Abstract
Introduction
Ixekizumab, a high-affinity monoclonal antibody that selectively targets interleukin-17A, is approved for the treatment of moderate-to-severe plaque psoriasis. Since scalp psoriasis can be burdensome and challenging to treat with non-systemic therapies, this post hoc analysis focused on scalp psoriasis in patients with moderate-to-severe plaque psoriasis and baseline scalp involvement. The analysis considered a holistic concept of clearance through 5 years of ixekizumab treatment.
Methods
Ixekizumab-treated patients with baseline scalp involvement were pooled from three multicenter, randomized, double-blind, placebo-controlled, phase 3 trials (integrated UNCOVER-1/2 and UNCOVER-3). Analyses were performed on a subpopulation of patients who achieved complete resolution of scalp psoriasis at Week 60 (i.e., Week 60 Psoriasis Scalp Severity Index [PSSI-0] responders) and on the overall patient population (i.e., Week 60 PSSI-0 responders and non-responders), which was used as a reference. Clinical outcomes (PSSI), patient-reported outcomes (Itch Numeric Rating Scale [NRS] score, Skin Pain Visual Analogue Scale [VAS]), quality of life (Dermatology Life Quality Index [DLQI]), and concurrent outcomes were assessed from baseline through 5 years. Descriptive statistics of observed data were reported.
Results
After 60 weeks of ixekizumab treatment, 88.4% (UNCOVER-1/2) and 75.9% (UNCOVER-3) of patients with baseline scalp involvement achieved complete clearance (PSSI-0) of scalp psoriasis. Substantial improvements in the clinical outcomes (PSSI), patient-reported outcomes (Itch NRS, Skin Pain VAS), and quality of life (DLQI) were achieved by Week 60 and sustained through Week 264 in the Week 60 PSSI-0 responders and in the overall patient population. Additionally, a significant proportion of Week 60 PSSI-0 responders achieved concurrent complete scalp and skin clearance and quality of life improvement through 5 years.
Conclusions
Continued treatment with ixekizumab provided long-term sustained scalp clearance over 5 years to patients with moderate-to-severe plaque psoriasis and baseline scalp involvement, and holistic improvements occurred across clinical outcomes, patient-reported outcomes, and quality of life.
Clinical Trial Numbers
NCT01474512 (UNCOVER-1), NCT01597245 (UNCOVER-2), and NCT01646177 (UNCOVER-3).
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Scalp psoriasis disproportionately impacts patient quality of life and can be challenging to treat. |
Highly effective biologic therapies are available but long-term durable efficacy data for scalp clearance are lacking. |
These data describe the long-term sustainability of scalp clearance and other outcomes in patients treated with the label dose of ixekizumab for up to 5 years. |
Combined clinical outcomes, patient-reported outcomes, and quality of life were also evaluated to provide a holistic view of clearance. |
Introduction
Psoriasis is a chronic inflammatory skin disease that affects 3.0% of the US adult population [1] and an estimated 55.8 million adults worldwide [2]. The scalp is the most affected body region, with 50–80% of patients reporting scalp involvement [3]. Patients with scalp psoriasis reported greater disease and itch severity and poorer health compared to patients affected by psoriasis in other body areas [4]. Scalp psoriasis causes social and psychologic effects on patients, disproportionately impacting the quality of life due to appearance, visible flaking onto clothing, and often severe pruritus [5, 6]. Importantly, scalp psoriasis has been cited as a risk factor for psoriatic arthritis [7].
Although topical therapy options exist, patients report a high level of dissatisfaction with currently available treatments, and the need for an effective therapy to treat scalp psoriasis remains unmet [8, 9]. Evidence suggests that interleukin (IL)-17A plays a central role in the pathogenesis of psoriasis and in other autoimmune disorders [10]. Ixekizumab, a high-affinity monoclonal antibody that selectively targets IL-17A [11], is approved for the treatment of moderate-to-severe plaque psoriasis in adult and pediatric populations. In the phase 3 trials UNCOVER-1 (NCT01474512) and UNCOVER-2 (NCT01597245), ixekizumab was well tolerated and efficacious in treating patients with moderate-to-severe plaque psoriasis through 12 and 60 weeks [12, 13]. In addition, the phase 3 trial UNCOVER-3 (NCT01646177) has demonstrated that ixekizumab provides a sustained long-term clinical response throughout the 5-year treatment period in patients with moderate-to-severe plaque psoriasis [14].
