Abstract
Introduction
Guidelines recommend insulin progression for patients with type 2 diabetes (T2D) with inadequate glycemic control. The Multinational Observational Study Assessing Insulin use (MOSAIc [ClinicalTrials.gov identifier, NCT01400971]) study is a 2-year observational study, investigating factors that influence insulin progression in T2D patients. In this first of two reports, we describe baseline clinical and psychosocial characteristics of Chinese, Japanese, and South Korean patients who participated in MOSAIc. Insulin treatment, factors affecting progression, and outcomes will be reported separately.
Methods
Patients with T2D using insulin for ≥3 months were eligible. Baseline demographic, clinical, and psychosocial data were collected from patients. Quality of life instruments, including the Diabetes Distress Scale (DDS), were used to assess patient’s concerns about disease management, support, and emotional burden. The association between the DDS and the selected covariates was also assessed.
Results
A total of 373 patients in China, 157 in Japan, and 141 in South Korea were enrolled from July 2011 to July 2013. Mean ± standard deviation duration (years) of T2D differed across countries (China 11.4 ± 7.5; Japan 13.8 ± 8.7; South Korea 15.7 ± 8.8; P < 0.0001). Japanese patients used more noninsulin anti-hyperglycemic agents than did Chinese or South Korean patients (P < 0.0001). Exclusive use of basal insulin was most common in Japan and South Korea compared with China, whereas approximately 66.8% of Chinese patients used mixed insulin. Covariates associated with the DDS were younger age [P = 0.044 (Japan)], higher incidence of monthly hypoglycemia [P = 0.036 [China]; P = 0.021 (South Korea)], and male gender [P = 0.037 (South Korea)].
Conclusions
There were significant differences amongst East Asian patients with T2D treated with insulin, including in quality of life scores. Results from the MOSAIc longitudinal analyses will further investigate trends of insulin intensification and barriers to insulin progression.
Funding
Eli Lilly and Company.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Type 2 diabetes (T2D) is a chronic progressive disease and is a major public health problem worldwide. Sustained hyperglycemia, measured by glycosylated hemoglobin A1c level (HbA1c), can result in preventable complications that affect health and quality of life and are costly for health care systems [1, 2]. The prevalence of T2D in Asia is substantial and is increasing over time, with recent estimates suggesting that the prevalence of diabetes is 9.3% in China, 7.6% in Japan, and 7.3% in South Korea [3].
Based on clinical trial results, insulin is the most effective glucose-lowering therapy and can improve quality of life by preventing hyperglycemia and reducing diabetic complications [4, 5]. International guidelines recommend that insulin treatment may be modified over time to achieve HbA1c targets [6], which are <7% (<53 mmol/mol) in Japan [7] and China [8] and <6.5% (<48 mmol/mol) in South Korea [9]; however, although most patients with T2D have HbA1c levels above these targets, many do not progress their insulin treatment (i.e., switch from basal to a mixed insulin regimen, add bolus doses, and/or increase dosing frequency) [10–12]. Overall, preliminary evidence suggests that various clinical and psychosocial factors prevent insulin progression at the patient, provider, and health care system levels [13]. As for patients, barriers may include fear, pain, concern over weight gain and/or disease progression, and inconvenience associated with injections [14, 15]. For the physician and health care system, barriers may include concerns over hypoglycemia, lack of experience, lack of qualified personnel, and lack of reimbursement for medicines or services [11, 14, 16]. Although the health burden of T2D is increasing in East Asia, only a few studies have actually examined patterns and trends of insulin progression or barriers associated with insulin treatment and its intensification in this population [17, 18].
The Multinational Observational Study Assessing Insulin use: understanding the challenges associated with progression of therapy (MOSAIc [ClinicalTrials.gov identifier, NCT01400971]) study is a 2-year, global, non-interventional, prospective, and observational cohort study designed to identify factors that influence insulin progression among patients with T2D [19]. Within this study, data from MOSAIc patients from three countries, China, Japan, and South Korea, have been investigated at baseline and longitudinally over 2 years to identify patterns and trends of insulin treatment and progression as well as its associated barriers with insulin progression. Thus, this first of two articles presents the baseline demographic, clinical, treatment, and psychosocial characteristics of Japanese, Chinese, and South Korean MOSAIc patients, while cross-sectional data of treatment progression and attitudes toward therapy will be analyzed separately.
