Abstract
Introduction
This study was designed to gain insight into the treatment experiences and expectations of patients with atrial fibrillation (AF) who were treated with vitamin K antagonists (VKA) or recently switched from VKA treatment to direct oral anticoagulant (DOAC) therapy. Little is known about the perceptions and expectations of patients with AF who are being prescribed oral anticoagulants (OACs), leading to different expectations of patient and doctor of their respective roles in disease management between the doctor [general practitioner (GP) or cardiologist] and patient on their respective roles in disease management.
Methods
A market research study was conducted consisting of two phases: (1) qualitative research (n = 16) in which in-depth interviews were conducted; and (2) quantitative research (n = 101), using a conjoint analysis.
Results
Patients reported that the three most important aspects of OAC treatment were (in order of priority) reduced risk of blood clots/stroke, low bleeding risk, and not having to use a thrombosis service. Only 12% of VKA-treated patients were familiar with DOAC, although 52% were open to switching when presented with a DOAC profile.
Conclusions
GPs and patients are waiting for the other to mention issues surrounding AF treatment such as switching, use of thrombosis service, and number of pills to take first. The perceptions and experiences of patients with AF regarding their disease and treatment highly influence the decisions GPs make, together with these patients, as well as considerations that patients have regarding their treatment; GPs need to be aware of their AF patients’ perceptions and experiences with their condition and medication’ in order to facilitate discussions with patients and improve clinical outcomes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Why carry out this study? |
The study was designed to gain insight into the treatment experiences and expectations of patients with atrial fibrillation (AF) who were treated with vitamin K antagonists (VKA) or recently switched from VKA treatment to direct oral anticoagulant (DOAC) therapy. |
What was learned from the study? |
GPs and patients are waiting for the other to mention issues surrounding AF treatment. |
The perceptions and experiences of patients with AF regarding their disease and treatment highly influence decisions GPs make with these patients. |
GPs need to be aware of their AF patients’ perceptions and experiences with their condition and medication in order to facilitate discussions with patients and improve clinical outcomes. |
Introduction
The 2017 Dutch College of General Practitioners (NHG) guidelines for atrial fibrillation (AF) state that vitamin K antagonists (VKA) and direct oral anticoagulants (DOAC) are equivalent alternatives. Following this AF guideline, Dutch general practitioners (GPs) can prescribe DOAC. As a result, one may have expected that the number of prescriptions for DOAC by GPs would increase substantially [1, 2]. However in 2019, the majority of Dutch patients who could benefit from OAC are still on ‘older’ agents such as VKAs. In July 2016, DOAC use in the Netherlands was 19.8% compared to 48.4% in Europe [3]. Almost 3 years later, in June 2019, DOAC use in the Netherlands stood at 48.3% versus 70.1% in the rest of Europe [3]. This clearly puts the Netherlands behind other European countries with regard to the implementation of this new treatment option, despite strong clinical evidence and assurance from both national and international guidelines [3,4,5,6,7,8,9,10]. Interestingly, the Dutch guidelines recommend that the GP should discuss treatment options with patients, which requires a certain amount of knowledge and correct information by both parties on these options, as well as the patient realizing that he or she is expected to be actively be involved in this discussion [2]. To evaluate the experiences and needs of patients with AF in relation to DOAC treatment and to gain insight into their current knowledge of DOAC treatment, a market research study of Dutch AF patients was conducted by SKIM Europe. This study surveyed the treatment experiences and expectations of patients with AF who were receiving VKA therapy or who had recently switched from VKA to DOAC therapy. The insights gained from this study may help GPs to better understand the patient’s perspective and needs regarding OAC treatment and therefore aid in shared decision making (SDM). Ultimately, this may lead to improvements in patient OAC care and clinical outcomes for patients with AF.
