Abstract
Introduction
Systemic toxicity of eutectic mixture of local anesthetics (EMLA) cream is rare and is most commonly observed in children, for example, upon extensive application, and rarely occurs in adults with certain dispositions.
Case Report
We report the case of a 71-year-old man who developed methemoglobinemia and systemic intoxication upon topical application of EMLA cream for leg ulcer and stasis dermatitis prior to surgical debridement. Approximately 45 min after application, the patient was found to be in a somnolent state, was unable to articulate, and showed peripheral cyanosis. The blood concentration of methemoglobin (MetHb) was 15.1%, and therefore, a diagnosis of systemic toxicity of EMLA due to methemoglobinemia was established. After removal of the cream, oxygen was applied, and further observation revealed that the patient’s condition rapidly improved without any residue. In the following, we also discuss literature related to systemic EMLA intoxication.
Conclusion
EMLA cream may cause severe systemic toxicity even in adults under certain conditions, for example, when applied on damaged skin or in extensive amounts.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
A case of severe systemic intoxication and methemoglobinemia resulting from the topical application of an eutectic mixture of local anesthetics (EMLA) cream on a leg ulcer is described. |
In this case, systemic toxicity resulted from the mistaken large-scale application of EMLA under occlusion on the damaged skin and stasis dermatitis. |
EMLA cream is considered safe in adults, with cases of systemic toxicity almost exclusively linked to hair removal. |
The present case illustrates that the risk factors for systemic intoxication with EMLA should be considered when applied to damaged skin. |
Introduction
The systemic toxicity of the Eutectic Mixture of Local Anesthetics (EMLA) cream is mediated by the active ingredients of the cream, the local anesthetics lidocaine and prilocaine, which are both present at a concentration of 2.5%. Systemic toxicity of EMLA may manifest as seizures, mainly due to systemic lidocaine intoxication [1], methemoglobinemia resulting from the oxidizing properties of prilocaine, and cyanosis. Therefore, a saturation gap between pulse oximeter oxygen saturation and arterial blood gas saturation exceeding 5% may occur, as traditional pulse oximetry fails to account for methemoglobin (metHb), leading to inaccurately elevated saturation values. This also hinders any improvement in pulse oximetry despite the application of oxygen. At higher concentrations, a chocolate-like color of the blood may be observed. Risk factors for methemoglobinemia due to local anesthetic intoxication include early age, the use of high quantities of drugs over an extended area, repeated application, and mutual intake of other drugs, such as celecoxib. Moreover, skin diseases involving an impaired skin barrier increase the possibility of intoxication. Such skin conditions include eczema, psoriasis, vascular malformation, molluska contagiosa and laser hair removal. Finally, glucose-6-phosphate dehydrogenase deficiency is also known to increase the likelihood of methemoglobinemia. Therapy for intoxication includes high-flow oxygen application, monitoring, and, in severe cases, intravenous application of methylene blue. We present a case of EMLA intoxication in a patient treated for a leg ulcer. Written informed consent was obtained from the patient for publication of this case report and any accompanying images.
Case Report
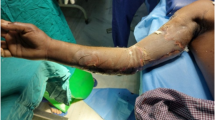
A 71-year-old male was admitted for inpatient treatment of a leg ulcer and concomitant stasis dermatitis primarily caused by arthrosis and immobility (Fig. 1). The patient did not take any medication. However, he had a Gram-negative foot and leg infection and internal secondary diagnoses, including lung emphysema, euthyroid sick syndrome, and renal failure due to immobility in the previous year. Otherwise, the patient presented as a healthy individual and was adequately oriented to all qualities, with no circulation problems in the legs, other metabolic previous illnesses or known genetic deficiencies or family history thereof. Epicutaneous patch testing and phlebological investigation did not reveal pathological findings.
Prior to surgical debridement of the ulcer, the application of EMLA cream as local anesthesia was ordered. By mistake, EMLA cream was applied occlusively not only to the ulcer but also to the entire lower leg and foot. After 45 min, the patient was found to be in a somnolent state. He was unable to articulate, had a Glasgow Coma Scale index of 11, and showed peripheral cyanosis. The occlusive dressing with EMLA cream was immediately removed, oxygen was administered, and the patient was transferred to the university emergency unit. His MetHb blood concentration was 15.1%, and his oxygen saturation was 91%. The MetHb concentration decreased to 7% after 8 h and to 1% after 24 h. The patient’s condition rapidly improved without any residue (Fig. 2).
