Abstract
Behçet’s disease (BD) is a systemic autoinflammatory vasculitis. It occurs predominantly in Turkey but very rarely in Europe. The clinical manifestations of BD involve the skin and mucosal membranes; cardiovascular, gastrointestinal and nervous systems; and the eyes and joints. A 26-year-old man was repeatedly hospitalized at the Department of Dermatology of the Medical University of Bialystok. He had a family history of family members' deaths from unknown cause and a long personal history of recurring headaches and nonspecific pain in the chest as well as a 2-year history of recurring painful erosions on the oral mucosa. Recently, before admission to hospital, another erosion had appeared on the scrotum, which rapidly evolved into a painful ulceration. The patient also presented a large erosion in the area of the right hip and acne lesions. He consulted doctors of different specialties and underwent laboratory and imaging tests. Considering the symptoms, BD was diagnosed. Azathioprine was introduced, along with topical treatment. Great improvement of the skin lesions was achieved. He was later admitted to the department a few times for follow-up visits and remains in good general condition. BD is an extremely rare disease in Europe, especially in Poland. The fact that BD is a rare disease outside Asia leads to lower awareness and the possibility of not considering it in the differential diagnosis. The great diversity of symptoms also causes difficulties in tracking this disease. The various manifestations of BD require a broad spectrum of additional tests and an interdisciplinary approach to the patient.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Behçet’s disease occurs predominantly in Asia, especially Turkey. In Europe, it is very rare, which leads to lower awareness and often failure to consider it in the differential diagnosis |
To the best of our knowledge, there have been only two cases of Behçet’s disease reported in Polish patients |
People’s migrations around the world may contribute to the more frequent occurrence of Behçet’s disease in Poland and Europe |
The diversity of symptoms also causes difficulties in matching all of the signs a patient presents and tracking the disease |
The various manifestations of Behçet’s disease also lead to a broad spectrum of additional tests and multispecialty consultations with an interdisciplinary approach to the patient |
Digital Features
This article is published with digital features, including a summary slide, to facilitate understanding of the article. To view digital features for this article go to https://doi.org/10.6084/m9.figshare.14541738.
Introduction
Behçet’s disease (BD) is a systemic autoinflammatory vasculitis that affects all types and sizes of blood vessels [1,2,3]. It occurs predominantly in countries located along the ‘Silk Road,’ an ancient trading route connecting Asia with Middle and Southern Europe—about 14–20 per 100,000 people—and the highest incidence is noted in Turkey (20–421/100,000) [2, 4]. In northern Europe, BD occurrence is estimated to be 0.3–4.9 per 100,000 [5]. BD is associated with HLA-51 (human leukocyte antigen B51) [4]. This antigen occurs much more frequently in patients with BD living along the Silk Road than in people without this disease or in other regions of the world [4]. The pathogenesis of BD is uncertain but it is suspected that the symptoms develop because of exposure to exogenic factors in genetically predisposed individuals [2]. The role of infectious as well as immunologic factors is taken into account, along with the presence of autoantibodies, especially anti-endothelial cell antibodies. Vascular disorders also play a key role in BD's manifestation [2, 6]. BD usually affects men more frequently than women, with the onset at 20–30 years old [4].
The range of clinical manifestations of BD is vast. BD affects the skin and mucosal membranes; cardiovascular, gastrointestinal and nervous systems; and the eyes and joints [7]. Moreover, patients with BD experience increased fatigue, depression, and anxiety [8]. An extraordinary phenomenon that can be observed in BD is also pathergy. Usually symptoms occur episodically, separated by periods of remission [7]. The clinical picture is essential for the diagnostic process.
The prognosis is dependent on the patient's sex, age and ethnicity and the type of manifestation. It is worse in young males, especially from the area of the Silk Road [7]. Poor prognosis is also associated with ocular, cardiovascular, nervous and gastrointestinal involvement [7]. The manifestation and severity of symptoms in individuals from non-endemic regions also depend on the primary origin of the patient [9].
