Abstract
Background and objective
This study proposes a model-informed approach for therapeutic drug monitoring (TDM) of rifampicin to improve tuberculosis (TB) treatment.
Methods
Two datasets from pulmonary TB patients were used: a pharmacokinetic study (34 patients, 373 samples), and TDM data (96 patients, 391 samples) collected at Radboud University Medical Center, The Netherlands. Nine suitable population pharmacokinetic models of rifampicin were identified in the literature and evaluated on the datasets. A model developed by Svensson et al. was found to be the most suitable based on graphical goodness of fit, residual diagnostics, and predictive performance. Prediction of individual area under the concentration–time curve from time zero to 24 h (AUC24) and maximum concentration (Cmax) employing various sampling strategies was compared with a previously established linear regression TDM strategy, using sampling at 2, 4, and 6 h, in terms of bias and precision (mean error [ME] and root mean square error [RMSE]).
Results
A sampling strategy using 2- and 4-h blood collection was selected to be the most suitable. The bias and precision of the two strategies were comparable, except that the linear regression strategy was more biased in prediction of the AUC24 than the model-informed approach (ME of 9.9% and 1.5%, respectively). A comparison of resulting dose advice, using predictions on a simulated dataset, showed no significant difference in sensitivity or specificity between the two methods. The model was successfully implemented in the InsightRX precision dosing platform.
Conclusion
Blood sampling at 2 and 4 h, combined with model-based prediction, can be used instead of the currently used linear regression strategy, shortening the sampling by 2 h and one sampling point without performance loss while simultaneously offering flexibility in sampling times.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
We propose a new model-informed therapeutic drug monitoring method for rifampicin. |
The proposed method uses only two blood samples at 2 and 4 h after dosing. |
In contrast to linear regression-based methods, the proposed method allows for flexible sampling times and prediction of optimal dose adjustment. |
1 Introduction
In 2016, the global incidence of tuberculosis (TB) was estimated at 10.4 million and it remains one of the most common causes of death worldwide, with approximately 1.7 million fatalities annually [1]. The treatment success rate for new and recurrent TB cases was estimated at 83% globally in 2015. A substantial portion of patients fail to respond to treatment, have a relapse of disease, or develop drug-resistant TB [1].
There are multiple reasons for suboptimal treatment response, one of which is low plasma concentrations of TB drugs [2, 3]. Low drug exposures can result from a variety of reasons, e.g. malabsorption caused by HIV co-infection, diabetes mellitus as a concomitant disease, or other unexplained interindividual variability in pharmacokinetics (PK) [4,5,6,7].
Therapeutic drug monitoring (TDM) is a tool to avoid suboptimal treatment by measuring an individual’s drug exposure, comparing the result with a drug-specific target level and adjusting the patient’s dose accordingly. The application of TDM and its benefits in TB clinical practice have previously been described [2]. As it is not practically feasible or desirable, from a patient perspective, to sample intensively to obtain a full PK curve, the estimation of exposure is often based on one or a few samples using a limited sampling strategy (LSS). The benefits of LSSs are apparent, including reduced inconvenience and possibly a shorter stay at a hospital facility for patients, as well as less labour and costs for the healthcare system. Traditionally, limited sampling of TB drugs was aimed at ‘catching’ and estimating the peak plasma concentration of TB drugs in an individual by sampling at 2 and 6 h after dosing, as described by Alsultan and Peloquin, and as applied by others [2, 5]. However, evolving data suggest that the total exposure (area under the concentration-time curve from time zero to 24 h [AUC24]) is more relevant to the efficacy of first-line TB drugs. Recently developed LSSs aim to predict the AUC24 for TB drugs [2, 3, 8,9,10].
Rifampicin is a pillar of current first-line TB treatment and is part of the World Health Organization’s List of Essential Medicines. Two of three identified proposed LSSs for rifampicin [9, 11] were established using linear regression that requires three plasma concentration measurements to calculate the total exposure. The LSS by Magis-Escurra et al. is currently used in Radboud University Medical Center (Radboudumc), The Netherlands, and utilises three plasma samples—2, 4, and 6 h after dosing [9]. A linear regression formula is used to estimate the AUC24 and the highest measured concentration as an approximation of the maximum concentration (Cmax). However, this linear regression approach has some limitations. For adequate predictions, the formulas demand use of fixed sampling time points with accurate sample timing. Additionally, the formulas are limited to using only concentration measurements from the current TDM occasion, ignoring patient characteristics and potential information from previous sampling. Furthermore, it is not possible to predict the change in exposure that would occur from a change in dosing regimen. Lastly, all current LSSs for rifampicin [9,10,11] have been developed in populations receiving a standard dose of 10 mg/kg and are therefore expected to have difficulties predicting exposure after higher or increased dosages, given the known supra-proportional increase in exposure with increasing doses [12].
