Abstract
Purpose of the Review
Chronic low back pain (CLBP) is a major contributor to societal disease burden and years lived with disability. Nonspecific low back pain (LBP) is attributed to physical and psychosocial factors, including lifestyle factors, obesity, and depression. Mechanical low back pain occurs related to repeated trauma to or overuse of the spine, intervertebral disks, and surrounding tissues. This causes disc herniation, vertebral compression fractures, lumbar spondylosis, spondylolisthesis, and lumbosacral muscle strain.
Recent Findings
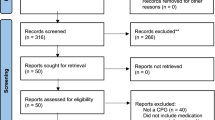
A systematic review of relevant literature was conducted. CENTRAL, MEDLINE, EMBASE, PubMed, and two clinical trials registry databases up to 24 June 2015 were included in this review. Search terms included: low back pain, over the counter, non-steroidal anti-inflammatory (NSAID), CLBP, ibuprofen, naproxen, acetaminophen, disk herniation, lumbar spondylosis, vertebral compression fractures, spondylolisthesis, and lumbosacral muscle strain. Over-the-counter analgesics are the most frequently used first-line medication for LBP, and current guidelines indicate that over-the-counter medications should be the first prescribed treatment for non-specific LBP. Current literature suggests that NSAIDs and acetaminophen as well as antidepressants, muscle relaxants, and opioids are effective treatments for CLBP. Recent randomized controlled trials also evaluate the benefit of buprenorphine, tramadol, and strong opioids such as oxycodone.
Summary
This systematic review discusses current evidence pertaining to non-prescription treatment options for chronic low back pain.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Chronic low back pain (LBP) is a major contributor to societal disease burden and years lived with disability. |
Over-the-counter analgesics are the most frequently used first-line medication for LBP, and current guidelines indicate that over-the-counter medications should be the first prescribed treatment for non-specific LBP. |
This systematic review discusses current evidence pertaining to non-prescription treatment options for chronic LBP. |
Digital Features
This article is published with digital features, including a summary slide, to facilitate understanding of the article. To view digital features for this article go to https://doi.org/10.6084/m9.figshare.13066040.
Introduction
Chronic low back pain (CLBP) is a major contributor to societal disease burden and years lived with disability [1, 2]. It is defined as pain occurring for > 3 months in the lower back region between the lower posterior rib margin and the horizontal gluteal fold [3]. Worldwide, CLBP affects around 23% of the population and recurs within 12 months in 24–80% of individuals [4]. CLBP is the leading cause of health-related premature retirement and is associated with substantial downstream economic losses and reduced quality of life. Nonspecific low back pain (LBP) is attributed to physical and psychosocial factors, including lifestyle factors, obesity, and depression [5]. Mechanical low back pain occurs because of repeated trauma to or overuse of the spine, intervertebral disks, and surrounding tissues. This causes disk herniation, vertebral compression fractures, lumbar spondylosis, spondylolisthesis, and lumbosacral muscle strain [6].
Over-the-counter analgesics are the most frequently used first-line medication for LBP. Current guidelines indicate that over-the-counter medications should be the first prescribed treatment for non-specific LBP. Current literature suggests that NSAIDs and acetaminophen as well as antidepressants, muscle relaxants, and opioids are effective treatments for CLBP. A 2019 randomized controlled trial also evaluate the benefit of buprenorphine, tramadol, and stronger opioids such as oxycodone [7]. This systematic review discusses current evidence pertaining to non-prescription treatment options for chronic low back pain. This review includes meta-analyses, Cochrane reviews, and randomized controlled trials published within the past 5 years evaluating acetaminophen, NSAIDs, magnesium, topical lidocaine or capsaicin creams, and TENS units. This article is based on previously conducted studies and does not contain any studies with human participants or animals performed by any of the authors.
Acetaminophen
Background
Acetaminophen (N-acetyl-p-aminophenol), also known as paracetamol internationally, is commonly used for its analgesic and antipyretic properties in children and adults. It is available in a variety of readily available over-the-counter formulations and is also commonly combined with other medication such as opioids, aspirin, or caffeine [8]. Acetaminophen acts on the hypothalamic heat-regulating center to lower body temperatures during fever and inhibits the cyclooxygenase activity of COX-3, resulting in significant analgesic and antipyretic effects [9,10,11,12]. Serious adverse reactions include hypersensitivity reactions, anaphylaxis, skin reactions, hepatotoxicity resulting in elevated serum transaminase levels acutely, renal tubular necrosis, nephropathy, anemia, and thrombocytopenia. Nausea, rashes, and headaches are common milder reactions. Acetaminophen is metabolized by the CYP450 1A2 and 2E1 liver enzymes and therefore contraindicated in patients with impaired hepatic functioning or chronic alcoholic use [9].
