Abstract
Introduction
The CAPTURE study estimated the global prevalence of established cardiovascular disease (CVD) and characterized the usage of glucose-lowering agents (GLAs) in adults with type 2 diabetes (T2D) across 13 countries. The purpose of this secondary analysis of data from the Japanese sites within CAPTURE (NCT03786406, NCT03811288) was to provide data about medication usage stratified by CVD status among Japanese participants with T2D.
Materials and methods
Data on GLA usage (including those with proven cardiovascular [CV] benefits) in Japanese participants with T2D managed in clinics or hospitals were collected and stratified by CVD subgroups.
Results
There were 800 Japanese participants in the CAPTURE study (n = 502 [no CVD group], n = 298 [CVD group], n = 268 [atherosclerotic CVD subgroup]). Oral antidiabetic agents and insulin were used by 88.5% and 23.4%, respectively, of participants overall. Among participants with established CVD, dipeptidyl peptidase-4 inhibitors (65.1%) were most frequently used, followed by biguanides (50.7%) and insulins (26.2%). The pattern was similar among participants with atherosclerotic CVD. A lower proportion of participants in the CVD group used glucagon-like peptide-1 receptor agonists (GLP-1 RAs) and sodium-glucose cotransporter-2 inhibitors (SGLT-2is) with proven CV benefits versus the no CVD group (GLP-1 RAs: 7.0% vs. 8.6%; SGLT-2is: 13.4% vs. 19.1%).
Conclusion
This analysis of the CAPTURE study provided a comprehensive overview of prescription patterns for the treatment of T2D in Japan. Use of GLAs with proven CV benefit was low, even in participants with established CVD, which was comparable to the findings from the global cohort.



Similar content being viewed by others
Data availability
Upon reasonable request, the datasets used and/or analyzed during the current study are available from the lead author.
References
International Diabetes Federation (IDF) (2019) IDF Diabetes Atlas, 9th edn. Brussels, Belgium: 2019. Available at: https://www.diabetesatlas.org. 2019 (Accessed 2 Sep 2021).
Sarwar N, Gao P, Seshasai SR, Gobin R, Kaptoge S, Di Angelantonio E, Ingelsson E, Lawlor DA, Selvin E, Stampfer M, Stehouwer CD, Lewington S, Pennells L, Thompson A, Sattar N, White IR, Ray KK, Danesh J. Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies. Lancet. 2010;375:2215–22.
Fujihara K, Sone H. Cardiovascular disease in Japanese patients with type 2 diabetes mellitus. Ann Vasc Dis. 2018;11:2–14.
Ikeda N, Nishi N, Noda H, Noda M. Trends in prevalence and management of diabetes and related vascular risks in Japanese adults: Japan National Health and Nutrition Surveys 2003–2012. Diabetes Res Clin Pract. 2017;127:115–22.
Marso SP, Daniels GH, Brown-Frandsen K, Kristensen P, Mann JF, Nauck MA, Nissen SE, Pocock S, Poulter NR, Ravn LS, Steinberg WM, Stockner M, Zinman B, Bergenstal RM, Buse JB. Liraglutide and cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2016;375:311–22.
Husain M, Birkenfeld AL, Donsmark M, Dungan K, Eliaschewitz FG, Franco DR, Jeppesen OK, Lingvay I, Mosenzon O, Pedersen SD, Tack CJ, Thomsen M, Vilsbøll T, Warren ML, Bain SC. Oral semaglutide and cardiovascular outcomes in patients with type 2 diabetes. N Engl J Med. 2019;381:841–51.
Zinman B, Wanner C, Lachin JM, Fitchett D, Bluhmki E, Hantel S, Mattheus M, Devins T, Johansen OE, Woerle HJ, Broedl UC, Inzucchi SE. Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med. 2015;373:2117–28.