An alternative to using a linear regression strategy for calculation of individual drug exposure is the model-informed approach using a population PK model [13]. This approach for TDM combines population PK and individual TDM data to estimate individual PK parameters, and addresses all of the above limitations as it allows more flexible sampling, prediction of future drug concentrations, and incorporation of previous sampling occasions. Model-based estimations are expected to perform better than limited sampling formulas and could possibly decrease the number of blood samples needed [14]. The aim of the current work was to develop a user-friendly TDM application and LSS for the pivotal TB drug rifampicin using the model-informed approach.
2 Methods
We used a five-step approach to reach our objective:
-
Step 1: Data collection of PK data from clinical care (TDM) and a previously conducted study.
-
Step 2: Identification of models, i.e. identification of all currently known and potentially suitable rifampicin population PK models using a PubMed search.
-
Step 3: Selection of the most suitable model, i.e. evaluation of all identified rifampicin models using collected PK data.
-
Step 4: Development of an optimal sampling strategy, i.e. comparison of the predictive performance of the model-informed method with multiple potential sampling strategies, and comparison of the performance of an established linear regression formula with a three-sample LSS.
-
Step 5: Numerical verification, i.e. comparison of model predictions and parameters between the software used in steps 2 and 3 and the user-friendly InsightRX dose individualization platform in which we incorporated our selected model and LSS [15].
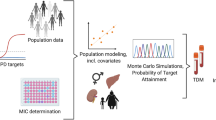
Figure 1 shows a schematic depiction of our approach. We used R version 3.2.4 [16] for data management, statistics, and graphical plotting. The models were analyzed using the nonlinear mixed-effects modelling software NONMEM version 7.3 [17], executed through the Pirana workbench [18]. Visual predictive checks (VPCs) and stochastic simulation and re-estimations (SSE) were performed using PsN version 4.7 [18]. Xpose4 [18] was used for graphical visualization of the VPCs in R.
Schematic representation of the study design. The coloured lines coming from the TDM and study data show the analyses for which these datasets are used. ME mean error, NONMEM nonlinear mixed effects modelling, NPDE normalized prediction distribution error, PK pharmacokinetic, RIF rifampicin, TDM therapeutic drug monitoring, RMSE root mean square error
2.1 Data (Step 1)
We extracted routine TDM data from the electronic patient record system at Radboudumc. Patient data were collected during routine care at the Department of Respiratory Diseases, Radboudumc–Dekkerswald, between 2007 and 2017. Following the local TDM protocol, rifampicin was administered in a fasted state, with sampling at 2, 4, and 6 h after dosing, at least 14 days after the start of rifampicin treatment [5, 9]. Some patients had several sampling occasions as the TDM procedure was sometimes repeated after dose adjustments. A second dataset included patients from Radboudumc and the University Medical Center Groningen, The Netherlands [9]. This study recorded full PK curves, with samples at 1, 1.5, 2, 2.5, 3, 4, 6, 8, 12 and 24 h after dosing.
Quantification of rifampicin in plasma was performed at Radboudumc using a chromatographic assay with ultraviolet detection, validated according to the most recent European Medicines Agency (EMA) guidelines for bioanalytical method validation [19]. The method has been previously described in depth [20]. In short, the intra- and interassay coefficients of variation were < 4% over the range of 0.28–30 mg/L. The lower limit of quantification was 0.28 mg/L.
Observations with unknown dose or dosing time were excluded. Data below the limit of quantification were replaced by half the lower limit of quantification (the ‘M5’ method, as defined by Beal [21]). Fat-free mass (FFM) was computed as described by Janmahasatian et al. [22]. If weight or FFM data were missing, we used the mean of the variable in the corresponding dataset. All data in this study were pseudonymised and the institutional Ethical Review Board approved a waiver for the requirement to obtain informed consent.
2.2 Identification of Models (Step 2)
A structural PubMed search was performed to identify rifampicin models (the search strategy is described in Online Resource 1), and the references in the selected publications were reviewed for any additional relevant studies. The selection of candidate models from the identified literature was based on the following five criteria: the paper should describe (1) a population PK model (2) of rifampicin (3) in adult humans. Furthermore, it should be (4) an original publication from which (5) the model with parameter values could be fully re-implemented.
2.3 Selection of the Most Suitable Model (Step 3)
The TDM and PK study datasets (step 1) were used independently to select the most suitable model. The datasets were used independently as they provided a better understanding of model performance on data of a specific nature. Selected models (step 2) were implemented in NONMEM for evaluation with the data. If a model had a variable enzyme induction component this was fixed at maximum induction since we could expect a state of full induction for all patients at the time of sampling.