Methods
Study Design
The rationale and design of the MOSAIc study have been reported elsewhere [13]. MOSAIc is a multinational, non-interventional, prospective, and observational cohort study. Patients were recruited from July 2011 to July 2013 in 18 countries. Within the East Asian analysis, study sites comprised specialist and general practice centers in urban and rural areas in Japan, China, and South Korea. Patients were observed for 2 years after study enrollment with visits approximately 6, 12, 18, and 24 months after the baseline visit, with all visits being part of the patient’s normal care.
The MOSAIc protocol was approved by local review boards and all patients provided written informed consent before participation in the study. The study was conducted in accordance with the Declaration of Helsinki guidelines on good clinical practices as well as applicable laws and regulations of the countries in which the study was conducted. This article is based on previously conducted studies and does not involve any new studies of human or animal subjects performed by any of the authors.
Study Population
Eligible study patients at screening were previously diagnosed with T2D, at least 18 years of age, presenting with T2D to a study site as part of normal medical care, and receiving any commercially available initial insulin therapy for at least 3 months, with or without any combination of approved noninsulin anti-hyperglycemic agents (AHAs) (e.g., metformin). Patients were considered ineligible if they were receiving intensive basal-bolus therapy or had initiated insulin at a dose of three injections of mixed insulin.
Baseline Data Collection and Patient-Reported Outcomes
Patient data regarding demographic and clinical characteristics, comorbid conditions, and treatment regimens were retrospectively collected from medical records at the study site for a period of up to 6 months before the baseline visit.
Patient reported outcomes (PROs) to assess emotional distress and disease knowledge were derived from previously validated diabetes instruments, and the translated questionnaires into Asian languages went through linguistic validation. The Diabetes Distress Scale (DDS) is a 25-item survey that examines the patient relationship with the health care provider and the physician perception of the patient [20]. The DDS was used to assess patient anxiety regarding the management of diabetes on a six-point Likert scale; scores ranged from 17 (no distress) to 102 (severe distress). The Brief Diabetes Knowledge Test, a nine-item test modified from the Diabetes Knowledge Test, was used to examine the patient’s diabetes knowledge [21]. In addition, the study team developed survey tools for MOSAIc [13], including the Hypoglycemia and Fasting Survey and the Insulin Specific Adherence Questionnaire. The Hypoglycemia and Fasting Survey examined the experience of and reactions to hypoglycemia, and included a question about the frequency with which the patient has experienced hypoglycemia-related events (between “Never” and “Always [every day]”). The Insulin Specific Adherence Questionnaire evaluated adherence to insulin therapy and assessed patients’ willingness to increase the frequency of injections.
Statistical Analysis
Baseline patient characteristics were analyzed by country by calculating the number and percentage of patients for categorical variables and the mean and standard deviation (SD) for continuous variables. Chained equation methods were used to impute missing items among independent variables [22]. Statistical significance was evaluated by calculating P values using ANOVA for demographic measures, pooled ANOVA for clinical measures and PROs, Cochran-Mantel–Haenszel test for comorbidities, and Chi-squared test for treatment profiles. Linear regression models were used to assess the association between DDS and selected covariates (age, sex, duration of diabetes, HbA1c, body mass index [BMI], number of noninsulin AHAs, injection frequency, Brief Diabetes Knowledge Test score, and rate of hypoglycemia per month). All analyses were performed using SAS 9.3 (SAS Institute; Cary, NC, USA) and Stata 13 (StataCorp LP; College Station, TX, USA).
Results
A total of 373 patients in China, 157 in Japan, and 141 in South Korea were evaluated. Baseline demographic and clinical characteristics varied among patients in the three countries (Table 1). A significantly higher proportion of female patients was observed in China (56.0%) compared with the proportions in Japan (38.9%) and South Korea (36.2%) (P < 0.0001). The mean (±SD) age differed significantly between countries, with the highest age in Japan (64.3 ± 12.7 years) and the lowest in China (60.8 ± 10.2 years).
