Abstract
Introduction
This study compared the clinical and economic outcomes of long-term use of liraglutide versus sitagliptin for the treatment of type 2 diabetes (T2DM) in real-world practice in the USA.
Methods
We identified adult patients (≥ 18 years old) with T2DM who initiated liraglutide or sitagliptin in 2010–2014 using a large claims database. Quarterly glycemic control measures and annual healthcare costs were assessed during the 1st and 2nd years of persistent medication use. Their associations with medication use (liraglutide or sitagliptin) were estimated using multivariable regression models adjusted for patient demographic and clinical characteristics.
Results
A total of 3113 patients persistently used liraglutide (N = 493) or sitagliptin (N = 2620) for ≥ 1 year [mean age (standard deviation, SD): 53 (8.5) vs. 56 (9.7) years; 48.3% vs. 62.3% males; both p < 0.05]; 911 (including 113 liraglutide users) were persistent users for ≥ 2 years. During the 1st-year follow-up, liraglutide users (versus sitagliptin users, after adjustment) experienced larger glycated hemoglobin (HbA1c) reductions from baseline (ranging from 0.34%-point in quarter 1 to 0.21%-point in quarter 4); higher likelihoods of obtaining HbA1c reductions of ≥ 1%-points or ≥ 2%-points [odds ratios (ORs) range 1.47–2.04]; and higher likelihoods of reaching HbA1c goals of < 6.5% or < 7% (ORs range 1.51–2.12) (all p < 0.05). Liraglutide users also experienced HbA1c reductions from baseline in the 2nd-year follow-up (0.53–0.33%-point, all p < 0.05). Although liraglutide users incurred higher healthcare costs than sitagliptin users during the 1st-year follow-up, they had $2674 (per patient) lower all-cause medical costs (adjusted cost ratio: 0.67, p < 0.05) and similar total costs (all-cause and diabetes-related) in the 2nd year.
Conclusion
Long-term use of liraglutide for 1 or 2 years was associated with better glycemic control than using sitagliptin. Savings in medical costs were realized for liraglutide users during the 2nd year of persistent treatment, which offset differences in pharmacy costs.
Funding
Novo Nordisk Inc.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Diabetes is an emerging global epidemic—this chronic metabolic condition affected 1 in every 11 adults worldwide in 2017 and 9.4% of the US population in 2015 [1, 2]. Diabetes can lead to many micro- and macrovascular complications [3] and accounted for 10.7% of global all-cause mortality among people 20–79 years old [2]. Diabetes was estimated to cost $727 billion (US dollars; USD) in 2017, responsible for 6–16.6% of total healthcare expenditures worldwide [2]. About half of the global diabetes budget is spent in the US, where patients with diagnosed diabetes on average spend about $13700 on medical services annually, which is about 2.3 times higher than that spent by people without diabetes [1].
Type 2 diabetes mellitus (T2DM), characterized by high blood glucose in the context of insulin resistance and relative insulin deficiency, accounts for approximately 90% of all diabetes cases [4]. Due to the progressive nature of diabetes, the initiation of pharmacologic agents is recommended at the time of diagnosis of T2DM, along with lifestyle modifications such as diet and exercise to achieve glycemic control [5,6,7]. With metformin as the preferred 1st-line therapy, additional anti-diabetic drugs are often considered and, as recommended by the American Diabetes Association (ADA), patient’s history of atherosclerotic cardiovascular (CV) disease plays a key role in the selection of the add-on therapy [5].
Liraglutide, which belongs to the class of glucagon-like peptide-1 (GLP-1) receptor agonists, is a commonly used anti-diabetic therapy. It was shown to reduce the risk of major adverse CV events in a recent clinical trial [8], and it is currently the only agent in its class that has been approved to reduce the risk of major adverse cardiovascular events (cardiovascular death, nonfatal MI or nonfatal stroke) in adults with T2DM and established cardiovascular disease [5].
