Abstract
Introduction
The REGAL (RSV evidence—a geographical archive of the literature) series provide a comprehensive review of the published evidence in the field of respiratory syncytial virus (RSV) in Western countries over the last 20 years. This third publication covers the risk and burden of RSV infection in infants with chronic lung disease (CLD), formerly called bronchopulmonary dysplasia (BPD).
Methods
A systematic review was undertaken of publications between January 1, 1995 and December 31, 2015 across PubMed, Embase, The Cochrane Library, and Clinicaltrials.gov. Studies reporting data for hospital visits/admissions for RSV infection among infants with CLD/BPD who were not prophylaxed, as well as studies reporting RSV-associated morbidity, mortality, and healthcare costs, were included. Burdens of disease data were compared with preterm infants without CLD/BPD, other high-risk groups and term infants. Study quality and strength of evidence (SOE) were graded using recognized criteria.
Results
A total of 1837 studies were identified and 39 were included. CLD/BPD is a significant independent risk factor for RSV hospitalization [RSVH (odds ratio 2.2–7.2); high SOE]. Infants and young children with CLD/BPD had high RSVH rates which were generally similar in Europe, the United States, and Canada, mostly varying between 12 and 21%. Infants with CLD also had a longer length of hospital stay than other high-risk groups and term infants (high SOE). On average, infants spent 4–11 days in hospital (moderate SOE). Once hospitalized for RSV, affected children were at risk for a more severe course of disease than children with no RSVH (moderate SOE).
Conclusion
Severe RSV infection in infants and young children with CLD/BPD poses a significant health burden in Western countries. Further studies focussing on the burden of RSV infection in this well-recognized population at high risk for severe disease are needed to help improve outcomes and plan allocation of healthcare resources.
Funding
AbbVie.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Respiratory syncytial virus (RSV) is the most important cause of severe respiratory infection in infants, accounting for over 3 million hospitalizations worldwide each year [1]. Chronic lung disease (CLD) [formerly called bronchopulmonary dysplasia (BPD)] is the most common pulmonary complication of premature birth and increases the risk of RSV infection because it compromises lung function, distorts airway architecture, and promotes a pro-inflammatory milieu [2, 3]. Severe RSV infection is associated with substantial morbidity and constitutes a considerable burden on healthcare systems [4]. During the first 2 years of life, children with CLD/BPD are hospitalized for severe RSV at a higher rate than children born at term or more than 36 weeks gestational age (wGA) [5–7]. High-risk infants, including those with CLD/BPD, also have a significantly higher intensive care unit (ICU) admission rate and length of stay (LOS) in hospital, and require more invasive and longer respiratory support than near-term or full-term infants [8]. There is currently no curative treatment for RSV infection. Treatment focuses primarily on supportive measures, such as providing supplemental oxygen and ensuring adequate hydration. RSV immunoprophylaxis is the mainstay of disease prevention and is indicated for specific children at high risk of developing serious disease. Current published guidelines recommend that RSV immunoprophylaxis is offered to infants with CLD/BPD who require medical therapy, such as supplemental oxygen, bronchodilator, diuretic or chronic corticosteroid treatment, within 6 months before the onset of the RSV season [9–15].
New RSV therapeutics are currently being developed [16]. Therefore, it is important that there is a greater understanding of CLD/BPD as a condition leading to enhanced risk for severe RSV disease in order to improve preventative and management strategies, improve overall patient outcomes, and reduce the burden on healthcare systems. To provide a comprehensive understanding of severe RSV disease in Western societies, a panel of experts in RSV from the United States, Canada and Europe undertook an evidence-based search of the literature which has accumulated over the past two decades. REGAL (RSV Evidence—a Geographical Archive of the Literature) defines the current state of the art in our understanding of RSV as well as, importantly, identifying gaps in our knowledge and future areas of research. This paper, which represents the third in a series of seven publications covering a range of topics on RSV disease, identifies and describes the risks and associated morbidity and mortality of severe RSV infection requiring hospitalization in infants and young children with CLD/BPD in Western societies.
Methods
Study Objective
REGAL addresses seven specific research questions, covering: overall epidemiology, prematurity, CLD/BPD, congenital heart disease (CHD), long-term respiratory morbidity, other high-risk groups (e.g. Down syndrome), and prevention, management and future perspectives. The systematic reviews undertaken to answer each research question all use the same broad methodology, which has been described elsewhere [17]. The full protocol and generic search terms for the systematic reviews are available as part of the online supplement. In brief, a systematic and comprehensive search of the medical literature electronically indexed in PubMed, EMBASE, the Cochrane Library and clinicaltrials.gov was conducted. The detailed search strategy used free-text search terms combined with Medical Subject Headings (MeSH). As per the ambit of REGAL, only studies conducted in Western countries were included, which we defined as the United States, Canada, and Europe (including Turkey and the Russian Federation).
Literature Search
In this systematic literature review, we sought to answer the key question: “What is the morbidity, long-term sequelae and mortality of infants and young children with CLD/BPD due to severe RSV lower respiratory tract infection?”
