Abstract
Introduction
When assessing the effect of a therapy for psoriasis (PsO), it is important to consider speed of response and cumulative response. However, responses among biologics may differ by body regions. This post hoc analysis compares speed of response and cumulative response for ixekizumab (IXE), an interleukin-17A antagonist, and guselkumab (GUS), an interleukin-23p19 inhibitor, in different body regions of patients with moderate-to-severe plaque PsO participating in the IXORA-R study, up to week 24.
Methods
The IXORA-R design has been previously described. Patients received the respective on-label dosing of IXE or GUS. The median time to first Psoriasis Area and Severity Index (PASI) 50, 75, 90, and 100 response (50%, 75%, 90%, and 100% improvement from baseline, respectively) and the cumulative days with clear skin for PASI 50, 75, 90, and 100 responses were assessed in four body regions: head, trunk, upper extremities, and lower extremities.
Results
A total of 1027 patients were enrolled and received IXE (N = 520) or GUS (N = 507). Median time to first PASI 50, 75, 90, and 100 response was shortest in the head region, followed by the remaining body regions in both IXE and GUS cohorts. In each body region, IXE was significantly faster than GUS (p < 0.001) in achieving PASI 50, 75, 90, and 100. Through 24 weeks, the number of days with clear skin for PASI 90 and 100 was greater in the head region, followed by trunk, upper extremities, and lastly lower extremities in both IXE and GUS cohorts. In each body region, through 24 weeks, patients on IXE experienced a significantly higher number of days with clear skin for PASI 50, 75, 90, and 100 than patients on GUS (p < 0.01).
Conclusions
As compared to GUS, IXE provided a faster skin clearance and more days with clear skin in all body regions of patients with moderate-to-severe plaque PsO through 24 weeks.
Trial Registration Number
https://www.clinicaltrials.gov/: NCT03573323 (IXORA-R).
Plain Language Summary
Psoriasis, a long-term, inflammatory skin disease, impacts patient’s lives, and response to treatment varies depending on the body region affected. Here, we assessed the speed of response and cumulative response through 24 weeks in different body regions (head, trunk, upper extremities, and lower extremities) of patients with moderate-to-severe plaque psoriasis treated with currently approved therapies: ixekizumab (IXE), an interleukin-17A antagonist, or guselkumab (GUS), an interleukin-23p19 inhibitor. We calculated the speed of response as the number of weeks to achieve first skin clearance, based on the Psoriasis Area and Severity Index (PASI) tool, and the cumulative response as the number of days with clear skin throughout the 24-week period. We found that the head region achieved skin clearance fastest and had a higher number of days with clear skin compared to the trunk, upper extremities, and lower extremities, in both groups of patients treated with IXE or GUS. Compared to GUS, IXE provided faster skin clearance and a higher number of days with clear skin in all body regions. For example, the head region of patients treated with IXE, as compared to GUS, achieved complete skin clearance twofold faster and experienced 18.7% more days of complete skin clearance. In conclusion, treatment with IXE through 24 weeks provided a faster response and a higher cumulative response than treatment with GUS in all four body regions of patients with moderate-to-severe plaque psoriasis.
Similar content being viewed by others
Why carry out this study? |
Responses among biologics for the treatment of moderate-to-severe plaque psoriasis may differ by body region. |
In this post hoc analysis, we assessed and compared the response to ixekizumab (IXE), an interleukin-17A antagonist, versus guselkumab (GUS), an interleukin-23p19 inhibitor, in different body regions of patients enrolled in the IXORA-R study. |
What was learned from the study? |
In both the IXE and GUS cohorts, the speed of response and the cumulative response for Psoriasis Area and Severity Index (PASI) 100 (complete skin clearance) were higher in the head region, followed by the trunk, upper extremities, and lastly lower extremities. |
As compared to GUS, IXE provided a significantly faster response and a significantly higher cumulative response in all body regions. |
Digital Features
An interactive infographic provided for this article: https://vahub.lilly.com/gooderham_dermatologyandtherapy_2024.
