Abstract
Introduction
Semaglutide is a high-profile glucose-lowering drug that medical decision-makers have acknowledged in recent years. This rapid review aims to provide evidence-based clinical recommendations for the treatment of type 2 diabetes mellitus (T2DM) with semaglutide.
Methods
We conducted a rapid review of randomized controlled trial (RCT)-based meta-analyses (MAs) and systematic reviews (SRs) of cost-effectiveness analyses (CEAs) compared to other glucagon-like peptide-1 receptor agonists (GLP-1 RAs) or placebo in patients with T2DM. Prospective cohort real-world studies (RWS) were also retrieved and subjected to MA. Four databases, including PubMed, the Cochrane Library, Embase, and ISPOR, were searched from inception to 5 March 2023. The outcomes of interest were hemoglobin A1c (HbA1c), body weight, major adverse cardiovascular events (MACE), and economic outcomes such as quality-adjusted life-years and total cost.
Results
We identified 33 publications: 22 RCT-based MAs, 1 SR of CEAs, and 10 RWS. Evidence showed that semaglutide at usual doses was associated with superior reductions in HbA1c and weight compared to most GLP-1 RAs in patients with T2DM who were drug naive, receiving basal insulin, or using oral hypoglycemic agents, and it was also associated with a lower number of MACE and was more cost-effective. Further, once-weekly semaglutide resulted in a significant reduction in HbA1c levels (−1.1%) and body weight (−4.88 kg) in routine clinical practice.
Conclusions
This review consolidates the positive current evidence base for prescribing semaglutide to patients with T2DM, but further rigorous studies are still urgently required to develop practice guidelines as innovative drugs become commercially available.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
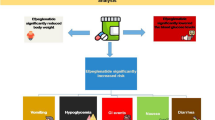
Type 2 diabetes mellitus (T2DM) imposes an enormous medical and economic burden worldwide. Semaglutide, a prominent hypoglycemic agent, has gained recognition from healthcare decision-makers for its potent ability to lower hemoglobin A1c (HbA1c), promote weight loss, and prevent major adverse cardiovascular events (MACE). |
This study provides a rapid review of systematic reviews of cost-effectiveness analyses of semaglutide for treating T2DM and meta-analyses of its efficacy concerning glycemic control, weight loss, and cardiovascular benefit. Additionally, we performed a meta-analysis of prospective cohort real-world studies. The aim of this research was to support evidence-based decision making. |
The pooled evidence showed that semaglutide at usual doses was associated with superior reductions in HbA1c and weight compared to most glucagon-like peptide-1 receptor agonists in patients who were drug naive, receiving basal insulin, or using oral hypoglycemic agents, and it was associated with a lower number of MACE and was more cost-effective. |
Further, once-weekly semaglutide resulted in significant reductions in HbA1c concentration and body weight in routine clinical practice. |
Introduction
Type 2 diabetes mellitus (T2DM) is a complex progressive disease characterized by impaired insulin secretion, increased glucagon secretion, and insulin resistance, which are worsened by obesity and result in hyperglycemia [1]. Therefore, in addition to lifestyle measures, pharmacological treatment should aim to target these abnormalities. In particular, glucagon-like peptide-1 receptor agonists (GLP-1 RAs) have emerged as potent agents for improving glycemic control without inducing hypoglycemia [2]. They achieve this by enhancing insulin secretion in response to glucose and inhibiting glucagon secretion. The latest consensus reports from the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD) highlight the critical role of GLP-1 RAs, especially in individuals with established cardiovascular disease (CVD) or multiple risk factors for CVD [1]. Furthermore, these agents have been shown to reduce the risk of major adverse cardiovascular events (MACE) in people with T2DM. Additionally, weight loss is emphasized as a therapeutic strategy to improve glycemic control, reduce the risk of weight-related complications, and enhance overall quality of life. Notably, GLP-1RAs and tirzepatide, which is the first dual glucose-dependent insulinotropic polypeptide (GIP)/GLP-1 RA, are associated with greater weight loss compared to other glucose-lowering agents [1]. Therefore, GLP-1 RAs have become a well-established class of glucose-lowering agents with a growing impact on the treatment of T2DM and potentially other diseases.
One prominent GLP-1 RA is semaglutide (Novo Nordisk A/S, Denmark), which exhibits greater efficacy in reducing plasma glucose and body weight. It is available in the form of weekly subcutaneous injections (0.5/1.0 mg) and once-daily oral administration (3/7/14 mg), and it has been approved by numerous regulatory agencies for the treatment of T2DM in adults.
While evidence of the efficacy and safety of semaglutide has accumulated through large multicenter randomized clinical trials (RCTs), these studies often have strict inclusion and exclusion criteria that limit how representative of real-world patients they are. Real-world studies (RWS), on the other hand, provide valuable real-world data (RWD) on the effectiveness of a drug in routine clinical practice, reflecting a broad range of clinical conditions [3]. Therefore, RWS can complement the findings of RCTs and contribute to a more comprehensive understanding of drug effectiveness. However, for people with T2DM, there is a notable lack of strong evidence for the real-world use of semaglutide. Additionally, considering the resource constraints in healthcare systems worldwide, selecting more cost-effective treatments is crucial. Cost-effectiveness analysis (CEA) is a widely used tool for evaluating the value for money of new interventions and maximizing health gains for populations [4].
In recent years, rapid reviews have emerged as a valuable tool for national and international health agencies. These reviews streamline the systematic review (SR) process and expedite evidence delivery, enabling timely and informed decisions based on the best available evidence [5]. In this study, we conducted a rapid review of meta-analyses (MAs) and SRs of CEAs comparing semaglutide with other GLP-1 RAs or placebo. Additionally, we performed a MA of RWS to provide a rapid review of the glycemic control, weight management, risk of MACE, and cost-effectiveness of semaglutide in patients with T2DM. By conducting this research, we aimed to provide valuable insights to support clinical and policy decision-making.
Methods
Protocol and Registration
This rapid review was conducted in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines [6] and following a protocol established a priori (PROSPERO: CRD42023407283). In addition, we strictly adopted the steps described by the Cochrane Rapid Reviews methods guidance [5]. This article was based on previously conducted studies and did not contain any new studies with human participants or animals performed by any of the authors.