GPs have little knowledge about how patients with atrial fibrillation (AF) perceive their oral anticoagulant (OAC) therapy with either vitamin K antagonists (VKAs) or direct oral anticoagulation (DOAC). The same is true for the beliefs and worries that these patients may have about their OAC therapy. This lack of knowledge extends to the issue of switching, in the sense that GPs expect patients to request when they want to switch from one OAC agent to another. However, as many patients are not aware of the availability of different types of OAC, it is unlikely that they will discuss (let alone request) the possibility of switching from one OAC to another with their GP. In other words: there seems to be little to no conversation around AF treatment and patients are unaware of other treatment options. This leads to complacency in their current treatment. As such, both the GP and the patient have different expectations of their unique role in OAC treatment.
Methods
The study consisted of two phases: phase 1 of the study involved qualitative research, and phase 2 quantitatively validated the finding of phase 1. Participation was voluntary and individuals could opt out of the survey at any time.
Phase 1
Phase 1 of the study aimed to establish what patients with AF consider to be important regarding the medicinal and non-medicinal aspects of their OAC treatment, and what aspects they consider to be less important or unimportant. It was also important to understand the general patient pathway, involvement of the different HCPs, and knowledge levels on their disease in general and medication options in particular. A semi-structured interview technique was used, and respondents were interviewed individually. The interview consisted of closed- and open-ended questions, which were often accompanied by follow-up why or how questions [11]. The main questions in phase 1 of the study were: (1) how do patients experience their disease and their VKA treatment; (2) what were the patient’s expectations of this treatment so far, were they met and what are their expectations for the future; (3) how do they perceive the information (or lack thereof) presented to them about and throughout the treatment; (4) how do they perceive the interaction with their healthcare professionals (HCPs) and the thrombosis service; and (5) what level of knowledge do they have regarding the newer DOAC treatments and how did they learn about these treatments, and what are their expectations of these treatments? The questionnaire exercises (consisting of the ‘heart and mind’ exercise as well as the patient-journey model and product profiles) are regularly used by the international market research group SKIM Europe, which conducted the research. The results are subject to validation by applying four principles of qualitative validity: credibility, transferability, dependability, and confirmability.
Phase 2
The aim of phase 2 of the study was to validate the qualitative research done in phase 1. Phase 2 was designed as a conjoint analysis, a statistical technique used to help determine how a limited number of individuals value different attributes and, more specifically, to determine what combination of a limited number of attributes is most influential on an individual’s choice or decision-making. Phase 2 was conducted using an online questionnaire. The main questions of the questionnaire were: (1) how do patients perceive their VKA treatment; (2) what aspects do they like about their current treatment; (3) what barriers do patients have regarding their current treatment; (4) are the expectations of their VKA treatment met; (5) what aspects of their VKA treatment would make them switch to other treatments; (6) are they familiar with the new DOAC treatments; and (7) how do they perceive the newer DOAC treatments?
To interpret the results correctly, participating AF patients were divided into two groups; those who were currently on VKA treatment and those who were previously treated with a VKA but currently with a DOAC. All participating AF patients were asked to evaluate the different OAC product attributes through both implicit and explicit methods. To understand which product attributes truly impacted treatment choice, participants were asked four times to choose between two product profiles, which consisted of a mix of both DOAC and VKA attributes. In order to prevent bias, this was done in such a way that it was not traceable to any specific product(s). For that same reason, the sponsor of the research was not mentioned.Footnote 1 Subsequently, to tease out which attributes were most salient to patients, individuals were specifically asked to rank the different attributes on a scale from 1 to 8, with 1 being the most important attribute and 8 the least important attribute; rankings were stratified by patient group (VKA or DOAC). Based on their choices across these exercises, researchers were able to determine which attribute is the deciding factor for individual patients.
Compliance with Ethics Guidelines
This was a non-interventional market research study and questionnaires were completed anonymously in accordance with the regulations and practice of market research governing bodies: European Society for Opinion and Marketing Research (ESOMAR) and European Pharmaceu615 tical Market Research Association (EphMRA) and thus is exempt from requiring Clinical Research Ethics Committee or Independent Review Board approval. SKIM received informed consent from the patients included.
