Abstract
Introduction
To date there is a lack of economic analysis comparing glucagon-like peptide-1 receptor agonists (GLP-1RAs) to sodium-glucose co-transporter 2 inhibitors (SGLT-2i) for the treatment of type 2 diabetes mellitus (T2DM). Liraglutide and dapagliflozin are the most commonly prescribed GLP-1RA and SGLT-2i in the UK. This analysis investigated the cost-effectiveness of liraglutide 1.2 and 1.8 mg/day compared to dapagliflozin 10 mg/day for the treatment of T2DM in the UK in patients on dual and triple antidiabetic therapy.
Methods
Cost-effectiveness analysis was conducted in the QuintilesIMS CORE Diabetes Model (CDM). The model estimated expected costs and outcomes over a lifetime horizon using the UK national payer perspective. Liraglutide efficacy estimates and patient characteristics were sourced from a trial in patients on prior metformin monotherapy, and from a trial in patients on prior combination therapy. Comparative efficacy data for the other interventions were derived from a network meta-analysis. Utility inputs were extracted from a systematic literature review. Costs are presented in Great British Pound (GBP), 2016 values.
Results
In dual and triple therapy, liraglutide 1.2 mg was less costly and more effective compared with dapagliflozin 10 mg, providing a QALY gain of 0.04 and cost savings of GBP 11 per patient in dual therapy, and a QALY gain of 0.06 and cost savings of GBP 71 per patient in triple therapy. For liraglutide 1.8 mg, increased efficacy and costs compared with dapagliflozin 10 mg were observed in both dual and triple therapy. In dual therapy, a QALY gain of 0.07 and additional costs of GBP 888 per patient yielded an ICER of GBP 13,227, whereas in triple therapy a QALY gain of 0.07 and additional cost of GBP 791 per patient gave an ICER of 11,857.
Conclusion
This long-term modelling analysis found that both dosages of liraglutide may be cost-effective treatment alternatives as part of a dual or a triple antidiabetic therapy in patients for whom an SGLT-2i therapy is considered.
Funding
Novo Nordisk.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Diabetes imposes a substantial societal and financial burden globally. In the UK, the prevalence of diabetes is 6% in people aged 20–79 years [1] and it accounts for 10% of the overall health expenditure [1]. The total economic cost of type 2 diabetes mellitus (T2DM) amounted to GBP 21.8 billion in 2010/11 [2], including both direct and indirect costs.
Glucagon-like peptide-1 receptor agonists (GLP-1RA) are a class of glucose-lowering drugs currently used in the UK for the treatment of T2DM. Guidelines for the treatment of T2DM by the National Institute for Health and Care Excellence (NICE) [3] recommend the use of GLP-1RAs in triple therapy when previous triple therapy with oral antidiabetes drugs (OADs) is not effective, not tolerated, or contraindicated [3].
Currently, there is evidence assessing the cost-effectiveness of the GLP1-RA liraglutide versus other GLP-1RAs [4, 5]. However, there is a lack of health economic analyses comparing liraglutide to SGLT-2is. The aim of this analysis was to assess the cost-effectiveness of liraglutide 1.2 and 1.8 mg/day, the most commonly used GLP-1RA in the UK, with dapagliflozin 10 mg, the most commonly used SGLT-2i in the UK, for the treatment of T2DM as part of a dual and a triple antidiabetic therapy.
This article does not contain any new studies with human or animal subjects performed by any of the authors.
Methods
This study used the CORE Diabetes Model (CDM), a widely published and previously validated simulation model [6–11]. The CDM estimates long-term health and cost outcomes of interventions in diabetes taking into account population characteristics at baseline and accounting for evolution of a range of micro- and macrovascular complications over a set time horizon. Model outputs include economic consequences, incidence of complications, life years and quality-adjusted life years (QALYs) gained, as well as incremental cost-effectiveness ratios (ICERs).
The interventions included in the study were the daily GLP-1RA liraglutide 1.2 mg daily and liraglutide 1.8 mg daily and the SGLT-2i dapagliflozin 10 mg daily. The current analyses assessed the interventions as dual or triple therapies in the management of patients with T2DM in the UK.
