Abstract
Introduction
Diabetes is one of the most common comorbidities of COVID-19. We aimed to conduct a multidimensional analysis of risk factors associated with the severity and mortality of patients with COVID-19 and diabetes.
Methods
In this retrospective study involving 1443 patients with COVID-19, we analyzed the clinical and laboratory characteristics and risk factors associated with disease severity in patients with COVID-19 with and without diabetes. Binary logistic regression analyses were performed to identify the risk factors associated with mortality in patients with COVID-19 and diabetes. The 84-day survival duration for critical patients with COVID-19 and diabetes who had different levels of leukocytes and neutrophils, or treated with immunoglobulin or not, was conducted using Kaplan–Meier survival curves.
Results
Of the 1443 patients with COVID-19, 256 (17.7%) had diabetes, had a median age of 66.0 [IQR 58.0–73.8] years, and were more likely to develop severe (41.8% vs. 35.6%) and critical disease (34.0% vs. 14.9%), followed by higher mortality (21.1% vs. 7.0%), than those without diabetes. Higher levels of leukocytes (> 5.37 × 109/L), older age, and comorbid cerebrovascular disease and chronic renal disease independently contributed to in-hospital death of patients with COVID-19 and diabetes. Leukocytes > 5.37 × 109/L and the application of immunoglobulin were associated with shorter survival duration and lower mortality, respectively, in critical patients with COVID-19 and diabetes.
Conclusions
More attention should be paid to patients with COVID-19 and diabetes, especially when they have high leukocyte counts (> 5.37 × 109/L). Timely and adequate intravenous immunoglobulin (IVIG) use may reduce the mortality of critical patients with COVID-19 and diabetes.
Similar content being viewed by others

Avoid common mistakes on your manuscript.
Why carry out this study? |
Diabetes is one of the most common comorbidities of COVID-19. |
We aimed to conduct a multidimensional analysis of risk factors associated with the severity and mortality of COVID-19 patients with diabetes. |
What was learned from the study? |
More attention should be paid to patients with COVID-19 and diabetes, especially when they have high leukocyte (> 5.37 × 109/L) and neutrophil counts (> 8.72 × 109/L), older age, cerebrovascular disease, or chronic kidney disease. |
Timely and adequate intravenous immunoglobulin (IVIG) use may reduce the mortality of critical COVID-19 patients with diabetes. |
Digital Features
This article is published with digital features to facilitate understanding of the article. To view digital features for this article go to https://doi.org/10.6084/m9.figshare.12968201.
Introduction
The spread of COVID-19, the disease caused by the novel coronavirus SARS-CoV-2, has reached pandemic levels and poses a threat of increased morbidity and mortality worldwide. By July 30, 2020, the virus had caused 87,830 confirmed cases and 4665 deaths in China and cases have also been reported in Africa, the Americas, the Eastern Mediterranean, Europe, Southeast Asia, the Western Pacific, and other regions. The disease severity varies from mild self-limiting flu-like illness to fulminant pneumonia, respiratory failure, and death.
Patients with comorbidities are more likely to develop severe disease and subsequently death, although the overall mortality rate of COVID-19 is low (1.4–2.3%) [1, 2]. The high incidence of diabetes mellitus (DM) globally makes this particularly concerning as the COVID-19 pandemic progresses. A study in China showed that the most common comorbidities were diabetes (22.0%) and cerebrovascular disease in 32 non-survivors from a group of 52 intensive care unit patients with COVID-19 [3]. The overall fatality rate was 2.3% in patients with COVID-19, but was increased to 7.3% in people with diabetes, as demonstrated by a recent summary report from the Chinese Center for Disease Control of 72,314 cases across the country [2]. Therefore, further investigations about COVID-19 cases are necessary to elaborate the prognostic risk factors and effective treatment measures for those with comorbid diabetes, and consequently to help identify risk factors for COVID-19.