Systematic Reviews
Acetaminophen is often preferred compared to other analgesics for conditions such as LBP because of its accessibility and availability as an inexpensive over-the-counter agent. It is also associated with fewer adverse effects than NSAIDs, specifically related to the gastrointestinal system [11,12,13]. This is particularly true among patients with symptoms of dyspepsia, gastritis, gastric ulcers, or the use of corticosteroids or anticoagulants, which preclude the use of NSAIDs [14]. However, the most updated Cochrane review concluded that acetaminophen, specifically 4 g per day, was not better than placebo in relieving acute LBP or improving quality of life and sleep quality in the short or long term [11]. Similarly, the PACE study also concluded that acetaminophen did not change LBP recovery time compared with placebo and also had no effect on pain, disability, function, symptomology, sleep, or the patient’s quality of life [15]. Of note, the studies evaluated the treatment of acute or post-surgical LBPs, which have different underlying pathologies and are therefore distinct from chronic LBP. There is a paucity of trials studying the effectiveness of acetaminophen for subacute or chronic non-surgical LBP [11, 16].
Additional Studies
Non-steroidal anti-inflammatory drugs are also commonly used first-line analgesic agents for LBP treatment and are frequently compared to acetaminophen or used in combination. NSAIDs are considered more effective than acetaminophen for LBP because of superior anti-inflammatory effects. Bedaiwi et al. reported that celecoxib showed increased efficacy for nonspecific LBP and that patients treated with celecoxib were four times more likely to reach targeted therapeutic pain control than patients receiving acetaminophen, though neither drug benefited inflammatory lesions of the sacroiliac joints or spine [14]. However, a randomized controlled trial (RCT) comparing the NSAID loxoprofen to acetaminophen found no statistical difference between the two drug classes [13].
Acetaminophen combination therapy was found to reduce pain with some formulations also improving motivation and symptoms of depression. A combination of ibuprofen and acetaminophen has been proven to provide quicker and more effective analgesia compared to ibuprofen monotherapy in an open-label study [12]. Additionally, acetaminophen and ibuprofen combination therapy was found to have similar efficacy, tolerability, and safety profiles as ibuprofen monotherapy [12]. Similarly, the combined use of acetaminophen and tramadol, a synthetic opioid with μ-opioid receptor activity, provides synergistic quick and effective short-term analgesia for patients experiencing CLBP[17].
Summary
Findings from recent acetaminophen trials have variable conclusions. Acetaminophen is recommended as a pain management option for CLBP because of lower risk for significant adverse effects compared to agents like NSAIDs [12]. However, new evidence suggests that acetaminophen may not be as effective in treating acute LBP as other drugs such as NSAIDs or antidepressants such as duloxetine and amitriptyline [16]. Most current international clinical practice guidelines continue to recommend acetaminophen as first-line treatment for CLBP. However, many international guidelines also advise against its use because of increasing evidence showing questionable benefit [18]. Among patients who can tolerate NSAIDs, multimodal analgesia through combination therapy of acetaminophen and ibuprofen may be a more effective treatment option, although additional RCTs are needed to confirm these findings [12]. Multimodal therapy including acetaminophen appears more effective in the management of CLBP than the singular use of acetaminophen [16, 17].
NSAIDS (Ibuprofen, Naproxen)
Background
Ibuprofen and naproxen are non-steroidal anti-inflammatory drugs (NSAIDs) that function as non-selective inhibitors of cyclooxygenase (COX) 1 and 2. Both COX 1 and 2 are involved in the synthesis of prostaglandins that are involved in the production of pain, inflammation, and fever [19]. Therefore, cyclooxygenase modulation contributes to the anti-inflammatory and analgesic qualities of ibuprofen and naproxen. Major adverse effects of NSAIDs involve the gastrointestinal, renal, and coagulation systems and may cause gastric pain, vomiting, bleeding, gastric ulcers, acute renal failure, interstitial nephritis, and nephritic syndrome [20]. About 15% of all drug-induced renal failure can be attributed to NSAIDs [19]. All NSAIDs have been linked to an increased number of cardiovascular events such as myocardial infarction and stroke [20].
Ibuprofen is available without a prescription in tablets with strength ranging from 200 to 800 mg. Typical dosing regimens range from 400 to 800 mg up to three times a day. Naproxen is available in both immediate release (220–550 mg), delayed release (375, 500 mg), and extended release tablets (375, 500, 750 mg). It is also available in a 220 mg capsule and a 25 mg/ml oral suspension.