Introduction
Psoriasis (PsO) is a chronic, lifelong, inflammatory skin disease that affects 3.0% of the US adult population [1] and an estimated 55.8 million adults worldwide [2]. The prevalence of PsO in children is lower than in adults, ranging from 0% in Taiwan to 2.1% in Italy [2]
The pathogenesis of PsO is thought to be related to an excessive activation of parts of the adaptive immune system [3]. Psoriatic lesions develop as a result of a complex interaction between cells and mediators of the immune system and skin epithelium and connective tissue [4]. For patients with mild PsO, topical treatments and/or targeted phototherapy are recommended. For patients with moderate-to-severe PsO or for patients with concurrent psoriatic arthritis, systemic treatments are recommended [3]. Specifically, biologic drugs and small molecules have become valuable options in recent years [5, 6].
PsO impacts multiple facets of a patient’s life [7]. This is reflected in the cumulative life course impairment, a concept that has been introduced to describe how the accumulation of physical, psychological, social, and economic burdens across a lifetime influence life-changing decisions and alter the course of the lives of many patients affected by PsO [8, 9]. Due to this, it is important to consider the cumulative benefits for patients when assessing the effect of a therapy for PsO. In addition to long-term efficacy, speed of response is also an important milestone when gauging therapeutic success, and it is a treatment goal for patients.
The efficacy and safety of ixekizumab (IXE), an interleukin (IL)-17A antagonist, and guselkumab (GUS), an IL-23p19 inhibitor, were assessed and compared in the IXORA-R head-to-head clinical trial. IXE was found to clear skin more rapidly and provide a greater cumulative benefit than GUS in patients with moderate-to-severe plaque PsO [10, 11].
Some areas of the body have additional impacts on patients’ quality of life [12]. For instance, patients with PsO in the scalp region have reported greater disease and itch severity and poorer health in comparison to patients with PsO affecting other body regions [13]. Likewise, some areas of the body respond faster to certain biologic therapies than other body regions [14,15,16,17].
The objective of this post hoc analysis is to compare speed of response and cumulative response by body regions for IXE versus GUS in patients with moderate-to-severe plaque PsO participating in the IXORA-R study, up to week 24.
Methods
Study Design
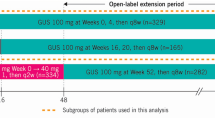
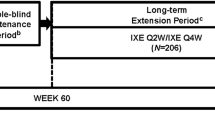
The study design of the phase IV, randomized, double-blind, head-to-head, multicenter IXORA-R clinical trial (ClinicalTrials.gov: NCT03573323) has been previously thoroughly described [10, 11]. Briefly, patients were randomly assigned 1:1 to receive subcutaneous injections of the respective on-label dosing of IXE or GUS. Specifically, patients on IXE received a 160-mg starting dose at week 0, followed by 80 mg every 2 weeks from weeks 2 to 12, and every 4 weeks thereafter. Patients on GUS received 100 mg at weeks 0, 4, 12, and 20.
The study protocol was approved by local ethics review boards (Electronic Supplementary Material Table S1) and was conducted according to the International Conference on Harmonization Good Clinical Practice guidelines and the Declaration of Helsinki. All patients were required to give informed consent for participation in the study.
Patient Population
Patients were enrolled in the trial if they were ≥ 18 years of age with chronic plaque PsO for at least 6 months before baseline, were a candidate for phototherapy and/or systemic therapy, and had a static Physician’s Global Assessment score ≥ 3, a Psoriasis Area and Severity Index (PASI) score ≥ 12, and a body surface area involvement ≥ 10% at screening and baseline.
Patients were excluded from the trial if they had a predominant pattern of pustular, erythrodermic, and/or guttate forms of PsO; a history of drug-induced PsO or a clinically significant flare of PsO during the 12 weeks before baseline; previous treatment with IL-23p19 antagonists (including GUS); concurrent or recent use of any biologic agent within the specified periods prior to baseline; previous treatment with IXE; or failure to respond to an IL-17 antagonist.
