Abstract
Purpose
Endocrinology and Metabolism Research Institute (EMRI), Tehran University of Medical Sciences, has achieved many advances in the understanding of epidemiology, pathology, and molecular biology of thyroid cancer (TC). This paper will focus on published literature in the field of TC research at EMRI since its inception.
Methods
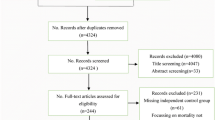
A comprehensive literature search of “Scopus”, “Web of Science (ISI)”, “PubMed”, and “SID” databases was done to identify TC-based studies in EMRI since 2005, using the predefined keywords.
Results
All the records were reviewed. Eventually, 46 articles that met the inclusion and exclusion criteria were considered. Timeline, characteristics, and summarized findings of the included most studies have been briefly described.
Conclusion
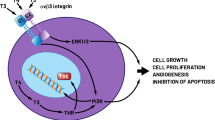
The main focus of the TC research at EMRI is to investigate genetic and epigenetic changes as well as the cellular and molecular aspects seen more frequently in TC patients, and find out how exactly these alterations lead to more aggressive TC behavior and resistance to the conventional treatment approaches in those patients.
Similar content being viewed by others
Abbreviations
- 1H-NMR:
-
hydrogen-1 nuclear magnetic resonance
- 3D:
-
three-dimensional
- ABC:
-
ATP binding cassette
- AGREE:
-
Appraisal of Guidelines Research and Evaluation
- ATC:
-
anaplastic thyroid carcinoma
- BRAF:
-
v-Raf murine sarcoma viral oncogene homolog B
- CASC2:
-
cancer susceptibility candidate 2
- CDH1:
-
cadherin 1
- cfDNA:
-
circulating cell-free DNA
- CFSE:
-
5,6-carboxyfluorescein N-hydroxysuccinimidyl ester
- CSC:
-
cancer stem cell
- ctDNA:
-
circulating tumor DNA
- Ci:
-
cuire
- DAPK:
-
death associated protein kinase
- DNMT1:
-
DNA methyltransferase 1
- DTC:
-
differentiated thyroid cancer
- EGFRvIII:
-
epithelial growth factor receptor variant III
- EMRI:
-
endocrinology and metabolism research institute
- FSCN1:
-
fascin actin-bundling protein 1
- FTA:
-
follicular thyroid adenoma
- FTC:
-
follicular thyroid carcinoma
- GAS5:
-
growth arrest special 5
- GBq:
-
gigabecquerel
- GM:
-
gut microbiome
- HLA-C:
-
major histocompatibility complex class I C
- HLA-DR:
-
major histocompatibility complex class II DR
- HLA-DRB1:
-
major histocompatibility complex class II DR beta1
- HOTAIRM1:
-
HOX antisense intergenic RNA myeloid 1
- IHC:
-
immunohistochemical
- I− :
-
iodine
- LncRNA:
-
long non-coding RNA
- IRMA:
-
immunoradiometric assay
- Klhl14:
-
kelch like family member 14
- MACS:
-
magnetic-activated cell sorting
- MALAT1:
-
metastasis associated lung adenocarcionoma transcript 1
- MEK:
-
mitogen-activated protein kinase kinase 1
- MEN 2A:
-
multiple endocrine neoplasia type 2A
- MGMT:
-
O-6-methylguanine-DNA methyltransferase
- MIR22HG:
-
MIR22 host gene
- miRNA:
-
micro RNA
- MMP-2:
-
matrix metallopeptidase 2
- MRI:
-
magnetic resonance imaging
- MS-HRM:
-
methylation-sensitive high resolution melting
- MTC:
-
medullary thyroid carcinoma
- NIS:
-
sodium/iodide symporter
- P16:
-
cyclin dependent kinase inhibitor 2A
- P53:
-
tumor protein P53
- PPARγ:
-
peroxisome proliferator activated receptor gamma
- PCA3:
-
prostate cancer antigen 3
- PTC:
-
papillary thyroid carcinoma
- PTEN:
-
phosphatase and tensin homolog
- RAI:
-
radioiodine
- RAIR:
-
radioiodine-refractory
- RAIR-DTC:
-
radioiodine-refractory differentiated thyroid cancer
- RARβ2:
-
retinoic acid receptor beta
- RASSF1A:
-
Ras association domain family member 1
- RFLP:
-
restriction fragment length polymorphism
- qRT-PCR:
-
quantitative real-time polymerase chain reaction; RAS association domain family member 1
- RET:
-
ret. proto-oncogene
- SLC5A8:
-
solute carrier family 5 member 8
- TC:
-
thyroid cancer
- TSH:
-
thyroid-stimulating hormone
- TSHR:
-
thyroid-stimulating hormone receptor.
