Abstract
Advanced or end-stage age-related macular degeneration (AMD) results in significant visual impairment and a substantially reduced quality of life for patients. Therapeutic options for people with bilateral moderate or profound vision loss caused by end-stage AMD are limited. Although medical treatment capable of reversing the functional vision loss that results from end-stage AMD is non-existent, there are now treatments that can reverse some of that functional vision loss, including the implantable miniature telescope (IMT). This review article discusses the science behind the IMT, evaluates the data from clinical studies, and weighs the pros and cons of the technology.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Age-related macular degeneration (AMD) is a well-known cause of visual impairment and a leading cause of blindness in the US [1–3]. Although the majority of people with AMD have the non-neovascular (or dry) form of AMD, the neovascular (or wet) form is responsible for 90% of severe vision loss due to the disorder [4].
In the past decade, the introduction of anti-vascular endothelial growth factor (VEGF) drugs has led to a paradigm change in how earlier stages of neovascular AMD are treated. These drugs have enabled clinicians to not only halt the progression of the disease, but to return some of the vision loss created by the disease. Despite these pharmacologic advances, however, there remain patients who will progress to severe vision loss due to the development of disciform scars and/or center-involving geographic atrophy (GA). In the Comparison for Age-Related Macular Degeneration study, almost one fifth of enrolled patients developed GA within 2 years of treatment [5, 6]. Conversely, Thalgott et al. found no evidence for acceleration of GA after long-term anti-VEGF use [7]. It remains unclear what role anti-VEGFs have in progression of GA, but it also remains clear that not all patients can be served by anti-VEGFs, and some will progress to more advanced forms of the disease.
The severity of this quality of life (QoL) impairment is often more severe than treating physicians realize. According to patient surveys, it ranged from 96% to 750% more than estimated by the treating ophthalmologist, depending on AMD disease severity [8], underlying how truly devastating this disease may be for the patient. With annual caregiving costs for patients with AMD ranging up to US $47,086 [9], the public health impact cannot be overlooked, and patients’ subjective experience with the advanced stages of the disease undermines the true societal costs.
Until recently, there were few treatment options for these patients beyond rehabilitation with low vision specialists. There is still no pharmacologic or surgical treatment capable of reversing vision loss from disciform scar or GA, but there are treatments that can reverse some of the functional vision loss the anatomic damage causes. One implantable option for patients with end-stage AMD is the implantable miniature telescope (IMT; VisionCare Ophthalmic Technologies, Saratoga, CA, USA), the first device to be approved as a therapy for patients with end-stage AMD. The remainder of this paper will discuss the IMT as well as other devices under investigation.
This article is based on previously conducted studies and does not involve any new studies of human or animal subjects performed by any of the authors.
Currently Available Treatment Options for Wet and Dry AMD
There are numerous treatment options for mild-to-moderate neovascular AMD, ranging from anti-VEGF injections, to laser treatments or photodynamic therapy [10–15]. End-stage AMD [defined as moderate (≤20/80) to profound (20/600 or worse) vision impairment due to bilateral central scotomas resulting from GA and/or disciform scar [16]] is not successfully treated with the interventions used for milder forms of the disease.
Dry AMD treatment strategies, on the other hand, currently concentrate on photoreceptor preservation and complement cascade inhibition [17], with prevention of disease progression through vitamin supplementation commonly employed as a treatment regimen [18, 19]. As with neovascular AMD, there are no pharmacologic treatment options for patients with the more advanced stages of vision loss as a result of dry AMD.
Treatments Under Investigation
Several companies are actively pursuing potential pharmacologic treatments for dry AMD/GA, including anti-Factor D compound lampalizumab in an intravitreal formulation (Genentech), Alimera Sciences’ Medidur fluocinolone acetonide as an intravitreal implant to treat GA, and sustained-release brimonidine implant. Novartis is investigating a compound designed to target the C5 complement pathway as a means to treat GA. Two groups are investigating oral compounds: Acucela is investigating emixustat hydrochloride to treat GA, and the MEDARVA Foundation is studying Oracea (doxycycline 40 mg) in a once-daily pill to treat GA. MacuCLEAR is investigating a topical eye drop to treat non-exudative AMD.