Gerstein HC, Colhoun HM, Dagenais GR, Diaz R, Lakshmanan M, Pais P, Probstfield J, Riesmeyer JS, Riddle MC, Rydén L, Xavier D, Atisso CM, Dyal L, Hall S, Rao-Melacini P, Wong G, Avezum A, Basile J, Chung N, Conget I, Cushman WC, Franek E, Hancu N, Hanefeld M, Holt S, Jansky P, Keltai M, Lanas F, Leiter LA, Lopez-Jaramillo P, Cardona Munoz EG, Pirags V, Pogosova N, Raubenheimer PJ, Shaw JE, Sheu WH, Temelkova-Kurktschiev T. Dulaglutide and cardiovascular outcomes in type 2 diabetes (REWIND): a double-blind, randomised placebo-controlled trial. Lancet. 2019;394:121–30.
Wiviott SD, Raz I, Bonaca MP, Mosenzon O, Kato ET, Cahn A, Silverman MG, Zelniker TA, Kuder JF, Murphy SA, Bhatt DL, Leiter LA, McGuire DK, Wilding JPH, Ruff CT, Gause-Nilsson IAM, Fredriksson M, Johansson PA, Langkilde AM, Sabatine MS. Dapagliflozin and cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2019;380:347–57.
Neal B, Perkovic V, Mahaffey KW, de Zeeuw D, Fulcher G, Erondu N, Shaw W, Law G, Desai M, Matthews DR. Canagliflozin and cardiovascular and renal events in type 2 diabetes. N Engl J Med. 2017;377:644–57.
Lee MMY, Ghouri N, McGuire DK, Rutter MK, Sattar N. Meta-analyses of results from randomized outcome trials comparing cardiovascular effects of SGLT2is and GLP-1RAs in asian versus white patients with and without type 2 diabetes. Diabetes Care. 2021;44:1236–41.
Cosentino F, Grant PJ, Aboyans V, Bailey CJ, Ceriello A, Delgado V, Federici M, Filippatos G, Grobbee DE, Hansen TB, Huikuri HV, Johansson I, Jüni P, Lettino M, Marx N, Mellbin LG, Östgren CJ, Rocca B, Roffi M, Sattar N, Seferović PM, Sousa-Uva M, Valensi P, Wheeler DC. 2019 ESC Guidelines on diabetes, pre-diabetes, and cardiovascular diseases developed in collaboration with the EASD. Eur Heart J. 2020;41:255–323.
American Diabetes Association. 9. Pharmacologic approaches to glycemic treatment: standards of medical care in diabetes—2022. Diabetes Care. 2021;45:S125–43. https://doi.org/10.2337/dc22-S009.
Araki E, Goto A, Kondo T, Noda M, Noto H, Origasa H, Osawa H, Taguchi A, Tanizawa Y, Tobe K, Yoshioka N. Japanese clinical practice guideline for diabetes 2019. Diabetol Int. 2020;11:165–223.
Araki E, Tanaka A, Inagaki N, Ito H, Ueki K, Murohara T, Imai K, Sata M, Sugiyama T, Ishii H, Yamane S, Kadowaki T, Komuro I, Node K. Diagnosis, prevention, and treatment of cardiovascular diseases in people with type 2 diabetes and prediabetes - a consensus statement jointly from the Japanese circulation society and the Japan diabetes society. Circ J. 2020;85:82–125.
Nishimura R, Kato H, Kisanuki K, Oh A, Hiroi S, Onishi Y, Guelfucci F, Shimasaki Y. Treatment patterns, persistence and adherence rates in patients with type 2 diabetes mellitus in Japan: a claims-based cohort study. BMJ Open. 2019;9:e025806.
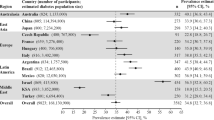
Mosenzon O, Alguwaihes A, Leon J, Bayram F, Darmon P, Davis T, Dieuzeide G, Eriksen KT, Hong T, Kaltoft MS, Lengyel C, Rhee NA, Russo GT, Shirabe S, Urbancova K, Vencio S. CAPTURE: a multinational, cross-sectional study of cardiovascular disease prevalence in adults with type 2 diabetes across 13 countries. Cardiovasc Diabetol. 2021;20:154.
