Abstract
The 2014–2015 outbreak of Ebola virus disease is the largest epidemic to date in terms of the number of cases, deaths, and affected areas. In October 2015, no antiviral agents had proven antiviral efficacy in patients. However, in September 2014, the World Health Organization inventoried and has since regularly updated a list of potential drug candidates with demonstrated antiviral efficacy in in vitro or animal models. This includes agents belonging to various therapeutic classes, namely direct antiviral agents (favipiravir and BCX4430), a combination of antibodies (ZMapp), type I interferons, RNA interference-based drugs (TKM-Ebola and AVI-7537), and anticoagulant drugs (rNAPc2). Here, we review the pharmacokinetic and pharmacodynamic information presently available for these drugs, using data obtained in healthy volunteers for pharmacokinetics and data obtained in human clinical trials or animal models for pharmacodynamics. Future studies evaluating these drugs in clinical trials are critical to confirm their efficacy in humans, propose appropriate doses, and evaluate the possibility of treatment combinations.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
In response to the 2014–2015 outbreak in West Africa, the World Health Organization prioritized a list of drug candidates developed or repurposed for Ebola virus infection treatment. |
Here, we report the available pharmacokinetic/pharmacodynamic information on the drugs considered for clinical development or already tested in clinical trials as of July 2015, according to the World Health Organization. |
As most information was gathered from healthy volunteer and non-human primate studies, assessment of these drugs in Ebola virus-infected patients requires further investigation. |
1 Introduction
1.1 Epidemiology
Ebola virus (EBOV) was first discovered in 1976 when an outbreak of Ebola hemorrhagic fever occurred in central Africa and caused 280 deaths out of 318 confirmed cases [1]. Since then, 24 outbreaks have occurred in several African countries. The 2014–2015 outbreak initiated in Guinea, before spreading to Sierra Leone, Liberia, and other surrounding countries and is the most severe and deadly outbreak to date with 28,331 reported cases and 11,310 reported deaths up to September 20, 2015 [2], corresponding to an overall fatality rate of 40 %. Depending on the viral strain and available medical care, larger fatality rates up to 90 % in some settings have been reported [3].
1.2 Ebola Virus
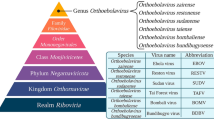
The genus Ebolavirus belongs to the Filoviridae family, order Mononegavirales. It includes four EBOV species highly pathogenic in humans: Zaire ebolavirus (responsible for the majority of cases reported until now), Sudan ebolavirus, Bundibugyo ebolavirus, and Taï Forest ebolavirus (formerly Cote d’Ivoire ebolavirus) [4, 5]. EBOV is a lipid-enveloped, heavily glycosylated, non-segmented, negative-strand RNA virus (Fig. 1) [6, 7]. Phylogenetic analysis indicates that the agent causing the recent outbreak in Western Africa, EBOV-Guinea, with isolated reference strains EBOV-Makona and EBOV-Gueckedou, belongs to an evolutionary lineage within the species Z. ebolavirus [8].
Structure of Ebola virus. Ebola virus is an enveloped virus presenting with a single-stranded RNA genome of nearly 19,000 nucleotides, encoding seven proteins: structural nucleoprotein (NP), polymerase cofactor (VP 35), VP 40, transcription activator (VP30), VP24, RNA-dependent RNA polymerase (L), and glycoprotein (GP). GP, also expressed in a soluble form (sGP), is responsible for host receptor binding and fusion with the cell membrane. Reproduced from Choi and Croyle. Biodrugs 2013 [7]
1.3 Natural History of the Disease
EBOV is transmitted between humans by mucosae contact with infected fluid [9]. Previous studies based on seroprevalence analysis in various African populations [10] have shown that filovirus infections can commonly be associated with asymptomatic or mild infections and that the EBOV genome could be detected in the blood of asymptomatic seroconverters exposed to documented EBOV symptomatic patients [11]. After an incubation period of 6–12 days, symptomatic patients enter an acute phase of infection during which they become highly contagious [6]. Early symptoms include fever, asthenia, and myalgia, and progress to gastrointestinal syndrome, including diarrhea and vomiting. This can lead to intravascular volume depletion, electrolyte perturbations, hypoperfusion, multi-organ failure including severe renal impairment, and finally shock [6, 12]. Then, disseminated intravascular coagulation and blood leakage, the consequences of massive cytokine release and viral replication in endothelial cells, may lead to hemorrhage syndrome, mostly represented by gastrointestinal bleeding. However, in the current outbreak, less than 20 % of patients submited bleeding [13]. In the case series of Sierra Leone, the average time from the reported onset of symptoms to death was 10 days, and surviving patients were discharged after a mean illness duration of 21 days [12].
1.4 Medical Care
1.4.1 Supportive Care
In the absence of an approved specific treatment, current medical care primarily relies on intensive supportive care [13], in particular, intravenous fluids and electrolytes solution, and oral rehydration to maintain intravascular volume. Sepsis management and blood transfusion can also be considered. Treatment of other concomitant disease such as malaria is recommended along with empiric antibiotics for enteric pathogens especially at the gastrointestinal phase of the illness [13, 14].
1.4.2 Convalescent Plasma
The use of convalescent plasma was among the first therapeutic approaches. These plasmas, collected in patients who recovered from EBOV infection, are expected to contain polyclonal immunoglobulins targeting EBOV proteins [15]. However, the kinetics of the immunoglobulins to EBOV, and more importantly that of sero-neutralizing antibodies are poorly characterized. They seem to be slower than in classical acute viral infections, probably because of the deep functional immunodeficiency observed during the disease. In fact, although clinical trials have attempted to assess the efficacy of convalescent plasma, no conclusive evidence has been reported yet [15].
1.4.3 Current Approaches for Specific Treatment
To accelerate and rationalize the evaluation of these putative agents, the World Health Organization (WHO) issued in 2014 and has frequently updated since then a document for Categorization and prioritization of drugs for consideration for testing or use in patients infected with Ebola [16]. Here, we review the pharmacokinetic and pharmacodynamic properties reported for the drugs categorized in class A and B in the 3 July, 2015 document, which are already or can be considered for clinical trials. These drugs are antivirals (favipiravir, BCX4430), immunotherapy based on monoclonal antibodies (ZMapp) or on immunomodulation (type-I interferons), and antisense therapy such as small interfering RNAs (TKM-Ebola) or oligonucleotides (AVI-7537). Other interventions based on drugs approved for other diseases have been proposed, but will not be discussed here as there is a lack of information on their efficacy in EBOV disease.
In the following session, we report for each drug candidate, the chemical structure or composition, mechanism of action (Table 1; Fig. 2), pharmacokinetic characteristics in humans or alternatively in animals (Table 2), available data on safety, in vitro half maximal effective concentration (EC50) assessment (Table 3), and efficacy in non-human primate (NHP) studies (Table 4; Fig. 3) if available or alternatively in rodents. Case reports and clinical trials are described to support efficacy in EBOV-infected patients.