Evaluation and selection of the most suitable model was based on model characteristics, graphical goodness of fit, residual diagnostics, and predictive performance. For the graphical goodness of fit, we visually inspected VPCs [23, 24], as well as individual predictions and/or time plotted against the measured rifampicin concentration, conditionally weighted residuals (CWRESs), and individual weighted residuals (IWRESs) [25]. These goodness-of-fit plots were used to evaluate the structural models and typical predictions of median and variability on the population level. Further residual diagnostic evaluation was performed using the normalized prediction distribution errors (NPDEs), calculated using 1000 simulated datasets [23, 26]. The NPDEs are normally distributed under the null hypothesis that the model adequately describes the dataset. As opposed to the VPC for model evaluation, this allows for a statistical value to be computed. The normality of the NPDE was assessed using distribution plots and global adjusted p values. The global adjusted p values were based on the Wilcoxon signed rank, Fisher and Shapiro–Wilks tests with Bonferroni adjustment [26, 27].
Lastly, a priori and a posteriori root mean square errors (RMSEs) of the model predictions were compared to evaluate bias and precision of prediction on the individual level with different amounts of pre-existing data. The a priori RMSE shows the predictive performance of the model without observed concentrations and was calculated from predictions based on the typical population estimates and patient covariate information, whereas the a posteriori RMSE shows the predictive performance if observed data from a first TDM occasion are also used to predict a future occasion. In this study, the a posteriori RMSE is more meaningful as it quantifies the predictive performance in the context of TDM. For the a priori and a posteriori RMSE calculation, only the TDM dataset was used as the study dataset did not contain the multiple sampling occasions per individual, needed for the calculations.
A single most suitable model was selected based on a joint assessment of the above-described evaluations. This model formed the basis for the model-based estimation in steps 4 and 5.
2.4 Development of a Sampling Strategy (Step 4)
Four potential LSSs, selected based on practical considerations, were evaluated. These practical considerations were based on the sampling times in our data and the desirability to shorten the total TDM time to < 6 h to increase patient friendliness of the sampling strategy. The LSSs had predefined fixed sampling at 2 h, 4 h, 2 and 4 h, and 2, 4 and 6 h after dosing. Evaluation of the fixed LSSs was performed using the study data and simulated data. For the latter, a rifampicin PK dataset of 1000 virtual individuals was simulated using random sampling from individual characteristic distributions derived from the National Health and Nutrition Examination Survey (NHANES) [28]. A more flexible windowed LSS, allowing sampling within a time window around selected time points, was also evaluated to check that the model could still give a good prediction when deviating from the fixed sampling points. Using the previously described base dataset with individual characteristics, we generated 500 datasets in which a randomly simulated observation time point was selected within ± 30 min of each fixed sampling time point.
The four fixed LSSs, and subsequently the windowed LSS, together with model-based exposure estimation, were evaluated for predictive performance in comparison with the currently used strategy at Radboudumc developed by Magis-Escurra et al. [9]. In addition, the performance of the model without any individual observed concentrations was assessed to evaluate the case without TDM. Predictive performance was assessed in terms of bias and precision (mean error [ME] and RMSE). For the study data, the model-predicted AUC24 on the full dataset was assumed to represent the true AUC24. For the simulation data, the simultaneously simulated AUC24 was the true AUC24. The results from the simulation data were split into three exposure groups to determine predictive performance specifically for patients with low, middle and high exposure. The middle-exposure group was of special interest as we expected predictions for the low and high groups to be too extreme to have a significant impact on dose advice. The first group comprised all individuals with a true AUC24 from zero to half the mean AUC24, as reported by Magis-Escurra et al. [9]. The second group ranged from half this mean to double, and the third group included patients having a true AUC24 higher than double this mean. The RMSEs of model-based exposure estimation and the linear regression strategy were tested for significant statistical differences using the Wilcoxon signed rank test. The selection of the most suitable LSS was based on predictive performance.
Subsequently, a comparison of the resulting dose advice based on the predictions was performed. For this purpose, the previously described dataset including 1000 virtual individuals was used. This dataset was used for estimation of the AUC24 applying the two exposure prediction approaches (linear regression vs. model-based). The dose advice, based on the estimated AUC24, was compared with the dose advice based on the true AUC24. The dose advice was determined by the guidelines used in clinical practice at Radboudumc. Advice to increase the dose is given when the estimated AUC24 is below 30.75 h·mg/L (defined as 75% of the mean AUC24 as identified by Magis-Escurra et al. [9]).
