Abstract
Purpose of Review
This review broadly discusses the consequences of inadequate consumption, by deficit or excess, of selected micronutrients on the quality of life and morbidity during aging, specifically considering increases in life expectancy and the costs of care in the older persons.
Recent Findings
A literature review of the periods 2012 to 2018, focusing on vitamins A, B12, and D, calcium, iron and folate, was completed as these micronutrients are found to significantly affect the aging process. Causation and application of these micronutrients to disorders related to aging are controversial and mixed. This review highlights research needs and controversial points on the role of these micronutrients.
Summary
Micronutrient deficiencies are a common and avoidable contributor to decreased quality of life and healthcare costs in the older persons. Further research is needed to determine adequate intakes and innovative uses, including appropriate thresholds for improved health outcomes for this population.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Purpose
The United Nations World Population Prospects projects the number of persons aged 80 years + will triple from 137 million in 2017 to 425 million in 2050 [1]. The prevalence of chronic diseases, such as cancer, cardiovascular, and neurodegenerative diseases, is anticipated to rise along with this elderly population [2].
Nutrition contributes to overall health and improves treatment response for chronic diseases (i.e., immune response, mobility, cognitive function, healing) [2, 3]. A compromised health status can increase hospital length of stay and promote the development of comorbidities, contributing to additional costs of $13,350–$19,530 per hospitalization and $77,000 per year of care associated with poor nutrition status [4].
Aging is associated with an overall decline in physiological functions that contribute to inadequate nutritional status (i.e., decreased metabolic rate and gastric secretions, decreased sensory functions in oral cavity, increased use of medications, changes in overall body mass and electrolyte distribution) [2,3,4,5]. The cumulative effects of aging and micronutrient deficiencies in the older persons result in frailty, cognitive decline, poor immune response, cardiovascular disease, cancer, and other factors of morbidity [2, 6, 7]. On the other hand, the widespread use of dietary supplements (52% of adults in the USA report the use of at least one supplement product) has been reported to be of no benefit for some nutrients and could have deleterious consequences in this age group [8,9,10,11].
The purpose of this review is to update knowledge and briefly discuss the role and new findings of vitamins A, B12, and D, calcium, iron, and folate on morbidity and quality of life during aging, especially considering the increased life expectancy and the costs of care of this age group.
Approach
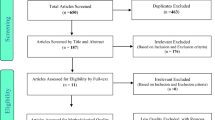
A literature review of the periods 2012 to 2018 in older people aged 65+ years, focusing on vitamin A, vitamin B12, vitamin D, calcium, iron, and folate, was performed in MEDLINE and Google Scholar as these micronutrients are found to significantly affect the aging process [9,10,11]. Although the United Nations agreed cutoff is 60+ years to refer to the older population [12], developed world countries accept the age of 65+ years as the working definition of elderly [13]. Because most published studies have been done in developed nations, 65+ years of age was used for this review. The lists of references from selected articles were also searched.
The review focused on the consequences of inappropriate consumption of some vitamins and minerals—by excess or deficit—on the aging process itself and on the health and wellbeing of this age group, highlighting interactions between nutrients, research needs, and controversial points, when applicable. The risk of excessive intakes of vitamins and minerals is a topic that is getting more and more relevance in recent studies, due to the consequences for health on all age groups. For each nutrient, a brief description on the function and role in aging, the recommended nutrient intakes (RNI) [14], and the tolerable upper intake levels (UL) [15] were included (Table 1).
Findings
Vitamin A
Importance of Vitamin A in Aging
Vitamin A has several important roles in the aging process: mainly immune function and oxidative processes. Deficiency is associated with defective immune response to infection. All-trans retinoic acid (RA), a common form of active vitamin A, plays a role in immune homeostasis through regulating cell homing and differentiation. During times of infection or autoimmune disease, it activates T cell responses [16]. Emerging research is focusing on the effects of vitamin A enhancing T cell responses to cancer, infection, intestinal inflammation, and immune-mediated diseases in humans including autoimmune disease—all associated with aging [16].
Deficiency
Effects of vitamin A deficiency include neurodegeneration, physiological function of steroid and thyroid hormones, and historically, vision and skin changes. All-trans RA has protective effects in neurodegeneration. It diminishes the production of amyloid-β peptides and their oligomerizations in the development of Alzheimer’s disease [17].
-
i.
Vision
Vitamin A roles on vision and skin changes are well studied. The carotenoids lutein and zeaxanthin confer the most benefit to the retina in age-related macular degeneration. However, vitamin A and other carotenoids are inconsistently associated with prevention or improvement in macular degeneration [18].
-
ii.
Skin
Age-related complications and diseases are associated with decreased retinoid signaling and the decline of various hormones, including steroids. RA plays a role in activating RARs and RXRs, steroid thyroid hormone receptor transcription factors. In 2015, it was reported that RA may restore steroidogenesis in epidermal keratinocytes of aged individuals [19]. Additionally, retinol increases epidermal thickness by upregulation of transcription factors, collagen genes responsible for wound healing, improving extracellular matrix microenvironment, extracellular matrix production, and activating dermal fibroblasts [20, 21].
Excess
A recent review reports that only a small percent of the older persons have intakes below the RNI, showing that in fact vitamin A intake in this age group is usually much higher than the RNI [22•]. Vitamin A excess is of special concern in the older persons who may have difficultly clearing it [22•]. Chronic vitamin A excess is associated with loss of hair, dry mucous membranes and skin, cortical bone loss and fractures, and potentially an increased risk of mortality [23, 24]. Vitamin A is a clear example of the importance of maintaining appropriate micronutrient intakes and concentrations avoiding extremes, both high and low.
-
i.
Bone Fractures
Reported health outcomes associated with excess vitamin A include premature skin aging in elderly HIV patients and increased risk of bone fractures [25, 26]. Retinol and carotenoids may support a chemo-preventive phytochemical role in estrogen-dependent cancers, common in post-menopausal women. β-Carotene levels were independently and inversely associated with estradiol levels in older women [27]. Previous reports on associations between vitamin A intake, serum retinol concentrations, and bone mineral density or fracture are controversial. The inconsistencies may be due, in part, to difficulties in obtaining an accurate assessment of vitamin A since it has been reported that serum retinol is a poor proxy for vitamin A status [28, 29].
