Abstract
In this paper, the neurological aspects of COVID-19 are presented, which may be of significance for physicians. Knowledge about the neurological symptoms of COVID-19 infection should help physicians in diagnoses and in taking appropriate precautions, as some manifestations can appear before typical pulmonary symptoms. Various mechanisms of SARS-CoV-2 neuroinvasion are discussed and symptoms are described, which can be subdivided into manifestations of the central nervous system (CNS) (headache, dizziness, stroke, impaired consciousness, encephalitis, meningitis, seizures) and peripheral nervous system (PNS) (characteristic hyposmia and hypogeusia, Guillain Barré syndrome, myalgia). Additionally, the implications of COVID-19 infection for treatment of patients with common neurological diseases and their management is presented. It can be concluded that neurological symptoms are part of a clinical spectrum of COVID-19 infection, involving the CNS and PNS. COVID-19 may influence decisions regarding the treatment of neurological disorders, especially those with an immune background.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Neurological symptoms may appear during SARS-CoV-2 infection. They may involve the central and peripheral nervous systems. |
COVID-19 infection may have an impact on the therapy for neurological disorders, especially those with an immune background. |
Therapeutic decisions must always be taken on an individual basis, evaluating the risk/benefit ratio. |
Appropriate precautions must be taken by healthcare providers to minimize transmission risk. |
Digital Features
This article is published with digital features to facilitate understanding of the article. You can access the digital features on the article’s associated Figshare page. To view digital features for this article go to https://doi.org/10.6084/m9.figshare.13201148
Introduction
Coronavirus disease 2019 (COVID-19), caused by coronavirus SARS-CoV-2 (severe acute respiratory syndrome coronavirus 2), emerged for the first time in December 2019 in Wuhan, China, and subsequently spread across the globe [1]. According to the World Health Organization, as of October 11, 2020, over 37,109,000 cases had been diagnosed, with 1,070,355 deaths worldwide. More than 27 million people had recovered from the disease thus far. COVID-19 is largely a respiratory infection, and its symptoms include fever and respiratory symptoms such as coughing, sore throat, and breathing difficulties. Other symptoms can include muscle or joint pain, nausea, diarrhea, vomiting, loss of appetite, and fatigue [2]. Complications of COVID-19 may include pneumonia, heart problems, blood clots, kidney injury, and acute respiratory distress syndrome (ARDS), characterized by rapid onset and respiratory insufficiency, and associated with severe inflammation in the lungs. The typical incubation period for COVID-19 is 5 to 6 days, and ranges anywhere from 1 to 14 days.
The disease course may vary, with some cases asymptomatic or mild (about 80%), while others may be severe and fatal [3]. The mortality rate differs in various regions of the world. Overall, mortality rates are different for men and women, with higher mortality in men, and a marked increase with age [4]. Comorbidities including diabetes mellitus, hypertension, and cardiovascular disease play a significant role in the risk profile and disease prognosis of the patient.
Neurological symptoms can be present in COVID-19 and can appear even before typical pulmonary symptoms. In this paper, data regarding neurological aspects of COVID-19 are presented, taking into account that knowledge of neurological manifestations in infected patients will help physicians in proper diagnosis and in taking appropriate precautions. Another important goal was to determine how the infection could influence treatment in common neurological disorders.
A literature search was conducted using PubMed, Google Scholar, and Ovid MEDLINE for a combination of disease terminology (COVID-19, SARS-CoV-2) and neurological terminology (neuroinvasion, neurological symptoms, stroke, encephalitis, epilepsy, multiple sclerosis, autoimmune neuropathy, headache, therapy, management). The search terms were used as keywords and in combination to maximize the literature findings. The search was conducted in September 2020. This article is based on previously conducted studies and does not contain any new studies with human participants or animals performed by the author.