More radical options include macular translocation surgery and stem cell therapies, but these are still in early stages. Macular translocation surgery is an experimental procedure for GA [14], but more research is necessary to determine if the visual outcomes are outweighed by the potentially high level of GA recurrence [20]. One of the major advantages to stem cells (especially allogenic and xenogenic) over other graft forms is their long-term survival [21]. Companies including Advanced Cell Technology, Janssen Pharmaceuticals, and Novartis are in various stages of investigation on stem cell use.
The dearth of commercially available treatment strategies available for end-stage AMD leaves many patients with little to no functional vision. Pharmacologic treatment and cataract surgery do not improve patients’ vision in the more advanced stages [13, 22]. These patients often turn to low vision rehabilitation to maintain self-sufficiency [23–27]. Low-vision magnifiers have served as a non-invasive means to improve QoL in patients with advanced AMD; other options including headset devices and/or closed circuit televisions have high cost/benefit ratios and have been unsuccessful over the long-term [23]. Other potential treatment strategies include telescopic contact lenses, which are said to magnify images by 2.8 times. Not yet in human trials, the lens works in conjunction with “smart glasses” so the patient can control the zoom feature [28]. One large observational study (n = 779 patients) found only 50–54% of patients presenting for outpatient low vision rehabilitation services show “clinically meaningful” differences in outcomes [29]. The same group found in a separate study that VA was the strongest predictor of visual ability and reading ability [25].
Implants and End-Stage AMD Disease
For those with end-stage AMD, several companies are developing retinal and intraocular implants as potential treatment options to slow the progression of the disease or to return some lost vision to the patient. Each of the implants has its own set of advantages and disadvantages. While there are numerous artificial vision projects ongoing worldwide [30], we have limited our discussion here to those that are the furthest along developmentally and commercially, or that are specifically addressing end-stage AMD.
Second Sight (Sylmar, CA, USA) has developed an epiretinal prosthesis (an “artificial retina,” per the company) that can bypass damaged photoreceptors and has been shown to provide vision to patients with bare- to no-light perceptions due to retinitis pigmentosa (RP). Unlike AMD, RP affects peripheral vision, but Second Sight believes the device can be effective in both disease states. The company has begun a feasibility study of the Argus II in people with late-stage dry AMD [31]. During the lengthy surgery, a 55-electrode chip is placed on top of the macular region and requires that the patient wear glasses that has a camera mounted on it. The device includes a wireless processor and a battery pack that patients wear on their belt. While the technology is very intriguing, the current electrode array provides only crude resolution, is very expensive, and requires a significant amount of post-implant training.
Other companies are developing implantable systems for patients with prominent central scotomas. The iol-AMD technology (London Eye Hospital Pharma, London, UK), includes two injectable, hydrophobic acrylic intraocular lenses (IOLs), and is under early stage evaluation as a treatment for early, intermediate and end-stage dry AMD in patients with concurrent cataract [32]. In the iol-AMD procedure, the IOLs are bilaterally implanted through a 3 mm incision. The IOLs work together like a Galilean telescope to magnify the image about 1.3 times and direct it to a healthier part of the retina. (Quereshi et al. 2014, manuscript in preparation. http://iolamd.com/clinical-results.php. Accessed March 20, 2015). Magnification of 1.3 times can, from a mathematical standpoint, provide one ETDRS line of VA improvement. The unpublished data seems to suggest a gain in distance VA of fewer than two lines. While there may be merit to the device, results are anecdotal at this time and much larger studies are needed before a true evaluation can be undertaken.
The Intraocular Lens for Visually Impaired People (IOL-VIP, Soleko, Ponecorvo, Italy) is being evaluated as a treatment option for patients with central scotomas due to macular disease [33]. This dual IOL system includes a biconcave IOL within the capsular bag and a biconvex IOL in the anterior chamber, also creating a Galilean telescope system that enlarges images 1.3 times. A pilot study in 40 eyes of 35 patients with central scotomas showed this system improved the logMAR score from 1.28 preoperatively to 0.77 after the procedure. Peripheral visual field and binocular vision were reported to not be limited, and corneal endothelial cell loss was 7% after 20 months [33]. However, published results are limited, and a prismatic effect exists [1]. Other limitations include a concern over the needed anterior segment space and the proximity of the two IOLs to “critical ocular structures such as the corneal endothelium and iris” [33].