Systematic Reviews
The role of NSAIDs in the management of chronic low back pain has been a topic of substantial research. A 2017 update of the 2008 Cochrane review compared NSAIDs to placebo in treatment of chronic low back pain [21]. Thirteen randomized, controlled trials (RCTs) from CENTRAL, MEDLINE, EMBASE, and PubMed and two clinical trial registry databases up to 24 June 2015 were included in this review. Of the included studies, six trials compared NSAIDs versus placebo [22,23,24,25,26]. Using these studies, the Cochrane review authors found a statistically significant benefit to receiving NSAIDs. There was a mean difference in pain intensity score from baseline of − 6.97 (95% CI − 10.74 to − 3.19) on a 0–100 visual analogue scale (VAS) with a median follow-up of 56 days [interquartile range (IQR) 13–91 days]. Four trials showed that NSAIDs were associated with reduced disability using the Roland Morris Disability Scale. There was a mean difference from baseline of − 0.85 (95% CI − 1.30 to − 0.40) on a scale from 0 to 24 with a median follow-up of 84 days (IQR 42–105 days). Three trials found no significant difference between different types of NSAIDs used [27,28,29]. One trial compared NSAIDs versus paracetamol and found that NSAIDs were not significantly more effective [30]. Another trial compared NSAIDs (celecoxib) versus tramadol and found superior global improvement after 6 weeks among patients taking celecoxib [31]. One trial compared NSAIDs to pregabalin and found no significant difference [32]. The authors concluded that NSAIDs were more effective than placebo in mitigating pain intensity and disability. However, many of the included studies are dated, the magnitude of effects was small, and the level of evidence was low [21].
Two additional systematic reviews also evaluated NSAIDs in the treatment of low back pain and again emphasized that although there is a statistically significant between NSAIDs vs. placebo the magnitude of the effect is small [16, 33]. However, these reviews included only studies previously discussed by the 2017 Cochrane review discussed above.
A 2015 Cochrane review assessed the efficacy of NSAIDs for chronic back pain specifically with a neuropathic component [34]. This review identified studies by searching CENTRAL, MEDLINE, and EMBASE along with reference lists and an online trial registry including randomized double-blind studies of ≥ 2 weeks. Two studies (251 participants) were qualified for inclusion in this review [32, 35]. One studied the effects of celecoxib alone and in combination with pregabalin compared with placebo and found a significant improvement in pain score was achieved with pregabalin and celecoxib in combination or pregabalin alone [32]. The other included study evaluated an experimental NSAID (GW40638) compared to placebo and found no significant difference [35]. The authors concluded that based on this third-tier evidence there was not enough information to make a decision on the efficacy or safety of the novel NSAIDs in treating chronic low back pain with a neuropathic component [34].
Additional Studies
In a 2017 RCT, Ostojic et al. assessed the efficacy of ibuprofen and paracetamol vs. ibuprofen only to treatment acute low back pain [12]. A statistically significant decrease in pain intensity was observed in both groups using the VAS (visual analog scale). Change in pain intensity was 65.4–22.1 (p < 0.001) at day 10 for the ibuprofen alone group. Researchers concluded that both treatment options were effective [12].
Summary
The available evidence shows that NSAIDs demonstrate a statistically significant but clinically small improvement over placebo in the treatment of chronic low back pain. Evidence continues to be low tier because of the limited number of trials and the methodologic shortcomings of these trials. The use of NSAIDs, especially over a prolonged time, is also not without risk. While short-term use is considered relatively safe, long-term use predisposes patients to considerable side effects. Recent American College of Physicians (ACP) guidelines recommend NSAIDs as a first-line pharmacologic agent.
Magnesium
Background
Magnesium acts as an NMDA receptor antagonist, blunting central nervous system sensitization to pain [36]. It is currently available in a variety of forms including magnesium oxide, citrate, and chloride. The most common adverse effects of magnesium are nausea, vomiting, and diarrhea. Magnesium also may interfere with coagulation and cause increased bruising and bleeding in those with clotting disorders. At toxic doses, magnesium may lead to hypotension, muscle weakness, depressed reflexes, and cardiac arrhythmias.
Randomized Controlled Trials
A 2012 double-blinded RCT evaluated magnesium therapy in patients with chronic low back pain with a neuropathic component [37]. All enrolled patients received gabapentin 300 mg orally three times daily, amitriptyline hydrochloride 25 mg orally at bedtime, and celecoxib 200 mg orally twice daily. Treatment (magnesium) group patients received an intravenous infusion of magnesium sulfate 1 g in 250 ml saline 0.9% given over 4 h every day for 2 weeks. This infusion was then replaced with oral magnesium therapy twice daily for 4 weeks using capsules containing magnesium oxide 400 mg and magnesium gluconate 100 mg. All patients rated their pain intensity using an independent pain physician and an 11-point numeric scale (NRS). Patients in the placebo and treatment groups reported a statistically significant reduction in pain intensity at 2 weeks. However, this pain reduction continued throughout the 6-month follow-up period only among patients receiving magnesium therapy. The researchers concluded that magnesium therapy contributed to a significant reduction in chronic pain intensity at 6 months compared with both baseline and control group values [37].