References
Jung CK, Little MP, Lubin JH, Brenner AV, Wells SA, Sigurdson AJ, et al. The increase in thyroid cancer incidence during the last four decades is accompanied by a high frequency of BRAF mutations and a sharp increase in RAS mutations. J Clin Endocrinol Metab. 2014;99(2):E276–E85.
Fugazzola L, Elisei R, Fuhrer D, Jarzab B, Leboulleux S, Newbold K, et al. 2019 European thyroid association guidelines for the treatment and follow-up of advanced radioiodine-refractory thyroid Cancer. Eur Thyroid J. 2019;8(5):227–45.
Aashiq M, Silverman DA, Na’ara S, Takahashi H, Amit M. Radioiodine-refractory thyroid Cancer: molecular basis of Redifferentiation therapies, management, and novel therapies. Cancers. 2019;11(9):1382.
Schneider DF, Chen H. New developments in the diagnosis and treatment of thyroid cancer. CA Cancer J Clin. 2013;63(6):373–94.
Larijani B, Mohagheghi MA, Bastanhagh MH, Mosavi-Jarrahi AR, Haghpanah V, Tavangar SM, et al. Primary thyroid malignancies in Tehran, Iran. Med Princ Pract. 2005;14(6):396–400.
Haghpanah V, Soliemanpour B, Heshmat R, Mosavi-Jarrahi A, Tavangar S, Malekzadeh R, et al. Endocrine cancer in Iran: based on cancer registry system. Indian J Cancer. 2006;43(2):80–5.
Haghpanah V, Shooshtarizadeh P, Heshmat R, Larijani B, Tavangar SM. Immunohistochemical analysis of survivin expression in thyroid follicular adenoma and carcinoma. Appl Immunohistochem Mol Morphol. 2006;14(4):422–5.
Haghpanah V, Ghaffari SH, Rahimpour P, Abbasi A, Saeedi M, Pak H, et al. Vitamin D receptor gene polymorphisms in patients with thyroid cancer. Gene Ther Mol Biol. 2007;11(2):299–304.
Haghpanah V, Khalooghi K, Adabi K, Amiri P, Tavangar SM, Amirzargar A, et al. Associations between HLA-C alleles and papillary thyroid carcinoma. Cancer Biomarkers. 2009;5(1):19–22.
Omidfar K, Moinfar Z, Sohi AN, Tavangar SM, Haghpanah V, Heshmat R, et al. Expression of EGFRvIII in thyroid carcinoma: immunohistochemical study by camel antibodies. Immunol Investig. 2009;38(2):165–80.
Tabriz HM, Adabi K, Lashkari A, Heshmat R, Haghpanah V, Larijani B, et al. Immunohistochemical analysis of nm23 protein expression in thyroid papillary carcinoma and follicular neoplasm. Pathol Res Prac. 2009;205(2):83–7.
Mohammadi-Asl J, Larijani B, Khorgami Z, Tavangar SM, Haghpanah V, Mehdipour P. Prevalence of BRAFV600E mutation in Iranian patients with papillary thyroid carcinoma: a single-center study. J Appl Sci. 2009;9(19):3593–7. https://doi.org/10.3923/jas.2009.3593.3597.
Amoli MM, Yazdani N, Amiri P, Sayahzadeh F, Haghpanah V, Tavangar SM, et al. HLA-DR association in papillary thyroid carcinoma. Dis Markers. 2010;28(1):49–53.
Alvandi E, Akrami SM, Chiani M, Hedayati M, Nayer BN, Tehrani MRM, et al. Molecular analysis of the RET proto-oncogene key exons in patients with medullary thyroid carcinoma: a comprehensive study of the iranian population. Thyroid. 2011;21(4):373–82. https://doi.org/10.1089/thy.2010.0267.