The search for this systematic review included studies conducted in children ≤18 years old and published between January 1, 1995 and December 31, 2015. The target population was infants and young children with CLD/BPD who had ‘proven’ or ‘probable’ RSV and had or had not received RSV immunoprophylaxis. We retained only studies that reported RSV hospitalization (RSVH) and outcome data for infants and young children with CLD/BPD. However, studies with mixed pediatric populations hospitalized with RSV were also considered if there were sufficient data on infants and young children with CLD/BPD. We limited publications by excluding meta-analyses and review articles. No language limits were set on the database searches, with the caveat that English translations of at least the abstract had to be available.
The following general terms and limits were used in MEDLINE (PubMed), EMBASE and the Cochrane Library: “RSV” OR “respiratory syncytial virus” AND “lower respiratory tract infection” OR “bronchiolitis” OR “pneumonia” AND “chronic lung disease” OR “CLD” OR “bronchopulmonary dysplasia” OR “BPD” AND “hospitalization” OR “predisposition” OR “risk factor” AND “limits: human, child (birth to 18 years)”. The search results were supplemented by a review of the bibliographies of key articles for additional studies and inclusion of relevant abstracts presented at key meetings. Other significant studies of the target population, published during the drafting of the manuscript, were also included in the review, as identified by the authors. Two reviewers (Smith and Blake) undertook the search, with any disagreements resolved after discussion with a third reviewer (Rodgers-Gray) and Carbonell-Estrany. All authors reviewed the search results, made any additions and amendments, and approved the final list of studies for inclusion.
Definition of CLD/BPD
It is recognized that the working definitions of CLD and BPD have evolved over recent years, now targeting extremely preterm infants with structurally immature lungs and pulmonary vasculature due to a predominant arrest of lung growth as “new BPD” in contrast to the “original BPD” based on the Northway classification [18–23]. Since studies involving RSV do not uniformly include a definition of CLD/BPD, for completeness all reports describing infants with CLD/BPD were considered for inclusion in this review in order to elucidate the additional risk of RSV infection in infants with respiratory issues at birth. In general terms, we defined BPD in infants born at <32 weeks post-menstrual age as follows, based on established criteria [24]:
-
Mild BPD: oxygen requirement for the first 28 days but in room air at 36 weeks post-menstrual age
-
Moderate BPD: oxygen requirement for the first 28 days and oxygen <30% at 36 weeks post-menstrual age
-
Severe BPD: oxygen requirement for the first 28 days and oxygen >30% or continuous positive airway pressure (CPAP) or mechanical ventilation at 36 weeks post-menstrual age.
For infants born >32 weeks post-menstrual age, the definition was adjusted for the time endpoint of 56 days of life instead of 36 weeks post-menstrual age [25]. CLD was defined as the continuous need for oxygen or respiratory support beyond 36 weeks post-menstrual age.
Outcomes of Interest
The outcomes of interest for this review included hospitalization rates due to severe RSV infection, hospital LOS, ICU admission and LOS, oxygen requirement, need for and duration of mechanical ventilation and/or non-invasive ventilation, and case-fatality rates.
Evaluation of Data
Included publications were graded according to the Oxford Centre for Evidence-Based Medicine Levels of Evidence [26, 27]: level 1 evidence [local and current random sample surveys (or censuses)]; level 2 evidence (systematic review of surveys that allow matching to local circumstances); level 3 evidence (local non-random sample); and level 4 evidence (case-series). For each study, we also conducted a risk of bias assessment using the RTI Item Bank (score of 1 = very high risk of bias; score of 12 = very low risk of bias) for observational studies [28].
Statement of Ethics Compliance
The analysis in this article is based on previously published studies and does not involve any new studies of human subjects performed by any of the authors.
Results and Discussion
Articles Selected
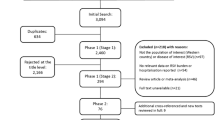
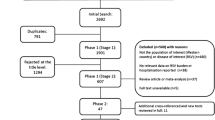
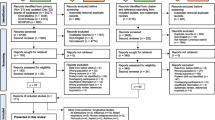
From the initial literature search, we identified 2422 potentially relevant articles, of which 592 were duplicates (Fig. 1). After phase 1 screening of the titles, 215 articles were considered and reviewed at abstract level, while 183 abstracts were rejected for not meeting the selection criteria, the majority because the studies did not focus on the population of interest (children ≤18 years old in Western countries) or disease of interest (RSV burden or hospitalization). Thirty-nine studies were included of which 32 were identified from the literature search and an additional 7 from reference lists/other sources. Data extraction tables for all 39 studies, including evidence grades and risk of bias assessments can be found in the online supplement.
Incidence of RSV Hospitalization
Studies from the United States, Canada and Europe have shown that infants with CLD/BPD, particularly those born prematurely, are at high risk for RSV-associated hospitalizations in the first 2 years of life [5, 29–46]. Across a number of studies, CLD/BPD had the highest or, in one case, the second highest, odds ratio (OR) of all independently significant risk factors for RSVH (Table 1). In a retrospective cohort study of 1721 premature infants [23–36 weeks gestational age (wGA)], CLD, defined as ≥28 days of perinatal oxygen, was found to be a significant risk factor for RSVH (OR 3.7; P < 0.001 vs. those who required <28 days of oxygen) [32]. Similarly, in a population-based cohort study of 1103 infants born <35 wGA, CLD, defined as oxygen requirement beyond 36 weeks post-conceptual age, was found to be independently associated with RSVH [adjusted OR 3.99, 95 % confidence interval (CI) 1.4–11.2] [31]. When restricted to studies using a definition of ‘a continued need for oxygen therapy at 36 weeks post-conceptual age’, the OR for RSVH was 2.2–3.99. Overall, studies report ORs of between 2.2 and 7.2 for CLD/BPD as a risk factor for RSVH.