In the present study, 1443 patients with COVID-19 were enrolled, 256 of whom had DM. In addition to discussing the effect of DM on the morbidity, disease characteristics, and outcomes of patients with COVID-19, our study further conducted multidimensional analyses to explore the risk factors associated with severity and mortality of patients with COVID-19 with or without DM, to provide useful clinical information for the decision of treatment options for patients with COVID-19 and DM.
Methods
Study Design and Participants
For this retrospective, singlecenter study, we collected the medical records of 1443 patients in Chinese from January 1 to March 24, 2020, at the Central Hospital of Wuhan, which is a designated hospital to treat patients with SARS-CoV-2 pneumonia. The enrolled patients in this study were all diagnosed with COVID-19 according to the World Health Organization (WHO) interim guidelines [4] and had a definite outcome (death or hospital discharge). The study was approved by the Wuhan Central Hospital ethics committee, and written informed consent was waived by the ethics commission because of the retrospective nature of this study.
Diabetes was ascertained through a diabetes diagnosis in medical records or a self-reported diagnosis confirmed by medical records reviewed by endocrinologists. Diabetes was defined according to the WHO diagnostic criteria: fasting plasma glucose ≥ 7.0 mmol/L (≥ 126 mg/dL) or 2-h plasma glucose ≥ 11.1 mmol/L (≥ 200 mg/dL). Diabetes was initially treated as a categorical variable (yes vs. no), and subsequently we divided the patients with diabetes or without diabetes into three subgroups (moderate, severe, and critical, respectively) according to the severity of the disease to elaborate the risk factors related to disease severity [5]. Briefly, moderate grade was defined as fever, respiratory symptoms, and changes on lung CT scans; severe grade was defined as respiratory rate ≥ 30 breaths per min, blood oxygen saturation ≤ 93%, oxygenation index ≤ 300 mmHg, and/or lung infiltrates increased > 50% within 24–48 h; and critical grade was defined as respiratory failure, septic shock, and/or multiple organ dysfunction or failure. In order to demonstrate the risk factors of death, we sorted the critically ill patients into two groups according to the disease outcome (survival or non-survival). The patients with diabetes in our study were those with confirmed diabetes prior to SARS-CoV-2 infection, excluding those with newly diagnosed diabetes during SARS-CoV-2 infection.
Data Collection
The epidemiological, demographic, clinical symptoms and signs, laboratory findings, management, and outcome data were obtained from the electronic medical records system of the Central Hospital of Wuhan. Laboratory validation of SARS-CoV-2 was performed at the Central Hospital of Wuhan [6]. The severity of COVID-19 was defined according to the diagnostic and treatment guidelines for SARS-CoV-2 issued by the Chinese National Health Committee (Version 5) [5].
Statistical Analysis
Categorical variables are presented as counts and percentages (%), and continuous variables are summarized using median and interquartile range (IQR) values. Categorical variables between groups were compared using the χ2 test or Fisher’s exact test, and continuous variables were analyzed using Students’s t test for normally distributed data or the Mann–Whitney U test for nonnormal distributed data. Factors related to disease severity of patients were analyzed by an ordered logistic regression model. A binary logistic regression analysis was applied to determine the potential risk factors associated with the composite endpoints, with the odds ratio (OR) and 95% confidence interval (95% CI) being reported. A receiver operating characteristic (ROC) curve was plotted to determine the cutoff point for the risk factors for death. Kaplan–Meier survival curves were used to compare the 84-day survival rate for critically ill patients with COVID-19 and diabetes by the log-rank test. All statistical analyses were performed using SPSS 20.0 software. P values less than 0.05 were considered significant.
