Abstract
Purpose
Pancreatic ductal adenocarcinoma (PDAC) is a highly aggressive disease with limited therapeutic options. The diversity and composition of the intratumoral microbiota are associated with PDAC outcomes, and modulating the tumor microbiota has the potential to influence tumor growth and the host immune response. Here, we explore whether intervention with butyrate-producing probiotics can limit PDAC progression.
Methods
Based on the TCGA (PAAD) database, we analyzed the differential communities of intratumoral microbiota in PDAC patients with long survival and short survival and explored the relevant mechanisms of Clostridium butyricum and its metabolite butyrate in the treatment of PDAC. Treatment with Clostridium butyricum or butyrate in combination with the ferroptosis inducer RSL3 in a PDAC mouse model has an inhibitory effect on PDAC progression. The potential molecular mechanisms were verified by flow cytometry, RNA-seq, Western blotting, qRT‒PCR and immunofluorescence.
Results
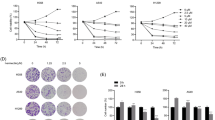
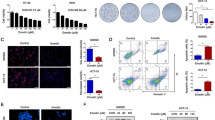
We found that the tumoral butyrate-producing microbiota was linked to a better prognosis and less aggressive features of PDAC. Intervention with Clostridium butyricum or its metabolite butyrate triggered superoxidative stress and intracellular lipid accumulation, which enhanced ferroptosis susceptibility in PDAC.
Conclusion
Our study reveals a novel antitumor mechanism of butyrate and suggests the therapeutic potential of butyrate-producing probiotics in PDAC.






Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request (GSE227418).
References
P. Rawla, T. Sunkara, V. Gaduputi, Epidemiology of pancreatic cancer: global trends, etiology and risk factors. World J. Oncol. 10, 10–27 (2019)
A. Rebelo, C.W. Michalski, J. Ukkat, J. Kleeff, Pancreatic cancer surgery with vascular resection: current concepts and perspectives. J. Pancreatol. 2, 1–5 (2019)
W. Wu, G. Jin, C. Wang, Y. Miao, H. Wang, W. Lou, X. Yu, B. Sun, H. Li, R. Qin, Z. Wu, W. Wang, K. Xu, L. Wang, T. Liang, C. Hao, H. Huang, Y. Li, G. Tan, Y. Zhao, J. Hao, Y. Wang, C. Peng, X. Liu, J. Ou, C. Yuan, X. Wang, Y. Yang, S. Cai, K. Guo, J. Jiang, X. Yu, J. Wei, F. Li, X. Wu and Y. Zhao, The current surgical treatment of pancreatic cancer in China: a national wide cross-sectional study. J. Pancreatol. 2, 16–21 (2019)
W. Wu, Q. Liu, J. Zhang, Y. Zhao, Survey on the current status of the diagnosis and treatment of pancreatic cancer in public tertiary hospitals in China: a cross-sectional questionnaire-based, observational study. J. Pancreatol. 4, 164–169 (2021)
L.D. Wood, M.B. Yurgelun, M.G. Goggins, Genetics of familial and sporadic pancreatic cancer. Gastroenterology 156, 2041–2055 (2019)
C.P. Zambirinis, G. Miller, Cancer manipulation of host physiology: lessons from pancreatic cancer. Trends Mol. Med. 23, 465–481 (2017)
J.L. Galeano Niño, H. Wu, K.D. LaCourse, A.G. Kempchinsky, A. Baryiames, B. Barber, N. Futran, J. Houlton, C. Sather, E. Sicinska, A. Taylor, S.S. Minot, C.D. Johnston, S. Bullman, Effect of the intratumoral microbiota on spatial and cellular heterogeneity in cancer. Nature. 611, 810–817 (2022)
B.A. Helmink, M.A.W. Khan, A. Hermann, V. Gopalakrishnan, J.A. Wargo, The microbiome, cancer, and cancer therapy. Nat. Med. 25, 377–388 (2019)
M. Stasiewicz, T.M. Karpiński, The oral microbiota and its role in carcinogenesis. Semin. Cancer Biol. 86, 633–642 (2022)
F. McAllister, M.A.W. Khan, B. Helmink, J.A. Wargo, The tumor microbiome in pancreatic cancer: bacteria and beyond. Cancer Cell 36, 577–579 (2019)