2.5 Numerical Verification (Step 5)
Implementation of the selected model in the InsightRX platform involved translation of the model code between programming languages. Similar to NONMEM [17], the InsightRX maximum a posteriori prediction (MAP) Bayesian estimation method uses the Broyden–Fletcher–Goldfarb–Shanno algorithm (BFGS, as implemented in the ‘optim’ package in R) to maximize the likelihood and obtain individual posterior parameter estimates. InsightRX uses the open source library PKPDsim [29] to obtain solutions for the differential equation PK model. The numerical verification comprised of the comparison of individual parameter estimates and concentration predictions between the NONMEM and InsightRX (R/PKPDsim) version of the model. An arbitrarily defined maximum allowed difference was set to 0.5%.
3 Results
3.1 Data (Step 1)
TDM data were available for 96 TB patients (391 samples), while the PK study provided 373 samples from 34 patients [9]. The characteristics of both the study and TDM data are shown in Table 1. The measured plasma concentrations for a standard rifampicin dose of 600 mg at 2, 4, and 6 h after dosing were comparable between the two datasets. Weight data were missing in 25% of patients in the TDM dataset, while FFM was missing in 26% of patients in the TDM dataset and 6% of patients in the study dataset.
3.2 Identification of Models (Step 2)
The PubMed search resulted in 271 hits. Twelve population PK models of rifampicin from between 1997 and 2017 were identified [10, 30,31,32,33,34,35,36,37,38,39,40]. No additional relevant publications were found in the references of the selected articles. The characteristics of the twelve models are summarised in Table 2 [10, 30,31,32,33,34,35,36,37,38,39,40,41,42]. Three of these models were not implemented for further testing as the publications either did not report the distribution shape of included interindividual variability [10] or reported it in a format not used by NONMEM [30, 32].
3.3 Selection of the Most Suitable Model (Step 3)
Based on assessment of the VPCs (shown in Online Resource 2), the best-performing models were those by Savic et al. [37], Milán Segovia et al. [34] and Svensson et al. [40]. Observed concentrations plotted against the individual prediction showed good predictive performance from the models by Smythe et al. [33], Chirehwa et al. [39] and Svensson et al. (data not shown, except for the models by Chirehwa et al. and Svensson et al. as reported in the online supplementary material). Based on the individual plots of the observed concentration versus time, the models by Chirehwa et al. and Svensson et al. had the best individual prediction (data not shown). Based on these assessments, we narrowed the candidates for the most suitable model down to those by Chirehwa et al. and Svensson et al.
Plots of CWRES and IWRES indicated that the model by Svensson et al. was preferable over the model by Chirehwa et al. (see Online Resource 3). The CWRES plotted against time showed a trend for both models, however the model by Svensson et al. performed better in the range of 2–12 h, in which most of the important PK of rifampicin are situated. The model by Svensson et al. performed better than the model by Chirehwa et al. on all IWRES plots.
Only the NPDEs from the model by Svensson et al. were shown to not differ from the normal distribution on the study data (global-adjusted p value of 0.07). No NPDEs were normally distributed for the models on the TDM data; however, the NPDEs from the model by Svensson et al. showed the least deviation from normality on the TDM dataset compared with the other models (data not shown).
The a priori and a posteriori RMSEs are shown in Fig. 2, and were calculated based on the PK data of patients from the TDM data who had a second TDM occasion (n =16). The least well-performing models were the models by Schipani et al. [38] and Wilkins et al. [31]. The model by Chirehwa et al. performed best, with the model by Svensson et al. a close second.
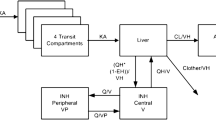
Overall, the models by Chirehwa et al. [39] and Svensson et al. [40] were found to have the best predictive performance, with minimal differences between the two. Ultimately, the model developed by Svensson et al. was considered the most suitable for TDM purposes as it was based on rifampicin doses from 10 to 40 mg/kg, instead of 10 mg/kg only in the model by Chirehwa et al., which may be important for TDM in the near future as high-dose rifampicin treatment may become more common [43]. The model by Svensson et al. is a one-compartment model with absorption through transit compartments, and includes an enzyme turnover model, concentration-dependent clearance, and dose-dependent bioavailability [40]. Figure 3 shows the VPCs of the model by Svensson et al. on our data.
Visual predictive checks of the model by Svensson et al. [40] on (a) the TDM data, and (b) the study data. The red lines represent the mean of the observed concentrations and the blue lines represent the 5th or 95th quartiles. The red and blue shaded areas represent the 95% confidence interval of the mean, and 5th or 95th quartiles, respectively, of the simulated concentrations. TDM therapeutic drug monitoring
3.4 Development of a Sampling Strategy (Step 4)
The predictive performance (ME and RMSE) using the study data of the four proposed model-informed LSSs, as well as the model without sampling, were compared with the linear regression strategy in Table 3. This comparison showed that every LSS performed better than model prediction without sampling. The fixed one-sample, model-informed LSSs performed worse than the currently used linear regression strategy. The 2- and 4-h and 2-, 4- and 6-h model-informed LSSs were less biased and as precise as the currently used linear regression strategy.
