Abstract
In order to study estrogen-driven microenvironment associated with type 1 endometrial carcinoma, we evaluated estrogen receptors (ERs), aromatase, and cyclooxygenase II (COX2) molecular and immunohistochemical profiles with correlation to clinicopathological features. We investigated aromatase, ERα, ERβ, and COX2 expression at the mRNA and protein levels using quantitative real-time PCR and immunohistochemical method in 51 endometrial carcinomas and 16 normal endometria. All the studied tumors, as well as normal endometria, expressed ERα, ERβ, and COX2 mRNAs. Five endometrial carcinoma tissues and one normal endometrium showed no aromatase mRNA expression. The majority of tumors expressed ERα (82 %), aromatase (80 %), and COX2 (88 %) proteins. Forty-one percent of the studied tumors were ERβ-negative. ERα and ERβ showed significantly decreased mRNA and protein expression levels in endometrial carcinoma as compared to normal endometrium. An opposite trend was shown for COX2 and aromatase proteins. ERα expression correlated positively with COX2 expression at both mRNA and protein levels (P < 0.005, r = 0.398; P < 0.0005, r = 0.510, respectively). There was also a positive correlation between COX2 and aromatase expression in cancer tissue (P < 0.002, r = 0.433 for transcriptional level; P < 0.0005, r = 0.614 for protein level). We observed positive correlations between ERβ and ERα, as well as between ERβ and COX2 at the transcriptional level only (P < 0.0005, r = 0.644; P < 0.002, r = 0.444, respectively). Negative correlations were found between pT category of primary tumor and levels of ERα and ERβ transcripts (P < 0.02, r = −0.332; P < 0.02, r = −0.348, respectively). A negative association between ERβ and the International Federation of Gynecology and Obstetrics (FIGO) staging was also found. The growth of EC1 with the presence of ERα and overexpression of aromatase and COX2 is dependent on estrogens. We believe that ERβ may be considered as a potential marker in the progression of disease in endometrial cancer patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Endometrial adenocarcinoma is the most common gynecologic malignancy in women worldwide. The precise molecular mechanism underlying endometrial carcinoma is poorly understood; however, it is known that the development of endometrial carcinoma (EC) occurs as a result of genetic, metabolic, and hormonal changes. A dualistic model of endometrial cancer was proposed based on histological and molecular pathology observations, i.e., type 1—estrogen-dependent adenocarcinoma with endometrioid morphology (EC1), and type 2—non-estrogen-dependent adenocarcinoma (EC2) [1, 2].
The risk of EC1 is postulated to be linked with prolonged estrogen exposure and action, especially that unopposed by progestogens [3–5]. Unbalanced estrogen excess can lead to an increase in the proliferation rate of endometrial cells with an increasing frequency of coding errors and somatic mutation appearance [6].
The biological effect of estradiol in the uterus is mediated through two estrogen receptors: estrogen receptor (ER) α and ERβ. The distinct role of these two receptors in the uterus was evaluated using ERα (αERKO) and ERβ (βERKO) knockout female mice study. ERα plays an important role in the differentiation and proliferation of epithelial cells, whereas the role of ERβ was proposed to act as ERα modulator exerting an antiproliferative function in the uterus [7]. The most important question is whether the same mechanisms of ER action observed in the uterus of knockout mice might exist in human healthy and/or malignant endometrial tissue.
In normal premenopausal endometrium, the ER expression and distribution change during the cycle. ERα and ERβ are mainly co-expressed in the glandular epithelial cells with similar cyclic changes in the uterus, with a markedly higher ERα expression compared to ERβ during proliferative as well as secretory phases. ERs were also shown to be expressed in stromal cells, with predominance of ERα and a weaker expression of ERβ in the proliferative phase and ERβ absence in the secretory phase [7].
The number of studies on the significance of ER-dependent signaling in endometrial tumor cells is still limited. Additionally, there are certain conflicting data on the usefulness of the estrogen receptor status as an independent prognostic factor in endometrial cancer patients.