Summary
Studies evaluating the use of magnesium in chronic low back pain are currently limited. However, existing evidence demonstrates an improvement over placebo for patients with chronic low back pain with a neuropathic component. Overall, magnesium appears to be a viable treatment option for those who have failed conventional treatment; however, further research is needed to identify the optimum dose and period of treatment.
TENS Unit
Background
Conventional transcutaneous electrical nerve stimulation (TENS) is a pain treatment modality that provides analgesia by delivering activating stimuli to Aβ afferent nerve fibers at various frequencies. This, in turn, is thought to decrease subsequent nociceptor activity and associated pain. The delivered frequency and current amplitude are both adjustable parameters of TENS therapy [38]. TENS units are a noninvasive, low-risk treatment of chronic low back pain; however, contraindications include pregnancy, epilepsy, and pacemaker use [38].
In a nationwide database review, Pivec et al. concluded that TENS usage for chronic low back pain is correlated with fewer hospital, clinic, and physical therapy visits compared to controls not using TENS therapy [39]. However, the benefit of chronic back pain treatment with a TENS unit is controversial, and several past studies have suggested equivocal and contradictory findings [40,41,42].
Meta-Analyses
In a 2016 meta-analysis, Jauregui et al. combined the results of nine studies for a total of 267 patients with a mean follow-up of 7 weeks (ranging from 2 to 24 weeks) and treatment duration of 6 weeks (ranging from 2 to 24 weeks). With a 0.844 mean difference in pain between pre- and post-treatment, patients treated with the TENS unit had statistically significant reduction in pain compared to control. However, this only held true for patients who received the therapy for < 5 weeks. After 5 weeks, statistical difference in chronic lower back pain severity between the control and TENS unit treatment groups disappeared, suggesting the benefit of TENS therapy may be most significant during short-term use [41].
Similarly, a 2018 meta-analysis by Wu et al. including 12 randomized controlled trials for a total of 700 patients reported significantly improved functional status among patients undergoing TENS therapy in short-term follow-up extending to 6 weeks with a loss of statistically significant benefit after 6 weeks [42].
In a separate 2018 meta-analysis, including seven randomized controlled trials and 655 patients, Resende et al. demonstrated significant relief for chronic lower back and chronic neck pain only while the patients were physically receiving TENS and interferential current therapy. No pain relief difference was demonstrated between treatment and control groups while between treatment sessions or 1–3 months after treatments concluded. The authors of this analysis described inconsistent treatment parameters and assessment timing across the included studies as limitations to forming definitive conclusions concerning the benefit of TENS therapy in the treatment of chronic low back pain [43].
Additional Studies
In 2016, Aguilar Ferrándiz et al. conducted a randomized clinical trial of 39 patients comparing patients receiving TENS therapy with mechanical pressure to patients receiving mechanical pressure without any electrical current [44]. Both groups received six treatment sessions. While there was a significant decrease in chronic low back pain and improvement in function in both groups compared to pre-treatment assessment, there was no difference in pain or functionality between the groups. Additionally, there were also no differences between the groups when assessing pain catastrophizing, central sensitization, illness perception, and kinesiophobia. While this study demonstrated significant chronic back pain improvement from baseline, TENS unit usage did not offer a superior benefit compared to placebo [44].
One of the most attractive aspects of adjuvant TENS unit therapy for chronic lower back pain is the potential for reduction of opioid usage in this patient population. Pivec et al. found 57.7% of patients receiving TENS therapy required opioids at 1-year follow-up compared to 60.3% of patients not receiving TENS therapy in a 2015 database review of approximately 45,000 patients [45]. This finding was statistically significant, but clinical relevance remains to be determined. However, reduced opioid consumption in this population resulted in reduced annual per-patient opioid costs: $169 in those receiving TENS therapy compared to $192 in those without [45].
Summary
TENS units remain a controversial chronic back pain therapy. Existing evidence suggests marginal to no benefit, particularly following long-term use. However, given very few contraindications to TENS therapy and its relative affordability, the devices may be useful adjuncts to an existing pain regimen or may provide a safe option for patients with contraindications to pharmacologic treatment. Further research is needed to more accurately predict which patient populations are most likely to clinically benefit from this therapy.
Topical Creams and Patches (Lidocaine and Capsaicin)
Background
Lidocaine and capsaicin may be used as topical analgesics in the treatment of chronic low back pain. Topical 5% lidocaine works by inhibiting fast voltage-gated sodium channels within neuronal cell membranes, thus halting nociceptive action potentials. It is currently recommended as one of several first-line treatments for chronic low back pain [46,47,48]. Capsaicin works as an agonist for the TRPV1 channel found on nociceptors and is approved for peripheral neuropathic pain in adults [49, 50]. Capsaicin is available as an over-the-counter cream in 0.025, 0.075, and 0.1% formulations and is also available as a one-time-use 8% patch applied for 60 min in the clinic setting [51].
