Abstract
Introduction
The aim of this study was to evaluate the safety and efficacy of a violet-light filtering intraocular lens (IOL) compared to a colorless IOL control.
Methods
This was a prospective, bilateral, randomized, comparative, patient/evaluator-masked multi-center clinical trial at 12 sites in the USA. Patients underwent standard small-incision phacoemulsification cataract extraction. Visual acuity, contrast sensitivity, and color vision were tested 12 months postoperatively. Patient satisfaction and vision-related quality of life were evaluated based on directed patient responses obtained from a binocular subjective questionnaire.
Results
A total of 250 subjects were bilaterally implanted with the violet-light filtering TECNIS monofocal ZV9003 (n = 126) and colorless TECNIS monofocal ZA9003 (n = 124). Mean uncorrected distance visual acuity (UDVA) was 0.123 LogMAR for ZV9003 and 0.116 LogMAR for the ZA9003 group. Mean corrected distance visual acuity (CDVA) was 0.00 LogMAR for both groups. No significant difference was found between the groups for 22/25 questionnaire categories, including color perception. A significant difference was found in favor of the ZV9003 group for day driving, night driving, and frustration with vision. Contrast sensitivity mean difference was < 0.05 log units across all lighting conditions and spatial frequencies.
Conclusion
No difference was found between groups for visual acuity, contrast sensitivity, color testing, and adverse events as well as with the majority of optical/visual symptoms. A statistical difference was noted in driving and frustration with eyesight that may be related to benefits of using a violet-light filtering chromophore. Overall, the violet-light filtering ZV9003 showed excellent visual acuity and contrast sensitivity results with a low incidence of optical/visual symptoms.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Intraocular lenses (IOLs) that filter high-energy visible light were introduced in the 1990s and have become increasingly popular. As the use of these lenses continue to grow, it is important to characterize the impact it has on patients. |
This clinical study evaluated the safety and efficacy of a violet-light filtering (referred to as OptiBlue) IOL (ZV9003) compared to a clear/colorless control (ZA9003). |
Overall, the OptiBlue violet-light filtering ZV9003 IOL provided patients with a safe and effective outcome with a low incidence of optical/visual symptoms. |
Both OptiBlue ZV9003 and clear ZA9003 IOLs provided excellent visual acuity and contrast sensitivity. Additionally, patients with the OptiBlue violet-light filtering ZV9003 IOL reported an improvement in daytime and nighttime driving vision as well as less overall “frustration with vision” compared to the clear control. |
Introduction
Intraocular lenses (IOLs) with UV-filtering chromophores were introduced in the early 1980s, and IOLs that absorb or filter high-energy visible light were introduced in the 1990s [1, 2]. These lenses have become increasingly popular over the past 30 years.
The filtering of any visible light needs careful consideration because of the trade-off between visual performance and protection against phototoxicity [3,4,5]. The theoretical disadvantages of implanting a high-energy visible light (also referred to as short-wavelength) filtering IOL have been raised over the last 25 years. Concerns or disadvantages that have been expressed around filtering high-energy visual light include patients noticing a blue tint after IOL implantation and a possible disruption of the circadian system. Benefits or advantages that have been discussed include a decreased glare and possible protection of retinal health due to evidence that short wavelength light may be harmful to the retina. While there is now a better understanding of the issues involved [3, 6,7,8,9,10,11,12], additional work is still needed to bridge the gaps in understanding the technology. For example, there is a gap in understanding of how the use of short-wavelength filtering chromophores in IOLs affects light scatter, scotopic vision, and color perception. There is also a lack of standardized nomenclature around how and what light is being filtered [4].
As high-energy/short-wavelength light filtering IOLs have become more popular, there have been many studies showing excellent visual outcomes and safety profile [13,14,15,16]. The current study was designed to evaluate the safety and effectiveness of the TECNIS® Monofocal Intraocular Lens, Model ZV9003 (Johnson & Johnson Vision, Irvine, CA, USA) modified light transmission [violet-light filtering (VLF)] acrylic IOL compared to the colorless TECNIS® Monofocal Intraocular Lens, Model ZA9003 (Johnson & Johnson Vision, Irvine, CA, USA).