Patient baseline characteristics for the dual therapy analysis, including glycemia, cardiovascular risk factors, and the presence of existing diabetic complications, were taken from the NN2211-1860 study [12], Table 1. This was an international, open-label, randomized trial of patients with T2DM who had inadequate glycemic control on metformin and who were randomized to receive 1.2 or 1.8 mg liraglutide once daily, subcutaneously or 100 mg sitagliptin once daily, orally. Patient baseline characteristics for the triple therapy analysis were derived from the Liraglutide Effect and Action in Diabetes 4 (LEAD-4) study, a double-blind, randomized, placebo-controlled, parallel-group, multicenter trial [13] in which patients were randomized to receive 1.2 or 1.8 mg of once-daily liraglutide or liraglutide placebo injected subcutaneously in combination with metformin and rosiglitazone in all three treatment groups. The proportion of smokers and alcohol consumption data were not available from the trials and were obtained from the World Health Organization [14] and Health and Social Care Information Centre (HSCIC) statistics on smoking [15].
As a result of the lack of head-to-head clinical trials comparing the efficacy of liraglutide versus dapagliflozin, estimation of the relative treatment effects between the interventions was derived from a network meta-analysis (NMA) [16]. The NMA included 17 randomized controlled trials (RCTs) (8784 patients), which were broadly consistent with the NN2211-1860 and LEAD-4 trials in terms of key baseline characteristics such as age and BMI (Table A1 in the online supplementary material); baseline HbA1c in the NN2211-1860 and LEAD-4 studies was at the upper end of trials included in the NMA.
NMA results indicated a greater percentage HbA1c reduction with liraglutide 1.2 mg (mean difference −0.64; 95% confidence interval [CI] −0.94, −0.34) and 1.8 mg (mean difference −0.81; 95% CI −1.11, −0.51) versus dapagliflozin 10 mg. Efficacy and safety parameters included in the model but not reported in the NMA were assumed equivalent in all arms.
The relative treatment effects reported in the NMA were then applied to the estimates for liraglutide on HbA1c, systolic blood pressure, weight, and hypoglycemic events (severe and mild) as reported in the NN2211-1860 and LEAD-4 studies in order to obtain estimates for dapagliflozin.
In the base case, all treatment arms assumed that patients remained on active treatment for a period of 3 years, followed by a switch to insulin glargine at a dose of 40 international units (IU) daily [17].
Long-term progressions of HbA1c, blood pressure, and lipids were estimated using UKPDS 68 risk equations [18]. BMI differences between the interventions were applied during the time on treatment only; patients were assumed to rebound to baseline values after treatment is changed to insulin at 3 years.
The model estimated expected costs and outcomes over a lifetime horizon adopting a UK national payer perspective (National Health Service). Only direct costs were considered. Annual therapy costs were calculated using daily doses of the interventions within the scope of the analysis. Unit costs of drugs, injection needles, and the self-monitoring of blood glucose were derived from the British National Formulary (BNF) and the Monthly Index of Medical Specialities (MIMS) [19, 20]. Underlying assumptions of drug management costs, derived from the BNF [19], were 20 mg statins (atorvastatin) daily, 2.5 mg angiotensin-converting enzyme (ACE) inhibitors (ramipril) twice-daily, and additionally 75 mg aspirin daily for patients with cardiovascular disease only. Costs associated with screening tests for eye disease, proteinuria, depression, and foot screening programs were taken from the Personal Social Services Research Unit (PSSRU) [21]. The cost of diabetes-related complications was obtained from published literature, inflated to 2015 values using the PSSRU Pay & Price index [21] wherever necessary. Costs of background OAD therapy were not included as these were expected to be equal in both treatment arms. In the base case, a discount rate of 3.5% was applied to future costs and outcomes, as per NICE guidelines [22]. Unit costs used in this study are presented in Table 2.
Health state utilities were derived from a published systematic literature review of utility values associated with T2DM [23] and are presented in Table 3. The disutility associated with loss of health-related quality of life due to an increase in BMI was applied as per the CODE-2 study by Bagust and Beale [24]. A diminishing approach was used to estimate utility decrements associated with non-severe hypoglycemia, based on results of a study by Lauridsen et al. [25].