Case Presentation
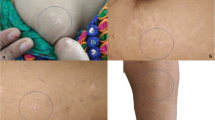
A 26-year-old man with a moderate extent of mental disability was admitted to the Department of Dermatology for diagnostics and treatment. He had a 2-year history of recurring painful erosions on the oral mucosa (about 3–7 times a year), recent history of rapidly evolving ulceration on the skin of the scrotum and a long history of recurring headaches and nonspecific pain in the chest. Physical examination revealed two ulcerations with necrotic bottoms on the skin of the scrotum (Fig. 1a), multiple aphtae on the oral mucosa (Fig. 2a) and one large erosion in the area of the right hip (Fig. 3a). Moreover, acne-like lesions were present on his face and back skin. The patient’s family history was also intriguing, since he reported an aortic aneurysm in his mother and death of unknown cause of his three brothers and mother’s sister at a young age. At the hospital, ophthalmologic and cardiologic consultations and laboratory tests revealed no significant abnormalities. Syphilis and HIV infection were also excluded. A laryngologist and dentist advised treatment of the oral aphtae and teeth. The patient underwent angio-CT of the chest and abdomen, which revealed no significant abnormalities and excluded aneurysms. Head MRI revealed small focal lesions in the white matter of the brain. Then, the examining neurologist noted only mild anisocoria but supported the suspicion of BD considering the whole clinical picture. The culture grown from the swab taken from the oral aphtae was negative, and the one taken from the genital lesions was positive for Escherichia coli. Azathioprine was introduced, first 50 mg and then 100 mg per day, along with topical treatment with silver, antiseptics and glucocorticoids as well as antibiotics (topical and systemic according to culture outcome). Great improvement of the skin lesions was achieved within only 1 month (Figs. 1b, 2b, 3b). Six months later, the patient experienced an episode of psychosis for which he was hospitalized at the Psychiatry Department and received zuclopenthixol and olanzapine. He has been treated in an ambulatory psychiatric care setting ever since. The patient was again admitted to the Department of Dermatology with a new erosion on the scrotum, which was successfully treated topically with glucocorticoids, and azathioprine was continued. Nine months later, the patient was again admitted to our department for a follow-up with no visible erosions or ulcerations but at that time features of Cushing syndrome were observed; therefore, the patient was referred to an endocrinologist who excluded hypercortisolemia. Three and 7 months later, the patient presented to the hospital again because of the recurrence of multiple oral aphtae. The patient is under constant and routine follow-up; he receives 100 mg per day of azathioprine and remains in good general condition with no skin involvement. He was referred to a doctor for genetic consultation. The patient provided informed written consent for the photographs and publication of this case report.
Discussion
BD is an extremely rare disease in Europe, especially in Poland. However, we diagnosed it in our patient, and it is possible that also other members of his family who had died from cardiovascular complications also suffered from BD. To the best of our knowledge, only two cases of BD in a Polish patient have been described [10, 11].
There is no single test that can confirm the diagnosis of BD [2]. It is made based on the clinical picture and simple exclusion of other diseases [7]. Diagnostic criteria for BD have been described. A main one that has to be met is recurrent oral ulcerations (at least three times a year), and there are others of which at least two have to be met: recurrent genital ulcerations (leaving scars), ocular lesions (anterior uveitis, posterior uveitis, presence of cells in the vitreous detected in the slit-lamp examination, retinal vasculitis), cutaneous lesions (erythema nodosum, pseudofolliculitis or papulopustular lesions, acneiform nodules in patients after adolescence and who are not using glucocorticoids) or positive pathergy test results with reading performed 24–48 h after the test [4]. In our patient we observed the main criterium as well as genital ulcerations, acne-like lesions and the pathergy phenomenon. Laboratory investigations in BD can reveal elevated levels of inflammatory markers such as CRP (C-reactive protein), erythrocyte sedimentation rate, white blood cells and serum inflammatory cytokines. Anemia due to chronic disease can also be noted. What is not typically observed in BD are antinuclear antibodies (ANA), rheumatoid factor (RF) and antineutrophil cytoplasmic antibodies (ANCA) [7]. Indeed, in the described case, ANA, ANCA and RF stayed within normal limits. Imaging tests can be helpful but due to the broad range of manifestations of BD, they should be adjusted to the presented symptoms.