Methods
Material
The ZV9003 is a three-piece ultraviolet filtering hydrophobic acrylic intraocular lens based on the TECNIS® acrylic IOL, Model ZA9003. The addition of a chromophore blocks 90% of wavelengths up to 428 nm, thus filtering short-wavelength violet light while allowing transmission of the blue light that is crucial to scotopic vision. The material and dimensions for the violet-light filtering (also referred to as OptiBlue or SENSAR-UV2) lens as well as the colorless control lens can be seen in Table 1. Both lenses are posterior chamber three-piece monofocal aspheric acrylic foldable lenses designed to be implanted in the capsular bag following phacoemulsification cataract extraction.
Study Design
This prospective, bilateral, randomized, comparative, patient-masked/evaluator-masked multicenter study was conducted at 12 investigational sites in the US between December 2006 and February 2008 (clinicaltrials.gov NCT00747227; retrospective registration). The study was approved by the regulatory and institutional review board (RCRC IRB) and was conducted in accordance with the US Code of Federal Regulations, the Declaration of Helsinki, and all other applicable laws and regulations. All patients provided written informed consent and signed the Authorization for Use/Disclosure of Health Information Form (HIPAA authorization) or similar medical treatment privacy law documentation before enrolling in the study.
Patients
Target enrollment was approximately 250 patients, randomized 1:1 to receive either the ZV9003 study lens or ZA9003 control lens bilaterally. The study included only patients undergoing bilateral primary cataract extraction and lens implantation. All patients underwent a full ophthalmic examination. The study included only patients who met all inclusion and exclusion criteria including preoperative corrected distance visual acuity (CDVA) worse than 20/40, corneal astigmatism of 1.5 D or less, and visual potential of 20/30 or better as determined by the surgeon. In addition, the Farnsworth-Munsell D-15 and Ishihara color perception tests were administered. Patients had to pass both color perception tests to be included in the study. For each study subject enrolled, the investigator opened a sequentially numbered sealed envelope (provided by the Sponsor biostatistician) on the day of surgery. The envelope contained the subject's randomization assignment to one of the two intraocular lens groups, the ZV9003 study lens or the ZA9003 control lens. The randomly assigned lens was implanted in the subject’s first eye. The same type of lens was then implanted in the subject’s fellow eye (Fig. S1).
Surgical Procedure
The lens power was selected to achieve emmetropia for all eyes. Surgeons used a standard small-incision, phacoemulsification cataract extraction surgical technique. Viscoelastic materials and preoperative and intraoperative medications were used as customary for each investigator. A routine medication regimen form was completed by each investigator; any deviations were reported on the operative case report form. If a surgical complication occurred, such as a capsular bag or zonular rupture, the study lens was not implanted, and the patient was to be exited from the study.
Postoperative Assessment
Postoperative uncorrected distance visual acuity (UDVA) and corrected distance visual acuity (CDVA) were measured using the ETDRS self-calibrating, retroilluminated box at a distance of 4 m (13 feet) with the 100% ETDRS acuity chart. Contrast sensitivity was measured using Vector Vision illumination box and CSV-1000 contrast sensitivity sine wave chart. Measurements were taken under both photopic and mesopic lighting conditions for 3.0, 6.0, 12.0, and 18.0 cycles per degree (cpd). Patient satisfaction and vision-related quality of life were evaluated based on patient responses to subjective questionnaires (National Eye Institute Visual Functioning Questionnaire-25 (VFQ-25). The questionnaires were administered via telephone by masked interviewers preoperatively and at the 12-month postoperative visit. Patient satisfaction and vision-related quality of life was evaluated based on patient responses to subjective questionnaires. Responses for each questionnaire category included possibilities such as ‘No difficulty at all,’ ‘A little difficulty,’ ‘Moderate difficulty,’ ‘Extreme difficulty,’ ‘Stopped because of eyesight,’ ‘Stopped for other reasons,’ and ‘Not reported.’
Statistical Analyses
The sample size of 125 subjects for the study lens was based upon the minimum sample size of 100 subjects required for a Level B modification of a parent IOL when compared to the historical control population. Additional subjects were added to account for screen failures and subjects lost to follow-up.
The primary effectiveness endpoint in this study was postoperative CDVA. Visual acuity outcomes are reported using ‘first-eye’ data unless otherwise stated. IOL group means were compared using a two-sample t-test. Additional descriptive statistics included frequency and proportion of eyes achieving each acuity line over time. Contrast sensitivity was evaluated by determining if the one-sided 95% confidence interval of the mean was within 0.15 log units of the control IOL (or lower value of a two-sided 90% confidence interval is within 0.15 log units). For questionnaire responses, comparisons between IOL groups were performed using the Wilcoxon rank-sum test for ordinal data, and the Pearson chi-square test or Fisher’s exact test (for small samples) was used for categorical data. Data from the 12-month postoperative visit were used for analysis.