Results
A total of 16 individuals (eight male, eight female) were selected (nationwide) to participate in phase 1 of the study. Of these, 56% patients (n = 9) were aged 60–70 years and 44% of patients (n = 7) were aged 70–80 years. Regarding their OAC medication, 31% of patients (n = 5) had been switched by their HCP from VKA to DOAC therapy, 25% (n = 4) had been initiated on DOAC therapy by their HCP and 44% patients (n = 7) were treated with VKAs. All individuals took part in an in-depth interview.
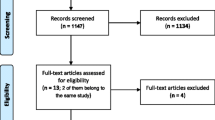
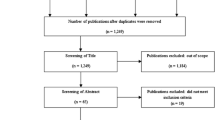
A total of 19,959 individuals aged ≥ 50 years were recruited from the general population to take part in the survey in phase 2 of the study, of which 10,826 started the online survey. The total number of patients with AF within this population was 453 (8%), of which 54 patients did not complete the survey and 43 were excluded due to comorbidities. A further 163 of 453 patients were not currently using a VKA or DOAC, three indicated that they used both a VKA and a DOAC and 76 were excluded as they had never used a DOAC before. Finally, two patients were excluded, as they fell outside of the set quota, one patient was using a VKA but was not using the thrombosis service (which was therefore considered an ‘Untrustworthy’ respondent as VKA usage is not possible without thrombosis service) and ten patients were removed from the cohort due to data cleaning. This resulted in 101 evaluable individuals; 68 patients (67%) were on VKA therapy and 33 (33%) were receiving DOACs. The patient characteristics of these 101 individuals are described in Fig. 1.
How Do Patients Rate Their Treatment?
Patients using acenocoumarol gave their treatment a mean score of 8.3 on a scale of 0–10, and those receiving fenprocoumon gave a mean treatment score of 7.9. The mean treatment score for the four DOACs ranged from 8.2 to 8.7. Patients who had switched from acenocoumarol to a DOAC (n = 16) gave a mean rating for their previous VKA therapy of 6.6, thus rating their previous VKA medication much lower than their current DOAC therapy.
What Barriers Do Patients Have Regarding Their Current Treatment?
For 17% of the 101 patients with AF, switching dosages is a barrier to adherence. Although the question ‘What is a barrier to adherence for you’ (or a similar question) was not asked explicitly, there was an open-ended question that led some respondents to respond along the lines of ‘Differing dosing makes it hard to be compliant.’ Responses on this were given in the ranking exercise, when respondents indicated that ‘having the same dosing every day’ was among the top 3 things most important to them. They were then asked why this was the case. Responses included comments such as: ‘It is harder to get the pills wrong, I think’ and ‘Easier to remember.’
Ranking the Different Aspects of OAC treatment – Implicit Importance
Patients were repeatedly (four times) prompted to choose between two product profiles, each consisting of a mix of both DOAC and VKA attributes, to establish the deciding factor for patients. DOAC attributes where generally preferred over VKA attributes, especially dosing schedule, lower chance of cerebral hemorrhage and no restrictions to diet were preferred.
Ranking the Different Aspects of OAC Treatment: Explicit Importance
In the ranking exercise, all 101 patients with AF (who were treated with either a VKA or a DOAC) evaluated the different VKA and DOAC product attributes specifically, ranking them from most important to least important. This resulted in the top three product attributes per patient group (Table 1). Although the attributes which feature in the top three are similar between the two groups, DOAC patients rated the two aspects ‘No INR check needed’ and ‘Once daily dosage (pill)’ as equally important, for both, 24% of DOAC patients put them in third place. Although 70% of all patients did not list experiencing a stroke, they still communicated that effective prevention of stroke was very important to them, while 7% of patients were especially concerned with higher treatment efficacy due to a previous history of stroke. Overall, 34% of VKA patients ranked ‘no thrombosis service checks’ in their top three attributes. When asked why they would like to not have the thrombosis service, 48% of these patients believed this would make it easier to fit their disease into daily life, and another 48% found the INR checks to be annoying or time-consuming. The perception of the thrombosis service differed greatly between VKA- and DOAC-treated patients, with 56% of patients on VKAs perceiving it as ‘Fine’ (vs. 23% of patients on DOAC). In contrast, 52% of DOAC recipients considered the thrombosis service to be ‘Time-consuming/difficult to fit into daily life’ (vs. 19% of VKA recipients) and 30% of DOAC recipients even considered it as ‘Horrible’ (vs. 9% of VKA recipients). Detailed perceptions on the thrombosis service by patients on VKA and DOAC are shown in Fig. 1.