Ebola viral lifecycle and targets of different therapeutic classes. Steps of virus life cycle: 1 attachment, 2 fusion with endosomal membranes, 3 nucleocapsid release, 4 mRNA transcription, 5 viral protein translation, 6 genome replication, and 7 viral assembly and release. Polymerase inhibitors hamper replication and transcription processes (4, 6), directly targeting the viral polymerase L. Monoclonal antibodies (ZMapp, MIL-77) bind to viral glycoprotein and therefore inhibit viral attachment (1) but also increase virions and infected cells clearance (not represented). Interfering RNAs inhibit the viral mRNA translation process (5), and enhance viral mRNA degradation. Type I interferons have pleiotropic indirect effects through host cell genes regulation, leading to viral mRNA degradation, inhibition of viral transcription (4) and translation (5), interference with the release of viral particles (7), facilitation apoptosis of infected cells, and enhancement of innate and adaptive immune response (not represented). Modified from Yazdanpanah et al., Intensive Care Med 2015 [13]
Survival of non-human primate-infected by Ebola virus and treated with highest doses of candidate drugs. Data from rhesus macaques and cynomolgus macaques are in red and blue, respectively. A colored solid line stands for post-exposure prophylaxis experiments (treatment initiation within 24-h post challenge) and a colored dashed line for curative treatment (treatment initiation after 24-h post challenge and a black line for the untreated control). + marks the end of the study follow-up. Survival plots were drawn from data reported in [28, 29, 31, 52, 53, 55, 64, 72] using the dose where the best survival rate was observed. IFN interferon
2 Drug Candidates
2.1 Favipiravir
Favipiravir (T-705) is a broad-spectrum antiviral developed by Toyama Chemical Co Ltd. It has been approved in Japan and is now in phase III of clinical development in USA for the treatment of complicated or resistant flu [17]. Favipiravir is a purine nucleic acid analog, which is ribosylated and phosphorylated intracellularly into its active form, T-705RTP. This active metabolite then interferes with viral replication, probably by inhibiting the RNA-dependent RNA polymerase [18]. It was also found to increase the mutation rate as observed with the influenza virus [19].
2.1.1 Pharmacokinetics and Safety
The pharmacokinetics of favipiravir was first characterized in Japanese healthy volunteers in several dose-escalating trials with doses ranging from 30 to 2400 mg for single administration and from 800 to 1200 mg daily for repeated administration. After a single oral dose, favipiravir concentration increases to a maximum plasma concentration within 2 h and then decreases rapidly with an elimination rate corresponding to a short half-life of 2–5.5 h (Toyama in-house documentation). Both time to the maximum plasma concentration and the half-life increase after multiple doses. Favipiravir is eliminated via metabolism, mainly by aldehyde oxidase, leading to the inactive metabolite T705M1, and marginally by xanthine oxidase. Most metabolites are excreted under hydroxylated forms via the kidney. The fraction of metabolites excreted in the urine increases over time to reach 80–100 % after 7 days. Favipiravir exhibits dose- and time-dependent pharmacokinetics, which is possibly owing to saturation and/or auto-inhibition of the main enzymatic pathway, as favipiravir was shown to inhibit aldehyde oxidase in vitro [20]. During the clinical development of favipiravir in USA, a lower plasma concentration of approximately 50 % has been observed in American patients as compared with Japanese patients.
The most frequent adverse events of favipiravir reported during the development for influenza treatment include mild to moderate diarrhea, asymptomatic increase of blood uric acid and transaminases, and a decrease in the neutrophil count [20].
2.1.2 Efficacy
Favipiravir was shown to have a high activity against EBOV in vitro. It effectively blocks the production of the infectious virus with an EC50 of 10 µg/mL in an in vitro experiment using Vero E6 cells and the wild-type Zaire EBOV Mayinga 1976 strain [21]. A higher EC50 value of about 31–63 µg/mL was reported in another study, using Vero C1008 cells and EBOV E718/EBOV Kikwit strains [22].
Preclinical data in murine models also demonstrated a strong efficacy of favipiravir against EBOV. In one study, A129 IFNα/β receptor−/− knockout mice were challenged by aerosol inoculation of 1000 focus-forming units of wild-type EBOV E718 and then left untreated (n = 12) or treated with 150 mg/kg twice daily (BID) 1-h post-challenge (n = 6) [22]. All mice starting treatment at day 6 survived, whereas all untreated mice died within 8 days post-challenge. In another study, C57BL/6 IFNα/β receptor−/− knockout mice were challenged by intranasal inoculation of 1000 focus-forming units of Zaire 1976 EBOV and then left untreated (n = 10) or treated with 150 mg/kg BID starting from day 6 (n = 5) or day 8 (n = 5) post-challenge. All mice receiving treatment at day 6 survived, while untreated mice and those receiving treatment at day 8 died within 10 days after infection [21]. The strong antiviral effect of favipiravir, with an average effectiveness in blocking viral production of 99.6 % at steady state was confirmed in a pharmacokinetic-viral kinetic model developed to characterize the data of the second study [23]. However, the analysis revealed that time was needed to achieve this steady state, with an anti-viral effectiveness of only 49.9 and 94.6 % at days 1 and 2, suggesting that favipiravir, to be fully effective, needs to be administered early. Studies in NHP models are ongoing but data are not yet available.
In the autumn of 2014, at the peak of the epidemic, favipiravir was the only drug meeting the three following criteria: a strong antiviral effect in animal models, a good safety profile, and large stocks of the drug readily available. This prompted the decision to evaluate favipiravir in a non-comparative proof-of-concept trial, in which all patients received favipiravir along with standardized care (JIKI trial) [24]. Using a modeling approach based on the pharmacokinetic data obtained in Japanese and preclinical results, a 10-day treatment with a loading dose of 6000 mg on day 1 and a maintenance dose of 2400 mg/day was used for adults [25]. These doses are larger than what is approved in Japan for complicated influenza (3200 mg on day 1, followed by 1200 mg for 4 days [20]). For children, doses were calculated in accordance with body weight [26]. Between December 2014 and April 2015, 126 patients were included, with a mortality rate of 52.6 % (excluding patients receiving also convalescent plasma, 95 % confidence interval 43.1–61.9), compared with 55 % in the pretrial period [24]. The baseline viral load was a critical predictor of survival with a mortality rate of 20 % (95 % confidence interval 11.6–32.4) in patients with less than 7.7 log10 copies/mL compared with 91 % (95 % confidence interval 78.8–96.4) in adults with more than 7.7 log10 copies/mL. In patients with less than 7.7 log10 copies/mL, the pretrial mortality was larger and equal to 30.5 %, suggesting that an effect of favipiravir merits further study in this population. Although the absence of a comparator group and the reduced number of included patients did not allow for a formal safety assessment, no signal of toxicity was reported in the JIKI trial [24].
2.2 BCX4430
BCX4430 is a broad-spectrum antiviral developed by BioCryst Pharmaceuticals, originally intended to target hepatitis C virus, but subsequently developed for the treatment of filovirus infections such as EBOV [27]. BCX4430 is an adenosine analog, which is metabolized into the triphosphate active form, BCX4430-TP. This active metabolite reduces the production of viral RNA by inhibiting the RNA polymerase activity via inducing premature termination of RNA chain synthesis [27]. The drug nucleotide has high selectivity for viral RNA polymerase. No evidence was found for the incorporation of the BCX4430 nucleotide into human DNA and RNA [27].
2.2.1 Pharmacokinetics and Safety
The pharmacokinetics of BCX4430 has been only evaluated in animal models, with doses ranging from 2 to 50 mg/kg. In rodents and cynomolgus macaques, BCX4430 concentration decreases rapidly in the plasma with a half-life of 5–10 min [27]. However, the half-life of its principal active metabolite, BCX4430-TP, in the liver in rats was substantially longer (6.2 h). High bioavailability and rapid absorption via the intramuscular route was observed in animal models [27]. In vitro experiments showed that BCX4430 exhibited no mutagenicity and produced no detectable chromosomal aberrations in human lymphocytes. A phase I study to evaluate the safety, tolerability, and pharmacokinetics of BCX4430 is ongoing [16].
2.2.2 Efficacy
BCX4430 exhibited a strong in vitro antiviral effect against EBOV with an EC50 of 3.13 µg/mL using HeLa cells and the EBOV Kikwit strain [27]. The efficacy of BCX4430 against EBOV infection has been evaluated in two different NHP models [28–30]. In one study, infected cynomolgus macaques were given various doses (from 3.4 to 16 mg/kg BID) 48 h post-challenge. The results of this study showed that BCX4430 significantly prolonged the survival time but did not improve the survival rate even at the highest dose tested [28]. In another study, infected rhesus macaque monkeys were given high intramuscular doses of BCX4430 (16 mg/kg BID or 25 mg/kg BID) 30–120 min after a virus challenge for 14 days [29, 30]. At the end of the follow-up period, all of the six NHPs receiving 25 mg/kg survived compared with four of six in the group receiving 16 mg/kg and none in the control group (n = 3, all dead within 9 days). The mean peak viral load (at day 8 in all animals) was 3 log10 copies/mL lower in treated NHP compared with untreated NHP (6 vs 9 log10 copies/mL, respectively) [29, 30].