Mechanisms of SARS-Cov-2 Neuroinvasion and Neurological Damage
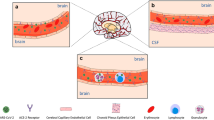
COVID-19 may damage the nervous system through a number of mechanisms. There is a well-known association between SARS-Cov-2 coronavirus and the angiotensin-converting enzyme 2 (ACE2). ACE2 is co-receptor for the virus spike proteins which play an important role in COVID-19 [5] (Fig. 1). After the spike protein binds with the ACE2 receptor in the target cell, the viral envelope fuses with the cell membrane and releases the viral genome into the target cell. ACE2 is expressed in the body in various tissues, including type II alveolar cells in the lungs [6]. It is also expressed in neurons and glial cells in the brain and spinal cord, which can explain brain tissue and spinal cord damage during infection by transsynaptic transfer across infected neurons. ACE2 has been detected in the substantia nigra, ventricles, middle temporal gyrus, posterior cingulate cortex, and olfactory bulb [7]. It is possible that the coronavirus can enter the brain by retrograde transfer from the olfactory epithelium to the brain. Another possibility is that during the viremia phase, the virus can pass through the blood–brain barrier across vascular endothelial cells and enter the brain directly. There is also a mechanism of blood–brain barrier spread through infected immune cells that cross the barrier into the CNS [8]. In addition to the direct viral damage to neurons after crossing the blood–brain barrier or retrograde transport, neuronal damage can occur as a result of pulmonary symptoms and subsequent hypoxic brain injury [9]. There may also be a mechanism of immune-mediated injury due to the cytokine storm, with activation of T lymphocytes, macrophages, and endothelial cells, and increased release of interleukins (IL-1ß, IL-2, IL-6, IL-7), interferons, and chemokines CCL2,CCL3, CXCL10. This causes chronic inflammation and neuronal damage. The development of new-generation immunologically based cytokine storm inhibitors is a promising tool for controlling inflammation during COVID-19 infection [10].
Neurological Symptoms and Complications of COVID-19
Knowledge regarding neurological symptoms in SARS-CoV-2 infection comes from retrospective cohort studies and case reports. These symptoms can be subdivided into features of the central nervous system (CNS) and peripheral nervous system (PNS).
The first retrospective study concerning neurological symptoms comes from China [11]. Of 214 patients with COVID-19, 78 patients (36.4%) had neurological manifestations. The symptoms were significantly more common in severe cases (45.5%) than in non-severe cases (30.2%). Among manifestations of the CNS, the most frequent were dizziness (16.8%) and headache (13.1%). Impaired consciousness was present in 7.5%, acute cerebrovascular disease in 2.8%, ataxia in 0.5%, and seizures in 0.5%. Among manifestations of the PNS, impaired taste was present in 5.6%, impaired smell in 5.1%, impaired vision in 1.4%, and skeletal muscle injury in 10.7% of cases. Neurological features in severe COVID-19 with ARDS were also described in an observational series of 58 patients from France [12]. In this group of patients, agitation was present in 40/58 (69%), corticospinal tract signs in 39/58 (67%), and dysexecutive syndrome in 14/39 (36%). Another retrospective case series was published by Chen et al. [13], which analyzed patients with COVID-19 who died (113) and recovered (161).
Among neurological symptoms, headache was present in 11%, dizziness in 8%, and hypoxic encephalopathy in 9%.
The clinical characteristics of 138 hospitalized patients with COVID-19 were described by Wang et al. [14]. In this group of patients, dizziness was present in 9% and headache in 7%.
A prospective study of neurological disorders in hospitalized COVID-19 patents in New York City was recently published by Frontera et al. [15]. Among 4491 patients with SARS-CoV-2 infection during the study time frame of March 10, 2020 to May 20, 2020, 606 (13.5%) developed neurological symptoms within a median of 2 days from COVID-19 symptom onset.
Toxic/metabolic encephalopathy was diagnosed in 6.0% of patients, seizure in 1.6%, stroke in 1.9%, hypoxic/ischemic injury in 1.4%, movement disorder in 0.9%, and neuropathy in 0.8%. COVID-19 patients with neurological disorders had increased risk of in-hospital mortality and lower rates of discharge home compared to COVID-19 patients without neurological disorders.
Headache
Headache is one of the symptoms of COVID-19, with an estimated frequency of 6–13% [11, 16]. However, it is not an isolated symptom, but often coexists with other symptoms such as fever and cough. In addition, it could be a manifestation of meningitis or encephalitis. Headache may be caused by many factors during SARS-CoV-2 infection, including the release of cytokines (cytokine storm), persistent coughing, anxiety, and lack of sleep.
Impaired Consciousness
Impaired consciousness was reported in 7.5% of patients in a study by Mao et al. [11] in Wuhan, China, with severe conditions in 14.9% of those patients. In another study, altered consciousness in ARDS patients, including agitation and confusion, was found in over 60% of patients with COVID-19 [12]. Different mechanisms responsible for impaired consciousness may explain these differences and may include viral encephalitis, toxic encephalopathy, seizures and post-ictal confusion, and vascular damage. From a practical point of view, it is vital to consider impaired consciousness as a possible manifestation of COVID-19 and take the appropriate precautions.