Outcomes
The PASI assesses the degree of skin area affected and the severity of skin disease in four body regions: the head (i.e., head, scalp, and neck), the trunk (i.e., chest, abdomen, back, axillae, and genitalia), the upper extremities (i.e., arms, hands, and palms, exclusive of nails), and the lower extremities (i.e., buttocks, legs, feet, and soles, exclusive of nails). A PASI improvement from baseline of 50%, 75%, 90%, and 100% is indicated as PASI 50, PASI 75, PASI 90, and PASI 100, respectively.
In this study, the speed of response was assessed as the median time to first PASI 50, 75, 90, and 100 responses in each body region, and the cumulative response was assessed as the number of days with clear skin for PASI 50, 75, 90, and 100 responses in each body region.
Statistical Analysis
The intent-to-treat population was analyzed through 24 weeks. The median time to first PASI 50, 75, 90, and 100 responses in each body region was calculated based on Kaplan–Meier analysis, and the treatment comparisons were performed using log-rank test. The cumulative days with clear skin for PASI 50, 75, 90, and 100 responses in each body region were calculated by the average number of days with PASI response up to the applicable time point and estimated by the percentage of the maximum area under the curve (AUC) over the total duration at that time point. The treatment comparisons were performed using the analysis of covariance (ANCOVA) adjusted for baseline PASI and pooled sites. Normality tests of continuous variables (e.g., PASI) have been carried out at the study level, as specified in the protocol of the IXORA-R study.
Missing data were imputed with non-responder imputation (NRI) for categorical variables, modified baseline observation carried forward (mBOCF) for continuous variables, and between visits extrapolation for patient-level AUC.
SAS version 9.4 software (SAS Institute, Cary, NC, USA) was used for statistical analysis.
Results
A total of 1027 patients were enrolled in the IXORA-R trial, among whom 520 received IXE and 507 received GUS.
Demographics and baseline characteristics were numerically similar across the two treatment arms (Table 1). The baseline mean (standard deviation [SD]) age was 49.0 (13.9) years for patients on IXE and 49.0 (14.9) years for patients on GUS, with almost two thirds of each treatment arm being males. The baseline mean (SD) PASI score was 19.5 (7.9) for patients on IXE and 19.3 (7.1) for patients on GUS. The regional baseline mean (SD) PASI score in patients treated with IXE versus GUS was highest in the lower extremities (8.9 [4.3] vs. 8.9 [3.9]), followed by trunk (5.3 [3.3] vs. 5.3 [3.2]), upper extremities (3.8 [1.9] vs. 3.6 [1.8]), and head (1.6 [1.2] vs. 1.6 [1.2]) (Table 1).
For the IXE treatment arm, the median time to first PASI 50, 75, 90, and 100 responses was shortest in the head region, followed by the trunk, upper extremities, and lastly the lower extremities (Fig. 1). Similarly, for the GUS treatment arm, the median time to first PASI 75, 90, and 100 responses was shortest in the head region, followed by the trunk, upper extremities, and lastly the lower extremities (Fig. 1). For the GUS treatment arm, however, the median time to first PASI 50 response was shortest in the head region, followed by all other body regions within a similar time frame (Fig. 1).
Median time to first PASI 50, 75, 90, and 100 responses by body regions (head, trunk, upper extremities, and lower extremities) in patients on IXE (N = 520) or GUS (N = 507). Data are presented as the median number of weeks with 95% CI. Asterisks indicate a statistically significant difference at ***p-value < 0.001 by the log-rank test. CI confidence interval, GUS guselkumab, IL interleukin, IXE ixekizumab, PASI Psoriasis Area and Severity Index. Interactive Infographic link: https://vahub.lilly.com/gooderham_dermatologyandtherapy_2024
In each body region, IXE was significantly faster than GUS (p < 0.001) in achieving PASI 50, 75, 90, and 100. Specifically, the median time to complete skin clearance (i.e., PASI 100) of the body regions in patients treated with IXE versus GUS was 4.1 versus 8.1 weeks (p < 0.001) in the head, 6.4 versus 10.1 weeks (p < 0.001) in the trunk, 8.1 versus 10.1 weeks (p < 0.001) in the upper extremities, and 10.1 versus 16.1 weeks (p < 0.001) in the lower extremities (Fig. 1).
