Abstract
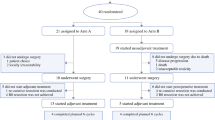
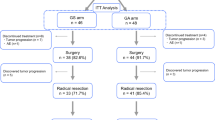
Patients with unresectable recurrent rectal cancer that progresses after systemic chemotherapy and radiotherapy are candidates for palliation with hypoxic pelvic perfusion (HPP). The aim of this observational retrospective study was to evaluate if a multimodality treatment including HPP and targeted-therapy may be useful to prolong clinical responses and survival of these patients. From a cohort of 77 patients with unresectable recurrent rectal cancer in progression after standard treatments and submitted to HPP, 21 patients underwent repeat HPP using mitomycin C (MMC) at the dose of 25 mg/m2. After the last HPP, 7 patients received a targeted-therapy with cetuximab according to overexpression of epidermal growth factor receptor in recurrence cancer cells. The median overall survival of these 21 patients from the diagnosis of unresectable recurrent rectal cancer was 23 months (iqr 18–24). After the first HPP, the median survival of the 21 patients until death or end of follow-up was 10 months (iqr 9–13). The 1-year and 2-year survival rates were 71.4%, and 4.8%, respectively. From the first HPP, age > 60 years, a recurrence shrinkage of at least 30% (partial response), and the addition of a post-HPP targeted-therapy with cetuximab significantly affected survival (P < 0.04). In conclusion, repeated MMC-HPP followed by targeted-therapy seems to be an effective palliative treatment for patients with unresectable recurrent rectal cancer in progression after systemic chemotherapy and radiation but the results of this study have to be confirmed by a larger phase III trial.


Similar content being viewed by others
References
Sammour T, Skibber JM (2018) Evaluation of treatment of locally recurrent rectal cancer. In: Chang G (ed) Rectal cancer. Springer, Cham, pp 231–245
Lee DJ, Sagar PM, Sadadcharam G, Tanand KY (2017) Advances in surgical management for locally recurrent rectal cancer: how far have we come? World J Gastroenterol 23:4170–4180. https://doi.org/10.3748/wjg.v23.i23.4170
Guadagni S, Aigner KR, Fiorentini G et al (2016) Pelvic perfusion for rectal cancer. In: Aigner KR, Stephens FO (eds) Induction chemotherapy. Springer, Berlin, pp 293–307. https://doi.org/10.1007/978-3-319-28773-7
Guadagni S, Kanavos E, Schietroma M, Fiorentini G, Amicucci G (2006) Selected hypoxic stop-flow perfusions: indication and limits. Tumori 92:402–406
Guadagni S, Clementi M, Valenti M et al (2007) Hypoxic abdominal stop-flow perfusion in the treatment of advanced pancreatic cancer: a phase II evaluation/trial. Eur J Surg Oncol 33:72–78
Guadagni S, Fiorentini G, Palumbo G et al (2001) Hypoxic pelvic perfusion with mitomycin C using a simplified balloon-occlusion technique in the treatment of patients with unresectable locally recurrent rectal cancer. Arch Surg 136:105–112. https://doi.org/10.1001/archsurg.136.1.105
Guadagni S, Fiorentini G, Clementi M, Palumbo P, Mambrini A, Masedu F (2017) Mitomycin C hypoxic pelvic perfusion for unresectable recurrent rectal cancer: pharmacokinetic comparison of surgical and percutaneous techniques. Updates Surg 69:403–410. https://doi.org/10.1007/s13304-017-0480-6
Eisenhauer EA, Therasse P, Bogaerts J et al (2009) New response valuation criteria in solid tumors: revised RECIST guideline (version 1.1). Eur J Cancer 45:228–247
Fiorentini G, Sarti D, Aliberti C, Carandina R, Mambrini A, Guadagni S (2017) Multidisciplinary approach of colorectal cancer liver metastases. World J Clin Oncol 8:190–202
Lingareddy V, Ahmad NR, Mohiuddin M (1997) Palliative reirradiation for recurrent rectal cancer. Int J Radiat Oncol Biol Phys 38:785–790
Susko M, Lee J, Salama J et al (2016) The use of re-irradiation in locally recurrent non metastatic rectal cancer. Ann Surg Oncol 23:3609–3615
van Ijken MG, van Etten B, Guetens G et al (2005) Balloon catheter hypoxic pelvic perfusion with mitomycin C and melphalan for locally advanced tumours in the pelvic region: a phase I-II trial. Eur J Surg Oncol 31:897–904. https://doi.org/10.1016/j.ejso.2005.06.004
Wanebo HJ, DiSiena M, Begossi G, Belliveau J, Gustafson E (2008) Isolated chemotherapeutic perfusion of pelvis as neoadjuvant or palliative therapy for advanced cancer of the rectum. Ann Surg Oncol 15:1107–1116. https://doi.org/10.1245/s10434-007-9652-923
Murata S, Onozawa S, Kim C et al (2014) Negative-balance isolated pelvic perfusion in patients with incurable symptomatic rectal cancer: results and drug dose correlation to adverse events. Acta Radiol 55:793–801. https://doi.org/10.1177/0284185113507253
Fiorentini G, Poddie DB, Cantore M et al (2004) Hepatic intra-arterial chemotherapy (HIAC) of high dose mitomycin and epirubicin combined with caval chemofiltration versus prolonged low doses in liver metastases from colorectal cancer: a prospective randomised study. J Chemother 16:51–54
Begossi G, Belliveau JF, Wanebo HJ (2008) Pelvic perfusion for advanced colorectal cancers. Surg Oncol Clin N Am 17:825–842. https://doi.org/10.1016/j.soc.2008.04.014
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The Authors declare that there is no conflict of interest regarding the publication of this paper.
Research involving human participants and/or animals
The retrospective observational study was performed at the University of L’Aquila, L’Aquila, Italy, after approval from the investigational review board (n.10/CE/2018) and following the consideration that the patients had an unresectable disease with a predictable course outcome.
Informed consent
Informed consent was obtained from all individual participants included in this study.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Guadagni, S., Clementi, M., Bencivenga, M. et al. Palliation with a multimodality treatment including hypoxic pelvic perfusion for unresectable recurrent rectal cancer: outcomes based on a retrospective study. Updates Surg 70, 441–447 (2018). https://doi.org/10.1007/s13304-018-0592-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13304-018-0592-7