The primary safety endpoints were complication and adverse event rates during the study. These rates were compared to the rates of the FDA’s historical control group (FDA Grid rates). The frequency and proportion of patients experiencing any complication or adverse event were reported over time.
Results
A total of 250 patients (126 ZV9003 patients and 124 ZA9003 patients) were enrolled between December 2006 and February 2008. The 12-month visit was completed by 120 ZV9003 patients and 120 ZA9003 patients. Table 2 shows the demographic data for the study population.
Surgical Procedure
All study eyes underwent standard small-incision, phacoemulsification cataract extraction surgery and folded intraocular lens implantation. All lenses were implanted in the capsular bag except for five ZV9003 eyes and two ZA9003 eyes that were implanted in the sulcus. Five ZV9003 patients (all second eyes) underwent additional surgical procedures. Three patients had a vitrectomy performed during IOL implantation, one patient had a surgical capsulotomy, and one patient had a lesion removed from the upper lid. Two ZA9003 patients underwent a secondary surgical procedure. One patient had a vitrectomy in the first eye, and one patient had a pupiloplasty in the second eye.
Visual Acuity
The mean UDVA was 0.123 LogMAR in the ZV9003 group and 0.116 LogMAR in the ZA9003 group. The mean difference between IOL groups was within a tenth of a line with the lower level of the 90% confidence interval within half a line. The mean CDVA was 0.00 LogMAR for both groups. The mean difference between IOL groups was within a quarter line with the lower level of the 90% confidence interval within half a line. There was no clinical or statistical difference between groups for UDVA or CDVA. Cumulative Snellen uncorrected and corrected visual acuity was also similar between lens groups (Fig. 1).
Patient Satisfaction
The questionnaire response categories are shown in full in Table S1. No significant difference was found between the two lens groups for most categories assessed (see Table S1). Notably, no significant difference was found in color vision, with 94.1% (111/118) of ZV9003 patients and 90.8% (108/119) of ZA9003 patients reporting no problem picking out or matching their own clothes (p = 0.7729).
A statistically significant difference was found between IOL groups favoring the ZV9003 group for daytime (p = 0.0330) and nighttime driving (p = 0.0169) as well as frustration with vision (p = 0.0325) (Fig. 2). A breakdown of the patient responses showed that most patients in either group [98.1% (106/108) of the ZV9003 and 91.7% (99/108) of the ZA9003] reported no difficulty at all with daytime driving, and one ZV9003 patient (0.9%, 1/108) reported a little difficulty while nine ZA9003 patients (8.3%, 9/108) reported a little difficulty. For night driving, 52.8% (57/108) of patients in the ZV9003 group and 44.4% (48/108) of patients in the ZA9003 group reported no difficulty at all, while 29.6% (32/108) of patients in the ZV9003 group and 40.7% (44/108) of patients in the ZA9003 group reported a little difficulty. A statistically significant difference was also found for ‘frustration a lot of the time because of eyesight.’ When asked how true the statement was, 89.1% (106/119) in the ZV9003 group and 80.5% (95/118) of subjects in the ZA9003 group reported definitely false, while 6.8% (8/118) in the ZV9003 group and 12.5% (15/119) in the ZA9003 group reported mostly false.
Contrast Sensitivity
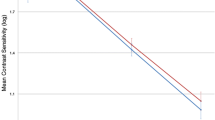
Binocular best-corrected distance contrast sensitivity testing was conducted at the 6-month postoperative visit on 120 patients implanted with ZV9003 and 119 patients implanted with ZA9003. Mean contrast sensitivity results were similar for the two IOL groups. Mean differences between IOL groups ranged between 0.00 and 0.05 log units. Under both lighting conditions and at all spatial frequencies, the lower limit of the 90% confidence interval was at or below 0.14 log units for both lens types, thus demonstrating similar results between IOL groups. Mean binocular log contrast sensitivity results for all patients are shown in Tables 3 and 4.