Ixekizumab has not been specifically studied for treatment of patients presenting with scalp psoriasis alone. However, in the UNCOVER trials, a significant proportion of patients had concomitant involvement of the scalp. The focus of this post hoc analysis was to evaluate long-term sustained clearance of scalp psoriasis and its relationship with other outcomes from the UNCOVER trials over a 5-year period. Outcomes examined included clinical outcomes, patient-reported outcomes, quality of life, and concurrent outcomes through 5 years of ixekizumab treatment in patients with moderate-to-severe plaque psoriasis and baseline scalp involvement.
Methods
Design of UNCOVER Clinical Trials and Participants
UNCOVER-1 (NCT01474512), UNCOVER-2 (NCT01597245), and UNCOVER-3 (NCT01646177) were phase 3, multicenter, randomized, double-blind, placebo-controlled, active-comparator (UNCOVER-2 and UNCOVER-3), parallel-group trials enrolling patients with moderate-to-severe plaque psoriasis. Details of the trial designs have previously been published [12, 13].
Eligible participants for UNCOVER-1, UNCOVER-2, and UNCOVER-3 trials were male or female patients aged 18 years or older who had a confirmed diagnosis of chronic plaque psoriasis, at least 6 months before randomization, who were candidates for phototherapy, systemic therapy, or both, and who had ≥ 10% body surface area involvement, a sPGA score ≥ 3, and a Psoriasis Area and Severity Index (PASI) score ≥ 12 at both screening and baseline visits. Patients with prior etanercept use were excluded from UNCOVER-2 and UNCOVER-3 studies.
The studies were conducted according to the principles of the Declaration of Helsinki and Council for International Organizations of Medical Sciences International Ethical Guidelines. An institutional review board reviewed and approved study protocols and informed consent forms at each participating site. All patients signed informed consent prior to undergoing study-related procedures.
Outcomes
Several secondary outcomes were assessed in the analyzed patient populations from baseline through 5 years, including at weeks 24, 60, 108, 156, 204, and 264. Among the clinical outcomes, the Psoriasis Scalp Severity Index (PSSI) score was used to assess the severity of scalp psoriasis. The PSSI is a composite score derived from the sum of scores for erythema, induration, and desquamation multiplied by a score for the extent of scalp area involved. PSSI ranges from 0 to 72, with PSSI-0 corresponding to complete clearance of scalp psoriasis. PASI100, a 100% improvement from baseline in the severity and extent of psoriasis in the whole body, was also assessed. Among the patient-reported outcomes, the Itch Numeric Rating Scale (NRS) and the Skin Pain Visual Analogue Scale (VAS) were used to assess the severity of itch and skin pain, respectively. Specifically, Itch NRS equal to 0 represented “no itch,” and Itch NRS equal to 10 represented “worst itch imaginable,” whereas Skin Pain VAS equal to 0 represented “no skin pain,” and Skin Pain VAS equal to 100 represented “severe skin pain.” The Dermatology Life Quality Index (DLQI) total score was used to assess the impact on dermatology-specific quality of life. Totals range from 0 to 30 (less to more impairment), and a 5-point change from baseline is considered clinically relevant [15]. The following concurrent outcomes were also evaluated as a holistic measurement among Week 60 PSSI-0 responders: concurrent PSSI-0 and PASI100 and concurrent PASI100 and DLQI-0,1.
Statistical Analysis
The analyses presented here are based on integrated data from UNCOVER-1/2 trials and UNCOVER-3 trial. Specifically, integrated data from the UNCOVER-1/2 trials included patients with baseline scalp involvement (PSSI > 0) that were IXE Q2W responders at Week 12 and who received IXE Q4W during the maintenance dosing period through Week 60 and continued the treatment in the long-term extension period through Week 264, excluding data from visits with titrated Q2W long-term dosing. Data from the UNCOVER-3 trial included patients with baseline scalp involvement (PSSI > 0) that received IXEQ 2W during the induction period through Week 12 and who received IXE Q4W during the long-term extension period through Week 264, excluding data from visits with titrated Q2W long-term dosing.