However, it has been shown that endometrial cancer cells are estrogen-responsive and are controlled by endogenous ERs and local estrogen biosynthesis [8]. Recent studies on estrogen-dependent tumors such as breast and endometrial cancers revealed the significance of in situ estrogen biosynthesis and metabolism in the biology of these tumors. The main source of intratissular estrogens in estrogen-dependent EC1 tumors is the bioconversion of androgen to estrogen in the stromal cells by the key enzyme involved in local estrogen production, i.e., aromatase [9]. Segawa et al. [10] revealed the role of aromatase in tumor progression, demonstrating a significant correlation between aromatase expression in stromal cells and poor prognosis in women suffering from endometrial cancer. The main secretory factor inducing aromatase expression in the surrounding stromal cells in breast tumor was found to be prostaglandin E2 (PGE2) [11, 12]. A similar mechanism of aromatase induction seems to occur in endometrial cancer. In EC1, similarly to breast cancer, the expression level of aromatase correlates with cyclooxygenase II (COX2), the enzyme responsible for PGE2 synthesis. In addition, estrogens which act through both estrogen receptors and are synthesized by aromatase in postmenopausal women could increase COX2 expression level in this way.
The aim of our study was to investigate ERs, aromatase, and COX2 expression in type 1 endometrial cancer and normal endometrium with the molecular and clinical correlations.
Materials and methods
Patients and samples
Tissue samples were obtained from 51 postmenopausal women who underwent total abdominal hysterectomy because of endometrial carcinoma. Standard histopathological parameters were determined by two independent pathologists. In each case, endometrial cancer risk factors such as age, the presence of hypertension, obesity, and type 2 diabetes were evaluated. The age of patients ranged from 48 to 80 years (mean 64 years). Tumor stage, age range, and body mass index (BMI) of endometrial cancer patients are presented in Table 1. Histologically, normal endometrium samples of middle to late proliferative phase of menstrual cycle were obtained during hysterectomies due to uterine leiomyomas from 10 (for immunohistochemical (IHC) study) and 16 (for molecular analysis) premenopausal women (age range 35–54 years). The specimens collected for molecular analysis were frozen in liquid nitrogen and kept at −80 °C until molecular studies were performed. For IHC study, tissue samples were fixed in 10 % buffered formaldehyde solution for 48 h and then embedded in paraffin blocks at 56 °C according to standard procedures. Tumor samples were cut into 5-μm-thick sections and stained with hematoxylin–eosin.
The protocol of this study was approved by the local ethical committee of the Medical University of Bialystok, Poland.
RNA extraction and cDNA synthesis
Total RNA was extracted from EC and endometrial control tissues according to the Chomczynski and Sacchi method with a minor modification [13]. RNA integrity was verified by electrophoresis in 1.5 % (w/v) agarose gel and staining with ethidium bromide, and by amplification of housekeeping gene, 18s rRNA. RNA was quantified spectrophotometrically at 260 nm. One microgram of total RNA was used to prepare cDNA. cDNA synthesis was performed in 50 mM Tris–HCl (pH 8.3), 75 mM KCl, 3 mM MgCl2, 10 mM DTT, 1 mM dNTP mix (Promega), 2.5 μM random hexamers, 20 U RNasin Ribonulease Inhibitor (Promega), and 100 U MMLV Reverse Transcriptase (Promega) in a final volume of 40 μl using an MJ Research Thermal Cycler (Model PTC-200, Watertown, Massachusetts, USA). For reverse transcription, the mixtures were incubated at 42 °C for 60 min and then heated at 95 °C for 5 min and finally rapidly cooled at 4 °C. Negative control samples were generated by omitting the enzymes and RNA template in the reverse transcription reaction.
