Abstract
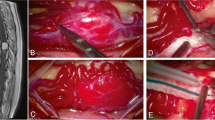
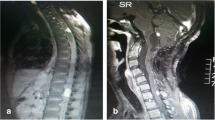
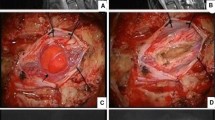
Purpose: total removal of spinal hemangioblastomas with satisfactory clinical outcomes remains a challenge. We aimed to evaluate the surgical outcomes of our spinal hemangioblastomas patients, summarize our experiences with this condition and review-related literature. Methods: records of 18 spinal hemangioblastoma patients who underwent microsurgical resection were analyzed retrospectively. Clinical features, surgical procedures and outcomes were reviewed to assess the prognosis of their spinal hemangioblastomas. The McCormick classification method was used to evaluate spinal function and MR scans used to assess location and features of the tumor pre-surgically, tumor recurrence and syringomyelia status post-surgically. Results: total resection of 37 tumors was achieved in all 18 cases. Of those patients, two (11%) were accompanied with von Hippel-Lindau (VHL). Of the 37 tumors, 3 (8.1%) were completely intramedullary, 16 (43.2%) intramedullary–extramedullary and 18 (48.6%) primarily extramedullary. Tumors accompanied with syringomyelia were present in 17 (94.4%) patients. Clinical symptoms such as pain were reduced within 48 h after surgery in 16 patients. Post-operative neurological functions improved in all cases at 3 months post-surgery. Over the subsequent 3–18 month follow-up period, pre-operative symptoms improved in all 18 patients and no tumor recurrence was present. Syringomyelia was reduced or absent within 3–6 months. Conclusions: our results indicated that a complete microscopic resection was effective in eliminating symptoms in these spinal hemangioblastoma patients, who showed a good prognosis after surgery. These improvements in clinical symptoms may be associated with the blood flow changes, but not with reductions and/or eliminations of syrinx after surgery.




Similar content being viewed by others
References
Mandigo CE, Ogden AT, Angevine PD, McCormick PC (2009) Operative management of spinal hemangioblastoma. Neurosurgery 65(6):1166–1177. https://doi.org/10.1227/01.NEU.0000359306.74674.C4
Conway JE, Chou D, Clatterbuck RE, Brem H, Long DM, Rigamonti D (2001) Hemangioblastomas of the central nervous system in von Hippel-Lindau syndrome and sporadic disease. Neurosurgery 48(1):55–62 (discussion 62–53)
Pietila TA, Stendel R, Schilling A, Krznaric I, Brock M (2000) Surgical treatment of spinal hemangioblastomas. Acta Neurochir (Wien) 142(8):879–886
Pan J, Jabarkheel R, Huang Y, Ho A, Chang SD (2018) Stereotactic radiosurgery for central nervous system hemangioblastoma: systematic review and meta-analysis. J Neurooncol 137(1):11–22. https://doi.org/10.1007/s11060-017-2697-0
Deng X, Wang K, Wu L, Yang C, Yang T, Zhao L, Yang J, Wang G, Fang J, Xu Y (2014) Intraspinal hemangioblastomas: analysis of 92 cases in a single institution: clinical article. J Neurosurg Spine 21(2):260–269. https://doi.org/10.3171/2014.1.SPINE13866
Dwarakanath S, Sharma BS, Mahapatra AK (2008) Intraspinal hemangioblastoma: analysis of 22 cases. J Clin Neurosci 15(12):1366–1369. https://doi.org/10.1016/j.jocn.2007.04.014
Lonser RR, Glenn GM, Walther M, Chew EY, Libutti SK, Linehan WM, Oldfield EH (2003) von Hippel-Lindau disease. Lancet 361(9374):2059–2067. https://doi.org/10.1016/S0140-6736(03)13643-4
Rebner M, Gebarski SS (1985) Magnetic resonance imaging of spinal-cord hemangioblastoma. AJNR Am J Neuroradiol 6(2):287–289
McCormick PC, Post KD, Stein BM (1990) Intradural extramedullary tumors in adults. Neurosurg Clin N Am 1(3):591–608
Lonser RR, Weil RJ, Wanebo JE, DeVroom HL, Oldfield EH (2003) Surgical management of spinal cord hemangioblastomas in patients with von Hippel-Lindau disease. J Neurosurg 98(1):106–116. https://doi.org/10.3171/jns.2003.98.1.0106
Na JH, Kim HS, Eoh W, Kim JH, Kim JS, Kim ES (2007) Spinal cord hemangioblastoma : diagnosis and clinical outcome after surgical treatment. J Korean Neurosurg Soc 42(6):436–440. https://doi.org/10.3340/jkns.2007.42.6.436
Siller S, Szelenyi A, Herlitz L, Tonn JC, Zausinger S (2017) Spinal cord hemangioblastomas: significance of intraoperative neurophysiological monitoring for resection and long-term outcome. J Neurosurg Spine 26(4):483–493. https://doi.org/10.3171/2016.8.SPINE16595