Encephalitis
The first confirmed case of meningoencephalitis was described by Moriguci et al. [17]. A 24-year-old man from Japan initially complained of headache, fever, and fatigue, and subsequently developed seizures and unconsciousness. He also experienced neck stiffness. His cerebral spinal fluid (CSF) cell count was 12/μL, and was positive for SARS-CoV-2 RNA, supporting neurotropic involvement of SARS-CoV-2. Diffusion-weighted images (DWI) in magnetic resonance imaging (MRI) showed hyperintensity along the wall of the inferior horn of the right lateral ventricle. Fluid-attenuated inversion recovery (FLAIR) showed hyperintense changes in the temporal lobe and hippocampus. Another case of COVID-19 with manifestations of encephalitis was reported in Ditan Hospital in Beijing, China in a 56-year-old patient. He had decreased consciousness, and CSF testing for SARS-CoV-2 was positive. Meningoencephalitis without respiratory failure in a young female patient from Los Angeles was described by Duong et al. [18].
Acute Hemorrhagic Necrotizing Encephalopathy
The case of this rare complication was described by Poyiadji et al. [19] and comes from the USA. A woman in her late-50s had a 3-day history of cough, fever, and altered mental status. A polymerase chain reaction (PCR) assay was positive for COVID-19. A brain MRI demonstrated hemorrhagic rim-enhancing lesions within the bilateral thalami, medial temporal lobes, and subinsular regions. It was noted that the condition could be related to intracranial cytokine storm.
Seizures
Seizures are one neurological symptom that may be experienced during COVID-19 infection. Mao et al. [11] reported a low incidence of seizures (0.5%) in a studied group of patients from Wuhan, China. However, additional studies are needed. Seizures may occur during COVID-19 encephalitis, and can also result from pneumonia and hypoxemia leading to brain damage. It must also be noted that fever during COVID-19 may be a factor triggering the seizures.
Stroke
Among 221 patients diagnosed with COVID-19 in Wuhan, China, in a retrospective study by Li et al. [20], 5% of the patients developed ischemic stroke, 0.5% cerebral venous sinus thrombosis, and 0.5% cerebral hemorrhage. Patients with cerebrovascular disease were older, had more cardiovascular risk factors such as diabetes mellitus or hypertension, and had higher C-reactive protein and D-dimer levels, culminating in accelerated thrombosis. In a study from the Netherlands by Klok et al. [21] in 184 patients hospitalized in the intensive care unit with proven COVID-19, the incidence of thrombotic complications (ischemic stroke, acute pulmonary embolism, deep-vein thrombosis, systemic arterial embolism) was 31%. A study from the USA, in New York, by Yaghi et al. [22] showed that of 3556 patients with a diagnosis of COVID-19, only 0.9% (32 patients) developed stroke. Another study from New York showed that young people (younger than 50 years) could also develop large vessel stroke during COVID-19 infection [23]. It can be concluded that patients with COVID-19 may develop stroke, especially those with multi-organ dysfunction. The risk is associated with hypercoagulopathy that develops during infection. The case of an 81-year-old man with COVID-19 who developed concomitant brain arterial and venous thrombosis has also been described [24].
Hyposmia and Hypogeusia
Hyposmia and hypogeusia have been described as symptoms present in patients with COVID-19, but with frequency ranging from about 5% of cases [11] to about 70% [25] or even over 79% [26]. Alterations in smell or taste were present in 64.4% of 202 patients from Italy positive for SARS-CoV-2 [27]. These alterations appeared prior to other symptoms (11.9%), concomitantly with other symptoms (22.8%), or after other symptoms (26.7%). Considering the relative absence of nasal congestion and rhinorrhea, the hyposmia seems to be associated with olfactory bulb damage. A case report of COVID-19 anosmia with definitive olfactory bulb atrophy compared with pre-COVID imaging was recently published [28]. The exact mechanism of hypogeusia has not yet been clarified. On the whole, these symptoms can be regarded as significant symptoms associated with COVID-19.
Posterior Reversible Encephalopathy Syndrome (PRES)
PRES is a clinical syndrome characterized by headache, altered consciousness, seizure, and visual loss, with white matter vasogenic edema predominantly in the posterior occipital and parietal lobes. Although the exact mechanism has not been fully explained, the syndrome is associated with disturbed cerebrovascular autoregulation, renal failure, and hypertension. Case reports of PRES during COVID-19 have recently been published [29, 30, 31]. In four cases described by Parauda et al. [29], all patients had elevated blood pressure and renal injury in the days preceding PRES, systemic inflammation, and hypercoagulopathy. In a case described by Llansó and Urra [30], the patient received anti IL-1 (anakinra) and anti IL-6 (tocilizumab) medications, as cytokine storm is involved in COVID-19 pathophysiology. In two cases described by Anand et al. [31], one patient received anti IL-1 and the second anti-IL-6 treatment. These drugs should not be used if PRES is diagnosed. Risk factors for PRES in COVID-19 may include underlying infection as well as immunomodulatory medications in conjunction with blood pressure fluctuations.