The efficacy and safety of liraglutide for the treatment of T2DM has been extensively studied in clinical trials. Liraglutide demonstrated superior glycemic control, greater weight loss, and better treatment satisfaction after 52 weeks as an add-on to metformin compared with another incretin-based therapy, sitagliptin [a dipeptidyl peptidase-4 (DPP-4) inhibitor] [9]. The findings were consistent with those observed at a shorter follow-up period [10,11,12], while gastrointestinal problems were common adverse reactions to liraglutide [13]. Based on data from the clinical trials, the annual mean cost per patient was estimated to be $5103–$6523 (2012 USD) lower with liraglutide than with sitagliptin to reach glycated hemoglobin (HbA1c) < 7.0% with no hypoglycemia or weight gain, and liraglutide was shown to be more cost-effective than sitagliptin after 5 years of use [14, 15].
Many studies have investigated the effectiveness of liraglutide outside the controlled settings of clinical trials, with recent attention paid to the long-term use of the therapy [16]. A 2-year prospective study of routine clinical practice in France found liraglutide to be as effective as observed in clinical trials [17]. However, the effectiveness of liraglutide and sitagliptin has usually been compared in a 6-month treatment period [18,19,20,21]. Effectiveness for a longer duration has only been examined in a 1-year survey conducted in the UK from 2009 to 2011 [22].
Data on the long-term effectiveness of liraglutide are needed to provide healthcare providers and patients with additional information to support T2DM treatment and management decisions. This study investigated the clinical and cost-effectiveness of liraglutide compared with sitagliptin in the US in a real-world setting for 1 and 2 years of treatment.
Methods
Data Source
This retrospective observational cohort study utilized data from January 2010 through December 2014 from the Truven Health MarketScan® Commercial and Medicare Supplemental Insurance Databases. The databases contain administrative claims and eligibility records for more than 30 million commercially insured individuals (i.e., working-age adults and their dependents) and 3 million enrollees in Medicare supplemental plans. The data represent the healthcare experience of employees, dependents, and retirees with primary or Medicare supplemental coverage through privately insured health plans. Data from the Truven Health MarketScan® Lab database, which contains 32.6 million laboratory test results for approximately 1.9 million unique privately insured patients, were linked to each patient’s healthcare claims. This article does not contain any studies with human participants or animals performed by any of the authors.
Sample Selection
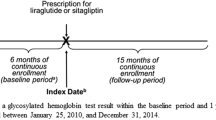
The study sample included patients with prescription fills of either liraglutide (Victoza®) or sitagliptin (Januvia® or Janumet®) between 1 January 2010 and 31 December 2014. The first pharmacy claim for liraglutide or sitagliptin defined the index therapy and the index date. Patients were required to be at least 18 years old at the index date and have continuous medical and pharmacy plan enrollment for at least 6 months prior to (the baseline period) and 12 months after the index date. Patients were excluded if they (1) had a prescription fill of any GLP-1 receptor agonist or any DPP-4 inhibitor during the baseline period or (2) had a diagnosis of type 1 diabetes, secondary diabetes, gestational diabetes, or pregnancy through the baseline period until the end of continuous health plan enrollment. Patients had to have at least one HbA1c measure around the index date (from 45 days prior to 7 days after the index date) and at least one HbA1c measure during the 1-year follow-up (from 45 days post index date to 45 days after the end of the follow-up period).
The study focused on patients who continuously used the index therapy during the follow-up periods (1 and 2 years, respectively) [23]. Patients who stopped using their index treatment for at least 90 consecutive days without a prescription fill were considered to have discontinued treatment [19]. Patients with any use of the competing therapy (i.e., sitagliptin for the liraglutide cohort and vice versa) during the follow-up period were excluded.
Study Measures
Patient characteristics included demographics measured at the index date (age, gender, geographic region, health plan type, and year of treatment initiation), baseline HbA1c (defined as the mean of values observed between 45 days prior to 7 days after the index date), and clinical characteristics measured over the 6-month baseline period: any visit to an endocrinologist; Charlson Comorbidity Index (CCI) [24]; the occurrence of common diabetes-related complications (i.e., retinopathy, nephropathy, neuropathy) and comorbidities (i.e., cardiovascular diseases, depression, obesity, hypertension, and hyperlipidemia) identified via the International Classification of Diseases, Ninth Revision, Clinical Modification (ICD-9-CM) codes [25]; and use of anti-diabetic drugs.
