Abstract
Introduction
The impact of flash glucose monitoring technology on HbA1c in type 2 diabetes managed by basal bolus insulin is uncertain. Three parallel European retrospective non-interventional chart review studies collected data reported in medical records. Each country’s study aim was to determine the effectiveness of the device on HbA1c when used by their population for 3–6 months as their standard of care for management of glycaemia in a real-world setting.
Methods
Medical records were eligible for adult patients with type 2 diabetes, on a basal bolus insulin regimen for 1 year or more, device use for 3 months or more before the start of the study, an HbA1c concentration up to 3 months prior to starting device use (patients were using blood glucose monitoring for self-management) between 64 and 108 mmol/mol (8.0–12.0%) plus an HbA1c determination 3–6 months after commencing flash glucose monitoring use.
Results
Records were analysed from 18 medical centres in Austria (n = 92), France (n = 88) and Germany (n = 183). Baseline HbA1c results, recorded up to 90 days before the start of device use, were comparable across the three countries and were reduced significantly by 9.6 ± 8.8 mmol/mol mean ± SD (Austria [0.9 ± 0.8%], p < 0.0001), 8.9 ± 12.5 mmol/mol (France [0.8% ± 1.1], p < 0.0001) and 10.1 ± 12.2 mmol/mol (Germany [0.9% ± 1.1], p < 0.0001). No significant differences were detected between age group, sex, BMI or duration of insulin use.
Conclusions
Three European real-world, chart review studies in people with type 2 diabetes managed using basal bolus insulin therapy each concluded that HbA1c was significantly reduced after changing to use of flash glucose monitoring for 3–6 months in a real-world setting.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The impact of flash glucose monitoring technology on HbA1c in type 2 diabetes managed by basal bolus insulin is uncertain |
These three pragmatic parallel European retrospective non-interventional chart review studies aimed to determine the effectiveness of device use as standard of care on HbA1c in a real-world setting over 3–6 months |
Change in HbA1c after device use was significant in all countries; combined analysis demonstrated that HbA1c reduced by − 9.7 mmol/mol ± 0.6 (mean ± SE [− 0.9% ± 0.05], p < 0.0001) |
The studies conclude that flash glucose monitoring use in a real-world setting for 3–6 months in type 2 diabetes managed with basal bolus insulin significantly reduced HbA1c |
Introduction
Currently, the HbA1c determination remains the principal standard method of assessing glycaemic control [1, 2]. The development of continuous glucose monitoring and glucose data availability augments clinical assessment of glycaemic control, particularly as an HbA1c result is unable to reflect time in hypoglycaemia [1]. The benefits of reduced hypoglycaemia and greater treatment satisfaction when flash glucose monitoring is used by individuals with type 2 diabetes managed with prandial insulin is established [3,4,5]. However, improvement in HbA1c in this population using flash monitoring is less certain [3, 5].
The purpose of these retrospective chart reviews was to determine the impact in the real-world of flash glucose monitoring on glycaemic control in patients with type 2 diabetes managed by basal bolus insulin therapy, assessed using HbA1c laboratory data collected from patient records.
Methods
Three parallel European retrospective non-interventional single-arm chart review studies were conducted in Austria, France and Germany (six diabetes centres in each country). The chart reviews included medical records between January 2015 and November 2018 in Austria, March 2017 and January 2019 in France and July 2015 and December 2018 in Germany.
Each centre searched their databases to create a list of potential medical records to be included in the review. As a result of the volume of eligible medical records available in France, a selection was made by the sites on a systematic basis (every nth medical record was selected where n was determined to select approximately 15 records from the list).
Paper or electronic medical records were eligible if they were for patients who were aged 18 years or older, diagnosed with type 2 diabetes, on a basal bolus insulin regimen for 1 year or more, had used the FreeStyle Libre™ Flash Glucose Monitoring System (Abbott, Diabetes Care, Witney, UK) for 3 months or more at the time of data collection (in Austria and Germany the rationale for switching from self- management of blood glucose (SMBG) to FreeStyle Libre device use was not specified; in France an additional inclusion criterion was that device use was driven by patient/physician decision only rather than a self-pay option), had an HbA1c concentration between 8.0% and 12.0% (64–108 mmol/mol) in the 3 months or less before starting to use the device plus an HbA1c measurement taken between 3 and 6 months after commencing use of the device.
Medical records not included in the data collection were for individuals who were pregnant, receiving dialysis treatment or participating in another study that could affect glucose measurements or management during device use.