Park DM, Zhuang Z, Chen L, Szerlip N, Maric I, Li J, Sohn T, Kim SH, Lubensky IA, Vortmeyer AO, Rodgers GP, Oldfield EH, Lonser RR (2007) von Hippel-Lindau disease-associated hemangioblastomas are derived from embryologic multipotent cells. PLoS Med 4(2):e60. https://doi.org/10.1371/journal.pmed.0040060
Vortmeyer AO, Frank S, Jeong SY, Yuan K, Ikejiri B, Lee YS, Bhowmick D, Lonser RR, Smith R, Rodgers G, Oldfield EH, Zhuang Z (2003) Developmental arrest of angioblastic lineage initiates tumorigenesis in von Hippel-Lindau disease. Cancer Res 63(21):7051–7055
Ang SO, Chen H, Gordeuk VR, Sergueeva AI, Polyakova LA, Miasnikova GY, Kralovics R, Stockton DW, Prchal JT (2002) Endemic polycythemia in Russia: mutation in the VHL gene. Blood Cells Mol Dis 28(1):57–62
Bostrom A, Hans FJ, Reinacher PC, Krings T, Burgel U, Gilsbach JM, Reinges MH (2008) Intramedullary hemangioblastomas: timing of surgery, microsurgical technique and follow-up in 23 patients. Eur Spine J 17(6):882–886. https://doi.org/10.1007/s00586-008-0658-1
Ammerman JM, Lonser RR, Dambrosia J, Butman JA, Oldfield EH (2006) Long-term natural history of hemangioblastomas in patients with von Hippel-Lindau disease: implications for treatment. J Neurosurg 105(2):248–255. https://doi.org/10.3171/jns.2006.105.2.248
Imagama S, Ito Z, Wakao N, Sakai Y, Kato F, Yukawa Y, Sato K, Ando K, Hirano K, Tauchi R, Muramoto A, Hashizume Y, Matsuyama Y, Ishiguro N (2011) Differentiation of localization of spinal hemangioblastomas based on imaging and pathological findings. Eur Spine J 20(8):1377–1384. https://doi.org/10.1007/s00586-011-1814-6
Hayashi N, Matsumae M, Yatsushiro S, Hirayama A, Abdullah A, Kuroda K (2015) Quantitative analysis of cerebrospinal fluid pressure gradients in healthy volunteers and patients with normal pressure hydrocephalus. Neurol Med Chir (Tokyo) 55(8):657–662. https://doi.org/10.2176/nmc.oa.2014-0339
Mitha AP, Turner JD, Abla AA, Vishteh AG, Spetzler RF (2011) Outcomes following resection of intramedullary spinal cord cavernous malformations: a 25-year experience. J Neurosurg Spine 14(5):605–611. https://doi.org/10.3171/2011.1.SPINE10454
Glasker S, Klingler JH, Muller K, Wurtenberger C, Hader C, Zentner J, Neumann HP, Velthoven VV (2010) Essentials and pitfalls in the treatment of CNS hemangioblastomas and von Hippel-Lindau disease. Cent Eur Neurosurg 71(2):80–87. https://doi.org/10.1055/s-0029-1234040
Kim TY, Yoon DH, Shin HC, Kim KN, Yi S, Oh JK, Ha Y (2012) Spinal cord hemangioblastomas in von hippel-lindau disease: management of asymptomatic and symptomatic tumors. Yonsei Med J 53(6):1073–1080. https://doi.org/10.3349/ymj.2012.53.6.1073
Lonser RR (2014) Surgical management of sporadic spinal cord hemangioblastomas. World Neurosurg 82(5):632–633. https://doi.org/10.1016/j.wneu.2014.08.026
Bamps S, Calenbergh FV, Vleeschouwer SD, Loon JV, Sciot R, Legius E, Goffin J (2013) What the neurosurgeon should know about hemangioblastoma, both sporadic and in Von Hippel-Lindau disease: a literature review. Surg Neurol Int 4:145. https://doi.org/10.4103/2152-7806.121110
Ampie L, Choy W, Khanna R, Smith ZA, Dahdaleh NS, Parsa AT, Bloch O (2016) Role of preoperative embolization for intradural spinal hemangioblastomas. J Clin Neurosci 24:83–87. https://doi.org/10.1016/j.jocn.2015.09.006
Lonser RR, Butman JA, Huntoon K, Asthagiri AR, Wu T, Bakhtian KD, Chew EY, Zhuang Z, Linehan WM, Oldfield EH (2014) Prospective natural history study of central nervous system hemangioblastomas in von Hippel-Lindau disease. J Neurosurg 120(5):1055–1062. https://doi.org/10.3171/2014.1.JNS131431
Feletti A, Anglani M, Scarpa B, Schiavi F, Boaretto F, Zovato S, Taschin E, Gardi M, Zanoletti E, Piermarocchi S, Murgia A, Pavesi G, Opocher G (2016) Von Hippel-Lindau disease: an evaluation of natural history and functional disability. Neuro Oncol 18(7):1011–1020. https://doi.org/10.1093/neuonc/nov313
Funding
This study was supported by National Science Foundation of Tianjin City, China, to Dr. Yang Nan (Grant No. 18JCZDJC98600) and Health and Family Planning Commission in Binhai New District of Tianjin City, China to Dr. Yang Nan (Grant No. 2018BWKZ003).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, H., Zhang, L., Wang, H. et al. Spinal hemangioblastoma: surgical procedures, outcomes and review of the literature. Acta Neurol Belg 121, 973–981 (2021). https://doi.org/10.1007/s13760-020-01420-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13760-020-01420-4