Other Neurological Symptoms
Among other neurological symptoms observed during COVID-19 and described in the literature, there have been case reports of acute transverse myelitis [32], Guillain Barré syndrome (GBS) [33, 34, 35], Miller Fisher syndrome, and polyneuritis cranialis [36]. Additionally, myalgia [11] and ataxia [11, 37] have been reported.
Neurological Complications in Multisystem Inflammatory Syndrome in Children Related to COVID-19
Neurological symptoms can also appear in the form of multisystem inflammatory syndrome in children (MIS-C) with COVID-19. Fever, abdominal pain, diarrhea, and vomiting are typical clinical presentations in MIS-C [38]. It is a severe illness needing hospitalization with involvement of two or more organ systems: cardiac, renal, respiratory, hematologic, gastrointestinal, dermatologic, or neurological.
Among neurological manifestations in MIS-C associated with COVID-19 were headache, positive meningeal signs (meningism), and altered mental status [39,40,41]. The prevalence of neurological involvement in these children is estimated at about 30%. Treatment with plasma exchange and intravenous immunoglobulin may be beneficial [42].
Neurological manifestations during COVID-19 have also been reviewed in previous papers [43,44,45,46,47]. Differences among published studies in the reported prevalence of neurological disorders in patients with SARS-CoV-2 infection may reflect differences in cohort size, methodology, and populations studied. More information is needed on the pathophysiology, neuropathology, and clinical aspects of neurological disorders developing during COVID-19. Roman et al. [46], on behalf of the Environmental Neurology Specialty Group of the World Federation of Neurology, underlined the importance of developing databanks around the globe to collect cases with neurological manifestations during the ongoing pandemic. With an increased number of patients with COVID-19, we should expect that there will be an increased number of patients with neurological complications.
The neurological symptoms during COVID-19 infection are multiple in number, should not be underestimated, and may come as first symptoms of COVID-19. It is crucial that neurologists are aware of this.
A summary of the main neurological symptoms of SARS-CoV-2 infection is presented in Table 1.
Impact of COVID-19 Infection on Patients with Common Neurological Diseases and Their Management
Patients with Multiple Sclerosis
The current epidemiological situation has an influence on the management and use of disease–modifying therapies in patients with multiple sclerosis (MS). Generally, it is associated with the influence of these therapies on the immune system. However, decisions regarding starting, continuing, or stopping therapy should be individualized, considering the benefit/risk profile [48].
Two important clinical situations and treatment decisions should be discussed: the first when MS patients have an active COVID-19 infection, and the second when they are not infected but taking disease-modifying drugs.
In the first situation, in patients with confirmed COVID-19 infection, the first- or second-line therapy should not be continued until clinical resolution, restarting fingolimod and natalizumab when possible to avoid the rebound effect (a period of increased disease activity following discontinuation of treatment).
For non-infected patients on disease-modifying therapies, treatment decisions, always individualized, must depend on the specific type of therapy. First-line therapies (beta interferons, glatiramer acetate, teriflunomide, dimethyl fumarate) fingolimod or natalizumab should be continued under routine laboratory and neurological examination evaluation.
The situation is more complex when it comes to second-line therapies, which are more powerful. The increased risk is associated with immune reconstitution therapies, which deplete lymphocyte numbers. It was shown that a total lymphocyte count less than 1100/mm3 is associated with an increased risk of infection and infection mortality, increasing in proportion to the decrease in the absolute lymphocyte count [49]. Therefore, during treatment with ocrelizumab, cladribine, mitoxantrone, or alemtuzumab, the decision to continue or delay therapy must be carefully considered according to individual factors. The second course of alemtuzumab may be safely delayed for 18 months, without risk of return disease activity.
Moreover, hematopoietic stem cell transplantation should only be performed when and where the risk of SARS-CoV-2 infection is low and only for patients with high disease activity, when other therapies were not effective [50].
Patients with Neuromyelitis Optica Spectrum Disorders (NMOSD)
Currently there is no evidence that patients with NMOSD have increased risk of COVID-19 infection. These patients are treated using medications affecting the immune system, including azathioprine, rituximab (anti-CD20), eculizumab (anti-complement protein C5), and tocilizumab (an IL-6 inhibitor). These drugs can be used on an individual basis, evaluating the risk/benefit ratio. At present no recommendations exist to stop treatment used in NMOSD [51].
Patients with Immune-Mediated Neuropathies
Recommendations for this group of patients have been developed by the Italian Association for the Study of the Peripheral Nervous System (ASNP), the Italian Society for Clinical Neurophysiology, and the Italian Society of Neurology (SIN) [52]. According to these recommendations, several points should be underlined.