The primary analysis considered was the incremental cost per QALY gained with each daily dose of liraglutide compared to dapagliflozin 10 mg/day. A number of sensitivity analyses were conducted to assess the impact of parameters on the base case cost-effectiveness results. One-way sensitivity analyses included variations in the discount rate (between 0% and 6%), time horizon (20, 30, and 40 years), and alternative risk equations (UKPDS82). The impact of the cost of diabetes-related complications was tested by varying these costs on ±10% of the mean value. We also tested the impact of using alternative costs sourced from a recent UK study of immediate and long-term costs of T2DM-related complications [26]. Management costs were varied by ±20% of their mean values. For the efficacy parameters, the effect of abolishing BMI and systolic blood pressure treatment differences was investigated.
Four scenario analyses were tested. The first scenario explored the impact of simulating more severe patients by using the upper limit of 95% confidence interval of the HbA1c value at baseline. A second scenario considered a treatment duration based on disease progression according to UKPDS 68 risk equations; patients remain on active treatment until their level of HbA1c reached 7.5%, at which point they were assumed to switch to insulin glargine. A third scenario analysis tested the impact of using a dose of 1.35 mg/day for liraglutide, reflective of the average daily dose in UK [27], for which costs and effects were linearly interpolated between the 1.2 and 1.8 mg doses. Finally, a fourth scenario explored the impact of comparing liraglutide with SGLT-2is as a class. Data from QuintilesIMS MIDAS was used to derive the current market shares of liraglutide 1.2 and 1.8 mg, dapagliflozin 5 and 10 mg, empagliflozin 10 and 25 mg, and canagliflozin 100 and 300 mg in the UK. A weighted average of the treatment effects of included SGLT-2i treatments from the NMA was applied for this scenario analysis.
Finally, probabilistic sensitivity analysis was conducted for all base case analyses, using 500 simulations with 25,000 patients throughout.
Results
Base Case: Dual Therapy
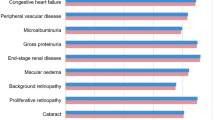
In the base case analysis, liraglutide 1.2 mg generated higher QALYs (0.039 per patient) and lower costs (GBP 11 per patient) compared with dapagliflozin 10 mg. Liraglutide 1.2 mg also showed increases in life expectancy compared to dapagliflozin 10 mg. Whilst higher treatment costs were observed for liraglutide 1.2 mg than for dapagliflozin 10 mg (GBP 1532 per patient), complication costs were on average lower for liraglutide 1.2 mg, overall resulting in lower total costs with liraglutide. Differences in complication cost between liraglutide 1.2 mg and dapagliflozin 10 mg were due to lower incidence of renal, eye, ulcer, amputation, and neuropathy-related complications associated with liraglutide 1.2 mg. Patients treated with liraglutide 1.2 mg on average were free of complications for three additional months compared with patients on dapagliflozin 10 mg. Base case results are reported in Table 4.
In the base case analysis of liraglutide 1.8 mg compared with dapagliflozin 10 mg, liraglutide 1.8 mg produced higher life expectancy and QALYs than dapagliflozin 10 mg. Liraglutide 1.8 mg was also associated with higher total costs relative to dapagliflozin 10 mg (GBP 888 per patient). As with liraglutide 1.2 mg, liraglutide 1.8 mg was associated with higher treatment costs but lower complication costs compared to dapagliflozin 10 mg, with fewer renal, ulcer, amputation, neuropathy, and eye-related complications. Overall, liraglutide 1.8 mg compared to dapagliflozin 10 mg generated an ICER of GBP 13,227 per QALY gained.
Base Case: Triple Therapy
In the base case analysis of liraglutide 1.2 mg versus dapagliflozin 10 mg, liraglutide 1.2 mg yielded a QALY gain of 0.064 and lower costs of GBP −261, resulting in liraglutide 1.2 mg dominating dapagliflozin 10 mg. In the base case analysis of liraglutide 1.8 mg compared with dapagliflozin 10 mg, liraglutide 1.8 mg produced a QALY gain of 0.067 and incremental costs of GBP 791, giving an ICER of GBP 11,857 per QALY gained.
Sensitivity Analyses
In both dual and triple therapy, liraglutide 1.2 mg remained either dominant (more effective and less costly) or cost-effective compared to dapagliflozin 10 mg in the majority of sensitivity analyses. The cost-effectiveness of liraglutide 1.2 mg was most sensitive to a discount rate of 0% applied to costs and outcomes, to a treatment switch at 5 years, and to a lowering of the time horizon to 10 years. Liraglutide 1.8 mg also remained cost-effective across the majority of analyses performed in both dual and triple therapy, mostly generating ICERs below GBP 20,000 per QALY gained. Overall, sensitivity analysis calculating undiscounted costs and outcomes, shortening the time horizon to 10 years, and extending the treatment duration to 5 years had the most significant impact on the ICER. Results of all univariate sensitivity analyses for dual and triple therapy are presented in Table 5 and 6, respectively.