The reported incidence of RSVH in infants and young children with CLD/BPD who had not received RSV immunoprophylaxis varies between 12 and 46%, with 8 of 10 studies reporting an incidence of between 12 and 21% (Table 2) [6, 31, 32, 36, 41, 48–52]. In the Munich RSV study, the risk of RSVH was higher in preterm infants (≤35 wGA) with CLD compared with preterm infants (≤35 wGA) without CLD (15.0% vs. 4.4%) [31]. Taken together and discounting any heterogeneity across study populations, the average, weighted incidence of RSVH among 895 children with BPD/CLD in the identified studies (Table 2) was 16.8%. When limited to studies with a definition of BPD/CLD as ‘a continued need for oxygen at 36 wGA’, the weighted mean was also 16.8%.
During the first 2 years of life, children with CLD/BPD are hospitalized for severe RSV at a higher rate than children born at term (≥36 wGA) [5–7]. There is also some evidence that children with CLD/BPD have higher RSVH rates than those with CHD [7] or preterm infants without comorbidities [5, 7]. In a retrospective cohort study of all children <3 years old enrolled in the Tennessee Medicaid program from July 1989 through June 1993 (248,652 child-years), the estimated RSVH rate per 1000 children in the first and second year of life was higher for those with BPD compared with other high-risk populations (Table 3) [7]. A population-based cohort study performed in the UK also reported higher RSVH rates during the first year of life among infants with CLD [56.2 per 1000 infants (95% CI 49.9–63.2)] compared with those born prematurely [47.3 per 1000 infants (95% CI 44.4–50.2)] and those born at term [22.4 per 1000 infants (95% CI 21.8–22.9)] [5]. In contrast, a Finnish study [6] showed that whilst significantly higher RSVH rates were reported for children with CLD than for children born at >36 wGA without CLD (12.0% vs. 1.9%; P = 0.003), differences in the admission rates between children with CLD and those born at ≤35 wGA were not significant. Comparing rates observed in various studies, particularly in children with CLD/BPD, is extremely difficult because of differences in methodology and the demographics of the study populations.
Data suggest that RSVH rates for infants with CLD/BPD have steadily decreased over the past 15 years [42, 53]. Findings from an 11-year cohort study (1998–2008) conducted in the US suggest that RSVH in children aged <2 years with CLD have steadily decreased even while all-cause hospitalizations in this high-risk population remained unchanged [53]. On average, about 966 hospitalizations for RSV (range 98–1373) per year were reported for children aged <2 years with CLD. Over the study period, the predicted rate of RSVH decreased significantly, by 48% (from 93.78 to 49.06 per 1 million children; P = 0.013). The authors suggest reasons for this decrease may include improved neonatal intensive care unit (NICU) and outpatient management of CLD, and possibly increased use of RSV immunoprophylaxis in this high-risk population [53].
Morbidity and Healthcare Resource Utilization
Studies have demonstrated that hospitalization due to RSV infection among infants with CLD/BPD not only leads to an increased risk of morbidity but also increased healthcare resource utilization, including admission to NICU, oxygen supplementation, and mechanical ventilation [8, 30, 38, 41, 51, 54–59]. The typical length of stay in hospital for RSV infection for infants with CLD/BPD is 4–11 days compared to 2–5 days in premature or term infants without CLD/BPD (Table 4) [38, 41, 51, 57, 58]. Multivariate analyses have shown CLD/BPD to be significantly and independently associated with a complicated course of disease and use and duration of mechanical ventilation [54, 55]. BPD (oxygen dependency beyond 28 days) has been associated with a requirement for extracorporeal membrane oxygenation (ECMO) support (OR 11.8, 95% CI 2.2–63.1; P = 0.004) [54].
Data from the Canadian PICNIC (Pediatric Investigators Collaborative Network on Infections in Canada) study [60] showed that there were no significant differences among infants with BPD and those with other pulmonary disorders (cystic fibrosis, recurrent aspiration pneumonitis, pulmonary malformation, neurogenic disorders interfering with pulmonary toilet, and tracheoesophageal fistula) for the morbidity measures: duration of hospitalization, ICU admission, duration of ICU stay, mechanical ventilation and duration of mechanical ventilation (overall hospitalization rate: 91 for infants with BPD vs. 68 for infants with other pulmonary disorders). However, the relatively small sample sizes of the respective sub-populations may have influenced the findings [60].