Interaction Between Nutrients
Vitamin A, a fat-soluble vitamin, is absorbed with vitamin D. Thus, serum retinol should always be assessed in the presence of vitamin D supplementation [23]. New research has found that retinoic acid and vitamin D calcitriol combined influence proliferation and differentiation of osteoblasts [30]. An increase in PPARγ2 expression was observed following retinoic acid administration, whereas a decrease was observed following calcitriol administration [30]. Additionally, cumulative serum retinol and zinc levels among older persons may help in high-frequency hearing loss [31]. Similarly, zinc supplementation in individuals aged 70–85 years increased vitamin A levels proportionately with zinc [32].
Gaps in Research—Further Research
Leukocyte telomere length (LTL) is a biomarker of the aging process. These repetitive sequences of DNA at the ends of chromosomes serve to protect the ends of DNA strands and are associated with risk of chronic disease. High oxidative stress can lead to DNA strand breaks, shortening telomeres. Several serum carotenoids, including β-carotene, β-cryptoxanthin, lutein, and zeaxanthin), were found to be associated with LTL. Vitamin A roles in immune function, inflammation, regulation of gene expression, and epigenetic modification, help maintain LTL [33•]. More research is needed to understand the association between vitamin A, LTL, and the potential use of this association during the aging process.
The potential for exacerbating an already serious public health problem, with intakes of vitamin A currently considered safe, indicates further research into this matter is needed.
Vitamin B12 and Folate
Importance of Vitamin B12 and Folate in Aging
Vitamin B12 and folate are associated with preventing chronic diseases associated with aging through the methylation of homocysteine [34]. This is a vital process preventing amyloid and tau protein accumulation which can cause cognitive decline [34]. The genetic polymorphism in the MTHFR 677TT gene is hypothesized to be a main contributor to metabolism in aging processes [35•]. Elevated homocysteine and lower vitamin B levels impact the immune system, causing increased inflammation and antioxidant damage which catalyze physiological aging in all systems [35•].
Deficiency
Vitamin B12 deficiency can lead to megaloblastic anemia and demyelinating neurological symptoms, including irreversible nerve damage and neuropathy. Older adults are at high risk of vitamin B12 malabsorption due to the lack of production of intrinsic factor [36]. Unfortunately, symptoms are often misdiagnosed because they mimic Alzheimer’s disease and other chronic conditions with non-specific symptoms [2]. Folate deficiency is associated with a poor diet and malabsorptive disorders. It can result in megaloblastic anemia, soreness, and shallow ulcerations in tongue and oral mucosa, and changes in hair, skin, and fingernails [37•].
-
i.
Cognitive Decline
Vitamin B12 and folate have a strong protective effect in mental health decline in the older persons [38]. Decreased dietary vitamin B12, folate, and vitamin B6 was shown to precede depression in this age group; while vitamin B12 was found to have protective effects against depression [39, 40].
Folate and vitamin B12 deficiencies result in increased total homocysteine levels associated with faster rates of total brain volume loss and cause severe neurocognitive decline [41, 42]. One study found high vitamin B12 levels were associated with a decreased rate of total brain volume loss, while folate levels were not [43]. On the other hand, other studies show that vitamin B12 was not associated with dementia and cognitive decline compared to folate. A large longitudinal study of elderly patients at risk of dementia found that higher dietary folate intake was associated with a decreased risk of dementia [44]. Another study found folate supplementation of 800 μg/day positively affected cognitive decline through significantly improving memory, sensorimotor speed, and information processing [34]. A study in 2016 reported that increases in folate intake in older persons worsened clinical outcomes in peripheral neuropathy associated with vitamin B12 deficiency [36].
-
ii.
Cardiovascular Disease
In older persons, high serum homocysteine and folate along with low vitamin B12 concentrations have been reported to increase the risk of cardiovascular disease (CVD) showing that there was strong evidence connecting stroke and heart disease with folic acid levels, treatment, and supplementation [35•]. Low vitamin B12 levels were found to increase blood pressure, contributing to CVD. In addition, decreases in vitamin B12 concentrations can result in hyperhomocysteinemia, which could quadruplicate elderly patients’ risk of stroke due to atrial fibrillation [45].
-
iii.
Bone Health
Folate and vitamin B12 have also been associated with bone health. Interestingly, elevated levels of homocysteine have been associated with fracture risk and bone mineral density (BMD) [35•]. Studies have found the MTHFR 677 polymorphism to be associated with a 23% increased risk of all fractures through changes in BMD. However, intervention studies using folate and vitamin B12 have reported no significant associations, suggesting that B vitamin interventions may be confined to at-risk groups with sub-optimal vitamin B12 and folate levels [35•].
Excess
There are no known adverse effects of large intakes of vitamin B12; rather, deficiency is of utmost concern [46]. A more pressing problem in regard to the older persons is excessive folate intake. In the USA, those 50 years and older have the highest folate intake and may be at risk of excessive folate intake due to supplementation and fortified foods [47]. Higher levels of folate have historically been seen to worsen anemia and cognition while masking low levels of vitamin B12. Another major concern in excess folate is its controversial and complex dual role in colorectal cancer. While some studies have found folate to be protective in risk of colorectal cancer, other studies have found folate supplementation to be potentially cancer-promoting [48]. Thus, the optimal intake for those over 65 years is unknown.
Interaction Between Nutrients
As the older persons have increased consumption of gastric acid inhibitors, they are at increased risk of vitamin B12 deficiency due to the lack of vitamin B12 absorption. Calcium supplementation has been found to positively affect the association between gastric acid inhibitors and vitamin B12 deficiency [49].
Gaps in Research—Further Research
It is still unknown to what extent B vitamins involved in one-carbon metabolism can affect DNA methylation throughout the life cycle. Some studies have found that long-term supplementation with folic acid and vitamin B12 in elderly subjects resulted in effects on DNA methylation of several genes, including those implicated in developmental processes. Furthermore, more research is needed on the effect of both folate and B12 on cognitive function, CVD, and bone health as they relate to aging. Public health conclusions in regard to folate and vitamin B12 point to fortification of foods, but safe upper level intake of folic acid and its interaction with vitamin B12 needs to be further researched. This is especially urgent in regard to the potentially positive role excess folate contributes to promoting colorectal cancer.
Iron
Importance in Aging
Iron is an essential functional component of vital metabolic functions such as oxygen transport, oxidative energy production, inactivation of harmful oxygen radicals, and DNA synthesis. It has a nutrigenomic effect in the central nervous system as a cofactor for oxidative phosphorylation, neurotransmitter production, nitric oxide metabolism, and oxygen transport, playing an important role in neuroprotection and neuronal activities [50].