Due to the inherent differences in the study designs, integrating the datasets from UNCOVER-1 and -2 with UNCOVER-3 was not statistically feasible. Nevertheless, this study design provided cohorts of patients with baseline scalp involvement that were continuously treated with ixekizumab over 5 years: IXE Q2W for the first 12 weeks and IXE Q4W for the following weeks through Week 264.
Statistical analyses were performed on (1) a subpopulation of patients who achieved complete resolution of scalp psoriasis at Week 60, as assessed by PSSI-0 (i.e., Week 60 PSSI-0 responders), and (2) on the overall patient population (i.e., Week 60 PSSI-0 responders and non-responders), which was used as a reference. Week 60 was selected as the cut-off for this subpopulation analysis because of study design. At Week 60, patients in the UNCOVER-1 and UNCOVER-2 trials entered the long-term extension period, while patients in the UNCOVER-3 trial could escalate to the higher dose regimen.
Descriptive statistics of observed data were applied to clinical outcomes, patient-reported outcomes, quality of life, and concurrent outcomes. The means and standard errors (SE) for total scores and percent improvement from baseline (PSSI score, DLQI total score, Itch NRS score, Skin Pain VAS) and the means and 95% confidence intervals for the response rates (PSSI-0, concurrent PSSI-0 and PASI100, and concurrent PASI100 and DLQI-0,1) were summarized.
Results
Patient Demographics and Baseline Characteristics
A total of 538 ixekizumab-treated patients, who had scalp psoriasis at baseline and a PSSI measurement at Week 60, were included in this post hoc analysis. Among them, 88.4% (167/189) of patients from UNCOVER-1/2 and 75.9% (265/349) of patients from UNCOVER-3 were Week 60 PSSI-0 responders, meaning that they achieved complete clearance of scalp psoriasis at Week 60 (Fig. 1). Patient demographics were balanced across the patient subpopulations from the UNCOVER trials (Table 1). Baseline characteristics were comparable between Week 60 PSSI-0 responders and the overall population of the UNCOVER-1/2 and the UNCOVER-3 trials, respectively, with a mean (SE) PSSI score ranging from 19.2 (0.8) to 20.7 (1.0) and a mean (SE) PASI score ranging from 19.2 (0.5) to 21.1 (0.5). Mean (SE) DLQI total score for Week 60 PSSI-0 responders and the overall population respectively were 12.8 (0.5) and 12.6 (0.5) in the UNCOVER-1/2, mean (SE) Itch NRS scores were 6.9 (0.2) and 6.8 (0.2) in the UNCOVER-1/2 and 6.5 (0.2) and 6.5 (0.1) in UNCOVER-3, and mean (SE) Skin Pain VASs were 47.0 (2.4) and 45.5 (2.2) in the UNCOVER-1/2 (Table 1). DLQI and Skin Pain VAS data were not collected past Week 12 in UNCOVER-3 trial; therefore, these outcomes were excluded from the analysis of the UNCOVER-3 data.
Clinical Outcomes
The proportion of Week 60 PSSI-0 responders achieving complete clearance of scalp psoriasis (PSSI-0) increased steadily from baseline to Week 60 and was maintained at or above 84.9% and 88.5% through Week 264 in the UNCOVER-1/2 and UNCOVER-3 trials, respectively (Fig. 2). For reference, the difference in response rates between the Week 60 PSSI-0 responders and the overall patient population ranged from 3.1% to 13.4% between Week 60 and Week 264 (Fig. 2). In terms of mean (SE) percent improvement from baseline, Week 60 PSSI-0 responders showed a substantial improvement in PSSI score of 68.3% (2.6) and 73.9% (1.9) in the UNCOVER-1/2 and UNCOVER-3 trials, respectively, as early as Week 2 (Fig. 3A). This increased steadily through Week 60 and was sustained through Week 264 at or above 82.5% (10.9) and 97.4% (1.1) in the UNCOVER-1/2 and UNCOVER-3 trials, respectively (Fig. 3A).
