Abstract
Background
Sacubitril-valsartan is a new medication that has recently been recommended as a replacement for enalapril in the treatment of patients with heart failure with reduced ejection fraction (HFrEF).
Objective
This study aimed to determine the cost effectiveness of sacubitril-valsartan compared with enalapril.
Methods
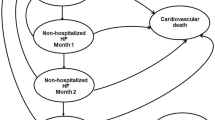
An analytical decision model was developed to estimate the long-term costs and outcomes from a healthcare perspective. Clinical inputs were mostly derived from the PARADIGM-HF study. Enalapril-related costs, risk of non-cardiovascular death, and all-cause readmission rate were based on data from Thailand. The costs and outcomes were discounted at 3% annually. The incremental cost-effectiveness ratio (ICER) was calculated and presented for the year 2017. A series of sensitivity analyses were also performed.
Results
For the base-case, the increased cost (144,146 vs. 16,048 Thai baht [THB]) of sacubitril-valsartan was associated with gains in both life-years (9.214 vs. 8.367 years) and quality-adjusted life-years (QALYs) (7.698 vs. 6.909) compared with enalapril, yielding an ICER of 162,276 THB/QALY ($US4857.11/QALY). This ICER is not considered to be cost effective at the willingness-to-pay (WTP) level of 160,000 THB/QALY. The risk of cardiovascular death and costs of both sacubitril-valsartan and hospitalization influenced the ICER. At a WTP of 160,000 THB/QALY, sacubitril-valsartan had a 48% probability of being a cost-effective treatment.
Conclusions
At its current price in Thailand, sacubitril-valsartan may not represent good value for the nations’s limited healthcare resources. The cost of sacubitril-valsartan needs to reduce by approximately 2% to yield an ICER below the threshold.





Similar content being viewed by others
References
Heidenreich PA, Albert NM, Allen LA, Bluemke DA, Butler J, Fonarow GC, et al. Forecasting the impact of heart failure in the United States: a policy statement from the American Heart Association. Circ Heart Fail. 2013;6(3):606–19.
Ponikowski P, Anker SD, AlHabib KF, Cowie MR, Force TL, Hu S, et al. Heart failure: preventing disease and death worldwide. ESC Heart Fail. 2014;1(1):4–25.
Owan TE, Hodge DO, Herges RM, Jacobsen SJ, Roger VL, Redfield MM. Trends in prevalence and outcome of heart failure with preserved ejection fraction. N Engl J Med. 2006;355(3):251–9.
Yancy CW, Jessup M, Bozkurt B, Butler J, Casey DE Jr, Colvin MM, et al. 2017 ACC/AHA/HFSA focused update of the 2013 ACCF/AHA guideline for the management of heart failure: a Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Failure Society of America. J Am Coll Cardiol. 2017;70(6):776–803.
Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JG, Coats AJ, et al. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: the Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC)Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur Heart J. 2016;37(27):2129–200.
McMurray JJ, Packer M, Desai AS, Gong J, Lefkowitz MP, Rizkala AR, et al. Angiotensin-neprilysin inhibition versus enalapril in heart failure. N Engl J Med. 2014;371(11):993–1004.
Packer M, Armstrong WM, Rothstein JM, Emmett M. Sacubitril-Valsartan in heart failure: why are more physicians not prescribing it? Ann Intern Med. 2016;165(10):735–6.
Sandhu AT, Ollendorf DA, Chapman RH, Pearson SD, Heidenreich PA. Cost-effectiveness of sacubitril-valsartan in patients with heart failure with reduced ejection fraction. Ann Intern Med. 2016;165(10):681–9.
King JB, Shah RU, Bress AP, Nelson RE, Bellows BK. Cost-effectiveness of sacubitril-valsartan combination therapy compared with enalapril for the treatment of heart failure with reduced ejection fraction. JACC Heart Fail. 2016;4(5):392–402.
Gaziano TA, Fonarow GC, Claggett B, Chan WW, Deschaseaux-Voinet C, Turner SJ, et al. Cost-effectiveness analysis of sacubitril/valsartan vs. enalapril in patients with heart failure and reduced ejection fraction. JAMA Cardiol. 2016;1(6):666–72.
van der Pol S, Degener F, Postma MJ, Vemer P. An economic evaluation of sacubitril/valsartan for heart failure patients in the Netherlands. Value Health. 2017;20(3):388–96.
Ramos IC, Versteegh MM, de Boer RA, Koenders JMA, Linssen GCM, Meeder JG, et al. Cost effectiveness of the angiotensin receptor neprilysin inhibitor sacubitril/valsartan for patients with chronic heart failure and reduced ejection fraction in the Netherlands: a country adaptation analysis under the former and current Dutch pharmacoeconomic guidelines. Value Health. 2017;20(10):1260–9.
Ademi Z, Pfeil AM, Hancock E, Trueman D, Haroun RH, Deschaseaux C, et al. Cost-effectiveness of sacubitril/valsartan in chronic heart-failure patients with reduced ejection fraction. Swiss Med Wkly. 2017;29(147):w14533.
Liang L, Bin-Chia WuD, Aziz MIA, Wong R, Sim D, Leong KTG, et al. Cost-effectiveness of sacubitril/valsartan versus enalapril in patients with heart failure and reduced ejection fraction. J Med Econ. 2018;21(2):174–81.