-
Although there are reports of GBS and Miller Fisher syndrome during COVID-19, there is no evidence of an association between SARS-COV-2 infection and the development of immune-mediated neuropathies. Immunosuppressive medications may increase susceptibility to infection.
-
It is recommended not to start any treatment with immunosuppressive or immunomodulatory medications which can suppress or delay the immune system response.
-
For patients already on treatment, the decision should be individualized considering the severity of neuropathy, particular medications, or hospital risk of infection.
-
Patients under treatment with first-line (i.e., steroids) and second/third-line medications (i.e., azathioprine, methotrexate, cyclosporine, mycophenolate mofetil, and oral cyclophosphamide) should continue treatment and take personal precautions. For infusion therapy with rituximab or cyclophosphamide, the risk/benefit ratio of postponing therapy should be considered. Intravenous or subcutaneous immunoglobulin administration and plasmapheresis does not increase the risk of SARS-CoV-2 infection.
-
In patients positive for SARS-CoV-2, it is recommended not to start any immunosuppressive therapy, to postpone therapy with rituximab and cyclophosphamide, and progressively reduce steroid therapy until suspension.
Patients with Myasthenia Gravis (MG) and Lambert–Eaton Syndrome (LEMS)
According to the guidelines of the International MG/COVID-19 Working Group [53], therapy decisions should be individualized. MG/LEMS patients should continue their current treatment and not stop using medications unless discussed with and decided by the healthcare provider. There is no scientific evidence that symptomatic therapies like pyridostigmine or 3,4-diaminopyridine increase the risk of infection. Currently there is no evidence that intravenous immunoglobulins (IVIG) or plasma exchange may be associated with risk of COVID-19 infection, but these treatments should be based on individual cases and should be reserved for patients with acute exacerbation. Precautions should always be taken in this group of patients. There is no evidence that eculizumab, a monoclonal antibody used in the disease treatment, increases susceptibility to COVID-19. In a situation of COVID-19 infection, temporarily pausing current immunosuppressive therapy should be considered, and change decisions need to be individualized based on the severity of COVID-19 and discussed with the patient.
Patients with Epilepsy
Epilepsy is not a risk factor for COVID-19. It must be remembered, however, that during infection, fever may be a trigger for seizures [54]. Another important issue is that potential drugs currently being investigated for COVID-19 should also be examined for potential interactions with antiepileptic drugs. Current therapies which affect the immune system, such as steroids for autoimmune epilepsy, must be considered in relation to SARS-CoV-2 infection. Viral infections may increase the risk of SUDEP (sudden unexpected death in epilepsy), although there is no evidence for such association with COVID-19 infection.
Patients with Stroke
Management of acute ischemic stroke in patients with COVID-19 infection has been broadly presented in the form of a report from an international panel, with practical implications suggested [55]. There was consensus that patients with COVID-19 carry the risk of developing stroke, with over 80% being ischemic stroke. Healthcare providers are at risk of acquiring COVID-19 from COVID-19 patients including those with stroke. It was clearly suggested that a patient with stroke and clinically suspected COVID-19 has to be evaluated under the assumption that the patient has COVID-19 infection. If a stroke patient is suspected of having COVID-19, chest tomography may be helpful in identifying radiological abnormalities suggestive of COVID-19 infection. The stroke team should use precautions to minimize the transmission risk during evaluation of acute stroke patients, including maintaining a distance of 2 m from the patient (except when absolutely necessary) and combining the use of surgical mask, gloves, gowns, and handwashing. The stroke team evaluating the patient should comprise the minimum number of healthcare providers. If Telestroke is available, it should be used and maximized in the current situation. Physicians should be aware of complications, as COVID-19 and stroke are both associated with a risk of renal insufficiency, considering computed tomography (CT) angiography for thrombectomy. Contrast exposure required for CT angiography and perfusion images may precipitate acute kidney injury and increase the risk of mortality. A detailed assessment of coagulation parameters to evaluate the risk/benefit ratio is necessary prior to intravenous recombinant tissue plasminogen activator (rt-PA) administration.
Patients with Parkinson’s Disease
Parkinson’s disease is not a risk factor for COVID-19 [56], and it is not associated with an unfavorable outcome resulting from COVID-19 infection.
However, it is important to remember that psychological stress associated with the COVID-19 pandemic can worsen motor symptoms of the disease, and lack of exercise due to imposed restrictions may also lead to a worsening of motor symptoms in Parkinson's disease [57].
Neurologists should be aware that treating various neurological disorders with steroids or immunosuppressants may increase the risk of infection. Thus, these patients must be carefully monitored.
