Abstract
BACKGROUND:
This study aimed to explore the effect of a nanomaterial-based miR-320a inhibitor sustained release system in trauma-induced osteonecrosis of the femoral head (TIONFH).
METHODS:
The miR-320a inhibitor-loaded polyethylene glycol (PEG)- Poly(lactic-co-glycolic acid) (PLGA)- Poly-L-lysine (PLL) nanoparticles were constructed using the double emulsion method. The TIONFH rabbit model was established to observe the effects of miR-320a inhibitor nanoparticles in vivo. Hematoxylin–eosin staining and microcomputed tomography scanning were used for bone morphology analysis. Bone marrow mesenchymal stem cells (BMSCs), derived from TIONFH rabbits, were used for in vitro experiments. Cell viability was determined using the MTT assay.
RESULTS:
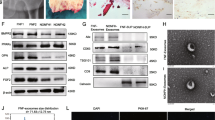
High expression of miR-320a inhibited the osteogenic differentiation capacity of BMSCs in vitro by inhibiting the expression of the osteoblastic differentiation markers ALP and RUNX2. MiR-320a inhibitor-loaded PEG-PLGA-PLL nanoparticles were constructed with a mean loading efficiency of 1.414 ± 0.160%, and a mean encapsulation efficiency of 93.45 ± 1.24%, which released 50% of the loaded miR-320a inhibitor at day 12 and 80% on day 18. Then, inhibitor release entered the plateau. After treatment with the miR-320a inhibitor nanoparticle, the empty lacunae were decreased in the femoral head tissue of TIONFH rabbits, and the osteoblast surface/bone surface (Ob.S/BS), osteoblast number/bone perimeter (Ob.N/B.Pm), bone volume fraction, and bone mineral density increased. Additionally, the expression of osteogenic markers RUNX2 and ALP was significantly elevated in the TIONFH rabbit model.
CONCLUSION:
The miR-320a inhibitor-loaded PEG-PLGA-PLL nanoparticle sustained drug release system significantly contributed to bone regeneration in the TIONFH rabbit model, which might be a promising strategy for the treatment of TIONFH.







Similar content being viewed by others
Data availability statement
The datasets used and/or analyzed during the present study are available from the corresponding author on reasonable request.
References
Cohen-Rosenblum A, Cui Q. Osteonecrosis of the femoral head. Orthop Clin North Am. 2019;50:139–49.
Xu J, Gong H, Lu S, Deasey MJ, Cui Q. Animal models of steroid-induced osteonecrosis of the femoral head-a comprehensive research review up to 2018. Int Orthop. 2018;42:1729–37.
Zhang Y, Zhuang Z, Wei Q, Li P, Li J, Fan Y, et al. Inhibition of miR-93-5p promotes osteogenic differentiation in a rabbit model of trauma-induced osteonecrosis of the femoral head. FEBS Open Bio. 2021;11:2152–65.
Guerado E, Caso E. The physiopathology of avascular necrosis of the femoral head: an update. Injury. 2016;47:S16-26.
Zhao D, Zhang F, Wang B, Liu B, Li L, Kim SY, et al. Guidelines for clinical diagnosis and treatment of osteonecrosis of the femoral head in adults (2019 version). J Orthop Translat. 2020;21:100–10.
Yang C, Liu X, Zhao K, Zhu Y, Hu B, Zhou Y, et al. miRNA-21 promotes osteogenesis via the PTEN/PI3K/Akt/HIF-1α pathway and enhances bone regeneration in critical size defects. Stem Cell Res Therapy. 2019;10:65.
Yin N, Zhu L, Ding L, Yuan J, Du L, Pan M, et al. MiR-135-5p promotes osteoblast differentiation by targeting HIF1AN in MC3T3-E1 cells. Cell Mol Biol Letters. 2019;24:51.
Kong Y, Chen ZT. MiR-146a regulates osteogenic differentiation and proliferation of bone marrow stromal cells in traumatic femoral head necrosis. Eur Rev Med Pharmacol Sci. 2020;24:11465.
Hamam D, Ali D, Vishnubalaji R, et al. microRNA-320/RUNX2 axis regulates adipocytic differentiation of human mesenchymal (skeletal) stem cells. Cell Death Dis. 2014;5:e1499.
Plonska-Brzezinska ME. Carbon nanomaterials: perspective of their applications in biomedicine. Curr Med Chem. 2019;26:6832–3.
Furtado D, Björnmalm M, Ayton S, Bush A, Kempe K, Caruso F. Overcoming the blood-brain barrier: the role of nanomaterials in treating neurological diseases. Adv Mater. 2018;30:e1801362.
Rehman A, Jafari SM, Tong Q, et al. Drug nanodelivery systems based on natural polysaccharides against different diseases. Adv Colloid Interface Sci. 2020;284:102251.
Muller M, Vehlow D, Torger B, Urban B, Woltmann B, Hempel U. Adhesive drug delivery systems based on polyelectrolyte complex nanoparticles (PEC NP) for bone healing. Curr Pharm Design. 2018;24:1341–8.
Lei L, Liu Z, Yuan P, Jin R, Wang X, Jiang T, et al. Injectable colloidal hydrogel with mesoporous silica nanoparticles for sustained co-release of microRNA-222 and aspirin to achieve innervated bone regeneration in rat mandibular defects. J Mater Chem B. 2019;7:2722–35.