The Scharioth Macula Lens (Medicontur, Hungary) has been designed for pseudophakic patients with advanced/dry AMD (Scharioth G. New add-on IOL for patients with advanced AMD. Paper presented at: ESCRS 2015, Barcelona, Spain: September 5, 2015.) Published data on this lens is limited to company information; a PubMed search yielded no findings.
Based on results from more than 217 implanted patients, the Food and Drug Administration initially approved the IMT in July 2010 [23, 34–36]. In October 2014, FDA expanded the label lowering the age requirement to 65 years. This remainder of this article concentrates on the IMT, its mechanism of action and its clinical study outcomes in the treatment of end-stage AMD.
The Implantable Miniature Telescope, Patient Management, and Implantation
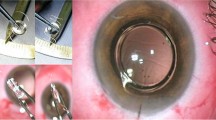
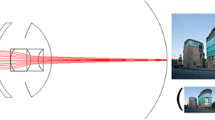
The IMT is approved for implantation in phakic patients 65 years or older with a visual acuity between 20/160 and 20/800 as a result of bilateral central scotomas associated with end-stage AMD. Patients must also have findings of disciform scar or GA, cataract, and show, in preoperative testing, an improvement of at least five letters with the aid of an external telescope. The IMT consists of wide-angle micro-optics that work in concert with the cornea to project a high resolution 2.7× magnified image over approximately 55° of the central and peripheral retina. The optical system is designed to allow patients to recognize images using natural eye movements that were previously difficult or impossible to discern. The telescope, optimized for intermediate vision, is implanted unilaterally and used for central vision, while the contralateral eye maintains peripheral vision for orientation and ambulation. Standard spectacles provide distance and near correction.
A four-step treatment program, CentraSight, has been developed to manage patient through diagnosis, surgical evaluation, and postoperative care. The retina specialist first confirms the diagnosis of end-stage AMD associated with bilateral central scotomas. Second, an evaluation is conducted by a low vision optometrist, who includes use of an external telescope simulator to ascertain whether or not the telescope prosthesis will benefit the patient and should involve recommendations about which eye is likely to result in patient satisfaction for visual processing [37]; the eye targeted for implantation then is selected and patient expectations are evaluated by a low vision occupational therapist. Third, provided the patient benefits from telescope magnification, the patient is seen by a cornea-trained cataract surgeon to make sure the eye is anatomically appropriate for the surgery and if so, implants the telescope.
The surgery, described by Colby and Chang [38], is more challenging than standard cataract surgery primarily due to the size of the implant. After crystalline lens removal, the limbal wound is enlarged to approximately 12 mm; a 7 mm or larger capsulorhexis is recommended to allow easy placement in the capsular bag. The anterior chamber and capsule are filled with a cohesive ophthalmic viscosurgical device (OVD) while the endothelium and device are coated with a dispersive OVD. The corneal lip is gently elevated and the telescope is passed into the capsular bag while avoiding endothelial cell layer touch. Seven to eight interrupted sutures are used to close the corneal incision, and a peripheral iridectomy is performed. A sub-Tenon’s steroid injection, betamethasone 6 mg or methylprednisolone 100 mg, is given along with a topical antibiotic. Postoperative sub-Tenon’s steroid injections were given during the initial clinical trials; currently most surgeons have found adequate inflammation control with topical administration alone. A topical nonsteroidal anti-inflammatory drug, topical steroids, and mydriatics are prescribed. An extended anti-inflammatory drug regimen is recommended.
After surgical recovery, spectacles are prescribed. The fourth and potentially most crucial treatment step is managed by low vision rehabilitation specialists who work with the patient over an average of six visits spread over 3–4 months to educate patients on how to use their new visual status and to reach patients’ preoperative therapy goals. One study noted the optometrist’s role in determining which eye would be most successful with the implant preoperatively can result in higher patient satisfaction postoperatively [37].