Quantitative real-time PCR
In order to determine the amounts of ERα, ERβ, aromatase, and COX2 expression levels, standard curves for each gene separately were constructed with serially diluted PCR products. PCR products were obtained by amplification of cDNA from Ischikawa cells using specific primers as follows: 5′TGCTTCAGGCTACCATTATGGAGTCTG3′ and 5′GTCAGGGACAAGGCCAGGCTG3′ for ERα; 5′TTTAAAAGAAGCATTCAAGGACATAATG3′ and 5′CGGTGAAGGGCGCACTG3′ for ERβ; 5′GCCACTGAGTTGATTTTAGC3′ and 5′CCAAATGGCTGAAAGTACC3′ for aromatase; 5′CTCAAACATGATGTTTGCATTC3′ and 5′CAGGGACTTGAGGAGGGTTAGATC3′ for COX2; and 5′CGTCTGCCCTATCAACTTTCG3′ and 5′CGCGGTCCTATTCCATTATTC3′ for 18s rRNA. PCR was carried out in a final volume of 20 μl using 10 pmol of each of the primers, 40 μM of each of dNTPs, 1 U HotStarTaq polymerase (Qiagen GmbH, Hilden, Germany), 2 μl 10× PCR buffer, and 2 μl cDNA. PCR was carried out under the following conditions: 15 min polymerase activation at 95 °C, 1 min denaturation at 94 °C, 1 min annealing at 65 °C, and 1 min extension at 72 °C for 40 cycles, with an additional 5 min of extension at 72 °C for the last cycle. Amplified products were separated on a 2 % (w/v) agarose gel, extracted, and purified from agarose slices using DNA Gel Extraction Kit (Millipore, USA), quantified by the use of One Dscan/Zero Dscan software (Scanalytics Inc., USA) and then serially diluted in sterile water.
We used Assays-on Demand Gene Expression Assays (Applied Biosystems) to determine the mRNA level of the studied genes. All the quantitative real-time (Q-RT) PCR reactions were performed using ABI Prism 7500 Sequence Detection System (Applied Biosystems, USA). For each PCR run, a reaction mix was prepared with 10 μl 2× TaqMan Gene Expression PCR Master Mix (Applied Biosystems), 1 μl 20× Assays-on Demand Gene Expression Assay Mix (Applied Biosystems), 2 μl cDNA, and sterile water to the final volume of 20 μl. To evaluate the amounts of the studied transcripts, all the results obtained in attogram or femtogram according to standard curves were converted to attomole or femtomole of each transcript and then normalized by the level of 18s rRNA. The relative quantification was given by the ratio between the mean value of the target gene and the mean value of the reference gene (18s rRNA) for each sample.
Immunohistochemistry
For immunohistochemical studies, we selected two representative sections from each case.
Five biological markers were investigated using IHC study: ERα, ERβ, COX2, aromatase, and Ki-67. ERα was detected with a mouse monoclonal antibody (Ab) F-10 (Santa Cruz Biotechnology, USA) at a dilution of 1:200. ERβ was detected with a monoclonal Ab EMR02 (NCL-ER-beta, Novocastra) at a dilution of 1:100. COX2 was assessed using monoclonal Ab (NCL-COX2, Novocastra) at a dilution of 1:200. Ki-67 was assessed using the monoclonal mouse Ab MIB-1 (Dako, Denmark) at a dilution of 1:100. Aromatase expression was assessed using a rabbit polyclonal Ab R-10-2 against cytochrome P450 aromatase at a dilution of 1:800 (a generous gift from Dr. Yoshio Osawa, Hauptman-Woodward Medical Research Institute, Buffalo, NY, USA).
The sections were deparaffinized in xylenes and hydrated through graded alcohols. Antigen unmasking was performed using heat treatment in a microwave oven at 750 W for 6 min in a container with 10 mM sodium citrate buffer at pH 6.0. The sections were allowed to cool in the buffer at room temperature for 30 min and were rinsed in deionized H20 three times for 2 min each. The endogenous peroxidase activity was blocked with 1 % hydrogen peroxide for 20 min. After rinsing in PBS, the sections were incubated for 1 h with a proper 1.5 % normal blocking serum in PBS. The blocking reagent was removed, and then the sections were incubated with MIB-1 antibody for 1 h at room temperature or with ERα, ERβ, COX2, and aromatase antibody at 4 °C overnight using staining chamber (The Binding Site, UK). Primary antibodies were diluted in PBS with 1.5 % normal blocking serum.
The studies for ERβ, COX2, and aromatase were performed with EnVision System (Dako, Denmark); for ERα, with avidin–biotin-peroxidase complex (ABC Staining System, Santa Cruz, USA); and for Ki-67, with streptavidin–biotin-peroxidase complex (LSAB Kit, Dako, Denmark) to reveal Ab–antigen reactions. Staining was routinely developed using 3,3′-diaminobenzidine as a chromogen (Dako, Denmark). The sections were counterstained with hematoxylin.