Are VKA Patients Familiar with the Newer DOAC Treatments?
Of the patients on VKAs taking part in the survey, 63% said they were not at all familiar with the newer DOACs; 25% were hardly/not very familiar and 12% were fairly/very familiar with DOAC therapy. Educational level, age, or cardiologist involvement did not impact patient awareness level. VKA recipients rated the information their HCP gave them with mean score of 7.2 out of 10 (range, 2–10). Whether a cardiologist or GP presented them with their confirmed AF diagnosis had no impact on the score given by patients on VKA for the level of information they received (7.4 out of 10 for both cardiologist and GP). DOAC recipients rated the information from their HCP with a mean score of 7.9 out of 10 (range, 6–10). Both VKA and DOAC recipients indicated that they expected HCPs to outline all treatment options at the start of treatment and discuss any new possible medications if they become available (Fig. 2).
How Do VKA Patients Perceive the Newer DOAC Treatments?
Patients on VKA were shown a profile of DOAC therapy to assess their perception about this type of OAC, consisting of the most important and characteristic features of DOAC, and naming all available DOAC agents without emphasizing any particular one of them (Table 2). When presented with the DOAC description, 49% of patients on VKAs had a (very/mostly) positive response. When prompted for the reasons for their (very/mostly) positive response, 64% indicated that losing the thrombosis service contributed to their evaluation, 18% said it was because of the set daily dosage, and 15% stated that higher efficacy was the reason for their positive response. A total of 38% of patients on VKAs responded neutrally to the DOAC description. Of these, 73% of patients did so because they were unfamiliar with DOAC or felt that they lacked medication knowledge; 27% responded neutrally because they were content with their current VKA regimen. Finally, 13% of patients on VKAs had a (mostly/very) negatively response to the DOAC profile. This subgroup was relatively small (n = 9) and their reasons for responding (mostly/very) negatively varied, with a fear of mismatch with comorbidities (e.g., kidney or liver disorders) being mentioned by 33% of patients (n = 3).
Willingness to Switch
When presented with the DOAC profile (Table 2), 52% of patients on VKA said they would choose to switch to a DOAC. However, 43% of patients on VKA indicated that when they were asked whether or not they would switch to a DOAC they would always choose to stay on their current medication. Of these non-switchers, 66% indicated that they did not want to switch because they were content with their current medication, and 21% stated that they were afraid to switch medication, with concerns including adverse effects that they might experience with new products, or feeling safe due to their thrombosis service check-ups. Of note, patients who were open to switching to a DOAC at the same time also stated that were afraid of doing so (Fig. 3).
Discussion
The findings of this study provide interesting and in-depth insight into the perceptions and beliefs of patients with AF who are treated with OACs. Of particular interest, results show that 85% of patients on VKA were unaware of DOAC therapy, with only 12% being (fairly/very) familiar with this class of OAC; however, 52% of current VKA-treated patients were willing to switch to a DOAC. At the same time, VKA-treated patients (as well as DOAC-treated patients) felt that their HCP should outline all OAC options at the start of treatment and discuss any new possible medications as they become available. This reveals a discrepancy between what is expected from HCPs and what is actually done in daily clinical practice. GPs and cardiologists, as the main prescribers of OAC, should be aware that patients expect them to provide information on OAC options, and that they expect to be updated when new treatment options become available. Nevertheless, even if patients with AF are willing to switch to DOAC therapy, there are barriers to switching. For both these patients and those who are less open to a switching, GPs need to understand the concerns patients might have, and proactively manage any concerns.