2.3 ZMapp
ZMapp, developed by Mapp Biopharmaceutical, is a combination of three humanized monoclonal antibodies (c13C6, c2G4, and c4G7 in equal proportions) targeting the EBOV glycoprotein [31]. ZMapp components are produced by bioengineering in Nicotiana benthamiana, a plant able to express pharmaceutical proteins. These antibodies were demonstrated to have a large neutralizing activity in vitro [31], suggesting an ability to link with a strong affinity to viral particles, inhibiting their fusion with the target cells and enhancing their clearance. Monoclonal antibodies were also thought to accelerate the elimination of infected cells expressing viral glycoprotein, through an antibody-dependent cellular cytotoxicity mechanism or complement [32, 33].
Another similar cocktail of three monoclonal antibodies addressing the same binding domain sequence as ZMapp, known as MIL-77, is produced by MabWorks using mammalian Chinese hamster ovary cells to obtain a larger yield. Because no proof of equivalence of MIL-77 and Zmapp has been provided, the WHO recommended to complete ZMapp therapeutic evaluation before considering MIL-77 [16].
2.3.1 Pharmacokinetics and Safety
A phase I clinical trial to assess the pharmacokinetics and safety of ZMapp is ongoing in healthy volunteers with a unique dose level of 50 mg/kg and results are planned to be released in 2016 [34]. Preliminary information on the safety of the drug can be obtained from seven infected repatriated patients receiving the drug as compassionate therapy. The common side effects reported during immunoglobulin infusion were fever, hypotension, tachycardia, rash, and polypnea [35], which were handled using preventive antihistamine treatment and acetaminophen co-medication. One patient experienced generalized seizures, which disappeared after a temporary interruption of treatment.
2.3.2 Efficacy
The efficacy of monoclonal antibody cocktails, such as MB003 and ZMab, in preventing and treating EBOV disease in rodents and NHPs has been proved in several studies [36–39], with survival rates of 50–100 % and 43 % in rhesus macaques treated with monoclonal antibody cocktails started at 1 day and 5 days after the challenge, respectively [36–38].
ZMapp combination was obtained by selecting the most efficient antibodies in the MB003 and ZMab cocktails [31]. The in vitro EC50 of the three monoclonal antibodies in ZMapp were reported between 0.1 and 1 µg/mL using the Ebola-Guinea strain in veroE6 cells culture. ZMapp was then evaluated in a NHP study where 21 rhesus macaques infected with 628 pfu of Kikwik Ebola virus by the intramuscular route were left untreated (n = 3) or treated with three doses of 50 mg/kg given at a 3-day interval. The treatment was initiated at 3, 4, or 5 days post-challenge (n = 6 in each group). All the treated animals survived, whereas all in the control group died within 8 days after infection. In monkeys whose treatment started on day 5 after the challenge, EBOV disease symptoms were reversed by day 7 and the viral load reached the limit of quantitation by day 9 after treatment initiation.
ZMapp clinical use was restricted because of its limited supply. The European Medicines Agency reported that five of seven patients who received the drug as a compassionate use at days 6–16 after the onset of symptoms, in combination with intensive supportive care, survived [35]. Yet no imputability can be assessed from these single-case observations, receiving different dosing and sometimes other investigational treatments. An adaptive randomized clinical trial is ongoing in West Africa, promoted by NIAID [40] to evaluate the efficacy of ZMapp with other potential candidate treatments as comparators, with a fixed dose of 50 mg/kg administered every 3 days.
2.4 Interferons
Interferons (IFN) α and β belong to the class of type-I IFN, a family of cytokines with antiviral, antiproliferative, and immunoregulatory properties [41, 42]. These cytokines are the major effectors of the innate immune response to viral infection, through host cell genes regulation. They hamper intracellular viral replication by several mechanisms, including viral mRNA degradation, inhibition of viral transcription and translation, and interference with the release of viral particles. Furthermore, they enhance the clearance of infected cells by activating the apoptosis mechanism and recruiting cytotoxic cells [43]. As EBOV infection is associated with a strong alteration of host immune response, started by the downregulation of type-I IFN [44, 45] and massive lymphocyte apoptosis [46], IFN supplementation may help control the infection and the associated unregulated inflammatory syndrome. Several recombinant IFNs with chemical structures close to the natural type I IFNs have been commercialized (IFNα-2a, IFNα-2b, IFNβ-1a, IFNβ-1b).
2.4.1 Pharmacokinetics and Safety
The usual dose per injection range is 3–36 MIU three times a week for IFNα and about 30–44 µg weekly for IFNβ, respectively, depending on the indication and administration route. The recombinant type-I IFNs are poorly absorbed from the gastrointestinal tract and therefore have to be given parenterally [47, 48]. Following an intravenous bolus administration, IFN concentration decreases rapidly with a terminal half-life of 4–16 h for IFNα and 1–2 h for IFNβ [47]. By the subcutaneous route, IFN has a good bioavailability (>80 %) and is rapidly absorbed, with peak serum concentrations observed after 1–8 h and 3–15 h for IFNα and IFNβ, respectively [47]. The terminal half-life of IFNβ is prolonged in a subcutaneous administration [49].
The type-I IFNs share a similar safety profile. The most frequently encountered side effects include influenza-like symptoms (myalgia, asthenia, fevers, fatigue, and headache), neuropsychiatric consequences (depression, irritability, memory impairment), myelosuppression (neutropenia and thrombocytopenia), dermatological conditions, and the development or exacerbation of autoimmune disease, in particular thyroiditis [41, 50]. These side effects were reported for long-term treatment, and may have less impact in short-term treatments for acute infection.
2.4.2 Efficacy
The antiviral activity of type-I IFN has been proved in vitro in VeroE6 cells, using an engineered EBOV (Zaire 76) expressing green fluorescent protein with an EC50 of <0.4 ng/mL for IFNβ and 2 ng/mL for IFNα [51].
The efficacy of IFN monotherapy in treating EBOV infection has been evaluated in two NHP studies. The results showed that IFN given in monotherapy as post-exposure therapy had no effect on survival rates but appeared to prolong the survival time from 6 days in the control group (n = 2) to 7.5 days in cynomolgus monkeys receiving IFNα-2b (n = 4) and from 8.3 days in the control group (n = 26, experiment and historical controls) to 13.8 days in monkeys treated with IFNβ (n = 5) [52, 53]. The peak of the viral load appeared later, at day 7 post-challenge, in monkeys receiving IFNα-2b (n = 4) [52] in comparison with non-treated monkeys (peak at day 5 post-challenge, n = 2). In a separate study including two species of NHP infected by 1000 pfu IM of EBOV Kikwit, administration of IFNα in combination with ZMab at day 3 or 4 after the challenge improved the survival rates up to 75 % in cynomolgus macaques (n = 4) and 100 % in rhesus macaques (n = 4), compared with a survival rate of 50 % in ZMab monotherapy (n = 4) [39, 54].
The WHO mentioned an ongoing clinical trial of IFN in Guinea (not yet registered on clinicaltrial.gov at the end of September 2015) including a patient with early onset of symptoms [16].
2.5 TKM-Ebola
TKM-Ebola, developed by Arbutus biopharma (formerly known as Tekmira), belongs to a new therapeutic class based on RNA interference technology. This drug is composed of two small interfering RNAs (siRNAs), siLpol-2 and siVP35-2, whose sequences are complementary to those of EBOV viral polymerase and VP35 genes, respectively. As siRNAs are very unstable, they are encapsulated and protected in lipid nanoparticles coated with polyethylene glycol molecules [35, 55]. The two siRNAs in TKM-Ebola silence the corresponding viral genes by inhibiting mRNA translation and enhancing host cell-mediated viral mRNA destruction [56].