Immunoreactivities were scored in light microscopy in ten different fields under magnification of ×200, and the mean percentage of tumor cells which showed positive staining was assessed. In discriminating protein-positive from -negative tumors, the cutoff was 10 % malignant cells that expressed the investigated marker from all the cancer cells of the microscopic slide. The expression of the studied markers (ERs, COX2, Ki-67) was graded in four-tiered system: 0 (defined as negative cases) less than 10 % positive cells (thus, this was in reality a very weak positive result); 1+ with immunoreactivity ranging from 10 to 50 % of positive cancer cells (moderately positive); 2+ with over 50 % of positive cells; and 3+ over 50 % of positive cells with a strong reaction. The expression of aromatase was graded in five-tiered system: 0 (defined as negative cases) less than 10 % positive cells; 1+ with immunoreactivity ranging from 10 to 50 % of positive cancer cells (moderately positive); 2+ with over 50 % of positive cells (positive reaction); 3+ less than 50 % of positive cells with a strong reaction; and 4+ over 50 % of positive cells with a strong reaction.
Statistical analysis
Mean values ± standard deviation (SD) and median were calculated. The Student t test was used to compare normally distributed continuous variables and Mann–Whitney for abnormally distributed ones. The Spearman’s and Pearson’s correlation coefficients were estimated. Linear regression analysis was also used. The analysis was done using statistical software package SPSS, accepting P < 0.05 as significant.
Results
Expression profile of ERα, ERβ, aromatase, and COX2 in EC and normal endometrium
To evaluate the levels of ERα, ERβ, aromatase, and COX2 mRNA expression, Q-RT-PCR with manually prepared curves was used. All results obtained in femtogram for ERα and COX2 or attogram for ERβ and aromatase were converted to femtomole or attomole of transcript per microgram of total RNA and then normalized by the level of 18s rRNA. All the studied tumors as well as normal endometria expressed ERα, ERβ, and COX2 mRNAs. Five EC tissues and one normal endometrium showed no aromatase mRNA expression. The studied cancerous samples showed the highest values of ERα transcript at femtomolar levels ranging from 0.43 to 286.98 with one cancerous tissue presenting elevated ERα mRNA level: 1,776.04 (mean 85.92 ± SD 258.58) comparing to normal endometria ranging from 38.7 to 681.4 (mean 253.99 ± SD 172.75). ERβ and aromatase were expressed at the lowest transcriptional attomolar level (0.0026 to 5.69, mean 0.48 ± SD 1.02 for ERβ in cancerous tissues; 0.36 to 2.94, mean 0.88 ± SD 0.81 for ERβ in control tissues; 0.0002 to 0.29, mean 0.02 ± SD 0.06 for aromatase in cancerous tissues; and 0.0005 to 0.24, mean 0.03 ± SD 0.02 for aromatase in normal endometria) (Table 2, Fig. 1).
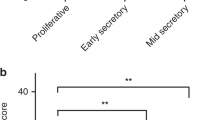
Comparative analysis of ERα (a), ERβ (b), aromatase (c), and COX2 (d) mRNA expression levels in endometrial cancer (EC) and normal proliferative endometrium (control). Statistically lower expression level of ERα, ERβ, and aromatase in cancerous tissues compared to normal endometrium were presented (P < 0.0005, P < 0.0005, and P < 0.012, respectively)
Antigen expressions were analyzed by immunohistochemistry in all the human endometrial tumors and normal endometria mentioned above; the results are presented in Tables 2 and 3. ERα (Fig. 2a) and Ki-67 (Fig. 2d) were detected in the nuclei, whereas ERβ (Fig. 2b) was found in the cytoplasm of cancer and normal endometrial cells. We observed COX2 expression mainly in the cytoplasm of normal endometrial and cancer cells, and only a few inflammatory cells showed a positive COX2 expression (Figs. 2e, f and 3a, b). Aromatase expression was detected mainly in the cytoplasm of cancer endometrial cells, and only weak immunostaining was found in part of normal endometria as well as in stromal cells (Figs. 2c and 3c, d).