Safety and Efficacy
IMT-002 was an open-label pivotal clinical trial of 2.7× and 2.2× IMTs conducted at 28 centers enrolling 217 participants with end-stage AMD, and a mean age of 76 years. VA ranged between 20/80 and 20/800; results have been previously published and will be summarized here [34, 35, 38]. This study aimed to assess the safety and efficacy of the IMT by comparing the eyes with implanted telescopes with the untreated eye. An extension study evaluated the same patients out to 5 years.
The study looked at the changes in VA and endothelial cell density (ECD). The National Eye Institute’s Visual Function Questionnaire-25 (VFQ-25) was used to assess subjective changes in the vision-related QoL of these patients. The mean change in distance BCVA at 12 months after telescope implantation was 3.4 lines. A doubling of VA was achieved in 67% of the implanted eyes at 1 year, compared to 13% of the control eyes (P < 0.0001). Gains in near VA were consistent with distance gains. Mean gains in VA for both telescope models exceeded 90% of their theoretically possible gains. Improvements in vision-related QoL were both clinically and statistically improved. Corneal ECD loss was 20% and 25% at 3 months and 1 year, respectively, reflecting the impact of 12 mm corneal incision and device manipulation involved in telescope implantation. While ECD loss was higher than anticipated at 3 months after implantation, the rate of cell loss decreased as time progressed. Two patients (1%) underwent corneal transplant after developing vision-impairing corneal edema and had large ECD losses after telescope implantation.
Visual acuity gains were retained over time; at 2-years there was an improvement in distance vision of three lines or more in 60% of implanted eyes, 103/173, compared to only 10% of fellow eyes (18/174); the difference was statistically significant [35]. Mean ECD decreased by 2.4% from 12% to 24 months, a rate consistent with conventional cataract surgery. Adverse effects included inflammatory deposits on the device (25%), pigment deposits on device (11%), guttae (8%), posterior synechiae (7%), iris transillumination defects (5%), and iritis (6%). One eye in the implant group (0.6%) lost three lines of vision; 13 eyes (7.5%) of control eyes lost three lines of vision (P = 0.0013) [35].
Data from the 5-year extension study confirmed results found in the initial studies [36]. At 5 years after telescope implantation, VA gains were generally retained and the safety profile was stable. ECD loss at 5 years is comparable to placement of an IOL. Younger patients (age 65–74 years) had better VA gains and fewer complications than their older (75 years or older) counterparts, which may also be a result of additional comorbidities in the older cohort. These 5-year results, stratified by age, led the US FDA to lower the age restriction to 65 years.
Cost-Effectiveness
Brown et al. conducted a value-based medicine analysis on the comparative effectiveness (patient value gain) and cost-effectiveness (cost-utility) of therapy with the IMT. Evidence-based data from the IMT-002 study was used. Ophthalmic utilities were obtained from a validated cohort of 1000 patients with ocular disease to determine the preference-based comparative efficacy and the cost-utility (cost-effectiveness) of the IMT, as determined by quality-adjusted life-year (QALY) [39]. On average, each patient had a gain of 12.5% in their quality of life. At the time of the analysis, interventions costing less than $100,000/QALY in the US were considered cost-effective, and those costing less than $50,000 were considered “very” cost-effective [39]. When compared to no therapy, the average cost-utility ratio was $14,389/QALY for IMT implantation. The authors concluded that treatment of patients with end-stage AMD with the implantable telescope “considerably improves quality of life, and at the same time is cost-effective by conventional standards” [39].
Drawbacks and Limitations
While a viable option for patients with end-stage disease, the IMT is not without its own drawbacks. An acknowledged limitation of the IMT is that it reduces the field of vision to 22°–25° [40]. Patients must undergo post-implantation rehabilitation. Expectations must be managed both preoperatively and after implantation. The IMT will not restore vision to patients’ pre-AMD state, but does return substantial functional vision and lessens the dependence upon caregivers. Patients, while not driving prior to implantation, will be advised to not drive after implantation. Further, anecdotal reports and a case report in the literature suggest this device may not be well suited for patients with active neovascular AMD, although medical intervention with anti-VEGF agents has been used to treat the neovascularization post-implantation [41]. Further, retinal examination and imaging patients with this device can be challenging, but mitigated somewhat with use of the Cirrus HD-OCT (Carl Zeiss Meditec) [42].