Eligibility Criteria
PI(E)COS (populations, interventions/exposures, comparators, outcomes, study design) study selection criteria were applied for this rapid review. The full selection criteria are presented in Supplementary Table 1.
We reviewed all potentially eligible papers. RCT-based MAs, prospective cohort RWS assessing the efficacy (effectiveness) and safety of T2DM, and SRs evaluating the cost-effectiveness of semaglutide were considered as potentially eligible papers. The predetermined study eligibility criteria were (1) patients with T2DM; (2) semaglutide as an intervention or exposure; (3) placebo or other GLP-1 RAs as controls, or a non-exposed control group (pre-semaglutide); (4) the efficacy (effectiveness) data of interest were reported—including effect sizes (estimated treatment differences) in hemoglobin A1c (HbA1c) or body weight as well as safety data, including effect sizes (incidence) for MACE—and economic outcomes were also included, such as changes in quality-adjusted life-years (QALYs), total cost, incremental cost-effectiveness ratio (ICER), willingness-to-pay threshold, and probability of being considered cost-effective; and (5) the study design included SRs of CEAs, prospective cohort studies, and MAs based on RCTs reporting outcomes lasting 24 weeks or longer. Non-human studies and studies without available data were excluded.
Search Strategy
We performed a systematic search for relevant articles in the Cochrane Library, PubMed, Embase, and ISPOR (International Society for Pharmacoeconomics and Outcomes Research) databases to 5 March 2023. The search strategy was adapted for each database. As the eligibility criteria of the rapid review were restricted to studies published in English, a supplementary search of conference papers and abstracts was conducted to ensure all potentially relevant studies had also been identified. The search items included medical subject headings (MeSH) and the keywords such as “semaglutide,” “systematic review,” and “type 2 diabetes mellitus.” The full strategy is shown in Supplementary Table 2.
Study Selection
Two reviewers were used to dual screen at least 20% of the abstracts with conflict resolution. One reviewer screened the remaining abstracts and a second reviewer was used to screen all excluded abstracts and, if needed, resolve conflicts. In addition, one reviewer screened all included full-text articles and a second reviewer was used to screen all excluded full-text articles.
Data Extraction
Extracts from eligible MAs for review included (1) studies; (2) synthesis methods used; (3) population; (4) duration; (5) interventions and comparators; (6) total sample size; (7) number of studies included; (8) estimated treatment differences with 95% confidence intervals (CIs) or credible intervals (CrIs); (9) the statistical methods used (fixed/randomized); (10) heterogeneity; and (11) tests of publication bias if possible. Data from RWS included (1) studies; (2) designs; (3) estimated treatment differences in HbA1c, body weight, and incidence of MACE; and (4) demographics. Additionally, the demographics and essential characteristics of SRs of CEAs such as models and countries were extracted, along with changes in QALYs, total cost, ICERs, and probabilities of being cost-effective.
One reviewer extracted data using a piloted form and another reviewer checked for correctness and completeness of extracted data. Any discrepancies were resolved by a third investigator for the final decision.
Methodological Quality and Risk of Bias Assessment
The methodological quality of the identified intervention MAs was assessed using the current version of the A MeaSurement Tool to Assess Reviews tool (AMSTAR 2) [7]. The tool consists of 16 items covering domains relevant to the quality of systematic reviewing, for which possible assessment responses include “yes,” “partial yes,” or “no.” In our assessments, we followed available guidance documents, where items 2 (protocol), 4 (literature search), 7 (justification for study exclusions), 9 (assessment of risk of bias in individual studies), 11 (methods of synthesis), 13 (incorporation of risk of bias assessment in the interpretation of the results), and 15 (assessment of publication bias) were identified as critical domains. Following the guidance, we classified the overall confidence in the results of the review as either high (maximum of one noncritical weakness), moderate (> one noncritical weakness), low (one critical flaw), or critically low (> one critical flaw).
We report in this rapid review the results of SRs of CEAs evaluating overall quality using the Consolidated Health Economic Evaluation Reporting Standard 2022 (CHEERS 2022) [8], a statement that evaluates the literature based on 24 items in six domains. The quality of the reviews is divided into three categories according to the degree of coverage, including “fully satisfactory,” “partially satisfactory,” and “unsatisfactory.”
RWS were evaluated using the Methods Guide for Comparative Effectiveness Reviews of the US Agency for Healthcare Research and Quality [9]. Five domains of bias (selection bias, performance bias, detection bias, attrition bias, and reporting bias) were assessed. Further, the GRADE (Grading of Recommendations Assessment, Development, and Evaluation) approach was used to rate the quality of the evidence from the MA of RWS and to determine the confidence in effect estimates for our outcomes, which takes into account the risk of bias, publication bias, inconsistency, indirectness, imprecision, effect size and other confounding factors [10]. In addition, we reported the grade of evidence provided by the included RCT-based MAs. A single reviewer graded the certainty of evidence, with all judgments (and footnoted rationales) verified by a second reviewer. The assessments of quality or risk of bias were conducted independently by two authors and any divergence was resolved by discussion.
Synthesis
The RCT-based MA evidence and SRs of CEAs were synthesized narratively, specifying the effect size used in the synthesis or presentation of results for each outcome.
The MA of RWS was conducted in R 4.2.2 using the “meta 6.1” package [11]. Continuous variables were expressed as mean differences (MDs) with their 95% CIs, and dichotomous data were reported as odds ratios (ORs) with 95% CIs. Higgins’ I-squared (I2) was determined as a measure of statistical heterogeneity for each outcome. Values close to 25% were considered to indicate low heterogeneity, I2 values close to 50% were considered to indicate moderate heterogeneity, and values ≥ 75% indicated high heterogeneity [12]. I2 values > 50% indicate a substantial level of heterogeneity. A random-effects model was used to merge the effects; otherwise, a fixed-effects model was used. A sensitivity analysis was conducted to evaluate the influence of each study by omitting one study at a time. Subgroup analysis was performed to explore sources of heterogeneity. Finally, potential publication bias was evaluated by visually inspecting funnel plots as well as through a quantitative analysis of Egger’s test [13].