a–f Immunohistochemical detection of ERα, ERβ, aromatase, Ki-67, and COX2 in the human endometrial cancer. a Strong nuclear immunostaining of ERα in endometrial cancer cells with most intense immunoreactivity in the invasive front of tumor. b Mainly cytoplasmic and only weak perinuclear localization of ERβ in cancerous cells. c Strong cytoplasmic immunostaining of aromatase in endometrial cancer cells. d Nuclear heterogeneous immunostaining of Ki-67. e–f Strong cytoplasmic immunostaining of COX2 in cancerous cells with focal perinuclear immunoreactivity. Original magnification: a ×100. b–e ×200. f ×400
a–d. Expression of COX2 and aromatase in endometrial cancer and adjacent normal endometrium. a, b Cytoplasmic localization of COX2 immunostaining in endometrial and cancer cells with weak or strong expression, respectively. c, d Strong cytoplasmic immunoreactivity of aromatase in endometrial cancer, while only weak immunostaining in part of normal endometrium as well as in stromal cells. Original magnification: a ×100. b–d ×200
In the present study, the analyzed EC tissues showed a much larger amount of both ERα and ERβ mRNAs than normal endometrial tissues (Fig. 1, Table 2). IHC study confirmed greater expression of ERα and ERβ proteins in normal endometrium compared with EC, yet with no significant difference (Table 2).
Aromatase mRNA levels in the normal and cancerous endometrial samples were extremely low. We observed small differences in aromatase mRNA expression levels between tumor and normal tissues with slightly elevated mRNA level in normal tissues (Fig. 1, Table 2). An opposite trend was found for aromatase at the protein level which was significantly higher in EC than in the control tissues (Table 2). Interestingly, 50 % of studied normal endometria showed no aromatase expression, and 50 % of those tissues showed only weak (1+) aromatase immunostaining (Table 3, aromatase). About 60 % of the studied cancerous endometria expressed aromatase at a high level (2+, 3+, 4+) (Table 3, aromatase).
The expression of COX2 was significantly elevated in EC in comparison to the control tissue (Tables 2 and 3, COX2; Fig. 1).
Correlations between ERα, ERβ, aromatase, and COX2 in EC
ERα expression correlated positively with COX2 expression at both mRNA and protein levels (P < 0.005, r = 0.398; P < 0.0005, r = 0.510, respectively). There was also a statistically significant positive correlation between COX2 and aromatase expression in cancer tissue (P < 0.002, r = 0.433 for the transcriptional level; P < 0.0005, r = 0.614 for the protein level). Positive correlations were also observed between ERβ and ERα as well as ERβ and COX2 at the transcriptional level only (P < 0.0005, r = 0.644; P < 0.002, r = 0.444, respectively). A negative correlation was found between ERα mRNA expression and Ki-67 status (P < 0.04, r = −0.299).
Correlations of ERα, ERβ, aromatase, and COX2 expression with selected clinical, pathological, and metabolic features
Statistically negative correlations were found between depth of myoinvasion—pT category (where T1A—tumor limited to the endometrium or invades less than one half of the myometrium; T1B—tumor invades one half or more of the myometrium; T2—tumor invades stromal connective tissue of the cervix but does not extend beyond the uterus; and T3—tumor involves the uterine serosa, parametrium, vagina, or adnexa) and levels of ERα and ERβ transcripts (P < 0.02, r = −0.332; P < 0.02, r = −0.348, respectively). Interestingly, ERβ expression assessed by Q-RT-PCR was negatively correlated with the International Federation of Gynecology and Obstetrics (FIGO) stage (P = 0.007, r = −0.385). Additionally, linear regression analysis, with FIGO stage as dependent variable, confirmed negative influence of ERβ mRNA expression (B coefficient = −0.386) and also ERβ protein level (B coefficient = −0.411) on FIGO with r square = 0.247.
We also found that the expression of ERα at mRNA and protein level was negatively associated with tumor differentiation (G) (P < 0.02, r = −0.337; P < 0.05, r = −0.288, respectively). Moreover, we observed weak statistically significant differences in Ki-67 proliferation status and G (P < 0.02, r = 0.321). We found no association between the expression levels of the studied factors and the age of patients.