All HbA1c results were from the medical records at each site. A baseline HbA1c result was defined as being performed 90 days or less before the patient commencing to use the device (index date). If more than one HbA1c test result was available, the most recent HbA1c result to the index date was extracted for use. An HbA1c result 3–6 months after initiation of the device was defined as being performed at least 90 days but less than 194 days following initiation of the device. If more than one HbA1c test was available, the test result closest to 135 days after the index date was used. If the date of starting the device was unclear, e.g. unknown day of the month, a conservative approach was used to ensure the baseline HbA1c value (when glucose monitoring was by SMBG) was before initiation of the device and within 90 days, and the final HbA1c value was within the specified 90–194 days period.
After reviewing their list of medical records for eligibility, sites extracted information that had been entered prior to the index date for age, blood pressure, concomitant disease and diabetes complications, duration of insulin use, height, medications, sex, weight, and device use start date and up to two HbA1c results measured 3–6 months following the start of device use are not entered prior to the index date. The French centres also extracted information for the number of SMBG tests at baseline, and method of insulin administration.
Final eligibility for inclusion in the data analysis was determined by statistical analysis only, utilising the information extracted by the sites.
For all three studies, HbA1c data collected from medical records for the baseline period (prior to the index date) was compared to HbA1c following 3–6 months’ use of flash glucose monitoring (within-patient analysis).
In Germany and Austria, the study protocol was submitted to ethics committees for review (Table S1, Supplementary Material); patient consent was not required as anonymised data was collected. In France, the Institut National des Données de Santé (INDS) was notified of the study and a statement of conformity with Methodology Reference 004 (MR004) was sent to the Commission Nationale de l’informatique et des Libertés (CNIL). Patients were provided with written notification of their pseudo-anonymised data being collected as part of the study and were given an opportunity to opt out.
In line with General Data Protection Regulation requirements a record of processing activities was maintained and communications pertaining to medical records included in the study remained anonymous and did not include any personal identification data [6]. Original data are stored at each study centre.
Outcomes
The primary outcome was evaluation of change from baseline HbA1c results, measured 3 months or less before initiation of device use, to an HbA1c measurement taken between 3 and 6 months after device use commenced.
In all three studies the primary endpoint was also analysed for the following subgroups: baseline HbA1c (< 75 mmol/mol [9.0%] and ≥ 75 mmol/mol [9.0%]), duration of insulin use (< 9 and ≥ 9 years), age (< 65 and ≥ 65 years), BMI (< 30 and ≥ 30), and sex.
In the French study the primary endpoint was also analysed for the following additional subgroups: number of SMBG tests at baseline and method of insulin administration (this information was only recorded in the patient records in this country).
Statistical Analysis
Differences between HbA1c at 3–6 months (90–194 days) after FreeStyle Libre start and baseline were assessed by a paired t test, for each country. To detect a change in HbA1c of 0.35% (3.8 mmol/mol) within each country with a power of 80% (at p < 0.05), a total of 78 medical records are needed, based on an SD of change in HbA1c of 1.1% [7]. For the primary endpoint, if more than one HbA1c test fulfilled the criteria then the test closest to the index date + 135 days was used. Meta-analysis of change in HbA1c was performed using a random effects model, using patient-level data, with country as a random effect. Cochran’s heterogeneity statistic (Q) and the I2 statistic were calculated [8].
Data analysis was performed by qualified statisticians at Abbott Diabetes Care (UK). Version 9.2 of SAS (or higher) was used for all analysis.
Results
All eligible medical records identified by the sites were included in the study (Table 1).
In the Austrian study, 118 medical records were collected and the total number included in the primary endpoint analysis was 92.
In the French study, 97 medical records were collected and the total number included in the primary endpoint analysis was 88.
In the German study, 213 medical records were collected and the total number of medical records included in the primary endpoint analysis was 183.
For the three studies combined, 428 medical records were submitted; the total number of medical records included in the meta-analysis was 363. Start of device use was between January 2015 and July 2018 in Austria, May 2017 and July 2018 in France and September 2015 and August 2018 in Germany. Baseline characteristics and demographics by country are listed in Table 2. Data for medical history are presented in Table 3.
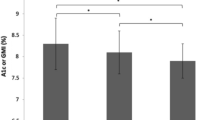
HbA1c decreased in each country; in the Austrian study by 9.6 mmol/mol ± 8.8 mean ± SD (− 0.9% ± 0.8, p < 0.0001), in the French study by 8.9 mmol/mol ± 12.5 (− 0.8% ± 1.1, p < 0.0001) and in the German study by 10.1 mmol/mol ± 12.2 mean ± SD (− 0.9% ± 1.1, p < 0.0001). See Table 4 and Fig. 1.