As mentioned, BD can involve many bodily organs and systems. The most common first manifestation of this disease is lesions in the oral cavity, whereas the most common manifestation in general is genital lesions. The mentioned skin and mucosal symptoms are both recurrent painful erosions and ulcerations [7]. Other dermatologic disorders can be acne-like, folliculitis-like or erythema nodosum. Oral aphthae should be differentiated from conventional aphthae, recurrent aphthae stomatitis, pemphigus vulgaris, herpes simplex, deep fungal infections, syphilis and trauma-related lesions [12, 13]. Genital ulcerations should be differentiated from syphilis, herpes simplex, chancroid, lymphogranuloma venereum and sexual trauma [14]. Acne-like lesions in BD are slightly different from classic acne vulgaris since they involve sterile pustules and comedones are usually absent: the lesions frequently occur on the trunk, buttocks and extremities [4, 12]. As for erythema nodosum in BD, the microscopic picture of the skin sample may help to distinguish it from the classic erythema because of the presence of vasculitis [4]. Skin ulceration should be distinguished from pyoderma gangrenosum—probably the most famous disease associated with the pathergy phenomenon [15]. Joint involvement manifests as painful inflammation usually of the knee, ankle, elbow or wrist joints, but with no erosions or deformation. Ocular complications usually appear a few years after skin symptoms and can be diverse, even leading to blindness. BD can also affect the gastrointestinal, cardiovascular and nervous systems. Intestinal mucosal erosions can be present as well as vomiting and diarrhea—these were not observed in our patient. Cardiovascular manifestations may be superficial or include deep thrombophlebitis, cardiomyositis and pericarditis or—as in our patient’s mother, and possibly also other family members, but not in the patient—aneurysms. The most common neurologic symptom in BD is headaches, and in the described case they had persisted for many years [7]. Headaches in BD are usually the primary type, especially migraines and tension type. Among secondary headaches, the most frequent is due to cerebral venous thrombosis and the second to parenchymal abnormalities [16]. The characteristics of our patient’s headaches were not precisely established because of his mental disability but small focal lesions in the white matter of the brain were found, which could suggest the parenchymal type of neurologic BD manifestation. Psychotic episodes can also appear in BD, and in our patient one occurred after the first hospitalization [7]. In general, our patient would have obtained a good prognosis, since he presented with oral, genital and cutaneous lesions with no other systems involved, except for the nervous system disturbances.
The pathergy phenomenon is observed with different frequencies depending on the ethnicity of the patient. It is usually observed in individuals from areas of high BD prevalence and is estimated to be positive in about 70% of cases [2]. It manifests as the appearance of skin lesions at the site of a minor or non-severe trauma [7]. It was also observed in our patient, especially in the area that was compressed by too tight underwear (Fig. 3a).
There is no causal therapy for BD. Treatment depends on the clinical manifestation, severity of symptoms, age, gender and possible contraindications to particular drugs [4, 17]. Various medicines are proposed, usually anti-inflammatory and immunosupressive agents: glucocorticoids, colchicine, cyclosporin A, azathioprine, dapsone, mycophenolate mofetil or cyclophosphamide [4]. Another promising group of drugs is biologics, such as tumor necrosis factor (TNF) alfa inhibitors and interferon (INF) alfa [4]. According to the literature, anti-TNF alfa agents may be beneficial in BD with ocular, vascular, neurologic and gastrointestinal involvement in cases that are refractory to standard immunosuppressive drugs. IL-1 and IL-6 blocking agents may be effective in ocular and neurologic manifestations. Also, apremilast, a phosphodiesterase 4 inhibitor, can be considered for oral and genital ulcerations. INF alfa is used in uveitis and neurologic symptoms [18]. Moreover, topical medicines play an important role in managing symptoms, mainly skin and mucosal manifestations. These are topical glucocorticoids, antibiotics and antiseptics [17]. Lastly, there is concern about whether to administer anticoagulants or not, considering the vascular complications [17].