The initial formulation of TKM-Ebola, TKM 100-802 siEbola-2, was 100 % sequence complementarity to the corresponding genes of the EBOV Kikwit strain. However, these siRNAs have several mismatches when compared with the gene sequences of the EBOV Guinea (Makona) strain. To address the potential loss of efficacy, Tekmira developed a new formulation TKM 100-802 siEbola-3 specifically targeting the Guinea strain [55], the major strain responsible of the outbreak in West Africa.
2.5.1 Pharmacokinetics and Safety
The pharmacokinetics of TKM-Ebola was characterized in healthy volunteers in a single escalating dose, phase I clinical trial [57] with doses ranging from 0.075 to 0.5 mg/kg. The two siRNAs, siLpol-2 and siVP35-2, were shown to have comparable plasma concentration time profiles, suggesting the drug’s pharmacokinetics is mostly ruled by the distribution and metabolism of lipid nanoparticles and this finding can be extrapolated to other siRNA sequences with the same vectorization [35]. Preliminary data obtained from 24 patients suggest a greater than dose-proportional increase in maximum plasma concentration and an approximately dose-proportional increase in the area under the curve.
Most of the reported adverse events, fever, rigors, dizziness, chest tightness, and a raised heart rate can be related to transient inflammatory responses, starting during the first 6 h of perfusion and disappearing within 24 h post-infusion [16, 58]. Furthermore, one case of severe cytokine release syndrome was diagnosed when treated with the highest dose (0.5 mg/kg). Thus, the maximal dose was limited at 0.3 mg/kg daily for future studies.
2.5.2 Efficacy
The efficacy of the two components of TKM-Ebola was demonstrated in vitro using both Kikwit and Guinea strains on HepG2 cells, with EC50 reported between 50 and 250 ng/mL [55]. A mixture of these two siRNAs and another targeting VP24 gene (2 mg/kg), was administered to two groups of rhesus macaques infected by 1000 pfu of Kikwit EBOV at 30 min after infection, followed by three doses given at a 2-day interval (n = 3) or six doses given at a 1-day interval (n = 4) for 6 days. All monkeys receiving the daily treatment survived compared with two out of three who received the 2-day interval treatment [59]. The two most effective siRNAs, siLpol-2 and siVP35-2, were selected among this cocktail to constitute TKM 100-802 siEbola-2. In a second study, three rhesus monkeys infected with EBOV Makona strain (1000 pfu) via the intramuscular route were given daily doses of 0.5 mg/kg of TKM 100-802 siEbola-3 by infusion at day 4 post-infection, when viremia and clinical symptoms were well established [55]. All three monkeys survived up to day 28 while the two untreated monkeys died on days 8 and 9. Median peak viral load was also strongly reduced (1–4 log10 copies/mL) in the treatment group compared with the control group [55].
TKM-Ebola has been used in USA in two adult patients as compassionate treatment in combination with extensive supportive care and convalescent plasma [58]. The two patients survived despite severe disease-related clinical and biological alterations. A phase II, single-arm clinical trial was conducted in Sierra Leone to evaluate the efficacy of TKM-Ebola in patients. In July 2015, Tekmira announced that a predefined statistical endpoint was reached in an intermediate analysis, indicating the trial would be discontinued because of a low probability of demonstrating an overall therapeutic benefit [60].
2.6 AVI-7537
AVI-7537, developed by Sarepta Therapeutics, is a small RNA-like oligomer, with linkage to a six-member ring, instead of the natural five-member ribose ring of RNA and DNA [61]. This structure, called PMOplus, renders the RNA-like oligomer metabolically stable and resistant to DNAse and RNAse cleavage. The inclusion of five positive charges in AVI-7537 enhances the stability of the drug and its binding to the negatively charged RNA [62]. Having the same principle as other antisense therapies, AVI-7537 targets the specific sequences of the VP24 gene of EBOV and interferes with the mRNA translation of this protein, therefore, affecting viral replication. Initially in its development, the product was part of a compound known as AVI-6002, which contained (in a 1:1 ratio) AVI-7537 and another oligomer targeting VP35 (AVI-7539) [62, 63].
2.6.1 Pharmacokinetics and Safety
The pharmacokinetics and safety of AVI-7537 were assessed in a phase I, single-ascending dose study, with doses ranging from 0.005 to 4.5 mg/kg [61]. The mean maximum plasma concentration and area under the curve values of AVI-7537 approximately follow dose-proportional pharmacokinetics. The half-life was about 2–5 h. Urinary excretion of intact drug accounted for no more than 44 % of the total elimination at the highest dose. Other pathways contributing to the elimination of AVI-7537 are uncertain. The AVI-7537 renal clearance was not measurable for lower doses (≤0.05 mg/kg) and increased linearly with dose. This is likely to be because of the low affinity between the PMOplus agent and plasma proteins, resulting in a greater filtered fraction in the kidney and the increased steady-state volume of distribution observed at higher doses, which is about 400 mL/kg, compared with 100–200 mL/kg in low doses (≤0.05 mg/kg).
AVI-7537 was safe and well tolerated across the doses studied. Adverse effects associated with treatment, including gastrointestinal and nervous systems disorders, occurred in 50 % of patients who received AVI-6002, but were dose independent.
2.6.2 Efficacy
AVI-7537 was shown to effectively inhibit viral mRNA translation in a cell-free, in vitro translation system using rabbit reticulocyte lysate with an EC50 of 585 nM [62].
In vivo efficacy of AVI-7537 was evaluated in several NHP studies using rhesus macaques challenged with 1000 pfu of the EBOV Kikwit strain by intramuscular injection. In two proof-of-concept studies, five out of eight rhesus monkeys treated with 40 mg/kg of AVI-6002, starting at 30–60 min after the challenge, survived whereas the untreated monkey died within 7 days [63]. A dose-escalating experiment was conducted subsequently, in which rhesus monkeys were treated 30–60 min after the challenge with either 4 mg/kg (n = 5), 16 mg/kg (n = 5), 28 mg/kg (n = 5), or 40 mg/kg (n = 5) of AVI-6002 or with a scramble control (a PMOplus formulation that does not target the EBOV gene sequences) or placebo (n = 4 and n = 1, respectively) [62, 63]. All monkeys in the control and scramble control groups died by day 8 after infection. A dose-dependent survival was observed in this study, with 0, 20, 60, and 60 % survival in the groups receiving 4, 16, 28, and 40 mg/kg, respectively [62, 63]. In the last study, rhesus monkeys were given intravenously 40 mg/kg of either AVI-6002 (n = 8), AVI-7537 (n = 8), AVI-7539 (n = 8), or saline solution (n = 6) at 30–60 min after the challenge then once daily for 14 days [64]. The survival rates were 62.5, 75, 0, and 0 %, respectively, indicating that AVI-7537 alone was sufficient to confer protection from EBOV infection [64]. The peak viral loads following AVI-7537 and AVI-6002 treatments showed no significant difference but they were significantly lower than those of AVI-7539 and control groups [64].
The clinical development of AVI-7527 (AVI-6002) was pending because of funding issues. Based on the body surface, the dose of 28–30 mg/kg needed to achieve 50 % survival in the NHPs was estimated to translate to 9 mg/kg of AVI-6002 or 4.5 mg/kg of AVI-7537 [61].