Wang L, Liu S, Ren C, Xiang S, Li D, Hao X, et al. Construction of hollow polydopamine nanoparticle based drug sustainable release system and its application in bone regeneration. Int J Oral Sci. 2021;13:27.
Kamaly N, Yameen B, Wu J, Farokhzad OC. Degradable controlled-release polymers and polymeric nanoparticles: mechanisms of controlling drug release. Chem Rev. 2016;116:2602–63.
Loira-Pastoriza C, Todoroff J, Vanbever R. Delivery strategies for sustained drug release in the lungs. Adv Drug Deliv Rev. 2014;75:81–91.
Ding D, Zhu Q. Recent advances of PLGA micro/nanoparticles for the delivery of biomacromolecular therapeutics. Mater Sci Eng C Mater Biol Appl. 2018;92:1041–60.
D’Souza AA, Shegokar R. Polyethylene glycol (PEG): a versatile polymer for pharmaceutical applications. Expert Opin Drug Deliv. 2016;13:1257–75.
Urello MA, Xiang L, Colombo R, Ma A, Joseph A, Boyd J, et al. Metabolite-based modification of Poly(l-lysine) for improved gene delivery. Biomacromolecules. 2020;21:3596–607.
Mitchell MJ, Billingsley MM, Haley RM, Wechsler ME, Peppas NA, Langer R. Engineering precision nanoparticles for drug delivery. Nat Rev Drug Discov. 2021;20:101–24.
Iturrioz-Rodríguez N, Correa-Duarte MA, Fanarraga ML. Controlled drug delivery systems for cancer based on mesoporous silica nanoparticles. Int J Nanomedicine.. 2019;14:3389–401.
Cherkasov VR, Mochalova EN, Babenyshev AV, Rozenberg JM, Sokolov IL, Nikitin MP. Antibody-directed metal-organic framework nanoparticles for targeted drug delivery. Acta Biomater. 2020;103:223–36.
Zhu X, Li J, Peng P, Hosseini Nassab N, Smith BR. Quantitative drug release monitoring in tumors of living subjects by magnetic particle imaging nanocomposite. Nano Lett. 2019;19:6725–33.
Zhao H, Wang YL, Peng JR, Zhang L, Qu Y, Chu BY, et al. Biodegradable Self-assembled micelles based on MPEG-PTMC copolymers: an ideal drug delivery system for vincristine. J Biomed Nanotechno. 2017;13:427–36.
Nel A, Xia T, Mädler L, Li N. Toxic potential of materials at the nanolevel. Science. 2006;311:622–7.
Zor F, Selek FN, Orlando G, Williams DF. Biocompatibility in regenerative nanomedicine. Nanomedicine (Lond). 2019;14:2763–75.
Naili S, van Rietbergen B, Sansalone V, Taylor D. Bone remodeling. J Mech Behav Biomed Materials. 2011;4:827–8.
García-Gareta E, Coathup MJ, Blunn GW. Osteoinduction of bone grafting materials for bone repair and regeneration. Bone. 2015;81:112–21.
Gage J, Liporace A, Egol A, McLaurin M. Management of bone defects in orthopedic trauma. Bull Hosp Jt Disease. 2013;2018:4–8.
Maruyama M, Rhee C, Utsunomiya T, Zhang N, Ueno M, Yao Z, et al. Modulation of the inflammatory response and bone healing. Front Endocrinol (Lausanne). 2020;11:386.
Zhang L, Tang Y, Zhu X, Tu T, Sui L, Han Q, et al. Overexpression of MiR-335-5p promotes bone formation and regeneration in mice. J Bone Miner Res. 2017;32:2466–75.
Komori T. Regulation of proliferation, differentiation and functions of osteoblasts by Runx2. Int J Mol Sci. 2019;20:1694.
Ching HS, Luddin N, Rahman IA, Ponnuraj KT. Expression of odontogenic and osteogenic markers in DPSCs and SHED: a review. Curr Stem Cell Res Therapy. 2017;12:71–9.
Kim JM, Lin C, Stavre Z, Greenblatt MB, Shim JH. Osteoblast-osteoclast communication and bone homeostasis. Cells. 2020;9:2073.
Maes C, Kobayashi T, Selig MK, Torrekens S, Roth SI, Mackem S, et al. Osteoblast precursors, but not mature osteoblasts, move into developing and fractured bones along with invading blood vessels. Dev Cell. 2010;19:329–44.
Acknowledgements
This work was supported by National Science Foundation of China (Grant Number 81774348 and 81874477); and Science and Technology Project of Henan Province (Grant number 212102310365).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical statement
All the experimental operations for rabbits was fully in accordance with the Guide for the Care and Use of Laboratory Animals, and this study was approved by the Henan Provincial Hospital orthopaedic ethics committee of Luoyang Orthopaedic Hospital Hospital (Approval no. 2014ZY02094).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, Y., Li, C., Wei, Q. et al. MiRNA320a Inhibitor-Loaded PLGA-PLL-PEG Nanoparticles Contribute to Bone Regeneration in Trauma-Induced Osteonecrosis Model of the Femoral Head. Tissue Eng Regen Med 21, 185–197 (2024). https://doi.org/10.1007/s13770-023-00580-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13770-023-00580-7