Conclusion
Neurological symptoms may appear during SARS-CoV-2 infection and are part of the clinical spectrum of COVID-19. They may result from different mechanisms of direct viral infection including viral damage to neurons after crossing the blood–brain barrier or retrograde transport, immune-mediated injury due to cytokine storm, or in relation to hypoxic brain injury or vessel thrombosis. The neurological symptoms can be divided into CNS and PNS manifestations and include encephalitis, meningitis, impaired consciousness, stroke, headache, hyposmia and hypogeusia, neuropathies, and muscle pain. Neurological symptoms may appear early during the course of the illness, even before typical pulmonary symptoms. COVID-19 influences the treatment of neurological disorders, especially those with an immune background. Steroids and immunosuppressive drugs may increase the risk of infection. Therapeutic decisions must always be taken on an individual basis, evaluating the risk/benefit ratio.
References
Zhu N, Zhang D, Wang W, et al. A novel coronavirus from patients with pneumonia in China. N Engl J Med. 2020;382:727–33.
Mingxuan X, Qiong C. Insight into 2019 novel coronavirus-an updated interim review and lessons from SARS-Cov and MERS-Cov. Int J Infect Dis. 2020;94:119–24.
Wu Z, McGoogan JM. Characteristics of and important lessons from the coronavirus disease 2019 (COVID 19) outbreak in China: summary of a report of 72 314 cases from the Chinese Center for Disease Control and Prevention. JAMA. 2020. https://doi.org/10.1001/jama.2020.2648.
Liu K, Chen Y, Lin R, Han K. Clinical features of COVID-19 in elderly patients: a comparison with young and middle-aged patients. J Infect. 2020. https://doi.org/10.1016/j.inf.2020.03.0.
Zhou P, Yang XL, Shi ZL. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. 2020;579:270–3.
Patel AB, Vermas A. COVID-19 and angiotensin-converting enzyme inhibitors and angiotensin receptor blockers. What is the evidence? JAMA. 2020;323:1769–70.
Chen R, Wang K, Yu J, Zhong C, Wen C, Xu Z. The spatial and cell-type distribution of SARS-CoV-2 receptor ACE2 in human and mouse brain. BioRxiv. 2020. https://doi.org/10.1101/2020.04.07.030650.
Zubair AS, Mc Alpine LS, Gardin T, Farhadian S, Kuruvlla DE, Spudich S. Neuropathogenesis and neurologic manifestations of the coronaviruses in the age of Coronavirus Disease 2019. JAMA Neurol. 2020. https://doi.org/10.1001/jamaneurol.2020.2065.
Tu H, Tu S, Gao S, Shao A, Sheng J. The epidemiological and clinical features of COVID-19 and lessons from this global infectious public health event. J Infect. 2020. https://doi.org/10.1016//j.inf.2020.04.011.
Vandenbark A, Meza-Romero R, Offner H. Surviving the storm. Dealing with COVID-19. Cell Immunol. 2020. https://doi.org/10.1016/j.cellimm.2020.104153.
Mao L, Wang M, Hu Y, et al. Neurologic manifestations of hospitalized patients with coronavirus disease 2019 in Wuhan, China. JAMA Neurol. 2020. https://doi.org/10.1001/jamaneurol.2020.1127.
Helms J, Kremer S, Merdji H, et al. Neurologic features ion severe SARS-CoV-2 infection. N Engl J Med. 2020. https://doi.org/10.1056/NEJMc2008597.
Chen T, Wu D, Chen H, et al. Clinical characteristics of 113 deceased patients with coronavirus disease 2019: retrospective study retrospective study. BMJ. 2020. https://doi.org/10.1136/bmj.m1091.
Wang D, Hu B, Hu C, et al. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA. 2020;323(11):1061–9.
Frontera JA, Sabadia S, La Ichan R, et al. A prospective study of neurological disorders in hospitalized COVID-19 patients in New York city. Neurology. 2020. https://doi.org/10.12112/WNL.0000000000010979.
Lahiri D, Ardila A. COVID-19 pandemic: a neurological perspective. Cureus. 2020. https://doi.org/10.7759/cureus.7889.
Moriguchi T, Harii N, Goto J, et al. A first case of meningitis/encephalitis associate with SARS-Coronavirus-2. Int J Infect Dis. 2020;94:55–8.
Duong L, Xu P, Liu A. Meningoencephalitis without respiratory failure in a young female patient with COVID-19 infection in Downtown Los Angeles, early April 2020. Brain Behav Immun. 2020. https://doi.org/10.1016/j.bbi.2020.04.024.
Poyiadji N, Shahin G, Noujaim D, Stone M, Patel S, Griffith B. COVID-19-associated acute hemorrhagic encephalopathy: CT and MRI features. Radiology. 2020. https://doi.org/10.1148/radiol.2020201187.