Similarly, the mean (±SD) duration of diabetes also differed, being longer in South Korea (15.7 ± 8.8 years) than in China (11.4 ± 7.5 years) and in Japan (13.8 ± 8.7 years) (P < 0.0001).
The baseline prevalence of some comorbidities also differed between countries. Diabetes-related comorbidities, whose prevalence differed significantly, included congestive heart failure, nephropathy, neuropathy, and retinopathy (Table 1). In particular, microvascular diseases (i.e., nephropathy, neuropathy, and retinopathy) were significantly more observed (≥35.5%) in South Korea than in China and Japan (P ≤ 0.0003).
Patient use of noninsulin AHAs, which include oral antidiabetic agents and glucagon-like peptide-1 (GLP-1) receptor agonists, differed significantly among the countries. Japanese patients used more AHAs (mean = 1.8 medicines) compared with Chinese (0.6 medicines) and South Korean (0.8 medicines) patients (Table 1). Sulfonylurea and dipeptidyl peptidase-4 (DPP-4) inhibitor treatments were highest amongst Japanese patients, whereas metformin was the most commonly used AHA in China and South Korea. There was no reported GLP-1 receptor agonist use among patients at baseline. Insulin regimens also differed significantly among the countries, with Chinese patients injecting insulin more frequently than Japanese and South Korean patients (Table 1). The most common insulin regimen in Japan and South Korea was once-daily basal insulin, whereas the most common regimen in China was twice-daily mixed insulin (Table 2).
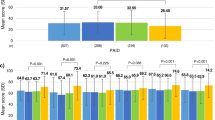
In terms of PROs, the DDS (mean ± SD) scores differed significantly across countries, with South Korean patients reporting greater DDS scores (43.3 ± 16.6) than those from China (28.1 ± 10.6) and Japan (31.5 ± 13.5) (Table 3). Results from the Brief Diabetes Knowledge Test demonstrated that Chinese patients recorded the highest number of questions correctly with a mean (±SD) score of 6.82 ± 1.75 questions answered correctly (Table 3). Using the Hypoglycemia and Fasting Survey, it was found that a significantly higher proportion of South Korean patients (46.8%) experienced at least 1 hypoglycemic episode per month, compared with Chinese (29.5%) and Japanese (20.4%) patients. Responses from the Insulin Specific Adherence Questionnaire demonstrated that a greater proportion of South Korean and Japanese patients (64.5% and 59.9%, respectively) was willing to increase their insulin injection frequency to control their diabetes compared with Chinese patients (29.5%), whose regimens already consisted of more frequent injections.
There were no notable differences among East Asian patients regarding the association between DDS and duration of diabetes, HbA1c, BMI, number of AHAs, or injection frequency (Table 4). However, Chinese and South Korean patients who experienced hypoglycemia more than once per month recorded higher DDS scores compared with those who experienced hypoglycemia less frequently [P = 0.036 (China); P = 0.021 (South Korea)]. Higher DDS scores were also recorded by younger Japanese patients (P = 0.044) compared with older patients and by male South Korean patients compared with female patients (P = 0.037). The Brief Diabetes Knowledge Test score was inversely associated with DDS in all three countries, but this was not statistically significant.
Discussion
This first of a two-part series reports the baseline characteristics of East Asian patients, who participated in the MOSAIc study over a 2-year period. To our knowledge, this is the first study to compare insulin treatment profiles and the impact of T2D and its treatment on patients over time across multiple countries in East Asia. The cross-sectional data presented here indicate that there are significant differences in term of demographic, clinical, treatment, and psychosocial characteristics among the MOSAIc patients who enrolled in China, Japan, and South Korea. Notably, there were significant differences in the treatment regimens selected by study physicians, in the PRO measures recorded by patients, and differences in the factors associated with diabetes-related distress. Our results suggest that both diabetes clinical practice and the patient experience of T2D differ markedly between countries in East Asia, and we expect the 2-year MOSAIc data will provide additional information.