Medical Findings
The most frequently reported medical finding was posterior capsule opacification (PCO). At 12 months, 27% of eyes in the ZV9003 group and 33% of eyes in the ZA9003 group had some degree of PCO. One patient in each group underwent a Nd:YAG capsulotomy prior to the 6-month visit. The second highest reported medical finding was vitreous detachment, found in 13% of eyes in the ZV9003 group and 9% of eyes in the ZA9003 group. There were no reports of retinal detachment at the 12-month postoperative visit in either group. One ZA9003 first eye underwent laser treatment to repair a retinal tear, and one ZV9003 second eye underwent cryopexy to repair a retinal tear. Both events were resolved without sequelae.
Discussion
The ZV9003 VLF IOL was shown to be similar to the ZA9003 colorless lens counterpart. Both models showed excellent distance visual acuity results. The similarity in visual acuity between lens groups (short wavelength or high energy visible light filtering lens versus a colorless control) is also consistent with findings of other published comparative trials [15, 17,18,19].
While visual acuity was similar between groups, it is important to understand the relationship between filtering high-energy light and the broader visual experience. This relationship is important since the goal of using light filtering chromophores is to balance photoreception and photoprotection with the intention of providing patients with excellent visual results while helping to protect eye health [4].
In addition to visual acuity, subjective feedback on activities of daily living and visual disturbances helps to determine the overall visual outcomes for a patient. Questionnaire feedback on driving showed that while patients in both groups (VLF and colorless control) had no or only a little difficulty driving during the day, a statistically significant difference was found in favor of the ZV9003 VLF group. In addition to an improvement in daytime driving, there was a statistically significant difference in nighttime driving in favor of the ZV9003 group as well. The results showing a fewer number of patients in the VLF group reporting difficulty with daytime and nighttime driving may be due to an improvement in or maintenance of visual quality under specific driving conditions [20]. Gray et al. found that patients implanted with a blue light filtering IOL had significantly lower glare susceptibility and safety execution when performing turns while driving in low light conditions [21]. However, as mentioned previously, the majority of patients in both groups reported relatively low difficulty when driving. Additional studies are necessary to confirm the findings in the current population and other previously published reports.
A statistically significant difference was also found for the question related to frustration with eyesight. ZV9003 patients reported less frustration with their eyesight compared to ZA9003 control patients. Frustration with vision may be related to the concept of “visual comfort,” which is an important consideration in the adoption of short-wavelength filtering IOLs, glasses, and contact lenses [22]. Zhao et al. reported that short-wavelength filtering lenses removed glare-related light components from natural light, resulting in comfortable vision [20]. While the current study did find a statistical difference between the two IOL groups, most patients in both groups indicated that they did not experience frustration with eyesight.
Although differences were noted between lens groups for three questions, patients in both IOL groups reported similar results related to their ability to perform vision-related activities and their degree of satisfaction with their eyesight. This included distinguishing colors through picking out and matching clothes. There was also no statistical difference between groups for color vision testing; 99.2% (118/119) of ZV9003 patients and 95.8% (115/120) of ZA9003 passed the color vision test at the 12-month visit, which indicates similar relative color discrimination particularly in the red/green spectrum but may not be reflective of overall color perception. Similarly, Bhattaacharjee et al. found no difference in color perception when comparing the AcrySof Natural IOL vs. AcrySof IOL (Alcon Inc, Fort Worth, TX) [15]. Wirtitsch et al. and Yuan et al. also found no difference in color vision between Hoya (Hoya Medical, Frankfurt, Germany) blue-light filtering and colorless IOLs [17, 19]. Additional specific color perception testing in the blue/violet range might identify a difference between lens groups, but the impact on a patient’s visual experience remains unclear.
The effect of short-wavelength filtering lenses on contrast sensitivity has also been discussed in the literature [15, 17,18,19, 23, 24]. As with the current study, Schmack et al., Mester et al., and Schmidinger et al. found no difference when comparing contrast sensitivity between short-wavelength filtering and colorless IOLs [18, 23, 24]. While the aforementioned studies found no difference, there were a number of studies that showed a minor difference between groups. Yuan et al. showed a statistically higher special contrast sensitivity at low and middle frequencies (1.5, 3, and 6 cpd) in the HOYA (Tokyo, Japan) blue-light filtering IOL group compared to the colorless IOL, and Bhattacharjee et al. found the AcrySof Natural IOL group was better than the colorless AcrySof IOL group when each group was compared separately to similarly aged phakic individuals with colorless lenses [15, 19]. The difference in contrast sensitivity results between studies may be due, in part, to lens material differences such as the chromatic aberration profile [25]. A lens with high chromatic aberration may benefit from short-wavelength light filtering as it will reduce the overall dispersion within the eye, whereas a lens with low chromatic aberration is likely to see little improvement in contrast sensitivity with the filtration of short-wavelength light.