2.7 rNAPc2
The Recombinant Nematode Anticoagulant Protein c2 (rNAPc2), originally cloned from a parasitic nematode, Ancylostoma caninum (dog hookworm) [65] is a potent long-acting anticoagulant developed by ARCA Pharma. It was shown to have no intrinsic antiviral action in vitro for a concentration range of 0.045–100 µg/mL. This protein, bound to the circulating coagulation Factor X, acts as an inhibitor of the complex Factor VIIa/Tissue Factor [65]. This complex physiologically enables the extrinsic pathway of the coagulation, and is widely implied in the unregulated, disseminated intravascular coagulation process leading to hemorrhagic symptoms in patients infected by EBOV [66]. Therefore, rNAPc2 was though to limit the coagulopathy and associated complications (renal failure, hemorrhage, multiple organ failure) [67].
2.7.1 Pharmacokinetics and Safety
The pharmacokinetics of rNAPc2 was assessed in humans following subcutaneous or intravenous administration in three phase I clinical studies using healthy volunteers with the doses ranging from 0.3 to 7.5 µg/kg [67, 68]. rNAPc2 was shown to have linear pharmacokinetics within the studied dose range [67, 68]. As a result of a high affinity between rNAPc2 and plasma clotting factor X, rNAPc2 has a prolonged elimination half-life of more than 50 h and is distributed predominantly in the plasma compartment, leading to a small distribution volume [67, 68]. The fact that rNAPc2 is closely bound to clotting Factor X in blood circulation, has a similar half-life, and is not detected in the urine suggest that the complex rNAPc2/Factor X may be cleared via the same elimination route of the unbound Factor X in the liver [68]. The accumulated data obtained in more than 700 patients from several phase I and II clinical studies suggest that rNAPc2 is safe and well tolerated following subcutaneous doses up to 10 µg/kg or intravenous doses up to 7.5 µg/kg in healthy volunteers [67–71]. Bleeding was the major side effect [69–71], but was related to invasive procedure (surgery and catheterization) or co-administration with platelet aggregation inhibitors. This adverse effect can be monitored and, if it occurs, can be reversed with recombinant Factor VIIa.
2.7.2 Efficacy
The efficacy of rNAPc2 has been evaluated in a NHP model using rhesus macaques challenged by 1000 pfu of Zaire 95 Ebola virus [72]. The drug was administered at the dose of 30 µg/kg daily by subcutaneous route at 10 min (n = 6) or 24 h (n = 3) after the viral challenge, respectively. Three of the nine treated monkeys survived, whereas all the three monkeys in the control group died. The mean survival time of dead animals was significantly longer in treated monkeys (11.7 vs 8.3 days).
3 Conclusion
The 2014–2015 outbreak has accelerated the development of various molecules for the treatment of EBOV disease. In this paper, we reviewed available pharmacokinetic/pharmacodynamic information of the most advanced therapeutic agents whose effectiveness against EBOV infection has been evaluated in vivo in clinical studies or in animal models.
The pharmacokinetic information reported in this review was collected only in healthy volunteers. However, EBOV disease causes dramatic alteration of vital functions [6], in particular, renal impairment, hepatic necrosis, blood leakage, coagulopathy, and multiple organ failure. These systemic syndromes, together with therapeutic interventions such as dialysis and large-volume electrolyte infusions may drastically modify drug plasma concentrations [73, 74]. Therefore, and despite the difficulties owing to the absence of analytical devices on the field and to the transfer of infectious samples to BSL4 facilities, it will remain particularly important to collect frequent measurements of drug concentrations in infected individuals to fully characterize the pharmacokinetics of a drug in the context of EBOV infection.
For most drugs, the NHP model is used to assess the in vivo efficacy before clinical development. However, important limitations of this model need to be kept in mind. First, the infection route is systematically via an intramuscular injection while it is not the common infection route in humans [9]. Second, the inoculum (usually 1000 pfu), set to correspond to the maximal amount of virus introduced by a needle stick accident [75], is probably much larger than in most human infections. Partly because of these two differences, the evolution of clinical symptoms and death in NHP models is much more rapid than in humans. In particular, there is no asymptomatic infection cases, no or only a short incubation period, and all untreated animals succumb within 10 days, compared with an incubation period of 2–21 days and a mortality rate of 40–90 % in humans [3]. As a consequence of the short natural history of the NHP infection and of the technical constraints that limit the number of experiments, all experiments published relied on early treatment compared with what can be done in the clinical setting [6]. In addition, given the small number of animals reported in NHP studies, subtle differences in the experimental conditions, such as the challenge used, the supportive care provided to treated animals, the decision process to euthanize animals, or the genetic differences across NHP species, can be sufficient to substantially modify the outcome of different studies. Therefore, the comparison of different NHP experiments should be done with caution, especially when they are not yet published in a peer-reviewed journal.
This review did not pretend to be exhaustive and we made the choice to present only drugs categorized in class A and B by the WHO. A number of agents that have shown anti-EBOV activity in vitro or in vivo in animals were not presented in this review. Among them, we can cite brincidofovir, a broad-spectrum antiviral developed by Chimerix. Its demonstrated in vitro efficacy against EBOV and clinical efficacy for other viral infection (cytomegalovirus) supported its evaluation in a clinical trial [76]. However, because of insufficient enrollment, the study was stopped and the development of brincidofovir for EBOV infection was discontinued by Chimerix. Recently, encouraging results of an antiviral developed by Gilead, GS-5734, have been reported as a late breaker abstract for the annual conference of the Infectious Diseases Society of America held in October 2015 [77]. GS-5734 is a prodrug of the adenine nucleotide analog, which undergoes fast conversion to a long half-life triphosphate metabolite (>10 h). GS-5734 inhibits EBOV (Kikwit and Makona strains) with a high in vitro efficacy (EC50 of 0.01–0.2 µM). Intravenous administration with a dose of 10 mg/kg initiated on day 3 led to 100 % survival and a 5 log10 copies/mL reduction in viral load in treated monkeys compared with the placebo group [77]. The first administration in a patient was allowed in October 2015 for compassionate care [78]. Several new compounds or drugs approved for other indications have also been identified to have activity against EBOV in vitro with different mechanisms of action such as preventing viral entry [79–84] or interfering with viral replication by targeting host factors [85–87] and may warrant future in vivo evaluation. Likewise, future developments will probably involve combination therapy with drugs having different mechanisms of action, as is done for other viral infections such as human immunodeficiency virus or hepatitis C virus. For instance, the combination of ZMab and IFNα was shown to improve the survival rates in monkeys compared with ZMab monotherapy [39] and a drug trial evaluating the combination of favipiravir and ZMapp is also planned.
In severe acute infection, as many patients may already develop high viremia and are in a critical condition when the treatment starts, it is crucial to rapidly achieve a high level of drug exposure. Consequently, clinical development plans of these drugs should consider the need for loading doses to reach the target exposure as quickly as possible to maximize clinical benefits.
Modeling and simulation of pharmacokinetic data obtained could be of critical importance to support the search for an optimal dosing regimen, in particular, in a sanitary crisis where the need for a therapeutic response may shorten the usual drug evaluation. Further, and following what has been done in other viral infections, such as influenza or hepatitis C virus [88, 89], a better anticipation of the effect of drugs on the outcome could be obtained by developing a mechanistic model of viremia. However, the use of this approach is still limited by the lack of data on the viral kinetics and other markers that may be related to treatment outcome.
Last, we focused on the effect of drugs during acute infection. However, some case reports have shown the presence of EBOV in semen as well as in ocular aqueous humor 3 months and 9 weeks after the clearance of viremia, respectively [90, 91]. These findings, if confirmed, suggest that antiviral therapy using drugs with high permeability to immune-privileged organs may also be needed in some patients long after the disappearance of EBOV-related symptoms.
Overall, vaccines remain the best way to prevent and rapidly control future outbreaks [92]. A number of vaccine candidates are currently under development, including an inactivated virus, virus-like particles, DNA vaccines, and recombinant viral vector-based vaccines [93]. One of the most advanced is rVSV-ZEBOV, a vaccine developed by Merck, showing promising results in an intermediate analysis of a phase III trial [94].