Scenario analysis explored the cost-effectiveness when comparing liraglutide to the weighted average costs and effects of SGLT-2is as an entire class. Assuming a willingness-to-pay (WTP) threshold between GBP 20,000 and GBP 30,000 per QALY gained, both liraglutide doses remained cost-effective versus the entire class of SGLT-2is, with ICERs ranging between GBP 2000 and GBP 21,000.
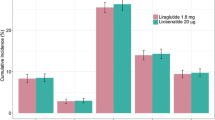
Finally, probabilistic sensitivity analysis (PSA) for the dual therapy analysis yielded respective ICERs for liraglutide 1.2 and 1.8 mg of GBP 2178 and GBP 18,154 per QALY gained. In the triple therapy comparison, PSA generated ICERs of GBP 1850 and GBP 16,156 per QALY gained for liraglutide 1.2 and 1.8 mg, respectively. Cost-effectiveness planes from PSA in dual and triple therapy for liraglutide 1.2 and 1.8 mg are presented in Fig. 1 and suggest that the majority of bootstrap samples were located in the north-eastern quadrant, denoting higher QALYs as well as higher costs for liraglutide 1.2 and 1.8 mg compared to dapagliflozin 10 mg. Cost-effectiveness acceptability curves (CEACs) presented in Fig. 2 suggest a respective probability for liraglutide 1.2 and 1.8 mg of 85% and 49% of being cost-effective in triple therapy at a willingness-to-pay (WTP) threshold of GBP 20,000, whereas the probability of cost-effectiveness of liraglutide 1.2 and 1.8 mg in dual therapy amounted to 70% and 48%, respectively, at the same WTP threshold.
Cost-effectiveness planes, liraglutide 1.2 and 1.8 mg vs. dapagliflozin 10 mg. Upper left Liraglutide 1.2 mg vs dapagliflozin 10 mg in dual therapy; upper right liraglutide 1.8 mg vs dapagliflozin 10 mg in dual therapy; lower left liraglutide 1.2 mg vs dapagliflozin 10 mg in triple therapy; lower right liraglutide 1.8 mg vs dapagliflozin 10 mg in triple therapy
Cost-effectiveness acceptability curves, liraglutide 1.2 and 1.8 mg vs. dapagliflozin 10 mg. Upper left Liraglutide 1.2 mg vs dapagliflozin 10 mg in dual therapy; upper right liraglutide 1.8 mg vs dapagliflozin 10 mg in dual therapy; lower left liraglutide 1.2 mg vs dapagliflozin 10 mg in triple therapy; lower right liraglutide 1.8 mg vs dapagliflozin 10 mg in triple therapy
Discussion
This analysis explored the cost-effectiveness of liraglutide compared to dapagliflozin, the most commonly used GLP-1RA and SGLT-2i treatments in the UK, for the treatment of T2DM in patients on dual and on triple antidiabetic therapy. For T2DM patients on dual and on triple antidiabetic therapy, analysis results suggested modest cost savings and health benefits for liraglutide 1.2 mg when compared to dapagliflozin 10 mg. Liraglutide 1.8 mg was found to be cost-effective vs. dapagliflozin 10 mg with an ICER below cost-effectiveness thresholds set by NICE (GBP 20,000–30,000) in both dual and triple therapy. Overall, observed differences between treatments in terms of costs and outcomes were modest, however, therefore both liraglutide doses and dapagliflozin 10 mg may be considered comparable in terms of cost-effectiveness.
A range of scenario and sensitivity analyses were conducted to test the robustness of model results and generally found these to be robust to plausible variations in input parameters and modelling assumptions. Notable exceptions were sensitivity analyses of liraglutide 1.8 mg reducing the time horizon to 10 years in the dual therapy analysis and extending the duration on treatment to 5 years in the triple therapy analysis.