Greenough et al. [50] reported that preterm infants with CLD who require hospitalization for RSV infection have significantly greater morbidity in the first 2 years after birth than those without RSV infection. In this retrospective study, 235 preterm infants (<32 wGA) who were admitted to NICU during the first week after their birth and subsequently developed CLD (defined as an oxygen dependency beyond 28 days after birth) were followed until they were 2 years of age. Forty-five infants (19 %) had at least one hospital admission for a proven RSV infection. Compared with preterm infants (<32 wGA) with CLD/BPD with probable bronchiolitis and those with other respiratory problems, preterm infants with CLD/BPD and proven RSV infection had a longer length of stay in hospital (median: 21 vs. 6.5 and 8 days, respectively; P < 0.001) and longer duration of stay in pediatric wards (median 16 vs. 4.5 and 6 days, respectively). Outpatient attendances per infant during the first 2 years of life were also significantly higher in the RSV proven group (P < 0.01), as were primary care consultations for respiratory illnesses (P < 0.05) compared with the other groups [50]. Findings from a subsequent retrospective study of 190 of the original cohort of 235 children with CLD, published in 2004, showed that children who had been hospitalized with a proven RSV infection in the first 2 years required more health care for respiratory problems in years 2–4 inclusive [61].
These retrospective studies demonstrate that severe RSV infection in preterm children with CLD/BPD causes considerable morbidity, as indicated by their significantly higher use of health care resources compared to full-term children hospitalized for RSV infection [38, 41, 50, 51, 57, 58, 61]. However, too few data are available on infants with CLD/BPD admitted to NICU to allow more detailed conclusions to be drawn. This highlights the need for more studies specifically considering severe RSV infection in infants with CLD/BPD, as the majority of data in this high-risk group come from mixed populations of previously healthy children and preterm infants with and without CLD/BPD.
Healthcare Costs
Data from the published literature show that RSVH in preterm infants with CLD is associated with substantial healthcare costs [4, 50, 61, 62]. In the 2001 retrospective study by Greenough et al. [50], preterm infants with CLD who had a proven RSV infection generated significantly higher costs of care, approximately three times those who were RSV-negative. In the subsequent study, published in 2004, costs were assessed over a 3-year period when the children were aged 2–4 years [61]. Compared with the non-RSVH group, these infants continued to incur significantly greater costs of care for respiratory problems in later childhood [median £2630 (€4000, US $4800), range £124–18,091 vs. £1360 (€2500, US $3000), range £5–18,929] [61]. In a population-based cohort study of 3458 infants and children hospitalized for severe RSV infection during the RSV seasons 1996–1997 to 1999–2000 in the Netherlands, RSVH costs were higher for infants with BPD (€5785) than for other high-risk groups, including those with lower gestational age (€5555), and lower birth weight (€3895). The authors observed that the differences in RSVH costs were mainly due to a longer duration of hospitalization [4]. Similarly, an observational, retrospective survey in Spain that analysed all RSVHs for children up to 5 years of age reported during the 1997–2011 period found that the average LOS and hospital costs were significantly higher in high-risk children, including those with BPD [62].
Estimates of RSVH costs have been reported in other studies, but these were not differentiated by patient characteristics such as CLD/BPD, making comparisons difficult.
Case-Fatality Rates
Few studies in the published literature on RSVH report case-fatality rates in infants with CLD/BPD, and therefore it is difficult to ascertain from the available data the precise number of true RSV deaths in this high-risk population. There are currently no data to suggest that case-fatality rates are higher in those children with CLD/BPD than in healthy term children or premature children without CLD/BPD [38, 51, 58, 63, 64].
Limitations
There are two main limitations that merit consideration. First, the changing definitions of CLD/BPD over time may have affected the cross-comparisons that were generated between studies. Second, there was a lack of studies specifically investigating CLD/BPD. The majority of the studies identified comprised mixed populations, a proportion of which had CLD/BPD. In addition, other factors, such as improvements in medical practice over time and the type of RSV testing and surveillance systems employed will have influenced interpretation of the results. New studies should recognize that the established criteria for the definition of BPD [24, 65] may be used as a framework but are in a state of evolution [18, 22, 66] and, ideally, should include control for prematurity (stratified by gestational age) as another well-recognized risk factor for RSVH. This will enable more meaningful comparisons between studies and thereby a more reliable assessment of the true burden of RSV infection in this at-risk population.
Conclusions
This review has assessed, quantified and summarized all the key evidence for the burden of RSV infection in infants and young children with CLD/BPD in Western countries over the last 20 years. Data show that this specific population are particularly susceptible to developing severe RSV disease necessitating re-hospitalization and medical therapy, including supplemental oxygen and mechanical ventilation, following discharge from NICUs. Data suggest that the course of illness is more severe in children with CLD/BPD compared with otherwise healthy preterm infants and is associated with longer duration of hospital stay. Rates of RSVH among this high-risk group in European countries appear to be generally similar to those in the United States and Canada.
This systematic review provides further evidence that severe RSV infections in infants and young children with CLD/BPD still pose a significant health burden in Western countries. Most of our knowledge, however, has come from studies conducted more than a decade ago. These findings highlight the need for more up-to-date studies of the relative importance of CLD/BPD as a risk factor for severe RSV disease. Improved surveillance of this population will provide a more informative insight into the burden of disease to help improve outcomes and plan allocation of health care resources.