The main limitation of the current study was that specific color vision testing was not performed clinically or addressed in detail in the subject questionnaire. Testing under specific lighting conditions and adding additional questions relating to color discrimination and visual comfort may help identify subtle differences between lens groups. Another limitation to note was that evaluation of visual acuity and visual performance indicators such as defocus curve testing and any correlation between residual uncorrected astigmatism and driving performance may have provided additional insight to differences between groups.
Conclusions
In conclusion, no difference was found between lens groups for visual acuity, contrast sensitivity, color testing, adverse events, and the majority of optical/visual symptoms. A statistical difference was noted in driving and frustration with eyesight that may be related to benefits of using a violet-light filtering chromophore. However, these differences require additional studies to better understand the clinical implications. Overall, the ZV9003 VLF IOL showed excellent visual acuity and contrast sensitivity results with a low incidence of optical/visual symptoms.
References
Mainster MA. The spectra, classification, and rationale of ultraviolet-protective intraocular lenses. Am J Ophthalmol. 1986;102(6):727–32.
Lindstrom RL, Doddi N. Ultraviolet light absorption in intraocular lenses. J Cataract Refract Surg. 1986;12(3):285–9.
Downes SM. Ultraviolet or blue-filtering intraocular lenses: what is the evidence? Eye (Lond). 2016;30(2):215–21.
Chang D, Pastuck T, Rosen R, Hollman S, Babic T, Stapars A. Violet and blue light: impact of high-energy light on vision and health. J Ophthalmic Stud. 2020;3(2).
Mainster MA. Spectral transmittance of intraocular lenses and retinal damage from intense light sources. Am J Ophthalmol. 1978;85(2):167–70.
Mainster MA. Violet and blue light blocking intraocular lenses: photoprotection versus photoreception. Br J Ophthalmol. 2006;90(6):784–92.
Mainster MA, Turner PL. Blue-blocking IOLs decrease photoreception without providing significant photoprotection. Surv Ophthalmol. 2010;55(3):272–89.
Henderson BA, Grimes KJ. Blue-blocking IOLs: a complete review of the literature. Surv Ophthalmol. 2010;55(3):284–9.
Cuthbertson FM, Peirson SN, Wulff K, Foster RG, Downes SM. Blue light-filtering intraocular lenses: review of potential benefits and side effects. J Cataract Refract Surg. 2009;35(7):1281–97.
Schmoll C, Khan A, Aspinall P, Goudie C, Koay P, Tendo C, et al. New light for old eyes: comparing melanopsin-mediated non-visual benefits of blue-light and UV-blocking intraocular lenses. Br J Ophthalmol. 2014;98(1):124–8.
Ichikawa K. Changes in blood pressure and sleep duration in patients with blue light-blocking/yellow-tinted intraocular lens (CHUKYO study). Hypertens Res. 2014;37(7):659–64.
Brøndsted AE, Haargaard B, Sander B, Lund-Andersen H, Jennum P, Kessel L. The effect of blue-blocking and neutral intraocular lenses on circadian photoentrainment and sleep one year after cataract surgery. Acta Ophthalmol. 2017;95(4):344–51.
Downie LE, Busija L, Keller PR. Blue-light filtering intraocular lenses (IOLs) for protecting macular health. Cochrane Database Syst Rev. 2018;5(5):Cd011977.
Barisić A, Dekaris I, Gabrić N, Bosnar D, Lazić R, Martinović ZK, et al. Blue light filtering intraocular lenses in phacoemulsification cataract surgery. Coll Antropol. 2007;31(Suppl 1):57–60.
Bhattacharjee H, Bhattacharjee K, Medhi J. Visual performance: Comparison of foldable intraocular lenses. J Cataract Refract Surg. 2006;32(3):451–5.
Espindle D, Crawford B, Maxwell A, Rajagopalan K, Barnes R, Harris B, et al. Quality-of-life improvements in cataract patients with bilateral blue light-filtering intraocular lenses: clinical trial. J Cataract Refract Surg. 2005;31(10):1952–9.