K. Hezaveh, R.S. Shinde, A. Klötgen, M.J. Halaby, S. Lamorte, M.T. Ciudad, R. Quevedo, L. Neufeld, Z.Q. Liu, R. Jin, B.T. Grünwald, E.G. Foerster, D. Chaharlangi, M. Guo, P. Makhijani, X. Zhang, T.J. Pugh, D.M. Pinto, I.L. Co, A.P. McGuigan, G.H. Jang, R. Khokha, P.S. Ohashi, G.M. O’Kane, S. Gallinger, W.W. Navarre, H. Maughan, D.J. Philpott, D.G. Brooks, T.L. McGaha, Tryptophan-derived microbial metabolites activate the aryl hydrocarbon receptor in tumor-associated macrophages to suppress anti-tumor immunity. Immunity 55, 324-340.e328 (2022)
E. Riquelme, Y. Zhang, L. Zhang, M. Montiel, M. Zoltan, W. Dong, P. Quesada, I. Sahin, V. Chandra, A. San Lucas, P. Scheet, H. Xu, S.M. Hanash, L. Feng, J.K. Burks, K.A. Do, C.B. Peterson, D. Nejman, C.D. Tzeng, M.P. Kim, C.L. Sears, N. Ajami, J. Petrosino, L.D. Wood, A. Maitra, R. Straussman, M. Katz, J.R. White, R. Jenq, J. Wargo, F. McAllister, Tumor microbiome diversity and composition influence pancreatic cancer outcomes. Cell. 178, 795–806.e712 (2019)
Y. Chen, S. Yang, J. Tavormina, D. Tampe, M. Zeisberg, H. Wang, K.K. Mahadevan, C.J. Wu, H. Sugimoto, C.C. Chang, R.R. Jenq, K.M. McAndrews, R. Kalluri, Oncogenic collagen I homotrimers from cancer cells bind to α3β1 integrin and impact tumor microbiome and immunity to promote pancreatic cancer. Cancer Cell 40, 818-834.e819 (2022)
S. Pushalkar, M. Hundeyin, D. Daley, C.P. Zambirinis, E. Kurz, A. Mishra, N. Mohan, B. Aykut, M. Usyk, L.E. Torres, G. Werba, K. Zhang, Y. Guo, Q. Li, N. Akkad, S. Lall, B. Wadowski, J. Gutierrez, J.A. Kochen Rossi, J.W. Herzog, B. Diskin, A. Torres-Hernandez, J. Leinwand, W. Wang, P.S. Taunk, S. Savadkar, M. Janal, A. Saxena, X. Li, D. Cohen, R.B. Sartor, D. Saxena, G. Miller, The Pancreatic Cancer Microbiome Promotes Oncogenesis by Induction of Innate and Adaptive Immune Suppression. Cancer Discov. 8, 403–416 (2018)
W. He, J. Wu, J. Shi, Y.M. Huo, W. Dai, J. Geng, P. Lu, M.W. Yang, Y. Fang, W. Wang, Z.G. Zhang, A. Habtezion, Y.W. Sun, J. Xue, IL22RA1/STAT3 signaling promotes stemness and tumorigenicity in pancreatic cancer. Cancer Res. 78, 3293–3305 (2018)
G.D. Poore, E. Kopylova, Q. Zhu, C. Carpenter, S. Fraraccio, S. Wandro, T. Kosciolek, S. Janssen, J. Metcalf, S.J. Song, J. Kanbar, S. Miller-Montgomery, R. Heaton, R. McKay, S.P. Patel, A.D. Swafford, R. Knight, Microbiome analyses of blood and tissues suggest cancer diagnostic approach. Nature 579, 567–574 (2020)
M. Vital, A.C. Howe, J.M. Tiedje, Revealing the bacterial butyrate synthesis pathways by analyzing (meta) genomic data. mBio 5, e00889 (2014)
L.T. Geller, M. Barzily-Rokni, T. Danino, O.H. Jonas, N. Shental, D. Nejman, N. Gavert, Y. Zwang, Z.A. Cooper, K. Shee, C.A. Thaiss, A. Reuben, J. Livny, R. Avraham, D.T. Frederick, M. Ligorio, K. Chatman, S.E. Johnston, C.M. Mosher, A. Brandis, G. Fuks, C. Gurbatri, V. Gopalakrishnan, M. Kim, M.W. Hurd, M. Katz, J. Fleming, A. Maitra, D.A. Smith, M. Skalak, J. Bu, M. Michaud, S.A. Trauger, I. Barshack, T. Golan, J. Sandbank, K.T. Flaherty, A. Mandinova, W.S. Garrett, S.P. Thayer, C.R. Ferrone, C. Huttenhower, S.N. Bhatia, D. Gevers, J.A. Wargo, T.R. Golub, R. Straussman, Potential role of intratumor bacteria in mediating tumor resistance to the chemotherapeutic drug gemcitabine. Science 357, 1156–1160 (2017)
M.K. Stoeva, J. Garcia-So, N. Justice, J. Myers, S. Tyagi, M. Nemchek, P.J. McMurdie, O. Kolterman, J. Eid, Butyrate-producing human gut symbiont, Clostridium butyricum, and its role in health and disease. Gut Microbes. 13, 1–28 (2021)
