Abstract
Purpose
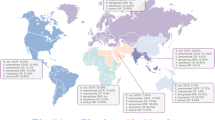
To analyze the impact of the International Nosocomial Infection Control Consortium (INICC) multidimensional infection control strategy including a practice bundle to reduce the rates of central line-associated bloodstream infection (CLAB) in patients hospitalized in pediatric intensive care units (PICUs) of hospitals, which are members of the INICC, from nine cities of five developing countries: Colombia, India, Mexico, Philippines, and Turkey.
Methods
CLAB rates were determined by means of a prospective surveillance study conducted on 1,986 patients hospitalized in nine PICUs, over a period of 12,774 bed-days. The study was divided into two phases. During Phase 1 (baseline period), active surveillance was performed without the implementation of the multi-faceted approach. CLAB rates obtained in Phase 1 were compared with CLAB rates obtained in Phase 2 (intervention period), after implementation of the INICC multidimensional infection control program.
Results
During Phase 1, 1,029 central line (CL) days were recorded, and during Phase 2, after implementing the CL care bundle and interventions, we recorded 3,861 CL days. The CLAB rate was 10.7 per 1,000 CL days in Phase 1, and in Phase 2, the CLAB rate decreased to 5.2 per 1,000 CL days (relative risk [RR] 0.48, 95% confidence interval [CI] 0.29–0.94, P = 0.02), showing a reduction of 52% in the CLAB rate.
Conclusions
This study shows that the implementation of a multidimensional infection control strategy was associated with a significant reduction in the CLAB rates in the PICUs of developing countries.
Similar content being viewed by others
Introduction
Central line-associated bloodstream infections (CLABs) have long been associated with excess lengths of stay (LOS), increased hospital costs, and attributable mortality in studies both from high-income countries [1–4] and limited-resource countries [5–7]. The vulnerability of children hospitalized in pediatric intensive care units (PICUs) to mortality and morbidity due to CLABs was highlighted in the scientific literature [6–9]. However, the burden of CLAB in the PICU is not limited to mortality, and in different studies, CLAB was related to other adverse consequences and independent risk factors, such as longer duration of mechanical ventilation, extended device use, unplanned hospital admissions, specific medical therapies, and the presence of noncardiac comorbidities [8, 10, 11].
In addition, the socio-economic level of a country was reported to have an adverse effect on device-associated healthcare-associated infection (DA-HAI) rates in the ICU settings of developing countries. CLAB rates were shown to be higher in low-income countries than in lower–middle- and upper–middle-income countries [12]. In the same manner, hospital type is also considered to be a significant factor influencing DA-HAI rates, which were reported to be substantially higher in “academic and public hospitals” than in private ones [12].
In a wide number of studies, it was demonstrated that implementing infection control programs and practice bundles—including hand hygiene, skin antisepsis, maximal barriers, and timely central line (CL) removal, among others—were associated with a reduction in the incidence density of CLAB [8, 11, 13–19].
Within the particular context of limited-resource countries, there is insufficient recognition of CLABs as a preventable DA-HAI, which is fundamental in order to achieve surveillance for measuring infection risks, outcomes, and processes [20, 21]. Nevertheless, in addition to the implementation of an effective infection control program, there is a pressing need for feedback of surveillance data [14, 19, 22]. Since 2002, the International Nosocomial Infection Control Consortium (INICC) has performed outcome and process surveillance, as part of an integral program specifically designed for ICUs in developing countries [23, 24]. The results reported from INICC hospitals revealed that DA-HAI rates in the ICUs of limited-resources countries are 3–5 times higher than rates in the ICUs of high-income countries [25, 26].
The implementation of the INICC multidimensional program for CLAB prevention is based on the recommendations and guidelines published by the Society for Healthcare Epidemiology of America (SHEA) and the Infectious Diseases Society of America (IDSA) in 2008. These guidelines describe different recommendations for CLAB prevention in the ICU that are classified into categories regarding the existing scientific evidence, applicability, and their prospective economic effects [27–29].
With the aim of reducing these high CLAB rates, we implemented a multidimensional infection control program—which included specific interventions for CLAB prevention, education, practice bundle, outcome surveillance, process surveillance, feedback of CLAB rates, as well as performance feedback of infection control practices—in 11 PICUs of the following five countries: Colombia, India, Mexico, Philippines, and Turkey.