Seino H, Onishi Y, Eguchi K, Nishijima K, Sato T, Shirabe S. Cardiovascular disease prevalence in adults with type 2 diabetes in Japan: results from the Japanese centers in the CAPTURE study. Diabetol Int. 2023. https://doi.org/10.1007/s13340-022-00612-y.
American Diabetes Association. 10. Cardiovascular disease and risk management: standards of medical care in diabetes—2022. Diabetes Care. 2021;45:S144–74. https://doi.org/10.2337/dc22-S010.
American Diabetes Association. 10. Cardiovascular disease and risk management: standards of medical care in diabetes-2020. Diabetes Care. 2020;43:S111–34.
World Medical Association. World Medical Association Declaration of Helsinki: ethical principles for medical research involving human subjects. JAMA. 2013;310:2191–4.
Epstein M. Guidelines for good pharmacoepidemiology practices (GPP). Pharmacoepidemiol Drug Saf. 2005;14:589–95.
Fukushima M, Usami M, Ikeda M, Nakai Y, Taniguchi A, Matsuura T, Suzuki H, Kurose T, Yamada Y, Seino Y. Insulin secretion and insulin sensitivity at different stages of glucose tolerance: a cross-sectional study of Japanese type 2 diabetes. Metabolism. 2004;53:831–5.
Yabe DKH, Iwasaki M, Seino Y. Why are incretin-based therapies more efficient in East Asians? Perspectives from the pathophysiology of type 2 diabetes and East Asian dietary habits. EMJ Diabet. 2015;3:57–65.
Katakami N, Mita T, Takahara M, Yajima T, Wada F, Kawashima M, Shimomura I, Watada H. Baseline characteristics of patients with type 2 diabetes initiating second-line treatment in Japan: findings from the J-DISCOVER Study. Diabetes Ther. 2020;11:1563–78.
Morita Y, Murayama H, Odawara M, Bauer M. Treatment patterns of drug-naive patients with type 2 diabetes mellitus: a retrospective cohort study using a Japanese hospital database. Diabetol Metab Syndr. 2019;11:90.
Kubota K, Kamijima Y, Kao Yang YH, Kimura S, Chia-Cheng Lai E, Man KKC, Ryan P, Schuemie M, Stang P, Su CC, Wong ICK, Zhang Y, Setoguchi S. Penetration of new antidiabetic medications in East Asian countries and the United States: a cross-national comparative study. PLoS ONE. 2018;13:e0208796.
Murayama H, Imai K, Odawara M. factors influencing the prescribing preferences of physicians for drug-naive patients with type 2 diabetes mellitus in the real-world setting in Japan: insight from a web survey. Diabetes Ther. 2018;9:1185–99.
Mishriky BM, Cummings DM, Tanenberg RJ. The efficacy and safety of DPP4 inhibitors compared to sulfonylureas as add-on therapy to metformin in patients with Type 2 diabetes: a systematic review and meta-analysis. Diabetes Res Clin Pract. 2015;109:378–88.
Kim YG, Hahn S, Oh TJ, Kwak SH, Park KS, Cho YM. Differences in the glucose-lowering efficacy of dipeptidyl peptidase-4 inhibitors between Asians and non-Asians: a systematic review and meta-analysis. Diabetologia. 2013;56:696–708.
Kohro T, Yamazaki T, Sato H, Harada K, Ohe K, Komuro I, Nagai R. Trends in antidiabetic prescription patterns in Japan from 2005 to 2011. Int Heart J. 2013;54:93–7.
Oh A, Kisanuki K, Nishigaki N, Shimasaki Y, Sakaguchi K, Morimoto T. Comparison of persistence and adherence between DPP-4 inhibitor administration frequencies in patients with type 2 diabetes mellitus in Japan: a claims-based cohort study. Curr Med Res Opin. 2020;36:387–95.