Summary box
Key statements/findings | Level of evidencea |
|---|---|
CLD/BPD is a highly significant independent risk factor for RSVH (OR 2.2–7.2) | Level 1 (level 1 studies: n = 2; risk of biasb: 11.0) |
CLD/BPD has been associated with a higher rate of RSVH than other high-risk groups (e.g. CHD, preterm without comorbidities) and term infants | Level 1 (level 1 studies: n = 3; risk of biasb: 10.7) |
The reported incidence of RSVH in infants and young children with CLD/BPD who have not received RSV immunoprophylaxis mostly varies between 12 and 21% | Level 1 (level 1 studies: n = 3; risk of biasb: 10.7) |
Median stay in hospital for RSV infection in children with CLD/BPD is 4–11 days | Level 1–2 (level 1 studies: n = 1; level 2 studies: n = 2; risk of biasb: 10.7) |
CLD/BPD is significantly and independently associated with a complicated course of disease, involving use and duration of mechanical ventilation and requirement for ECMO support | Level 1–3 (level 1 studies: n = 1; level 3 studies: n = 1; risk of biasb: 10.0) |
Key areas for research | |
More up-to-date research and specific studies are needed on the burden of severe RSV infection in infants and young children with CLD/BPD | |
Comparison of the morbidity and mortality incurred by infants with “OLD” versus “NEW” CLD/BPD | |
References
Nair H, Nokes DJ, Gessner BD, Dherani M, Madhi SA, Singleton RJ, et al. Global burden of acute lower respiratory infections due to respiratory syncytial virus in young children: a systematic review and meta-analysis. Lancet. 2010;375:1545–55.
Hilgendorff A, Reiss I, Ehrhardt H, Eickelberg O, Alvira CM. Chronic lung disease in the preterm infant. Lessons learned from animal models. Am J Respir Cell Mol Biol. 2014;50:233–45.
Piedmonte G, Perez MK. Respiratory syncytial virus and bronchiolitis. Pediatr Rev. 2014;35:519.
Rietveld E, De Jonge HC, Polder JJ, Vergouwe Y, Veeze HJ, Moll HA, et al. Anticipated costs of hospitalization for respiratory syncytial virus infection in young children at risk. Pediatr Infect Dis J. 2004;23:523–9.
Murray J, Bottle A, Sharland M, Modi N, Aylin P, Majeed A, Medicines for Neonates Investigator Group, et al. Risk factors for hospital admission with RSV bronchiolitis in England: a population-based birth cohort study. PLoS ONE. 2014;9:e89186.
Heikkinen T, Valkonen H, Lehtonen L, Vainionpää R, Ruuskanen O. Hospital admission of high risk infants for respiratory syncytial virus infection: implications for palivizumab prophylaxis. Arch Dis Child Fetal Neonatal Ed. 2005;90:F64–8.
Boyce TG, Mellen BG, Mitchel EF Jr, Wright PF, Griffin MR. Rates of hospitalization for respiratory syncytial virus infection among children in Medicaid. J Pediatr. 2000;137:865–70.
Berger TM, Aebi C, Duppenthaler A, Stocker M, Swiss Pediatric Surveillance Unit. Prospective population-based study of RSV-related intermediate care and intensive care unit admissions in Switzerland over a 4-year period (2001–2005). Infection. 2009;37:109–16.
American Academy of Pediatrics Committee on Infectious Diseases, American Academy of Pediatrics Bronchiolitis Guidelines Committee. Updated guidance for palivizumab prophylaxis among infants and young children at increased risk of hospitalization for respiratory syncytial virus infection. Pediatrics. 2014;134:415–20.
Robinson JL, Le Saux N, Canadian Paediatric Society, Infectious Diseases and Immunization Committee. Preventing hospitalizations for respiratory syncytial virus infection. Paediatr Child Health. 2015;20:321–33.
Bollani L, Baraldi E, Chirico G, Dotta A, Lanari M, Del Vecchio A, Italian Society of Neonatology, et al. Revised recommendations concerning palivizumab prophylaxis for respiratory syncytial virus (RSV). Ital J Pediatr. 2015;41:97.
Figueras Aloy J, Carbonell Estrany X, Comité de Estándares de la SENeo, et al. Update of recommendations on the use of palivizumab as prophylaxis in RSV infections. An Pediatr (Barc). 2015;82:199e1–2.
Mori M, Kawashima H, Nakamura H, Nakagawa M, Kusuda S, Saji T, et al. Nationwide survey of severe respiratory syncytial virus infection in children who do not meet indications for palivizumab in Japan. J Infect Chemother. 2011;17:254–63.
Chi H, Hsu CH, Chang JH, Chiu NC, Hung HY, Kao HA, et al. A novel six consecutive monthly doses of palivizumab prophylaxis protocol for the prevention of respiratory syncytial virus infection in high-risk preterm infants in Taiwan. PLoS ONE. 2014;27(9):e100981.
AlAql F, Al-Hajjar S, Bin Mahoud L, Al-Alaiyan S, Tufenkji H, Abuzaid S, et al. Guidelines for palivizumab prophylaxis in infants and young children at increased risk for respiratory syncytial virus infection in Saudi Arabia. Int J Pedatric Adolesc Med. 2016;3:38–42.
Mazur NI, Martinón-Torres F, Baraldi E, Fauroux B, Greenough A, Heikkinen T, et al. Lower respiratory tract infection caused by respiratory syncytial virus: current management and new therapeutics. Lancet Respir Med. 2015;3:888–900.