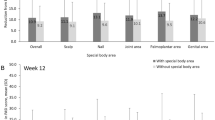
Mean percent improvement in A Psoriasis Scalp Severity Index (PSSI) score, B Dermatology Life Quality Index (DLQI) total score, C Itch Numeric Rating Scale (NRS) score, and D skin pain visual analogue scale (VAS) score among Week 60 PSSI-0 responders and overall patient population (i.e., responders and non-responders) from UNCOVER-1/2 and UNCOVER-3 trials. Mean observed data with standard error (SE) are presented. The timepoints for which SEs are < 2 may not be visible on figures
Patient-Reported Outcomes and Quality of Life
Patient-reported outcomes among Week 60 PSSI-0 responders showed substantial mean (SE) percent improvement from baseline as early as Week 12 in DLQI total score: 88.1% (1.5) in UNCOVER-1/2 trials (Fig. 3B); Itch NRS score: 82.6% (2.1) and 84.0% (1.7) in the UNCOVER-1/2 and UNCOVER-3 trials, respectively (Fig. 3C); and Skin Pain VAS score: 84.4% (2.8) in the UNCOVER-1/2 trial (Fig. 3D). These improvements were sustained through Week 264 when patients reported a 94.3% (1.1) improvement in the DLQI total score (Fig. 3B), 90.8 (1.6) and 86.4% (2.0) in the Itch NRS score in each trial, respectively (Fig. 3C), and 95.2% (1.1) in the Skin Pain VAS score (Fig. 3D). For reference, the Week 60 PSSI-0 responders of UNCOVER-1/2 and UNCOVER-3 trials had higher mean percent improvements for Itch NRS and Skin Pain VAS than the respective overall patient population, ranging from 0.3% to 7.5% higher at each timepoint, from Week 4 throughout Week 264 (Fig. 3C, D). A similar trend was observed for DLQI total score from Week 24 throughout Week 264 (Fig. 3B).
Concurrent Outcomes
At Week 60, the proportions of patients with concurrent PSSI-0 and PASI100 were 70.7% and 73.2% for the Week 60 PSSI-0 responders in the UNCOVER-1/2 and UNCOVER-3 trials, respectively, and these responses were maintained stable in the ranges of 70.7% to 61.3% and 73.2% to 58.5% in each trial, respectively, through Week 264 (Fig. 4A). At Week 60, the proportions of patients with concurrent PASI100 and DLQI-0,1 were 63.5% for the Week 60 PSSI-0 responders in the UNCOVER-1/2 trials, and these responses stayed stable in the range of 63.5% to 55.4% through Week 264 (Fig. 4B). DLQI data were not collected past induction Week 12 in the UNCOVER-3 trial.
Proportion of patients with A concurrent Psoriasis Scalp Severity Index (PSSI-0) and Psoriasis Area and Severity Index (PASI100) and B concurrent Psoriasis Area and Severity Index (PASI100) and Dermatology Life Quality Index (DLQI-0,1) among week 60 PSSI-0 responders from UNCOVER-1/2 and UNCOVER-3 trials. Observed data with 95% confidence interval (CI) are presented
Discussion
Among patients with psoriasis, unmet needs for those with scalp involvement remain. Indeed, the scalp is considered a challenging body area along with nails, face, intertriginous, genitals, and palmoplantar regions [16], which play a role in defining disease severity because of levels of disease burden that are disproportionate to the body surface area involved [17]. For the scalp, relative difficulty in using topical therapies or phototherapy means that systemic therapies are often required for treatment [4, 18]. As was the case in our patient population, scalp involvement is frequently seen among patients with moderate-to-severe psoriasis, and understanding the mid- and long-term outcomes for this body region as part of the treatment journey is important for informing shared patient goals.
In this post hoc analysis, we found that most patients with moderate-to-severe psoriasis who had baseline scalp involvement achieved complete scalp clearance at Week 60 and experienced sustained clearance with continuous ixekizumab treatment through 5 years. Additionally, a significant proportion of these patients also achieved complete skin clearance (PASI100) and sustained improvements in patient-reported outcomes (itch, skin pain) and quality of life through 5 years. Similarly, among the Week 60 PSSI-0 responders, we assessed the proportion of patients with concurrent complete skin clearance (PASI100) and “No effect at all on patient’s life” (DLQI-0,1) and found a high proportion of patients achieved this combined outcome.