This study examined the following glycemic control endpoints: absolute reduction in HbA1c from baseline; reductions in HbA1c of ≥ 1%-points and ≥ 2%-points; and HbA1c goal attainment (< 6.5% and < 7%). The glycemic control endpoints were measured at the end of each quarter during the 1st year of persistent use of the index therapies, where the quarterly follow-up HbA1c was the mean value in the 45-day window at the end of a quarter. Quarterly HbA1c was also measured during the 2nd year of persistent use among the subgroup of patients continuously enrolled in their health plan and persistently used their index therapy without competing drugs for at least 2 years. Annual healthcare costs during the 1st and 2nd year of persistent use of the index therapy were examined. Annual all-cause costs were measured by medical and pharmacy claims paid by patients and insurers. Diabetes-related costs were identified by ICD-9-CM diagnosis codes (250.xx) on medical claims and by anti-diabetic drug types from pharmacy claims. All costs were adjusted to the 2016 value based on the Consumer Price Index Medical Component [26].
Statistical Analysis
The study measures were compared between treatment groups using Student’s t test for continuous variables and the chi-square test for categorical variables. Generalized linear model (GLM) regressions, specific to the outcome distribution, were used to assess the adjusted association between the index therapy (liraglutide or sitagliptin) and the outcomes.
Ordinary least squares regression was used to assess the relationship between the index therapy and quarterly measures of absolute HbA1c reductions from baseline during the 1st and 2nd year of persistent use. Logistic regression was used for the quarterly measures of HbA1c reductions of ≥ 1%- and ≥ 2%-points and HbA1c goal attainment. A generalized estimating equation (GEE) approach was incorporated to account for multiple observations per individual. The regression adjusted for patient demographic characteristics, baseline HbA1c and other baseline clinical characteristics, and time-varying covariates (any use of other non-insulin anti-diabetic medications and any use of insulin in each quarter).
The coefficients on liraglutide versus sitagliptin were reported, including the direct impact on absolute HbA1c reduction from baseline, and the odds ratio (OR) for HbA1c reduction of ≥ 1%- and ≥ 2%-points and HbA1c goal attainment. Based on the regression results, the differences in quarterly glycemic control endpoints associated with liraglutide versus sitagliptin (i.e., marginal effects) were estimated using the method of recycled predictions, where the adjusted outcomes were predicted for each patient in the sample by assuming liraglutide or sitagliptin as the index therapy, respectively [27].
The annual healthcare costs during the persistent use of index therapy were analyzed by GLM with log link and gamma distribution. The regressions were adjusted for patient demographic characteristics and the following baseline covariates: HbA1c, other clinical characteristics, drug use, and total healthcare costs (all cause or diabetes related). The cost regressions for the 2nd year of persistent use of the index therapy were also adjusted for drug use during the 1st year of follow-up. The ratio of costs associated with liraglutide versus sitagliptin was generated from the regression. The method of recycled predictions was used to estimate differences in costs between liraglutide and sitagliptin users.
Results
The study sample included 3113 patients (493 in the liraglutide cohort and 2620 in the sitagliptin cohort) who had persistently used the index therapy for at least 12 months after applying inclusion/exclusion criteria (Fig. 1). The characteristics of patients in the liraglutide cohort differed from those in the sitagliptin cohort in many aspects (Table 1). Liraglutide users were younger [mean age (standard deviation, SD): 53 (8.5) years vs. 56 (9.7) years], less likely to be male (48.3% vs. 62.3%), more likely to live in the South, and more likely to be enrolled in health plans covering out-of-network services (all p < 0.05). In addition, liraglutide users were more likely to visit endocrinologists, use insulin, and have a diagnosis of obesity or hypertension during the baseline period (all p < 0.05). Baseline HbA1c was similar between the cohorts [8.1 (1.7) % vs. 8.2 (1.7) %; p ≥ 0.05]. The mean HbA1c reduction among liraglutide users during follow-up ranged from 1.2 (%-point) in quarter 1 to 0.9 in quarter 8; reductions ranged from 0.9 to 0.4 among sitagliptin users (Table 2). Baseline pharmacy costs were higher in the liraglutide group than the sitagliptin group before starting index therapy (Table 1). Medical costs were also higher at baseline for the liraglutide group; however, differences were not statistically significant.