ECD loss after the implantation of the telescope has raised some concerns about the procedure; however, the loss is comparable to that after large-incision cataract extraction [38, 43], and the cell loss seems to have stabilized at 2 years after surgery [35]. These ECD losses are comparable to those reported in other high-risk patient populations [1, 44–46]. Long-term follow-up suggests that the loss in the endothelial cells was not related to continuous damage, but rather as the result of the surgery [34].
Lastly, surgeons should expect a learning curve, as ECD loss has been reported to be higher in the first three surgeries than in subsequent surgeries [35]. The acute cell loss reported during early surgical series suggests that patients with corneal dystrophies such as guttata be excluded and that baseline ECD coupled with baseline patient age be given primary consideration during the patient selection process [35].
Patient Experience
For patients who have lost their central vision and independence due to advanced dry AMD, the IMT provides the promise of regaining some of that back. One author’s (VSH) patient stated she “got her life back” when postop day 1 she was able to watch TV and see her daughter’s face for the first time in years. Because her end-stage AMD had been progressing over the previous 6–7 years, she “had missed out” on truly seeing 16 great-grandchildren’s faces. Post-implant, her vision improved, as has her confidence—she now feels able to go shopping on her own, cook, and clean her house, as well as drive her golf cart around the neighborhood. Anecdotally, she did complain that she cleans her house more than ever now because she could never see the dust and didn’t realize how dirty her house had been; this same patient said within the first week she returned her curtains “because I didn’t realize how ugly they were” until she could see them clearly post-implant.
It is not the authors’ contention that every patient will have these kinds of outcomes, nor is it our contention that patients who do achieve these outcomes will do so rapidly. Patients implanted with the IMT need to undergo intense postoperative vision rehabilitation with low vision specialists in order to achieve their best possible vision and regain some of their autonomy.
Conclusion
Although major advances have been made in the past decade in treatment for AMD, there still remains large room for improvement, particularly in the more advanced or end-stage AMD. The majority of patients will continue to progress to more advanced stages, with limited treatment options. One potential treatment, implantation with the IMT, has shown substantial improvement in VA and vision-related QoL in patients with end-stage AMD. The potential side effects and concerns about ECD loss are more than offset by the vision and QoL gains, and the device has been shown to be a cost-effective option for these patients.
We believe the IMT is a viable option for people who otherwise have limited options to improve QoL due to end-stage AMD. In the right patient, the IMT implant can make a profound positive impact in a patient who is otherwise left without an alternative viable treatment option.
The IMT, coupled with other devices under investigation, are providing much-needed options to those with profound vision loss from end-stage AMD.
References
Singer MA, Amir N, Herro A, et al. Improving quality of life in patients with end-stage age-related macular degeneration: focus on miniature ocular implants. Clin Ophthalmol. 2012;6:33–9.
World Health Organization. Universal eye health: a global action plan. 2014–2019. http://www.who.int/blindness/en/. Accessed Feb 18, 2015.
Congdon N, O’Colmain B, Klaver CC, et al. Causes and prevalence of visual impairment among adults in the United States. Arch Ophthalmol. 2004;122(4):477–85.
American Academy of Ophthalmology Retina Panel. Preferred practice pattern: age-related macular degeneration. San Francisco: AAO; 2015.
Grunwald JE, Daniel E, Huang J, et al. Risk of geographic atrophy in the comparison of age-related macular degeneration treatments trials. Ophthalmology. 2014;121(1):150–61.
Grunwald JE, Pistilli M, Ying GS, et al. Growth of geographic atrophy in the comparison of age-related macular degeneration treatments trials. Ophthalmology. 2015;122(4):809–16.
Thalgott V, Feucht N, Lohmann CP, Maier M. Long-term results in neovascular age-related macular degeneration: changes in visual acuity and geographic atrophy during long-standing anti-VEGF therapy. Ophthalmologe. 2016. doi:10.1007/s00347-016-0228-6.