Studies reveal iron is essential to maintain immune and antioxidant function during aging [51]. Iron status becomes impaired in situations that involve chronic inflammation, such as obesity or aging [50, 52] and malnutrition exacerbates these effects of inflammation [53•]. Inflammation affects hepcidin, a peptide hormone that regulates iron homeostasis [53•].
Anemia and iron deficiency are two of the most prevalent disorders worldwide, affecting people in all regions and ages, including older persons. Iron overload, although usually associated to pathological conditions, also has important consequences on health and could be of relevance during aging [54].
Deficiency
Post-menopausal women and older men are at an increased risk of iron deficiency because of chronic blood loss from disease conditions, decreased absorption due to reduced acid secretion, use of medications such as antacids, or a diet low in iron [2, 48]. The current RNI and UL for iron (Table 1) are controversial because of the effect that age, gender, race, and ethnicity could have on the level and functionality of iron [52].
-
i.
Anemia and Depression
The most common form of nutritional anemia, iron deficiency anemia, is associated with impaired cognitive performance, depressive symptoms, reduced quality of life, and increased hospitalization and mortality in the older persons [53•, 55, 56]. According to the World Health Organization definition of anemia, over 10% of community-dwelling adult aged ≥ 65 are classified as anemic [57, 58]. The prevalence of anemia increases significantly with advancing age and exceeds 20% in those aged 85+ years [55]. A NHANES study from 2004 found that out of those diagnosed with anemia, only one third had nutritional deficiency, primarily of iron [59].
Depressive symptoms were significantly higher in a cross-sectional study of 1875 elderly men and women across England with low iron status (low Hb and high sTfR) [60]. However, chronic illness decreased the association and depressive symptoms were not associated with ferritin, suggesting anemia of chronic disease and not necessarily an iron intake problem [53•].
Excess
Iron-overloaded states, especially hemochromatosis, a disease resulting in excess levels of iron in the liver, results in increased iron-induced cell damage, fibrosis, cirrhosis, and hepatocellular cancer [54]. Those with iron overload are also at increased risk of infection. Pathogens also benefit for administered iron, causing caution with iron supplementation, which promotes health in iron deficiency, but require previous treatment of any ongoing infection [61].
-
i.
Cardiovascular Disease
Increased tissue iron stores have been associated with increased risk of a number of chronic diseases, including heart disease, diabetes mellitus, and potentially cancer in middle-aged and older populations [53•]. Positive associations have been found between ferritin, low serum iron, and cardiovascular disease markers in elderly population [53•, 62, 63]. However, causality could not be indicated because of similar concerns of biomarkers used and the discrepancies between inflammation and iron serum levels.
-
ii.
Neurodegenerative Disorders
During aging, iron accumulates in different brain regions associated with motor and cognitive impairments. The link between inflammation and iron is complex, but inflammatory mediators (such as tumor necrosis factor alpha, interleukin-6, and ferroportin-1) stimulate hepcidin, thereby upregulating iron deposition in the brain. This disruption in homeostasis has been seen on magnetic resonance imaging, a potential diagnostic biomarker of neurodegenerative disorders [64], although there has not been clear proof of a causal relationship. The associated oxidative damage from brain iron accumulation could be responsible for pathogenesis of dementia [61]. More studies are needed to see if iron-induced oxidation contributes to Alzheimer’s disease and Parkinson’s disease.
-
iii.
Iron-Overload, Cancer, and Infection
Because iron interacts with DNA at a genomic level, high iron levels could be involved with specific cancer growth and angiogenesis [65, 66]. Iron is pro-inflammatory and promotes oxidative damage. Its carcinogenicity has been initially researched in animal studies [67]. However, a broad review by the Scientific Advisory Committee on Nutrition found insufficient data regarding a true link between iron and colorectal cancer [68].
Interaction Between Nutrients
Vitamin C might increase the absorption of dietary iron by up to 10% and calcium decreases iron absorption. Therefore, if both are needed, it is advised to take iron and calcium hours apart [69, 70]. Additionally, if taken without food, large doses of iron supplements impair the absorption of zinc [50].
Gaps in Research—Further Research
The diagnosis of iron deficiency anemia is highly controversial. Based on the differences in iron absorption and chronic inflammation, as well as the prevalence of comorbidities, the diagnosis of iron deficiency and iron excess in the older persons needs specific review. It may also be appropriate for future diagnosis standards of iron deficiency to be based on differences in iron absorption, age, gender, and race.
Vitamin D and Calcium
Importance of Vitamin in Aging
Vitamin D intake and absorption drastically decreases with age due to decreased sunlight exposure, nutrient intake, fat absorption, and conversion of vitamin D to its active form [2]. In regard to aging, vitamin D is associated with cognition, depression, cancer, and cardiovascular disease [10, 24, 71]. Vitamin D stimulates clearance and phagocytosis by macrophages, protecting immune cells against apoptosis by regulating both extranuclear protein functions and gene expression signaling [72].
Calcium and vitamin D interact to effect vasculature, lipid metabolism, and neuromodulation. Strongly influenced by age, the efficiency of calcium absorption from the gastrointestinal tract decreases significantly after age 60 in both sexes: with those aged 70 years and older absorbing approximately one-third less calcium than do younger adults. Women are at an even greater risk of decreased calcium because of a decreased fractional calcium absorption after menopause, estrogens acceleration on bone loss, and increased urinary calcium losses [73, 74].
Deficiencies
In 2013, 40–100% of elder populations globally were below the WHO standard of vitamin D sufficiency (< 50 nmol/L) [11, 75, 76]. Yet, some groups have found changes in cognition at significantly lower thresholds (< 10 ng/mL) [72]. Inadequate vitamin D and calcium has been linked with many conditions and symptoms. In a recent systematic review of micronutrient intakes in older persons, nearly 65% of the population of men and 73% of the women studied were at risk of inadequate intakes of calcium based on the RNIs in Table 1 [77•].
-
i.
Falls and Fracture Risk
Fracture risk, bone loss, and the resulting osteoporotic fractures are the predominant bone health concern for those over 70 years of age. Vitamin D and calcium, alongside of exercise, are well-known preventive measures for preventing bone loss in the older persons [73, 78].