Results
Characteristics and Clinical Outcomes of Involved Patients
A total of 1443 patients diagnosed with COVID-19 were included in our study, 256 of whom had diabetes (17.74%). Patients with diabetes were older (66.0 [IQR 58.0–73.8] vs. 53.0 [IQR 37.0–66.0]) and had higher frequencies of cerebrovascular disease (23.4% vs. 6.8%), coronary heart disease (23.8% vs. 8.2%), heart failure (3.9% vs. 1.7%), hypertension (68.0% vs. 26.0%), digestive disorder (36.7% vs. 29.7%, including gastritis, gastric ulcer, and duodenal ulcer), COPD (4.7% vs. 2.2%), solid tumor (6.6% vs. 3.5%), and chronic renal disease (14.8% vs. 3.3%). The most common symptom for both groups was fever (63.8%), followed by cough (47.8%). Fatigue and chest tightness were less common. Patients with diabetes had more fever (85.9% vs. 66.3%) and felt sick and vomiting (7.8% vs. 4.5%). According to chest CT images, 181 (70.7%) patients with diabetes showed bilateral pneumonia, and the incidence was higher than that of those without diabetes [739 (62.3%)].
Major laboratory markers were tracked on admission. The blood test results of all patients on the day of hospital admission showed normal leukocyte counts. Patients with diabetes had higher levels of leukocytes and neutrophils and lower levels of lymphocytes and monocytes. Moreover, C-reactive protein (CRP), another indicator of inflammation, was significantly higher in patients with diabetes than in patients without diabetes (2.6 [IQR 0.5–5.5] vs. 0.7 [IQR 0.1–3.0]). These data showed that patients with COVID-19 and diabetes have a higher inflammatory state. Hemoglobin was below the normal range in all patients, and the hemoglobin and albumin level and albumin-to-globulin ratios were lower in patients with diabetes. Indicators of coagulation function disorder and organ dysfunction were more serious in patients with diabetes. These results indicated that organ dysfunction and metabolic disorders were more obvious in patients with diabetes than in patients without diabetes, which may signify a poorer prognosis of COVID-19.
Patients with diabetes had a greater occurrence of septic shock (3.5% vs. 1.0%) and ARDS (acute respiratory distress syndrome, 25.0% vs. 11.5%) and were more likely to develop severe (41.8% vs. 35.6%) and critical (34.0% vs. 14.9%) disease. Moreover, patients with pre-existing diabetes received significantly more intensive integrated treatments to manage their symptoms of COVID-19 than those without diabetes. Antibiotics, antifungal drugs, glucocorticoids, and invasive and noninvasive mechanical ventilation were more widely used in patients with diabetes, who had longer hospital stays (22.5 [IQR 15–34.8] vs. 16 [IQR 10–24]) and higher mortality (21.1% vs. 7.0%) (Table 1).
Risk Factors Associated with Disease Severity of Patients with COVID-19
To elaborate on the factors related to disease severity, we divided patients with COVID-19 with and without diabetes into three subgroups: medium, severe, and critical (Table 2 and Table S1). As shown in Table 2, in both patients with and without diabetes, the disease severity increased with age, but there were no significant differences of age (P = 0.309) in the three subgroups of patients with diabetes; however, the difference was obvious in patients without diabetes (P = 0.000), as most patients under 40 years old had moderate disease, and with the increase of age, patients over 60 years old were more likely to develop critical disease. In patients without diabetes, the disease profile of female patients was mostly moderate to severe, while that of male patients was more likely to develop into critical disease.
Among the chronic complications, the proportions of cerebrovascular disease, coronary heart disease, digestive disorders, and COPD were significantly different in the subgroups (moderate, severe, and critical) of patients with and without diabetes, indicating that those complications were closely related to disease severity in patients with COVID-19, whether they had diabetes or not, as shown in Table 2 and Table S2. However, there were no significant differences in the proportion of heart failure (P = 0.562), hypertension (P = 0.406), solid tumor (P = 0.194), chronic renal disease (P = 0.055), and hepatitis (P = 0.186) among different subgroups of patients with diabetes. The proportion of heart failure (P = 0.000) and hypertension (P = 0.000) were significantly different among subgroups of patients without diabetes, and the higher the proportion of those complications, the more severe was the patient's condition.
In terms of treatment, the application of glucocorticoids and immunoglobulin was closely related to the severity of the disease. The more severe the patient’s condition on admission, the greater was the likelihood of glucocorticoids and immunoglobulin administration.