This study analyzes the particular effect of this preventive multidimensional strategy on CLAB rates in the PICUs of developing countries from October 2003 to December 2010.
Methods
Setting and study design
The study was conducted in nine PICUs in nine hospitals which are members of the INICC in the following five countries: Colombia, India, Mexico, Philippines, and Turkey. Each hospital had been actively participating in the INICC surveillance program for at least 3 months and has an infection control team (ICT) comprised of a medical doctor trained in pediatrics, with formal education and background in internal medicine, infectious diseases, and/or hospital epidemiology, and infection control professionals (ICPs). This study was performed in two phases: Phase 1 (baseline period) and Phase 2 (intervention period). The Institutional Review Board (IRB) at each hospital approved the study protocol. Other hospital and PICU characteristics are summarized in Table 1.
Intervention period (Phase 2)
The intervention period was initiated after 3 months of participation in the INICC surveillance program. The average length of the intervention period was 12.8 months ± standard deviation (SD) 8.9 (range 3–24). The INICC multidimensional infection control strategy includes the following: (1) bundle of infection control interventions, (2) education, (3) outcome surveillance, (4) process surveillance, (5) feedback of CLAB rates, and (6) performance feedback of infection control practices.
Components of the CL care bundle for CLABs
The bundle consisted of the following interventions:
-
1.
Performance of hand hygiene before CL insertion or manipulation [24].
-
2.
Use a chlorhexidine-based antiseptic for skin preparation [16, 30, 31].
-
3.
Use of an all-inclusive catheter cart or kit [32].
-
4.
Use of maximal sterile barrier precautions during CL insertion [33].
-
5.
Disinfection of line hubs, needleless connectors, and infection ports before accessing the CL [34, 35].
- 6.
Education
Education of healthcare personnel involved in the insertion, care, and maintenance of CLs about CLAB prevention [38].
INICC methodology
The INICC surveillance program includes two components: outcome surveillance (DA-HAI rates and their adverse effects, including mortality rates) and process surveillance (adherence to hand hygiene and other basic preventive infection control practices) [23].
Investigators were required to complete outcome and process surveillance forms at their hospitals, which were then sent to the INICC headquarters office in Buenos Aires, Argentina, for their monthly analysis.
Outcome surveillance
The performance of active surveillance for CLAB was associated with a reduction of CLAB rates [39].
The INICC surveillance program applies methods and definitions for HAI developed by the U.S. Centers for Disease Control and Prevention (CDC) for the National Nosocomial Infections Surveillance/National Healthcare Safety Network (NNIS/NHSN) program [40, 41]; however, INICC methods have been adapted to the setting of developing countries, due to their different socio-economic status and specific resource limitations 23.
Outcome surveillance includes rates of CLAB, ventilator-associated pneumonia (VAP), and catheter-associated urinary tract infection (CAUTI) per 1,000 device-days, microorganism profile, bacterial resistance, length of stay, and mortality in their ICUs.
Process surveillance
The infection control and prevention strategies implemented in INICC member hospitals are based on inexpensive and basic evidence-based measures, including outcome surveillance, process surveillance, education, and performance feedback of outcome surveillance and process surveillance [19, 24, 42, 43].
Process surveillance was designed to assess compliance with easily measurable key infection control practices, such as the surveillance of compliance rates for hand hygiene practices and specific measures for the prevention of CLAB, CAUTI, and VAP [23]. Hand hygiene compliance by healthcare workers (HCWs)—based on the frequency with which hand hygiene is performed when clearly indicated—is monitored by the ICPs during randomly selected 1-h observation periods three times a week. Although HCWs are aware that hand hygiene practices are regularly monitored, they are not informed of the schedule for hand hygiene observations. Contacts are monitored through direct observation, and the ICPs record the hand hygiene opportunities and compliance before contact with each patient. ICPs are trained to detect hand hygiene compliance and record it on a form specifically designed for the study. In particular, the INICC direct observation comprises the “five moments for hand hygiene” as recommended by the World Health Organization (WHO). The “five moments” were designed on the basis of the evidence concerning HAI prevention and control, being rational, plausible, and fully appropriate for the healthcare setting. Namely, they include the monitoring of the following moments: (1) before patient contact, (2) before an aseptic task, (3) after body fluid exposure risk, (4) after patient contact, and (5) after contact with patient surroundings [44].