Brown GC, Brown MM, Sharma S, et al. The burden of age-related macular degeneration: a value-based medicine analysis. Trans Am Ophthalmol Soc. 2005;103:173–84 (discussion 84–6).
Schmier JK, Halpern MT, Covert D, et al. Impact of visual impairment on use of caregiving by individuals with age-related macular degeneration. Retina. 2006;26(9):1056–62.
Singer M. Advances in the management of macular degeneration. F1000Prime Rep. 2014;6:29.
Mu Y, Zhao M, Su G. Stem cell-based therapies for age-related macular degeneration: current status and prospects. Int J Clin Exp Med. 2014;7(11):3843–52.
Geltzer A, Turalba A, Vedula SS. Surgical implantation of steroids with antiangiogenic characteristics for treating neovascular age-related macular degeneration. Cochrane Database Syst Rev. 2013;1:CD005022.
Jager RD, Mieler WF, Miller JW. Age-related macular degeneration. N Engl J Med. 2008;358(24):2606–17.
Fernandez-Robredo P, Sancho A, Johnen S, et al. Current treatment limitations in age-related macular degeneration and future approaches based on cell therapy and tissue engineering. J Ophthalmol. 2014;2014:510285.
Schmidt-Erfurth U, Chong V, Loewenstein A, et al. Guidelines for the management of neovascular age-related macular degeneration by the European Society of Retina Specialists (EURETINA). Br J Ophthalmol. 2014;98(9):1144–67.
Colenbrander A. Visual standards: aspects and ranges of vision loss with emphasis on population surveys. Sydney: International Council of Ophthalmology; 2002.
Khan M, Agarwal K, Loutfi M, Kamal A. Present and possible therapies for age-related macular degeneration. ISRN Ophthalmol. 2014;2014:608390.
Age-Related Eye Disease Study 2 Research Group. Lutein + zeaxanthin and omega-3 fatty acids for age-related macular degeneration: the Age-Related Eye Disease Study 2 (AREDS2) randomized clinical trial. JAMA. 2013;309(19):2005–15.
Age-Related Eye Disease Study Research Group. The Age-Related Eye Disease Study system for classifying age-related macular degeneration from stereoscopic color fundus photographs: the Age-Related Eye Disease Study report number 6. Am J Ophthalmol. 2001;132(5):668–81.
Cahill MT, Mruthyunjaya P, Bowes Rickman C, Toth CA. Recurrence of retinal pigment epithelial changes after macular translocation with 360 degrees peripheral retinectomy for geographic atrophy. Arch Ophthalmol. 2005;123(7):935–8.
Garcia JM, Mendonca L, Brant R, et al. Stem cell therapy for retinal diseases. World J Stem Cells. 2015;7(1):160–4.
Forooghian F, Agron E, Clemons TE, et al. Visual acuity outcomes after cataract surgery in patients with age-related macular degeneration: age-related eye disease study report no. 27. Ophthalmology. 2009;116(11):2093–100.
Hooper P, Jutai JW, Strong G, Russell-Minda E. Age-related macular degeneration and low-vision rehabilitation: a systematic review. Can J Ophthalmol. 2008;43(2):180–7.
Chan TL, Goldstein JE, Massof RW. Comparison of clinician-predicted to measured low vision outcomes. Optom Vis Sci. 2013;90(8):776–87.
Goldstein JE, Chun MW, Fletcher DC, et al. Visual ability of patients seeking outpatient low vision services in the United States. JAMA Ophthalmol. 2014;132(10):1169–77.
Rovner BW, Casten RJ, Hegel MT, et al. Low vision depression prevention trial in age-related macular degeneration: a randomized clinical trial. Ophthalmology. 2014;121(11):2204–11.
Zebardast N, Swenor BK, van Landingham SW, et al. Comparing the impact of refractive and nonrefractive vision loss on functioning and disability: the salisbury eye evaluation. Ophthalmology. 2015;122(6):1102–10.
Tremblay E. Smart glasses and telescopic contact lenses for macular degeneration. AAAS 2015 Annual Meeting, San Jose, CA, February 13, 2015.