The study has a number of limitations. Relative treatment effects of liraglutide and dapagliflozin have yet to be established in head-to-head RCTs; therefore, indirect estimates were derived from a network meta-analysis. As the NMA only included studies investigating dual therapy, relative estimates of effectiveness were assumed equivalent in patients on triple therapy. The CDM predicts long-term outcomes of T2DM patients based on the impact of therapies in short-term studies; although the CDM has been validated [8–10] as capable of reliably predicting long-term patient outcomes, direct evidence is lacking. The generalizability of the findings is limited by potential differences between RCT populations and patients who would receive these drugs in usual practice in the UK. Future research is warranted to generate evidence from real-world clinical data to help provide insights into the comparative real-life effectiveness of liraglutide and dapagliflozin and other SGLT-2is in terms of life expectancy or microvascular complications, including scenarios when these treatments are used in addition to insulin glargine.
Many different classes of products are available to treat T2DM. Often, new drugs are evaluated against very similar agents or against placebo. Liraglutide was previously compared with other GLP-1RA products in the UK [4, 5, 28] and was recommended by the Scottish Medicines Consortium on the basis of acceptable cost-effectiveness compared to other GLP-1RAs [29, 30]. Treatment decisions, however, need to weigh the merits and risks of different drug classes for a patient, but UK studies comparing liraglutide against drugs from other classes are infrequent. A 2011 study found that liraglutide at a dose of 1.2 and 1.8 mg was associated with a cost per QALY gained of GBP 9851 and GBP 10,405, respectively, when compared to sitagliptin, and a cost per QALY gained of GBP 9449 and GBP 16,501, respectively, compared to glimepiride [31]. This study is the first of which we are aware that compares the cost-effectiveness of liraglutide to dapagliflozin from a UK perspective.
Whereas guidelines from the American Diabetes Association and the European Association for the Study of Diabetes suggest that GLP1-RA drugs are considered as options at first treatment escalation after failure on metformin [32], NICE guidelines recommend that GLP1-RA drugs are considered as an option after triple therapy with OADs (including SGLT-2is) has failed to achieve glycemic control. Potential reasons for placing GLP1-RA after OADs in the NICE pathway include the injected route of administration, gastrointestinal side effects, and higher cost. This study therefore evaluated the cost-effectiveness of treatment options which are recommended at different positions in the treatment pathway as per UK clinical guidelines.
In common with other studies, this economic evaluation relied on a simulation model to estimate the occurrence of long-term complications based on changes in diabetic risk factors shown in studies of 6–12 months duration. Long-term direct data on the impact of therapy on outcomes would be preferable to modelling. A recent study found that liraglutide reduces the incidence of cardiovascular events [33] in patients at high risk of cardiovascular disease, though results of similar studies with other agents have been mixed. Future evaluations might consider this direct evidence of impact on outcomes as well as making estimates based on risk factors.
Conclusion
This long-term health economic modelling analysis found that liraglutide 1.2 mg was cost-effective when compared to dapagliflozin 10 mg in patients with T2DM as part of a dual and a triple antidiabetic therapy in the UK setting. Additionally, liraglutide 1.8 mg is cost-effective vs. dapagliflozin 10 mg under the cost-effectiveness thresholds set by NICE in both a dual and a triple combination therapy. Both dosages of liraglutide may therefore present a cost-effective treatment alternative in patients for whom an SGLT-2i therapy is considered.
References
International Diabetes Federation. IDF diabetes atlas 2015. http://www.diabetesatlas.org. Accessed 18 Aug 2016.
Hex N, Bartlett C, Wright D, Taylor M, Varley D. Estimating the current and future costs of type 1 and type 2 diabetes in the UK, including direct health costs and indirect societal and productivity costs. Diabet Med. 2012;29(7):855–62.
National Institute of Health and Care Excellence (NICE). Clinical Guideline Update (NG28). Type 2 diabetes in adults: management. https://www.nice.org.uk/guidance/ng28. Accessed 18 Aug 2015.
Scott LJ. Liraglutide: a review of its use in adult patients with type 2 diabetes mellitus. Drugs. 2014;74(18):2161–74.
Ashley D, Vega G, Hunt B, Valentine WJ. Evaluating the cost-effectiveness of GLP-1 receptor agonists for the treatment of type 2 diabetes in the UK. Value Health. 2015;18(7):A606.