Buse JB, Wexler DJ, Tsapas A, Rossing P, Mingrone G, Mathieu C, D’Alessio DA, Davies MJ. 2019 update to: management of hyperglycemia in type 2 diabetes, 2018. a consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care. 2020;43:487–93.
Davies MJ, Aroda VR, Collins BS, Gabbay RA, Green J, Maruthur NM, Rosas SE, Del Prato S, Mathieu C, Mingrone G, Rossing P, Tankova T, Tsapas A, Buse JB. Management of hyperglycemia in type 2 diabetes, 2022. A consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care. 2022;45:2753–86.
Harashima SI, Nishimura A, Inagaki N. Attitudes of patients and physicians to insulin therapy in Japan: an analysis of the Global Attitude of Patients and Physicians in Insulin Therapy study. Expert Opin Pharmacother. 2017;18:5–11.
Patorno E, Pawar A, Bessette LG, Kim DH, Dave C, Glynn RJ, Munshi MN, Schneeweiss S, Wexler DJ, Kim SC. Comparative effectiveness and safety of sodium-glucose cotransporter 2 inhibitors versus glucagon-like peptide 1 receptor agonists in older adults. Diabetes Care. 2021;44:826–35.
Peyrot M, Barnett AH, Meneghini LF, Schumm-Draeger PM. Insulin adherence behaviours and barriers in the multinational Global Attitudes of Patients and Physicians in Insulin Therapy study. Diabetic Med. 2012;29:682–9.
Ishigaki Y, Strizek A, Aranishi T, Arai N, Imaoka T, Cai Z, Maegawa H. Glucagon-like peptide-1 receptor agonist utilization in type 2 diabetes in Japan: a retrospective database analysis (JDDM 57). Diabetes Ther. 2021;12:345–61.
Seino Y, Rasmussen MF, Nishida T, Kaku K. Efficacy and safety of the once-daily human GLP-1 analogue, liraglutide, vs glibenclamide monotherapy in Japanese patients with type 2 diabetes. Curr Med Res Opin. 2010;26:1013–22.
Kaku K, Yamada Y, Watada H, Abiko A, Nishida T, Zacho J, Kiyosue A. Safety and efficacy of once-weekly semaglutide vs additional oral antidiabetic drugs in Japanese people with inadequately controlled type 2 diabetes: a randomized trial. Diabetes Obes Metab. 2018;20:1202–12.
Kaku K, Chin R, Naito Y, Iliev H, Ikeda R, Ochiai K, Yasui A. Safety and effectiveness of empagliflozin in Japanese patients with type 2 diabetes: interim analysis from a post-marketing surveillance study. Expert Opin Drug Saf. 2020;19:211–21.
Koike Y, Shirabe SI, Maeda H, Yoshimoto A, Arai K, Kumakura A, Hirao K, Terauchi Y. Effect of canagliflozin on the overall clinical state including insulin resistance in Japanese patients with type 2 diabetes mellitus. Diabetes Res Clin Pract. 2019;149:140–6.
Odawara M, Miyagawa J, Iwamoto N, Takita Y, Imaoka T, Takamura T. Once-weekly glucagon-like peptide-1 receptor agonist dulaglutide significantly decreases glycated haemoglobin compared with once-daily liraglutide in Japanese patients with type 2 diabetes: 52 weeks of treatment in a randomized phase III study. Diabetes Obes Metab. 2016;18:249–57.
Pharmaceuticals and Medical Devices Agency (2015) New Drugs Approved in FY 2015. Available at: https://www.pmda.go.jp/files/000229077.pdf (Accessed Sep 13, 2021).
Frias JP, Wynne AG, Matyjaszek-Matuszek B, Bartaskova D, Cox DA, Woodward B, Li YG, Tham LS, Milicevic Z. Efficacy and safety of an expanded dulaglutide dose range: a phase 2, placebo-controlled trial in patients with type 2 diabetes using metformin. Diabetes Obes Metab. 2019;21:2048–57.