No correlations between hypertension, smoking, and diabetes and the expression level of the studied genes were found. However, aromatase at the protein level was positively associated with BMI (P < 0.01, r = 0.346).
Discussion
The incidence of estrogen-dependent type 1 endometrial cancer is the highest in postmenopausal women when the ovaries have ceased producing estrogen. Despite its relatively good prognosis when diagnosed in its early stages, more than 20 % of patients die due to endometrial carcinoma [14, 15]. This data may reflect, at least partly, the failure of currently available diagnostic tools in EC, especially in identifying premalignant stages. There are still gaps in developing efficient prognostic markers and individual treatment in EC.
Type 1 endometrial adenocarcinoma is accepted to be an endocrine-related neoplasm and an established target of estrogen action. In order to study the estrogen-driven microenvironment associated with EC, we evaluated ERs, aromatase, and COX2 status in endometrial cancer patients. Estrogen in postmenopausal EC women originates from peripheral sites, mainly from adipose tissue and in cancerous endometrium from precursors of adrenal or ovarian origin via aromatase pathway. However, the data on aromatase expression in both normal and cancerous endometria seem rather unclear. There are discrepancies in the results presented in the available literature. The available studies show no aromatase mRNA in nonmalignant tissue versus cancerous tissue [16] and no significant differences between cancerous and adjacent normal endometrium [17–19], or demonstrate increased aromatase activity in neoplastic endometrium [20]. Our present study shows that the aromatase mRNA level was slightly higher in normal tissue in comparison to cancerous endometrium. Interestingly, protein expression and distribution analysis revealed aromatase overexpression in cancer tissue. More than 60 % of the studied EC showed strong cytoplasmic immunoreactivity, whereas normal endometrium presented very low (1+) or negative aromatase expression in glandular epithelial and stromal cells. We showed no correlation between aromatase expression and clinicopathological EC characteristics; however, aromatase at the protein level was positively associated with BMI. BMI is an unquestionable risk factor of endometrial cancer [21, 22]. It is not surprising that aromatase expression responsible for hyperestrogenic state in postmenopausal women is associated with the excess of adipose tissue as we have shown in the present study. However, some studies, focused on the increased BMI and treatment outcome in EC, revealed that elevated BMI is not an unfavorable prognosticator [23–25], in contrast with breast, ovary, prostate, and colorectal malignancies. Recent findings from the MRC ASTEC trial indicated that obesity related to hyperestrogenic state is associated with an increased incidence of the less aggressive type of endometrial cancer (type 1) and thus predicts for a more favorable outcome after treatment [26].
The statistically positive correlation between aromatase and COX2 shown in our study confirms that apart from aromatase, COX2 seems to be another important player in the hormonal loop implicated in estrogen production in EC. We have shown that COX2 is expressed at a markedly higher level in cancerous endometrium compared to normal endometrium. Despite the evident differences between the mean values of COX2 transcript levels in cancerous versus normal endometrium, we observed no significant association. Interestingly, at the protein level, COX2 was statistically significantly elevated in tumor as compared to normal endometrium controls. Moreover, all of the studied endometrial tumor samples expressed COX2 in the cytoplasm of cancer as well as inflammatory cells; however, 40 % of control tissues did not show the COX2 expression. We observed a very high immunoreactivity (2+ and 3+) in cancerous cells in 55 % of the patients.