T.C. Kenny, M.L. Gomez, D. Germain, Mitohormesis, UPR(mt), and the complexity of mitochondrial DNA landscapes in cancer. Cancer Res. 79, 6057–6066 (2019)
K.C. Corn, M.A. Windham, M. Rafat, Lipids in the tumor microenvironment: From cancer progression to treatment. Prog. Lipid. Res. 80, 101055 (2020)
J.J. Grachan, M. Kery, A.J. Giaccia, N.C. Denko and I. Papandreou, Lipid droplet storage promotes murine pancreatic tumor growth. Oncol. Rep. 45, 21 (2021)
C.N. Rozeveld, K.M. Johnson, L. Zhang, G.L. Razidlo, KRAS Controls Pancreatic Cancer Cell Lipid Metabolism and Invasive Potential through the Lipase HSL. Cancer Res. 80, 4932–4945 (2020)
M. Lafontan, D. Langin, Lipolysis and lipid mobilization in human adipose tissue. Prog. Lipid. Res. 48, 275–297 (2009)
E. Recazens, E. Mouisel, D. Langin, Hormone-sensitive lipase: sixty years later. Prog. Lipid. Res. 82, 101084 (2021)
B.R. Stockwell, Ferroptosis turns 10: Emerging mechanisms, physiological functions, and therapeutic applications. Cell 185, 2401–2421 (2022)
X. Chen, R. Kang, G. Kroemer, D. Tang, Broadening horizons: the role of ferroptosis in cancer. Nat. Rev. Clin. Oncol. 18, 280–296 (2021)
E.M. Park, M. Chelvanambi, N. Bhutiani, G. Kroemer, L. Zitvogel, J.A. Wargo, Targeting the gut and tumor microbiota in cancer. Nat. Med. 28, 690–703 (2022)
V. Matson, C.S. Chervin, T.F. Gajewski, Cancer and the microbiome-influence of the commensal microbiota on cancer, immune responses, and immunotherapy. Gastroenterology 160, 600–613 (2021)
T. Maekawa, R. Fukaya, S. Takamatsu, S. Itoyama, T. Fukuoka, M. Yamada, T. Hata, S. Nagaoka, K. Kawamoto, H. Eguchi, K. Murata, T. Kumada, T. Ito, M. Tanemura, K. Fujimoto, Y. Tomita, T. Tobe, Y. Kamada, E. Miyoshi, Possible involvement of Enterococcus infection in the pathogenesis of chronic pancreatitis and cancer. Biochem. Biophys. Res. Commun. 506, 962–969 (2018)
M.Y. Wei, S. Shi, C. Liang, Q.C. Meng, J. Hua, Y.Y. Zhang, J. Liu, B. Zhang, J. Xu, X.J. Yu, The microbiota and microbiome in pancreatic cancer: more influential than expected. Mol. Cancer. 18, 97 (2019)
A. Koh, F. De Vadder, P. Kovatcheva-Datchary, F. Bäckhed, From dietary fiber to host physiology: short-chain fatty acids as key bacterial metabolites. Cell 165, 1332–1345 (2016)
W.M. de Vos, H. Tilg, M. Van Hul, P.D. Cani, Gut microbiome and health: mechanistic insights. Gut 71, 1020–1032 (2022)
C. Panebianco, A. Villani, F. Pisati, F. Orsenigo, M. Ulaszewska, T.P. Latiano, A. Potenza, A. Andolfo, F. Terracciano, C. Tripodo, F. Perri, V. Pazienza, Butyrate, a postbiotic of intestinal bacteria, affects pancreatic cancer and gemcitabine response in in vitro and in vivo models. Biomed. Pharmacother. 151, 113163 (2022)
M. Luu, Z. Riester, A. Baldrich, N. Reichardt, S. Yuille, A. Busetti, M. Klein, A. Wempe, H. Leister, H. Raifer, F. Picard, K. Muhammad, K. Ohl, R. Romero, F. Fischer, C.A. Bauer, M. Huber, T.M. Gress, M. Lauth, S. Danhof, T. Bopp, T. Nerreter, I.E. Mulder, U. Steinhoff, M. Hudecek, A. Visekruna, Microbial short-chain fatty acids modulate CD8(+) T cell responses and improve adoptive immunotherapy for cancer. Nat. Commun. 12, 4077 (2021)
F. Puca, F. Yu, C. Bartolacci, P. Pettazzoni, A. Carugo, E. Huang-Hobbs, J. Liu, C. Zanca, F. Carbone, E. Del Poggetto, J. Gumin, P. Dasgupta, S. Seth, S. Srinivasan, F.F. Lang, E.P. Sulman, P.L. Lorenzi, L. Tan, M. Shan, Z.P. Tolstyka, M. Kachman, L. Zhang, S. Gao, A.K. Deem, G. Genovese, P.P. Scaglioni, C.A. Lyssiotis, A. Viale, G.F. Draetta, Medium-chain acyl-CoA dehydrogenase protects mitochondria from lipid peroxidation in glioblastoma. Cancer Discov. 11, 2904–2923 (2021)