Results
Study Selection
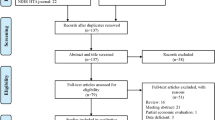
A total of 943 initially relevant publications were identified. 196 duplicate records were removed and 705 records were excluded due to their failure to meet the predetermined eligibility criteria. After full-text screening, five MAs were excluded because the reported outcomes were for less than 24 weeks or an unclear period, and four studies were excluded from the analysis as they failed to report the necessary outcomes. Finally, 33 studies were included in this rapid review [14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46], These studies comprised 22 MAs based on RCTs that compared the efficacy and safety of semaglutide with placebo or other GLP-1 RAs for HbA1c, body weight, and MACE in patients with T2DM [14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35]. Among these, there were two conference abstracts [27, 29] and one MA of a non-SR [15]. Ten prospective cohort studies conducted in real-world settings to examine the impact of semaglutide dosing on variations in HbA1c levels and body weight were also identified [36,37,38,39,40,41,42,43,44,45]. Furthermore, we included a SR of CEAs to comprehensively evaluate the economic implications associated with semaglutide therapy [46]. The results are shown in the PRISMA diagram presented in Fig. 1.
Study Characteristics
For the purpose of our rapid review, we examined various dosages of injectable semaglutide from RCT-based MAs, including 0.05 mg once-daily (QD), 0.1 mg QD, 0.5 mg once-weekly (QW), and 1.0 mg QW, as well as oral dosages of 3 mg QD, 7 mg QD, and 14 mg QD. These dosages were included in our analysis for descriptive purposes, with the aim being to provide a comprehensive overview of the available data under the ideal scenarios in RCTs. Overall, 14 RCT-based MAs reported on the outcomes of HbA1c [14,15,16,17, 19, 23, 26, 28, 30,31,32,33,34,35], of which 8 studies did not restrict the characteristics of the population being treated [14,15,16, 19, 23, 26, 28, 32], 1 MA analyzed drug-naive patients and those receiving metformin-based background therapy [30], 2 MAs evaluated patients receiving 1–2 oral antihyperglycemic drugs (OADs) [31, 35], 2 MAs assessed patients who were previously receiving basal insulin [17, 34], and 1 MA analyzed a population of Japanese patients [33]. Weight outcomes were reported in 15 MAs [14,15,16,17, 19, 21, 23, 26, 28, 29, 31,32,33,34,35], of which 10 studies were not limited to a specific group profile [14,15,16, 19, 21, 23, 26, 28, 29, 32]. Two MAs examined patients receiving 1–2 OADs [31, 35], two MAs analyzed patients who were previously receiving basal insulin [17, 34], and one MA analyzed a population of Japanese patients [33]. Further, six articles reported the estimated effect size in MACE [18, 20, 22, 24, 25, 27]. Most MAs had a low risk of bias in trials and were based on trial-level data.
According to the baseline demographic characteristics of the 10 RWS, there were a total of 3558 participants who were initiating once-weekly subcutaneous semaglutide. All included studies were published between 2021 and 2023. All studies had a single-arm design and were open-label [36,37,38,39,40,41,42,43,44,45].
The one SR of CEAs included studies from high-income countries or high-resource settings, with research contexts focused on Europe and North America; they were mostly payer-based analyses [46].
The characteristics of the MAs, RWS, and SR of CEAs are summarized in Tables 1, 2, and 3, respectively .
Methodological Quality and Risk of Bias
Overall, the methodological quality of the MAs was deemed critically low in 13 studies [14, 16,17,18,19, 23,24,25,26, 31, 33,34,35], low in 4 studies [20,21,22, 28], moderate in 1 study [32], and high in 1 study [30]; 3 publications [15, 27, 29] were deemed inapplicable to the AMSTAR2 (Table 4).
In ten prospective cohort RWS, the overall risk of bias was considered moderate (Fig. 2) and was evaluated as having a low selection bias, performance bias, attrition bias, and reporting bias, but the detection bias was considered high [36,37,38,39,40,41,42,43,44,45]. Also, the presence of other biases was a concern because nine of the studies were sponsored by the manufacturers [36,37,38,39, 41,42,43,44,45] (one was not [40]).
The one identified SR of CEAs in the review was rated overall as “fully satisfactory” and “partially satisfactory” by the majority of the CHEERS 2022 items [46].
Evidence from RCT-Based MAs
The results for HbA1c changes, as presented in Supplementary Table 3, demonstrate a notable reduction in HbA1c levels among subjects receiving semaglutide compared to both the placebo group and other doses of GLP-1 RAs [14,15,16,17, 19, 23, 26, 28, 30,31,32,33,34,35]. However, it is important to note that certain specific comparisons did not yield statistically significant differences. For QD subcutaneous semaglutide, doses of 0.05 mg resulted in a lower reduction in HbA1c versus QD liraglutide 1.8 mg [MD = 0.45%, 95% CI (0.02 to 0.88), p < 0.05]. On the other hand, doses of 0.1 mg did not lead to a statistically significant variance in HbA1c reduction versus QD liraglutide 1.8 mg [MD = 0.13%, 95% CI (− 0.32 to 0.58), p > 0.05]. Similarly, QD oral semaglutide doses of 3 mg [26 weeks, MD = 0.54%, 95% CI (0.33 to 0.75), p > 0.05], 7 mg [26 weeks, MD = 0.15%, 95% CI (− 0.05 to 0.35), p > 0.05], and 14 mg [26 weeks, MD = − 0.1%, 95% CI (− 0.26 to 0.05), p > 0.05] did not result in statistically significant differences in HbA1c reduction compared to QD liraglutide 1.8 mg [16]. In patients receiving basal insulin therapy, no significant difference was observed with QW semaglutide 0.5 mg or QD semaglutide 7 mg versus QD liraglutide 1.8 mg [17, 34]. In patients treated with 1–2 OADs, there was no significant difference between both QW semaglutide 0.5 mg and QD semaglutide 14 mg in comparison with QD liraglutide 1.8 mg or QW dulaglutide 1.5 mg [31, 35]. In addition, the evidence revealed that QW semaglutide 0.5 mg might be as effective as QW exenatide 2 mg [31].