Combined analysis of the three countries for change in HbA1c after device use was significant. HbA1c measurements reduced by − 9.7 mmol/mol ± 0.6 (mean ± SE [− 0.9% ± 0.05], p < 0.0001) from baseline of 73.3 mmol/mol ± 9.8 mg/dL (mean ± SD, [8.9% ± 0.9]) to 63.6 ± 10.6 mmol/mol [8.0% ± 1.0] in the final phase (days 190–194).
The combined analysis of observed HbA1c improvements showed no heterogeneity between the three countries with an I2 value of 0 (Cochran’s Q = 0.7, p = 0.7113).
Sensitivity Analysis
Mean number of days from start of device use to the final HbA1c value used in the analysis was 136.7 (median 135 days).
Sensitivity analysis on the primary endpoint of change in HbA1c with narrower time windows centred around day 135 demonstrated that the HbA1c result remained the same (Fig. 2).
HbA1c change remained significant when baseline measurements were compared to HbA1c levels for the time windows of 3–4, 4–5, 5–6 and 5.5–6.5 months after device use was started (Fig. 3).
Subgroup Analysis
The decrease in HbA1c from baseline was more pronounced in all three countries for levels ≥ 75 mmol/mol (Fig. 4).
HbA1c improvement was observed across age (< 65 years, ≥ 65 years), sex, duration of insulin use (< 9 years, ≥ 9 years) and BMI (< 30.0 m2, ≥ 30.0 m2) for each country (Fig. 4). There was no significant difference in the effect on HbA1c between subgroups (< 65 vs ≥ 65 years, [p = 0.2767], male/female [p = 0.5990], duration of insulin use [< 9 vs ≥ 9 years, p = 0.2389] or BMI [< 30 vs ≥ 30 kg/m2, p = 0.0785]).
French Study: Additional Subgroup Analysis
Change in HbA1c was unaffected by method of insulin administration (p = 0.2093) improving for both insulin injection users (n = 66, 76%), by − 7.7 mmol/mol ± 12.4 (mean ± SD, [− 0.7% ± 1.1], p < 0.0001) and for insulin pump users (n = 21) by − 11.3 ± 11.2 mmol/mol (− 1.0% ± 1.0, p = 0.0001), Table 5.
Where three or fewer SMBG tests per day were reported at baseline, HbA1c improved; and for more than three reported SMBG tests daily at baseline, HbA1c fell without reaching significance (Table 6).
Discussion
To our knowledge these are the first reported real-world data of flash glucose monitoring use in type 2 diabetes and basal-bolus insulin therapy (delivered by multiple insulin injections or insulin pump). Three European retrospective chart review clinical studies with almost identical methodology demonstrated significant improvement in HbA1c in this population 3–6 months after commencing use of flash glucose monitoring technology. The robust achievement of the primary endpoint in each country is supported by the sensitivity analysis which demonstrates the stability of the effect on HbA1c value. Meta-analysis of the three studies also demonstrated a reduction in HbA1c measurement associated with device use and without any statistical heterogeneity between the three European countries.
The REPLACE study [3], a pre-market randomised controlled trial in a similar population, reported HbA1c improvement in participants younger than 65 years and no change in those older than 65 years. The reason for the contrast in HbA1c outcome in the two studies in unclear. Speculatively, it may in part be due to the less restrictive real-world setting of the current studies, increased healthcare provider familiarity with the technology since 2014 when it became available, improved patient education, patient contact with the diabetes care team and wider experience of reviewing ambulatory glucose profile (AGP) reports for diabetes specialists and patients.
Mean HbA1c reduction of 10.9 mmol/mol (0.9%) in a comparable insulin therapy cohort using real-time continuous glucose monitoring (CGM) was reported by Beck et al. [9] and this finding is supported by the current studies. However, in contrast to Beck et al., the demonstrated HbA1c improvement was achieved without the use of alarms. Glycaemic benefit from real-time CGM use without alarms has been reported previously in type 2 diabetes [10].
Duration of diabetes was not recorded in the current studies; however, the mean age, duration of insulin use, and incidence of micro- and macrovascular complications in the medical records’ data suggest that for many the diagnosis of type 2 diabetes was not recent. For an individual with a similar age and medical history a less stringent personal HbA1c goal of 64–69 mmol/mol (8–8.5%) would likely be agreed at review [1, 11]. For each of the studies, mean HbA1c level at study end was at the lower end of this range following use of flash glucose monitoring.