Discussion
We present the uncommon case of methemoglobinemia and systemic toxicity resulting from large-scale application of EMLA cream on the lower leg prior to wound debridement. EMLA cream is widely used for local anesthesia before small superficial surgeries. Its safety has already been studied, and several reports have demonstrated the safety of this cream, especially in the context of wound debridement [2]. However, several cases of intoxication have been reported, both for children and adults [1, 3]. In the following, selected cases will be displayed, and the safety and correct usage of EMLA cream will be discussed.
Approximately two-thirds of the reported cases of EMLA cream intoxication involved children. The most common cause of intoxication is exposure prior to circumcision [4,5,6,7,8]. Symptoms reported included lethargy, cyanosis, and cardiopulmonary instability. Other common causes reported in children include application prior to catheter insertion or punctation [9,10,11,12]; omission of removing EMLA cream, long duration of application [11, 12]; molluscum contagiosum removal [13,14,15,16,17]; underlying skin conditions with an impaired skin barrier such as eczema [13, 16]; other small interventions, such as allergy skin testing, including application over an extensive area of skin [18]; and accidental ingestion of EMLA cream, resulting in status epilepticus in a 25-month-old child [19].
In adults, the use of an EMLA cream is considered safe, and cases of systemic toxicity are almost exclusively linked to hair removal [1, 20,21,22,23,24,25]. Patients who present with systemic EMLA intoxication often have risk factors, including a damaged skin barrier due to previous treatments and the application of inappropriately high amounts of EMLA over an extended area of the skin, e.g., both legs or even the back and all four extremities [23]. However, even for patients whose face was treated for a limited amount of time (25 cm2 for 30 min), there are reports of cyanosis and collapse [22]. For higher doses of local anesthetics in creams applied in the context of laser-assisted hair removal, deaths have even been reported, resulting in an Food and Drug Administration (FDA) warning for skin numbing cream in 2007 [26, 27].
The package instructions for the EMLA cream include the use of 1 g of cream for an area of 10 cm2, for a total of 10 g under occlusion. It is also advised to refrain from using EMLA cream for skin rash or eczema. Common local side effects also include purpura, skin paleness, or minor allergic reactions [28, 29].
There is a limited body of evidence concerning the absorption of active agents from the EMLA through the skin. One study investigated the absorption and suitability of EMLA for the treatment of second-degree burns [30]. Here it could be shown that prilocaine for second-degree burns has a bioavailability of up to 30%, making the possibility of intoxication unlikely. This underlines the importance of avoiding the use of EMLA cream on eczematous skin, as there might be a similar impairment of the skin barrier and therefore greater absorption.
While there are few reported cases of EMLA intoxication, it is possible that some cases were overlooked. For example, in our patient, the primary consideration was a diagnosis of exsiccation under the motto “common things are common.” In such situations, the ongoing use of occlusive EMLA dressings might be easily missed. Therefore, in our opinion, it is important to raise awareness of this issue.
Conclusions
Caution should be taken when applying EMLA cream to leg ulcers. It is important to recognize that this medication functions similarly to the injection of local anesthetics and can also lead to systemic toxicity.
Data Availability
Data sharing does not apply to this article, as no datasets were generated.
References
Shamriz O, Cohen-Glickman I, Reif S, Shteyer E. Methemoglobinemia induced by lidocaine-prilocaine cream. Isr Med Assoc J. 2014;16:250–4 (PMID: 24834764).
Blanke W, Hallern BV. Sharp wound debridement in local anesthesia using EMLA cream: 6 years’ experience in 1084 patients. Eur J Emerg Med. 2003;10:229–31. https://doi.org/10.1097/00063110-200309000-00014.
Tran AN, Koo JY. Risk of systemic toxicity with topical lidocaine/prilocaine: a review. J Drugs Dermatol. 2014;13(9):1118–22 (PMID: 25226014).
Kumar AR, Dunn N, Naqvi M. Methemoglobinemia associated with a prilocaine-lidocaine cream. Clin Pediatr (Phila). 1997;36(4):239–40. https://doi.org/10.1177/000992289703600410. (PMID: 9114997).
Couper RT. Methaemoglobinaemia secondary to topical lignocaine/prilocaine in a circumcised neonate. J Paediatr Child Health. 2000;36(4):406–7. https://doi.org/10.1046/j.1440-1754.2000.00508.x. (PMID: 10940184).