In both IXE and GUS treatment arms, through 24 weeks, the number of days with clear skin for PASI 90 and PASI 100 was greatest in the head region, followed by the trunk, upper extremities, and lastly by the lower extremities (Fig. 2). Conversely, no substantial difference in the number of days with clear skin for PASI 50 and 75 was observed among body regions, in both treatment arms, through 24 weeks (Fig. 2).
Days of clear skin for PASI 50, 75, 90, and 100 responses by body regions (head, trunk, upper extremities, and lower extremities) in patients on IXE (N = 514) or GUS (N = 506) through 24 weeks. Data are presented as least-squares means with 95% CI. Asterisks indicate statistically significant differences at **p-value < 0.01 and ****p-value < 0.0001 by analysis of covariance. CI confidence interval, GUS guselkumab, IL interleukin, IXE ixekizumab, LSM least-squares mean, PASI Psoriasis Area and Severity Index.
In each body region, through 24 weeks, patients on IXE experienced a significantly higher number of days with clear skin for PASI 50, 75, 90, and 100 as compared to patients on GUS (p < 0.01). Specifically, the number of days with complete skin clearance (i.e., PASI 100) in patients treated with IXE versus GUS was 107.5 versus 90.6 days (p < 0.0001) in the head, 97.7 versus 83.9 days (p < 0.0001) in the trunk, 85.0 versus 75.6 days (p = 0.002) in the upper extremities, and 75.7 versus 59.8 days (p < 0.0001) in the lower extremities (Fig. 2).
Discussion
The impact of PsO on patients’ quality of life varies depending on the body region affected [12]. For instance, the head and the upper extremities are visible body regions and, therefore, their involvement has been reported to be associated with higher feelings of stigmatization and levels of social anxiety [18]. The trunk includes the genitals, and genital involvement has been shown to impact patients’ intimate relationships [19].
Consequently, it is important that PsO treatments achieve a rapid and cumulative response in all body regions, especially in those that carry a higher burden [20]. The speed of response of a biologic therapy for PsO has been seen to be an important factor in improving not only the quality of life and satisfaction of patients, but also the treatment persistence, perhaps because, among other factors [21, 22], it builds trust and confidence between the patient and the healthcare provider. The cumulative response of a biologic therapy for PsO is also a paramount factor in counterbalancing the cumulative life course impairment caused by PsO [8, 9].
This analysis examined the speed of response and cumulative response in the four body regions assessed by the PASI score, namely, the head, trunk, lower extremities, and upper extremities, and compared responses between two biologics currently approved for the treatment of moderate-to-severe PsO: IXE vs. GUS.
In terms of differences in body regions, in both groups of patients treated with IXE or GUS, skin clearance was achieved faster in the head region as compared to the remaining body regions. Specifically, the median time to achieve the first PASI 100 in the head region was approximately half of the median time required to achieve the first PASI 100 in the upper extremities (for IXE only) and in the lower extremities (for both IXE and GUS). This finding is in accordance with the authors’ clinical observations, data from real-world clinical practice [14], and data from other trials [15,16,17].
In a real-world retrospective study, Cheng et al. found that the head and upper extremities regions had the lowest PASI scores (PASI 75, 90, and 100) as compared to the lower extremities in patients with moderate-to-severe PsO who completed 2-year ustekinumab or secukinumab treatment [14].
Blauvelt et al. observed that the head and trunk of patients with moderate-to-severe PsO treated with IXE for 12 weeks responded more quickly than the upper and lower extremities, especially in terms of reduced scaling and thickness [15]. Similarly, Armstrong et al. reported that, in patients with moderate-to-severe PsO treated with adalimumab for 16 weeks, the trunk and head showed greater responses than the upper and lower extremities, as measured by regional PASI reduction from baseline [16]. Griffiths et al. also reported that, in patients with moderate-to-severe PsO treated with etanercept (50 mg once weekly for 24 weeks), the median time to PASI 75 was faster for the head and trunk (both 12 weeks), followed by upper and lower extremities (both 18 weeks). By week 24, ≥ 84% of patients achieved PASI 75 for the head region, whereas ≥ 64% achieved PASI 75 for the lower extremities [17].