In summary, a large number of molecules are currently tested in animals and in clinical trials. These drugs, used alone or in combination, hold the promise that a significant breakthrough may occur in the near future. However, for that purpose, a considerable amount of information needs to be collected to better understand the effect of these drugs on the course of the disease and optimize the search for a cure.
References
Report of an International Commission. Ebola haemorrhagic fever in Zaire, 1976. Bull World Health Organ. 1978;56:271–93.
World Health Organization. Ebola Situation Report, 23 September 2015. Ebola [Internet]. http://apps.who.int/iris/bitstream/10665/185279/1/ebolasitrep_23Sept2015_eng.pdf?ua=1. Cited 28 Sep 2015.
Feldmann H, Geisbert TW. Ebola haemorrhagic fever. Lancet. 2011;377:849–62.
Bukreyev AA, Chandran K, Dolnik O, Dye JM, Ebihara H, Leroy EM, et al. Discussions and decisions of the 2012–2014 International Committee on Taxonomy of Viruses (ICTV) Filoviridae Study Group, January 2012–June 2013. Arch Virol. 2014;159:821–30.
Kuhn JH, Becker S, Ebihara H, Geisbert TW, Johnson KM, Kawaoka Y, et al. Proposal for a revised taxonomy of the family Filoviridae: classification, names of taxa and viruses, and virus abbreviations. Arch Virol. 2010;155:2083–103.
Ansari AA. Clinical features and pathobiology of Ebolavirus infection. J Autoimmun. 2014;55:1–9.
Choi JH, Croyle MA. Emerging targets and novel approaches to Ebola virus prophylaxis and treatment. BioDrugs Clin Immunother Biopharm Gene Ther. 2013;27:565–83.
Dudas G, Rambaut A. Phylogenetic analysis of Guinea 2014 EBOV Ebolavirus outbreak. PLoS Curr Outbreaks. 2014;6. doi:10.1371/currents.outbreaks.84eefe5ce43ec9dc0bf0670f7b8b417d.
Beeching NJ, Fenech M, Houlihan CF. Ebola virus disease. BMJ. 2014;349:g7348.
Moyen N, Thirion L, Emmerich P, Dzia-Lepfoundzou A, Richet H, Boehmann Y, et al. Risk factors associated with Ebola and Marburg viruses seroprevalence in blood donors in the Republic of Congo. PLoS Negl Trop Dis. 2015;9:e0003833.
Leroy EM, Baize S, Volchkov VE, Fisher-Hoch SP, Georges-Courbot MC, Lansoud-Soukate J, et al. Human asymptomatic Ebola infection and strong inflammatory response. Lancet Lond Engl. 2000;355:2210–5.
Schieffelin JS, Shaffer JG, Goba A, Gbakie M, Gire SK, Colubri A, et al. Clinical illness and outcomes in patients with Ebola in Sierra Leone. N Engl J Med. 2014;371:2092–100.
Yazdanpanah Y, Arribas JR, Malvy D. Treatment of Ebola virus disease. Intensive Care Med. 2015;41:115–7.
Fowler RA, Fletcher T, Fischer WA, Lamontagne F, Jacob S, Brett-Major D, et al. Caring for critically ill patients with Ebola virus disease: perspectives from West Africa. Am J Respir Crit Care Med. 2014;190:733–7.
van Griensven J, De Weiggheleire A, Delamou A, Smith PG, Edwards T, Vandekerckhove P, et al. The use of Ebola convalescent plasma to treat Ebola virus disease in resource-constrained settings: a perspective from the field. Clin Infect Dis. 2016;62(1):69–74.
World Health Organization. Categorization and prioritization of drugs for consideration for testing or use in patients infected with Ebola. In: Ebola treatments and interventions. 3 July 2015 [Internet]. http://www.who.int/medicines/ebola-treatment/2015_0703TablesofEbolaDrugs.pdf?ua=1. Cited 7 Sep 2015.
Li TCM, Chan MCW, Lee N. Clinical implications of antiviral resistance in influenza. Viruses. 2015;7:4929–44.
Furuta Y, Gowen BB, Takahashi K, Shiraki K, Smee DF, Barnard DL. Favipiravir (T-705), a novel viral RNA polymerase inhibitor. Antivir Res. 2013;100:446–54.
Arias A, Thorne L, Goodfellow I. Favipiravir elicits antiviral mutagenesis during virus replication in vivo. eLife. 2014;3:e03679.
Toyama Chemicals. Summary of product characteristics of Avigan (unpublished reference).
Oestereich L, Lüdtke A, Wurr S, Rieger T, Muñoz-Fontela C, Günther S. Successful treatment of advanced Ebola virus infection with T-705 (favipiravir) in a small animal model. Antivir Res. 2014;105:17–21.
Smither SJ, Eastaugh LS, Steward JA, Nelson M, Lenk RP, Lever MS. Post-exposure efficacy of oral T-705 (Favipiravir) against inhalational Ebola virus infection in a mouse model. Antivir Res. 2014;104:153–5.
Madelain V, Oestereich L, Graw F, Nguyen THT, de Lamballerie X, Mentré F, et al. Ebola virus dynamics in mice treated with favipiravir. Antivir Res. 2015;123:70–7.
Sissoko D, Laouenan C, Folkessons E, M’Lebing AB, Beavogui AH, Baize S et al. Favipiravir for treatment of Ebola virus disease (the JIKI Trial): a historically-controlled, single arm proof-of-concept trial in Guinea. PLOS Medicine. 2016. (In press)
Mentré F, Taburet A-M, Guedj J, Anglaret X, Keïta S, de Lamballerie X, et al. Dose regimen of favipiravir for Ebola virus disease. Lancet Infect Dis. 2015;15:150–1.
Bouazza N, Treluyer J-M, Foissac F, Mentré F, Taburet A-M, Guedj J, et al. Favipiravir for children with Ebola. Lancet. 2015;385:603–4.
Warren TK, Wells J, Panchal RG, Stuthman KS, Garza NL, Van Tongeren SA, et al. Protection against filovirus diseases by a novel broad-spectrum nucleoside analogue BCX4430. Nature. 2014;508:402–5.
Stonehouse J, Staab T, Bennett R. 26th Annual Piper Jaffray Healthcare Conference. New York, USA; 2014.
Stonehouse J, Sheridan B, Staab T, Bennett R. Citi 10th Annual Biotech Conference. Boston, USA; 2015.
BioCryst Pharmaceuticals Inc. BioCryst announces study results for BCX4430 in a non-human primate model of Ebola virus infection. In: Press Release. 23 Dec 2014 [Internet]. http://investor.shareholder.com/biocryst/releasedetail.cfm?ReleaseID=888802. Cited 7 Sep 2015.
Qiu X, Wong G, Audet J, Bello A, Fernando L, Alimonti JB, et al. Reversion of advanced Ebola virus disease in nonhuman primates with ZMapp. Nature. 2014;514:47–53.
Murin CD, Fusco ML, Bornholdt ZA, Qiu X, Olinger GG, Zeitlin L, et al. Structures of protective antibodies reveal sites of vulnerability on Ebola virus. Proc Natl Acad Sci. 2014;111:17182–7.
Zeitlin L, Pettitt J, Scully C, Bohorova N, Kim D, Pauly M, et al. Enhanced potency of a fucose-free monoclonal antibody being developed as an Ebola virus immunoprotectant. Proc Natl Acad Sci. 2011;108:20690–4.
National Institute of Allergy and Infectious Diseases. Safety and Pharmacokinetics of a Single ZMappTM Administration in Healthy Adult Volunteers [Internet]. https://clinicaltrials.gov/ct2/show/NCT02389192?term=zmapp+ebola&rank=2. Cited 7 Sep 2015.
European Medicines Agency. Medicinal products under development for the treatment of Ebola. In: Interim assessment report, 22 Jan 2015 [Internet]. http://www.ema.europa.eu/docs/en_GB/document_library/Report/2014/12/WC500179062.pdf. Cited 7 Sep 2015.