Current data revels the beneficial effect of vitamin D supplementation on muscle strength, physical performance, and prevention of falls and fractures in elderly female populations [79]. While lower 25-[OH]D levels in institutionalized older persons were associated with hip fractures, falls alone were hardly associated to vitamin D status [80]. Interestingly, elevated parathyroid hormone (PTH) was inversely correlated with vitamin D status and was the only predictor of hip fractures [81]. Additionally, accumulating evidence suggests vitamin D deficiency is associated with sarcopenia in elderly women [82].
Overall, there is good evidence (a review of 17 RCTs) that vitamin D (doses < 800 IU) plus calcium (500 mg) results in small increases in bone mineral density (of the spine, total body, femoral neck, and total hip). However, it is less certain if vitamin D alone improves bone density. Calcium supplementation alone was not significantly different than the combination of vitamin D plus calcium, suggesting that calcium alone may help replete bone mineral density [83•].
-
ii.
Cognition
The existing body of evidence provides proof that people with 25-[OH]D concentrations < 10 ng/mL have the greater risk of cognitive disorders [84]. However, vitamin D’s role in cognitive decline remains unclear.
Previously, low vitamin D concentrations have been associated with worse cognitive performance and cognitive decline than persons with adequate levels. However, several vitamin D supplementation studies in large elderly cohorts showed no significant improvement in cognition compared with controls [85,86,87]. There is a need for more studies on true association of vitamin D and calcium on cognition in elderly adults, a clear definition of cognition, and appropriate thresholds for vitamin impacts on cognition.
Excess
Vitamin D excess is measured through hypercalciuria and hypercalcemia (25(OH)D) levels above 88 ng/mL). Serious consequences of vitamin D overuse are acute kidney injury and pancreatitis, secondary to hypercalcemia. The increase in supplementation has been a cause for concern due to the inconsistencies in safe vitamin level intake [11, 73, 88]. The thresholds of vitamin D are widely debated [77•]. In 2010, more than 50% of older men and almost 70% of older women in the USA were taking supplemental calcium [89]. Non-skeletal effects of calcium, especially potential adverse effects on cardiovascular health, are not well established and remain controversial. Over-supplementation still needs to be studied for both of these vitamins as adverse effects are unknown and current supplementation to prevent poor health outcomes.
-
i.
Cardiovascular Disease and Mortality
Following inconclusive results of vitamin D reduction of cardiovascular disease and all-cause mortality, a recent review of vitamin D found that higher levels of vitamin D had inverse association with mortality probably through an effect of vitamin D on lipid status [71, 83•]. A study on excess dietary calcium intake was associated with higher Framingham Risk Score (FRS), a proxy measure of cardiovascular health. This study suggests that excess (> 1200 mg/day) as well as very low (< 300 mg/day) dietary calcium intakes is related to higher FRS in both genders [90]. However, two comprehensive reviews including over 87 clinical trials, 100 literature reviews, and 200 primary articles could not support claims on the combined effect of vitamin D and calcium on cardiovascular health or all-cause mortality [83•, 91•].
Interactions Between Nutrients
Vitamin D forms the basis of calcium’s homeostatic mechanism. Calcium and vitamin D interact through regulated feedback and are dependent on each other for maintenance of appropriate levels. Vitamin D insufficiency may result in a relative hypocalcemia and high serum PTH concentrations, which alone has been linked to poor health outcomes [73]. This secondary hyperparathyroidism can be attenuated by the administration of vitamin D supplements. Calcium can compete or interfere with the absorption of iron, zinc, and magnesium [92] and must be addressed if older persons are at risk of these deficiencies.
Gaps in Research—Further Research
Due to vitamin D’s unique activation processes (requiring sun exposure), accurate levels of RNI are hard to discern and are widely debated [73]. Those that are institutionalized, homebound, have limited sun exposure, dark skin, or malabsorption are at increased risk for vitamin D deficiency and recommended to consume more with a goal of achieving levels of ≥ 30 ng/mL [93]. A cohesive definition of vitamin D insufficiency must be addressed. Vitamin D thresholds for deficiency and excess need to be reviewed for all age groups, since the signs and symptoms of deficiency are not always related to the current cutoff points.
Most research relating calcium and aging has been in conjunction with vitamin D. Yet, according to recent findings, calcium may be a critical nutrient in neurocognitive protection and bone health. Recent reviews have not found a clear link between many of the recommended intake levels of vitamin D or calcium with improvements in health outcomes and more research is needed to determine accurate thresholds for the elderly. Additionally, more robust research is needed to determine causation of vitamin D on health outcomes and dose-dependent effects of both vitamin D and calcium on bone health [9, 71, 82].
Limitations/Implications
This review did not include all micronutrients contributing to the aging process and health outcomes in the elderly (i.e., thiamin, riboflavin, magnesium, selenium, zinc, or vitamin C) which will be important for further reviews as current evidence reveals inadequate intakes in the elderly population and consequential harm [77•].
Overall, there are insufficient studies on the elderly age group and on different outcomes by gender. Within the older persons, studies must sub-classify and subgroup cohorts. For example, a recent systematic review on all health outcomes associated with vitamin D contained very limited information on individuals older than 70 years. It would be interesting to consider subgrouping ages in the old people group, especially for some nutrients and functions that are not necessarily the same for 70- or 80-year-old individuals.
Due to the brevity of this review, details and limitations of each review presented were not mentioned. Populations studied, sample size, and overlapping age ranges may not be generalizable to all elderly. In addition, the detail we were able to provide on each study was limited.
Final Comments
As the use of supplements increases and prevention is emphasized, the application of these micronutrients should be adequately studied for safe treatment recommendations in the elderly population. Low dietary intakes and all micronutrient deficiencies mentioned in this review are associated with functional decline, decreased quality of life, and increased healthcare costs. However, over supplementation is also dangerous and more studies on the subclinical effects and interactions with other nutrients are needed.
Seeking to understand the definitive thresholds of the different vitamins and minerals on their association with health outcomes, both in deficiencies (such as vitamin D) and excess (such as vitamin A and calcium), is important for setting clinical guidelines and policies. There is a need for more robust and focused research to determine micronutrient effects and application to medical conditions related to aging, such as neurocognitive disorders, cardiovascular disease, and cancer.
Finally, it is difficult to assess the value of nutrition interventions since most clinical trials do not assess the costs acquired from morbidity and mortality secondary to malnutrition. More studies are needed to determine the link of nutritional deficiencies with hospital length of stay, preventable healthcare use, and costs.