Kuiper-Prins E, Kerkhof GF, Reijnen CG, van Dijken PJ. A 12-day-old boy with methemoglobinemia after circumcision with local anesthesia (Lidocaine/Prilocaine). Drug Saf Case Rep. 2016;3(1):12. https://doi.org/10.1007/s40800-016-0033-9. (PMID: 27747692; PMCID: PMC5035648).
Kjellgard C, Westphal S, Flisberg A. Överdos av prilokain/lidokain kan ge svår methemoglobinemi - Tre fall där krämen gett toxiska effekter hos spädbarn (Intoxication with prilocaine/lidocaine can cause serious methemoglobinemia). Lakartidningen. 2019;116:FPFT (in Swedish; PMID: 31573668).
Woo NL, Cherian S, Heaney M, Wahl G. Methaemoglobinaemia secondary to topical prilocaine toxicity: a cautionary circumcision tale. J Paediatr Child Health. 2021;57(1):149–50. https://doi.org/10.1111/jpc.14841. (PMID: 32129535).
Jakobson B, Nilsson A. Methemoglobinemia associated with a prilocaine-lidocaine cream and trimetoprim-sulphamethoxazole: a case report. Acta Anesthesiol Scand. 1985;29(4):453–5. https://doi.org/10.1111/j.1399-6576.1985.tb02232.x. (PMID: 4013630).
Sinisterra S, Miravet E, Alfonso I, Soliz A, Papazian O. Methemoglobinemia in an infant receiving nitric oxide after the use of eutectic mixture of local anesthetic. J Pediatr. 2002;141(2):285–6. https://doi.org/10.1067/mpd.2002.125732. (PMID: 12183731).
Shachor-Meyouhas Y, Galbraith R, Shavit I. Application of topical analgesia in triage: a potential for harm. J Emerg Med. 2008;35(1):39–41. https://doi.org/10.1016/j.jemermed.2007.07.071. (PMID: 18281179).
Khan A, Eldos Y, AlAnsari KM. Acquired methemoglobinemia in an infant: consequence of prolonged application of eutectic mixture of local anesthetics (EMLA) cream for spontaneous abscess drainage. Cureus. 2022;14(11): e31304. https://doi.org/10.7759/cureus.31304. (PMID: 36398037; PMCID: PMC9646534).
Capron F, Perry D, Capolaghi B. Crise convulsive et méthémoglobinémie après application de crème anesthésique (convulsive crisis and methemoglobinemia after the application of anesthetic cream). Arch Pediatr. 1998;5(7):812. https://doi.org/10.1016/s0929-693x(98)80074-2. (in French; PMID: 9759285).
Rincon E, Baker RL, Iglesias AJ, Duarte AM. CNS toxicity after topical application of EMLA cream on a toddler with molluscum contagiosum. Pediatr Emerg Care. 2000;16(4):252–4. https://doi.org/10.1097/00006565-200008000-00009. (PMID: 10966344).
Touma S, Jackson JB. Lidocaine and prilocaine toxicity in a patient receiving treatment for molluska contagiosa. J Am Acad Dermatol. 2001;44(2 Suppl):399–400. https://doi.org/10.1067/mjd.2001.111898. (PMID: 11174427).
Schmitt C, Matulic M, Kervégant M, Tichadou L, Boutin A, Glaizal M, de Haro L. Méthémoglobinémie après application de crème Emla® chez un enfant : circonstances et conséquences d’un surdosage (Methaemoglobinaemia in a child treated with Emla® cream: circumstances and consequences of overdose). Ann Dermatol Venereol. 2012;139(12):824–7. https://doi.org/10.1016/j.annder.2012.06.035. (PMID: 23237281).
Cho YS, Chung BY, Park CW, Kim HO. Seizures and methemoglobinemia after topical application of eutectic mixture of lidocaine and prilocaine on a 3.5-year-old child with molluscum contagiosum and atopic dermatitis. Pediatr Dermatol. 2016;33(5):e284–5. https://doi.org/10.1111/pde.12927. (PMID: 27397059).
Parker JF, Vats A, Bauer G. EMLA toxicity after application for allergy skin testing. Pediatrics. 2004;113(2):410–1. https://doi.org/10.1542/peds.113.2.410. (PMID: 14754960).
McMahon K, Paster J, Baker KA. Local anesthetic systemic toxicity in the pediatric patient. Am J Emerg Med. 2022;54:325.e3-325.e6. https://doi.org/10.1016/j.ajem.2021.10.021. (PMID: 34742600).
