for by Pfizer, Novartis, Ipsen, Teijin, GlaxoSmithKline, and Menarini (mostly post-licensing regulatory requested studies). In the last 3 years, he has been paid consulting fees by Novartis. Pär Karlsson, Love Linnér, and Ingvild Odsbu are employed at the Centre for Pharmacoepidemiology, Karolinska Institutet, which receives grants from several entities (pharmaceutical companies, regulatory authorities and contract research organizations) for the performance of drug safety and drug utilization studies. Miguel Cainzos-Achirica has participated in a research study funded by a non-conditioned research grant from Vifor. Tania Schink and Bianca Kollhorst are working at an independent non-profit research institute, the Leibniz Institute for Prevention Research and Epidemiology – BIPS. Unrelated to this study, BIPS occasionally conducts studies financed by the pharmaceutical industry. Almost exclusively, these are post-authorization safety studies requested by health authorities. The design and conduct of these studies as well as the interpretation and publication are not influenced by the pharmaceutical industry.
Ethics approval
All relevant authorities reviewed and approved the study on ethical grounds in the UK, Germany, and Sweden. The data used in this study were obtained from databases of anonymized medical and pharmacy records and not directly from human subjects.
Consent to participate
Not applicable.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Gilsenan, A., Fortuny, J., Cainzos-Achirica, M. et al. Cardiovascular Safety of Prucalopride in Patients with Chronic Constipation: A Multinational Population-Based Cohort Study. Drug Saf 42, 1179–1190 (2019). https://doi.org/10.1007/s40264-019-00835-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40264-019-00835-0