Fonseca T, Clegg J, Caputo G, Norrbacka K, Dilla T, Alvarez M. The cost-effectiveness of exenatide once weekly compared with exenatide twice daily and insulin glargine for the treatment of patients with type two diabetes and body mass index ≥30 kg/m2 in Spain. J Med Econ. 2013;16(7):926–38.
Huetson P, Palmer JL, Levorsen Ae, Fournier M, Germe M, McLeod E. Cost-effectiveness of once daily GLP-1 receptor agonist lixisenatide compared to bolus insulin both in combination with basal insulin for the treatment of patients with type 2 diabetes in Norway. J Med Econ. 2015;18(8):573–85.
McEwan P, Foos V, Palmer JL, Lamotte M, Lloyd A, Grant D. Validation of the IMS CORE Diabetes Model. Value Health. 2014;17(6):714–24.
Palmer AJ, Roze S, Valentine WJ, et al. The CORE Diabetes Model: projecting long-term clinical outcomes, costs and costeffectiveness of interventions in diabetes mellitus (types 1 and 2) to support clinical and reimbursement decision-making. Curr Med Res Opin. 2004;20(Suppl. 1):S5–26.
Palmer AJ, Roze S, Valentine WJ, et al. Validation of the CORE Diabetes Model against epidemiological and clinical studies. Curr Med Res Opin. 2004;20(sup1):S27–40.
Tzanetakos C, Melidonis A, Verras C, Kourlaba G, Maniadakis N. Cost-effectiveness analysis of liraglutide versus sitagliptin or exenatide in patients with inadequately controlled type 2 diabetes on oral antidiabetic drugs in Greece. BMC Health Serv Res. 2014;14(1):1.
Pratley RE, Nauck M, Bailey T, et al. Liraglutide versus sitagliptin for patients with type 2 diabetes who did not have adequate glycaemic control with metformin: a 26-week, randomised, parallel-group, open-label trial. Lancet. 2010;375(9724):1447–56.
Zinman B, Gerich J, Buse JB, et al. Efficacy and safety of the human glucagon-like peptide-1 analog liraglutide in combination with metformin and thiazolidinedione in patients with type 2 diabetes (LEAD-4 Met + TZD). Diabetes Care. 2009;32(7):1224–30.
World Health Organisation. WHO Global Alcohol Report 2014: Country Profiles. http://www.who.int/entity/substance_abuse/publications/global_alcohol_report/msb_gsr_2014_2.pdf?ua=1. Accessed 1 Dec 2016.
Health & Social Care Information Centre (HSCIC). Statistics on smoking: England 2014. http://content.digital.nhs.uk/catalogue/PUB14988/smok-eng-2014-rep.pdf. Accessed 1 Dec 2016.
Lorenzi M, Ploug UJ, Langer J, Skovgaard R, Jansen J. Liraglutide versus SGLT2 inhibitors in people with type 2 diabetes: a network meta-analysis. Poster 0226-P presented at the World Diabetes Conference, 30 November–4 December 2015, Vancouver, Canada.
World Health Organisation. WHOCC - ATC/DDD Index. World Health Organisation. Available from: http://www.whocc.no/atc_ddd_index/?showdescription=yes&code=A10AE04. Accessed 16 Dec 2015.
Clarke PM, Gray AM, Briggs A, et al. A model to estimate the lifetime health outcomes of patients with type 2 diabetes: the United Kingdom Prospective Diabetes Study (UKPDS) Outcomes Model (UKPDS no. 68). Diabetologia. 2004;47(10):1747–59.
Joint Formulary Committee. British national formulary 71. London: BMJ Group and Pharmaceutical Press; 2016.
MIMS Monthly Index of Medical Specialities (MIMS). http://www.mims.co.uk/. Accessed Jun 2016.
Personal Social Services Research Unit. Unit costs of health and social care 2015. Personal Social Services Research Unit 2014. http://www.pssru.ac.uk/project-pages/unit-costs/2015/. Accessed Jun 2016.
National Institute for Health and Care Excellence. Guide to the methods of technology appraisal 2013. National Institute for Health and Care Excellence 2015. https://www.nice.org.uk/article/pmg9/chapter/foreword. Accessed 1 Dec 2016.
Beaudet A, Clegg J, Thuresson PO, Lloyd A, McEwan P. Review of utility values for economic modeling in type 2 diabetes. Value Health. 2014;17(4):462–70.
