Abstract
Purpose
The feasibility, in terms of safety and potential efficacy, of a new drug combination for binocular use as a noninvasive pharmacological solution for treating presbyopia was examined.
Methods
Fourteen emmetropic presbyopic subjects (28 eyes) were given one drop of the preparation under study in each eye. For each patient, the uncorrected distance visual acuity, uncorrected near visual acuity, near and far refraction, best corrected visual acuity, best corrected far-near visual acuity, photopic and scotopic pupil size, Schirmer’s test, endothelial cell count, intraocular pressure, keratometry, pachymetry, and anterior chamber depth were all performed or assessed prior to the administration of the eye drops and then 0.5, 1, 2, 3, 4, and 5 h, 1 week, and 1 month post-administration prospectively in each eye and binocularly.
Results
The results showed that near uncorrected visual acuity improved by about 2–3 lines from baseline in each eye and binocularly. There was no degradation in uncorrected far vision in each eye and binocularly in any patient. Refractive measurements performed in this study showed there was a maximum myopic shift of just 0.5 D that progressively reduced and disappeared at 4 h.
Conclusion
The new topical drug treatment analyzed herein significantly improved near vision without affecting far vision. This binocular pharmacologic treatment of presbyopia has the potential to ameliorate the reading vision of presbyopes and possesses the advantages of a nonmonovision therapy. A randomized, controlled, double-masked clinical trial with a twice-a-day treatment schedule is ongoing at our institution.
Funding
This study was supported in part by the Spanish Ministry of Health, Instituto Carlos III, Red Temática de Investigación Oftalmológica (OFTALRED), and Fundación Oftalmológica Vejarano (Popayán, Colombia).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Presbyopia, which is due to progressive age-related accommodative loss, begins to affect near visual tasks at around 40 years of age, and is associated with substantial negative effects on vision-targeted health-related quality of life [1]. In 2015, more than 2.5 billion people around the world were aged 40 years or older; given that the global population is growing and ageing, presbyopia will affect even more people in the future [2]. However, the pathophysiology of presbyopia is poorly understood, so the correction of presbyopia and the restoration of accommodation are among the most important targets of ophthalmology research. Although surgical compensation for presbyopia has improved over the past decade, it is still limited, so there has recently been increasing interest in nonsurgical treatments [3]. Topical treatment of presbyopia is an attractive approach which, if available and effective, would be the treatment of choice for many patients. The few potential topical treatments for presbyopia that are currently being studied claim to work on different aspects of the accommodative process, but each of these approaches presents some disadvantages [4–7]. The topical treatment presented herein contains a parasympathetic, a NSAID, two alpha-agonist agents, and an anticholinesterase agent, is administered bilaterally, and promises to ameliorate the symptoms of presbyopia through pharmacological stimulation of iris and ciliary muscle, thus minimizing the drawbacks associated with a purely parasympathetic action [8]. Here, we report the initial outcomes obtained in a pilot investigation with the new drug combination for binocular use in presbyopic patients.