In terms of weight loss efficacy (Supplementary Table 4), medication priority differences were similar to those for glucose lowering. The results revealed significant weight reductions with both oral and subcutaneous semaglutide when compared to placebo and other doses of GLP-1 RAs [14,15,16,17, 19, 21, 23, 26, 28, 29, 31,32,33,34,35], except for specific comparisons that did not exhibit statistically significant differences. Notably, QD subcutaneous semaglutide doses of 0.05 mg [MD = 0.84 kg, 95% CI (− 5.85 to 7.53), p > 0.05] and 0.1 mg [MD = 0.33 kg, 95% CI (− 6.19 to 6.85), p > 0.05], as well as QD oral semaglutide doses of 7 mg [MD = 0.48 kg, 95% CI (− 0.55 to 1.51), p > 0.05] and 14 mg [MD = − 0.71 kg, 95% CI (− 1.56 to 0.14), p > 0.05], were found to be nonsuperior to QW liraglutide 1.8 mg, but QD oral semaglutide 3 mg resulted in a lower weight reduction versus QD liraglutide 1.8 mg [MD = 1.57 kg, 95% CI (− 0.57 to 2.57), p < 0.05] [16]. In patients insufficiently controlled on basal insulin, the weight loss achieved through QW semaglutide 0.5 mg and QD semaglutide 7 mg or 14 mg was not significantly different from the weight loss achieved with other maximum doses of GLP-1 RAs [17, 34]. It was observed that QW semaglutide 0.5 mg appeared to be consistent with twice-daily exenatide 10 μg or QD liraglutide 1.8 mg in patients who were previously receiving 1–2 OADs [31, 35].
Pooled evidence (Supplementary Table 5) showed that subcutaneously administered semaglutide QW significantly reduced the risk of MACE versus placebo and lixisenatide QD (p < 0.05) [18, 20, 22, 24, 25]. However, compared with other GLP-1 RAs, it did not reduce the risk of MACE (p > 0.05). There was no significant difference in QD oral semaglutide versus placebo and other GLP-1 RAs (p > 0.05) [18, 20, 22, 24, 25].
Evidence from Economic Evaluation
The SR of CEAs [46], presented in Supplementary Table 6, showed that the QALYs gain for QW semaglutide 0.5 mg ranged from 0.02 to 0.39 while the QALYs gain for QW semaglutide 1.0 mg ranged from 0.05 to 0.71 when compared to QW exenatide 2 mg, QW dulaglutide, QD lixisenatide, and QD liraglutide. The ICERs showed that QW semaglutide was the dominant strategic therapy, except when comparing QW semaglutide 0.5 mg with QW exenatide 2 mg or QD liraglutide 1.2 mg. However, there was a possibility of an increase in the total cost.
The MA of RWS
Data on MACE derived from the RWS were not available. Consequently, only the data on outcomes related to HbA1c and body weight were submitted to the MA (Supplementary Table 7).
The results of the main analysis (Fig. 3) indicate that, among routine clinical practice patients, QW semaglutide led to a significant reduction in HbA1c levels [MD = − 1.10%, 95% CI (− 1.21, − 0.99), p < 0.00001, I2 = 58%] (Fig. 3A) as well as body weight [MD = − 4.88 kg, 95% CI (− 5.52, − 4.23), p < 0.00001, I2 = 0%] (Fig. 3B). The HbA1c outcome displayed moderate heterogeneity, while no heterogeneity was observed for body weight. The sensitivity analysis results remained unchanged after excluding each study, indicating the robustness of the findings (Supplementary Fig. 1).
A subgroup analysis was conducted to investigate the relationship between changes in HbA1c and baseline HbA1c, obesity classification, the dose at the end of the study, and the proportion of GLP-1 RA-experienced patients in the cohort. A summary of the results is presented in Fig. 4, and Supplementary Figs. 2, 3, 4, and 5 display the generated forest plots. Our analysis showed no significant correlation between baseline variables such as obesity classification, the dose at the end of the study, and the change in HbA1c. In trials where at least 20% of the cohort consisted of patients with prior experience of GLP-1 RAs, semaglutide resulted in less effective reductions in HbA1c [MD = − 0.98%, 95% CI (− 1.11, − 0.84)] compared to cohorts in which less than 20% of the patients had this experience [MD = − 1.19%, 95% CI (− 1.28, − 1.09)]. The interaction was significant (p = 0.01). Furthermore, there could be an interaction between different baseline levels of HbA1c and the HbA1c-lowering effect of semaglutide (p = 0.03). The above findings suggest that both variables played a significant role in the heterogeneity observed in the main analysis.
As shown in Supplementary Fig. 6, visual inspection of the funnel plots for the analyses showed a certain dissymmetry. Furthermore, a quantitative analysis of Egger’s test was performed to detect the publication bias at the level of statistics. The quantitative analysis failed to find a significant presence of publication bias, suggesting that the publication bias was acceptable overall.
Certainty of Evidence
The MAs included in this rapid review lacked comprehensive reporting on evidence certainty. Certainty assessments for HbA1c, body weight, and MACE outcomes are displayed in Supplementary Tables 3, 4, and 5, respectively.
Meanwhile, Table 5 presents the results of the GRADE appraisal of the MA of RWS for each outcome, with a low evidence rating obtained for HbA1c outcome and a moderate evidence rating obtained for body weight outcome.
Discussion
This study is a rapid review conducted to evaluate the efficacy (effectiveness), cardiovascular safety, and cost-effectiveness of semaglutide in patients with T2DM. The review included 22 RCT-based MAs, 1 SR of CEAs, and 10 prospective cohort RWS that were incorporated into a MA.
The included MAs exhibited consistency in the same population, comparison group, and follow-up period. The findings indicate that semaglutide shows reduced efficacy in patients who have received 1–2 OADs or metformin as a background therapy. However, there appears to be consistency in the therapeutic effects of semaglutide among patients who have been administered basal insulin. Further evidence-based studies directly addressing this topic are required to confirm these findings.