CL care compliance is also monitored and recorded 5 days a week by means of completing surveillance forms that evaluate whether infection control procedures were correctly carried out by the HCW. The ICP observing the activity in the ICU filled out a standardized form that contained the following data: total number of inserted CLs for each patient for the whole ICU; total number of dressings placed to protect the puncture site; total number of dressings, specifying the type of dressing (sterile gauze or transparent dressing) used to protect the puncture site; total number of dressings in correct condition, evaluating whether the dressing was clean, dry, and correctly adhered to the puncture site; and the total number of cases, in which the dates of insertion were written in the administration set of the patient or the dressing [23].
Performance feedback
Performance feedback of infection control processes is an essential tool for improving adherence with preventive strategies and guidelines, as shown in different INICC studies [19, 24, 42, 43, 45].
Upon processing the hospitals’ surveillance data on a monthly basis, the INICC research team, at INICC Headquarters located in Buenos Aires, Argentina, prepares and sends to each ICT a final report on the results of outcome surveillance, that is, monthly DA-HAI rates, length of stay, bacterial profile and resistance, and mortality, as well as process surveillance rates, including compliance with hand hygiene, care of CL and urinary catheter, and measures for VAP prevention [23].
Performance feedback is provided to HCWs working in the PICU by communicating the assessment of practices routinely performed by them. The resulting rates are reviewed by the ICT at monthly meetings, where charts are analyzed, and statistical graphs and visuals are posted inside the ICU, to provide an overview of rates of DA-HAIs and rates measuring compliance with infection control practices. This infection control tool is key to enabling the ICT and ICU staff to focus on the necessary strategies for the improvement of low compliance rates.
Definitions
Laboratory-confirmed CLAB
When CLAB is suspected, the CL is removed aseptically and the distal 5 cm of the catheter is amputated and cultured, using the standardized semi-quantitative method [46]. Concomitant blood cultures are drawn percutaneously in most cases. In each hospital, standard laboratory methods are used to identify microorganisms and standardized susceptibility testing is performed.
A patient with a CL who has a recognized pathogen isolated from one or more percutaneous blood cultures after 48 h of catheterization; the pathogen cultured from blood is not related to an infection at another site; and a patient has one or more of the following signs or symptoms: fever (≥38°C), chills, or hypotension. With skin commensals (diphtheroids, Bacillus spp., Propionibacterium spp., coagulase-negative staphylococci or micrococci), the organism has been recovered from two or more separate blood cultures [41].
Clinically suspected CLAB
A patient with a CL who has at least one of the following clinical signs, with no other recognized cause: fever (≥38°C), hypotension (systolic blood pressure ≤90 mmHg), or oliguria (≤20 mL/h), but blood cultures were either not obtained or no organisms were recovered from blood cultures; there is no apparent infection at another site; and the physician instigates antimicrobial therapy [41].
Statistical methods
Patient characteristics during the baseline and intervention periods in each PICU were compared using Fisher’s exact test for dichotomous variables and unmatched Student’s t-test for continuous variables. Relative risk (RR) ratios with 95% confidence intervals (CIs) were calculated for comparisons of rates of CLAB and CL care bundle at baseline and the subsequent intervention period. P-values <0.05 by two-sided tests were considered to be significant.
We used a negative binomial regression model to attempt to describe the relationship between the lengths of time an ICU participates in the INICC with the CLAB rate recorded. The dependent variable is the number of CLABs recorded (a negative binomial model is used because, although this is count data, there are a large number of zero counts) and the independent variable is the length of time that a unit participated in the INICC in months. CLAB counts are grouped across ICUs in 1-month periods.
Results
Over the whole study period, 1,986 patients hospitalized for 12,774 days in nine PICUs were enrolled, and totaling 4,890 CL days. The participating hospitals were summarized and classified according to number of PICUs, type of hospital, and country. The first ICUs that participated in the study began collecting data in October 2003, and the latest information we included in this analysis is from November 2010 (Table 1).