G. Svegliati-Baroni, I. Pierantonelli, P. Torquato, R. Marinelli, C. Ferreri, C. Chatgilialoglu, D. Bartolini, F. Galli, Lipidomic biomarkers and mechanisms of lipotoxicity in non-alcoholic fatty liver disease. Free Radic. Biol. Med. 144, 293–309 (2019)
F. Canet, P. Díaz-Pozo, C. Luna-Marco, M. Fernandez-Reyes, T. Vezza, M. Marti, J.D. Salazar, I. Roldan, C. Morillas, S. Rovira-Llopis, M. Rocha, V.M. Víctor, Mitochondrial redox impairment and enhanced autophagy in peripheral blood mononuclear cells from type 1 diabetic patients. Redox. Biol. 58, 102551 (2022)
D. Liang, A.M. Minikes, X. Jiang, Ferroptosis at the intersection of lipid metabolism and cellular signaling. Mol. Cell. 82, 2215–2227 (2022)
Y. Zhao, J. Li, W. Guo, H. Li, L. Lei, Periodontitis-level butyrate-induced ferroptosis in periodontal ligament fibroblasts by activation of ferritinophagy. Cell Death Discov. 6, 119 (2020)
Z. Bian, X. Sun, L. Liu, Y. Qin, Q. Zhang, H. Liu, L. Mao and S. Sun, Sodium Butyrate Induces CRC Cell Ferroptosis via the CD44/SLC7A11 Pathway and Exhibits a Synergistic Therapeutic Effect with Erastin. Cancers (Basel). 15, 423 (2023)
M.A. Badgley, D.M. Kremer, H.C. Maurer, K.E. DelGiorno, H.J. Lee, V. Purohit, I.R. Sagalovskiy, A. Ma, J. Kapilian, C.E.M. Firl, A.R. Decker, S.A. Sastra, C.F. Palermo, L.R. Andrade, P. Sajjakulnukit, L. Zhang, Z.P. Tolstyka, T. Hirschhorn, C. Lamb, T. Liu, W. Gu, E.S. Seeley, E. Stone, G. Georgiou, U. Manor, A. Iuga, G.M. Wahl, B.R. Stockwell, C.A. Lyssiotis, K.P. Olive, Cysteine depletion induces pancreatic tumor ferroptosis in mice. Science 368, 85–89 (2020)
S. Uchiyama, T. Shimizu, T. Shirasawa, CuZn-SOD deficiency causes ApoB degradation and induces hepatic lipid accumulation by impaired lipoprotein secretion in mice. J. Biol. Chem. 281, 31713–31719 (2006)
R.M. Lebovitz, H. Zhang, H. Vogel, J. Cartwright Jr., L. Dionne, N. Lu, S. Huang, M.M. Matzuk, Neurodegeneration, myocardial injury, and perinatal death in mitochondrial superoxide dismutase-deficient mice. Proc. Natl. Acad. Sci. U S A. 93, 9782–9787 (1996)
Funding
This work was supported by the National Natural Science Foundation of China (No. 81970553, No. 81770628, No. 82022049, J. X); Shanghai Municipal Education Commission-Gaofeng Clinical Medicine Grant Support (No. 20161312, J.X.); Innovative Research Team of High-Level Local Universities in Shanghai (J.X.); 111 Projects (No. B21024, J.X.).
Author information
Authors and Affiliations
Contributions
J.X. and XT.Y. designed the experiment and interpreted the data; XT.Y. and ZY.Z. performed most of the experiments; XQ.S., JY.X. and YW.W. assisted in some experiments; W.W. provided the key materials and assisted in some discussion; J.X. and YX.T. wrote the manuscript; J.X. and W.W. provided overall guidance.
Corresponding authors
Ethics declarations
Ethical approval
All animal experiments were approved by the Animal Care and Use Committees at Ren Ji Hospital (RJ2020-0505), Shanghai Jiao Tong University School of Medicine.
Competing interests
No potential conflict of interest was reported by the author(s).
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, X., Zhang, Z., Shen, X. et al. Clostridium butyricum and its metabolite butyrate promote ferroptosis susceptibility in pancreatic ductal adenocarcinoma. Cell Oncol. 46, 1645–1658 (2023). https://doi.org/10.1007/s13402-023-00831-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13402-023-00831-8