After adjustment for covariates, use of liraglutide was associated with a higher reduction in HbA1c from baseline in all quarters during the 1st year of follow-up, as reflected by the positive coefficients (all p < 0.05; Table 3). Specifically, the larger reduction in HbA1c associated with the use of liraglutide versus sitagliptin was estimated to range from 0.34 (%-point) [95% confidence interval (CI) 0.23, 0.45] in quarter 1 to 0.21 (95% CI 0.07, 0.35) in quarter 4. The use of liraglutide was also associated with a higher likelihood of obtaining an HbA1c reduction of ≥ 1%-points [ORs ranging from 1.47 to 2.37] and reductions of ≥ 2%-points (ORs ranging from 1.67 to 2.04; all p < 0.05). Lastly, the use of liraglutide was associated with a higher likelihood of attaining HbA1c goals: with ORs around 2 of achieving HbA1c < 6.5% and around 1.6 of achieving HbA1c < 7% in all quarters (all p < 0.05). Among the patients with at least 2 years of persistent use of the index therapy, the use of liraglutide was associated with a higher reduction in HbA1c in all quarters during the 2nd year of follow-up as well as with a higher chance of an HbA1c reduction of ≥ 1%-points (except for quarter 6), of achieving HbA1c < 6.5% (except for quarter 6), and of achieving HbA1c < 7% (in quarter 5) (all p < 0.05). The small sample size was insufficient to estimate the association between HbA1c reduction ≥ 2%-point and persistent use of index therapy during the 2nd year of follow-up.
Adjusted outcomes and the marginal effects of liraglutide versus sitagliptin were calculated (Figs. 2, 3). The marginal effects on HbA1c reductions from baseline were the same as the regression coefficients due to the model specification. For the other endpoints, 13.4% more patients (48.1% vs. 34.7%, p < 0.05) would obtain HbA1c reduction ≥ 1%-point and 4.4% more (21.9% vs. 17.5%, p < 0.05) would obtain HbA1c reduction ≥ 2%-point in quarter 1 if they used liraglutide rather than sitagliptin, and 10.4% more (34.5% vs. 24.1%, p < 0.05) or 10.5% more (57.4% vs. 46.9%, p < 0.05) patients would reach an HbA1c goal of < 6.5% or < 7.0% in quarter 1, respectively (all p < 0.05). The marginal effects were stable across all quarters during the 1st year of persistent medication use, while more variation was observed during the 2nd year of persistent medication use.
Adjusted glycemic control outcomes during the 1st-year persistent use of liraglutide or sitagliptin. *p < 0.05. Outcomes adjusted for baseline characteristics and time-varying covariates (any used of other non-insulin anti-diabetic medications, and any use of insulin in each quarter). HbA1c glycated hemoglobin
Adjusted glycemic control outcomes during the 2nd-year persistent use of liraglutide or sitagliptin. *p < 0.05. Outcomes adjusted for baseline characteristics and time-varying covariates (any used of other non-insulin anti-diabetic medications, and any use of insulin in each quarter). Based on a subgroup of patients with persistent use of index medications for ≥ 24 months (liraglutide cohort; N = 113; sitagliptin cohort: N = 798). HbA1c glycated hemoglobin
The unadjusted and adjusted predicted costs for each cohort, along with the cost ratios, for the 1st and 2nd years of persistent treatment are presented in Table 4. The adjusted total and medical costs in each cohort and year of follow-up are also illustrated in Fig. 4. In the 1st year, there was no difference in medical costs between persistent users of liraglutide and sitagliptin. The liraglutide cohort had higher total costs (both all cause and diabetes related) than the sitagliptin cohort due to the higher pharmacy costs (p < 0.05). During the 2nd year of persistent drug use, all-cause medical costs were 33% lower for liraglutide patients than sitagliptin patients (adjusted cost ratio 0.67, 95% CI 0.50, 0.89), resulting in a savings of $2674 per patient (adjusted costs: $5410 vs. $8084, p < 0.05). This saving offset the higher pharmacy costs observed in the liraglutide group in the 2nd year and resulted in $602 lower all-cause total costs than in the sitagliptin group (not statistically significant). No significant differences between the cohorts were found for the diabetes-related medical costs and total costs during the 2nd-year follow-up.