Bont L, Checchia P, Fauroux B, Figueras-Aloy J, Manzoni P, Paes B, et al. Defining the epidemiology and burden of severe respiratory syncytial virus infection among infants and children in western countries. Infect Dis Ther. 2016 (Epub ahead of print).
Jensen EA, Schmidt B. Epidemiology of bronchopulmonary dysplasia. Birth Defects Res A. 2014;100:145–57.
Bancalari E. Is persistent need for supplemental oxygen a good indicator of adverse pulmonary outcome in very immature infants? Arch Dis Child Fetal Neonatal Ed. 2014;99:F254–5.
Jain D, Bancalari E. Bronchopulmonary dysplasia: clinical perspective. Birth Defects Res A. 2014;100:134–44.
Northway WH Jr, Rosan RC, Porter DY. Pulmonary disease following respiratory therapy of hyaline-membrane disease: bronchopulmonary dysplasia. N Engl J Med. 1967;276:357–68.
Maitre NL, Ballard RA, Ellenberg JH, Davis SD, Greenberg JM, Hamvas A, Prematurity and Respiratory Outcomes Program, et al. Respiratory consequences of prematurity: evolution of a diagnosis and development of a comprehensive approach. J Perinatol. 2015;35:313–21.
Poindexter BB, Feng R, Schmidt B, Aschner JL, Ballard RA, Hamvas A, Prematurity and Respiratory Outcomes Program, et al. Comparisons and limitations of current definitions of bronchopulmonary dysplasia for the prematurity and respiratory outcomes program. Ann Am Thorac Soc. 2015;12:1822–30.
Walsh MC, Szefler S, Davis J, Allen M, Van Marter L, Abman S, et al. Summary proceedings from the bronchopulmonary dysplasia group. Pediatrics. 2006;117:S52–6.
Walsh MC, Wilson-Costello D, Zadell A, Newman N, Fanaroff A. Safety, reliability, and validity of a physiologic definition of bronchopulmonary dysplasia. J Perinatol. 2003;23:451–6.
OCEBM Levels of Evidence Working Group. The Oxford 2011 Levels of Evidence. Oxford Centre for Evidence-Based Medicine. http://www.cebm.net/index.aspx?o=5653. Accessed March 2016.
OCEBM Levels of Evidence Working Group. The Oxford 2009 Levels of Evidence. Oxford Centre for Evidence-Based Medicine. http://www.cebm.net/oxford-centre-evidence-based-medicine-levels-evidence-march-2009/. Accessed March 2016.
Viswanathan M, Berkman ND, Dryden DM, Hartling L. Assessing risk of bias and confounding in observational studies of interventions or exposures: further development of the RTI item bank. Methods Research Report. AHRQ Publication No. 13-EHC106-EF. Rockville, MD: Agency for Healthcare Research and Quality; August 2013. www.effectivehealthcare.ahrq.gov/reports/final.cfm. Accessed March 2016.
Ricart S, Marcos MA, Sarda M, Anton A, Muñoz-Almagro C, Pumarola T, et al. Clinical risk factors are more relevant than respiratory viruses in predicting bronchiolitis severity. Pediatr Pulmonol. 2012;48:456–63.
Tatochenko V, Uchaikin V, Gorelov A, Gudkov K, Campbell A, Schulz G, et al. Epidemiology of respiratory syncytial virus in children ≤2 years of age hospitalized with lower respiratory tract infections in the Russian Federation: a prospective, multicenter study. Clin Epidemiol. 2010;2:221–7.
Liese JG, Grill E, Fischer B, Roeckl-Wiedmann I, Carr D, Belohradsky BH. Incidence and risk factors of respiratory syncytial virus-related hospitalizations in premature infants in Germany. Eur J Pediatr. 2003;162:230–6.
Joffe S, Escobar GJ, Black SB, Armstrong MA, Lieu TA. Rehospitalization for respiratory syncytial virus among premature infants. Pediatrics. 1999;104:894–9.
Rossi GA, Medici MC, Merolla R, Osservatorio VRS Study Group. Incidence of respiratory syncytial virus positivity in young Italian children referred to the emergency departments for lower respiratory tract infection over two consecutive epidemic seasons. Infection. 2005;33:18–24.
Simon A, Müller A, Khurana K, Engelhart S, Exner M, Schildgen O, DSM RSV Paed Study Group, et al. Nosocomial infection: a risk factor for a complicated course in children with respiratory syncytial virus infection—results from a prospective multicenter German surveillance study. Int J Hyg Environ Health. 2008;211:241–50.
Medici MC, Arcangeletti MC, Rossi GA, Lanari M, Merolla R, Paparatti UD, Osservatorio VRS Study Group, et al. Four year incidence of respiratory syncytial virus infection in infants and young children referred to emergency departments for lower respiratory tract diseases in Italy: the Osservatorio VRS Study (2000–2004). New Microbiol. 2006;29:35–43.
Carbonell-Estrany X, Quero J, Bustos G, Cotero A, Doménech E, Figueras-Aloy J, IRIS Study Group, et al. Rehospitalization because of respiratory syncytial virus infection in premature infants younger than 33 weeks of gestation: a prospective study. Pediatr Infect Dis J. 2000;19:592–7.