Goldstein JE, Jackson ML, Fox SM, et al. Clinically meaningful rehabilitation outcomes of low vision patients served by outpatient clinical centers. JAMA Ophthalmol. 2015;133(7):762–9.
Maghami MH, Sodagar AM, Lashay A, et al. Visual prostheses: the enabling technology to give sight to the blind. J Ophthalmic Vis Res. 2014;9(4):494–505.
Second Sight announces first age-related macular degeneration patient receives the Argus II Retinal Prosthesis System as part of groundbreaking study. Sylmar: Second Sight; 2015.
Hengerer FH, Artal P, Kohnen T, Conrad-Hengerer I. Initial Clinical results of a new telescopic IOL implanted in patients with dry age-related macular degeneration. J Refract Surg. 2015;31(3):158–62.
Orzalesi N, Pierrottet CO, Zenoni S, Savaresi C. The IOL-Vip System: a double intraocular lens implant for visual rehabilitation of patients with macular disease. Ophthalmology. 2007;114(5):860–5.
Hudson HL, Lane SS, Heier JS, et al. Implantable miniature telescope for the treatment of visual acuity loss resulting from end-stage age-related macular degeneration: 1-year results. Ophthalmology. 2006;113(11):1987–2001.
Hudson HL, Stulting RD, Heier JS, et al. Implantable telescope for end-stage age-related macular degeneration: long-term visual acuity and safety outcomes. Am J Ophthalmol. 2008;146(5):664–73.
Boyer D, Freund KB, Regillo C, et al. Long-term (60-month) results for the implantable miniature telescope: efficacy and safety outcomes stratified by age in patients with end-stage age-related macular degeneration. Clin Ophthalmol. 2015;9:1099–107.
Primo SA. Implantable miniature telescope: lessons learned. Optometry. 2010;81(2):86–93.
Colby KA, Chang DF, Stulting RD, Lane SS. Surgical placement of an optical prosthetic device for end-stage macular degeneration: the implantable miniature telescope. Arch Ophthalmol. 2007;125(8):1118–21.
Brown GC, Brown MM, Lieske HB, et al. Comparative effectiveness and cost-effectiveness of the implantable miniature telescope. Ophthalmology. 2011;118(9):1834–43.
Chan TL. Implantable miniature telescope. Cataract and refractive surgery today, vol. 26. Bryn Mawr: BMC Publications; 2013.
Joondeph BC. Anti-vascular endothelial growth factor injection technique for recurrent exudative macular degeneration in a telescope-implanted eye. Retin Cases Brief Rep. 2014;8(4):342–4.
Schlimgen M, Fortin MJ, Joondeph B. OCT imaging in eyes with an implanted telescope. Retina today, vol. 10. Bryn Mawr: BMC Publications; 2015.
Bourne WM, Nelson LR, Hodge DO. Continued endothelial cell loss ten years after lens implantation. Ophthalmology. 1994;101(6):1014–22 (discussion 22–3).
Dhasmana R, Singh IP, Nagpal RC. Corneal changes in diabetic patients after manual small incision cataract surgery. J Clin Diagn Res. 2014;8(4):VC03–6.
Ing JJ, Ing HH, Nelson LR, et al. Ten-year postoperative results of penetrating keratoplasty. Ophthalmology. 1998;105(10):1855–65.
Eghrari AO, Gottsch JD. Fuchs’ corneal dystrophy. Expert Rev Ophthalmol. 2010;5(2):147–59.
Acknowledgments
No funding or sponsorship was received for this study or publication of this article.
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval for the version to be published.
Disclosures
VSH and NL have no disclosures to report. MD received financial support from VisionCare Ophthalmic Technologies to prepare this paper.
Compliance with Ethics Guidelines
This article is based on previously conducted studies and does not involve any new studies of human or animal subjects performed by any of the authors.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced content
To view enhanced content for this article go to http://www.medengine.com/Redeem/1E84F0607834233E.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Hau, V.S., London, N. & Dalton, M. The Treatment Paradigm for the Implantable Miniature Telescope. Ophthalmol Ther 5, 21–30 (2016). https://doi.org/10.1007/s40123-016-0047-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40123-016-0047-5