In terms of reducing HbA1c levels and weight, liraglutide 1.8 mg QD proved comparable to semaglutide 0.5 mg QW and 7 mg QD but superior to semaglutide 3 mg QD. The MA of RWS demonstrated that the use of QW semaglutide in a diverse population of adults with T2DM in routine clinical practice was associated with clinically significant reductions in HbA1c and body weight. After approximately 30 weeks, HbA1c levels decreased by 1.1% compared to baseline, indicating reduced effectiveness in comparison to the effects reported in the SUSTAIN programs and the identified MAs based on RCTs. Nevertheless, the extent of weight reduction from baseline was parallel to the range of reported effects, with a comparable effect of approximately − 4.88 kg. The statistical analysis of endpoints in RWS utilized the effectiveness analysis set, which has the potential to inflate the estimated effects, while financial sponsorship provided by manufacturers in these trials raises concerns and warrants careful consideration. Moreover, the ongoing COVID-19 pandemic during the SURE program might have affected the study population and the results [47]. Also, Di Dalmazi et al. [48] reported that semaglutide caused more significant reductions in HbA1c and weight compared to the maximum doses of exenatide and dulaglutide available in Italy.
Semaglutide has demonstrated superior efficacy in decreasing MACE in comparison to other GLP-1 RAs presently accessible in the market, except for lixisenatide, where the contrast was insignificant. Previous retrospective studies suggested that the SUSTAIN-6 trial population may not adequately represent the real-world T2DM population in the United States, Spain, China, and the United Kingdom [49,50,51,52]. A meta-regression analysis shows that the cardiovascular benefits of GLP-1 RAs are linked to their beneficial effects on glycemic control [53]. The RWS included in the analysis did not provide information on the incidence of MACE. As a result, additional general trials are required to generate enhanced RWD that can supplement RCTs. Further inquiry is necessary to establish the distinct cardiovascular advantages of semaglutide.
Additionally, it has been observed that oral semaglutide is less effective than the subcutaneous formulation in reducing HbA1c levels, body weight, and the incidence of MACE. Relevant studies have also highlighted significant barriers faced by oral semaglutide, including low bioavailability, poor stability in the gastrointestinal tract, difficulty in crossing epithelial barriers, and variable pharmacokinetics. These challenges make it more difficult to achieve the desired therapeutic levels through oral administration [54]. However, with improved patient adherence to oral administration, there is the potential for advancements in drug delivery systems, particularly through exploring new small-molecule delivery options [55].
In the included SR of CEAs, QW semaglutide was found to be more effective in achieving each endpoint, resulting in a greater gain in QALYs and suggesting that it is a dominant or highly cost-effective treatment compared to other GLP-1 RAs over the projected lifetime horizon. Furthermore, the value of QW semaglutide appeared to be underestimated, particularly when compared to exenatide 2 mg and lixisenatide, as the cardiovascular benefits of QW semaglutide have not been fully captured in current modeling studies. Therefore, the development and improvement of diabetes models that consider cardiovascular outcomes are necessary for further economic evaluation of semaglutide. However, it is important to note that the evidence presented here indicates a decrease in the effectiveness of semaglutide in reducing HbA1c in real-world settings. It is crucial to consider that the clinical input used for the CEAs lacks relevant RWD.
This review has several limitations. The included MAs had low methodological quality, while the included RCTs were deemed to have a low risk of bias, somewhat reducing the quality concerns. The MA conducted in this study included ten open-label trials, and it is important to note that non-masked designs usually inflate the final effect. In real-world settings, the potential bias from open-label trials in physician-reported outcomes can be reduced through careful trial design and analysis methods, especially when patients are aware of the medication being used. Additionally, the relevant studies were limited to Europe and North America, with significant variations in population characteristics from East Asian as well as Southeast Asian groups, including body weight differences. Therefore, it is important to exercise caution when generalizing the findings of this study to non-Western populations. It has been demonstrated that semaglutide has negative effects on the thyroid and pancreas [56], and it caused the highest number of intolerable gastrointestinal adverse reactions among GLP-1 RAs [57]; however, these adverse reactions were not further explored in this study. Finally, despite conducting subgroup and sensitivity analyses, moderate heterogeneity was observed in the HbA1c outcome.
Tirzepatide, a novel QW dual GIP/GLP-1 RA approved by the FDA, was not included in this rapid review, and so comparison results with semaglutide are not available. However, multiple MAs of the SURPASS trial program have shown that tirzepatide, in a dose-dependent manner, demonstrates superior glycemic efficacy and noticeable reductions in body weight compared to other GLP-1 RAs, while maintaining a satisfactory safety profile [58,59,60]. In particular, two CEAs have indicated that the 5, 10, and 15 mg doses of tirzepatide are likely to be cost-effective compared to the 1.0 mg dose of semaglutide for the treatment of T2DM in the United States [61, 62].
Based on the available evidence, the current data suggest that semaglutide exhibits favorable properties in terms of glycemic control, weight loss, and a greater benefit in reducing MACE compared to other GLP-1 RAs. Additionally, our findings indicate that QW semaglutide demonstrates favorable real-world application in routine clinical practice, although its effectiveness in reducing HbA1c may be slightly lower than the ideal scenarios observed in placebo-controlled RCTs. Moreover, semaglutide offers a cost-effective solution for treating T2DM with GLP-1 RAs under current conditions in both Canada and most European countries.
Conclusions
We suggest using semaglutide as the primary medication for T2DM and urge its consideration as the first option in the medical decision-making process among GLP-1 RAs. However, more thorough comparisons of semaglutide with new agents like tirzepatide are necessary to offer medical decision makers a more all-encompassing understanding.
Data Availability
All data generated or analyzed during this study are included in this published article/as supplementary information files.
References
Davies MJ, Aroda VR, Collins BS, et al. Management of hyperglycaemia in type 2 diabetes. a consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetologia. 2022;65(12):1925–66. https://doi.org/10.1007/s00125-022-05787-2.
Nauck MA, Quast DR, Wefers J, et al. GLP-1 receptor agonists in the treatment of type 2 diabetes—state-of-the-art. Mol Metab. 2021;46: 101102. https://doi.org/10.1016/j.molmet.2020.101102.
Blonde L, Khunti K, Harris SB, et al. Interpretation and impact of real-world clinical data for the practicing clinician. Adv Ther. 2018;35(11):1763–74. https://doi.org/10.1007/s12325-018-0805-y.
Cookson R, Mirelman AJ, Griffin S, et al. Using cost-effectiveness analysis to address health equity concerns. Value Health. 2017;20(2):206–12. https://doi.org/10.1016/j.jval.2016.11.027.