In terms of treatment comparison, we found that patients treated with IXE experienced a significantly faster response and a significantly higher cumulative response, through 24 weeks, in all body regions as compared to patients treated with GUS.
When looking at the time to complete skin clearance, IXE was 2.0-fold faster than GUS in achieving PASI 100 in the head region, 1.6-fold faster in the trunk, 1.2-fold faster in the upper extremities, and 1.6-fold faster in the lower extremities. As compared to patients treated with GUS, patients receiving IXE had 18.7% more days of PASI 100 in the head region, 16.4% more days in the trunk, 12.4% more days in the upper extremities, and 26.5% more days in the lower extremities.
In light of the new frontier in PsO management which gravitates towards a personalized medicine [23], our findings are relevant and offer the foundation to tailor the PsO treatments based on the body region affected.
The main limitations of this study were: (1) the duration of 24 weeks; (2) the clinical trial population limiting generalizability; and (3) lack of a placebo control.
Conclusion
Skin clearance in the head region was achieved faster than in the trunk, upper extremities, and lower extremities in patients with moderate-to-severe plaque PsO treated with IXE (IL-17A antagonist) or GUS (IL-23p19 inhibitor). Patients treated with IXE experienced a significantly faster response with shorter time to first PASI 50, 75, 90, and 100 in all body regions as compared to patients treated with GUS. Also, patients treated with IXE experienced a significantly higher cumulative response, through 24 weeks, with more days of clear skin for PASI 50, 75, 90, and 100 in all body regions as compared to patients treated with GUS.
In conclusion, as compared to GUS, IXE provided a faster response and a higher cumulative response in all body regions of patients with moderate-to-severe plaque PsO.
Data Availability
Eli Lilly and Company provides access to all individual participant data collected during the trial, after anonymization, except for pharmacokinetic or genetic data. Data are available to request 6 months after the indication studied has been approved in the USA and EU and after primary publication acceptance, whichever is later. No expiration date of data requests is currently set once data are made available. Access is provided after a proposal has been approved by an independent review committee identified for this purpose and after receipt of a signed data sharing agreement. Data and documents, including the study protocol, statistical analysis plan, clinical study report, and blank or annotated case report forms, will be provided in a secure data sharing environment. For details on submitting a request, see the instructions provided at www.vivli.org.
References
Armstrong AW, Mehta MD, Schupp CW, et al. Psoriasis prevalence in adults in the United States. JAMA Dermatol. 2021;157(8):940–6.
Parisi R, Iskandar IYK, Kontopantelis E, et al. National, regional, and worldwide epidemiology of psoriasis: systematic analysis and modelling study. BMJ. 2020;369: m1590.
Armstrong AW. Pathophysiology, clinical presentation, and treatment of psoriasis. A review. JAMA. 2020;23(19):1945-60. https://doi.org/10.1001/jama.2020.4006.
Nestle FO, Kaplan DH, Barker J. Psoriasis. N Engl J Med. 2009;361(5):496–509.
Megna M, Camela E, Battista T, et al. Efficacy and safety of biologics and small molecules for psoriasis in pediatric and geriatric populations. Part I: focus on pediatric patients. Expert Opin Drug Saf. 2023;22(1):25–41.
Megna M, Camela E, Battista T, et al. Efficacy and safety of biologics and small molecules for psoriasis in pediatric and geriatric populations. Part II: focus on elderly patients. Expert Opin Drug Saf. 2023;22(1):43–58.
Armstrong AW, Schupp C, Wu J, et al. Quality of life and work productivity impairment among psoriasis patients: findings from the National Psoriasis Foundation survey data 2003–2011. PLoS ONE. 2012;7(12): e52935.
Warren RB. Cumulative life course impairment in psoriasis: patient perception of disease-related impairment throughout the life course. Br J Dermatol. 2011;164[Suppl 1]:1-14. https://doi.org/10.1111/j.1365-2133.2011.10280.x.
Kimball AB, Gieler U, Linder D, et al. (2010) Psoriasis: is the impairment to a patient’s life cumulative? J Eur Acad Dermatol Venereol. 2010;24:989–1004.