Risk Factors for Mortality in Patients with COVID-19 with or Without Diabetes
To further identify the risk factors related to the mortality of critically ill patients with COVID-19, we divided critically ill patients into two subgroups based on disease outcomes: death and survival. As shown in Table 3, the mortality rate of critical patients with COVID-19 and diabetes was 62.1% (54/87) and that of patients with COVID-19 without diabetes was 46.9% (83/177). Age was undoubtedly an important indicator of disease outcome in critically ill patients; the older the patient, the higher was the risk of death. Furthermore, the age of non-survivors in patients with COVID-19 and diabetes was younger than that in patients without diabetes (69.5 [IQR 53.5–81.3] vs. 75.0 [IQR 66.0–85.0]). Regardless of whether patients with COVID-19 had diabetes or not, those with cerebrovascular disease and chronic kidney disease had higher mortality. Combined with Table 2, cerebrovascular disease was closely related to the disease severity and mortality of patients with COVID-19, which may be an effective indicator to evaluate the disease progression and prognosis of patients with COVID-19, while hypertension may be an independent risk factor for progression and outcome only in patients with COVID-19 without diabetes.
In the blood test parameters in Table 3, we observed that the levels of leukocytes, neutrophils, serum urea, serum creatinine, creatine kinase isoenzyme, and procalcitonin were associated with a poor prognosis in patients with COVID-19. The levels of hemoglobin, prothrombin time, albumin, albumin-to-globulin ratio, alpha-hydroxybutyrate dehydrogenase, B-type brain natriuretic peptide, and troponin were different between survivor and non-survivor in patients without diabetes, but not in patients with diabetes. Lung CT imaging data showed that among the survivors, the proportion of patients with double pneumonia and multiple military mottling and ground-glass opacities was higher.
In critical patients with COVID-19 and diabetes, there were no significant differences in the use of antibiotics, antivirals, and glucocorticoids between survivors and non-survivors. We found a positive correlation between the use of immunoglobulin and survival in patients with COVID-19 and diabetes.
Risk Factors for Non-survivors in the Critical Group with Diabetes
The significant risk factors (Table 3) were analyzed using binary logistic regression taking death as the dependent variable. Nine variables, namely age, cerebrovascular disease, chronic renal disease, bilateral pneumonia, multiple military mottling and ground-glass opacities, immunoglobulin, noninvasive mechanical ventilation, leukocyte and neutrophil count, were independent risk factors for in-hospital death in patients with COVID-19 and diabetes. Even after adjustment for age, cerebrovascular disease, chronic renal disease, bilateral pneumonia, multiple military mottling and ground-glass opacities, immunoglobulin, and noninvasive mechanical ventilation, the counts of leukocytes and neutrophils maintained a significant association with a lower odds ratio (OR) for risk of death in the critical group with diabetes (all P < 0.05) (Table 4).
To further illustrate the relationship between the application of immunoglobulin or noninvasive mechanical ventilation and mortality in critical patients with COVID-19 and diabetes, we analyzed the characteristics of those patients who use immunoglobulin and noninvasive mechanical ventilation or not, and found that in immunoglobulin-free group, the rates of hypertension and mortality were higher (Table S3); after adjustment for hypertension, there was still a significant association between immunoglobulin use and mortality in critically ill patients with diabetes (Table 4). Whereas, patients who did not use noninvasive mechanical ventilation had higher rate of cerebrovascular disease and mortality, and the incidence of ARDS and use of glucocorticoids were lower (Table S4). After adjustment for cerebrovascular disease, ARDS, and glucocorticoids, we found that noninvasive mechanical ventilation was not associated with mortality of critically ill patients with COVID-19 and diabetes (Table 4).