Garritty C, Gartlehner G, Nussbaumer-Streit B, et al. Cochrane rapid reviews methods group offers evidence-informed guidance to conduct rapid reviews. J Clin Epidemiol. 2021;130:13–22. https://doi.org/10.1016/j.jclinepi.2020.10.007.
Page MJ, McKenzie JE, Bossuyt PM, et al. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. 2021;372: n71. https://doi.org/10.1136/bmj.n71.
Shea BJ, Reeves BC, Wells G, et al. AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ. 2017;358: j4008. https://doi.org/10.1136/bmj.j4008.
Husereau D, Drummond M, Augustovski F, et al. Consolidated Health Economic Evaluation Reporting Standards 2022 (CHEERS 2022) statement: updated reporting guidance for health economic evaluations. BMC Med. 2022;20(1):23. https://doi.org/10.1186/s12916-021-02204-0.
Viswanathan M, Ansari MT, Berkman ND, et al. Assessing the risk of bias of individual studies in systematic reviews of health care interventions. In: Agency for Healthcare Research and Quality, editor. Methods guide for effectiveness and comparative effectiveness reviews. Rockville, MD: Agency for Healthcare Research and Quality; 2012.
Guyatt GH, Oxman AD, Vist G, et al. GRADE guidelines: 4. rating the quality of evidence–study limitations (risk of bias). J Clin Epidemiol. 2011;64(4):407–15. https://doi.org/10.1016/j.jclinepi.2010.07.017.
Balduzzi S, Rücker G, Schwarzer G. How to perform a meta-analysis with R: a practical tutorial. Evid Based Ment Health. 2019;22(4):153–60. https://doi.org/10.1136/ebmental-2019-300117.
Higgins JP, Thompson SG, Deeks JJ, et al. Measuring inconsistency in meta-analyses. BMJ. 2003;327(7414):557–60. https://doi.org/10.1136/bmj.327.7414.557.
Egger M, Davey Smith G, Schneider M, et al. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315(7109):629–34. https://doi.org/10.1136/bmj.315.7109.629.
Alhindi Y, Avery A. The efficacy and safety of oral semaglutide for glycaemic management in adults with type 2 diabetes compared to subcutaneous semaglutide, placebo, and other GLP-1 RA comparators: a systematic review and network meta-analysis. Contemp Clin Trials Commun. 2022;28: 100944. https://doi.org/10.1016/j.conctc.2022.100944.
Lingvay I, Bauer R, Baker-Knight J, et al. An indirect treatment comparison of semaglutide 2.0 mg vs dulaglutide 3.0 mg and 4.5 mg using multilevel network meta-regression. J Clin Endocrinol Metab. 2022;107(5):1461–9. https://doi.org/10.1210/clinem/dgab905.
Zaazouee MS, Hamdallah A, Helmy SK, et al. Semaglutide for the treatment of type 2 diabetes mellitus: a systematic review and network meta-analysis of safety and efficacy outcomes. Diabetes Metab Syndr. 2022;16(6): 102511. https://doi.org/10.1016/j.dsx.2022.102511.
Chubb B, Gupta P, Gupta J, et al. Once-daily oral semaglutide versus injectable GLP-1 RAs in people with type 2 diabetes inadequately controlled on basal insulin: Systematic review and network meta-analysis. Diabetes Ther. 2021;12(5):1325–39. https://doi.org/10.1007/s13300-021-01034-w.
Duan X-Y, Liu S-Y, Yin D-G. Comparative efficacy of 5 sodium glucose cotransporter 2 inhibitor and 7 glucagon-like peptide 1 receptor agonists interventions on cardiorenal outcomes in type 2 diabetes patients. Medicine (Baltimore). 2021;100(30): e26431. https://doi.org/10.1097/MD.0000000000026431.
Li J, He K, Ge J, et al. Efficacy and safety of the glucagon-like peptide-1 receptor agonist oral semaglutide in patients with type 2 diabetes mellitus: a systematic review and meta-analysis. Diabetes Res Clin Pract. 2021;172: 108656. https://doi.org/10.1016/j.diabres.2021.108656.
Qiu M, Ding LL, Wei XB, et al. Comparative efficacy of glucagon-like peptide 1 receptor agonists and sodium glucose cotransporter 2 inhibitors for prevention of major adverse cardiovascular events in type 2 diabetes: a network meta-analysis. J Cardiovasc Pharmacol. 2021;77(1):34–7. https://doi.org/10.1097/fjc.0000000000000916.
Tsapas A, Karagiannis T, Kakotrichi P, et al. Comparative efficacy of glucose-lowering medications on body weight and blood pressure in patients with type 2 diabetes: a systematic review and network meta-analysis. Diabetes Obes Metab. 2021;23(9):2116–24. https://doi.org/10.1111/dom.14451.
Wei XB, Wei W, Ding LL, et al. Comparison of the effects of 10 GLP-1 RA and SGLT2 inhibitor interventions on cardiovascular, mortality, and kidney outcomes in type 2 diabetes: a network meta-analysis of large randomized trials. Prim Care Diabetes. 2021;15(2):208–11. https://doi.org/10.1016/j.pcd.2020.08.017.
Zhong P, Zeng H, Huang M, et al. Efficacy and safety of subcutaneous and oral semaglutide administration in patients with type 2 diabetes: a meta-analysis. Front Pharmacol. 2021;12: 695182. https://doi.org/10.3389/fphar.2021.695182.
Zhuo C, Lin C, Zhou C, et al. Comparative cardio-renal outcomes of type 2 diabetes patients administered glucagon-like peptide-1 receptor agonists: a network meta-analysis. Front Pharmacol. 2021;12: 759262. https://doi.org/10.3389/fphar.2021.759262.
Alfayez OM, Almohammed OA, Alkhezi OS, et al. Indirect comparison of glucagon like peptide-1 receptor agonists regarding cardiovascular safety and mortality in patients with type 2 diabetes mellitus: network meta-analysis. Cardiovasc Diabetol. 2020;19(1):96. https://doi.org/10.1186/s12933-020-01070-z.
Avgerinos I, Michailidis T, Liakos A, et al. Oral semaglutide for type 2 diabetes: a systematic review and meta-analysis. Diabetes Obes Metab. 2020;22(3):335–45. https://doi.org/10.1111/dom.13899.