Common adverse effects of topical lidocaine include localized erythema and rash. There is also a risk of systemic toxicity should the patch be worn for > 12 h a day [47]. Common adverse effects of topical capsaicin are similar with the ability to produce localized erythema and rash; however, this agent may also produce an uncomfortable burning sensation where it is applied. It is advised to avoid eye or mucosal contact with topical capsaicin cream, and it acts as an irritant in this setting [47].
Additional Studies
Lidocaine
Several past studies over the past 15 years have demonstrated 5% lidocaine patches as an efficacious treatment in the reduction of low back pain [51]. These findings, in combination with a low adverse effect profile, user-friendliness, and relative affordability, have resulted in topical 5% lidocaine patches being one of the recommended first-line therapies for the treatment of chronic lower back pain [47].
One of the most recent studies was a 2012 randomized controlled trial from Hashmi et al. of 30 patients comparing lower back pain improvement and brain activity via fMRI in patients treated with lidocaine patches vs. placebo. Both groups exhibited an approximately 50% decrease in low back pain after 2 weeks of treatment with corresponding decreases in fMRI nociceptive brain activity. With no statistical difference between placebo or treatment group, the authors suggested the placebo effect may be a considerable factor in the effectiveness of lidocaine patches in chronic back pain patients [52].
A randomized controlled trial by Castro et al. from 2017 found 3.6% over-the-counter lidocaine combined with 1.25% menthol was just as efficacious in reducing chronic lower back pain as 5% lidocaine patches. These results lead to the theorization that menthol improves skin permeability to lidocaine, and this combination serves as a more affordable option to patients [53].
Overall, 5% lidocaine patches have proven the ability to attenuate chronic low back pain, whether from nociceptive input blockage, placebo effect, or a combination of both. The effectiveness, affordability, and very low risk of adverse effects continue to make it a recommendable first-line treatment for chronic low back pain.
Capsaicin
A 2010 randomized double-blind multi-center trial from Chrusbasik et al. of 142 patients with chronic back pain demonstrated 73.2% pain sum score improvement after 3 weeks of treatment with 0.05% topical capsaicin cream compared to 49.3% in placebo. In addition, 59.2% of patients receiving topical capsaicin for 3 weeks experienced at least a 50% pain sum score improvement compared to only 33.8% in placebo [54]. These findings suggest topical capsaicin as a reasonable choice for chronic back pain treatment.
A 2016 open-label study from Zis et al. of 90 patients with lumbosacral neuropathic pain found statistically significant reductions in pain at 2, 8, and 12 weeks of follow-up in patients receiving the topical 8% capsaicin patch. The same study also found significant improvements in mobility, self-care, usual activities, pain/discomfort, and anxiety/depression at the same time points [55].
Similar findings were exhibited in a 2017 randomized controlled trial by Baron et al. of 50 participants investigating chronic lumbosacral radiculopathy treatment with a topical 8% capsaicin patch and found at least a 30% improvement of pain in 71.4% and 39.1% of patients with 3 months to 2 years duration of pain and > than 2 years duration of pain, respectively [53]. Both these studies suggest topical capsaicin as a rational choice for the treatment of neuropathic lumbosacral pain.
Summary
In summary, topical lidocaine and capsaicin have both demonstrated analgesic abilities in the management of chronic lower back pain with favorable side effect profiles compared to systemic pharmacotherapies. Specifically, 5% lidocaine patches have repeatedly demonstrated the ability to reduce chronic lower back pain, with no recent literature suggesting otherwise. Therefore, using lidocaine patches as a first-line treatment of general chronic lower back pain remains advisable. Recent literature also highlights capsaicin cream’s ability to relieve chronic neuropathic back pain and associated radiculopathies. These findings suggest, when choosing a topical analgesic, it is most appropriate to treat patients with conventional chronic lower back pain with 5% lidocaine patches and patients with any associated radiculopathy with OTC capsaicin cream or the 8% capsaicin patch, which has been more researched than topical capsaicin cream within the past 3 years.
Conclusion
Chronic low back pain is lumbosacral pain occurring for > 3 months and may be idiopathic or caused by mechanical factors including disk herniation, lumbar spondylosis, vertebral compression fractures, spondylolisthesis, and lumbosacral muscle strain [6]. Chronic low back pain is a major cause of disability and has a well-described impact on patient quality of life and societal disease burden [1, 2].