Pettitt J, Zeitlin L, Kim DH, Working C, Johnson JC, Bohorov O, et al. Therapeutic intervention of ebola virus infection in rhesus macaques with the MB-003 monoclonal antibody cocktail. Sci Transl Med. 2013;5:199ra113.
Olinger GG, Pettitt J, Kim D, Working C, Bohorov O, Bratcher B, et al. Delayed treatment of Ebola virus infection with plant-derived monoclonal antibodies provides protection in rhesus macaques. Proc Natl Acad Sci. 2012;109:18030–5.
Qiu X, Audet J, Wong G, Fernando L, Bello A, Pillet S, et al. Sustained protection against Ebola virus infection following treatment of infected nonhuman primates with ZMAb. Sci Rep. 2013;3:3365.
Qiu X, Wong G, Fernando L, Audet J, Bello A, Strong J, et al. mAbs and Ad-vectored IFN-α therapy rescue Ebola-infected nonhuman primates when administered after the detection of viremia and symptoms. Sci Transl Med. 2013;5:207ra143.
National Institute of Allergy and Infectious Diseases. Putative investigational therapeutics in the treatment of patients with known ebola infection—full text view—ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02363322?term=zmapp+ebola&rank=1. Cited 7 Sep 2015.
George PM, Badiger R, Alazawi W, Foster GR, Mitchell JA. Pharmacology and therapeutic potential of interferons. Pharmacol Ther. 2012;135:44–53.
Bekisz J, Schmeisser H, Hernandez J, Goldman ND, Zoon KC. Human interferons alpha, beta and omega. Growth Factors. 2004;22:243–51.
Lin F, Young HA. Interferons: success in anti-viral immunotherapy. Cytokine Growth Factor Rev. 2014;25:369–76.
Basler CF, Amarasinghe GK. Evasion of interferon responses by Ebola and Marburg viruses. J Interferon Cytokine Res. 2009;29:511–20.
Wong G, Kobinger GP, Qiu X. Characterization of host immune responses in Ebola virus infections. Expert Rev Clin Immunol. 2014;10:781–90.
Geisbert TW, Hensley LE, Gibb TR, Steele KE, Jaax NK, Jahrling PB. Apoptosis induced in vitro and in vivo during infection by Ebola and Marburg viruses. Lab Invest. 2000;80:171–86.
Jonasch E, Haluska FG. Interferon in oncological practice: review of interferon biology, clinical applications, and toxicities. Oncologist. 2001;6:34–55.
Radwanski E, Perentesis G, Jacobs S, Oden E, Affrime M, Symchowicz S, et al. Pharmacokinetics of Interferon α-2b in Healthy Volunteers. J Clin Pharmacol. 1987;27:432–5.
Vidal 2015 dictionary [Internet]. https://www.vidal.fr/. Cited 7 Sep 2015.
Rogge MC, Liu Y, Galluppi GR. Interferon beta assessment in non-Chinese and Chinese subjects: pharmacokinetics and pharmacodynamic activity of an endogenous cytokine are not race dependent. J Clin Pharmacol. 2014;54:1153–61.
Subramanian GM, Moore PA, Gowen BB, Olsen AL, Barnard DL, Paragas J, et al. Potent in vitro activity of the albumin fusion type 1 interferons (albumin-interferon-alpha and albumin-interferon-beta) against RNA viral agents of bioterrorism and the severe acute respiratory syndrome (SARS) virus. Chemotherapy. 2008;54:176–80.
Jahrling PB, Geisbert TW, Geisbert JB, Swearengen JR, Bray M, Jaax NK, et al. Evaluation of immune globulin and recombinant interferon-alpha2b for treatment of experimental Ebola virus infections. J Infect Dis. 1999;179(Suppl 1):S224–34.
Smith LM, Hensley LE, Geisbert TW, Johnson J, Stossel A, Honko A, et al. Interferon-β therapy prolongs survival in rhesus macaque models of Ebola and Marburg hemorrhagic fever. J Infect Dis. 2013;208:310–8.
Qiu X, Audet J, Wong G, Pillet S, Bello A, Cabral T, et al. Successful treatment of Ebola virus-infected cynomolgus macaques with monoclonal antibodies. Sci Transl Med. 2012;4:138ra81–138ra81.
Thi EP, Mire CE, Lee ACH, Geisbert JB, Zhou JZ, Agans KN, et al. Lipid nanoparticle siRNA treatment of Ebola-virus-Makona-infected nonhuman primates. Nature. 2015;521:362–5.
Castanotto D, Rossi JJ. The promises and pitfalls of RNA-interference-based therapeutics. Nature. 2009;457:426–33.
Tekmira Pharmaceuticals Corporation. Safety, tolerability and pharmacokinetic first in human (FIH) study for intravenous (IV) TKM-100802—ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02041715?term=tkm+ebola&rank=2. Cited 7 Sep 2015.
Kraft CS, Hewlett AL, Koepsell S, Winkler AM, Kratochvil CJ, Larson L, et al. The use of TKM-100802 and convalescent plasma in 2 patients with Ebola virus disease in the United States. Clin Infect Dis. 2015;61:496–502.
Geisbert TW, Lee ACH, Robbins M, Geisbert JB, Honko AN, Sood V, et al. Postexposure protection of non-human primates against a lethal Ebola virus challenge with RNA interference: a proof-of-concept study. Lancet. 2010;375:1896–905.
US Securities and Exchange Commission. Tekmira provides update on TKM-Ebola-Guinea [Internet]. 2015. http://www.sec.gov/Archives/edgar/data/1447028/000117184315003522/newsrelease.htm. Cited 30 Sep 2015.
Heald AE, Iversen PL, Saoud JB, Sazani P, Charleston JS, Axtelle T, et al. Safety and pharmacokinetic profiles of phosphorodiamidate morpholino oligomers with activity against Ebola virus and marburg virus: results of two single-ascending-dose studies. Antimicrob Agents Chemother. 2014;58:6639–47.
Iversen PL, Warren TK, Wells JB, Garza NL, Mourich DV, Welch LS, et al. Discovery and early development of AVI-7537 and AVI-7288 for the treatment of Ebola virus and Marburg virus infections. Viruses. 2012;4:2806–30.
Warren TK, Warfield KL, Wells J, Swenson DL, Donner KS, Van Tongeren SA, et al. Advanced antisense therapies for postexposure protection against lethal filovirus infections. Nat Med. 2010;16:991–4.
Warren TK, Whitehouse CA, Wells J, Welch L, Heald AE, Charleston JS, et al. A single phosphorodiamidate morpholino oligomer targeting VP24 protects rhesus monkeys against lethal ebola virus infection. mBio. 2015;6:e02344–14.
Stassens P, Bergum PW, Gansemans Y, Jespers L, Laroche Y, Huang S, et al. Anticoagulant repertoire of the hookworm Ancylostoma caninum. Proc Natl Acad Sci. 1996;93:2149–54.
Geisbert TW, Young HA, Jahrling PB, Davis KJ, Kagan E, Hensley LE. Mechanisms underlying coagulation abnormalities in ebola hemorrhagic fever: overexpression of tissue factor in primate monocytes/macrophages is a key event. J Infect Dis. 2003;188:1618–29.
de Pont ACJM, Moons AHM, de Jonge E, Meijers JCM, Vlasuk GP, Rote WE, et al. Recombinant nematode anticoagulant protein c2, an inhibitor of tissue factor/factor VIIa, attenuates coagulation and the interleukin-10 response in human endotoxemia. J Thromb Haemost. 2004;2:65–70.
Vlasuk GP, Bradbury A, Lopez-Kinninger L, Colón S, Bergum PW, Maki S, et al. Pharmacokinetics and anticoagulant properties of the factor VIIa-tissue factor inhibitor recombinant Nematode anticoagulant protein c2 following subcutaneous administration in man. Dependence on the stoichiometric binding to circulating factor X. Thromb Haemost. 2003;90:803–12.