Patient characteristics, such as gender, underlying diseases, previous infection, and length of stay with the CL in place, were similar during the baseline and intervention phases (Table 2).
The microorganisms profile is shown in Table 3.
In relation to compliance rates, during Phase 2, hand hygiene compliance improved significantly to 79%. Likewise, the presence of CLs with sterile gauze or sterile transparent dressing rose from 84.0 to 97.2% (RR 1.16, 95% CI 1.07–1.26, P = 0.0004) and the presence of sterile gauze or sterile transparent dressing in good condition rose from 83.9 to 93.9% (RR 1.12, 95% CI 1.03–1.21, P = 0.0068), showing a significant improvement in the performance of infection control practices (Table 4).
Regarding CLAB rates, during Phase 1 (baseline period), there were 1,029 documented CL days, for a mean CL use of 0.41. There were 11 CLABs, for an overall baseline rate of 10.7 CLABs per 1,000 CL days. In Phase 2, after the implementation of the multidimensional infection control program, there were 3,861 CL days, for a mean CL use of 0.38. There were 20 CLABs, for an incidence density of 5.2 per 1,000 CL days. These results showed a CLAB rate reduction from a baseline of 52% (10.7–5.2 CLABs per 1,000 CL days; RR 0.48, 95% CI 0.29–0.94, P = 0.0271) (Table 5).
Our negative binomial regression model describes the relationship between the lengths of time an ICU participates in the INICC with the CLAB rate recorded. Although this method does not account for the correlation in counts across ICUs over the study period, it is a simple way to describe the relationship between the two, and, as the data is sparse (only 31 CLAB in total across the whole study) and the number of CL days contributed in each study period low, it provides a simple graph that is relatively easy to interpret. Figure 1 shows the pooled mean CLAB rate per 1,000 CL days plotted for each month, with the predicted line giving the CLAB count from this negative binomial model.
Central line-associated bloodstream infection (CLAB) rates by month with fitted values: negative binomial regression. Note that the variation in the predicted CLAB rate is shown as a straight line because of the variation in central line (CL) days contributed by the intensive care units (ICUs) during the study period
Discussion
Our findings showed how improvements in CL care practices are associated with a reduction in the risk of CLABs. Our multidimensional infection control program was focused on CLAB outcome and process surveillance, the implementation of a bundle of CL care techniques, education, adherence to infection control guidelines, and performance feedback, which were adapted as a simple but effective strategy for the limited-resource setting.
The reduction of CLABs is considered of primary importance in public health in the developed world. In developing countries, CLAB rates were reported to be 3–5 times higher than in US ICUs [26, 47]. There are intrinsic factors which contribute to these higher DA-HAI rates, associated with their lower socio-economic level and lack of adequate financial resources, personnel levels, and medical supplies [12]. CLAB rates in ICUs from developing countries were found to be higher in low-income countries than in lower–middle and upper–middle-income countries [12]. Similarly, the type of hospital also influences DA-HAI rates in ICUs, which were shown to be statistically significantly higher in “academic and public hospitals” than in “private” ones [12].
Successful CLAB preventive strategies have been described in the literature over the last several decades [8, 11, 15–18, 48]. It was shown that the CLAB rate in the PICU can be reduced by more than 30% [15, 16]. The implementation of a multidimensional infection control program focused on CLAB surveillance was proved to be an essential tool to countervail CLABs and their severe consequences in the PICU setting [8, 11, 13, 17]. In a study conducted by the INICC in 15 developing countries, it was shown that, after the inception of a strategy that included education, performance feedback, outcome, and process surveillance, there was a cumulative reduction of 54% in the CLAB rate and of 58% in the mortality rate in the ICU [49].
The INICC multidimensional strategy for CLAB prevention is based on the guidelines published by the SHEA and the IDSA in 2008. These guidelines provide evidence-based recommendations and cost-effective infection control measures, which can be feasibly adapted to the ICU setting in developing countries [29]. Our multidimensional approach was based on infection control measures, which were previously assessed in the developed world, such as hand hygiene [24, 45] and CL care techniques, education, and performance feedback [50, 51]. The successful results obtained with performance feedback have also been evaluated as a key measure to reduce and control DA-HAI in different studies conducted in the INICC member hospitals and the developing world [19, 24, 42, 43, 45, 49, 52–55].