The 2- and 4-h and 2-, 4- and 6-h model-informed LSSs were also compared with the linear regression strategy regarding predictive performance using simulated data. This comparison is shown in Table 4 and is grouped according to true exposure. In the low- and middle-exposure groups, the model-informed approach had similar performance compared with the linear regression strategy. In the high-exposure group, the linear regression strategy generally outperformed the model-informed approach on predictive performance, except for the RMSE of Cmax prediction.
The model-informed LSS using 2- and 4-h sampling was selected as the most suitable for model-informed TDM, based on the fact that the predictive performance was satisfactory, and on the practical benefit of having only two sampling points instead of three. A windowed variant of this LSS was evaluated (its predictive performance is also shown in Table 4). Overall, the performance was comparable with its fixed sampling counterpart, demonstrating that the model also generates good predictions with flexible sampling points or deviations in sampling times.
A comparison of the resulting dose advice from predictions on the simulated data between the fixed 2- and 4-h model-informed LSS and the linear regression strategy is shown in Table 5. No statistically significant difference in sensitivity and specificity was found between the model-informed approach and the linear regression strategy.
3.5 Numerical Verification (Step 5)
Comparison of individual parameter estimates for the model by Svensson et al. obtained with the InsightRX MAP estimation engine versus parameters obtained using the same model implemented in NONMEM deviated only minimally (< 0.5%), as shown in Online Resource 4. Consequently, concentration predictions from the InsightRX PK simulation engine (based on the obtained individual estimates) versus predictions from NONMEM showed a negligible difference (< 10−3 mg/L) [see Online Resource 5].
4 Discussion
With this work, we have shown that model-informed precision dosing of rifampicin is feasible and offers benefits over the standard limited-sampling approach. After following a careful procedure for model evaluation focusing on exposure prediction, we selected the population PK model by Svensson et al. as the best model suitable for TDM of rifampicin for our population. We developed and validated a sampling strategy with only two flexible time points to estimate individual exposures.
There are multiple benefits to using the model-informed approach instead of a linear regression approach for the purpose of TDM. (1) It is flexible in handling sampling time deviations. Where a linear regression strategy can only use fixed sampling times, a model is far more flexible in using different sampling times. In current clinical practice, real sampling times often deviate from the scheduled times. These deviations decrease predictive performance when using a linear regression approach, but not as much with a model-informed approach. (2) Individual characteristics and dose history are regarded, which provides more informed individual predictions. (3) Additionally, previous pharmacokinetic observations may also be taken into account for predictions. (4) A model-informed approach can predict future exposure resulting from a proposed adjusted dose. (5) Specific to the model by Svensson et al. [40] is that it can handle the nonlinear PK of rifampicin, which is beneficial for exposure prediction of changes in dose, especially as patients are increasingly prescribed higher doses of rifampicin [12, 40, 43,44,45]. (6) Furthermore, the model is also able to capture variable absorption, theoretically giving it an edge over the linear regression strategy in case of delayed absorption.
Although the model-informed approach has many advantages, a downside could be its complexity; it requires sophisticated software, understanding of the technology and a significant time investment [10, 46]. Implementation of the model in a user-friendly interface, such as the InsightRX platform, is expected to greatly improve the ease of use in clinical practice and facilitate its implementation in clinical practice.
Although the selected population pharmacokinetic model could be used to investigate optimal dosing regimens in silico for the population, this was beyond the scope of our study. Our aim was to develop and validate a model-informed precision dosing strategy, independent of starting dose, which can also be further implemented in other populations and strategies. We point out that implementation of our strategy in other populations or settings should not be employed without ‘fit-for-purpose qualification’ [48]. However, as the selected model by Svensson et al. [40] was based on a South African population, and the datasets for development and validation were from a Dutch clinical setting, this may indicate that the selected model may also perform well in other settings.
A secondary contribution of this work was to provide a blueprint for how to evaluate and select population PK models to be used in TDM procedures. In this regard, some points should be mentioned. For the prediction performance comparison using the study data, it could be argued that a noncompartmental method for estimation of the true AUC24 could be more fitting than model estimation on the full dataset. However, it is thought that estimation by the model can be a better approximation of the truth as it is able to take measurement errors into account, which is why the model-predicted AUC24 was used [47]. In addition, since part of the data utilised in our evaluation of the LSS was initially used in the development of the linear regression strategy, it may be that the predictive performance of the linear regression strategy is inflated. The fact that these data have no sampling time deviations probably adds to the performance overestimation of the linear regression strategy for clinical practice. The probable overestimation of performance for the linear regression strategy further strengthens the notion that the proposed model-informed approach would outperform the linear regression strategy in clinical practice.