As the treatment landscape has evolved with several therapies capable of delivering higher than historical PASI75 thresholds, a combination of complete skin clearance (PASI100), clearance in challenging body areas (e.g., scalp), and improvements in patient-reported outcomes is increasingly attainable and delivers a more holistic assessment of improvement in overall disease [19,20,21]. The novelty of this analysis is that it considers a more stringent, holistic concept of clearance that includes a challenging body area (i.e., the scalp), complete clearance, and quality of life over a 5-year period. This view of treatment outcomes provides an elevated threshold to consider as a concept of resolution that goes beyond the PASI100 definition.
A limitation of this study is that data from the UNCOVER-1/2 trials and from the UNCOVER-3 trial could not be pooled into an integrated dataset because of differences in the trial study designs. As a result, patient populations from UNCOVER-1/2 and UNCOVER-3 were analyzed separately. Additionally, it is difficult to ascertain how much of the difference in outcomes between the Week 60 PSSI-0 responder group and the overall patient population (i.e., reference) is attributable to response or non-response of scalp psoriasis as opposed to other body areas.
Conclusion
In conclusion, scalp psoriasis is burdensome and may be linked with other disease outcomes. Patients with moderate-to-severe psoriasis who also have scalp involvement achieve a high level of efficacy with ixekizumab that is sustained over 5 years. Additionally, a significant proportion of patients achieves concurrent complete scalp and skin clearance and quality of life improvement through 5 years. This holistic view of outcomes sets a more stringent threshold for disease clearance and informs clinicians on expectations over the long-term treatment journey of patients on ixekizumab.
Data Availability
Eli Lilly and Company provides access to all individual participant data collected during the trial, after anonymization, except for pharmacokinetic or genetic data. Data are available to request 6 months after the indication studied has been approved in the United States and European Union and after primary publication acceptance, whichever is later. No expiration date of data requests is currently set once data are made available. Access is provided after a proposal has been approved by an independent review committee identified for this purpose and after receipt of a signed data sharing agreement. Data and documents, including the study protocol, statistical analysis plan, clinical study report, blank, or annotated case report forms, will be provided in a secure data sharing environment. For details on submitting a request, see the instructions provided at www.vivli.org.
References
Armstrong AW, Mehta MD, Schupp CW, Gondo GC, Bell SJ, Griffiths CEM. Psoriasis prevalence in adults in the United States. JAMA Dermatol. 2021;157(8):940–6.
Parisi R, Iskandar IYK, Kontopantelis E, et al. National, regional, and worldwide epidemiology of psoriasis: systematic analysis and modelling study. BMJ. 2020;369: m1590.
Papp K, Berth-Jones J, Kragballe K, Wozel G, de la Brassinne M. Scalp psoriasis: a review of current topical treatment options. J Eur Acad Dermatol Venereol. 2007;21(9):1151–60.
Callis Duffin K, Mason MA, Gordon K, et al. Characterization of patients with psoriasis in challenging-to-treat body areas in the Corrona Psoriasis Registry. Dermatology. 2021;237(1):46–55.
Choi J, Koo JY. Quality of life issues in psoriasis. J Am Acad Dermatol. 2003;49(2 Suppl):S57-61.
van de Kerkhof PC, de Hoop D, de Korte J, Kuipers MV. Scalp psoriasis, clinical presentations and therapeutic management. Dermatology. 1998;197(4):326–34.
Cheng PS, Hou PC, Yang CC, Chu CB. Variation of body regional responses to ustekinumab and secukinumab in psoriasis patients: a real-world retrospective study and literature review. Dermatol Ther. 2022;35:e15950.
Christophers E, Griffiths CE, Gaitanis G, van de Kerkhof P. The unmet treatment need for moderate to severe psoriasis: results of a survey and chart review. J Eur Acad Dermatol Venereol. 2006;20(8):921–5.
Dubertret L, Mrowietz U, Ranki A, et al. European patient perspectives on the impact of psoriasis: the EUROPSO patient membership survey. Br J Dermatol. 2006;155(4):729–36.
Gaffen SL, Jain R, Garg AV, Cua DJ. The IL-23-IL-17 immune axis: from mechanisms to therapeutic testing. Nat Rev Immunol. 2014;14(9):585–600.