Methods
This pilot study was begun after approval was obtained from the ethics committee of Fundación Oftalmológica Vejarano in Popayán, Colombia. Each participant provided written informed consent, and the study followed the tenets of the Declaration of Helsinki. The pharmacological stimulation protocol was developed and submitted for patent in 10 countries by Dr. Vejarano, who had been using his own product and achieving satisfactory results with it for five and a half years previously (since July 2010) [9]. The study group comprised 14 presbyopic subjects (28 eyes): 9 natural emmetropes and 5 stable emmetropes post LASIK surgery, with an average age of 48.21 years (range 41–55 years). Participants were randomly selected volunteers. Presbyopia was considered to be present if the patient needed to use a spectacle lens ≥ +1.00 D to read a print size of Jaeger 0.8. Each subject was given only one drop of the ophthalmic formulation containing pilocarpine 0.247%, phenylephrine 0.78%, polyethyleneglycol 0.09%, nepafenac 0.023%, pheniramine 0.034%, and naphazoline 0.003% in each eye. All of the drugs administered in this study are approved by the US Food and Drug Administration and have been used for years as safe and effective agents for treating ocular pathologies. Various ophthalmologic measurements were taken prior to the administration of the eye drops and then 0.5, 1, 2, 3, 4, and 5 h, 1 week, and 1 month post administration in each eye and binocularly. The measurements, which were performed by the same independent examiner in the same room with the same instruments, included uncorrected distance (UDVA) and near (UNVA) visual acuity, far and near refraction, best spectacle-corrected distance (CDVA) and near (CNVA) visual acuity, near visual acuity with best far spectacle correction (CFNVA), photopic and scotopic pupil size, Schirmer’s test, endothelial cell count, intraocular pressure, keratometry, pachymetry, and anterior chamber depth. Distance visual acuity was measured using the standard Snellen projector chart at 4 m. Near visual acuity was assessed at 40 cm using a hand-held Rosenbaum chart with Jaeger notation, always employing the same luminosity of 160 cd/m2. Pupil diameter was measured using an AL-Scan optical biometer (Nidek Co., Ltd., Japan), a Pentacam (Oculus Optikgeräte GmbH, Germany), and an auto ref/keratometer (Nidek Co., Ltd.). ECC was measured using a CellCheck clinical specular microscope (Konan Medical Inc., Japan). Intraocular pressure was measured with a Goldmann AT-900 applanation tonometer (Haag-Streit AG, Switzerland) and a Pascal dynamic contour tonometer (Ziemer Ophthalmic Systems AG, Switzerland). Keratometry was performed using the auto ref/keratometer (Nidek Co.). Pachymetry and anterior chamber depth were measured with the Pentacam (Oculus Optikgeräte GmbH). The inclusion criteria applied admitted patients who were aged between 40 and 65 years, emmetropic (cycloplegic spherical equivalent, ±1.00 D; astigmatism, ≤0.50 D), had a binocular UDVA of at least 20/25, and had no additional ocular or systemic pathology. None of the patients included in the study had received any chronic mydriatic or miotic therapy previously. During the study, the subjects were closely monitored and regularly asked to report the grade of satisfaction and any adverse effects; although this pilot study was designed to assess the feasibility of applying a single drop to each eye, the topical formulation is intended to for twice-daily use: once in the morning and once in the afternoon before performing near visual tasks. Due to the characteristics of the data, a Friedman test was run to determine if there were any significant changes in the values of the monitored variables during the study period (from 30 min to 1 month after administration) in the analyzed eyes. Pairwise comparisons were performed with a Bonferroni correction for multiple comparisons (SPSS, 2015) to compare the post-instillation data with baseline.
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964, as revised in 2013. Informed consent was obtained from all patients before they were included in the study.
Results
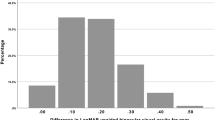
Table 1 summarizes the data for some variables of particular interest. Figures 1, 2, 3, and 4 present the time trends for the variables, which show significant changes from 30 min to 1 month after administration. Pairwise comparisons (Bonferroni corrected) were performed between the post- and pre-administration values of each variable, and significant differences are marked by asterisks (*) in the figures. Statistically significant changes in photopic pupil diameter (χ 2(8) = 68.581, p < 0.001), scotopic pupil diameter (χ 2(8) = 30.856, p < 0.001), intraocular pressure (χ 2(8) = 52.507, p < 0.001), CFNVA (χ 2(8) = 22.467, p < 0.004), binocular CFNVA (χ 2(8) = 61.685, p < 0.001), UDVA (χ 2(8) = 20.358, p < 0.009), UNVA (χ 2(8) = 95.324, p < 0.001), binocular UNVA (χ 2(8) = 101.205, p < 0.001), binocular UDVA (χ 2(8) = 37.989, p < 0.001), spherical equivalent (χ 2(8) = 118.524, p < 0.001), and best near addition (χ 2(8) = 25.213, p < 0.001) were observed. However, clinically relevant improvements over time were only observed in binocular UNVA (Fig. 2c), with an improvement of ≥3 lines noted at 5 h in 6 patients (42.9% of the total); UNVA (Fig. 3b), with an improvement of ≥3 lines seen at 5 h in 7 patients (50.0% of the total); and spherical equivalent (Fig. 4b), with an improvement obtained at 3 h (0.32 ± 0.55 versus 0.03 ± 0.54). Notably, binocular (Fig. 2a) and monocular (Fig. 3a) UDVA did not show clinically relevant changes. Pupil diameter was significantly increased under photopic conditions until the first hour had elapsed after adminstration, and was significantly decreased under scotopic conditions between 4 and 5 h after instillation of the topical treatment. Patient satisfaction was probed by asking them if they were still enjoying the improved near vision that they had after the eye drops were applied, and whether they would like to continue using the eye drops in order to maintain this enhanced near vision. All patients answered affirmatively to the question. No adverse effects were reported.