Li Y, Wang M, Zhou Y et al. Cerebrovascular disease following COVID-19: a single center, retrospective observational study SVN. 2020.
Klok FA, Kruip MJ, van der Meer NJ, et al. Incidence of thrombotic complications in critically ill ICU patients with COVID-19. Thromb Res. 2020;191:145–7.
Yaghi S, Ishida K, Torres J, et al. Stroke in a New York healthcare system. Stroke. 2020. https://doi.org/10.1161/STROKEAHA.1200.
Oxley T, Mocco J, Majidi S, et al. Large-vessel stroke as a presenting feature of COVID-19 in young. N Engl J Med. 2020. https://doi.org/10.1056/NEJM:c2009787.
Malentacchi M, Gned D, Angelino V, et al. Concomitant brain arterial and venous thrombosis in a COVID-19 patient. Eur J Neurol. 2020. https://doi.org/10.1111/ene.14380.
Yan CH, Faraji F, Prajapati DP, Boone CE, DeCoonde AS. Association of chemosensory dysfunction and COVID-19 in patients presenting with influenza-like symptoms. Int Forum Allergy Rhinol. 2020. https://doi.org/10.1002/air.22579.
Lechien JR, Chiesa-Estomba CM, De Siati DR. Olfactory and gustatory dysfunctions as a clinical presentation of mild-to-moderate forms of the coronavirus disease (COVID-19): a multicenter European study. Eur Arch Otorhinolaryngol. 2020. https://doi.org/10.1007/s00405-020-05965-1.
Spinato G, Fabbris C, Polesel J, et al. Alterations in smell and taste in mildly symptomaqtic outpatients with SARS-CoV-2 infection. JAMA. 2020;323:2089–90.
Chiu A, Fischbein N, Wintermatk M, et al. COVID-19-induced anosmia associated with olfactory bulb atrophy. Neuroradiology. 2020. https://doi.org/10.1007/s00234-020-02554-1.
Parauda SC, Gao V, Gewirtz AN, et al. Posterior reversible encephalopathy syndrome in patients with COVID-19. J Neurol Sci. 2020. https://doi.org/10.1016/j.jns.2020.117019.
Liansó L, Urra X. Posterior reversible encephalopathy syndrome in COVID-19 disease: a case report. SN Compr Clin Med. 2020. https://doi.org/10.1007/s42399-020-00470-2.
Anand P, Vincent Lau KH, Chung DY, et al. Posterior reversible encephalopathy syndrome in patients with coronavirus disease 2019: two cases and a review of the literature. J Stroke Cerebrovasc Dis. 2019;2020:1.
Zhao K, Huang J, Dai D, Feng Y, Liu L, Nie S. Acute myelitis after SARS-CoV-2 infection: a case report. 2020. https://www.medrxv.org/content/10.1101/2020.0316.20035105v2
Sedaghat Z, Karimi N. Guillain Barré syndrome associated with COVID-19 infection: a case report. J Clin Neurosci. 2020;76:223–35.
Toscano G, Palmerini F, Ravavaglia S, et al. Guillain-Barré syndrome associated with SARS-CoV-2. N Engl J Med. 2020. https://doi.org/10.1056/NEJMc2009191.
Virani A, Rabold E, Hanson T, et al. Guillain-Barré Syndrome associated with SARS-CoV-2 infection. ID Cases. 2020. https://doi.org/10.1016/j.idcr.2020e00771.
Gutiérrez-Ortiz C, Méndez A, Rodrigo-Ray S, et al. Miller Fisher syndrome and polyneuritis cranialis in COVID-19. Neurology. 2020. https://doi.org/10.1212/WNL0000000000009619.
Balestrino R, Rizzone H, Zibetti M, et al. Onset of COVID-19 with impaired consciousness and ataxia: a case report. J Neurol. 2020. https://doi.org/10.1007/s00415-020-09879-0.
Ahmed M, Advani S, Moreira A, et al. Multisystem inflammatory syndrome in children: a systematic review. EClinicalMedicine. 2020. https://doi.org/10.1016/j.eclinm.2020.100527.
Pouletty M, Borocco C, Ouldali A, et al. Pediatric multisystem inflammatory syndrome temporally associated with SARS-CoV-2 mimicking Kawasaki disease (Kawa-COVID-19): a multicenter cohort. Ann Rheum Dis. 2020. https://doi.org/10.1136/annrheumdis-2020-217960.
Toublana J, Poirault C, Corsta A, et al. Kawasaki-like multisystem inflammatory syndrome in children during the covid-19 pandemic in Paris, France: prospective observational study. BMJ. 2020;2020:m2094.