Ito D, Iuchi T, Kurihara S, Inoue I, Katayama S, Inukai K. Efficacy and clinical characteristics of liraglutide in Japanese patients with type 2 diabetes. J Clin Med Res. 2015;7:694–9.
Kaku K. Liraglutide for the treatment of diabetes mellitus in Japan. Diabetes Manage. 2011;1:451–63.
Pharmaceuticals and Medical Devices Agency (2019) New Drugs Approved in FY 2019. Available at: https://www.pmda.go.jp/files/000235289.pdf. Accessed on June 10, 2021.
Marso SP, Bain SC, Consoli A, Eliaschewitz FG, Jódar E, Leiter LA, Lingvay I, Rosenstock J, Seufert J, Warren ML, Woo V, Hansen O, Holst AG, Pettersson J, Vilsbøll T. Semaglutide and cardiovascular outcomes in patients with type 2 diabetes. N Engl J Med. 2016;375:1834–44.
Pharmaceuticals and Medical Devices Agency (2017) List of approved products FY 2017. Available at: https://www.pmda.go.jp/files/000232769.pdf. (Accessed on Aug 3, 2022).
Poole RM, Dungo RT. Ipragliflozin: first global approval. Drugs. 2014;74:611–7.
Poole RM, Prossler JE. Tofogliflozin: first global approval. Drugs. 2014;74:939–44.
Markham A, Elkinson S. Luseogliflozin: first global approval. Drugs. 2014;74:945–50.
Pharmaceuticals and Medical Devices Agency (2013) List of approved products FY 2013. Available at: https://www.pmda.go.jp/files/000232771.pdf. (Accessed on Sep 2, 2021).
Ohsugi M, Eiki JI, Iglay K, Tetsuka J, Tokita S, Ueki K. Comorbidities and complications in Japanese patients with type 2 diabetes mellitus: retrospective analyses of J-DREAMS, an advanced electronic medical records database. Diabetes Res Clin Pract. 2021;178:108845.
Gallagher D, Heymsfield SB, Heo M, Jebb SA, Murgatroyd PR, Sakamoto Y. Healthy percentage body fat ranges: an approach for developing guidelines based on body mass index. Am J Clin Nutr. 2000;72:694–701.
de Boer SA, Lefrandt JD, Petersen JF, Boersma HH, Mulder DJ, Hoogenberg K. The effects of GLP-1 analogues in obese, insulin-using type 2 diabetes in relation to eating behaviour. Int J Clin Pharm. 2016;38:144–51.
Yu DN, Qiu L, Ning SY, Guo LX. Evaluation of efficacy and safety of DPP-4 inhibitors for Chinese elderly patients with type 2 diabetes mellitus. Diabetol Metab Syndr. 2020;12:35.
Viljoen AMC, Gadsby R, Viljoen S, Langerman H, Sinclair AJ. The tolerability and safety of DPP-4 inhibitors for the treatment of older people with type 2 diabetes mellitus: an observational study. British J Diabetes Vascular Dis. 2013;13:187–91.
Hata J, Ninomiya T, Hirakawa Y, Nagata M, Mukai N, Gotoh S, Fukuhara M, Ikeda F, Shikata K, Yoshida D, Yonemoto K, Kamouchi M, Kitazono T, Kiyohara Y. Secular trends in cardiovascular disease and its risk factors in Japanese: half-century data from the Hisayama Study (1961–2009). Circulation. 2013;128:1198–205.
Tajima A, Tobe K, Eiki JI, Origasa H, Watada H, Shimomura I, Tokita S, Kadowaki T. Treatment patterns and satisfaction in patients with type 2 diabetes newly initiating oral monotherapy with antidiabetic drugs in Japan: results from the prospective real-world observational study on patient outcomes in diabetes (RESPOND). BMJ Open Diabetes Res Care. 2022. https://doi.org/10.1136/bmjdrc-2022-003032.