Some limitations specific to this study should be discussed. One potential shortcoming is that a more efficient LSS could have been developed by means of optimal design experiments. Nonetheless, we were able to validate the proposed strategy on already existing data with predefined sampling times. Another drawback is that the model by Chirehwa et al. [39] had similar predictive performance results as the model by Svensson et al. [40], but only the latter was used to develop the LSS. The model by Svensson et al. was regarded as being more representative for high-dose rifampicin as it was based on data with a wide dose range of 10–40 mg/kg, instead of only 10 mg/kg. Furthermore, the linear regression strategy from Magis-Escurra et al., to which we compare our model-informed approach, was developed to be optimal for five TB drugs, including rifampicin [9]. While the final linear regression strategy from that study was not the most optimal for rifampicin, all feasible suggested alternatives included a late sampling time at 6 h after dosing, which was avoided in the development of our LSS in order to reduce the time spent in the clinic by the patient. Lastly, the proposed model-informed strategy is seemingly outperformed by the linear regression strategy in individuals in the high-exposure group. This effect is inherent to the model-informed method as predictions are weighted towards the typical individual by the prior information. The individuals in the high-exposure group are extremes, with a relatively high exposure for this dosing schedule and population; therefore, their model-based predictions will be weighted down toward the typical individual. In practice, the dosing platform would give warnings when the fit is poor and suggest different courses of action for the clinician to take, e.g. to downweigh the model priors to rely more on the observed data and/or to gather more data on the patient to confirm or disprove the extreme values [48]. However, as predictions for individuals with extreme exposure are still well-removed from the dose-adjustment target, misprediction in these individuals will not affect dose-adjustment decisions. The clinical relevance of these mispredictions are therefore of negligible clinical relevance.
5 Conclusions
Our model-informed TDM strategy effectively shortens the sampling time by 2 h and removes one sampling point without performance loss compared with the sampling currently implemented in our hospital. Furthermore, it is more flexible, provides a more informed prediction, and can account for variable absorption and the nonlinear PK of rifampicin compared with all commonly used linear regression strategies. TDM can improve the response to TB treatment, and, in this study, we show that model-informed methods can simplify TDM, reducing its implementation hurdles, which may translate to benefit in TB patients.
References
World Health Organization. Global tuberculosis report 2017. http://www.who.int/tb/publications/global_report/en/. Accessed Aug 2018.
Alsultan A, Peloquin CA. Therapeutic drug monitoring in the treatment of tuberculosis: an update. Drugs. 2014;74(8):839–54.
Pasipanodya JG, McIlleron H, Burger A, Wash PA, Smith P, Gumbo T. Serum drug concentrations predictive of pulmonary tuberculosis outcomes. J Infect Dis. 2013;208(9):1464–73.
Griffin GE. Malabsorption, malnutrition and HIV disease. Bailliere’s Clin Gastroenterol. 1990;4(2):361–73.
Magis-Escurra C, van den Boogaard J, Ijdema D, Boeree M, Aarnoutse R. Therapeutic drug monitoring in the treatment of tuberculosis patients. Pulm Pharmacol Ther. 2012;25(1):83–6.
The Lancet Diabetes Endocrinology. Diabetes and tuberculosis: a wake-up call. Lancet Diabetes Endocrinol. 2014;2(9):677.
Chang J-T, Dou H-Y, Yen C-L, Wu Y-H, Huang R-M, Lin H-J, et al. Effect of type 2 diabetes mellitus on the clinical severity and treatment outcome in patients with pulmonary tuberculosis: a potential role in the emergence of multidrug-resistance. J Formos Med Assoc. 2011;110(6):372–81.
Jayaram R, Gaonkar S, Kaur P, Suresh BL, Mahesh BN, Jayashree R, et al. Pharmacokinetics–pharmacodynamics of rifampin in an aerosol infection model of tuberculosis. Antimicrob Agents Chemother. 2003;47(7):2118–24.
Magis-Escurra C, Later-Nijland HM, Alffenaar JW, Broeders J, Burger DM, van Crevel R, et al. Population pharmacokinetics and limited sampling strategy for first-line tuberculosis drugs and moxifloxacin. Int J Antimicrob Agents. 2014;44(3):229–34.
Sturkenboom MG, Mulder LW, de Jager A, van Altena R, Aarnoutse RE, de Lange WC, et al. Pharmacokinetic modeling and optimal sampling strategies for therapeutic drug monitoring of rifampin in patients with tuberculosis. Antimicrob Agents Chemother. 2015;59(8):4907–13.
Medellin-Garibay SE, Correa-Lopez T, Romero-Mendez C, Milan-Segovia RC, Romano-Moreno S. Limited sampling strategies to predict the area under the concentration-time curve for rifampicin. Ther Drug Monit. 2014;36(6):746–51.