Chiotos K, Bassiri H, Behrens EM, et al. Multisystem inflammatory syndrome in children during the COVID-19 pandemic: a case series. J Pediatric Infect Dis Soc. 2020. https://doi.org/10.1093/jpids/piaa069.
Chen TH. Neurological involvement associated with COVID-19 infection in children. J Neurol Sci. 2020. https://doi.org/10.1016/j.jns.2020.117096.
Ahmad I, Rathore FA. Neurological manifestations and complications of COVID 19: a literature review. J Clin Neurosci. 2020;77:13–6. https://doi.org/10.1016/j.jocn.2020.05.017.
Montalvan V, Lee J, Bueso T, et al. Neurological manifestations of COVID 19 and other coronavirus infections. Clin Neurol Neurosurg. 2020. https://doi.org/10.1016/j.clineuro.2020.105921.
Ellul MA, Benjamin L, Singh B, et al. Neurological associations of COVID-19. Lancet Neurol. 2020;19(9):767–703. https://doi.org/10.1016/S1474-4422920)30221-0.
Roman GC, Spencer PS, Reis J, et al. The neurology of COVID-19 revisited: a proposal from the Environmental Neurology Specialty Group of the World Federation of Neurology to implement international neurological registries. J Neurol Sci. 2020. https://doi.org/10.1016/j,jns.2020.116004.
Asadi-Pooya AA, Simani L. Central nervous system manifestations of COVID-19: a systematic review. J Neurol Sci. 2020. https://doi.org/10.1016/j.jns.2020.116032.
Giovannoni G, Hawkes CH, Lechner-Scott J, Levy M, Waubant E, Gold J. The COVID-19. Pandemic and the use of MS disease-modifying therapies. MSARD. 2020. https://doi.org/10.1016/j.msard.2020.102073.
Warny M, Helby J, Nordestgaard BG, Birgens H, Bojesen SE. Lymphopenia and risk of infection and infection-related death in 98 344 individuals from prospective Danish population-based study. PLoS Med. 2018;15(11):e1002685.
Samaha R, Kattan J. Hematopoietic stem cell transplantation dilemma during the COVID-19 era. Future Oncol. 2020. https://doi.org/10.2217/fon-2020-0414.
Contentti EC, Correa J. Immunosuppression during the COVID-19 pandemic in neuromyelitis optica spectrum disorders patients: a new challenge. MSARD. 2020. https://doi.org/10.1016/j.msard.2020.102097.
Dubbioso R, Nobile-Orazio E, Manganelli F, et al. Dealing with immune-mediated neuropathies during COVID-19 outbreak: practical recommendations from the task force of the Italian Society of Neurology (SIN), the Italian Society of Clinical Neurophysiology (SINC) and the Italian Peripheral System Association (ASNP). Neurol Sci. 2020;41:1345–8.
International MG/COVID-19 Working Group. Guidance for the management of myasthenia gravis (MG) and Lambert-Eaton myasthenic syndrome (LEMS) during the COVID-19 pandemic. J Neurol Sci. 2020. https://doi.org/10.1016/j.jns2020.1.116803
Kuroda N. Epilepsy and COVID-19 associations and important considerations. Epilepsy Behav. 2020. https://doi.org/10.1016/j.yebeh.2020.107122.
Qureshi AI, Abd-Allah F, Al-Senani F, et al. Management of acute ischemic stroke in patients with COVID-19 infection: insights from an international panel. Am J Emerg Med. 2020. https://doi.org/10.1016/j.ajem.2020.05.018.
Papa SM, Brundin P, Fung VS, et al. Impact of the COVID-19 pandemic on Parkinson’s disease and movement disorders. Mov Disord. 2020;35:711–5.
Helmich RC, Bloem BR. The impact of the COVID-19 pandemic on Parkinson’s Disease: hidden sorrows and emerging opportunities. J Parkinson’s Dis. 2020;10:351–4.
Acknowledgements
I would like to thank Marlena Wójcicka and Elżbieta Kaufman from the Department of Neurology for technical support during the process of preparing the manuscript.
Funding
No funding or sponsorship was received for this study or publication of this article. The Rapid Service Fee was funded by the author.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Disclosures
Jacek Losy has nothing to disclose.
Compliance with Ethics Guidelines
This article is based on previously conducted studies and does not contain any new studies with human participants or animals performed by the author.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Losy, J. SARS-CoV-2 Infection: Symptoms of the Nervous System and Implications for Therapy in Neurological Disorders. Neurol Ther 10, 31–42 (2021). https://doi.org/10.1007/s40120-020-00225-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40120-020-00225-0