In this respect, it was shown in studies performed in Argentina and in Mexico that the sequential implementation of education and performance feedback programs led to substantial reductions in the incidence of CLAB [19, 54].
The analysis on our baseline data showed a high incidence density of CLAB in our PICUs, which was reduced by 52% after the implementation of the multidimensional strategy. During baseline and intervention, patients’ characteristics (gender, underlying diseases [abdominal surgery, thoracic surgery, previous infection], and CL duration) were similar. All participating hospitals are from countries with low, lower–middle, and upper–middle economies. The type of hospital was not considered to be a factor that could explain the high CLAB incidence, because most of the enrolled patients were from academic and private hospitals, and only 12% were from public hospitals, whose DA-HAI rates have been reported to be negatively affected by their limited financial resources and insufficient ICU staff if compared to the other types of hospitals [12].
We found statistically significant improvements in hand hygiene compliance, within the CL care bundle, in relation to the presence and good condition of catheters with sterile gauze or sterile transparent dressing, and we had a significant reduction in the use ratio of CL. In this respect, in a study performed in Argentina, it was demonstrated that the inception of a program focused on education and frequent performance feedback resulted in a sustained improvement with hand hygiene compliance, which also coincided with a reduction in DA-HAI rates in the ICU setting [24].
These findings were similar to the results reported in a study performed in Mexico, in which the effectiveness of an infection control program consisting of education, process control, and performance feedback was associated to significant reductions in the rates of CLAB and mortality [54].
In conclusion, an analysis of the implementation of the multidimensional infection control program for CLAB prevention showed that the reduction in the CLAB rate of our PICUs was associated with the effective impact of our multidimensional strategy in the pediatric setting of developing countries. Clearly, the results from Fig. 1 are encouraging: the CLAB rates dropped to almost zero as the time in the INICC increases.
However, despite our motivating results, we consider that our rates also indicated there is a need for continuous and sustained improvement in practices, as they are higher than the rates reported from the developed world [26, 47].
Limitations of this study are based around the fact that our findings are not to be generalized to PICU patients from every developing country; however, this study proved that a multidimensional approach, including process and outcome surveillance in addition to a bundle of CL interventions, is fundamental to understand and fight against the adverse effects of CLAB in the PICUs of limited-resource settings. Second, the setting of a 3-month baseline period may be short and might have overestimated the effect of the intervention; however, this duration of baseline period is common in the scientific literature [18]. Finally, we could not quantify in detail information for each PICU on the compliance of each bundle component and other nonquantifiable interventions included in our multidimensional approach, such as education and training.
We expect that the infection control and prevention multifaceted approach fostered by the INICC will increasingly be carried out in the context of the developing world to achieve successful reductions in DA-HAIs.
References
Digiovine B, Chenoweth C, Watts C, et al. The attributable mortality and costs of primary nosocomial bloodstream infections in the intensive care unit. Am J Respir Crit Care Med. 1999;160:976–81.
Warren DK, Quadir WW, Hollenbeak CS, et al. Attributable cost of catheter-associated bloodstream infections among intensive care patients in a nonteaching hospital. Crit Care Med. 2006;34:2084–9.
Biwersi C, Hepping N, Bode U, et al. Bloodstream infections in a German paediatric oncology unit: prolongation of inpatient treatment and additional costs. Int J Hyg Environ Health. 2009;212:541–6.
Prowle JR, Echeverri JE, Ligabo EV, et al. Acquired bloodstream infection in the intensive care unit: incidence and attributable mortality. Crit Care. 2011;15:R100.
Higuera F, Rangel-Frausto MS, Rosenthal VD, et al. Attributable cost and length of stay for patients with central venous catheter-associated bloodstream infection in Mexico City intensive care units: a prospective, matched analysis. Infect Control Hosp Epidemiol. 2007;28:31–5.
Gupta A, Kapil A, Lodha R, et al. Burden of healthcare-associated infections in a paediatric intensive care unit of a developing country: a single centre experience using active surveillance. J Hosp Infect. 2011;78:323–6.