Adjusted annual healthcare costs during persistent use of liraglutide or sitagliptin. *p < 0.05. aOutcomes adjusted for baseline characteristics. bBased on a subgroup of patients with persistent use of index medications for ≥ 24 months (liraglutide cohort: N = 113; sitagliptin cohort: N = 798); and outcomes adjusted for baseline characteristics and drug use in the 1st year of follow-up (any use of other non-insulin anti-diabetic medications, and any use of insulin)
Discussion
This study extends previous studies by providing integrated evidence on the long-term clinical and cost-effectiveness of treatment with liraglutide versus sitagliptin in real-world clinical practice in the US. Even after adjusting for baseline patient characteristics and the use of antidiabetic medications during follow-up, we found that patients persistently using liraglutide for 1 or 2 years experienced improved glycemic control (in terms of higher reduction of HbA1c from baseline, higher likelihood to reach high reduction in HbA1c, and higher likelihood to reach HbA1c target levels) compared with those using sitagliptin. Patients in both cohorts incurred similar medical costs during the 1st year of medication use, while during the 2nd year, liraglutide users had significantly lower all-cause medical costs, which offset their higher pharmacy costs than sitagliptin users.
The 6-month clinical effectiveness of liraglutide in this study is similar to previously published data. Compared with sitagliptin, use of liraglutide has been found to be associated with 0.31–0.41 (%-point) greater reduction of HbA1c from baseline, an 8–15% greater chance to reach HbA1c < 7%, and an 11% greater chance to reach A1C ≤ 6.5% after 6 months since treatment initiation [18, 19], and these were reflected by $994 (2013 US dollar) lower diabetes-related medical costs during the 6 months of follow-up (all p < 0.05) [19].
Trends of clinical effectiveness over 2 years of medication use continued to be favorable for liraglutide versus sitagliptin, as found in our study. Specifically, the difference in HbA1c reduction between the two treatments was highest after 3 months of medication use and then stabilized for the remainder of the year; no obvious trend was observed in the effectiveness in terms of likelihood to obtain high HbA1c reduction or reach HbA1c goals in the 1st year of follow-up. During the 2nd year of medication use, there was much more variation over time in the clinical effectiveness of liraglutide versus sitagliptin, possibly because of the small sample size (liraglutide cohort: N = 113; sitagliptin cohort: N = 798); nevertheless, the clinical effectiveness of liraglutide remained stable.
The improved glycemic control associated with liraglutide relative to sitagliptin led to cost savings, especially for patients treated for longer than 1 year. The findings on the costs during the 2nd year of persistent treatment may be obscured because of the small sample size and large variation in healthcare costs. Thus, a post hoc analysis was conducted on annual costs after the 1st year of persistent use of the index therapy among patients who did not necessarily have persistent use of index therapy during the 2nd year after treatment initiation. The results from the post hoc analysis showed that after 1 year of persistent treatment, medical costs (both diabetes related and all cause) were significantly lower in the liraglutide cohort (Supplementary Appendix Table 6). Further, no difference between the cohorts was found in the annual costs for diabetes-related healthcare, and the annual all-cause healthcare costs were significantly lower for the liraglutide cohort.