Baseline demographic and clinical characteristics varied among the three countries. This variability may be due to differences in the timing of insulin initiation in the patient’s diabetes treatment regimen or differences in treatment patterns after insulin initiation, although our country-specific results were generally similar to those in other studies [23–26].
In terms of gender, the proportion of female patients in China (56.0%) was higher than one in Japan (38.9%) and South Korea (36.2%) in our study; the gender distributions in each country were consistent with the other country-specific large observational research on insulin usage, though epidemiologically there was more male population in the whole T2D patients in each country [27–29]. Furthermore, the higher incidence of diabetes-related complications in patients in South Korea compared with those in China and Japan may be related to more severe disease, as suggested by the longer mean duration of diabetes, we observed in South Korean patients. In addition, the different levels of access to tertiary-level hospitals in the three countries may have affected the rate of detection and accounted for some of the differences in reported proportions of some diabetes-related complications.
The insulin regimens used by MOSAIc patients also differed among the three countries; markedly fewer Chinese patients were initiated on basal insulin compared with Japanese and South Korean patients. Local guidelines in China and Japan do not recommend specific insulins for initiation, and the choice of insulin relies largely on the health care provider’s discretion [26, 30]. In South Korea, there are no treatment guidelines; however, recommendations suggest that a patient commences on basal insulin if HbA1c <8.5% (<69 mmol/mol) and mixed insulin if HbA1c ≥8.5% (≥69 mmol/mol) [31]. Possible explanations for the infrequent use of basal insulin in China include the higher cost of this therapy compared with short-acting and mixed insulin, which may be prohibitive to patients [32]; differing levels of reimbursement for insulin products, for example, short-acting insulin, premixed insulin, and Neutral Protamine Hagedorn insulin are on the Chinese National Essential Medicines list and are usually fully reimbursed by the insurance system [33]; and the tendency for Chinese physicians to choose mixed insulin to manage both fasting and high postprandial plasma glucose resulting from the high-carbohydrate diets of Chinese patients [34]. The 2-year MOSAIc follow-up data will provide further information as to how these differences in insulin therapy in China will affect treatment progression.
A notable result of our study is the marked difference in treatment choices made by physicians from three countries, with patients in Japan being prescribed significantly more AHAs compared with patients in China or South Korea. These results reflect the differences in reimbursement and medicine access in East Asia. Utilization of DPP-4 inhibitors also varies dramatically across the region, with nearly half of Japanese patients in our study receiving medicines from this class at baseline, compared with less than 1% of patients in China and South Korea. This trend is explained by the earlier availability and reimbursement of DPP-4 inhibitors in Japan compared to China and South Korea. Similarly, no patient in this study recorded use of a GLP-1 receptor agonist at baseline; an observation that is reflective of the fact that GLP-1 receptor agonists only recently became available in the region. As the DPP-4 inhibitor class is now reimbursed in South Korea, and the GLP-1 receptor agonist class is reimbursed in both Japan and South Korea and available in China, the use of these medicines is expected to increase in these countries, demonstrating the pivotal role access and reimbursement has in enabling patient treatment across the region [35].
Differences in baseline quality of life and diabetes distress scores between patients from various countries may be explained in part by ethnic cultural differences. For example, it may explain why Japanese patients were less likely to report higher diabetes distress rates as a result of hypoglycemia compared with Chinese or South Korean patients. However, differences in treatment regimens and other factors, such as variations in the understanding of definitions of hypoglycemia, may also contribute to this finding. In contrast to other findings published in the literature [36, 37], our baseline data results did not reflect that patients with a higher knowledge of diabetes reported a lower DDS. The longitudinal changes in quality of life and DDS as well as any impact on insulin progression and health outcomes will be reported in the second article of this series, which will describe the findings of the 2-year East Asian MOSAIc follow-up analyses.