Conclusion
A literature review of the periods 2012 to 2017, focusing on vitamin A, vitamin B12, vitamin D, calcium, iron, and folate, was completed and these micronutrients are found to significantly affect the aging process. Micronutrient inadequacies are a common and avoidable contributor to decreased quality of life in the elderly. Further research is needed to determine adequate intakes, including appropriate thresholds for health outcomes and safety from over supplementation for this population.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
United Nations. World population prospects: the 2015 revision, key findings and advance tables. New York: United Nations, Department of Economic and Social Affairs. Population Division; 2015.
Watson R. Handbook of nutrition in the aged, third edition modern nutrition. Edited by Ronald R. Watson CRC Press LLC; 2001. 384 p.
Aunan JR, Cho WC, Søreide K. The biology of aging and cancer: a brief overview of shared and divergent molecular hallmarks. Aging Dis. 2017;8(5):628–42. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5614326/
Cangelosi MJ, Rodday AM, Saunders T, Cohen JT. Evaluation of the economic burden of diseases associated with poor nutrition status. JPEN J Parenter Enteral Nutr. 2014;38(2 Suppl):35S–41S.
Brownie S. Why are elderly individuals at risk of nutritional deficiency? Int J Nurs Pract. 2006;12(2):110–8. Available from: http://onlinelibrary.wiley.com/doi/10.1111/j.1440-172X.2006.00557.x/abstract
Knight JA. The biochemistry of aging. In: Advances in clinical chemistry: Elsevier; 2001. p. 1–62. Available from: http://www.sciencedirect.com/science/article/pii/S006524230135014X.
Crogan NL. Nutritional problems affecting older adults. Nurs Clin North Am. 2017;52(3):433–45. Available from: http://www.sciencedirect.com/science/article/pii/S0029646517300567
Rautiainen S, Manson JE, Lichtenstein AH, Sesso HD. Dietary supplements and disease prevention—a global overview. Nat Rev Endocrinol. 2016;12(7):407–20.
Moyer VA, U.S. Preventive Services Task Force. Vitamin, mineral, and multivitamin supplements for the primary prevention of cardiovascular disease and cancer: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med. 2014;160(8):558–64.
Fortmann SP, Burda BU, Senger CA, Lin JS, Whitlock EP. Vitamin and mineral supplements in the primary prevention of cardiovascular disease and cancer: an updated systematic evidence review for the U.S. Preventive Services Task Force. Ann Intern Med. 2013;159(12):824–34.
Kantor ED, Rehm CD, Du M, White E, Giovannucci EL. Trends in dietary supplement use among US adults from 1999–2012. JAMA. 2016;316(14):1464–74.
WHO. Proposed working definition of an older person in Africa for the MDS Project. WHO Health statistics and information systems. 2002 [cited 2018 Mar 15]. Available from: http://www.who.int/healthinfo/survey/ageingdefnolder/en/.
Orimo H, Ito H, Suzuki T, Araki A, Hosoi T, Sawabe M. Reviewing the definition of “elderly”. Geriatr Gerontol Int. 2006;6:149–58. [cited 2018 Mar 19]. Available from: https://onlinelibrary.wiley.com/doi/abs/10.1111/abstract
WHO/FAO. Vitamin and mineral requirements in human nutrition: report of a joint FAO/WHO expert consultation. Bangkok, Thailand 21–30 September 1998. WHO Library Cataloguing-in-Publication Data;2005. 362p.
IOM. Dietary reference intakes: applications in dietary assessment. Washington, DC: The National Academies Press; 2000. [cited 2018 Feb 9]. Available from: https://www.nap.edu/read/9956/chapter/1
Raverdeau M, Mills KHG. Modulation of T cell and innate immune responses by retinoic acid. J Immunol. 2014;192(7):2953. Available from: http://www.jimmunol.org/content/192/7/2953.abstract
Gruz-Gibelli E, Chessel N, Allioux C, Marin P, Piotton F, Leuba G, et al. The vitamin A derivative all-trans retinoic acid repairs amyloid-β-induced double-strand breaks in neural cells and in the murine neocortex. Neural Plast. 2016;2016:3707406.
Schleicher M, Weikel K, Garber C, Taylor A. Diminishing risk for age-related macular degeneration with nutrition: a current view. Nutrients. 2013;5(7):2405–56. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3738980/
Manna PR, Stetson CL, Daugherty C, Shimizu I, Syapin PJ, Garrel G, et al. Up-regulation of steroid biosynthesis by retinoid signaling: implications for aging. Mech Ageing Dev. 2015;150:74–82. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4583817/
Shao Y, He T, Fisher GJ, Voorhees JJ, Quan T. Molecular basis of retinol anti-ageing properties in naturally aged human skin in vivo. Int J Cosmet Sci. 2017;39(1):56–65. Available from: http://onlinelibrary.wiley.com/doi/10.1111/ics.12348/abstract
Kong R, Cui Y, Fisher GJ, Wang X, Chen Y, Schneider LM, et al. A comparative study of the effects of retinol and retinoic acid on histological, molecular, and clinical properties of human skin. J Cosmet Dermatol. 2016;15(1):49–57. Available from: http://onlinelibrary.wiley.com/doi/10.1111/jocd.12193/abstract
• Bolzetta F, Veronese N, De Rui M, Berton L, Toffanello ED, Carraro S, et al. Are the recommended dietary allowances for vitamins appropriate for elderly people? J Acad Nutr Diet. 2015;115(11):1789–97. Bolzetta: This is a global study analyzing the sufficiency of the American, European, and Italian RDAs in elderly women over the age of 65 years. Larger, higher quality studies of this nature should be conducted to provide stronger direction for research in micronutrients and aging.
Mahan LK, Raymond JL. Krause’s food & the nutrition care process-E-book: Elsevier Health Sciences; Saunders Eds. 2016. 1152 p. ISBN: 9780323340755 71. Skaaby T. The relationship of vitamin D status to risk of cardiovascular disease and mortality. Dan Med J. 2015;62(2) pii: B5008.
Bjelakovic G, Nikolova D, Gluud LL, Simonetti RG, Gluud C. Antioxidant supplements for prevention of mortality in healthy participants and patients with various diseases. Cochrane Database Syst Rev. 2012;3:CD007176.
Mischo M, von Kobyletzki LB, Bründermann E, Schmidt DA, Potthoff A, Brockmeyer NH, et al. Similar appearance, different mechanisms: xerosis in HIV, atopic dermatitis and ageing. Exp Dermatol. 2014;23(6):446–8.