The summary statistics of healthcare resource utilization (see Supplementary Appendix Table 5 for results) showed lower use of inpatient and emergency room services when taking liraglutide. Specifically, patients treated with liraglutide had a shorter length of hospital stay during the 1st year [all-cause, mean days (SD): 0.2 (1) vs. 0.4 (2.3); diabetes-related, 0.2 (0.8) vs. 0.3 (1.9); all p < 0.05] and 2nd year [all cause: 0.1 (0.6) vs. 0.4 (2.3); diabetes related, 0.1 (0.6) vs. 0.3 (2.0); all p < 0.01] of persistent treatment than sitagliptin users. Liraglutide users also had fewer visits to the emergency department during the 2nd year of persistent treatment. No differences between treatment groups were observed in other healthcare resource utilization. These findings suggest that hospitalization and emergency room visits may be the main drivers of cost savings associated with liraglutide, and further research is warranted to investigate this hypothesis.
The lower medical costs in the liraglutide cohort compared with sitagliptin during the 2nd year of persistent treatment were statistically significant for all-cause healthcare services, but not for diabetes-related services. This may reflect the nonglycemic benefits of liraglutide (including weight loss and reduced risks of CV events), while sitagliptin had neutral effects [5]. The finding also suggests that better glycemic control can improve a patient’s overall health.
Our analyses adjusted for many potential confounding factors including demographics, baseline clinical characteristics, baseline healthcare costs, and the use of antidiabetic agents during the follow-up period. During the 1st year of persistent medication use, more than 80% of the patients used oral antidiabetic medications (mostly metformin) in conjunction with liraglutide or sitagliptin. Patients in the liraglutide cohort were more likely to use insulin than those in the sitagliptin cohort during both the baseline and follow-up periods (p < 0.05; results not shown), but the need for add-on insulin increased more quickly in the sitagliptin cohort. Specifically, the percentages of patients using insulin in the liraglutide cohort versus the sitagliptin cohort were 19.5% vs. 6.7% in the 6-month baseline period and 21.5% vs. 11% in the 1st year of follow-up. This may indicate that liraglutide was more successful in reaching the treatment goal and/or patient satisfaction and thus was associated with less need to intensify treatment with insulin.
The results of this study should be interpreted with consideration of the limitations associated with studies based on administrative claims data. First, due to the nonexperimental nature of the data and the study design, this study does not allow for causal inferences; unmeasured confounders such as prescription bias may influence the results. Our study considered a wide range of covariates, including socio-demographic and clinical measures, to reduce the residual confounding. Second, although clinical trials determined the efficacy of liraglutide 1.2 mg separately from 1.8 mg, our study considered the overall use of liraglutide. It is challenging to calculate the dose of liraglutide used in clinical practice from claims data since the National Drug Codes may not completely capture the clinical practice of dosing and titration, which may also vary over the considered follow-up period. Third, HbA1c measurements were available for only a subset of T2DM patients; the availability of HbA1c is not expected to be related with patient characteristics and thus should not lead to bias in our findings. Finally, patients 65 years or older are under-represented since the MarketScan databases used in this study contain only Medicare enrollees who purchased supplemental commercial health insurance. However, MarketScan is one of the largest commercial healthcare claims databases in the US, and our findings can be interpreted in a population with commercial health insurance.
Conclusion
In real-world clinical practice in the US, long-term use of liraglutide for 1 or 2 years was associated with better glycemic control compared with sitagliptin. The medical costs were similar between liraglutide users and sitagliptin users during the 1st year of persistent treatment, but savings in medical costs were realized for liraglutide users during the 2nd year of persistent treatment, which offsets differences in pharmacy costs.
References
Centers for Disease Control and Prevention (CDC). National Diabetes Statistics Report, 2017: estimates of diabetes and its burden in the United States. https://www.cdc.gov/diabetes/pdfs/data/statistics/national-diabetes-statistics-report.pdf. Accessed 29 January 2018.
International Diabetes Federation (IDF). IDF Diabetes Atlas—8th Edition. http://www.diabetesatlas.org/. Accessed 29 January 2018.
Group AC, Patel A, MacMahon S, Chalmers J, Neal B, Billot L, et al. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Engl J Med. 2008;358(24):2560–72.
Centers for Disease Control and Prevention (CDC). At a glance 2016: diabetes. https://www.cdc.gov/chronicdisease/resources/publications/aag/pdf/2016/diabetes-aag.pdf. Accessed 12 April 2017.