Fazioli KT, Borrelli E, Bradt P, et al. PDB9 The comparative efficacy of oral semaglutide for the treatment of type 2 diabetes mellitus (T2DM): a systematic review and network meta-analysis (NMA). Value Health. 2020;23(Supplement 1):S109. https://doi.org/10.1016/j.jval.2020.04.198.
Hussein H, Zaccardi F, Khunti K, et al. Efficacy and tolerability of sodium-glucose co-transporter-2 inhibitors and glucagon-like peptide-1 receptor agonists: a systematic review and network meta-analysis. Diabetes Obes Metab. 2020;22(7):1035–46. https://doi.org/10.1111/dom.14008.
Kakotrichi P, Karagiannis T, Avgerinos I, et al. Comparative effects of medications for type 2 diabetes on body weight: a systematic review and network meta-analysis of 394 trials. Diabetologia. 2020;63(Supplement 1):S257. https://doi.org/10.1007/s00125-020-05221-5.
Tsapas A, Avgerinos I, Karagiannis T, et al. Comparative effectiveness of glucose-lowering drugs for type 2 diabetes: a systematic review and network meta-analysis. Ann Intern Med. 2020;173(4):278–86. https://doi.org/10.7326/M20-0864.
Nuhoho S, Gupta J, Hansen BB, et al. Orally administered semaglutide versus glp-1 ras in patients with type 2 diabetes previously receiving 1–2 oral antidiabetics: Systematic review and network meta-analysis. Diabetes Ther. 2019;10(6):2183–99. https://doi.org/10.1007/s13300-019-00706-y.
Shi FH, Li H, Cui M, et al. Efficacy and safety of once-weekly semaglutide for the treatment of type 2 diabetes: a systematic review and meta-analysis of randomized controlled trials. Front Pharmacol. 2018;9:576. https://doi.org/10.3389/fphar.2018.00576.
Webb N, Orme M, Witkowski M, et al. A network meta-analysis comparing semaglutide once-weekly with other GLP-1 receptor agonists in Japanese patients with type 2 diabetes. Diabetes Ther. 2018;9(3):973–86. https://doi.org/10.1007/s13300-018-0397-1.
Witkowski M, Wilkinson L, Webb N, et al. A systematic literature review and network meta-analysis comparing once-weekly semaglutide with other GLP-1 receptor agonists in patients with type 2 diabetes previously receiving basal insulin. Diabetes Ther. 2018;9(3):1233–51. https://doi.org/10.1007/s13300-018-0428-y.
Witkowski M, Wilkinson L, Webb N, et al. A systematic literature review and network meta-analysis comparing once-weekly semaglutide with other GLP-1 receptor agonists in patients with type 2 diabetes previously receiving 1–2 oral anti-diabetic drugs. Diabetes Ther. 2018;9(3):1149–67. https://doi.org/10.1007/s13300-018-0424-2.
Menzen M, Landsvig Berentzen T, Catarig A-M, et al. Real-world use of once-weekly semaglutide in type 2 diabetes: results from SURE Germany. Exp Clin Endocrinol Diabetes. 2023;131(4):205–15. https://doi.org/10.1055/a-2007-2061.
Mohammedi K, Belhatem N, Berentzen TL, et al. Once-weekly semaglutide use in patients with type 2 diabetes: results from the SURE France multicentre, prospective, observational study. Diabetes Obes Metab. 2023;25(7):1855–64. https://doi.org/10.1111/dom.15045.
Napoli R, Berra C, Catarig AM, et al. Once-weekly semaglutide use in patients with type 2 diabetes: real-world data from the SURE Italy observational study. Diabetes Obes Metab. 2023;25(6):1658–67. https://doi.org/10.1111/dom.15020.
Bellido V, Abreu Padín C, Catarig A-M, et al. Once-weekly semaglutide use in patients with type 2 diabetes: results from the SURE Spain multicentre, prospective, observational study. J Clin Med. 2022;11(17):4938. https://doi.org/10.3390/jcm11174938.
Volpe S, Lisco G, Racaniello D, et al. Once-weekly semaglutide induces an early improvement in body composition in patients with type 2 diabetes: A 26-week prospective real-life study. Nutrients. 2022;14(12):2414. https://doi.org/10.3390/nu14122414.
Wolffenbuttel BHR, Brugts MP, Catarig AM, et al. Once-weekly semaglutide use in type 2 diabetes: real-world data from the SURE Netherlands observational study. Adv Ther. 2023;40(3):920–33. https://doi.org/10.1007/s12325-022-02385-x.
Holmes P, Bell HE, Bozkurt K, et al. Real-world use of once-weekly semaglutide in type 2 diabetes: results from the sure UK multicentre, prospective. Obs Study Diabetes Ther. 2021;12(11):2891–905. https://doi.org/10.1007/s13300-021-01141-8.
Rajamand Ekberg N, Bodholdt U, Catarig AM, et al. Real-world use of once-weekly semaglutide in patients with type 2 diabetes: Results from the SURE Denmark/Sweden multicentre, prospective, observational study. Prim Care Diabetes. 2021;15(5):871–8. https://doi.org/10.1016/j.pcd.2021.06.008.
Rudofsky G, Catarig AM, Favre L, et al. Real-world use of once-weekly semaglutide in patients with type 2 diabetes: Results from the SURE Switzerland multicentre, prospective, observational study. Diabetes Res Clin Pr. 2021;178: 108931. https://doi.org/10.1016/j.diabres.2021.108931.
Yale JF, Catarig AM, Grau K, et al. Use of once-weekly semaglutide in patients with type 2 diabetes in routine clinical practice: Results from the SURE Canada multicentre, prospective, observational study. Diabetes Obes Metab. 2021;23(10):2269–78. https://doi.org/10.1111/dom.14468.
Ruan Z, Yang L, Shi H, et al. The cost-effectiveness of once-weekly semaglutide compared with other GLP-1 receptor agonists in type 2 diabetes: a systematic literature review. Expert Rev Pharmacoecon Outcomes Res. 2021;21(2):221–33. https://doi.org/10.1080/14737167.2021.1860022.