Recent studies, presenting proteomic approach, confirmed that there exist several dysregulated and metabolic networks in EC [27]. Indeed, the authors revealed the significant interactions between some of the altered molecule families associated with oxidative phosphorylation, mitochondrial dysfunction, and inflammatory process. Among the candidate biomarkers associated with the early stages of tumorigenesis process in EC, COX2 was found to correlate with NFkB-regulated cytokines and their receptors and, indirectly, with the protein from peroxiredoxin family (PRD3) involved in supporting tumor maintenance in cancer cells [27]. The role of estrogens and their receptors in this oxidative/inflammatory network is still not clear. However, contrary to others [28], our study reveals the correlation between ERα and COX2, at both transcriptional and protein levels, whereas ERβ is associated with COX2 only at the mRNA level, suggesting that there might be a similar biological pathway in endometrial cancer cells that could sustain steroid hormones and COX2-mediated cellular activities. The divergent pattern of ERα and COX2 distributions in endometrial cancer do not exactly exclude the positive correlation between these studied factors. It is possible that in the tumors possessing ERα, the ERα expression level is positively correlated with COX2, despite the divergent distribution of these transcripts/proteins in cancerous versus control tissues. It is well accepted that estrogenic effect in endocrine-dependent cancers, including endometrial cancer, occurs predominantly through ERα; however, the role of ERβ in endometrial carcinogenesis process or tumor phenotype and biology still remains an open question. Our present study is in accordance with the previous data showing higher ERs expressed in noncancerous endometrium compared with endometrial cancer [29]. However, Knapp et al. [30] showed elevated ER protein level in endometrial cancer compared to a healthy mucosa. The analysis of the early stage of endometrial carcinoma (FIGO I stage only) and use of Western blot method for estimating protein level of ERs with different antibodies may explain the discrepancy. Moreover, our present study reveals that ERα is always expressed in normal endometrium, while about 18 % of the studied ECs are ERα-negative. ERβ is differently expressed in these two types of tissues. In contrast to ERα, ERβ is absent in 20 % of normal proliferative endometrial tissues, and 41.2 % of the examined cancer tissues are ERβ-negative.
It is believed that the imbalance in the ERα/ERβ expression could be a possible critical step in the progress of estrogen-dependent tumorigenesis. Some authors proposed that altered balance of ERα/ERβ toward decreasing ERα/ERβ ratio due to significantly lower ERα expression could lead to a perturbed effect on cell-cycle progression and further increase the cell risk of transforming mutations [31, 32]. However, our data showed no statistically significant differences in the ERα/ERβ ratio between normal and cancerous endometrium.
In the present study, we revealed mainly cytoplasmic and only weak perinuclear localization of ERβ in cancerous cells. This cytosolic existence of ERβ might indicate the mechanism of ER action on tumor biology that is probably different from the classical one. The presence of ERβ within the mitochondria and therefore its action with mitochondrial molecules or proteins might presumably influence the hormonal phenotype of EC1. Interestingly, we demonstrated a negative association between ERβ and FIGO stage using linear regression analysis. However, it should be noted that the majority (66 %) of EC1, included in this study, was diagnosed as FIGO I, grades 1–3. Our observation favors the idea about the potential protective role of ERβ against endometrial tumor progression.
It should be noted, that the estrogen effect can be mediated not only by genomic action through classical ERs but also by the nongenomic pathway through membrane estrogen receptor, i.e., G protein-coupled estrogen receptor (GPER). Indeed, GPER together with ERα recently were found to be expressed in epithelial and stromal cells of normal human endometrium, especially in the proliferative phase [33]. Interestingly, loss of GPER in ERα-positive patients suffering from endometrial cancer resulted in reduced 5-year survival [34]. These data, together with our results, could direct future studies to delineate the role of classical ERs and membrane ER-dependent pathways in endometrial cancer pathology.
In summary, when we compared EC1 versus noncancerous endometrial tissue, we were able to show decreased mRNA and protein expression of ERs in EC1. Aromatase and COX2 protein overexpression and distribution in EC1 provide estrogen source in these tumors. Altogether, estrogens produced locally in EC1 (by the aromatase–COX2 loop) through ERα may possibly enhance tumor growth. This statement should be verified using in vitro studies. The role of ERβ in the cancerous process in endometrial tissue is still not precisely defined. However, our observations suggest that ERβ may play an important role in the etiology and biology of EC1 and may protect against the growth-promoting effects of the estrogens.
References
Bokhman JV. Two pathogenetic types of endometrial carcinoma. Gynecol Oncol. 1983;15:10–7.
Rose PG. Endometrial carcinoma. N Engl J Med. 1996;335:640–9.
Zeleniuch-Jacquotte A, Akhmedkhanov A, Kato I, Koenig KL, Shore RE, Kim MY, et al. Postmenopausal endogenous oestrogens and risk of endometrial cancer: results of a prospective study. Br J Cancer. 2001;84:975–81.