Liu L, Lu J, Allan BW, et al. Generation and characterization of ixekizumab, a humanized monoclonal antibody that neutralizes interleukin-17A. J Inflamm Res. 2016;9:39–50.
Gordon KB, Colombel JF, Hardin DS. Phase 3 trials of ixekizumab in moderate-to-severe plaque psoriasis. N Engl J Med. 2016;375(21):2102.
Griffiths CE, Reich K, Lebwohl M, et al. Comparison of ixekizumab with etanercept or placebo in moderate-to-severe psoriasis (UNCOVER-2 and UNCOVER-3): results from two phase 3 randomised trials. Lancet. 2015;386(9993):541–51.
Blauvelt A, Lebwohl MG, Mabuchi T, et al. Long-term efficacy and safety of ixekizumab: a 5-year analysis of the UNCOVER-3 randomized controlled trial. J Am Acad Dermatol. 2021;85(2):360–8.
Basra MK, Fenech R, Gatt RM, Salek MS, Finlay AY. The Dermatology Life Quality Index 1994–2007: a comprehensive review of validation data and clinical results. Br J Dermatol. 2008;159(5):997–1035.
Merola JF, Qureshi A, Husni ME. Underdiagnosed and undertreated psoriasis: Nuances of treating psoriasis affecting the scalp, face, intertriginous areas, genitals, hands, feet, and nails. Dermatol Ther. 2018;31(3): e12589.
Strober B, Ryan C, van de Kerkhof P, et al. Recategorization of psoriasis severity: Delphi consensus from the International Psoriasis Council. J Am Acad Dermatol. 2020;82(1):117–22.
Kivelevitch D, Frieder J, Watson I, Paek SY, Menter MA. Pharmacotherapeutic approaches for treating psoriasis in difficult-to-treat areas. Expert Opin Pharmacother. 2018;19(6):561–75.
Mrowietz U, Kragballe K, Reich K, et al. Definition of treatment goals for moderate to severe psoriasis: a European consensus. Arch Dermatol Res. 2011;303(1):1–10.
Puig L. PASI90 response: the new standard in therapeutic efficacy for psoriasis. J Eur Acad Dermatol Venereol. 2015;29(4):645–8.
Puig L, Thom H, Mollon P, Tian H, Ramakrishna GS. Clear or almost clear skin improves the quality of life in patients with moderate-to-severe psoriasis: a systematic review and meta-analysis. J Eur Acad Dermatol Venereol. 2017;31(2):213–20.
Acknowledgements
Eli Lilly and Company would like to thank the clinical trial participants and their caregivers, without whom this work would not be possible. The authors acknowledge Can Mert, PhD, contractor at HaaPACS GmbH, for the statistical review of the manuscript.
Medical Writing and/or Editorial Assistance.
Writing assistance was provided by Roisin McCarthy, Ph.D., former employee of Eli Lilly and Company, and Elisa Di Carlo, Ph.D., employee of Eli Lilly and Company.
Funding
This study was funded by Eli Lilly and Company, which contributed to study design, data collection, data analysis, data interpretation, manuscript preparation, and publication decisions (including Rapid Access fees).
Author information
Authors and Affiliations
Contributions
All named authors (Alexander Egeberg, Jason E. Hawkes, Najwa Somani, Russel Burge, Kyoungah See, Gaia Gallo, Missy McKean-Matthews, Melinda Gooderham, George Han, April Armstrong) meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, had full access to all the data in this study, take responsibility for the integrity of data and accuracy of the data analysis, and have given their approval for this version to be published. Specifically, Najwa Somani, Russel Burge, and Gaia Gallo contributed to the conception and design of the study, to the interpretation of the data and to the drafting of the manuscript. Kyoungah See and Missy McKean-Matthews performed the statistical analysis and contributed to the interpretation of the data and to the drafting of the manuscript. Alexander Egeberg, Jason E. Hawkes, Melinda Gooderham, George Han, and April Armstrong contributed to the critical revision of the manuscript for important intellectual content and participated sufficiently in the work to agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All named authors (Alexander Egeberg, Jason E. Hawkes, Najwa Somani, Russel Burge, Kyoungah See, Gaia Gallo, Missy McKean-Matthews, Melinda Gooderham, George Han, April Armstrong) meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, had full access to all the data in this study, take responsibility for the integrity of data and accuracy of the data analysis, and have given their approval for this version to be published.