Blauvelt A, Leonardi C, Elewski B, et al. A head-to-head comparison of ixekizumab vs. guselkumab in patients with moderate-to-severe plaque psoriasis: 24-week efficacy and safety results from a randomized, double-blinded trial. Br J Dermatol. 2021;184(6):1047–58.
Blauvelt A, Papp K, Gottlieb A, et al. A head-to-head comparison of ixekizumab vs. guselkumab in patients with moderate-to-severe plaque psoriasis: 12-week efficacy, safety and speed of response from a randomized, double-blinded trial. Br J Dermatol. 2020;182(6):1348–58.
Sojević Timotijević Z, Majcan P, Trajković G, et al. The impact of changes in psoriasis area and severity index by body region on quality of life in patients with psoriasis. Acta Dermatovenerol Croat 2017;25(3):215–22.
Callis Duffin K, Mason MA, Gordon K, et al. Characterization of patients with psoriasis in challenging-to-treat body areas in the corrona psoriasis registry. Dermatology. 2021;237(1):46–55.
Cheng PS, Hou PC, Yang CC, et al. Variation of body regional responses to ustekinumab and secukinumab in psoriasis patients: a real-world retrospective study and literature review. Dermatol Ther. 2022;35:e15950.
Blauvelt A, Muram TM, See K, et al. Improvements in psoriasis within different body regions vary over time following treatment with ixekizumab. J Dermatol Treat. 2018;29(3):220–9.
Armstrong AW, Villanueva Quintero DG, Echeverría CM, et al. Body region involvement and quality of life in psoriasis: analysis of a randomized controlled trial of adalimumab. Am J Clin Dermatol. 2016;17(6):691–9.
Griffiths CE, Sterry W, Brock F, et al. Pattern of response in patients with moderate-to-severe psoriasis treated with etanercept. Br J Dermatol. 2015;172(1):230–8.
Łakuta P, Marcinkiewicz K, Bergler-Czop B, et al. Associations between site of skin lesions and depression, social anxiety, body-related emotions and feelings of stigmatization in psoriasis patients. Postepy Dermatol Alergol. 2018;35(1):60–6.
Kędra K, Janeczko K, Michalik I, et al. Sexual dysfunction in women and men with psoriasis: a cross-sectional questionnaire-based study. Medicina. 2022;58(10):1443.
Gorelick J, Shrom D, Sikand K, et al. Understanding treatment preferences in patients with moderate to severe plaque psoriasis in the USA: results from a cross-sectional patient survey. Dermatol Ther. 2019;9(4):785–97.
de la Cueva DP, Notario J, Ferrándiz C, et al. Expert consensus on the persistence of biological treatments in moderate-to-severe psoriasis. J Eur Acad Dermatol Venereol. 2019;33(7):1214–23.
Murage MJ, Tongbram V, Feldman SR, et al. Medication adherence and persistence in patients with rheumatoid arthritis, psoriasis, and psoriatic arthritis: a systematic literature review. Patient Prefer Adherence. 2018;12:1483–503.
Camela E, Potestio L, Fabbrocini G, et al. New frontiers in personalized medicine in psoriasis. Expert Opin Biol Ther. 2022;22(12):1431–3.
Acknowledgements
Eli Lilly and Company would like to thank the clinical trial participants and their caregivers, without whom this work would not be possible.
Medical Writing and Editorial Assistance
The authors would like to acknowledge Elsa Inman, PhD, MS, McKean-Matthew, MS, and Elisa Di Carlo, PhD, MS, employees of Eli Lilly and Company, for medical review, statistical review, and writing assistance, respectively.
Funding
This study was funded by Eli Lilly and Company, which contributed to study design, data collection, data analysis, data interpretation, manuscript preparation, and publication decisions (including Rapid Access Fees).
Author information
Authors and Affiliations
Contributions
All named authors (Melinda Gooderham, Ronald Vender, Jeffrey Crowley, H. Chih-Ho Hong, Meghan Feely, Alyssa Garrelts, Kyoungah See, Bruce Konicek and Lawrence Green) meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, had full access to all the data in this study, take responsibility for the integrity of data and accuracy of the data analysis, and have given their approval for this version to be published.