Non-prescription or over-the-counter analgesics are currently recommended as first-line medications for the treatment of chronic low back pain. Various formulations and potencies are being developed and will be available for clinical use in the future. In this regard, both physicians and patients should be aware of the dosing, concentrations, side effects, and potential for error when using these over-the-counter drug preparations. However, there is abundant literature demonstrating efficacy for chronic low back pain in many existing over-the-counter analgesics. In this review, therefore, we have evaluated recent Cochrane reviews, meta-analyses, and randomized controlled trials evaluating commonly used non-prescription treatments, including acetaminophen, NSAIDs, magnesium, topical creams, and TENS units. Many of these preparations show efficacy and tolerability.
References
Vos T, Allen C, Arora M, Barber RM, Brown A, Carter A, et al. Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990–2015: a systematic analysis for the global burden of disease study 2015. Lancet. 2016;388(10053):1545–602.
Vos T, Barber RM, Bell B, Bertozzi-Villa A, Biryukov S, Bolliger I, et al. Global, regional, and national incidence, prevalence, and years lived with disability for 301 acute and chronic diseases and injuries in 188 countries, 1990–2013: a systematic analysis for the global burden of disease study 2013. Lancet. 2015;386(9995):743–800.
Deyo RA, Dworkin SF, Amtmann D, Andersson G, Borenstein D, Carragee E, et al. Report of the NIH task force on research standards for chronic low back pain. Phys Ther. 2015;95(2):e1–18.
Hoy D, Brooks P, Blyth F, Buchbinder R. The epidemiology of low back pain. Best Pract Res Clin Rheumatol. 2010;24(6):769–81.
Maher C, Underwood M, Buchbinder R. Non-specific low back pain. Lancet. 2017;389(10070):736–47.
Will J, Bury D, Miller JA. Mechanical low back pain: prevention. Am Fam Physician. 2018;98(7):421–8.
Chaparro LE, Furlan AD, Deshpande A, Mailis-Gagnon A, Atlas S, Turk DC. Opioids compared to placebo or other treatments for chronic low-back pain. Cochrane Database Syst Rev. 2013. https://doi.org/10.1002/14651858.CD004959.pub4.
Prescott L. Kinetics and metabolism of paracetamol and phenacetin. Br J Clin Pharmacol. 1980;10(Suppl 2):291S-298S.
Chandrasekharan NV, Dai H, Roos KLT, Evanson NK, Tomsik J, Elton TS, et al. COX-3, a cyclooxygenase-1 variant inhibited by acetaminophen and other analgesic/antipyretic drugs: cloning, structure, and expression. Proc Natl Acad Sci USA. 2002;99(21):13926–31.
Jozwiak-Bebenista M, Nowak JZ. Paracetamol: mechanism of action, applications and safety concern. Acta Pol Pharm. 2014;71(1):11–23.
Saragiotto BT, Machado GC, Ferreira ML, Pinheiro MB, Abdel Shaheed C, Maher CG. Paracetamol for low back pain. Cochrane Database Syst Rev. 2016;2016(6):CD012230.
Ostojic P, Radunovic G, Lazovic M, Tomanovic-Vujadinovic S. Ibuprofen plus paracetamol versus ibuprofen in acute low back pain: a randomized open label multicenter clinical study. Acta Reumatol Port. 2017;42(1):18–25.
Miki K, Ikemoto T, Hayashi K, Arai YC, Sekiguchi M, Shi K, et al. Randomized open-labbel non-inferiority trial of acetaminophen or loxoprofen for patients with acute low back pain. J Orthop Sci. 2018;23(3):483–7.
Bedaiwi MK, Sari I, Wallis D, O’Shea FD, Salonen D, Haroon N, et al. Clinical efficacy of celecoxib compared to acetaminophen in chronic nonspecific low back pain: results of a randomized controlled trial. Arthritis Care Res (Hoboken). 2016;68(6):845–52.
Williams CM, Maher CG, Latimer J, McLachlan AJ, Hancock MJ, Day RO, et al. Efficacy of paracetamol for acute low-back pain: a double-blind, randomised controlled trial. Lancet. 2014;384(9954):1586–96.
Chou R, Deyo R, Friedly J, Skelly A, Weimer M, Fu R, et al. Systemic pharmacologic therapies for low back pain: a systematic review for an American College of physicians clinical practice guideline. Ann Intern Med. 2017;166(7):480–92.
Tetsunaga T, Tetsunaga T, Tanaka M, Nishida K, Takei Y, Ozaki T. Effect of tramadol/acetaminophen on motivation in patients with chronic low back pain. Pain Res Manag. 2016;2016:7458534.
Oliveira CB, Maher CG, Pinto RZ, Traeger AC, Lin CWC, Chenot JF, et al. Clinical practice guidelines for the management of non-specific low back pain in primary care: an updated overview. Eur Spine J. 2018;27(11):2791–803.