Rosenthal VD, Guzman S, Migone O, et al. The attributable cost, length of hospital stay, and mortality of central line-associated bloodstream infection in intensive care departments in Argentina: a prospective, matched analysis. Am J Infect Control. 2003;31:475–80.
Kline AM. Pediatric catheter-related bloodstream infections: latest strategies to decrease risk. AACN Clin Issues. 2005;16:185–98; quiz 272–4.
Grisaru-Soen G, Sweed Y, Lerner-Geva L, et al. Nosocomial bloodstream infections in a pediatric intensive care unit: 3-year survey. Med Sci Monit. 2007;13:CR251–7).
Costello JM, Graham DA, Morrow DF, et al. Risk factors for central line-associated bloodstream infection in a pediatric cardiac intensive care unit. Pediatr Crit Care Med. 2009;10:453–9.
Odetola FO, Moler FW, Dechert RE, et al. Nosocomial catheter-related bloodstream infections in a pediatric intensive care unit: risk and rates associated with various intravascular technologies. Pediatr Crit Care Med. 2003;4:432–6.
Rosenthal VD, Lynch P, Jarvis WR, et al. Socioeconomic impact on device-associated infections in limited-resource neonatal intensive care units: findings of the INICC. Infection. 2011;39:439–50
Miller MR, Griswold M, Harris JM 2nd, et al. Decreasing PICU catheter-associated bloodstream infections: NACHRI’s quality transformation efforts. Pediatrics. 2010;125:206–13.
Jeffries HE, Mason W, Brewer M, et al. Prevention of central venous catheter-associated bloodstream infections in pediatric intensive care units: a performance improvement collaborative. Infect Control Hosp Epidemiol. 2009;30:645–51.
Bhutta A, Gilliam C, Honeycutt M, et al. Reduction of bloodstream infections associated with catheters in paediatric intensive care unit: stepwise approach. BMJ. 2007;334:362–5.
Soothill JS, Bravery K, Ho A, et al. A fall in bloodstream infections followed a change to 2% chlorhexidine in 70% isopropanol for catheter connection antisepsis: a pediatric single center before/after study on a hemopoietic stem cell transplant ward. Am J Infect Control. 2009;37:626–30.
McCaskey MS. Preventing catheter-related bloodstream infections: a pediatric case study. Home Healthc Nurse. 2009;27:124–6.
Pronovost P, Needham D, Berenholtz S, et al. An intervention to decrease catheter-related bloodstream infections in the ICU. N Engl J Med. 2006;355:2725–32.
Rosenthal VD, Guzman S, Pezzotto SM, et al. Effect of an infection control program using education and performance feedback on rates of intravascular device-associated bloodstream infections in intensive care units in Argentina. Am J Infect Control. 2003;31:405–9.
Hughes JM. Study on the efficacy of nosocomial infection control (SENIC Project): results and implications for the future. Chemotherapy. 1988;34:553–61.
Rosenthal VD. Central line-associated bloodstream infections in limited-resource countries: a review of the literature. Clin Infect Dis. 2009;49:1899–907.
Dueñas L, Bran de Casares A, Rosenthal VD, et al. Device-associated infections rates in pediatrics and neonatal intensive care units in El Salvador: findings of the INICC. J Infect Dev Ctries 2011;5:445–51.
Rosenthal VD, Maki DG, Graves N. The International Nosocomial Infection Control Consortium (INICC): goals and objectives, description of surveillance methods, and operational activities. Am J Infect Control. 2008;36:e1–12.
Rosenthal VD, Guzman S, Safdar N. Reduction in nosocomial infection with improved hand hygiene in intensive care units of a tertiary care hospital in Argentina. Am J Infect Control. 2005;33:392–7.
Rosenthal VD, Maki DG, Jamulitrat S, et al. International Nosocomial Infection Control Consortium (INICC) report, data summary for 2003–2008, issued June 2009. Am J Infect Control. 2010;38:95–104.e2.
Edwards JR, Peterson KD, Mu Y, et al. National Healthcare Safety Network (NHSN) report: data summary for 2006 through 2008, issued December 2009. Am J Infect Control. 2009;37:783–805.