Wang EE, Law BJ, Robinson JL, Dobson S, Al Jumaah S, Stephens D, et al. PICNIC (Pediatric Investigators Collaborative Network on Infections in Canada) study of the role of age and respiratory syncytial virus neutralizing antibody on respiratory syncytial virus illness in patients with underlying heart or lung disease. Pediatrics. 1997;99:E9.
Eriksson M, Bennet R, Rotzén-Ostlund M, von Sydow M, Wirgart BZ. Population-based rates of severe respiratory syncytial virus infection in children with and without risk factors, and outcome in a tertiary care setting. Acta Paediatr. 2002;91:593–8.
Berner R, Schwoerer F, Schumacher RF, Meder M, Forster J. Community and nosocomially acquired respiratory syncytial virus infection in a German paediatric hospital from 1988 to 1999. Eur J Pediatr. 2001;160:541–7.
Bonillo Perales A, Díez Delgado Rubio J, Ortega Montes A, Infante Márquez P, Jiménez Liria M, Batlles Garrido J, et al. Perinatal history and hospitalization for bronchiolitis. A comparison with the impact-RSV Study Group. An Esp Pediatr. 2000;53:527–32.
Deshpande SA, Northern V. The clinical and health economic burden of respiratory syncytial virus disease among children under 2 years of age in a defined geographical area. Arch Dis Child. 2003;88:1065–9.
Weigl JA, Puppe W, Schmitt HJ. Incidence of respiratory syncytial virus-positive hospitalizations in Germany. Eur J Clin Microbiol Infect Dis. 2001;20:452–9.
Pezzotti P, Mantovani J, Benincori N, Mucchino E, Di Lallo D. Incidence and risk factors of hospitalization for bronchiolitis in preterm children: a retrospective longitudinal study in Italy. BMC Pediatr. 2009;9:56.
Frogel M, Nerwen C, Cohen A, VanVeldhuisen P, Harrington M, Boron M, Palivizumab Outcomes Registry Group. Prevention of hospitalization due to respiratory syncytial virus: results from the Palivizumab Outcomes Registry. J Perinatol. 2008;28:511–7.
Pérez Pérez G, Navarro Merino M, Romero Pérez MM, Sáenz Reguera C, Pons Tubío A, Polo Padillo J. Respiratory morbidity after hospital discharge in premature infants born at < or =32 weeks gestation with bronchopulmonary dysplasia. An Pediatr (Barc). 2004;60:117–24.
Broughton S, Bhat R, Roberts A, Zuckerman M, Rafferty G, Greenough A. Diminished lung function, RSV infection, and respiratory morbidity in prematurely born infants. Arch Dis Child. 2006;91:26–30.
Jobe AH, Bancalari E. Bronchopulmonary dysplasia. Am J Respir Crit Care Med. 2001;163:1723–9.
The IMpact-RSV Study Group. Palivizumab, a humanized respiratory syncytial virus monoclonal antibody, reduces hospitalization from respiratory syncytial virus infection in high-risk infants. Pediatrics. 1998;102:531–7.
Pedersen O, Herskind AM, Kamper J, Nielsen JP, Kristensen K. Rehospitalization for respiratory syncytial virus infection in infants with extremely low gestational age or birthweight in Denmark. Acta Paediat. 2003;92:240–2.
Greenough A, Cox S, Alexander J, Lenney W, Turnbull F, Burgess S, et al. Health care utilisation of infants with chronic lung disease, related to hospitalisation for RSV infection. Arch Dis Child. 2001;85:463–8.
Thomas M, Bedford-Russell A, Sharland M. Hospitalisation for RSV infection in ex-preterm infants—implications for use of RSV immune globulin. Arch Dis Child. 2000;83:122–7.
Grimaldi M, Gouyon B, Michaut F, Huet F, Gouyon JB, Burgundy Perinatal Network. Severe respiratory syncytial virus bronchiolitis: epidemiologic variations associated with the initiation of palivizumab in severely premature infants with bronchopulmonary dysplasia. Pediatr Infect Dis J. 2004;23:1081–5.
Groothuis JR, Fryzek JP, Makari D, Steffey D, Martone WJ. Respiratory syncytial virus hospitalization trends in infants with chronic lung disease of infancy, 1998–2008. Clin Epidemiol. 2011;3:245–50.
Flamant C, Hallalel F, Nolent P, Chevalier JY, Renolleau S. Severe respiratory syncytial virus bronchiolitis in children: from short mechanical ventilation to extracorporeal membrane oxygenation. Eur J Pediatr. 2005;164:93–8.
Simon A, Ammann RA, Wilkesmann A, Eis-Hübinger AM, Schildgen O, Weimann E, DSM RSV Paed Study Group, et al. Respiratory syncytial virus infection in 406 hospitalized premature infants: results from a prospective German multicentre database. Eur J Pediatr. 2007;166:1273–83.
Grimaldi M, Cornet B, Milou C, Gouyon JB. Prospective regional study of an epidemic of respiratory syncytial virus (RSV) bronchiolitis. Arch Pediatr. 2002;9:572–80.