The top three most important attributes for all AF patients regarding OAC therapy demonstrated that the main concern of patients was the occurrence of blood clots or suffering a stroke (efficacy aspect), even though 70% had not previously experienced a stroke. AF patients were highly aware of the reasons why they were on OAC therapy. Therefore, it is not surprising that higher efficacy was mentioned by 90% of VKA- and DOAC-treated patients as a top three ranked attribute. GPs need to understand the importance of high treatment efficacy to patients. Furthermore, prescribing medication that is more effective with regard to prevention of blood clots or stroke could help give peace of mind to patients. Less bleeding risk (safety aspect) was ranked second, emphasizing the importance of this topic, as both VKA- and DOAC-treated patients regarded bleeding as dangerous and cumbersome. Again, this finding underlines the need for GPs to be aware of this sentiment amongst patients with AF. Particular attention needs to be paid by GPs to patients on VKA, who are more likely to experience specific bleeding events, which are not only dangerous, but also have a negative impact on the patient’s daily life [3,4,5,6,7,8,9,10]. Finally, no need for thrombosis service (logistical aspect) ranked third, with one-third of VKA-treated patients stating that they would like to discontinue visiting the thrombosis service. Many found it time-consuming or annoying, which is something that GPs need to realize. Of interest, 64% of DOAC-treated patients ranked ‘Not needing INR checks’ in their top three important aspects of OAC therapy, which shows that they are happy that they don’t have to attend these visits. Therefore, GPs need to realize that, as many of their OAC-treated patients are elderly, attending frequent visits to the thrombosis service can be burdensome, and omitting these visits offers freedom to patients. Patients also stated that they felt adherence would be easier if the OAC dose was the same every day. This is something that is not straightforward when using VKA, particularly when combined with the fact that patients ranked prevention of stroke as the most important aspect of OAC therapy. Explicitly understanding the attributes of OAC that were ranked as most important by patients may help them choose between VKA and DOAC therapy. If we combine this with the finding that patients expect information on new OAC options from their HCP, there is a strong urgency for pro-active communication on treatment options and attributes from the HCP. The dislike of the thrombosis service checks in the DOAC group (patients with knowledge that they are not required with DOAC therapy) is a strong indicator that patients are happier without the need for these checks.
The main limitation of this study was the intra-individual subjectivity of the participants, which is inevitable when using a standardized questionnaire. Some patients did not completely understand the question(s) and their context, which resulted in differing personal perceptions and subsequent responses.
Conclusions
This study analyzed the perceptions and experiences of patients with AF regarding their disease and treatment, with the top two aspects of OAC treatment for patients consisting of safety (reduced risk of blood clots or stroke and lower bleeding risk) and not having to use the thrombosis service. VKA-treated patients valued the higher efficacy and safety profile of DOACs, in terms of reduced risk of both blood clots and bleeding and responded positively to the DOAC medication profile. Higher efficacy and lower risk of bleeding were valuable attributes to VKA-treated patients as these patients were afraid of experiencing a stroke and bothersome bleeding events. The thrombosis service was a burden to most patients, even though it seemed that VKA-treated patients were not particularly bothered. In fact, patients treated with VKAs accepted the thrombosis service as a necessity, hypothetically because they were largely unaware that another OAC option was available with no need for INR checks. Patients who had switched to DOAC therapy, on the other hand, were very appreciative of no longer needing regular check-ups to monitor their INR levels. These patients were therefore even more critical of the burden of these visits. VKA-treated patients hardly questioned the efficacy and safety of their medication or whether their medication could be more convenient. Our study showed that over half of the VKA-treated patients were willing to switch to DOAC therapy. Again, low patient awareness impacted their perceptions, making them less critical of VKA therapy than DOAC users who had previously received a VKA. Increasing awareness of DOAC therapy may enable VKA-treated patients to be more receptive to switching to a DOAC. Explicitly understanding the attributes of OAC that are ranked as most important by patients may help HCPs and patients choose between VKA and DOAC therapy. When combined with the finding that patients expect HCPs to provide information on new treatment options, there is a clear need for pro-active communication from the HCP on OAC treatment options and attributes. Raising awareness amongst HCPs about the perceptions and experiences of patients with AF may facilitate discussions between patients and their HCPs, which may ultimately result in improved outcomes for patients with AF [12].