Acknowledgements
This study was funded by Novo Nordisk A/S. The authors would like to thank the study participants, investigators, and coordinators. Medical writing support was provided by Dhara P. Patel and Beth Campbell, on behalf of Ashfield MedComms, and editorial assistance provided by Helen Marshall of Ashfield MedComms, an Inizio company, and funded by Novo Nordisk A/S.
Funding
Novo Nordisk A/S.
Author information
Authors and Affiliations
Contributions
YO, SS, and HS were investigators in the study and collected data. TS and KN contributed to statistical analyses required for the Japan data. All authors reviewed and edited drafts of the manuscript prior to submission. The authors confirm that they meet the International Committee of Medical Journal Editors uniform authorship requirements and that they have contributed to critical analysis and interpretation of the data, critically revised the article, and share in the final responsibility for manuscript content, as well as the decision to submit it for publication.
Corresponding author
Ethics declarations
Conflict of interest
YO has received honoraria/lecture fees from Novo Nordisk Pharma Ltd. and Sumitomo Pharma. SS has received honoraria/lecture fees from Eli Lilly Japan K.K., Novo Nordisk Pharma Ltd. and Sumitomo Pharma. KE and TS are employees of Novo Nordisk. KN holds shares in and is an employee of Novo Nordisk. HS has received research funding from Astellas Pharma Inc., Taisho Toyama Pharmaceutical, Takeda Pharmaceutical, Novo Nordisk Pharma, Sanofi, Mitsubishi Tanabe Pharma Co., Novartis Pharma K.K., Shionogi Pharma Co. Ltd., Boehringer Ingelheim, AstraZeneca K.K., and MSD; and honoraria from Shionogi Pharma Co., Mitsubishi Tanabe Pharma Co., Astellas Pharma Inc., Novartis Pharma K.K., Eli Lilly, Ono Pharmaceutical Co., MSD, and Sanofi.
Ethical approval
The protocol was approved by the IEC or other appropriate body and was provided by each investigator prior to undertaking any study-related activities. Specifically, the protocol was approved by: Institute for Adult Diseases, Asahi Life Foundation Institutional Review Board (approval date: 03 Dec 2018; approval number: 11000766); Medical Corporation Ichi YouKai Institutional Review Board Makato Honda Board (approval date: 13 Feb 2019; approval number: 14000077); Seino Naika Clinic Chairman, Ethical Review Board (approval date: 15 Dec 2018; approval number: 18000150); Shinagawa East One Medical Clinic Ethical Review Board Shinagawa East One Medical Clinic (approval date: 26 Nov 2018; approval number: 11000993); Nihonbashi Sakura Clinic Institutional Review Board (approval date: 05 Dec 2018; approval number: 11001007); Heiwadai Hospital Institutional Review Board (approval date: 21 Nov 2018; approval number: 11000861); Jinnouchi Hospital Ethical Review Board (approval date: 10 Dec 2018; approval number: 16000034); Kouhoukai Ethical Committee (approval date: 03 Dec 2018; approval number: 18000145); Hospital Joint Institutional Review Board (approval date: 21 Dec 2018; approval number: 14000050); and Institutional Review Board for Considering the Ethics of Special Non-Profit Entity Clinical Trials (approval date: 28 Jan 2019; approval number: 12000065).
Human research
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and/or with the Helsinki Declaration of 1964 and later versions. Informed consent was provided by each participant prior to undertaking any study-related activities (during the first and only study visit).
Informed consent
Informed consent was provided by each participant prior to undertaking any study-related activities (during the first and only study visit).
Approval date of registry and registration no. of the study/trial
NCT03786406, 26 December 2018 and NCT03811288, 22 January 2019.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be submitted.
Prior presentation
Some of the results from this study were previously presented at the 64th Annual Meeting of the Japanese Diabetes Society, virtual meeting, 2021.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Onishi, Y., Shirabe, S., Eguchi, K. et al. Use of diabetes medications in adults with T2D and CVD in Japan: secondary analysis of the CAPTURE study. Diabetol Int 14, 363–371 (2023). https://doi.org/10.1007/s13340-023-00638-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13340-023-00638-w