Boeree MJ, Diacon AH, Dawson R, Narunsky K, du Bois J, Venter A, et al. A dose-ranging trial to optimize the dose of rifampin in the treatment of tuberculosis. Am J Respir Criti Care Med. 2015;191(9):1058–65.
Proost JH. Adaptive control of drug dosage regimens using maximum a posteriori probability Bayesian fitting. Int J Clin Pharmacol Ther. 1995;33(10):531–6.
Alsultan A, An G, Peloquin CA. Limited sampling strategy and target attainment analysis for levofloxacin in patients with tuberculosis. Antimicrob Agents Chemother. 2015;59(7):3800–7.
InsightRX. The InsightRX platform. San Francisco, CA; 2017. http://insight-rx.com/. Accessed Aug 2018.
R Core Team. R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. 2016. https://www.R-project.org/. Accessed Aug 2018.
Beal S, Sheiner LB, Boeckmann A, Bauer RJ. NONMEM user’s guides (1989–2009). Ellicott City: Icon Development Solutions; 2009.
Keizer RJ, Karlsson MO, Hooker A. Modeling and simulation workbench for NONMEM: Tutorial on pirana, PsN, and Xpose. CPT Pharmacometr Syst Pharmacol. 2013;2(6):e50.
European Medicines Agency. Guideline on bioanalytical method validation. 2011. http://www.ema.europa.eu/ema/index.jsp?curl=pages/includes/document/document_detail.jsp?webContentId=WC500109686%26mid=WC0b01ac058009a3dc. Accessed Aug 2018.
Ruslami R, et al. Pharmacokinetics and tolerability of a higher rifampin dose versus the standard dose in pulmonary tuberculosis patients. Antimicrob Agents Chemother. 2007;51(7):2546–51.
Beal SL. Ways to fit a PK model with some data below the quantification limit. J Pharmacokinet Pharmacodyn. 2001;28(5):481–504.
Janmahasatian S, Duffull SB, Ash S, Ward LC, Byrne NM, Green B. Quantification of lean bodyweight. Clin Pharmacokinet. 2005;44(10):1051–65.
Zhao W, Kaguelidou F, Biran V, Zhang D, Allegaert K, Capparelli EV, et al. External evaluation of population pharmacokinetic models of vancomycin in neonates: the transferability of published models to different clinical settings. Br J Clin Pharmacol. 2013;75(4):1068–80.
Bergstrand M, Hooker AC, Wallin JE, Karlsson MO. Prediction-corrected visual predictive checks for diagnosing nonlinear mixed-effects models. AAPS J. 2011;13(2):143–51.
Nguyen TH, Mouksassi MS, Holford N, Al-Huniti N, Freedman I, Hooker AC, et al. Model evaluation of continuous data pharmacometric models: metrics and graphics. CPT Pharmacometr Syst Pharmacol. 2017;6(2):87–109.
Comets E, Brendel K, Mentré F. Computing normalised prediction distribution errors to evaluate nonlinear mixed-effect models: the npde add-on package for R. Comput Methods Progr Biomed. 2008;90(2):154–66.
Wright SP. Adjusted P-values for simultaneous inference. Biometrics. 1992;48(4):1005–13.
Centers for Disease Control and Prevention, et al. National Health and Nutrition Examination Survey Data. Hyattsville: National Center for Health Statistics; 2017.
Keizer RJ. PKPDsim documentation. http://www.pkpdsim-docs.com. Accessed Aug 2018.
Peloquin CA, Jaresko GS, Yong CL, Keung AC, Bulpitt AE, Jelliffe RW. Population pharmacokinetic modeling of isoniazid, rifampin, and pyrazinamide. Antimicrob Agents Chemother. 1997;41(12):2670–9.
Wilkins JJ, Savic RM, Karlsson MO, Langdon G, McIlleron H, Pillai G, et al. Population pharmacokinetics of rifampin in pulmonary tuberculosis patients, including a semimechanistic model to describe variable absorption. Antimicrob Agents Chemother. 2008;52(6):2138–48.
Goutelle S, Bourguignon L, Maire PH, Van Guilder M, Conte JE Jr, Jelliffe RW. Population modeling and Monte Carlo simulation study of the pharmacokinetics and antituberculosis pharmacodynamics of rifampin in lungs. Antimicrob Agents Chemother. 2009;53(7):2974–81.
Smythe W, Khandelwal A, Merle C, Rustomjee R, Gninafon M, Bocar Lo M, et al. A semimechanistic pharmacokinetic-enzyme turnover model for rifampin autoinduction in adult tuberculosis patients. Antimicrob Agents Chemother. 2012;56(4):2091–8.
