Abstract
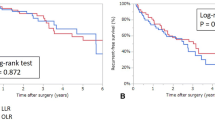
To date, there is little knowledge about the value of laparoscopic liver resection (LLR) for hepatocellular carcinoma (HCC) patients with Barcelona Clinic Liver Cancer (BCLC) stage B. Thus, this study was performed to assess the perioperative and oncological outcomes of LLR for these patients by comparison with open liver resection (OLR). Between April 2015 and October 2018, a total of 217 resectable HCC patients with BCLC stage B were eligible for this study. Patients were divided into the LLR group and the OLR group according to different procedures. Propensity score matching (PSM) was conducted to adjust for known confounders. Short- and long-term outcomes were compared between the two groups. LLR was performed in 75 of the 217 included patients. After PSM, 72 patients with well-balanced baseline levels were enrolled into each group. Although the operative time was significantly longer in the LLR group than in the OLR group (median, 237.5 vs. 210 min, P = 0.024), the intraoperative blood loss was significantly less in the LLR group than in the OLR group (median, 200 vs. 350 ml, P = 0.005). Patients in the LLR group had fewer complications than those in the OLR group (P = 0.035). Furthermore, overall survival (OS, P = 0.827) and recurrence-free survival (RFS, P = 0.694) were comparable between the two groups. LLR for resectable HCC patients with BCLC stage B is safe and feasible in carefully selected patients and has superior perioperative outcomes and similar survival rates compared with OLR.


Similar content being viewed by others
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A et al (2021) Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 71:209–249. https://doi.org/10.3322/caac.21660
Forner A, Reig M, Bruix J (2018) Hepatocellular carcinoma. Lancet 391:1301–1314. https://doi.org/10.1016/s0140-6736(18)30010-2
Park JW, Chen M, Colombo M, Roberts LR, Schwartz M, Chen PJ et al (2015) Global patterns of hepatocellular carcinoma management from diagnosis to death: the BRIDGE Study. Liver Int 35:2155–2166. https://doi.org/10.1111/liv.12818
European association for the study of the L, European organisation for R, treatment of C (2012) EASL-EORTC clinical practice guidelines: management of hepatocellular carcinoma. J Hepatol. 56:908–943. https://doi.org/10.1016/j.jhep.2011.12.001
Reig M, Forner A, Rimola J, Ferrer-Fábrega J, Burrel M, Garcia-Criado A et al (2021) BCLC strategy for prognosis prediction and treatment recommendation barcelona clinic liver cancer (BCLC) staging system The 2022 update. J Hepatol. https://doi.org/10.1016/j.jhep.2021.11.018
Yin L, Li H, Li AJ, Lau WY, Pan ZY, Lai EC et al (2014) Partial hepatectomy vs. transcatheter arterial chemoembolization for resectable multiple hepatocellular carcinoma beyond milan criteria: a RCT. J Hepatol 61:82–88. https://doi.org/10.1016/j.jhep.2014.03.012
Vitale A, Burra P, Frigo AC, Trevisani F, Farinati F, Spolverato G et al (2015) Survival benefit of liver resection for patients with hepatocellular carcinoma across different barcelona clinic liver cancer stages: a multicentre study. J Hepatol 62:617–624. https://doi.org/10.1016/j.jhep.2014.10.037
Ciria R, Lopez-Cillero P, Gallardo AB, Cabrera J, Pleguezuelo M, Ayllon MD et al (2015) Optimizing the management of patients with BCLC stage-B hepatocellular carcinoma: modern surgical resection as a feasible alternative to transarterial chemoemolization. Eur J Surg Oncol 41:1153–1161. https://doi.org/10.1016/j.ejso.2015.05.023
Lin CT, Hsu KF, Chen TW, Yu JC, Chan DC, Yu CY et al (2010) Comparing hepatic resection and transarterial chemoembolization for barcelona clinic liver cancer (BCLC) stage B hepatocellular carcinoma: change for treatment of choice? World J Surg 34:2155–2161. https://doi.org/10.1007/s00268-010-0598-x
Kim H, Ahn SW, Hong SK, Yoon KC, Kim HS, Choi YR et al (2017) Survival benefit of liver resection for barcelona clinic liver cancer stage B hepatocellular carcinoma. Br J Surg 104:1045–1052. https://doi.org/10.1002/bjs.10541
Vogel A, Cervantes A, Chau I, Daniele B, Llovet J, Meyer T et al (2018) Hepatocellular carcinoma: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol. 29:iv238–iv255. https://doi.org/10.1093/annonc/mdy308
Omata M, Cheng AL, Kokudo N, Kudo M, Lee JM, Jia J et al (2017) Asia-Pacific clinical practice guidelines on the management of hepatocellular carcinoma: a 2017 update. Hepatol Int 11:317–370. https://doi.org/10.1007/s12072-017-9799-9
Wakabayashi G, Cherqui D, Geller DA, Buell JF, Kaneko H, Han HS et al (2015) Recommendations for laparoscopic liver resection: a report from the second international consensus conference held in Morioka. Ann Surg 261:619–629. https://doi.org/10.1097/sla.0000000000001184
Franken C, Lau B, Putchakayala K, DiFronzo LA (2014) Comparison of short-term outcomes in laparoscopic vs open hepatectomy. JAMA Surg 149:941–946. https://doi.org/10.1001/jamasurg.2014.1023
Witowski J, Rubinkiewicz M, Mizera M, Wysocki M, Gajewska N, Sitkowski M et al (2019) Meta-analysis of short- and long-term outcomes after pure laparoscopic versus open liver surgery in hepatocellular carcinoma patients. Surg Endosc 33:1491–1507. https://doi.org/10.1007/s00464-018-6431-6