Brosh-Nissimov T, Ingbir M, Weintal I, Fried M, Porat R. Central nervous system toxicity following topical skin application of lidocaine. Eur J Clin Pharmacol. 2004;60(9):683–4. https://doi.org/10.1007/s00228-004-0814-4. (PMID: 15568142).
Hahn IH, Hoffman RS, Nelson LS. EMLA-induced methemoglobinemia and systemic topical anesthetic toxicity. J Emerg Med. 2004;26(1):85–8. https://doi.org/10.1016/j.jemermed.2003.03.003. (PMID: 14751483).
Elsaie ML. Cardiovascular collapse developing after topical anesthesia. Dermatology. 2007;214(2):194. https://doi.org/10.1159/000098877. (PMID: 17341877).
Esteban-Sánchez M, Izquierdo-Gil A, Hurtado-Gómez MF. Metahemoglobinemia secundaria a la administración tópica del anestésico local para depilación láser (Methaemoglobinaemia due to topical administration of local anesthetic for laser depilation). Farm Hosp. 2013;37(6):559–61. https://doi.org/10.7399/FH.2013.37.6.969. (in Spanish; PMID: 24256021).
Caré W, Larabi IA, Langrand J, Medernach C, Alvarez JC, Villa A. Poisoning associated with inappropriate use of a eutectic mixture of lidocaine and prilocaine before laser-assisted hair removal: approximately 3 cases. Int J Legal Med. 2019;133(3):843–6. https://doi.org/10.1007/s00414-018-1858-9. (PMID: 29785585).
Lerner RP, Lee E. EMLA-induced methemoglobinemia after laser-assisted hair removal procedure. Am J Emerg Med. 2019;37(11):2119.e1-2119.e2. https://doi.org/10.1016/j.ajem.2019.158415. (PMID: 31477356).
Torjesen, I. Minimizing the risk of lidocaine toxicity. Dermatology times, 2018.
Staff. FDA alerts public about danger of skin-numbing products. US Pharm. 2009;34(3):14.
de Waard-van der Spek FB, Oranje AP. Purpura caused by Emla is of toxic origin. Contact Dermat. 1997;36(1):11–3. https://doi.org/10.1111/j.1600-0536.1997.tb00915.x. (PMID: 9034681).
Kluger N, Raison-Peyron N, Michot C, Guillot B, Bessis D. Acute bullous irritant contact dermatitis caused by EMLA® cream. Contact Dermatitis. 2011;65(3):181–3. https://doi.org/10.1111/j.1600-0536.2011.01944.x. (PMID: 21827512).
Lillieborg S, Aanderud L. EMLA anesthetic cream for debridement of burns: a study of plasma concentrations of lidocaine and prilocaine and a review of the literature. Int J Burns Trauma. 2017;7(6):88–97 (PMID: 29119061; PMCID: PMC5665840).
Acknowledgements
We thank the patient for agreeing to publication of this case.
Medical Writing/Editorial Assistance. The Springer Nature Research Editing Service, an AI program, was applied to improve the writing style.
Funding
No funding or sponsorship was received for this study or publication of this article. The Rapid Service Fee was funded by the authors.
Author information
Authors and Affiliations
Contributions
Sarah Marie Hoffmann, Anna Luisa Hartmann, and Christoph Mathis Schempp were responsible for the patient during his dermatological inpatient stay. The authors had full access to all of the patient data. Pablo Nieratschker and Michael Berthold Mussler took care of the patient at the emergency unit and detected methemoglobinemia; all the authors take responsibility for the integrity of the data and were involved in the interpretation of the data, drafting of the manuscript, and critical revision of the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
Sarah Marie Hoffmann, Anna Luisa Hartmann, Pablo Nieratschker, Michael Berthold Mussler, and Christoph Mathis Schempp declare that they have no conflicts of interest to disclose.
Ethical Approval
Given that this was a single case report, ethics committee approval was not needed. Written informed consent was obtained from the patient for publication of this case report and accompanying images.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Hoffmann, S.M., Hartmann, A.L., Nieratschker, P. et al. Acute Systemic Toxicity Caused by Topical Application of EMLA Cream on a Leg Ulcer: Case Report and Review of Literature. Dermatol Ther (Heidelb) 14, 1057–1062 (2024). https://doi.org/10.1007/s13555-024-01139-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13555-024-01139-7