Ambrosini GL, Alfonso H, Reid A, Mackerras D, Bremner AP, Beilby J, et al. Plasma retinol and total carotenes and fracture risk after long-term supplementation with high doses of retinol. Nutrition. 2014;30(5):551–6. [cited 2018 Feb 6]. Available from: http://www.nutritionjrnl.com/article/S0899-9007(13)00452-8/abstract
Maggio M, de Vita F, Lauretani F, Bandinelli S, Semba RD, Bartali B, et al. Relationship between carotenoids, retinol, and estradiol levels in older women. Nutrients. 2015;7(8):6506–19. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4555135/
Ribaya-Mercado JD, Blumberg JB. Vitamin A: is it a risk factor for osteoporosis and bone fracture? Nutr Rev. 2007;65(10):425–38.
Joo N-S, Yang S-W, Song BC, Yeum K-J. Vitamin A intake, serum vitamin D and bone mineral density: analysis of the Korea National Health and nutrition examination survey (KNHANES, 2008–2011). Nutrients. 2015;7(3):1716–27. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4377877/
Bosetti M, Sabbatini M, Calarco A, Borrone A, Peluso G, Cannas M. Effect of retinoic acid and vitamin D3 on osteoblast differentiation and activity in aging. J Bone Miner Metab. 2016;34(1):65–78. [cited 2018 Feb 6]. Available from: https://link.springer.com/article/10.1007/s00774-014-0642-2
Lasisi TJ, Lasisi AO. Evaluation of serum antioxidants in age-related hearing loss. Aging Clin Exp Res. 2015;27(3):265–9. [cited 2018 Feb 6]. Available from: https://link.springer.com/article/10.1007/s40520-014-0282-3
Venneria E, Intorre F, Foddai MS, Azzini E, Palomba L, Raguzzini A, et al. Antioxidant effect of zinc supplementation on both plasma and cellular red-ox status markers in a group of elderly Italian population. J Nutr Health Aging. 2014;18(4):345–50.
• Nomura SJ, Robien K, Zota AR. Serum folate, vitamin B-12, vitamin A, γ-tocopherol, α-tocopherol, and carotenoids do not modify associations between cadmium exposure and leukocyte telomere length in the general US adult population. J Nutr. 2017;147(4):538–48. Nomura: This study utilized US NHANES data to find associations between various serum levels of micronutrients and leukocyte telomere length (LTL). LTL is a promising new biomarker for future research in aging. Further studies should focus on this biomarker in relation to chronic disease prevention.
Erdman J, MacDonald I, Zeisel S. Present knowledge in nutrition. 10th ed. 2012 [cited 2018 Feb 6]. 1328 p. Available from: https://www.wiley.com/en-us/Present+Knowledge+in+Nutrition%2C+10th+Edition-p-9780470959176.
• Porter K, Hoey L, Hughes CF, Ward M, McNulty H. Causes, consequences and public health implications of low B-vitamin status in ageing. Nutrients. 2016;8(11) Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5133110/. Porter: This article provides a comprehensive review of current and future research on the vitamin B family for aging.
Sawaengsri H, Bergethon PR, Qiu WQ, Scott TM, Jacques PF, Selhub J, et al. Transcobalamin 776C→G polymorphism is associated with peripheral neuropathy in elderly individuals with high folate intake. Am J Clin Nutr. 2016;104(6):1665–70.
• Ho RCM, Cheung MWL, Fu E, Win HH, Zaw MH, Ng A, et al. Is high homocysteine level a risk factor for cognitive decline in elderly? A systematic review, meta-analysis, and meta-regression. Am J Geriatr Psychiatry. 2011;19(7):607–17. Ho: This review provides comprehensive high quality data summarizing the effect of homocysteine levels on cognitive decline in the elderly, which can be strongly associated with micronutrient intake.
Elstgeest LEM, Brouwer IA, Penninx BWH, van Schoor NM, Visser M. Vitamin B12, homocysteine and depressive symptoms: a longitudinal study among older adults. Eur J Clin Nutr. 2017;71(4):468–75.
Petridou ET, Kousoulis AA, Michelakos T, Papathoma P, Dessypris N, Papadopoulos FC, et al. Folate and B12 serum levels in association with depression in the aged: a systematic review and meta-analysis. Aging Ment Health. 2016;20(9):965–73.
Gougeon L, Payette H, Morais JA, Gaudreau P, Shatenstein B, Gray-Donald K. A prospective evaluation of the depression-nutrient intake reverse causality hypothesis in a cohort of community-dwelling older Canadians. Br J Nutr. 2017;117(7):1032–41.
Miles LM, Mills K, Clarke R, Dangour AD. Is there an association of vitamin B12 status with neurological function in older people? A systematic review. Br J Nutr. 2015;114(4):503–8.
Smith AD, Smith SM, de Jager CA, Whitbread P, Johnston C, Agacinski G, et al. Homocysteine-lowering by B vitamins slows the rate of accelerated brain atrophy in mild cognitive impairment: a randomized controlled trial. PLoS One. 2010;5(9):e12244. [cited 2018 Feb 8]. Available from: http://journals.plos.org/plosone/article?id=10.1371/journal.pone.0012244
Hooshmand B, Mangialasche F, Kalpouzos G, Solomon A, Kåreholt I, Smith AD, et al. Association of vitamin B12, folate, and sulfur amino acids with brain magnetic resonance imaging measures in older adults: a longitudinal population-based study. JAMA Psychiatry. 2016;73(6):606–13.
Lefèvre-Arbogast S, Féart C, Dartigues J-F, Helmer C, Letenneur L, Samieri C. Dietary B vitamins and a 10-year risk of dementia in older persons. Nutrients. 2016;8(12):761. [cited 2018 Feb 6]. Available from: http://www.mdpi.com/2072-6643/8/12/761
Spence JD. Increased coagulation with aging: importance of homocysteine and vitamin B12. Circ J. 2017;81(2):268.
Reynolds EH. What is the safe upper intake level of folic acid for the nervous system? Implications for folic acid fortification policies. Eur J Clin Nutr. 2016;70(5):537–40.
Bailey RL, McDowell MA, Dodd KW, Gahche JJ, Dwyer JT, Picciano MF. Total folate and folic acid intakes from foods and dietary supplements of US children aged 1–13 y. Am J Clin Nutr. 2010;92(2):353–8.
Mason JB, Tang SY. Folate status and colorectal cancer risk: a 2016 update. Mol Asp Med. 2017;53:73–9.