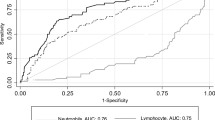
A ROC curve analysis was performed to verify the diagnostic accuracy of the count of leukocytes and neutrophils for the risk of death in the critical group with diabetes. The area under the curve (AUC) for leukocytes and neutrophils was 0.68 (95% CI 0.57–0.80, P < 0.01) and 0.65 (95% CI 0.53–0.76, P < 0.05), respectively. The optimal cutoff points for leukocytes and neutrophils were 5.37 × 109/L and 8.72 × 109/L, respectively. At this level, the Youden index was 0.35 (leukocytes) and 0.34 (neutrophils); sensitivity was 74.07% (leukocytes, 95% CI 0.60–0.85) and 42.59% (neutrophils, 95% CI 0.27–0.57); and specificity was 60.61% (leukocytes, 95% CI 0.42–0.77) and 90.91% (neutrophils, 95% CI 0.76–0.98). The AUC for leukocytes was higher than that for neutrophils (Fig. 1a, b). Therefore, leukocytes may be a better predictive marker (cutoff point 5.37 × 109/L) for the risk of death in the critical group with diabetes.
a, b ROC analysis of leukocytes and neutrophils for the risk of death in the critical group with diabetes (n = 87). c, d Kaplan–Meier survival curve for critically ill patients with COVID-19 and diabetes with different counts of leukocytes (P = 0.0448) and neutrophils (P = 0.1426), and who use immunoglobulin or not (e)
The Kaplan–Meier survival curve also showed a trend toward poorer survival in patients with COVID-19 and diabetes whose leukocytes were > 5.37 × 109/L than for those whose leukocytes were ≤ 5.37 × 109/L (P = 0.0448), and the HR was 1.784 (95% CI 1.014–3.140) (Fig. 1c). However, there was no difference in survival time between patients with COVID-19 and diabetes whose neutrophils were > 8.72 × 109/L and those whose neutrophils were ≤ 8.72 × 109/L (P = 0.1426). Moreover, patients treated with immunoglobulin had longer survival times than patients who did not receive IVIG, P < 0.05 [HR 0.5278 (95% CI 0.2891–0.9621)].
Discussion
Our study analyzed the characteristics of patients with COVID-19 with and without diabetes. Among patients hospitalized with COVID-19, the prevalence of diabetes was 17.7%. Patients with diabetes were older (66.0 [IQR 58.0–73.8]) and more likely to have chronic complications. Consistent with previous publications [7, 8], the most common symptoms for patients with COVID-19 were fever and cough. Patients with diabetes were more likely to suffer bilateral pneumonia, more severe organ dysfunction, and metabolic disorder, so they had a greater occurrence of septic shock and ARDS, more severe disease, and a significantly higher mortality. Since diabetes has more significant harmful effects on microvascular and macrovascular systems and digestive system functions [9] when cerebrovascular diseases, coronary heart disease, hypertension, and digestive disorders coexist with diabetes, they affect each other, forming a vicious cycle, and patients' conditions are more likely to develop into critical illness.
Based on the pathological mechanism of diabetes and its influence on other systems (immune system, etc.) [10, 11], immune dysregulation (impaired neutrophil function and reduced T cell-mediated immune response [12]) and the exaggerated pro-inflammatory cytokine response [13] might be the key drivers of poor clinical outcomes in patients with COVID-19 and diabetes. Moreover, the cell surface receptor for SARS-CoV-2, angiotensin-converting enzyme 2 (ACE2) [14], can be upregulated by thiazolidinediones (a class of insulin sensitizer), which may have contributed to the disease progression of patients with COVID-19 and diabetes. The difference of disease profile between male and female individuals may be due to the high expression of ACE2 in the testis, which increased the duration of SARS-CoV-2 virus in the body and made it more difficult to clear the virus, thus causing higher disease severity in male patients [15].