Notes
Upon request, sponsor name would have been released after completion of research.
References
IPSOS. GPs—embrace independent NOAC prescription in the Netherlands. 2019.
NHG-werkgroep Atriumfibrilleren. NHG-Standaard Atriumfibrilleren. Huisarts Wet. 2017;60(9):460.
IQVIA Midas. Data on file. 2019.
Ruff CT, et al. Comparison of the efficacy and safety of new oral anticoagulants with warfarin in patients with atrial fibrillation: a meta-analysis of randomised trials. Lancet. 2014;383:955–62.
Lip GYH, et al. Effectiveness and safety of oral anticoagulants among nonvalvular atrial fibrillation patients. Stroke. 2018;49:2933–44.
Deitelzweig S, et al. Comparison of effectiveness and safety of treatment with apixaban vs. other oral anticoagulants among elderly nonvalvular atrial fibrillation patients. Curr Med Res Opin. 2017;33:1745–54.
Halvorsen S, et al. A nationwide registry study to compare bleeding rates in patients with atrial fibrillation being prescribed oral anticoagulants. Eur Heart J Cardiovasc Pharmacother. 2017;3:28–36.
Li X, et al. Effectiveness and safety of apixaban versus warfarin in non-valvular atrial fibrillation patients in “real-world” clinical practice. A propensity-matched analysis of 76,940 patients. Thromb Haemost. 2017;117:1072–82.
Yao X, et al. Effectiveness and safety of dabigatran, rivaroxaban, and apixaban versus warfarin in nonvalvular atrial fibrillation. J Am Heart Assoc. 2016;5(6):e003725.
Graham DJ, et al. Comparative stroke, bleeding, and mortality risks in older Medicare patients treated with oral anticoagulants for nonvalvular atrial fibrillation. Am J Med. 2019;132:596–604.
Adams WC. Conducting semi-structured interviews. In: Newcomer KE, et al., editors. Handbook of practical program evaluation. 4th ed. New York: Wiley Online Library; 2019.
SKIM. Understanding patient needs in Atrial Fibrillation. Patient understanding 101. 2019.
Acknowledgements
Funding
This research and the journal's rapid service fee were funded by Pfizer. The questionnaires used were aligned between sponsor and international market research group SKIM Europe; these questionnaires have been subjected to and passed all mandatory procedures and compliance checks as requested by the sponsor. Participating individuals received a nominal fee covering their expenses of €60 for in-home interviews and interviews by telephone and €70 if the interviews were conducted at the central location in Rotterdam.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Medical Writing and Editorial Assistance
The authors would like to thank Sarah Greig, PhD, of Springer Healthcare Communications, who provided English-language editing services. This medical writing assistance was funded by Pfizer.
Disclosures
Janneke van den Bent and author Marcel Slavenburg work at SKIM and received funding from Pfizer for the study. Thierry Barten is an employee of Pfizer and Margje Reijs-Scheijgrond is an independent project management professional working for Pfizer. Constance de Koning works at Medscope as an independent scientific writer.
Compliance with Ethics Guidelines
This was a non-interventional market research study and questionnaires were completed anonymously in accordance with the regulations and practice of market research governing bodies: European Society for Opinion and Marketing Research (ESOMAR) and European Pharmaceutical Market Research Association (EphMRA) and thus is exempt from requiring Clinical Research Ethics Committee or Independent Review Board approval. SKIM received informed consent from the patients included.
Data availability
The datasets during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author information
Authors and Affiliations
Corresponding author
Additional information
Digital features
To view digital features for this article go to https://doi.org/10.6084/m9.figshare.12162015.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Slavenburg, M., van den Bent, J.H., Barten, T. et al. Perceptions and Experiences of Atrial Fibrillation Patients on Their Condition and Oral Anticoagulant Treatment. Cardiol Ther 9, 409–420 (2020). https://doi.org/10.1007/s40119-020-00173-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40119-020-00173-8