Xiangfei M, Yinzhe X, Yingwei P, Shichun L, Weidong D (2019) Open versus laparoscopic hepatic resection for hepatocellular carcinoma: a systematic review and meta-analysis. Surg Endosc 33:2396–2418. https://doi.org/10.1007/s00464-019-06781-3
Liu F, Xu H, Li Q, Wei Y, Li H, Wang W et al (2018) Outcomes of pure laparoscopic Glissonian pedicle approach hepatectomy for hepatocellular carcinoma: a propensity score matching analysis. Surg Endosc 33:1155–1166. https://doi.org/10.1007/s00464-018-6380-0
Liu F, Wei Y, Li H, Wang W, Wen T, Wu H et al (2018) LigaSure versus CUSA for parenchymal transection during laparoscopic hepatectomy in hepatocellular carcinoma patients with cirrhosis: a propensity score-matched analysis. Surg Endosc 32:2454–2465. https://doi.org/10.1007/s00464-017-5947-5
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Balzan S, Belghiti J, Farges O, Ogata S, Sauvanet A, Delefosse D et al (2005) The “50–50 criteria” on postoperative day 5: an accurate predictor of liver failure and death after hepatectomy. Ann Surg. 242:824–828 (discussion 828-829)
Ishizawa T, Hasegawa K, Kokudo N, Sano K, Imamura H, Beck Y et al (2009) Risk factors and management of ascites after liver resection to treat hepatocellular carcinoma. Arch Surg 144:46–51. https://doi.org/10.1001/archsurg.2008.511
Rahbari NN, Garden OJ, Padbury R, Maddern G, Koch M, Hugh TJ et al (2011) Post-hepatectomy haemorrhage: a definition and grading by the international study group of liver surgery (ISGLS). HPB (Oxford) 13:528–535. https://doi.org/10.1111/j.1477-2574.2011.00319.x
Koch M, Garden OJ, Padbury R, Rahbari NN, Adam R, Capussotti L et al (2011) Bile leakage after hepatobiliary and pancreatic surgery: a definition and grading of severity by the international study group of liver surgery. Surgery 149:680–688. https://doi.org/10.1016/j.surg.2010.12.002
Shehta A, Han HS, Yoon YS, Cho JY, Choi Y (2016) Laparoscopic liver resection for hepatocellular carcinoma in cirrhotic patients: 10-year single-center experience. Surg Endosc 30:638–648. https://doi.org/10.1007/s00464-015-4253-3
Meguro M, Mizuguchi T, Kawamoto M, Ota S, Ishii M, Nishidate T et al (2015) Clinical comparison of laparoscopic and open liver resection after propensity matching selection. Surgery 158:573–587. https://doi.org/10.1016/j.surg.2015.02.031
Xu HW, Liu F, Li HY, Wei YG, Li B (2018) Outcomes following laparoscopic versus open major hepatectomy for hepatocellular carcinoma in patients with cirrhosis: a propensity score-matched analysis. Surg Endosc 32:712–719. https://doi.org/10.1007/s00464-017-5727-2
Yoon YI, Kim KH, Kang SH, Kim WJ, Shin MH, Lee SK et al (2017) Pure laparoscopic versus open right hepatectomy for hepatocellular carcinoma in patients with cirrhosis: a propensity score matched analysis. Ann Surg 265:856–863. https://doi.org/10.1097/sla.0000000000002072
Komatsu S, Brustia R, Goumard C, Perdigao F, Soubrane O, Scatton O (2016) Laparoscopic versus open major hepatectomy for hepatocellular carcinoma: a matched pair analysis. Surg Endosc 30:1965–1974. https://doi.org/10.1007/s00464-015-4422-4
Stoot JH, van Dam RM, Busch OR, van Hillegersberg R, De Boer M, Olde Damink SW et al (2009) The effect of a multimodal fast-track programme on outcomes in laparoscopic liver surgery: a multicentre pilot study. HPB (Oxford) 11:140–144. https://doi.org/10.1111/j.1477-2574.2009.00025.x
Wong-Lun-Hing EM, van Dam RM, van Breukelen GJ, Tanis PJ, Ratti F, van Hillegersberg R et al (2017) Randomized clinical trial of open versus laparoscopic left lateral hepatic sectionectomy within an enhanced recovery after surgery programme (ORANGE II study). Br J Surg 104:525–535. https://doi.org/10.1002/bjs.10438
Fretland AA, Dagenborg VJ, Bjornelv GMW, Kazaryan AM, Kristiansen R, Fagerland MW et al (2018) Laparoscopic versus open resection for colorectal liver metastases: The OSLO-COMET randomized controlled trial. Ann Surg 267:199–207. https://doi.org/10.1097/sla.0000000000002353
Funding
This work was supported by grants from the National Natural Science Foundation of China (Nos. 81602910, 81302344, and 81802095) and the Sichuan Science and Technology Program (Nos. 2019YFS0370, 2019YFS0372, and 2017FZ0043).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval and Informed consent
This study was conducted in accordance with the principles of the Declaration of Helsinki and a written informed consent was obtained from all participants. The study was approved by the Ethics Committee of West China Hospital of Sichuan University.
Research involving human participants and/or animals
This article does not contain any studies with human participants performed by any of the authors (retrospective study).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Peng, Y., Chen, K., Li, B. et al. Laparoscopic versus open liver resection for resectable HCC with BCLC stage B: a propensity score-matched analysis. Updates Surg 74, 1291–1297 (2022). https://doi.org/10.1007/s13304-022-01309-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13304-022-01309-2