The extensive MOSAIc observational, real-world, self-reported data will assist in identifying patient, provider, and health care environmental factors that influence insulin regimens among T2D patients in East Asia. The data reported that in this first of a two-part series provides a baseline and introduction for the 2-year study results. In addition, although other studies have examined real-world use of insulin therapy in East Asia, the MOSAIc study provides clinical and psychosocial analyses over a longer duration of follow-up, and is specifically aimed at addressing the current lack of evidence regarding insulin progression and the barriers to achieving optimal care in East Asia. However, the study does have some limitations. Study participants were volunteered to answer the questionnaires, because patients were not collected in random sampling; therefore, socio-demographic and psychological characteristics may not represent the whole population. Patient records were only available from physicians participating in the study, which may limit the collection of the data if the study patients were treated by additional health care providers. In addition, the observational study design prevented the inclusion of data beyond routine diabetes care or the control of country-specific variables that may have limited the ability to directly compare the countries.
Conclusion
The MOSAIc baseline results suggest significant differences in baseline demographic, clinical, treatment, and psychosocial characteristics among Chinese, Japanese, and South Korean patients with T2D receiving insulin therapy. Physician treatment decisions differed among countries due to cultural, health care system, reimbursement, and access factors. The second part of this article series will present 2-year results from this study population and provide further insights on insulin treatment and progression and its impact on glycemic control for this East Asian population.
References
Inzucchi SE, Bergenstal RM, Buse JB, Diamant M, Ferrannini E, Nauck M, et al. Management of hyperglycemia in type 2 diabetes: a patient-centered approach: position statement of the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care. 2012;35:1364–79.
Wang W, McGreevey WP, Fu C, Zhan S, Luan R, Chen W, et al. Type 2 diabetes mellitus in China: a preventable economic burden. Am J Manag Care. 2009;15:593–601.
International Diabetes Federation. IDF Diabetes Atlas: Sixth Edition. International Diabetes Federation Brussels, Belgium. Available at http://www.idf.org/diabetesatlas. Accessed May 20, 2015.
Holman RR, Farmer AJ, Davies MJ, Levy JC, Darbyshire JL, Keenan JF, et al. Three-year efficacy of complex insulin regimens in type 2 diabetes. N Engl J Med. 2009;361:1736–47.
Shim YT, Lee J, Toh MP, Tang WE, Ko Y. Health-related quality of life and glycaemic control in patients with Type 2 diabetes mellitus in Singapore. Diabet Med. 2012;29:e241–8.
Nathan DM, Buse JB, Davidson MB, Ferrannini E, Holman RR, Sherwin R, et al. Medical management of hyperglycemia in type 2 diabetes: a consensus algorithm for the initiation and adjustment of therapy: a consensus statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care. 2009;32:193–203.
Japan Diabetes Society. Treatment Guide for Diabetes 2012–2013. http://www.jds.or.jp/modules/en/index.php?content_id=1. Accessed Apr 1, 2015.
Chinese Diabetes Society. China guideline for type 2. Diabetes. 2013;2014(6):447–98.
Korean Diabetes Association. Korean Diabetes Research Foundation, and International Conference on Diabetes and Metabolism 2013. Diabetes Fact Sheet in Korea 2013. http://www.diabetes.or.kr/english/. Accessed Apr 10, 2015.
Blak BT, Smith HT, Hards M, Curtis BH, Ivanyi T. Optimization of insulin therapy in patients with type 2 diabetes mellitus: beyond basal insulin. Diabet Med. 2012;29:e13–20.
Cuddihy RM, Philis-Tsimikas A, Nazeri A. Type 2 diabetes care and insulin intensification: is a more multidisciplinary approach needed? Results from the MODIFY survey. Diabetes Educ. 2011;37:111–23.
Patrick AR, Fischer MA, Choudhry NK, Shrank WH, Seeger JD, Liu J, et al. Trends in insulin initiation and treatment intensification among patients with type 2 diabetes. J Gen Intern Med. 2014;29:320–7.
Polinski JM, Curtis BH, Seeger JD, Choudhry NK, Zagar A, Shrank WH. Rationale and design of the multinational observational study assessing insulin use: the MOSAIc study. BMC Endocr Disord. 2012;12:20.
Tan AM, Muthusamy L, Ng CC, Phoon KY, Ow JH, Tan NC. Initiation of insulin for type 2 diabetes mellitus patients: what are the issues? A qualitative study. Singap Med J. 2011;52:801–9.