Trends in best near addition (a), monocular (b), and binocular (c) near visual acuity with best far spectacle correction over time from 30 min to 1 month after instillation of the eye drops into the 28 studied eyes. Asterisks indicate values that are significantly different from the baseline. Best near addition and monocular near visual acuity with best far spectacle correction did not show any statistically significant changes. Binocular near visual acuity with best far spectacle correction only showed significant changes at 4 h post-instillation and at 1 month post-instillation
Trends in binocular far uncorrected visual acuity (a), defocus equivalent (b), and binocular near uncorrected visual acuity (c) over time from 30 min to 1 month after instillation of the eye drops into the 28 studied eyes. Asterisks indicate values that are significantly different from the baseline. Binocular far uncorrected visual acuity and defocus equivalent did not show any statistically significant changes. Binocular near uncorrected visual acuity gradually improved over the course of 5 h following eye drop instillation
Trends in monocular far (a) and near (b) uncorrected visual acuity and intraocular pressure (c) over time from 30 min to 1 month after instillation of the eye drops into the 28 studied eyes. Asterisks indicate values that are significantly different from the baseline. Intraocular pressure was only significantly lower at 5 h after eye drop instillation. Far uncorrected visual acuity did not show any statistically significant changes. Near uncorrected visual acuity gradually improved over the course of 5 h following eye drop instillation
Trends in photopic pupil diameter (a), spherical equivalent (b), and scotopic pupil diameter (c) over time from 30 min to 1 month after instillation of the eye drops into the 28 studied eyes. Asterisks indicate values that are significantly different from the baseline. Pupil diameter under photopic conditions increased significantly for the first hour. Under scotopic conditions, pupil diameter did not change significantly until 3 h after eye drop instillation, and it then significantly decreased between 4 and 5 h after instillation. Spherical equivalent improved for 3 h following eye drop instillation
Discussion
Several studies have been conducted to determine how much each factor involved in the accommodative process contributes to it [10–14]. The few topical treatments for presbyopia currently under study claim to work on different aspects of the accommodative process: they involve monovision parasympathetic-mediated miosis and ciliary muscle stimulation or lens softening in order to restore its shape-changing ability [4–7]. Each of these approaches presents some disadvantages. Pure parasympathetic treatments result in a rather small pupil diameter and a myopic shift, compromising far distance vision, and they also cause several well-known adverse reactions due to the muscarinic stimulation of ciliary muscle and pupil sphincter [5]. Even a safe lens-softening treatment could be less effective than expected because changes in mechanical properties seem to be less important in the advent and progression of presbyopia than changes in lens geometry [12]. A monovision treatment could reduce visual performance in reduced light conditions compared to a binocular approach [14]. For this reason, the treatment used in our pilot study is instilled in both eyes. The Vejarano (patent pending) eye drops both stimulate the contraction of the ciliary body and maintain a physiological pupil diameter variation. In this context, binocular treatment avoids the worsening of visual performance in reduced light and allows physiological image merging with clear focus at near, intermediate, and distance. Pilocarpine provides both miosis and ciliary body contraction, stimulating accommodation, and may improve tear production by stimulating lacrimal gland secretion [15]. Phenylephrine, nepafenac, and pheniramine, each in different ways and amounts, stop excess pupil constriction and counteract ciliary muscle spasm, vascular congestion, and hyperemia induced by pilocarpine [6, 16–18]. Naphazoline intensifies the relaxing effect of pilocarpine on dilator pupillae