Thavorncharoensap M, Teerawattananon Y, Natanant S, Kulpeng W, Yothasamut J, Werayingyong P. Estimating the willingness to pay for a quality-adjusted life year in Thailand: does the context of health gain matter? Clinicoecon Outcomes Res. 2013;5:29–36.
Owens DK. Interpretation of cost-effectiveness analyses. J Gen Intern Med. 1998;13(10):716–7.
Rajadurai J, Tse HF, Wang CH, Yang NI, Zhou J, Sim D. Understanding the epidemiology of heart failure to improve management practices: an Asia-Pacific perspective. J Card Fail. 2017;23(4):327–39.
Kristensen SL, Martinez F, Jhund PS, Arango JL, Belohlavek J, Boytsov S, et al. Geographic variations in the PARADIGM-HF heart failure trial. Eur Heart J. 2016;37(41):3167–74.
Tanvejsilp P, Ngorsuraches S. Defining the scope of health technology assessment and types of health economic evaluation. J Med Assoc Thai. 2014;97(Suppl 5):S10–6.
Janwanishstaporn S. National trend, in-hospital and long term outcomes in the hospitalized heart failure patients in Thailand. Thai Heart Journal. 2015;28:128.
Bundhamcharoen K, Aungkulanon S. Burden of disease in Thai population 2009: International Health Policy Program; 2012.
Health Statistics, Strategy and Planning Division, Ministry of Public Health. Mortality rate per 100,000 Thai population by causes of death during 1998–2016. 2016 [cited 2 February 2018]. http://social.nesdb.go.th/SocialStat/StatReport_Final.aspx?reportid=441&template=2R1C&yeartype=M&subcatid=15.
Packer M, McMurray JJ, Desai AS, Gong J, Lefkowitz MP, Rizkala AR, et al. Angiotensin receptor neprilysin inhibition compared with enalapril on the risk of clinical progression in surviving patients with heart failure. Circulation. 2015;131(1):54–61.
Desai AS, Claggett BL, Packer M, Zile MR, Rouleau JL, Swedberg K, et al. Influence of sacubitril/valsartan (LCZ696) on 30-day readmission after heart failure hospitalization. J Am Coll Cardiol. 2016;68(3):241–8.
Drug and Medical Supply Information Center, Ministry of Public Health. 2017 [cited 1 September 2017]. http://dmsic.moph.go.th.
Riewpaiboon A. Measurement of costs for health economic evaluation. J Med Assoc Thai. 2014;97(Suppl 5):S17–26.
Bank of Thailand. Foreign exchange rates 2017 [cited 28 September 2017]. https://www.bot.or.th/english/statistics/financialmarkets/exchangerate/_layouts/application/exchangerate/ExchangeRate.aspx.
Permsuwan U, Guntawongwan K, Buddhawongsa P. Handling time in economic evaluation studies. J Med Assoc Thai. 2014;97(Suppl 5):S50–8.
Limwattananon S. Sensitivity analysis for handling uncertainty in an economic evaluation. In: Chaikledkaew U, Teerawattananon Y, editors. Guidelines for health technology assessment in Thailand. 2nd ed. Nonthaburi: Wacharin; 2013. p. 105–19.
Briggs AH. Handling uncertainty in cost-effectiveness models. Pharmacoeconomics. 2000;17(5):479–500.
Zethraeus N, Johannesson M, Jonsson B, Lothgren M, Tambour M. Advantages of using the net-benefit approach for analysing uncertainty in economic evaluation studies. Pharmacoeconomics. 2003;21(1):39–48.
Safraj S, Ajay VS, Prabhakaran D. Heart failure: meeting the challenges of surveillance and knowledge translation in resource-poor settings. Curr Cardiol Rev. 2013;9(2):99–101.
Callender T, Woodward M, Roth G, Farzadfar F, Lemarie JC, Gicquel S, et al. Heart failure care in low- and middle-income countries: a systematic review and meta-analysis. PLoS Med. 2014;11(8):e1001699.
Laothavorn P, Hengrussamee K, Kanjanavanit R, Moleerergpoom W, Laorakpongse D, Pachirat O, et al. Thai acute decompensated heart failure registry (Thai ADHERE). CVD Prevention and Control. 2010;5(3):89–95.
Acknowledgements
The authors gratefully acknowledge Ahthit Yindeengam for the technical assistance.
Author information
Authors and Affiliations
Contributions
RK: research design, data acquisition and interpretation, drafting and critical revision of the manuscript. UP: data acquisition, model development and analysis, interpretation of results, drafting and critical revision of the manuscript.
Corresponding author
Ethics declarations
Funding
No sources of funding were used to conduct this study or prepare this manuscript.
Conflict of interest
Rungroj Krittayaphong and Unchalee Permsuwan have no conflicts of interest that are directly relevant to the content of this study.
Ethical approval
This project did not involve the study of human subjects or animals.
Rights and permissions
About this article
Cite this article
Krittayaphong, R., Permsuwan, U. Cost-Effectiveness Analysis of Sacubitril-Valsartan Compared with Enalapril in Patients with Heart Failure with Reduced Ejection Fraction in Thailand. Am J Cardiovasc Drugs 18, 405–413 (2018). https://doi.org/10.1007/s40256-018-0288-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40256-018-0288-x