Corresponding author
Ethics declarations
Conflict of interest
Alexander Egeberg is now an employee of LEO Pharma, has received research funding from Pfizer, Eli Lilly and Company, Novartis, Bristol-Myers Squibb, AbbVie, Janssen Pharmaceuticals, Boehringer Ingelheim, the Danish National Psoriasis Foundation, the Simon Spies Foundation, and the Kgl Hofbundtmager Aage Bang Foundation, and honoraria as consultant and/or speaker from AbbVie, Almirall, LEO Pharma, Zuellig Pharma Ltd., Galápagos NV, Sun Pharma, Samsung Bioepis Co., Ltd., Pfizer, Eli Lilly and Company, Novartis, Union Therapeutics, Galderma, Dermavant, UCB, Mylan, Bristol-Myers Squibb, McNeil Consumer Healthcare, Horizon Therapeutics, Boehringer Ingelheim, and Janssen Pharmaceuticals. Jason E. Hawkes currently serves on the medical board and scientific advisory committee of the National Psoriasis Foundation and as a consultant for AbbVie, Arcutis, Boehringer Ingelheim, Bristol-Myers Squibb, Janssen, LEO Pharma, Eli Lilly and Company, Novartis, Pfizer, Regeneron-Sanofi, Sun Pharma, and UCB. Najwa Somani, Russel Burge, Kyoungah See, and Gaia Gallo are employees and stockholders of Eli Lilly and Company. Missy McKean-Matthews reports working for Eli Lilly and Company through Syneos Health. Melinda Gooderham has received honoraria, grants, and/or research funding as a speaker, investigator, advisory board member, data safety monitoring board member, and/or consultant for AbbVie, Amgen, Arcutis, AnaptysBio, Aristea, Bausch Health, Boehringer Ingelheim, Celgene, Dermira, Dermavant, Eli Lilly and Company, Galderma, GlaxoSmithKline, Janssen, Kyowa Kirin, LEO Pharma, MedImmune, Merck Sharp & Dohme, Meiji, Moonlake, Nimbus, Novartis, Pfizer, Regeneron, Roche, Sanofi Genzyme, Sun Pharma, Takeda, Tarsus, UCB Pharma, and Ventyx. George Han is or has been an investigator, consultant/advisor, or speaker for AbbVie, Arcutis, Athenex, Boehringer Ingelheim, Bond Avillion, Bristol-Myers Squibb, Celgene Corporation, Dermavant, Eli Lilly and Company, Incyte, Janssen, LEO Pharma, MC2, Novartis, Ortho Dermatologics, PellePharm, Pfizer, Regeneron, Sanofi Genzyme, Sun Pharma, and UCB. April Armstrong has served as a research investigator and/or scientific advisor to AbbVie, Almirall, Arcutis, ASLAN, Beiersdorf, BI, Bristol-Myers Squibb, EPI, Incyte, LEO Pharma, UCB, Janssen, Eli Lilly and Company, Nimbus, Novartis, Ortho Dermatologics, Sun Pharma, Dermavant, Dermira, Sanofi, Regeneron, and Pfizer.
Ethical Approval
The studies were conducted according to the principles of the Declaration of Helsinki and Council for International Organizations of Medical Sciences International Ethical Guidelines. An institutional review board reviewed and approved study protocols and informed consent forms at each participating site. All patients signed informed consent prior to undergoing study-related procedures.
Additional information
Prior Presentation: This manuscript is based on work that has been previously presented in the form of a poster at the European Academy of Dermatology and Venereology (EADV)—30th Congress on 29 September 2021 (online) and at the Innovations in Dermatology: Spring Conference 2022 on 27 April 2022 in Scottsdale, AZ, USA.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Egeberg, A., Hawkes, J.E., Somani, N. et al. Sustained Improvements in Clinical and Patient-Reported Outcomes and Quality of Life Through 5 Years Among Ixekizumab-Treated Patients with Complete Clearance of Scalp Psoriasis by Week 60. Dermatol Ther (Heidelb) 14, 1007–1018 (2024). https://doi.org/10.1007/s13555-024-01147-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13555-024-01147-7