Behçet’s disease is very uncommon in locations other than Asia and along the Silk Road. The fact that there have only been a few cases of BD in Polish patients leads to lower awareness, and it is often not considered in the differential diagnosis. People’s migrations around the world may contribute to the more frequent occurrence of BD in Poland and Europe. The diversity of symptoms also causes difficulties in matching all of the signs that the patient presents and tracking the disease. The various manifestations of BD also lead to a broad spectrum of additional tests being carried out and multispecialty consultations with an interdisciplinary approach to the patient with medical surveillance.
References
Leccese P, Ozguler Y, Christensen R, Esatoglu SN, Bang D, Bodaghi B, Celik AF, et al. Management of skin, mucosa and joint involvement of Behçet’s syndrome: a systematic review for update of the EULAR recommendations for the management of Behçet’s syndrome. Semin Arthritis Rheum. 2019;48:752–62.
Bulur I, Onder M. Behçet disease: new aspects. Clin Dermatol. 2017;35:421–34.
Hu YC, Chiang BL, Yang YH. Clinical manifestations and management of pediatric Behçet’s disease. Clin Rev Allergy Immunol. 2020;7:1–10.
Scherrer M, Rocha V, Garcia L. Behçet’s disease: review with emphasis on dermatological aspects. An Bras Dermatol. 2017;92:452–64.
Mahr A, Maldini C. Epidemiology of Behçet’s disease. La Revue de Medecine Interne. 2014;35:81–9.
Balta S, Balta I, Ozturk C, Celik T, Iyisoy A. Behçet’s disease and risk of vascular events. Curr Opin Cardiol. 2016;31:451–7.
Zeidan MJ, Saadoun D, Garrido M, Klatzmann D, Six A, Cacoub P. Behçet’s disease physiopathology: a contemporary review. Auto Immun Highlights. 2016;7:4.
Davatchi F. Behçet’s disease. Int J Rheum Dis. 2018;21:2057–8.
Leccese P, Yazici Y, Olivieri I. Behcet’s syndrome in nonendemic regions. Curr Opin Rheumatol. 2017;29:12–6.
Niedzielska A, Chelminska K, Jaremin B. Behcet’s disease—diagnostic difficulties. Pol Arch Med Wewn. 2007;117:427–9.
Romańska-Gocka K, Gocki J, Placek W, et al. Behcet’s disease—case report and literature review. Adv Dermatol Allergol. 2009;26:224–8.
Alpsoy E, Zouboulis CC, Ehrlich GE. Mucocutaneous lesions of Behcet’s disease. Yonsei Med J. 2007;48:573–85.
Fitzpatrick SG, Cohen DM, Clark AN. Ulcerated lesions of the oral mucosa: clinical and histologic review. Head Neck Pathol. 2019;13:91–102.
Roett MA. Genital ulcers: differential diagnosis and management. Am Fam Phys. 2020;101:355–61.
George C, Deroide F, Rustin M. Pyoderma gangrenosum—a guide to diagnosis and management. Clin Med (Lond). 2019;19:224–8.
Vinokur M, Burkett JG. Headache in Behçet’s disease. Curr Pain Headache Rep. 2020;24:50.
Karadag O, Bolek EC. Management of Behcet’s syndrome. Rheumatology. 2020;59:108–17.
Ozguler Y, Hatemi G. Management of Behçet’s syndrome. Curr Opin Rheumatol. 2016;28:45–50.
Acknowledgements
We thank the patient for his consent for participation.
Funding
This case report required no funding during its preparation. The Medical University of Bialystok, Poland, supported the study and the journal’s rapid service fee.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this article, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Authors' Contributions
J.N.: conceptualization, original draft writing and editing; A.B.: editing, supervision; J.A.K.; editing; I.F.: head of the Department, supervision.
Disclosures
Julia Nowowiejska, Anna Baran, Julita A. Krahel and Iwona Flisiak have nothing to disclose.
Compliance with Ethics Guidelines
The patient provided an informed written consent for publication. A copy of the consent form is available for review by the Editor.
Data Availability
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Nowowiejska, J., Baran, A., Krahel, J.A. et al. Behçet’s Disease in a Polish Patient: A Case Report. Dermatol Ther (Heidelb) 11, 1435–1441 (2021). https://doi.org/10.1007/s13555-021-00551-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13555-021-00551-7