Giugliano RP, Wiviott SD, Stone PH, Simon DI, Schweiger MJ, Bouchard A, et al. Recombinant nematode anticoagulant protein c2 in patients with non-ST-segment elevation acute coronary syndrome: the ANTHEM-TIMI-32 trial. J Am Coll Cardiol. 2007;49:2398–407.
Lee A, Agnelli G, Büller H, Ginsberg J, Heit J, Rote W, et al. Dose-response study of recombinant factor VIIa/tissue factor inhibitor recombinant nematode anticoagulant protein c2 in prevention of postoperative venous thromboembolism in patients undergoing total knee replacement. Circulation. 2001;104:74–8.
Moons AHM, Bijsterveld NR, Koch KT, Meijers JCM, Tijssen JGP, van der Poll T, et al. Inhibition of the tissue factor pathway of coagulation by recombinant nematode anticoagulant protein c2 during elective coronary stent implantation. Neth Heart J. 2004;12:48–54.
Geisbert TW, Hensley LE, Jahrling PB, Larsen T, Geisbert JB, Paragas J, et al. Treatment of Ebola virus infection with a recombinant inhibitor of factor VIIa/tissue factor: a study in rhesus monkeys. Lancet. 2003;362:1953–8.
Hites M, Dell’Anna AM, Scolletta S, Taccone FS. The challenges of multiple organ dysfunction syndrome and extra-corporeal circuits for drug delivery in critically ill patients. Adv Drug Deliv Rev. 2014;77:12–21.
Roberts DJ, Hall RI. Drug absorption, distribution, metabolism and excretion considerations in critically ill adults. Expert Opin Drug Metab Toxicol. 2013;9:1067–84.
Shurtleff AC, Warren TK, Bavari S. Nonhuman primates as models for the discovery and development of ebolavirus therapeutics. Expert Opin Drug Discov. 2011;6:233–50.
Chimerix. An Open-Label, Multicenter study of the safety and anti viral activity of brincidofovir (BCV, CMX001) for Ebola virus disease—full text view—ClinicalTrials.gov [Internet]. https://clinicaltrials.gov/ct2/show/NCT02271347?term=brincidofovir+ebola&rank=1. Cited 25 Sep 2015.
Warren T, Jordan R, Lo M, Soloveva V, Ray A, Bannister R, et al. Nucleotide prodrug GS-5734 is a broad-spectrum filovirus inhibitor that provides complete therapeutic protection against the development of Ebola virus disease (EVD) in infected non-human primates. 2015;IDweek 2015:LB-2. https://idsa.confex.com/idsa/2015/webprogram/Paper54208.html. Accessed 1 Dec 2015.
Gilead Sciences. Gilead provides update on investigational compound, GS-5734, for the treatment of Ebola virus disease, Gilead [Internet]. http://www.gilead.com/news/press-releases/2015/10/gilead-provides-update-on-investigational-compound-gs5734-for-the-treatment-of-ebola-virus-disease. Cited 1 Dec 2015.
Shoemaker CJ, Schornberg KL, Delos SE, Scully C, Pajouhesh H, Olinger GG, et al. Multiple cationic amphiphiles induce a Niemann-Pick C phenotype and inhibit Ebola virus entry and infection. PLoS One. 2013;8:e56265.
Gehring G, Rohrmann K, Atenchong N, Mittler E, Becker S, Dahlmann F, et al. The clinically approved drugs amiodarone, dronedarone and verapamil inhibit filovirus cell entry. J Antimicrob Chemother. 2014;69:2123–31.
Neveu G, Barouch-Bentov R, Ziv-Av A, Gerber D, Jacob Y, Einav S. Identification and targeting of an interaction between a tyrosine motif within hepatitis C virus core protein and AP2M1 essential for viral assembly. PLoS Pathog. 2012;8:e1002845.
Basu A, Li B, Mills DM, Panchal RG, Cardinale SC, Butler MM, et al. Identification of a small-molecule entry inhibitor for filoviruses. J Virol. 2011;85:3106–19.
Wolf MC, Freiberg AN, Zhang T, Akyol-Ataman Z, Grock A, Hong PW, et al. A broad-spectrum antiviral targeting entry of enveloped viruses. Proc Natl Acad Sci. 2010;107:3157–62.
Côté M, Misasi J, Ren T, Bruchez A, Lee K, Filone CM, et al. Small molecule inhibitors reveal Niemann-Pick C1 is essential for Ebola virus infection. Nature. 2011;477:344–8.
Warren TK, Warfield KL, Wells J, Enterlein S, Smith M, Ruthel G, et al. Antiviral activity of a small-molecule inhibitor of filovirus infection. Antimicrob Agents Chemother. 2010;54:2152–9.
Kinch MS, Yunus AS, Lear C, Mao H, Chen H, Fesseha Z, et al. FGI-104: a broad-spectrum small molecule inhibitor of viral infection. Am J Transl Res. 2009;1:87–98.
Aman MJ, Kinch MS, Warfield K, Warren T, Yunus A, Enterlein S, et al. Development of a broad-spectrum antiviral with activity against Ebola virus. Antivir Res. 2009;83:245–51.
Nguyen T, Guedj J. HCV kinetic models and their implications in drug development. CPT Pharmacomet Syst Pharmacol. 2015;4:231–42.
Canini L, Perelson AS. Viral kinetic modeling: state of the art. J Pharmacokinet Pharmacodyn. 2014;41:431–43.
Bausch DG, Towner JS, Dowell SF, Kaducu F, Lukwiya M, Sanchez A, et al. Assessment of the risk of Ebola virus transmission from bodily fluids and fomites. J Infect Dis. 2007;196:S142–7.
Varkey JB, Shantha JG, Crozier I, Kraft CS, Lyon GM, Mehta AK, et al. Persistence of Ebola virus in ocular fluid during convalescence. N Engl J Med. 2015;372:2423–7.
Tully CM, Lambe T, Gilbert SC, Hill AVS. Emergency Ebola response: a new approach to the rapid design and development of vaccines against emerging diseases. Lancet Infect Dis. 2015;15:356–9.
Martínez MJ, Salim AM, Hurtado JC, Kilgore PE. Ebola virus infection: overview and update on prevention and treatment. Infect Dis Ther. 2015;4(4):365–90.
Henao-Restrepo AM, Longini IM, Egger M, Dean NE, Edmunds WJ, Camacho A, et al. Efficacy and effectiveness of an rVSV-vectored vaccine expressing Ebola surface glycoprotein: interim results from the Guinea ring vaccination cluster-randomised trial. Lancet. 2015;386:857–66.
Acknowledgments
We thank Toyama Chemicals for providing us with the favipiravir pharmacokinetic data from their phase I clinical trials. We also wish to acknowledge Benoit Visseaux for his assistance with Fig. 2.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This project has received funding from the European Union’s Horizon 2020 Research and Innovation Programme under grant agreement No. 666092.
Conflicts of interest
The UMR 1137 research team, to which belong Vincent Madelain, Thi Huyen Tram Nguyen, Jeremie Guedj, and France Mentre, as well as Xavier de Lamballerie, received grants from the European Union and from Saint Luke University (Japan) to evaluate the PKPD of favipiravir in NHPs and in patients. THT Nguyen is conducting a post-doctoral research funded by the European Union project for favipiravir evaluation in Ebola virus patients. Anaelle Olivo and Anne-Marie Taburet declare that they have no conflict of interest related to the submitted manuscript.
Additional information
V. Madelain and T. H. T. Nguyen contributed equally to this manuscript.
Rights and permissions
About this article
Cite this article
Madelain, V., Nguyen, T.H.T., Olivo, A. et al. Ebola Virus Infection: Review of the Pharmacokinetic and Pharmacodynamic Properties of Drugs Considered for Testing in Human Efficacy Trials. Clin Pharmacokinet 55, 907–923 (2016). https://doi.org/10.1007/s40262-015-0364-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40262-015-0364-1