Irani S, Rashidian A, Yousefi-Nooraie R, Soltani A. Evaluating clinical practice guidelines developed for the management of thyroid nodules and thyroid cancers and assessing the reliability and validity of the AGREE instrument. J Eval Clin Pract. 2011;17(4):729–36. https://doi.org/10.1111/j.1365-2753.2010.01561.x.
Mohammadi-asl J, Larijani B, Khorgami Z, Tavangar SM, Haghpanah V, Kheirollahi M, et al. Qualitative and quantitative promoter hypermethylation patterns of the P16, TSHR, RASSF1A and RARβ2 genes in papillary thyroid carcinoma. Med Oncol. 2011;28(4):1123–8.
Fallahi B, Adabi K, Majidi M, Fard-Esfahani A, Heshmat R, Larijani B, et al. Incidence of second primary malignancies during a long-term surveillance of patients with differentiated thyroid carcinoma in relation to radioiodine treatment. Clin Nucl Med. 2011;36(4):277–82.
Malehmir M, Haghpanah V, Larijani B, Ahmadian S, Alimoghaddam K, Heshmat R, et al. Multifaceted suppression of aggressive behavior of thyroid carcinoma by all-trans retinoic acid induced re-differentiation. Mol Cell Endocrinol. 2012;348(1):260–9.
Yazdani N, Sayahpour FA, Haghpanah V, Amiri P, Shahrabi-Farahani M, Moradi M, et al. Survivin gene polymorphism association with papillary thyroid carcinoma. Pathol Res Pract. 2012;208(2):100–3.
Sanii S, Saffar H, Tabriz HM, Qorbani M, Haghpanah V, Tavangar SM. Expression of matrix metalloproteinase-2, but not caspase-3, facilitates distinction between benign and malignant thyroid follicular neoplasms. Asian Pac J Cancer Prev. 2012;13(5):2175–8.
Saffar H, Sanii S, Emami B, Heshmat R, Panah VH, Azimi S, et al. Evaluation of MMP2 and Caspase-3 expression in 107 cases of papillary thyroid carcinoma and its association with prognostic factors. Pathol Res Pract. 2013;209(3):195–9. https://doi.org/10.1016/j.prp.2012.06.011.
Samimi H, Ghadami M, Khashayar P, Soleimani M, Larijani B, Haghpanah V. MicroRNAs networks in thyroid cancers: focus on miRNAs related to the fascin. J Diabetes Metab Disord. 2013;12(1):31.
Samimi H, Ghadami M, Khashayar P, Soleimani M, Larijani B, Haghpanah V. Essential genes in thyroid cancers: focus on fascin. J Diabetes Metab Disord. 2013;12(1):32.
Masbi MH, Mohammadiasl J, Galehdari H, Ahmadzadeh A, Tabatabaiefar MA, Golchin N, et al. Characterization of wild-type and mutated RET proto-oncogene associated with familial medullary thyroid cancer. Asian Pac J Cancer Prev. 2014;15:2027–33.
Haghpanah V, Malehmir M, Larijani B, Ahmadian S, Alimoghaddam K, Heshmat R, et al. The beneficial effects of valproic acid in thyroid cancer are mediated through promoting redifferentiation and reducing stemness level: an in vitro study. J Thyroid Res. 2014;2014:1–9.
Haghpanah V, Fallah P, Tavakoli R, Naderi M, Samimi H, Soleimani M, et al. Antisense-miR-21 enhances differentiation/apoptosis and reduces cancer stemness state on anaplastic thyroid cancer. Tumor Biol. 2016;37(1):1299–308.
Haghpanah V, Fallah P, Naderi M, Tavakoli R, Soleimani M, Larijani B. Cancer stem-like cell behavior in anaplastic thyroid cancer: a challenging dilemma. Life Sci. 2016;146:34–9.
Khatami F, Larijani B, Heshmat R, Keshtkar A, Mohammadamoli M, Teimoori-Toolabi L et al. Meta-analysis of promoter methylation in eight tumor-suppressor genes and its association with the risk of thyroid cancer. 2017;12(9):e0184892. https://doi.org/10.1371/journal.pone.0184892.
Samimi H, Fallah P, Sohi AN, Tavakoli R, Naderi M, Soleimani M, et al. Precision medicine approach to anaplastic thyroid cancer: advances in targeted drug therapy based on specific signaling pathways. Acta Medica Iranica. 2017:200–8.