Ejaz P, Bhojani K, Joshi VR. NSAIDs and kidney. J Assoc Physicians India. 2004;52:632–40.
Grosser T. Cardiovascular safety of celecoxib, naproxen, or ibuprofen for arthritis. N Engl J Med. 2017;375:2519–29.
Enthoven WTM, Roelofs PDDM, Deyo RA, van Tulder MW, Koes BW. Non-steroidal anti-inflammatory drugs for chronic low back pain. N Engl J Med. 2016;375(26):2519–29.
Allegrini A, Nuzzo L, Pavone D, Tavella-Scaringi A, Giangreco D, Bucci M, et al. Efficacy and safety of piroxicam patch versus piroxicam cream in patients with lumbar osteoarthritis: a randomized, placebo-controlled study. Arzneimittel-Forschung Drug Res. 2009;59(8):403–9.
Berry H, Bloom B, Hamilton EBD, Swinson DR. Naproxen sodium, diflunisal, and placebo in the treatment of chronic back pain. Ann Rheum Dis. 1982;41(2):129–32.
Birbara CA, Puopolo AD, Munoz DR, Sheldon EA, Mangione A, Bohidar NR, et al. Treatment of chronic low back pain with etoricoxib, a new cyclo-oxygenase-2 selective inhibitor: improvement in pain and disability—a randomized, placebo-controlled, 3-month trial. J Pain. 2003;4(6):307–15.
Coats TL, Borenstein DG, Nangia NK, Brown MT. Effects of valdecoxib in the treatment of chronic low back pain: results of a randomized, placebo-controlled trial. Clin Ther. 2004;26(8):1249–60.
Kivitz AJ, Gimbel JS, Bramson C, Nemeth MA, Keller DS, Brown MT, et al. Efficacy and safety of tanezumab versus naproxen in the treatment of chronic low back pain. Pain. 2013;154(7):1009–21.
Driessens M, Famaey JP, Orloff S, Chochrad I, Cleppe D, de Brabanter G, et al. Efficacy and tolerability of sustained-release ibuprofen in the treatment of patients with chronic back pain. Curr Ther Res. 1994;55(11):1283–92.
Videman T, Osterman K. Double-blind parallel study of piroxicam versus indomethacin in the treatment of low back pain. Ann Clin Res. 1984;16(3):156–60.
Zerbini C, Ozturk ZE, Grifka J, Maini M, Nilganuwong S, Morales R, et al. Efficacy of etoricoxib 60 mg/day and diclofenac 150 mg/day in reduction of pain and disability in patients with chronic low back pain: results of a 4-week, multinational, randomized, double-blind study. Curr Med Res Opin. 2005;21(12):2037–49.
Hickey RF. Chronic low pack pain: a comparison of diflunisal with paracetamol. N Z Med J. 1982;95(707):312–4.
O’Donnell JB, Ekman EF, Spalding WM, Bhadra P, McCabe D, Berger MF. The effectiveness of a weak opioid medication versus a cyclo-oxygenase-2 (COX-2) selective non-steroidal anti-inflammatory drug in treating flare-up of chronic low-back pain: results from two randomized, double-blind, 6-week studies. J Int Med Res. 2009;37(6):1789–802.
Romanò CL, Romanò D, Bonora C, Mineo G. Pregabalin, celecoxib, and their combination for treatment of chronic low-back pain. J Orthop Traumatol. 2009;10(4):185–91.
Koes BW, Backes D, Bindels PJE. Pharmacotherapy for chronic non-specific low back pain: current and future options. Expert Opin Pharmacother. 2018;19(6):537–45.
Moore RA, Chi CC, Wiffen PJ, Derry S, Rice ASC. Oral nonsteroidal anti-inflammatory drugs for neuropathic pain. Cochrane Database Syst Rev. 2015;2015(10):CD010902.
Shackelford S, Rauck R, Quessy S, Blum D, Hodge R, Philipson R. A randomized, double-blind, placebo-controlled trial of a selective COX-2 inhibitor, GW406381, in patients with postherpetic neuralgia. J Pain. 2009;10(6):654–60.
Vink R, Nechifor M. Magnesium in the central nervous system. Adelaide: University of Adelaide Press; 2011.
Yousef AA, Al-Deeb AE. A double-blinded randomised controlled study of the value of sequential intravenous and oral magnesium therapy in patients with chronic low back pain with a neuropathic component. Anaesthesia. 2013;68(3):260–6.
Simon CB, Riley JL, Fillingim RB, Bishop MD, George SZ. Age group comparisons of TENS response among individuals with chronic axial low back pain. J Pain. 2015;16(12):1268–79.
Pivec R, Stokes M, Chitnis AS, Paulino CB, Harwin SF, Mont MA. Clinical and economic impact of TENS in patients with chronic low back pain: analysis of a nationwide database. Orthopedics. 2013;36(12):922–8.