Milán Segovia RC, Dominguez Ramirez AM, Jung Cook H, Magana Aquino M, Vigna Perez M, Brundage RC, et al. Population pharmacokinetics of rifampicin in Mexican patients with tuberculosis. J Clin Pharm Ther. 2013;38(1):56–61.
Seng KY, Hee KH, Soon GH, Chew N, Khoo SH, Lee LS. Population pharmacokinetics of rifampicin and 25-deacetyl-rifampicin in healthy Asian adults. J Antimicrob Chemother. 2015;70(12):3298–306.
Jing Y, Zhu LQ, Yang JW, Huang SP, Wang Q, Zhang J. Population pharmacokinetics of rifampicin in chinese patients with pulmonary tuberculosis. J Clin Pharmacol. 2016;56(5):622–7.
Savic RM, Ruslami R, Hibma JE, Hesseling A, Ramachandran G, Ganiem AR, et al. Pediatric tuberculous meningitis: model-based approach to determining optimal doses of the anti-tuberculosis drugs rifampin and levofloxacin for children. Clin Pharmacol Ther. 2015;98(6):622–9.
Schipani A, Pertinez H, Mlota R, Molyneux E, Lopez N, Dzinjalamala FK, et al. A simultaneous population pharmacokinetic analysis of rifampicin in Malawian adults and children. Br J Clin Pharmacol. 2016;81(4):679–87.
Chirehwa MT, Rustomjee R, Mthiyane T, Onyebujoh P, Smith P, McIlleron H, et al. Model-based evaluation of higher doses of rifampin using a semimechanistic model incorporating autoinduction and saturation of hepatic extraction. Antimicrob Agents Chemother. 2016;60(1):487–94.
Svensson RJ, Aarnoutse RE, Diacon AH, Dawson R, Gillespie SH, Boeree MJ, et al. A population pharmacokinetic model incorporating saturable pharmacokinetics and auto-induction for high rifampicin doses. Clin Pharmacol Ther. 2017;103(4):674–83.
Conte JE, Golden JA, Kipps JE, Lin ET, Zurlinden E. Effect of sex and AIDS status on the plasma and intrapulmonary pharmacokinetics of rifampicin. Clin Pharmacokinet. 2004;43(6):395–404.
McIlleron H, Rustomjee R, Vahedi M, Mthiyane T, Denti P, Connolly C, et al. Reduced antituberculosis drug concentrations in HIV-infected patients who are men or have low weight: implications for international dosing guidelines. Antimicrob Agents Chemother. 2012;56(6):3232–8.
Svensson EM, Svensson RJ, te Brake LHM, Boeree MJ, Heinrich N, Konsten S, et al. The potential for treatment shortening with higher rifampicin doses: relating drug exposure to treatment response in patients with pulmonary tuberculosis. Clin Infect Dis. 2018;67(1):34–41.
Svensson RJ, Svensson EM, Aarnoutse RE, Diacon AH, Dawson R, Gillespie SH, et al. Greater early bactericidal activity at higher rifampicin doses revealed by modeling and clinical trial simulations. J Infect Dis. 2018;218(6):991–9.
Boeree MJ, Heinrich N, Aarnoutse R, Diacon AH, Dawson R, Rehal S, et al. High-dose rifampicin, moxifloxacin, and SQ109 for treating tuberculosis: a multi-arm, multi-stage randomised controlled trial. Lancet Infect Dis. 2017;17(1):39–49.
Donagher J, Martin JH, Barras MA. Individualised medicine: why we need Bayesian dosing. Intern Med J. 2017;47(5):593–600.
Sarem S, Li J, Barriere O, Litalien C, Theoret Y, Lapeyraque AL, et al. Bayesian approach for the estimation of cyclosporine area under the curve using limited sampling strategies in pediatric hematopoietic stem cell transplantation. Theor Biol Med Model. 2014;11:39.
Keizer RJ, et al. Model-informed precision dosing at the bedside: scientific challenges and opportunities. CPT Pharmacometr Syst Pharmacol. 2018. https://doi.org/10.1002/psp4.12353 (Epub 25 Sep 2018).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for either this study or for the preparation of this manuscript.
Conflict of interest
Ron J. Keizer is a co-founder and employee of InsightRX. Stijn W. van Beek, Rob ter Heine, Cecile Magis-Escurra, Rob E. Aarnoutse, and Elin M. Svensson declare no conflicts of interest that could have influenced the submitted work.
Ethical approval
The study protocols were approved by the Institutional Review Board of Radboudumc.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
OpenAccess This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
van Beek, S.W., ter Heine, R., Keizer, R.J. et al. Personalized Tuberculosis Treatment Through Model-Informed Dosing of Rifampicin. Clin Pharmacokinet 58, 815–826 (2019). https://doi.org/10.1007/s40262-018-00732-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40262-018-00732-2