With the increase in disease severity, patients' inflammatory indicators, d-dimer and fibrinogen levels, and hepatic and renal dysfunction indicators were significantly upregulated. Blood glucose levels on admission were also elevated with the increase in disease severity, and it was higher and changed more significantly in patients with COVID-19 and diabetes. Infection of SARS-CoV-2 in patients with diabetes might trigger a stress response and increased secretion of hyperglycemic hormones, such as glucocorticoids and catecholamines, which results in elevated blood glucose, abnormal glucose variability, and diabetic complications. The use of glucocorticoids for treatment will also have the aforementioned negative effects. Although there was no significant association between blood glucose levels on admission and mortality in patients with COVID-19, timely and standardized blood glucose management for patients with COVID-19 and diabetes is urgently needed. Li et al. found that, compared with individuals with poor blood glucose control (blood glucose variability in the upper limit of 10.0 mmol/L), the mortality rate of individuals with good blood glucose control (blood glucose variability in the range of 3.9–10.0 mmol/L) was significantly reduced (1.1% vs. 11.0%). Moreover, good blood glucose control will enable cured patients to have a better state of recovery after a negative viral nucleic acid test, with less multiorgan dysfunction. Therefore, good blood glucose control is an effective auxiliary measure for the treatment of patients with COVID-19 [16].
Leukocytes > 5.37 × 109/L was associated with a higher risk of death and shorter survival time in patients with COVID-19 and diabetes. Leukocytes and neutrophils are indicators of inflammation. Critical patients with COVID-19 exhibited extremely high inflammatory parameters [17], and previous studies reported that the association between diabetes and lung dysfunction may be partly explained by systemic inflammation [18, 19]. Therefore, consideration of inflammatory responses is necessary when clinically managing patients with diabetes who have COVID-19, and the determination of how to block inflammation and when to initiate anti-inflammatory therapy is critical for reducing the death rate of COVID-19.
Consistent with previous studies [20], our binary logistic regression analysis showed that age, cerebrovascular disease, and chronic renal disease were independent risk factors for death in patients with COVID-19 and diabetes. Studies have shown that hypertension was the most common comorbidity in patients with COVID-19, followed by diabetes and coronary heart disease [20], and hypertension was a risk factor for disease progression in patients with COVID-19 [21]. However, we found no association between hypertension and poor outcomes in patients with COVID-19 and diabetes, but did find an association in patients with COVID-19 without diabetes, which may demonstrate that the impact of diabetes on disease severity and mortality in patients with COVID-19 was greater than that of hypertension. Age-dependent decreases in cellular and humoral immune function in elderly patients have been reported before, especially with regard to adaptive immune function [22]. The high risks of elderly patients with diabetes could be due to their poor overall health condition and greater number of comorbidities [7].
In terms of treatment measures, we found that the use of immunoglobulin increased with the severity of the disease, and it was associated with lower death in patients with COVID-19 and diabetes. We found that albumin, hemoglobin level, and the albumin-to-globulin ratio were obviously lower in patients with COVID-19 and diabetes than in those without diabetes, and the levels decreased with increasing disease severity. Moreover, these indicators were lower in patients who died than those who survived, although there was no significant difference, suggesting that patients’ nutritional status and immune function were worsening with the progression of the disease. IVIG could significantly increase the serum IgG level, not only improving the patient's ability to resist infections and reduce the incidence of complications but also significantly reducing the duration of antibiotic use and hospital stay [23]. IVIG plays an important role in modulating immune function, especially in a hyperinflammatory state. Therefore, active and adequate use of immunoglobulin may be an effective means to reduce mortality in critically ill patients with COVID-19 and diabetes.
Diabetes is a chronic inflammatory metabolic disease that is accompanied by damage to multiple organ system functions, such as the cardiovascular, cerebrovascular, kidney, and digestive systems [9]. Patients with COVID-19 were in a hyperinflammatory state, especially critically ill patients, who were more likely to suffer “cytokine storm”; therefore, during the progression of disease, the inflammatory biomarkers and metabolic or organ dysfunction indicators were not significantly different among the subgroups (moderate, severe, and critical) in patients with COVID-19 and diabetes. This phenomenon also suggested that diabetes played a vital role in influencing disease severity and mortality in patients with COVID-19, and the changes in many indicators (such as hypertension and heart failure) were not sufficient to affect the disease progress in patients with COVID-19 and diabetes.