Presse N, Perreault S, Kergoat M-J. Vitamin B12 deficiency induced by the use of gastric acid inhibitors: calcium supplements as a potential effect modifier. J Nutr Health Aging. 2016;20(5):569–73.
IOM. Dietary reference intakes for vitamin A, vitamin K, arsenic, boron, chromium, copper, iodine, iron, manganese, molybdenum, nickel, silicon, vanadium, and zinc. The National Academies Press; 2001 [cited 2018 Feb 5]. 800 p. Available from: https://www.nap.edu/read/10026/chapter/1.
Mocchegiani E, Costarelli L, Giacconi R, Piacenza F, Basso A, Malavolta M. Micronutrient (Zn, Cu, Fe)–gene interactions in ageing and inflammatory age-related diseases: implications for treatments. Ageing Res Rev. 2012;11(2):297–319. Available from: http://www.sciencedirect.com/science/article/pii/S1568163712000050
Dao MC, Meydani SN. Iron biology, immunology, aging, and obesity: four fields connected by the small peptide hormone hepcidin. Adv Nutr. 2013;4(6):602–17.
• Fairweather-Tait SJ, Wawer AA, Gillings R, Jennings A, Myint PK. Iron status in the elderly. Mech Ageing Dev. 2014;136–137:22–8. Fairweather: A thorough, summative review on the latest information of iron metabolism in the elderly population and a randomized trial on iron’s effects on inflammation in the elderly using innovative measurements of serum iron.
Anderson ER, Shah YM. Iron homeostasis in the liver. Compr Physiol. 2013;3(1):315–30. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3936199/
Goodnough LT, Schrier SL. Evaluation and management of anemia in the elderly. Am J Hematol. 2014;89(1):88–96. [cited 2018 Feb 5]. Available from: http://onlinelibrary.wiley.com/doi/10.1002/ajh.23598/abstract
Moll R, Davis B. Iron, vitamin B12 and folate. Medicine (Baltimore). 2017;45(4):198–203. Available from: http://www.sciencedirect.com/science/article/pii/S135730391730021X
FAO, WHO. World declaration and plan of action for nutrition. International Conference on Nutrition. Rome, Food and Agriculture Organization of the United Nations, f. 1992 Dec; Available from: http://whqlibdoc.who.int/hq/1992/a34303.pd.
Beutler E, Waalen J. The definition of anemia: what is the lower limit of normal of the blood hemoglobin concentration? Blood. 2006;107(5):1747–50.
Guralnik JM, Eisenstaedt RS, Ferrucci L, Klein HG, Woodman RC. Prevalence of anemia in persons 65 years and older in the United States: evidence for a high rate of unexplained anemia. Blood. 2004;104(8):2263–8.
Stewart R, Hirani V. Relationship between depressive symptoms, anemia, and iron status in older residents from a national survey population. Psychosom Med. 2012;74(2):208–13.
Smith MA, Zhu X, Tabaton M, Liu G, DW MK Jr, et al. Increased iron and free radical generation in preclinical Alzheimer disease and mild cognitive impairment. J Alzheimers Dis. 2010;19(1):363–72. [cited 2018 Feb 8]. Available from: https://content.iospress.com/articles/journal-of-alzheimers-disease/jad01239
Sung K-C, Kang S-M, Cho E-J, Park JB, Wild SH, Byrne CD. Ferritin is independently associated with the presence of coronary artery calcium in 12 033 Men. Arterioscler Thromb Vasc Biol. 2012;32(10):2525–30. [cited 2018 Feb 8]. Available from: http://atvb.ahajournals.org/content/32/10/2525
Hsu H-S, Li C-I, Liu C-S, Lin C-C, Huang K-C, Li T-C, et al. Iron deficiency is associated with increased risk for cardiovascular disease and all-cause mortality in the elderly living in long-term care facilities. Nutrition. 2013;29(5):737–43.
Ward RJ, Zucca FA, Duyn JH, Crichton RR, Zecca L. The role of iron in brain ageing and neurodegenerative disorders. Lancet Neurol. 2014;13(10):1045–60. Available from: http://www.sciencedirect.com/science/article/pii/S1474442214701176
Knekt P, Reunanen A, Takkunen H, Aromaa A, Heliövaara M, Hakuunen T. Body iron stores and risk of cancer. Int J Cancer. 1994;56(3):379–82. Available from: http://onlinelibrary.wiley.com/doi/10.1002/ijc.2910560315/abstract
Torti SV, Torti FM. Ironing out cancer. Cancer Res. 2011;71(5):1511–4. [cited 2018 Feb 8]. Available from: http://cancerres.aacrjournals.org/content/71/5/1511
Toyokuni S. Iron as a target of chemoprevention for longevity in humans. Free Radic Res. 2011;45(8):906–17. https://doi.org/10.3109/10715762.2011.564170.
Scientific Advisory Committee on Nutrition. Iron and health report. Public Health England; 2011. p. 374. [cited 2018 Feb 8]. Available from: https://www.gov.uk/government/publications/sacn-iron-and-health-report.
Lindblad AJ, Cotton C, Allan GM. Iron deficiency anemia in the elderly. Can Fam Physician. 2015;61(2):159. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4325864/
Lane DJR, Jansson PJ, Richardson DR. Bonnie and Clyde: vitamin C and iron are partners in crime in iron deficiency anaemia and its potential role in the elderly. Aging. 2016;8(5):1150–2. [cited 2018 Mar 19]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4931859/
Skaaby T. The relationship of vitamin D status to risk of cardiovascular disease and mortality. Dan Med J. 2015;62(2) pii: B5008.
Mizwicki MT, Menegaz D, Zhang J, Barrientos-Durán A, Tse S, Cashman JR, et al. Genomic and nongenomic signaling induced by 1α,25(OH)2-vitamin D3 promotes the recovery of amyloid-β phagocytosis by Alzheimer’s disease macrophages. J Alzheimers Dis JAD. 2012;29(1):51–62.
IOM. Dietary reference intakes for calcium and vitamin D. Washington, DC: The National Academies Press; 2011. [cited 2018 Feb 4]. Available from: https://www.nap.edu/read/13050/chapter/7
Nordin BEC, Need AG, Morris HA, O’Loughlin PD, Horowitz M. Effect of age on calcium absorption in postmenopausal women. Am J Clin Nutr. 2004;80(4):998–1002.