ADA. Pharmacologic approaches to glycemic treatment: standards of medical care in diabetes. Diabetes Care. 2018;41(Suppl 1):S73–85.
International Diabetes Federation (IDF). Treatment algorithm for people with type 2 diabetes. http://www.idf.org/treatment-algorithm-people-type-2-diabetes. Accessed 3 Feb 2016.
National Institute for Health and Care Excellence (NICE). Algorithm for blood glucose lowering therapy in adults with type 2 diabetes 2015. http://www.nice.org.uk/guidance/ng28/resources/algorithmfor-blood-glucose-lowering-therapy-in-adults-withtype-2-diabetes-2185604173. Accessed 3 Feb 2016.
Marso SP, Daniels GH, Brown-Frandsen K, Kristensen P, Mann JF, Nauck MA, et al. Liraglutide and cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2016;375(4):311–22.
Pratley R, Nauck M, Bailey T, Montanya E, Cuddihy R, Filetti S, et al. One year of liraglutide treatment offers sustained and more effective glycaemic control and weight reduction compared with sitagliptin, both in combination with metformin, in patients with type 2 diabetes: a randomised, parallel-group, open-label trial. Int J Clin Pract. 2011;65(4):397–407.
Pratley RE, Nauck M, Bailey T, Montanya E, Cuddihy R, Filetti S, et al. Liraglutide versus sitagliptin for patients with type 2 diabetes who did not have adequate glycaemic control with metformin: a 26-week, randomised, parallel-group, open-label trial. Lancet. 2010;375(9724):1447–56.
Charbonnel B, Steinberg H, Eymard E, Xu L, Thakkar P, Prabhu V, et al. Efficacy and safety over 26 weeks of an oral treatment strategy including sitagliptin compared with an injectable treatment strategy with liraglutide in patients with type 2 diabetes mellitus inadequately controlled on metformin: a randomised clinical trial. Diabetologia. 2013;56(7):1503–11.
King AB, Montanya E, Pratley RE, Blonde L, Svendsen CB, Donsmark M, et al. Liraglutide achieves A1C targets more often than sitagliptin or exenatide when added to metformin in patients with type 2 diabetes and a baseline A1C < 8.0%. Endocr Pract. 2013;19(1):64–72.
Li M, Yang Y, Jiang D, et al. Efficacy and safety of liraglutide versus sitagliptin both in combination with metformin in patients with type 2 diabetes: a systematic review and meta-analysis. Medicine. 2017;96(39):e8161.
Langer J, Hunt B, Valentine WJ. Evaluating the short-term cost-effectiveness of liraglutide versus sitagliptin in patients with type 2 diabetes failing metformin monotherapy in the United States. J Manag Care Pharm JMCP. 2013;19(3):237–46.
Lee WC, Samyshkin Y, Langer J, Palmer JL. Long-term clinical and economic outcomes associated with liraglutide versus sitagliptin therapy when added to metformin in the treatment of type 2 diabetes: a CORE Diabetes Model analysis. J Med Econ. 2012;15(Suppl 2):28–37.
Ostawal A, Mocevic E, Kragh N, Xu W. Clinical effectiveness of liraglutide in type 2 diabetes treatment in the real-world setting: a systematic literature review. Diabetes Ther Res Treat Educ Diabetes Relat Disord. 2016;7(3):411–38.
Gautier JF, Martinez L, Penfornis A, Eschwege E, Charpentier G, Huret B, et al. Effectiveness and persistence with liraglutide among patients with type 2 diabetes in routine clinical practice—EVIDENCE: a prospective, 2-year follow-up, observational, post-marketing study. Adv Ther. 2015;32(9):838–53.
Lee WC, Dekoven M, Bouchard J, Massoudi M, Langer J. Improved real-world glycaemic outcomes with liraglutide versus other incretin-based therapies in type 2 diabetes. Diabetes Obes Metab. 2014;16(9):819–26.