Garaud T, Gervais C, Szekely B, Michel-Cherqui M, Dreyfus JF, Fischler M. Randomized study of the impact of a therapeutic education program on patients suffering from chronic low-back pain who are treated with transcutaneous electrical nerve stimulation. Medicine (Baltimore). 2018;97(52):e13782.
Jauregui JJ, Cherian JJ, Gwam CU, Chughtai M, Mistry JB, Elmallah RK, et al. A meta-analysis of transcutaneous electrical nerve stimulation for chronic low back pain. Surg Technol Int. 2016;28:296–302.
Wu LC, Weng PW, Chen CH, Huang YY, Tsuang YH, Chiang CJ. Literature review and meta-analysis of transcutaneous electrical nerve stimulation in treating chronic back pain. Reg Anesth Pain Med. 2018;43(4):425–33.
Resende L, Merriwether E, Rampazo P, Dailey D, Embree J, Deberg J, et al. Meta-analysis of transcutaneous electrical nerve stimulation for relief of spinal pain. Eur J Pain. 2018;22(4):663–78.
Ferrándiz MEA, Nijs J, Gidron Y, Roussel N, Vanderstraeten R, van Dyck D, et al. Auto-targeted neurostimulation is not superior to placebo in chronic low back pain: a fourfold blind randomized clinical trial. Pain Physician. 2016;19(5):E707–19.
Pivec R, Minshall ME, Mistry JB, Chughtai M, Elmallah RK, Mont MA. Decreased opioid utilization and cost at one year in chronic low back pain patients treated with transcutaneous electric nerve stimulation (TENS). Surg Technol Int. 2015;31(27):268–74.
Baron R, Binder A, Attal N, Casale R, Dickenson AH, Treede RD. Neuropathic low back pain in clinical practice. Eur J Pain. 2016;20(6):861–73.
Uhl RL, Roberts TT, Papaliodis DN, Mulligan MT, Dubin AH. Management of chronic musculoskeletal pain. J Am Acad Orthop Surg. 2014;22(2):101–10.
Morlion B. Pharmacotherapy of low back pain: targeting nociceptive and neuropathic pain components. Curr Med Res Opin. 2011;27(1):11–33.
Wagner T, Poole C, Roth-Daniek A. The capsaicin 8% patch for neuropathic pain in clinical practice: a retrospective analysis. Pain Med. 2013;14(8):1202–11.
Mou J, Paillard F, Turnbull B, Trudeau J, Stoker M, Katz NP. Efficacy of Qutenza® (capsaicin) 8% patch for neuropathic pain: a meta-analysis of the qutenza clinical trials database. Pain. 2013;154(9):1632–9.
Argoff CE, Galer BS, Jensen MP, Oleka N, Gammaitoni AR. Effectiveness of the lidocaine patch 5% on pain qualities in three chronic pain states: assessment with the Neuropathic Pain Scale. Curr Med Res Opin. 2004;20(Suppl 2):S21–8.
Hashmi JA, Baliki MN, Huang L, Parks EL, Chanda ML, Schnitzer T, et al. Lidocaine patch (5%) is no more potent than placebo in treating chronic back pain when tested in a randomised double blind placebo controlled brain imaging study. Mol Pain. 2012;24(8):29.
Baron R, Treede RD, Birklein F, Cegla T, Freynhagen R, Heskamp ML, et al. Treatment of painful radiculopathies with capsaicin 8% cutaneous patch. Curr Med Res Opin. 2017;33:1401–11.
Chrubasik S, Weiser T, Beime B. Effectiveness and safety of topical capsaicin cream in the treatment of chronic soft tissue pain. Phytother Res. 2010;24(12):1877–85.
Zis P, Bernali N, Argira E, Siafaka I, Vadalouca A. Effectiveness and impact of capsaicin 8% patch on quality of life in patients with lumbosacral pain: an open-label study. Pain Res Manag. 2019;2019:8346161.
Acknowledgements
Funding
No funding or sponsorship was received for this study or publication of this article.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Disclosures
Jacquelin Peck, Ivan Urits, Sandy Peoples, Lukas Foster, Akshara Malla, Amnon A. Berger, Elyse M. Cornett, Hisham Kassem, and Jared Herman have nothing to disclose. Alan D. Kaye and Omar Viswanath are members of the journal’s Editorial Board.
Compliance with Ethics Guidelines
This article is based on previously conducted studies and does not contain any studies with human participants or animals performed by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Peck, J., Urits, I., Peoples, S. et al. A Comprehensive Review of Over the Counter Treatment for Chronic Low Back Pain. Pain Ther 10, 69–80 (2021). https://doi.org/10.1007/s40122-020-00209-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40122-020-00209-w