Yekta RF, Oskouie AA, Tavirani MR, Mohajeri-Tehrani MR, Soroush AR. Decreased apolipoprotein A4 and increased complement component 3 as potential markers for papillary thyroid carcinoma: a proteomic study. Int J Biol Markers. 2018;33(4):455–62. https://doi.org/10.1177/1724600818787752.
Yekta RF, Tavirani MR, Oskouie AA, Mohajeri-Tehrani MR, Soroush AR, Baghban AA. Serum-based metabolic alterations in patients with papillary thyroid carcinoma unveiled by non-targeted 1H-NMR metabolomics approach. Iran J Basic Med Sci. 2018;21(11):1140–7. https://doi.org/10.22038/ijbms.2018.30375.7323.
Khatami F, Larijani B, Heshmat R, Nasiri S, Saffar H, Shafiee G, et al. Promoter methylation of four tumor suppressor genes in human papillary thyroid carcinoma. Iran J Pathol. 2019;14(4):290–9. https://doi.org/10.30699/IJP.2019.94401.1922.
Khatami F, Teimoori-Toolabi L, Heshmat R, Nasiri S, Saffar H, Mohammadamoli M, et al. Circulating ctDNA methylation quantification of two DNA methyl transferases in papillary thyroid carcinoma. J Cell Biochem. 2019;120(10):17422–37. https://doi.org/10.1002/jcb.29007.
Samimi H, Haghpanah V, Irani S, Arefian E, Sohi AN, Fallah P, et al. Transcript-level regulation of MALAT1-mediated cell cycle and apoptosis genes using dual MEK/Aurora kinase inhibitor “BI-847325” on anaplastic thyroid carcinoma. Daru. 2019;27:1–7.
Abbasifarid E, Sajjadi-Jazi SM, Beheshtian M, Samimi H, Larijani B, Haghpanah V. The role of ATP-binding cassette transporters in the Chemoresistance of anaplastic thyroid Cancer: a systematic review. Endocrinology. 2019;160(8):2015–23.
Samimi H, Haghpanah V, Irani S, Fallah P, Arefian E, Soleimani M. Determination of ATP-competitive inhibitor drug toxicity in anaplastic thyroid Cancer based on cell characteristics and three-dimensional cell culture. Modares Journal of Biotechnology. 2019;10(3):503–9.
Mahdiannasser M, Haghpanah V, Damavandi E, Kabuli M, Tavangar SM, Larijani B, et al. Investigation of promoter methylation of FSCN1 gene and FSCN1 protein expression in differentiated thyroid carcinomas. Mol Biol Rep. 2020;47(3):2161–9. https://doi.org/10.1007/s11033-020-05315-8.
Khatami F, Larijani B, Heshmat R, Nasiri S, Haddadi-Aghdam M, Teimoori-Toolabi L, et al. Hypermethylated RASSF1 and SLC5A8 promoters alongside BRAFV600E mutation as biomarkers for papillary thyroid carcinoma. J Cell Physiol. 2020;235(10):6954–68. https://doi.org/10.1002/jcp.29591.
Samimi H, Haghpanah V. Gut microbiome and radioiodine-refractory papillary thyroid carcinoma pathophysiology. Trends Endrocrinol Metab. 2020;31:627–30.
Samimi H, Sajjadi-Jazi SM, Seifirad S, Atlasi R, Mahmoodzadeh H, Faghihi MA, et al. Molecular mechanisms of long non-coding RNAs in anaplastic thyroid cancer: a systematic review. Cancer Cell Int. 2020;20(1):1–15.
Gholizadeh Siahmazgi Z, Irani S, Ghiaseddin A, Fallah P, Haghpanah V. BIOINFORMATIC study on effect of XANTHOHUMOL as bioactive compound of hop in the inhibition of the MAPK/ERK pathway in thyroid cancer. Iranian Journal of Diabetes and Metabolism. 2020;19(4):225–33.
Farrokhi Yekta R, Rezaie Tavirani M, Arefi Oskouie A, Mohajeri-Tehrani MR, Soroush AR. The metabolomics and lipidomics window into thyroid cancer research. Biomarkers. 2017;22(7):595–603. https://doi.org/10.1080/1354750X.2016.1256429.
