Abstract
Objective design
We describe a case series of patients colonized with KPC-producing Enterobacteriaceae related to dialysis drains at patient’s bedside.
Setting
The study was set at the intensive care unit (ICU) of a tertiary referral hospital.
Patients
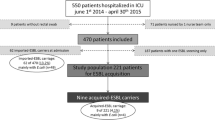
In March 2016, we discovered four ICU patients to be colonized with KPC-producing Enterobacteriaceae in routine screening. All of these patients had already received contact isolation, and all of them were treated with continuous veno-venous dialysis. Environmental examinations showed KPC-producing Enterobacteriaceae in dialysis drains in different ICU rooms and even in rooms not hosting KPC-colonized patients.
Interventions
Based on our findings, we suspected the dialysis drains as a reservoir of KPC-producing Enterobacteriaceae with a potential risk for the patients. Therefore, we decided to change the dialysis waste management.
Results
As a result, no KCP-producing Enterobacteriaceae were detected during the following weekly screening of the patients.
Conclusions
Installation of dialysis connection units including a drain system at the patient’s bedside is a comfortable way to provide water supply. In many ICUs, such dialysis drains are installed near the patients’ head and directly besides the infusion systems. When the drains are not used properly, in our opinion, they pose a risk of transmission of pathogens from the drain to the patient. Our findings support the need of specific precautions.

Similar content being viewed by others
References
Hajime Kanamori DJ, Weber WA. Rutala healthcare outbreaks associated with a water reservoir and infection prevention strategies. Clin Infect Dis 2016;62:1423–1435.
Ashita Tolwani MD. Continuous renal-replacement therapy for acute kidney injury. N Engl J Med. 2012;367:2505–14.
Kaufman J, Dhakal M, Patel B, et al. Community-acquired acute renal failure. Am J Kidney Dis. 1991;17:191–8.
Lameire N, Van Biesen W, Vanholder R. The changing epidemiology of acute renal failure. Nat Clin Pract Nephrol. 2006;2:364–77.
Uchino S, Kellum JA, Bellomo R, et al. Acute renal failure in critically ill patients: a multinational, multicenter study. JAMA. 2005;294:813–8.
Carstens A, Kepper U, Exner M, Hauri Kaase M, Wendt C. Plasmid-vermittelter Multispezies-Ausbruch mit Carbapenem-resistenten Enterobacteriaceae. Epid Bull. 2014;47:455–9. https://www.rki.de.
Robert Koch-Institut. Häufung von KPC-2 produzierenden Stämmen verschiedener Enterobacteriaceae-Spezies in Hessen. Epid Bull. 2014;21:183–4.
Mathers AJ, Cox HL, Kitchel B, Bonatti H, Brassinga AK, Carroll J, Scheld WM, Hazen KC, Sifri CD. Molecular dissection of an outbreak of carbapenem-resistant enterobacteriaceae reveals Intergenus KPC carbapenemase transmission through a promiscuous plasmid. MBio. 2011;2:e00204–11 (21:183–184)
Modul HAND-KISS_S. Referenzdaten. Nationales Referenzzentrum für die Surveillance von nosokomialen Infektionen. http://www.nrz-hygiene.de/fileadmin/nrz/module /hand/HAND_S_Referenzdaten_2015_DE.pdf. Published May 17, 2016. Accessed 2 Jan 2018.
Falagas ME, Tansarli GS, Karageorgopoulos DE, et al. Deaths attributable to carbapenem-resistant Enterobacteriaceae infections. Emerg Infect Dis. 2014;20:1170–5.
Salm F, Deja M, Kola A, et al. Prolonged outbreak of clonal MDR Pseudomonas aeruginosa on an intensive care unit: contaminated sinks and contamination of ultra-filtrate bags as possible route of transmission? Antimicrob Resist Infect Control. 2016;5:53.
Funding
None reported.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors report no conflicts of interest relevant to this article.
Rights and permissions
About this article
Cite this article
Ross, B., Krull, M., Rath, P. et al. Dialysis drains as a possible source for carbapenem-resistant pathogens causing an ICU outbreak. Infection 47, 233–238 (2019). https://doi.org/10.1007/s15010-018-1239-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-018-1239-9