Eberle C, Stichling S. Impact of COVID-19 lockdown on glycemic control in patients with type 1 and type 2 diabetes mellitus: a systematic review. Diabetol Metab Syndr. 2021;13(1):95. https://doi.org/10.1186/s13098-021-00705-9.
Di Dalmazi G, Coluzzi S, Baldassarre M, et al. Effectiveness and tolerability of once-weekly GLP-1 receptor agonists in clinical practice: a focus on switching between once-weekly molecules in type 2 diabetes. Front Endocrinol (Lausanne). 2022;13: 892702. https://doi.org/10.3389/fendo.2022.892702.
Romera I, Artime E, Ihle K, et al. A retrospective observational study examining the generalizability of glucagon-like peptide 1 receptor agonist cardiovascular outcome trials to the real-world population with type 2 diabetes in Spain: the Represent study. Adv Ther. 2022;39(8):3589–601. https://doi.org/10.1007/s12325-022-02196-0.
Boye KS, Sapin H, García-Pérez L-E, et al. The real-world observational prospective study of health outcomes with dulaglutide and liraglutide in type 2 diabetes patients (TROPHIES): baseline patient-reported outcomes. Diabetes Ther Res Treat Educ Diabetes Relat Disord. 2020;11(10):2383–99. https://doi.org/10.1007/s13300-020-00908-9.
Webb J, Mount J, von Arx LB, et al. Cardiovascular risk profiles: a cross-sectional study evaluating the generalizability of the glucagon-like peptide-1 receptor agonist cardiovascular outcome trials REWIND, LEADER and SUSTAIN-6 to the real-world type 2 diabetes population in the United Kingdom. Diabetes Obes Metab. 2022;24(2):289–95. https://doi.org/10.1111/dom.14580.
Cai X, Ji L. Generalizability of the results of cardiovascular outcome trials of glucagon-like peptide 1 receptor agonists in Chinese patients with type 2 diabetes mellitus. Diabetes Ther. 2021;12(7):1861–70. https://doi.org/10.1007/s13300-021-01079-x.
Ghosal S, Sinha B. The cardiovascular benefits of GLP1-RAs are related to their positive effect on glycemic control: a meta-regression analysis. Diabetes Res Clin Pr. 2022;186: 109824. https://doi.org/10.1016/j.diabres.2022.109824.
Bandyopadhyay I, Dave S, Rai A, et al. Oral semaglutide in the management of type 2 DM: clinical status and comparative analysis. Curr Drug Targets. 2022;23(3):311–27. https://doi.org/10.2174/1389450122666210901125420.
Griffith DA, Edmonds DJ, Fortin JP, et al. A small-molecule oral agonist of the human glucagon-like peptide-1 receptor. J Med Chem. 2022;65(12):8208–26. https://doi.org/10.1021/acs.jmedchem.1c01856.
Smits MM, Van Raalte DH. Safety of semaglutide. Front Endocrinol (Lausanne). 2021;12:786732. https://doi.org/10.3389/fendo.2021.645563.
Zhang Z, Zhang Q, Tan Y, et al. GLP-1RAs caused gastrointestinal adverse reactions of drug withdrawal: a system review and network meta-analysis. Front Endocrinol (Lausanne). 2023;14:1149328. https://doi.org/10.3389/fendo.2023.1149328.
Guan R, Yang Q, Yang X, et al. Efficacy and safety of tirzepatide in patients with type 2 diabetes mellitus: a bayesian network meta-analysis. Front Pharmacol. 2022;13: 998816. https://doi.org/10.3389/fphar.2022.998816.
Lisco G, De Tullio A, Disoteo O, et al. Basal insulin intensification with GLP-1RA and dual GIP and GLP-1RA in patients with uncontrolled type 2 diabetes mellitus: A rapid review of randomized controlled trials and meta-analysis. Front Endocrinol (Lausanne). 2022;13: 920541. https://doi.org/10.3389/fendo.2022.920541.
Karagiannis T, Avgerinos I, Liakos A, et al. Management of type 2 diabetes with the dual GIP/GLP-1 receptor agonist tirzepatide: a systematic review and meta-analysis. Diabetologia. 2022;65(8):1251–61. https://doi.org/10.1007/s00125-022-05715-4.
Valentine WJ, Hoog M, Mody R, et al. Long-term cost-effectiveness analysis of tirzepatide versus semaglutide 1.0 mg for the management of type 2 diabetes in the United States. Diabetes Obes Metab. 2023;25(5):1292–300. https://doi.org/10.1111/dom.14979.
Zhang X, McAdam MC. Short-term cost-effectiveness analysis of tirzepatide for the treatment of type 2 diabetes in the United States. J Manag Care Spec Pharm. 2023;29(3):276–84. https://doi.org/10.18553/jmcp.2023.29.3.276.
Acknowledgements
Medical Writing/Editorial Assistance
Special thanks to Kui Yang for editorial assistance provided freely. No funding was required for medical writing and editorial assistance.
Funding
The study and the Rapid Service Fee were funded by the Anhui Province Key Technologies R & D Program of China (grant number 1604a0802097) and China GuangHua Science and Technology Foundation (grant number KY20060212).
Author information
Authors and Affiliations
Contributions
Si-Hua Wang designed the study and drafted and critically revised the manuscript. Si-Hua Wang, Sheng Wang, and Yan Wang contributed to the literature search, literature selection, and data extraction. Si-Hua Wang, Sheng Wang, and Jia-Jie Luan made contributions to the statistical analyses, data interpretation, and assessment of the quality of the studies. All authors critically reviewed the report and approved the final draft. Jia-Jie Luan obtained funding for this study.
Corresponding author
Ethics declarations
Conflict of Interest
Si-Hua Wang, Sheng Wang, Yan Wang and Jia-Jie Luan declare that they have no conflict of interests.
Ethical Approval
This article is based on previously conducted studies and does not contain any new studies with human participants or animals performed by any of the authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Wang, S., Wang, S., Wang, Y. et al. Glycemic Control, Weight Management, Cardiovascular Safety, and Cost-Effectiveness of Semaglutide for Patients with Type 2 Diabetes Mellitus: A Rapid Review and Meta-analysis of Real-World Studies. Diabetes Ther 15, 497–519 (2024). https://doi.org/10.1007/s13300-023-01520-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13300-023-01520-3