Zaw W, McDonald J. Respiratory syncytial virus bronchiolitis in ex-preterm infants in the Scottish highlands: review of hospital admissions and an analysis of hospital cost. Scott Med J. 2003;48:108–10.
Duppenthaler A, Gorgievski-Hrisoho M, Aebi C. Regional impact of prophylaxis with the monoclonal antibody palivizumab on hospitalisations for respiratory syncytial virus in infants. Swiss Med Wkly. 2001;131:146–51.
Van de Steen O, Miri F, Gunjaca M, Klepac V, Gross B, Notario G, et al. The burden of severe respiratory syncytial virus disease among children younger than 1 year in Central and Eastern Europe. Infect Dis Ther. 2016 (Epub ahead of print).
Arnold SR, Wang EE, Law BJ, Pediatric Investigators Collaborative Network on Infections in Canada, et al. Variable morbidity of respiratory syncytial virus infection in patients with underlying lung disease: a review of the PICNIC RSV database. Pediatr Infect Dis J. 1999;18:866–9.
Greenough A, Alexander J, Burgess S, et al. Health care utilisation of prematurely born, preschool children related to hospitalisation for RSV infection. Arch Dis Child. 2004;89:673–8.
Gil-Prieto R, Gonzalez-Escalada A, Marín-García P, Gallardo-Pino C, Gil-de-Miguel A. Respiratory syncytial virus bronchiolitis in children up to 5 years of age in Spain: epidemiology and comorbidities: an observational study. Medicine (Baltimore). 2015;94:e831.
Wang EE, Law BJ, Stephens D. Pediatric Investigators Collaborative Network on Infections in Canada (PICNIC) prospective study of risk factors and outcomes in patients hospitalized with respiratory syncytial viral lower respiratory tract infection. J Pediatr. 1995;126:212–9.
Navas L, Wang E, de Carvalho V, Robinson J, Pediatric Investigators Collaborative Network on Infections in Canada. Improved outcome of respiratory syncytial virus infection in a high-risk hospitalized population of Canadian children. J Pediatr. 1992;121:348–54.
Ehrenkranz RA, Walsh MC, Vohr BR, Jobe AH, Wright LL, Fanaroff AA, et al. Validation of the National Institutes of Health consensus definition of bronchopulmonary dysplasia. Pediatrics. 2005;116:1353–60.
McEvoy CT, Jain L, Schmidt B, Abman S, Bancalari E, Aschner JL. Bronchopulmonary dysplasia: NHLBI Workshop on the Primary Prevention of Chronic Lung Diseases. Ann Am Thorac Soc. 2014;11(Suppl 3):S146–53.
Acknowledgements
Sponsorship and article processing charges for this study were funded by AbbVie. Dr. Joanne Smith, Julie Blake (reviewers 1 and 2) and Dr. Barry Rodgers-Gray (reviewer 3), from Strategen Limited, undertook the systematic review following the protocol approved by the authors. AbbVie provided funding to Strategen to undertake the systematic review. All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval to the version to be published. Editorial assistance in the preparation of this manuscript was provided by Julie Blake and Dr. Barry Rodgers-Gray. Julie Blake and Dr. Barry Rodgers-Gray developed a first draft of the manuscript, based on the results of the systematic review and input/approval from all authors, which was initially edited by Xavier Carbonell-Estrany and Bosco Paes and then circulated among the other authors for input, further edits and subsequent approval. Support for this assistance was funded by AbbVie. AbbVie had the opportunity to review and comment on the completed manuscript but final editorial control rested fully with the authors.
Disclosures
The institute of Louis Bont received money for investigator initiated studies by MeMed, AstraZeneca, AbbVie, and Janssen. The institute of Louis Bont received money for consultancy by AstraZeneca, AbbVie, MedImmune, Janssen, Gilead and Novavax. Paul Checchia has acted as an expert advisor and speaker for AbbVie and has received honoraria in this regard. He has also received research grant funding from AstraZeneca. Brigitte Fauroux has received compensation as a neonatology board member from AbbVie. Josep Figueras-Aloy has acted as an expert advisor and speaker for AbbVie and has received honoraria in this regard. Paolo Manzoni has acted as a speaker for AbbVie, and as an expert advisor for AbbVie, TEVA, Medimmune, AstraZeneca, Janssen, and has received honoraria in this regard. Bosco Paes has received research funding from AbbVie Corporation and compensation as an advisor or lecturer from AbbVie and MedImmune. Eric Simões has received grant funding to his institution from Medimmune Inc, Glaxo Smith Kline Inc, and received consultancy fees to the institution, from AbbVie. Xavier Carbonell-Estrany has acted as an expert advisor and speaker for AbbVie and has received honoraria in this regard.
Compliance with Ethics Guidelines
The analysis in this article is based on previously published studies and does not involve any new studies of human or animal subjects performed by any of the authors.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced content
To view enhanced content for this article go to www.medengine.com/Redeem/F6E4F06044E2A44B.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Paes, B., Fauroux, B., Figueras-Aloy, J. et al. Defining the Risk and Associated Morbidity and Mortality of Severe Respiratory Syncytial Virus Infection Among Infants with Chronic Lung Disease. Infect Dis Ther 5, 453–471 (2016). https://doi.org/10.1007/s40121-016-0137-7
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40121-016-0137-7