As a result of the retrospective nature of the study and the unprecedented scale of the COVID-19 pandemic, this study has several limitations. (1) We have not distinguished “diabetes” as type 1 diabetes and type 2 diabetes. (2) Missing data on some variables, such as detailed information on blood parameters, may cause bias in the estimation and a reduction in the representativeness of the samples. (3) The laboratory parameters were measured upon admission and may indicate the severity of COVID-19. The causal relationship between abnormal laboratory findings and severity could not be determined. (4) Other diabetes-associated parameters, including glycated hemoglobin, “peak levels” or “postprandial levels” of plasma glucose could better reflect the association of plasma glucose control and mortality in patients with COVID-19 if that data was available.
Conclusion
Compared with patients with COVID-19 without diabetes, patients with comorbid diabetes had more severe disease and higher mortality. Age, cerebrovascular disease, coronary heart disease, digestive disorders, and COPD were associated with disease severity in patients with or without diabetes, while heart failure and hypertension were related to disease severity in patients without diabetes only. More attention should be paid to patients with COVID-19 and diabetes, especially when they have high leukocyte (> 5.37 × 109/L) and neutrophil counts (> 8.72 × 109/L), older age, cerebrovascular disease, or chronic kidney disease, owing to cases of missed diagnosis and rapid disease deterioration. Leukocytes (> 5.37 × 109/L) were associated with higher mortality and shorter survival time in critically ill patients with COVID-19 and diabetes. In clinical practice, timely and adequate immunoglobulin use in critical patients may reduce the mortality of patients with COVID-19 and diabetes.
References
Guan WJ, Ni ZY, Hu Y, et al. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. 2020;382(18):1708–20. https://doi.org/10.1056/NEJMoa2002032.
Wu Z, McGoogan JM. Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: summary of a report of 72314 cases from the Chinese Center for Disease Control and Prevention. JAMA. 2020. https://doi.org/10.1001/jama.2020.2648.
Yang X, Yu Y, Xu J, et al. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. Lancet Respir Med. 2020;8(5):475–81. https://doi.org/10.1016/s2213-2600(20)30079-5.
World Health Organization. Clinical management of severe acute respiratory infection when novel coronavirus (2019-nCoV) infection is suspected: interim guidance. WHO. 2020. https://apps.who.int/iris/bitstream/handle/10665/330893/WHO-nCoV-Clinical-2020.3-eng.pdf?sequence51&isAllowed5y. Accessed 28 Jan 2020.
Wu Z, McGoogan JM. Characteristics of and important lessons from the coronavirus disease 2019 (COVID-19) outbreak in China: summary of a report of 72,314 cases from the Chinese Center for Disease Control and Prevention. JAMA. 2020. https://doi.org/10.1001/jama.2020.2648.
Wang D, Hu B, Hu C, et al. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan China. JAMA. 2020. https://doi.org/10.1001/jama.2020.1585.
Shi Q, Zhang X, Jiang F, et al. Clinical characteristics and risk factors for mortality of COVID-19 patients with diabetes in Wuhan, China: a two-center, retrospective study. Care Diabetes. 2020. https://doi.org/10.2337/dc20-0598.
Chen N, Zhou M, Dong X, et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet. 2020;395(10223):507–13. https://doi.org/10.1016/s0140-6736(20)30211-7.
Morsi M, Maher A. A shared comparison of diabetes mellitus and neurodegenerative disorders. J Cell Biochem. 2018;119(2):1249–56. https://doi.org/10.1002/jcb.26261.
Ilonen J, Lempainen J, Veijola R. The heterogeneous pathogenesis of type 1 diabetes mellitus. Nat Rev Endocrinol. 2019;15(11):635–50. https://doi.org/10.1038/s41574-019-0254-y.
Cobo-Vuilleumier N, Lorenzo PI, Rodríguez NG, et al. LRH-1 agonism favours an immune-islet dialogue which protects against diabetes mellitus. Nat Commun. 2018;9(1):1488. https://doi.org/10.1038/s41467-018-03943-0.
Muller LM, Gorter KJ, Hak E, et al. Increased risk of common infections in patients with type 1 and type 2 diabetes mellitus. Clin Infect. 2005;41(3):281–8. https://doi.org/10.1086/431587.