Brouwer-Brolsma EM, Bischoff-Ferrari HA, Bouillon R, Feskens EJM, Gallagher CJ, Hypponen E, et al. Vitamin D: do we get enough? A discussion between vitamin D experts in order to make a step towards the harmonisation of dietary reference intakes for vitamin D across Europe. Osteoporos Int. 2013;24(5):1567–77.
WHO Scientific Group on the Prevention and Management of Osteoporosis (2000: Geneva S. Prevention and management of osteoporosis: report of a WHO scientific group. 2003 [cited 2018 Feb 4]; Available from: http://www.who.int/iris/handle/10665/42841.
• ter Borg S, Verlaan S, Hemsworth J, Mijnarends DM, JMGA S, Luiking YC, et al. Micronutrient intakes and potential inadequacies of community-dwelling older adults: a systematic review. Br J Nutr. 2015;113(8):1195–206. [cited 2018 Feb 4]. Available from: https://www.cambridge.org/core/journals/british-journal-of-nutrition/article/micronutrient-intakes-and-potential-inadequacies-of-communitydwelling-older-adults-a-systematic-review/1F708F9E5F20DBA3957F5CDCA73AB79D. Borg: A systematic review following the preferred reporting items for systematic reviews and meta-analyses statement was performed on observational cohort and longitudinal studies of dietary intakes of older adults. The review reports the percentages at risk for inadequate micronutrient intakes from 37 articles including 20 nutrients.
Pfortmueller CA, Lindner G, Exadaktylos AK. Reducing fall risk in the elderly: risk factors and fall prevention, a systematic review. Minerva Med. 2014;105(4):275–81.
Anagnostis P, Dimopoulou C, Karras S, Lambrinoudaki I, Goulis DG. Sarcopenia in post-menopausal women: is there any role for vitamin D? Maturitas. 2015;82(1):56–64.
Avenell A, Mak JCS, O’Connell D. Vitamin D and vitamin D analogues for preventing fractures in post-menopausal women and older men. Cochrane Database Syst Rev. 2014;4:CD000227.
Shinkov A, Borissova A-M, Dakovska L, Vlahov J, Kassabova L, Svinarov D, et al. Differences in the prevalence of vitamin D deficiency and hip fractures in nursing home residents and independently living elderly. Arch Endocrinol Metab. 2016;60(3):217–22.
Bjelakovic G, Gluud LL, Nikolova D, Whitfield K, Krstic G, Wetterslev J, et al. Vitamin D supplementation for prevention of cancer in adults. Cochrane Database Syst Rev. 2014;(6): CD007469. Available from: https://doi.org/10.1002/14651858.CD007469.pub2.
• Newberry SJ, Chung M, Shekelle PG, Booth MS, Liu JL, Maher AR, et al. Vitamin D and calcium: a systematic review of health outcomes (update). Agency for Healthcare Research and Quality (US). 2014. Available from: https://www.effectivehealthcare.ahrq.gov/reports/final.cfm. https://doi.org/10.23970/AHRQEPCERTA217. Evidence Report/Technology Assessment No. 217. (Prepared by the Southern California Evidence-based Practice Center under Contract No. 290-2012-00006-I.) AHRQ Publication No. 14-E004-EF. Rockville, MD: Agency for Healthcare Research and Quality.
Annweiler C, Beauchet O. Vitamin D in older adults: the need to specify standard values with respect to cognition. Front Aging Neurosci. 2014;6. [cited 2018 Jan 20]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3995037/.
Goodwill AM, Szoeke C. A systematic review and meta-analysis of the effect of low vitamin D on cognition. J Am Geriatr Soc. 2017;65(10):2161–8.
Maddock J, Zhou A, Cavadino A, Kuźma E, Bao Y, Smart MC, et al. Vitamin D and cognitive function: a Mendelian randomisation study. Sci Rep. 2017;7. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5643555/.
Rossom RC, Espeland MA, Manson JE, Dysken MW, Johnson KC, Lane DS, et al. Calcium and vitamin D supplementation and cognitive impairment in the women’s health initiative. J Am Geriatr Soc. 2012;60(12):2197–205. Available from: http://onlinelibrary.wiley.com/doi/10.1111/jgs.12032/abstract
Kaur P, Mishra SK, Mithal A. Vitamin D toxicity resulting from overzealous correction of vitamin D deficiency. Clin Endocrinol. 2015;83(3):327–31.
Bailey RL, Dodd KW, Goldman JA, Gahche JJ, Dwyer JT, Moshfegh AJ, et al. Estimation of total usual calcium and vitamin D intakes in the United States. J Nutr. 2010;140(4):817–22.
Choi S-J, Yeum K-J, Park S-J, Choi B, Joo N-S. Dietary calcium and Framingham Risk Score in vitamin D deficient male (KNHANES 2009–2011). Yonsei Med J. 2015;56(3):845–52.
• Theodoratou E, Tzoulaki I, Zgaga L, Ioannidis JPA. Vitamin D and multiple health outcomes: umbrella review of systematic reviews and meta-analyses of observational studies and randomised trials. BMJ. 2014;348:g2035. Theodoratou: This comprehensive umbrella review of systematic reviews and meta-analyses of observational studies and RCTs provided highly convincing evidence that the association of Vitamin D in different health outcomes does not consistently exist.
Straub DA. Calcium supplementation in clinical practice: a review of forms, doses, and indications. Nutr Clin Pract. 2007;22(3):286–96.
American Geriatrics Society Workgroup on Vitamin D Supplementation for Older Adults. Recommendations abstracted from the American Geriatrics Society Consensus Statement on vitamin D for prevention of falls and their consequences. J Am Geriatr Soc. 2014;62(1):147–52.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Maria Nieves Garcia-Casal is a full staff member of the World Health Organization (WHO). WHO gratefully acknowledges the financial contribution of the Bill & Melinda Gates Foundation, USA. Jessica Watson, Marissa Lee and Maria Nieves Garcia-Casal declare no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Disclaimer
The authors alone are responsible for the views expressed in this article and they do not necessarily represent the views, decisions or policies of the institutions with which they are affiliated.
Additional information
This article is part of the Topical Collection on Nutrition, Obesity and Diabetes
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Watson, J., Lee, M. & Garcia-Casal, M.N. Consequences of Inadequate Intakes of Vitamin A, Vitamin B12, Vitamin D, Calcium, Iron, and Folate in Older Persons. Curr Geri Rep 7, 103–113 (2018). https://doi.org/10.1007/s13670-018-0241-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13670-018-0241-5