Bagust A, Beale S. Modelling EuroQol health-related utility values for diabetic complications from CODE-2 data. Health Econ. 2005;14(3):217–30.
Lauridsen JT, Lonborg J, Gundgaard J, Jensen HH. Diminishing marginal disutility of hypoglycaemic events: results from a time trade-off survey in five countries. Qual Life Res. 2014;23(9):2645–50.
Alva ML, Gray A, Mihaylova B, Leal J, Holman RR. The impact of diabetes-related complications on healthcare costs: new results from the UKPDS (UKPDS 84). Diabet Med. 2015;32(4):459–66.
Divino V, DeKoven M, Hallinan S, et al. Glucagon-like peptide-1 receptor agonist treatment patterns among type 2 diabetes patients in six European countries. Diabetes Ther. 2014;5(2):499–520.
Charokopou M, Chuang L, Verheggen B, Gibson D, Grandy S, Kartman B. Cost-effectiveness analysis of exenatide once-weekly versus dulaglutide, liraglutide and lixisenatide for the treatment of type 2 Diabetes Mellitus: an analysis from the UK NHS Perspective. Value Health. 2015;18(7):A606.
Scottish Medicines Consortium. Scottish Medicines Consortium liraglutide (Victoza). Scottish Medicines Consortium 2015 May 11. https://www.scottishmedicines.org.uk/SMC_Advice/Advice/1044_15_liraglutide_Victoza/liraglutide_Victoza. Accessed 9 Nov 2016.
Scottish Medicines Consortium. Scottish Medicines Consortium liraglutide (Victoza). Scottish Medicines Consortium 2009 December 7. http://www.scottishmedicines.org.uk/SMC_Advice/Advice/585_09_liraglutide___Victoza_/liraglutide__Victoza_. Accessed 9 Nov 2016.
Davies MJ, Chubb BD, Smith IC, Valentine WJ. Cost–utility analysis of liraglutide compared with sulphonylurea or sitagliptin, all as add-on to metformin monotherapy in type 2 diabetes mellitus. Diabet Med. 2012;29(3):313–20.
Inzucchi SE, Bergenstal RM, Buse JB, et al. Management of hyperglycemia in type 2 diabetes, 2015: a patient-centered approach: update to a position statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care. 2015;38(1):140–9.
Marso SP, Daniels GH, Brown-Frandsen K, et al. Liraglutide and cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2016;375(4):311–22.
Novo Nordisk. Clinical Trial Report. Liraglutide Effect and Action in Diabetes (LEAD 4): effect on glycemic control of liraglutide in combination with rosiglitazone plus metformin versus rosiglitazone plus metformin in type 2 diabetes (a twenty-six week double-blind parallel trial to investigate safety and efficacy). Trial Phase: 3a. 1-2-2008. Data on file.
Department of Health. NHS Reference Costs 2014 to 2015. https://www.gov.uk/government/publications/nhs-reference-costs-2014-to-2015. Accessed 1 Dec 2016.
National Institute of Health and Care Excellence. NICE guideline CG48: MI–secondary prevention; Secondary prevention in primary and secondary care for patients following a myocardial infarcation. National Institute of Health and Care Excellence 2007. Available from: http://www.nice.org.uk/guidance/cg48. Accessed 1 Dec 2016.
Cameron CG, Bennett HA. Cost-effectiveness of insulin analogues for diabetes mellitus. Can Med Assoc J. 2009;180(4):400–7.
Dyer MT, Goldsmith KA, Khan SN, et al. Clinical and cost-effectiveness analysis of an open label, single-centre, randomised trial of spinal cord stimulation (SCS) versus percutaneous myocardial laser revascularisation (PMR) in patients with refractory angina pectoris: the SPiRiT trial. Trials. 2008;9:40.
Youman P, Wilson K, Harraf F, Kalra L. The economic burden of stroke in the United Kingdom. Pharmacoeconomics. 2003;21(1):43–50.
National Institute of Health and Care Excellence. Chronic kidney disease: early identification and management of chronic kidney disease in adults in primary and secondary care (CG73). National Institute of Health and Care Excellence 2008. http://www.nice.org.uk/guidance/cg73. Accessed 1 Dec 2016.
National Institute for Health and Care Excellence. Type 2 diabetes: the management of type 2 diabetes (CG 87). National Institute for Health and Care Excellence 2014. http://www.nice.org.uk/guidance/cg87. Accessed 1 Dec 2016.