Wong S, Lee J, Ko Y, Chong MF, Lam CK, Tang WE. Perceptions of insulin therapy amongst Asian patients with diabetes in Singapore. Diabet Med. 2011;28:206–11.
Polinski JM, Smith BF, Curtis BH, Seeger JD, Choudhry NK, Connolly JG, et al. Barriers to insulin progression among patients with type 2 diabetes: a systematic review. Diabetes Educ. 2013;39:53–65.
Ishii H, Terauchi Y, Jinnouchi H, Taketsuna M, Takeuchi M, Imaoka T. Effects of insulin changes on quality of life and glycemic control in Japanese patients with type 2 diabetes mellitus: the insulin-changing study intending to gain patients’ insights into insulin treatment with patient-reported health outcomes in actual clinical treatments (INSIGHTs) study. J Diabetes Investig. 2013;4:560–70.
Polinski JM, Connolly JG, Curtis BH, Seeger JD, Gaskins K, Perez M, et al. Patterns and trends in insulin intensification among patients with type 2 diabetes: a systematic review. Prim Care Diabetes. 2014;8:101–9.
Polinski JM, Kim SC, Jiang D, Hassoun A, Shrank WH, Cos X, et al. Geographic patterns in patient demographics and insulin use in 18 countries, a global perspective from the multinational observational study assessing insulin use: understanding the challenges associated with progression of therapy (MOSAIc). BMC Endocr Disord. 2015;15:46.
Polonsky WH, Fisher L, Earles J, Dudl RJ, Lees J, Mullan J, et al. Assessing psychosocial distress in diabetes: development of the diabetes distress scale. Diabetes Care. 2005;28:626–31.
Fitzgerald JT, Funnell MM, Hess GE, Barr PA, Anderson RM, Hiss RG, et al. The reliability and validity of a brief diabetes knowledge test. Diabetes Care. 1998;21:706–10.
van Buuren S, Boshuizen HC, Knook DL. Multiple imputation of missing blood pressure covariates in survival analysis. Stat Med. 1999;18:681–94.
Ji L, Su Q, et al. Glycemic control and self-monitoring of blood glucose in Chinese patients with type 2 diabetes on insulin: baseline results from the COMPASS study. Diabetes Res Clin Pract. 2016;112:82–7.
Ji L, Zhang P, et al. Observational Registry of Basal Insulin Treatment (ORBIT) in patients with type 2 diabetes uncontrolled by oral hypoglycemic agents in china-study design and baseline characteristics. Diabetes Technol Ther. 2015;17(10):735–44.
Kanatsuka A, Kawai K, Hirao K, Yokoyama H, Kobayashi M. The initiation of insulin therapy in type 2 diabetic patients treated with oral anti-diabetic drugs: an observational study in multiple institutes across Japan (JDDM27). Diabetol Int. 2012;3:164–73.
Kim SS, Kim IJ, Kim YK, Yoon KH, Son HY, Park SW, et al. Duration of diabetes and effectiveness of insulin in the management of insulin-naive Korean patients uncontrolled on oral antidiabetic drugs: a sub-analysis of the MOdaliTy of Insulin treatment eValuation (MOTIV) registry results. Acta Diabetol. 2014;51:655–61.
Yang W, Lu J, et al. Prevalence of diabetes among men and women in China. N Engl J Med. 2010;362(12):1090–101.
Charvat H, Goto A, et al. Impact of population aging on trends in diabetes prevalence: a meta-regression analysis of 160,000 Japanese adults. J Diabetes Investig. 2015;6(5):533–42.
Korean Diabetes Association. Korean Diabetes Fact Sheet 2015 Edition. http://www.diabetes.or.kr/temp/KDA_fact_sheet%202015.pdf. Accessed Apr 28, 2016.
Tsai ST, Pathan F, Ji L, Yeung VT, Chadha M, Suastika K, et al. First insulinization with basal insulin in patients with Type 2 diabetes in a real-world setting in Asia. J Diabetes. 2011;3:208–16.