O’Grady NP, Alexander M, Burns LA, et al. Guidelines for the prevention of intravascular catheter-related infections. Am J Infect Control. 2011;39:S1–34.
O’Grady NP, Alexander M, Burns LA, et al. Summary of recommendations: guidelines for the prevention of intravascular catheter-related infections. Clin Infect Dis. 2011;52:1087–99.
Marschall J, Mermel LA, Classen D, et al. Strategies to prevent central line-associated bloodstream infections in acute care hospitals. Infect Control Hosp Epidemiol. 2008;29(Suppl 1):S22–30.
Humar A, Ostromecki A, Direnfeld J, et al. Prospective randomized trial of 10% povidone–iodine versus 0.5% tincture of chlorhexidine as cutaneous antisepsis for prevention of central venous catheter infection. Clin Infect Dis. 2000;31:1001–7.
Chaiyakunapruk N, Veenstra DL, Lipsky BA, Saint S. Chlorhexidine compared with povidone–iodine solution for vascular catheter-site care: a meta-analysis. Ann Intern Med. 2002;136:792–801.
Berenholtz SM, Pronovost PJ, Lipsett PA, et al. Eliminating catheter-related bloodstream infections in the intensive care unit. Crit Care Med. 2004;32:2014–20.
Raad II, Hohn DC, Gilbreath BJ, et al. Prevention of central venous catheter-related infections by using maximal sterile barrier precautions during insertion. Infect Control Hosp Epidemiol. 1994;15:231–8.
Casey AL, Worthington T, Lambert PA, et al. A randomized, prospective clinical trial to assess the potential infection risk associated with the PosiFlow needleless connector. J Hosp Infect. 2003;54:288–93.
Luebke MA, Arduino MJ, Duda DL, et al. Comparison of the microbial barrier properties of a needleless and a conventional needle-based intravenous access system. Am J Infect Control. 1998;26:437–41.
Parenti CM, Lederle FA, Impola CL, et al. Reduction of unnecessary intravenous catheter use. Internal medicine house staff participate in a successful quality improvement project. Arch Intern Med. 1994;154:1829–32.
Lederle FA, Parenti CM, Berskow LC, et al. The idle intravenous catheter. Ann Intern Med. 1992;116:737–8.
Eggimann P, Harbarth S, Constantin MN, et al. Impact of a prevention strategy targeted at vascular-access care on incidence of infections acquired in intensive care. Lancet. 2000;355:1864–8.
Gastmeier P, Geffers C, Brandt C, et al. Effectiveness of a nationwide nosocomial infection surveillance system for reducing nosocomial infections. J Hosp Infect. 2006;64:16–22.
Emori TG, Culver DH, Horan TC, et al. National nosocomial infections surveillance system (NNIS): description of surveillance methods. Am J Infect Control. 1991;19:19–35.
Horan TC, Andrus M, Dudeck MA. CDC/NHSN surveillance definition of health care-associated infection and criteria for specific types of infections in the acute care setting. Am J Infect Control. 2008;36:309–32.
Rosenthal VD, Guzman S, Crnich C. Impact of an infection control program on rates of ventilator-associated pneumonia in intensive care units in 2 Argentinean hospitals. Am J Infect Control. 2006;34:58–63.
Rosenthal VD, Guzman S, Safdar N. Effect of education and performance feedback on rates of catheter-associated urinary tract infection in intensive care units in Argentina. Infect Control Hosp Epidemiol. 2004;25:47–50.
Sax H, Allegranzi B, Chraïti MN, et al. The World Health Organization hand hygiene observation method. Am J Infect Control. 2009;37:827–34.
Rosenthal VD, McCormick RD, Guzman S, et al. Effect of education and performance feedback on handwashing: the benefit of administrative support in Argentinean hospitals. Am J Infect Control. 2003;31:85–92.
Maki DG, Weise CE, Sarafin HW. A semiquantitative culture method for identifying intravenous-catheter-related infection. N Engl J Med. 1977;296:1305–9.
Guanche-Garcell H, Requejo-Pino O, Rosenthal VD, et al. Device-associated infection rates in adult intensive care units of Cuban university hospitals: International Nosocomial Infection Control Consortium (INICC) findings. Int J Infect Dis. 2011;15:e357–62.