This meaningful improvement in HbA1c is a notable achievement in a clinical environment rather than a formal clinical trial setting. The expected trajectory of glycaemic control following the introduction of insulin therapy in type 2 diabetes management is a decrease in HbA1c followed by maintenance and an inexorable, slow increase as disease duration progresses [12]. A parallel rise in hypoglycaemic risk and the need for individualised targets offer further challenges to improving glycaemic control. In the current studies, significant HbA1c improvement was observed irrespective of age, an observation which supports the recent finding of Yaron et al. [5] and contrasts with Haak et al. [3] who reported an HbA1c reduction in younger participants only. Furthermore, in the current studies, HbA1c was reduced after the prespecified minimum of 3 months’ device use, or each month thereafter (Fig. 3). Glycaemic benefit has been reported within weeks of sensor data utilisation in a similar population [3] and in an unspecified diabetes population in a recent large real-world study of this technology [13].
The current studies used retrospective, anonymised data extracted from medical records without the need for patient consent. This ethical method of data collection [14] was appropriate as there was virtually no influence on inclusion eligibility by the sites, no effect from patient behaviour, and clinical care was not disrupted by any discussion or administration of the trial allowing the usual standard of diabetes care to be maintained [15]. The entry of changing to a flash sensor monitoring method in the medical record suggests that this decision was likely a result of clinical review and discussion between patient and physician. In Austria, France and Germany reimbursement for flash glucose monitoring technology was possible from 2014 to 2015 and the analysis used data from 2015 onwards.
The demographic and baseline characteristics data extracted from the medical records were broadly similar across the three studies; mean baseline HbA1c value, percentage of data for male patients, age, use of basal bolus insulin therapy, and BMI measurements are comparable to other studies in the same population [3, 9] and to a large, national European database for type 2 diabetes [16].
In line with international guidance [2], the most commonly prescribed oral medication in all three countries was metformin (54–63%, Table 2). Use of oral medications was comparable for the three countries except DPP4 inhibitors and SGLT inhibitors which were notably less used in France (Table 2).
Data for medical history (Table 3) was comparable to other studies in type 2 diabetes for cardiovascular disease [17], previous myocardial infarction [9], renal complications [18], depression [19], neuropathy and peripheral vascular disease [20]. Duration of insulin therapy use and recorded medical history are typical of established type 2 diabetes. In combination, the data extracted are representative of the type 2 diabetes population and the results should be generalizable across clinical care for adults with type 2 diabetes managed with insulin therapy.
It might be assumed that individuals who choose not to test SMBG regularly or frequently will also be non-concordant with scanning or that a minimum daily scanning frequency is needed to gain glycaemic benefit from this technology. In the French centres HbA1c values improved irrespective of a lower SMBG testing frequency reported prior to using the device (Table 6). However, this observation is based on a small quantity of data. A recent small study which reported no association between HbA1c level and SMBG frequency in type 2 suggested that lack of glucose pattern information and education on how to use it is a contributor to suboptimal HbA1c levels in this population when SMBG testing is used to manage their diabetes [21]. A large European real-world study reported a relationship between scanning frequency and glycaemic control. Scanning frequency of about four per day was associated with an HbA1c of 64 mmol/mol (8%) [13].
There are three main strengths in these studies: (1) this is the first reported real-world data for flash glucose technology in type 2 diabetes, (2) the broadly similar methodology across the three studies allowed confident meta-analysis of the results and (3) device use was standard of care for management of glycaemia in each country and not mandated by the protocol. There are some limitations including minimal characteristic and demographic data and other variables such as socio-economic status, education level, ethnicity, duration of diabetes, previous CGM use and the reason for use of the study device. However, usual exclusion criteria such as renal disease [10], planned dialysis [3] or recent myocardial infarction were also not applied, adding to the generalisability of the primary endpoint.
Using the same HbA1c measurement for inclusion and baseline makes this analysis susceptible to regression to the mean. However, in the Yaron et al. study [5], change in HbA1c in the control arm was − 0.33% which gives some indication of the overall magnitude of the combination of regression to the mean and study effect.
Changes made to the regimen during the study were largely unknown although likely as HbA1c was improved [22]. The purpose of device use is to provide information to the user and healthcare provider, support identification of any glycaemic issues and guide changes as necessary; it is not a treatment in itself. As noted by Beck et al. [9], longer-term maintenance of glycaemic benefit from technology use in this population is unknown. Additional, longer-term studies in this population are now required.