Corresponding author
Ethics declarations
Conflict of Interest
Melissa Gooderham has received honoraria, grants, and/or research funding as a speaker, investigator, advisory board member, data safety monitoring board member, and/or consultant for AbbVie, Amgen, Arcutis, Aristea, AnaptysBio, Apogee, Bausch Health, Boehringer Ingelheim, Dermira, Dermavant, Eli Lilly and Company, Galderma, GlaxoSmithKline, Janssen, Kyowa Kirin, LEO Pharma, MedImmune, Merck, Meiji, Moonlake, Novartis, Nimbus, Pfizer, Regeneron, Sanofi Genzyme, Sun Pharma, Takeda, Tarsus, UCB Pharma, Union, and Ventyx. Ron Vender has received grants, research support, speakers bureau funding, honoraria, and/or consulting fees from AbbVie, Actelion, Amgen, Aralez Bio, Arcutis, Bausch Health, Boehringer Ingelheim, Bristol Myers Squibb, Celgene, Centocor, Cipher Pharmaceuticals, Dermavant Dermira, Eli Lilly and Company, Galderma, GlaxoSmithKline, Janssen, KabiCare, LEO Pharma, Meiji Seika Pharma, Merck, Nimbus Therapeutics, Novartis, Paladin Labs, Pfizer, Regeneron, Sandoz, Sun Pharma, Takeda, UCB Pharma, and Viatris-Mylan. Jeffrey Crowley has received honoraria as a speaker and/or served as a consultant for AbbVie, Amgen, Arcutis, BMS, Eli Lilly and Company, Janssen, Novartis, Pfizer, Regeneron, Sanofi-Aventis, and Sun Pharma, and is an owner and employee of Bakersfield Dermatology, which has received grant and/or research support from AbbVie, Amgen, BMS, Celgene, Eli Lilly and Company, Janssen, Novartis, and Pfizer; he also serves on the Data Safety Monitoring Board for Cara Pharmaceuticals and Alumis. H. Chih-Ho Hong has been a speaker, investigator, advisory board member, and/or consultant for AbbVie, Amgen, Arcutis, Avillion, Bausch Health, Boehringer Ingelheim, Bristol Myers Squibb, Celgene, Cutanea, Dermavant, Dermira, DS Biopharma, Eli Lilly and Company, Evelo Biosciences, Galderma, GlaxoSmithKline, Incyte Corp., Janssen, LEO Pharma, MedImmune, Merck, Mirimar, Novartis, Pfizer, Regeneron, Sanofi Genzyme, Regeneron, Roche, and UCB Pharma. Meghan Feely is associate staff at Mount Sinai Hospital and has received grants and/or consulting fees from Aerolase, Castle Biosciences, CeraVe-L’Oréal, Galderma, Glow Recipe, La Roche-Posay-L’Oréal, Revian, Sonoma Pharmaceuticals, Sun Pharma, and Suneva Medical. Meghan Feely, Alyssa Garrelts, Kyoungah See, and Bruce Konicek are employees and shareholders of Eli Lilly and Company. Lawrence Green is an investigator, speaker, and/or consultant for AbbVie, Amgen, Arcutis, Dermavant, Eli Lilly and Company, Janssen, MC2 Therapeutics, Ortho Dermatologics, Sun Pharma, and UCB Pharma.
Ethical Approval
The study protocol was approved by local ethics review boards (Table S1) and was conducted according to the International Conference on Harmonization Good Clinical Practice guidelines and the Declaration of Helsinki. All patients were required to give informed consent for participation in the study.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Gooderham, M., Vender, R., Crowley, J. et al. Speed and Cumulative Responses According to Body Regions in Patients with Moderate-to-Severe Plaque Psoriasis Treated with Ixekizumab (Interleukin-17A Antagonist) versus Guselkumab (Interleukin-23p19 Inhibitor). Dermatol Ther (Heidelb) 14, 441–451 (2024). https://doi.org/10.1007/s13555-023-01075-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13555-023-01075-y