Khatami F, Tavangar SM. Circulating tumor DNA (ctDNA) in the era of personalized cancer therapy. J Diabetes Metab Disord. 2018;17(1):19–30. https://doi.org/10.1007/s40200-018-0334-x.
Khatami F, Tavangar SM. Genetic and epigenetic of medullary thyroid cancer. Iran Biomed J. 2018;22(3):142–50. https://doi.org/10.22034/ibj.22.3.142.
Khatami F, Tavangar SM. A review of driver genetic alterations in thyroid cancers. Iran J Pathol. 2018;13(2):125–35. https://doi.org/10.30699/ijp.13.2.125.
Khatami F, Tavangar SM. Liquid biopsy in thyroid cancer: new insight. Int J Hematol Oncol Stem Cell Res. 2018;12(3):234–47.
Khatami F, Larijani B, Nasiri S, Tavangar SM. Liquid biopsy as a minimally invasive source of thyroid cancer genetic and epigenetic alterations. Int J Mol Cell Med. 2019;8:19–29. https://doi.org/10.22088//IIJMCM.BUMS.8.2.19.
Khatami F, Larijani B, Nikfar S, Hasanzad M, Fendereski K, Tavangar SM. Personalized treatment options for thyroid cancer: current perspectives. Pharmgenomics Pers Med. 2019;12:235–45. https://doi.org/10.2147/PGPM.S181520.
Khatami F, Payab M, Sarvari M, Gilany K, Larijani B, Arjmand B, et al. Oncometabolites as biomarkers in thyroid cancer: a systematic review. Cancer Manag Res. 2019;11:1829–41. https://doi.org/10.2147/CMAR.S188661.
Homayouni M, Mohammad Arabzadeh SA, Nili F, Razi F, Amoli MM. Evaluation of the presence of Epstein-Barr virus (EBV) in Iranian patients with thyroid papillary carcinoma. Pathol Res Pract. 2017;213(7):854–6. https://doi.org/10.1016/j.prp.2017.01.020.
Larijani B, Aghakhani S, Khajeh-Dini H, Baradar-Jalili R. Clinico-pathological features of thyroid cancer as observed in five referral hospitals in Iran. Acta Oncol. 2003;42(4):334–7.
Farzadfar F, Peykari N, Larijani B, Rahimzadeh S, Rezaei-Darzi E, Saeedi MS. A comprehensive study on national and sub national trend in thyroid cancer prevalence in the iranian population, 1990–2010. Iranian Journal of Diabetes and Metabolism. 2016;15(2):91–100.
Mohammadi E, Aminorroaya A, Fattahi N, Azadnajafabad S, Rezaei N, Farzi Y, et al. Epidemiologic pattern of cancers in Iran; current knowledge and future perspective. J Diabetes Metab Disord. 2020. https://doi.org/10.1007/s40200-020-00654-6.
Rahbari R, Zhang L, Kebebew E. Thyroid cancer gender disparity. Future Oncol. 2010;6(11):1771–9.
Song H-J, Qiu Z-L, Shen C-T, Wei W-J, Luo Q-Y. Pulmonary metastases in differentiated thyroid cancer: efficacy of radioiodine therapy and prognostic factors. Eur J Endocrinol. 2015;173(3):399–408.
Sampson E, Brierley JD, Le LW, Rotstein L, Tsang RW. Clinical management and outcome of papillary and follicular (differentiated) thyroid cancer presenting with distant metastasis at diagnosis. Cancer. 2007;110(7):1451–6.
Acknowledgements
In Memory of Professor Mohammad Hasan Bastan Hagh.
Prof. Mohammad Hasan Bastan Hagh was the founder of the Thyroid Research Group of Endocrinology and Metabolism Research Institute of Tehran University of Medical Sciences and left long-lasting scientific attainments.
May his soul rest in peace and he will be cherished in our memories forever.
The authors would like to thanks Dr. Mahmood Naderi for his helpful suggestions and advice. Also, the authors are grateful to Ms. Rasha Atlasi for literature search.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Samimi, H., Shirzad, N., Sajjadi-Jazi, S.M. et al. Thyroid Cancer research at endocrinology and metabolism research institute (EMRI): a report of scientific activities between 2005 and 2020. J Diabetes Metab Disord (2021). https://doi.org/10.1007/s40200-020-00702-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40200-020-00702-1