Li Q, Chitnis A, Hammer M, Langer J. Real-world clinical and economic outcomes of liraglutide versus sitagliptin in patients with type 2 diabetes mellitus in the United States. Diabetes Ther Res Treat Educ Diabetes Relat Disord. 2014;5(2):579–90.
Lind M, Matsson PO, Linder R, Svenningsson I, Jorgensen L, Ploug UJ, et al. Clinical effectiveness of liraglutide vs sitagliptin on glycemic control and body weight in patients with type 2 diabetes: a retrospective assessment in Sweden. Diabetes Ther Res Treat Educ Diabetes Relat Disord. 2016;7(2):321–33.
Nyeland ME, Ploug UJ, Richards A, Garcia Alvarez L, Demuth D, Muthutantri A, et al. Evaluation of the effectiveness of liraglutide and sitagliptin in type 2 diabetes: a retrospective study in UK primary care. Int J Clin Pract. 2015;69(3):281–91.
Evans M, McEwan P, O’Shea R, George L. A retrospective, case-note survey of type 2 diabetes patients prescribed incretin-based therapies in clinical practice. Diabetes Ther Res Treat Educ Diabetes Relat Disord. 2013;4(1):27–40.
Maciejewski ML, Bryson CL, Wang V, Perkins M, Liu CF. Potential bias in medication adherence studies of prevalent users. Health Serv Res. 2013;48(4):1468–86.
D’Hoore W, Bouckaert A, Tilquin C. Practical considerations on the use of the Charlson comorbidity index with administrative data bases. J Clin Epidemiol. 1996;49(12):1429–33.
Young BA, Lin E, Von Korff M, Simon G, Ciechanowski P, Ludman EJ, et al. Diabetes complications severity index and risk of mortality, hospitalization, and healthcare utilization. Am J Manag Care. 2008;14(1):15–23.
United States Department of Labor, Bureau of Labor Statistics. Consumer Price Index 2014. http://www.bls.gov/cpi/. Accessed 12 April 2017.
Graubard BI, Korn EL. Predictive margins with survey data. Biometrics. 1999;55(2):652–9.
Acknowledgements
Funding
Novo Nordisk Inc. provided the funding for the study and the article processing charges. All authors had full access to all of the data in this study and take complete responsibility for the integrity of the data and accuracy of the data analysis.
Editorial Assistance
Editorial support was provided by Colleen Dumont, an employee of Evidera, and was funded by Novo Nordisk Inc.
Authorship
All authors participated in data analysis and interpretation and contributed to the development of the manuscript. All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval to the version to be published.
Disclosures
Qian Li is employed by Evidera (a division of PPD), which provides consulting and other research services to pharmaceutical, medical device, and related organizations. In their salaried positions, they work with a variety of companies and organizations and are precluded from receiving payment or honoraria directly from these organizations for services rendered. Evidera received funding from Novo Nordisk Inc. to participate in the study and for the development of this manuscript. Rahul Ganguly is employed by Novo Nordisk Inc. Michael Ganz is employed by Evidera (a division of PPD), which provides consulting and other research services to pharmaceutical, medical device, and related organizations. In their salaried positions, they work with a variety of companies and organizations and are precluded from receiving payment or honoraria directly from these organizations for services rendered. Evidera received funding from Novo Nordisk Inc. to participate in the study and for the development of this manuscript. Cory Gamble is employed by Novo Nordisk Inc. Tam Dang-Tan is employed by Novo Nordisk Inc.
Compliance with Ethics Guidelines
This article does not contain any studies with human participants or animals performed by any of the authors.
Data Availability
The data sets generated and/or analyzed during the current study are not publicly available because of data license agreement, but programming codes are available from the corresponding author upon reasonable request.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced Digital Features
To view enhanced digital features for this article, go to https://doi.org/10.6084/m9.figshare.6133790.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Li, Q., Ganguly, R., Ganz, M.L. et al. Real-World Clinical Effectiveness and Cost Savings of Liraglutide Versus Sitagliptin in Treating Type 2 Diabetes for 1 and 2 Years. Diabetes Ther 9, 1279–1293 (2018). https://doi.org/10.1007/s13300-018-0432-2
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13300-018-0432-2