Wirtitsch MG, Schmidinger G, Prskavec M, Rubey M, Skorpik F, Heinze G, et al. Influence of blue-light-filtering intraocular lenses on color perception and contrast acuity. Ophthalmology. 2009;116(1):39–45.
Schmack I, Schimpf M, Stolzenberg A, Conrad-Hengerer I, Hengerer FH, Dick HB. Visual quality assessment in patients with orange-tinted blue light-filtering and clear ultraviolet light-filtering intraocular lenses. J Cataract Refract Surg. 2012;38(5):823–32.
Yuan Z, Reinach P, Yuan J. Contrast sensitivity and color vision with a yellow intraocular len. Am J Ophthalmol. 2004;138(1):138–40.
Zhao HL, Jiang J, Yu J, Xu HM. Role of short-wavelength filtering lenses in delaying myopia progression and amelioration of asthenopia in juveniles. Int J Ophthalmol. 2017;10(8):1261–7.
Gray R, Hill W, Neuman B, Houtman D, Potvin R. Effects of a blue light-filtering intraocular lens on driving safety in glare conditions. J Cataract Refract Surg. 2012;38(5):816–22.
Hammond MD, Potvin R. Visual outcomes, visual quality and patient satisfaction: comparing a blended bifocal approach to bilateral extended depth of focus intraocular lens implantation. Clin Ophthalmol (Auckland, NZ). 2019;13:2325–32.
Mester U, Holz F, Kohnen T, Lohmann C, Tetz M. Intraindividual comparison of a blue-light filter on visual function: AF-1 (UY) versus AF-1 (UV) intraocular lens. J Cataract Refract Surg. 2008;34(4):608–15.
Schmidinger G, Menapace R, Pieh S. Intraindividual comparison of color contrast sensitivity in patients with clear and blue-light-filtering intraocular lenses. J Cataract Refract Surg. 2008;34(5):769–73.
Tavazzi S, Ponzini E, Caridi A, Secreti S, Miglio F, Duse A, et al. Does blue-violet filtering in contact lenses improve contrast sensitivity? Contact Lens Anterior Eye J Br Contact Lens Assoc. 2022;45(5):101558.
Acknowledgements
Funding
This study and the journal’s Rapid Service Fee was supported by Johnson & Johnson Surgical Vision, Inc., which participated in the design and conduct of the study.
Author Contributions
DHC: Concept and design of the study and review and editing of draft; VMT: Concept and design of the study and review and editing of draft; WCC: Concept and design of the study and review and editing of draft; YRC: Concept and design of the study and review and editing of draft; RSV: Data analysis and drafted the original manuscript.
Disclosures
The authors have made the following disclosures: Daniel H Chang: Investigator and consultant for Johnson & Johnson Surgical Vision, Inc., and an investigator for AcuFocus; Vance M Thompson: Consultant and researcher for Alcon, Bausch & Lomb, BVI, Johnson & Johnson Surgical Vision, Rayner and Zeiss; William C Christie: Consultant for Johnson & Johnson Surgical Vision and Abbvie; Y Ralph Chu: No financial disclosures; Ryan S Vida: Employee of Johnson & Johnson Surgical Vision. The authors report no other conflicts of interest in this work.
Compliance with Ethics Guidelines
The study was approved by the regulatory and institutional review board (RCRC IRB) and was conducted in accordance with the US Code of Federal Regulations, the Declaration of Helsinki, and all other applicable laws and regulations. All patients provided written informed consent and signed the Authorization for Use/Disclosure of Health Information Form (HIPAA authorization) or similar medical treatment privacy law documentation before enrolling in the study.
Data Availability
The authors do not intend to share individual deidentified participant data. A summarized report with endpoints data tables based on statistical plan and analysis may be requested directly from the corresponding author for consideration. Access to anonymized data may be granted following review. Content with granted access will be available through email or other appropriate formats and for 3 months, upon review and consideration.
Author information
Authors and Affiliations
Corresponding author
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Chang, D.H., Thompson, V.M., Christie, W.C. et al. Clinical Evaluation of a Modified Light Transmission Short-Wavelength Filtering Intraocular Lens Compared to a Colorless Control. Ophthalmol Ther 12, 1775–1785 (2023). https://doi.org/10.1007/s40123-023-00709-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40123-023-00709-w