Chubb B, Jensen MM, Frier BM. Self-reported frequency and impact of non-severe hypoglycaemia in insulin-treated adults in the UK. Value Health. 2014;17(7):A354–5.
Clarke P, Gray A, Legood R, Briggs A, Holman R. The impact of diabetes-related complications on healthcare costs: results from the United Kingdom prospective diabetes study (UKPDS Study No. 65). Diabet Med. 2003;20(6):442–50.
Meads C, Hyde C. What is the cost of blindness? Br J Ophthalmol. 2003;87(10):1201–4.
Ghatnekar O, Willis M, Persson U. Cost-effectiveness of treating deep diabetic foot ulcers with Promogran in four European countries. J Wound Care. 2002;11(2):70–4.
Clarke P, Gray A, Holman R. Estimating utility values for health states of type 2 diabetic patients using the EQ-5D (UKPDS 62). Med Decis Mak. 2002;22(4):340–9.
Wasserfallen JB, Halabi G, Saudan P, et al. Quality of life on chronic dialysis: comparison between haemodialysis and peritoneal dialysis. Nephrol Dial Transpl. 2004;19(6):1594–9.
Kiberd BA, Jindal KK. Screening to prevent renal failure in insulin dependent diabetic patients: an economic evaluation. BMJ. 1995;311(7020):1595–9.
Fenwick EK, Xie J, Ratcliffe J, et al. The impact of diabetic retinopathy and diabetic macular edema on health-related quality of life in type 1 and type 2 diabetes. Investig Ophthalmol Vis Sci. 2012;53(2):677–84.
Lee AJ, Morgan CL, Morrissey M, Wittrup-Jensen K, Kennedy-Martin T, Currie CJ. Evaluation of the association between the EQ-5D index (health-related utility) and body mass index (obesity) in hospital-treated people with type 1 diabetes, type 2 diabetes and with no diagnosed diabetes. Diabet Med. 2005;22(11):1482–6.
Evans M, Khunti K, Mamdani M, et al. Health-related quality of life associated with daytime and nocturnal hypoglycaemic events: a time trade-off survey in five countries. Health Qual Life Outcomes. 2013;11(1):90.
Nauck M, Frid A, Hermansen K, et al. Efficacy and safety comparison of liraglutide, glimepiride, and placebo, all in combination with metformin, in type 2 diabetes: the LEAD (liraglutide effect and action in diabetes)-2 study. Diabetes Care. 2009;32(1):84–90.
Bailey CJ, Gross JL, Pieters A, Bastien A, List JF. Effect of dapagliflozin in patients with type 2 diabetes who have inadequate glycaemic control with metformin: a randomised, double-blind, placebo-controlled trial. Lancet. 2010;375(9733):2223–33.
Bolinder J, Ljunggren O, Kullberg J, et al. Effects of dapagliflozin on body weight, total fat mass, and regional adipose tissue distribution in patients with type 2 diabetes mellitus with inadequate glycemic control on metformin. J Clin Endocrinol Metab. 2012;97(3):1020–31.
Lambers Heerspink HJ, de ZD, Wie L, Leslie B, List J. Dapagliflozin a glucose-regulating drug with diuretic properties in subjects with type 2 diabetes. Diabetes Obes Metab. 2013;15(9):853–62.
Acknowledgements
Sponsorship for this study and article processing charges were funded by Novo Nordisk.
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval to the version to be published.
Disclosures
Gabriela Vega-Hernandez is a full-time employee of Novo Nordisk Ltd. Radek Wojcik is a full-time employee of QuintilesIMS and served as paid consultant to Novo Nordisk for this study. Max Schlueter is a full-time employee of QuintilesIMS and served as paid consultant to Novo Nordisk for this study.
Compliance with Ethics Guidelines
This article does not contain any new studies with human or animal subjects performed by any of the authors.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced content
To view enhanced content for this article go to http://www.medengine.com/Redeem/17F7F060606BDCD7.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Vega-Hernandez, G., Wojcik, R. & Schlueter, M. Cost-Effectiveness of Liraglutide Versus Dapagliflozin for the Treatment of Patients with Type 2 Diabetes Mellitus in the UK. Diabetes Ther 8, 513–530 (2017). https://doi.org/10.1007/s13300-017-0250-y
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13300-017-0250-y