Korean Diabetes Association. Korean Diabetes Association Guidelines 2013.
National Development and Reform Commission of the People’s Republic of China. Notification Number [2012]4134: Maximum Retail Pricing of Drugs. http://www.ndrc.gov.cn/zwfwzx/zfdj/jggg/yaopin/201301/W020130121540619076885.pdf. Accessed Apr 13, 2015.
National Health and Family Planning Commission of the People’s Republic of China. National essential drug list (2012 edition). http://www.sdpc.gov.cn/zcfb/zcfbtz/201301/W020130110304201259649.pdf. Accessed Oct 2, 2015.
Yang J, Li J. Premixed or basal insulin: the insulin initiation consideration in Chinese patients with type 2 diabetes mellitus. Chin J Endocrinol Metab. 2013;29(5):5b–1.
Kohro T, Yamazaki T, Sato H, Harada K, Ohe K, Komuro I, et al. Trends in antidiabetic prescription patterns in Japan from 2005 to 2011. Int Heart J. 2013;54:93–7.
Zagarins SE, Allen NA, Garb JL, Welch G. Improvement in glycemic control following a diabetes education intervention is associated with change in diabetes distress but not change in depressive symptoms. J Behav Med. 2012;35:299–304.
Wardian J, Sun F. Factors associated with diabetes-related distress: implications for diabetes self-management. Soc Work Health Care. 2014;53:364–81.
Acknowledgments
Sponsorship and article processing charges for this study were funded by Eli Lilly and Company. Medical writing assistance was provided by Elise Magatova, PhD and Rebecca Lew, PhD, CMPP of ProScribe-Envision Pharma Group, and was funded by Eli Lilly Japan K.K. ProScribe’s services complied with international guidelines for Good Publication Practice (GPP2).
This work was funded by a grant to Brigham and Women’s Hospital from Eli Lilly for the MOSAIc study (Fund Number 2200-107512). The authors retained independent and complete control over the design and implementation of the study, as well as the analyses and writing of the manuscript, the manuscript contents, and the decision to publish. Eli Lilly reviewed the manuscript, but the final decision to publish and decisions as to what was published were retained by the study authors.
All authors participated in reviewing the data and providing comments to the manuscript. All authors approved the final version of the manuscript and take full responsibility for the content. IM, DJ, JH, KW, LS, SS, and SK were involved in the study design. IM, TS, KT, AK, HM, HT, KT, MA, MK, SK, SU, and TA acted as trial investigators. IM, TS, KT, AK, HM, HT, KT, MA, MK, SK, SJ, and TA were involved in data collection. DJ, KU, and SK were involved in data analysis. All authors were involved in data interpretation. DJ and SS wrote the manuscript.
The authors thank all the patients and study sites involved in these studies.
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval for the version to be published.
Disclosures
S Suzuki is an employee of Eli Lilly Japan K.K. D. Jiang was an employee of Eli Lilly and Company when the work was completed, and is a minor stock shareholder of Eli Lilly and Company. K. Wang and L. Shen are employees of Eli Lilly Suzhou Pharmaceutical Company. J. Han is an employee of Lilly Korea Ltd. S. Kim has received research grants from Pfizer and AstraZeneca for unrelated studies. I. Matsuba has received research grants from Kowa Pharmaceutical for unrelated studies. T. Sawa, M. Ajima, T. Asakura, S. Umezawa, S. Kim, M. Kaneshiro, T. Kawata, A. Kanamori, H. Machimura, H. Takeda and K. Tanaka have nothing to disclose.
Compliance with Ethics Guidelines
This article is based on previously conducted studies and does not involve any new studies of human or animal subjects performed by any of the authors.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced content
To view enhanced content for this article go to www.medengine.com/Redeem/87D4F0601ADAD36B.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Matsuba, I., Sawa, T., Kawata, T. et al. Cross-National Variation in Glycemic Control and Diabetes-Related Distress Among East Asian Patients Using Insulin: Results from the MOSAIc Study. Diabetes Ther 7, 349–360 (2016). https://doi.org/10.1007/s13300-016-0178-7
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13300-016-0178-7