while relieving its side effects, increasing acetylcholine release and reducing norepinephrine release [18]. The lubricating effect of polyethyleneglycol makes the eye drops more tolerable by stopping the burning sensation typically caused by most of the compounds present in the eye drops. The synergistic effect observed by Vejarano between these compounds permits improved near vision and preserves distance vision in all subjects. The synergism reduces symptoms of headache and hyperemia, allowing lower doses of miotics to be used. There was no evidence of tachyphylaxis in this study. No ocular complications were detected in any of the treated eyes during the entire follow-up period. The results showed that UNVA improved by about 2–3 lines in each eye and binocularly from a baseline mean of about J 3.5 to about J 1.5. No patient presented any UDVA degradation in an eye or binocularly. Whereas other drops for treating presbyopia improve near vision by causing extreme miosis or a myopic shift that can reduce far vision [5], refractive measurements performed in this study showed there was a maximum myopic shift of just 0.5 D, which progressively reduced and disappeared after 3 h. Pupil diameter was also measured and found to be mildly affected by the topical treatment, so the mechanism for near vision improvement might be due to factors other than miosis. However, we cannot clarify this issue based on the evidence provided by the present study, so a controlled study of a larger number of patients in which the dynamic changes in refraction are investigated objectively is required. Moreover, the measurements showed that the treatment seemed to mitigate significant pupil enlargement under scotopic conditions as well as significant contraction under photopic conditions. Other assessments showed that there were no clinical changes in tear film quality or quantity or in endothelial cell count, showing that the eye drops had no adverse effects on the lacrimal film, corneal epithelium, or endothelial cells. The study also showed that there was a significant decrease in intraocular pressure of almost 2 mmHg 5 h after eye drop instillation. There is clinical evidence that the trabecular meshwork stiffens with age, which leads to increased prevalence and incidence of glaucoma with age [19]. The daily movement of the scleral spur induced by the eye drops could reduce this stiffening of the trabecular meshwork, thereby suppressing the increase in glaucoma incidence with age.
Conclusion
This preparation improves near vision by 2–3 lines without affecting far vision. Binocular pharmacologic treatment of presbyopia with the Vejarano (patent pending) eye drops has the potential to ameliorate the reading vision of presbyopes and has the advantages of a nonmonovision therapy. This topical agent is noninvasive and, we believe, meets all of the criteria for an ideal treatment of presbyopia; despite the small number and the heterogeneity of the patients involved in this pilot study, its findings suggest that this treatment is very promising [20, 21]. Our group is currently conducting a randomized controlled double-masked clinical trial to test the capacity of the Vejarano eye drops to improve presbyopia.
References
McDonnell PJ, Lee P, Spritzer K, Lindblad AS, Hays RD. Associations of presbyopia with vision-targeted health-related quality of life. Arch Ophthalmol. 2003;121(11):1577–81.
U.S. Census Bureau. International data base of world population by age and sex (year 2015 selected). https://www.census.gov/population/international/data/idb/worldpop.php. Accessed 26 Jan 2016.
Charman WN. Developments in the correction of presbyopia. II: Surgical approaches. Ophthal Physiol Opt. 2014;34(4):397–426.
Abdelkader A. Improved presbyopic vision with miotics. Eye Contact Lens Sci Clin Pract. 2015;41(5):323–7.
Glasser A. Accommodation: mechanism and measurement. Ophthalmol Clin N Am. 2006;19:1–12.
Benozzi J, Benozzi G, Orman B. Presbyopia: a new potential pharmacological treatment. Med Hypothesis Discov Innov Ophthalmol. 2012;1(1):3–5.
Crawford KS, Garner WH, Burns W. Dioptin™: a novel pharmaceutical formulation for restoration of accommodation in presbyopes. Invest Ophthalmol Vis Sci. 2014;55(13):3765.