Conclusions
These three studies in type 2 diabetes managed with basal bolus insulin or insulin pump therapy demonstrated the glycaemic benefit of improved HbA1c using flash glucose monitoring technology.
References
American Diabetes Association. Standards of medical care in diabetes 2019. Diabetes Care. 2019;42(Suppl 1):S1–S2. https://doi.org/10.2337/dc19-Sint01.
Davies MJ, D’Alessio DA, Fradkin J, et al. Management of hyperglycaemia in type 2 diabetes, 2018. A consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetologia. 2018;2018(61):2461.
Haak T, Hanaire H, Ajjan R, Hermanns N, Riveline J-P, Rayman G. Flash glucose-sensing technology as a replacement for blood glucose monitoring for the management of insulin-treated type 2 diabetes: a multicenter, open-label randomized controlled trial. Diabetes Ther. 2017;8(1):55–73.
Haak T, Hanaire H, Ajjan R, Hermanns N, Riveline J-P, Rayman G. Use of flash glucose-sensing technology for 12 months as a replacement for blood glucose monitoring in insulin-treated type 2 diabetes. Diabetes Ther. 2017;8(3):573–86.
Yaron M, Roitman E, Aharon-Hananel G, et al. Effect of flash glucose monitoring technology on glycemic control and treatment satisfaction in patients with type 2 diabetes. Diabetes Care. 2019;42(7):1178–84. https://doi.org/10.2337/dc18-0166.
European Commission What is personal data? https://ec.europa.eu/info/law/law-topic/data-protection/reform/what-personal-data_en. Accessed 16 Aug 2019.
Abbott Diabetes Care. Data on file. 2015.
Higgins JPT, Thompson SG, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557–60.
Beck RW, Riddlesworth TD, Ruedy K, et al. Continuous glucose monitoring versus usual care in patients with type 2 diabetes receiving multiple daily injections. A randomized trial. Ann Intern Med. 2017. https://doi.org/10.7326/M16-2855.
Ajjan RA, Abougila K, Bellary S, et al. Sensor and software use for the glycaemic management of insulin-treated type 1 and type 2 diabetes patients. Diabetes Vasc Dis Res. 2016;13(3):211–9.
Department of Veterans Affairs and the Department of Defense. VA/DoD clinical practice guideline for the management of type 2 diabetes mellitus in primary care 2017. https://www.healthquality.va.gov/guidelines/CD/diabetes/Vadoddmcpgfinal508.pdf. Accessed 16 Aug 2019.
UK Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet. 1998;352(9131):837–53.
Dunn TC, Xu Y, Hayter G, Ajjan RA. Real-world flash glucose monitoring patterns and associations between self-monitoring frequency and glycaemic measures: a European analysis of over 60 million glucose tests. Diabetes Res Clin Pract. 2018;137(37–4):6.
Council for International Organizations of Medical Sciences (CIOMS). International ethical guidelines for health-related research involving humans. Geneva. 2016 https://cioms.ch/shop/product-category/recently-published/?filterby=ethics. Accessed 12 Sept 2019.
Dal-Ré R, Avendaño-Solà C, Bloechl-Daum B, et al. Low risk pragmatic trials do not always require participants’ informed consent. BMJ. 2019;364:1092.
Blak BT, Thompson M, Dattani H, Bourke A. Generalisability of The Health Improvement Network (THIN) database: demographics, chronic disease prevalence and mortality rates. Inform Prim Care. 2011;19:251–5.
Einarson TR, Acs A, Ludwig C, Panton UH. Prevalence of cardiovascular disease in type 2 diabetes: a systematic literature review of scientific evidence from across the world in 2007–2017. Cardiovasc Diabetol. 2018;17:83.
Lipska KJ, Warton M, Huang ES, et al. HbA1c and risk of severe hypoglycemia in type 2 diabetes the diabetes and aging study. Diabetes Care. 2013;36:3535–42.
Nowakowska M, Zghebi SS, Ashcroft DM, et al. The comorbidity burden of type 2 diabetes mellitus: patterns, clusters and predictions from a large English primary care cohort. BMC Med. 2019;17:145.
Mørkrid K, Ali L, Hussain A. Risk factors and prevalence of diabetic peripheral neuropathy: a study of type 2 diabetic outpatients in Bangladesh. Int J Diabetes Dev Ctries. 2010;30(1):11–7.