Geerlings SE, Hoepelman AI. Immune dysfunction in patients with diabetes mellitus (DM). FEMS Immunol Med Microbiol. 1999;26(3–4):259–65. https://doi.org/10.1111/j.1574-695X.1999.tb01397.x.
Kuba K, Imai Y, Rao S, et al. A crucial role of angiotensin converting enzyme 2 (ACE2) in SARS coronavirus-induced lung injury. Nat Med. 2005;11(8):875–9. https://doi.org/10.1038/nm1267.
Shastri A, Wheat J, Agrawal S, et al. Delayed clearance of SARS-CoV2 in male compared to female patients: high ACE2 expression in testes suggests possible existence of gender-specific viral reservoirs. medRxiv. 2020. https://doi.org/10.1101/2020.04.16.20060566.
Zhu L, She ZG, Cheng X, et al. Association of blood glucose control and outcomes in patients with COVID-19 and pre-existing type 2 diabetes. Cell Metab. 2020. https://doi.org/10.1016/j.cmet.2020.04.021.
Zhang W, Zhao Y, Zhang F, et al. The use of anti-inflammatory drugs in the treatment of people with severe coronavirus disease 2019 (COVID-19): the perspectives of clinical immunologists from China. Clin Immunol. 2020;214:108393. https://doi.org/10.1016/j.clim.2020.108393.
Giovannelli J, Trouiller P, Hulo S, et al. Low-grade systemic inflammation: a partial mediator of the relationship between diabetes and lung function. Ann Epidemiol. 2018;28(1):26–322. https://doi.org/10.1016/j.annepidem.2017.11.004.
Chen H, Liu C, Cheng C, Zheng L, Huang K. Effects of apelin peptides on diabetic complications. Curr Protein Pept Sci. 2018;19(2):179–89. https://doi.org/10.2174/1389203718666170918154728.
Wu C, Chen X, Cai Y, et al. Risk factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan China. JAMA Intern Med. 2020. https://doi.org/10.1001/jamainternmed.2020.0994.
Jiang G, Cai Y, Yi X, et al. The impact of laryngopharyngeal reflux disease on 95 hospitalized patients with COVID-19 in Wuhan, China: a retrospective study. J Med Virol. 2020. https://doi.org/10.1002/jmv.25998.
Opal SM, Girard TD, Ely EW. The immunopathogenesis of sepsis in elderly patients. Clin Infect Dis. 2005;41(Suppl 7):S504–S512512. https://doi.org/10.1086/432007.
Elluru SR, Kaveri SV, Bayry J. The protective role of immunoglobulins in fungal infections and inflammation. Semin Immunopathol. 2015;37(2):187–97. https://doi.org/10.1007/s00281-014-0466-0.
Acknowledgements
We thank all health-care workers involved in the diagnosis and treatment of patients in Wuhan.
Funding
This study and the journal’s Rapid Service Fee were supported by the Health and Family Planning Commission of Wuhan City (WX18M02).
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Authorship Contributions
Concept and design: J Huang and S Jin. Acquisition, analysis, or interpretation of data: J Huang, L Zhu, XL Bai, X Jia, YJ Lu, AP Deng, JY Li and S Jin. Statistical analysis: J Huang and L Zhu. Drafting the paper: J Huang and L Zhu. J Huang and L Zhu contributed equally.
Disclosures
Juan Huang, Lin Zhu, Xiangli Bai, Xiong Jia, Yajing Lu, Aiping Deng, Juyi Li and Si Jin have nothing to disclose.
Compliance with Ethics Guidelines
The study was approved by the Wuhan Central Hospital ethics committee, and written informed consent was waived by the ethics commission because of the retrospective nature of this study.
Data Availability
The data used to support the findings of this study are included within the article. The datasets generated and analyzed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Huang, J., Zhu, L., Bai, X. et al. Multidimensional Analysis of Risk Factors for the Severity and Mortality of Patients with COVID-19 and Diabetes. Infect Dis Ther 9, 981–1002 (2020). https://doi.org/10.1007/s40121-020-00359-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40121-020-00359-6