Fraunfelder FT, Fraunfelder FW, Chambers WA. Drug-induced ocular side effects. 7th ed. Philadelphia: Elsevier Saunders; 2015. p. 320–323.
Vejarano LF. Ophthalmic formulation and method for ameliorating presbyopia. US patent number 20140024642 A1. 2014.
Benozzi G, Leiro J, Facal S, Perez C, Benozzi J, Orman B. Developmental changes in accommodation evidenced by an ultrabiomicroscopy procedure in patients of Different Ages. Med Hypothesis Discov Innov Ophthalmol. 2013;2(1):8–13.
Hickenbotham A, Tiruveedhula P, Roorda A. Comparison of spherical aberration and small-pupil profiles in improving depth of focus for presbyopic corrections. J Cataract Refract Surg. 2012;38(12):2071–9.
Van De Sompel D, Kunkel GJ, Hersh PS, Smits AJ. Model of accommodation: contributions of lens geometry and mechanical properties to the development of presbyopia. J Cataract Refract Surg. 2010;36(11):1960–71.
Richdale K, Sinnott LT, Bullimore MA, et al. Quantification of age-related and per diopter accommodative changes of the lens and ciliary muscle in the emmetropic human eye. Investig Ophthalmol Vis Sci. 2013;54(2):1095–105.
Schwarz C, Manzanera S, Prieto PM, et al. Comparison of binocular through-focus visual acuity with monovision and a small aperture inlay. Biomed Opt Express. 2014;5:3355–66.
Mauduit P, Jammes H, Rossignol B. M3 muscarinic acetylcholine receptor coupling to PLC in rat exorbital lacrimal acinar cells. Am J Physiol. 1993;264:1550–60.
Yu Y, Kawarai M, Koss MC. Histamine H3 receptor-mediated inhibition of sympathetically evoked mydriasis in rats. Eur J Pharmacol. 2001;419(1):55–9.
Sarkar S, Hasnat AM, Bharadwaj SR. Revisiting the impact of phenylephrine hydrochloride on static and dynamic accommodation. Indian J Ophthalmol. 2012;60(6):503–9.
Greiner JV, Udell IJ. A comparison of the clinical efficacy of pheniramine maleate/naphazoline hydrochloride ophthalmic solution and olopatadine hydrochloride ophthalmic solution in the conjunctival allergen challenge model. Clin Ther. 2005;27(5):568–77.
Morgan JT, Raghunathan VK, Chang YR, Murphy CJ, Russel P. The intrinsic stiffness of human trabecular meshwork cells increases with senescence. Oncotarget. 2015;6(17):15362–74.
Vejarano LF. Topical drops show promise as treatment for presbyopia. Ophthalmology Times. 2016 Feb 1.
Cole J. A closer look at presbyopia. Rev Optom. 2016;153:54.
Acknowledgments
This study was supported in part by the Spanish Ministry of Health, Instituto Carlos III, Red Temática de Investigación Oftalmológica (OFTALRED), and Fundación Oftalmológica Vejarano (Popayán, Colombia).
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval of the version to be published. This study is part of the final research work of Dr. Antonio Renna in the specialization course Clinical Methodology in Refractive, Cataract and Cornea Surgery at Miguel Hernandez University, Spain, 2016.
Disclosure
Antonio Renna, Ernesto De la Cruz, and Jorge L. Alió have nothing to disclose. L. Felipe Vejarano is the inventor of the eye drops mentioned in this paper.
Compliance with ethics guidelines
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964, as revised in 2013. Informed consent was obtained from all patients before they were included in the study.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced content
To view enhance content for this article go to http://www.medengine.com/Redeem/B2C4F0603E6051FB.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Renna, A., Vejarano, L.F., De la Cruz, E. et al. Pharmacological Treatment of Presbyopia by Novel Binocularly Instilled Eye Drops: A Pilot Study. Ophthalmol Ther 5, 63–73 (2016). https://doi.org/10.1007/s40123-016-0050-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40123-016-0050-x