Royer T. Implementing a better bundle to achieve and sustain a zero central line-associated bloodstream infection rate. J Infus Nurs. 2010;33:398–406.
Rosenthal VD, Maki DG, Rodrigues C, et al. Impact of International Nosocomial Infection Control Consortium (INICC) strategy on central line-associated bloodstream infection rates in the intensive care units of 15 developing countries. Infect Control Hosp Epidemiol. 2010;31:1264–72.
Barsuk JH, Cohen ER, Feinglass J, et al. Use of simulation-based education to reduce catheter-related bloodstream infections. Arch Intern Med. 2009;169:1420–3.
Marshall C, Black J. Education-based intervention to prevent catheter-associated bloodstream infection. Infect Control Hosp Epidemiol. 2007;28:370; author reply 370–1.
Franzetti F, Rosenthal VD, Cappoia S, et al. Outcome surveillance plus feedback effect on rates of ventilator associated pneumonia and mortality in Italian intensive care units. In: Proceedings and Abstracts of the 7th Annual Meeting of the International Federation of Infection Control (IFIC), Spier Estate, Stellenbosch, South Africa, 4th July 2006. p. 34.
Higuera F, Duarte P, Franco G, et al. Multi-center national prospective study to evaluate hand washing compliance in public hospitals from Mexico. Behaviour comparison between different stratums. In: Proceedings and Abstracts of the Fifth Pan American Congress of Infection Control and Hospital Epidemiology, Lima, Peru, 7th to 10th October 2004. p. 21.
Higuera F, Rosenthal VD, Duarte P, et al. The effect of process control on the incidence of central venous catheter-associated bloodstream infections and mortality in intensive care units in Mexico. Crit Care Med. 2005;33:2022–7.
Santana SL, Furtado GH, Wey SB, et al. Impact of an education program on the incidence of central line-associated bloodstream infection in 2 medical-surgical intensive care units in Brazil. Infect Control Hosp Epidemiol. 2008;29:1171–3.
Lin DM, Weeks K, Bauer L, et al. Eradicating central line-associated bloodstream infections statewide: the Hawaii experience. Am J Med Qual. 2011 [Epub ahead of print].
Acknowledgments
The authors thank the many healthcare professionals at each member hospital who assisted with the conduct of surveillance in their hospital, including the surveillance nurses, clinical microbiology laboratory personnel, and the physicians and nurses providing care for the patients during the study, without their cooperation and generous assistance, this INICC would not be possible; Mariano Vilar, Debora Lopez Burgardt, and Alejo Ponce de Leon, who work at the INICC headquarters in Buenos Aires, Argentina, for their hard work and commitment to achieve the INICC goals; the INICC country coordinators (Altaf Ahmed, Carlos A. Álvarez-Moreno, Apisarnthanarak Anucha, Luis E. Cuéllar, Bijie Hu, Hakan Leblebicioglu, Eduardo A. Medeiros, Yatin Mehta, Lul Raka, Toshihiro Mitsuda, and Virgilio Bonilla Sanchez); the INICC advisory board (Carla J. Alvarado, Gary L. French, Nicholas Graves, William R. Jarvis, Patricia Lynch, Dennis Maki, Russell N. Olmsted, Didier Pittet, Wing Hong Seto, and William Rutala), who have so generously supported this unique international infection control network; and Patricia Lynch, who inspired and supported us to follow our dreams, despite obstacles. The authors declare that they did not receive any personal funding, and the funding for the activities carried out at the INICC headquarters were provided by the corresponding author, Victor D. Rosenthal, and the Foundation to Fight against Nosocomial Infections.
Conflict of interest
The authors state that they do not have any conflicts of interest to declare.
Ethical standard
Every hospital’s Institutional Review Board agreed to the study protocol, and patient confidentiality was protected by codifying the recorded information, making it identifiable only to the ICT.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rosenthal, V.D., Ramachandran, B., Villamil-Gómez, W. et al. Impact of a multidimensional infection control strategy on central line-associated bloodstream infection rates in pediatric intensive care units of five developing countries: findings of the International Nosocomial Infection Control Consortium (INICC). Infection 40, 415–423 (2012). https://doi.org/10.1007/s15010-012-0246-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-012-0246-5