Machado S, Marques R, Nascimento E, Matos A, Henriques C. Relationship between HbA1c and capillary blood glucose self-monitoring in type 2 diabetes. Romanian J Intern Med. 2019;57(2):125–32.
Reznik Y, Joubert M. The OPT2MISE study—a review of the major findings and clinical implications. Eur Endocrinol. 2015;11(2):70–4.
Acknowledgements
The authors thank Zoe Welsh and Katie Cranfield for statistical support (Statistics, Abbott, Diabetes Care, UK) and the many individuals involved in the collection of data at the study sites in Austria: Prof. Peter Fasching (Chief Investigator), Wilhelminenspital der Stadt Wien; Dr. Schelkshorn, Landesklinikum Korneuburg—Stockerau; Dr. Brath, Ordination Brath; Prof. Raimund Weitgasser, Diakonissen & Wehrle Privatklinik GmbH Standort Andräviertel; Prof. Ebenbichler, Medizinische Universität Innsbruck; Prof. Pieber, Universitätsklinikum für Innere Medizin); France: Prof. Hélène Hanaire (Chief Investigator), Centre Hospitalier Universitaire Toulouse—Hopital Rangueil, Toulouse; Dr. Salha Fendri, Centre Hospitalier Universitaire Amiens Picardie, Amiens; Dr. Sandrine Favre, Centre Hospitalier Annecy Génevois, Annecy; Prof. Michael Joubert, Centre Hospitalier Universitaire Caen Normandie, Caen; Dr. Clémence Bures, Groupe Hospitalier du Havre, Le Havre; Prof. Pierre-Yves Benhamou, Centre Hospitalier Universitaire Grenoble, Grenoble and Germany: Dr. Jens Kröger (Chief Investigator), Zentrum für Diabetologie, Hamburg, Dr. Ulrich Aigner, Versdias GmbH, Sulzbach-Rosenburg; Dr. Björn Paschen, Diabetologische Schwerpunktpraxis, Harburg; Dr. Ludgar Rose, Institut für Diabetesforschung, Münster; Stephan Maxeiner, Diabetologisch Hausärztliche Gemeinschaftspraxis, Bad Kreuznach; Dr. Oliver Schubert, Diabetologische Schwerpunktpraxis, Buxtehude.
Funding
The study protocols were designed by Abbott, Diabetes Care, Witney UK in collaboration with the principal investigator for each country’s study. Abbott, Diabetes Care provided all study materials, was involved in data, analysis and reporting but was not part of the authors’ interpretation of study results. The journal’s Rapid Service Fee was funded by Abbott, Diabetes Care. All authors had full access to all of the data in these studies and take complete responsibility for the integrity of the data and the accuracy of the data analysis.
Authorship
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship, take responsibility for the integrity of the work as a whole, and have given their approval for this version to be published.
Medical Writing Assistance
Amanda Cartmale provided editorial assistance with manuscript preparation (Scientific Affairs, Abbott, Diabetes Care, UK).
Disclosures
Jens Kröger reports personal fees, non-financial support and other from Abbott, Diabetes Care during the conduct of the study; personal fees, non-financial support and other from Abbott, Diabetes Care outside the submitted work. Hélène Hanaire reports grants from Abbott, Diabetes Care during the conduct of the study; grants from Abbott, Diabetes Care, grants from LifeScan, and other from Roche Diabetes Care outside the submitted work. Peter Fasching reports grants from Medical Science Company Wilhelminenspital during the conduct of the study and personal fees from Abbott, Diabetes Care outside the submitted work.
Compliance with Ethics Guidelines
In Germany and Austria, the study protocol was submitted to ethics committees for review (Table S1, Supplementary Material); patient consent was not required as anonymised data were collected. In France, the Institut National des Données de Santé (INDS) was notified of the study and a statement of conformity with Methodology Reference 004 (MR004) was sent to the Commission Nationale de l’informatique et des Libertés (CNIL). Patients were provided with written notification of their pseudo-anonymised data being collected as part of the study and were given an opportunity to opt out.
Data Availability
The datasets generated during and/or analysed during the current studies are available from the corresponding author on reasonable request.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced Digital Features
To view enhanced digital features for this article go to https://doi.org/10.6084/m9.figshare.11217407.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Kröger, J., Fasching, P. & Hanaire, H. Three European Retrospective Real-World Chart Review Studies to Determine the Effectiveness of Flash Glucose Monitoring on HbA1c in Adults with Type 2 Diabetes. Diabetes Ther 11, 279–291 (2020). https://doi.org/10.1007/s13300-019-00741-9
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13300-019-00741-9