Potischman N, Hoover RN, Brinton LA, Siiteri P, Dorgan JF, Swanson CA, et al. Case–control study of endogenous steroid hormones and endometrial cancer. J Natl Cancer Inst. 1996;88:1127–35.
Parazzini F, la Vecchia C, Bocciolone L, Franceschi S. The epidemiology of endometrial cancer. Gynecol Oncol. 1991;41:1–16.
Park CK, Apte S, Acs G, Harris EER. Cancer endometrium. In: Abeloff M, Armitage J, Niederhuber J, Kastan M, McKenna W, editors. Abeloff’s clinical oncology. 4th ed. Philadelphia: Elsevier; 2008.
Weihua Z, Saji S, Mäkinen S, Cheng G, Jensen EV, Warner M, et al. Estrogen receptor (ER) beta, a modulator of ERalpha in the uterus. Proc Natl Acad Sci U S A. 2000;97:5936–41.
Matsumoto M, Yamaguchi Y, Seino Y, Hatakeyama A, Takei H, Niikura H, et al. Estrogen signaling ability in human endometrial cancer through the cancer-stromal interaction. Endocr Relat Cancer. 2008;15:451–63.
Bulun SE, Chen D, Lu M, Zhao H, Cheng Y, Demura M, et al. Aromatase excess in cancers of breast, endometrium and ovary. J Steroid Biochem Mol Biol. 2007;106:81–96.
Segawa T, Shozu M, Murakami K, Kasai T, Shinohara K, Nomura K, et al. Aromatase expression in stromal cells of endometrioid endometrial cancer correlates with poor survival. Clin Cancer Res. 2005;11:2188–94.
Zhao Y, Agarwal VR, Mendelson CR, Simpson ER. Estrogen biosynthesis proximal to a breast tumor is stimulated by PGE2 via cyclic AMP, leading to activation of promoter II of the CYP19 (aromatase) gene. Endocrinology. 1996;137:5739–42.
Singh A, Purohit A, Ghilchik MW, Reed MJ. The regulation of aromatase activity in breast fibroblasts: the role of interleukin-6 and prostaglandin E2. Endocr Relat Cancer. 1999;6:139–47.
Chomczynski P, Sacchi N. Single-step method of RNA isolation by acid guanidinium thiocyanate–phenol–chloroform extraction. Anal Biochem. 1987;162:156–9.
Llauradó M, Ruiz A, Majem B, Ertekin T, Colás E, Pedrola N, et al. Molecular bases of endometrial cancer: new roles for new actors in the diagnosis and the therapy of the disease. Mol Cell Endocrinol. 2012;358:244–55.
Jereczek-Fossa B, Badzio A, Jassem J. Surgery followed by radiotherapy in endometrial cancer: analysis of survival and patterns of failure. Int J Gynecol Cancer. 1999;9:285–94.
Bulun SE, Imir G, Utsunomiya H, Thung S, Gurates B, Tamura M, et al. Aromatase in endometriosis and uterine leiomyomata. J Steroid Biochem Mol Biol. 2005;95:57–62.
Jongen VH, Thijssen JH, Hollema H, Donker GH, Santema JG, van der Zee AG, et al. Is aromatase cytochrome P450 involved in the pathogenesis of endometrioid endometrial cancer? Int J Gynecol Cancer. 2005;15:529–36.
Pathirage N, di Nezza LA, Salmonsen LA, Jobling T, Simpson ER, Clyne CD. Expression of aromatase, estrogen receptors, and their coactivators in patients with endometrial cancer. Fertil Steril. 2006;86:469–72.
Smuc T, Rizner TL. Aberrant pre-receptor regulation of estrogen and progesterone action in endometrial cancer. Mol Cell Endocrinol. 2009;301:74–82.
Watanabe K, Sasano H, Harada N, Ozaki M, Niikura H, Sato S, et al. Aromatase in human endometrial carcinoma and hyperplasia. Immunohistochemical, in situ hybridization, and biochemical studies. Am J Pathol. 1995;146:491–500.
Renehan AG, Tyson M, Egger M, Heller RF, Zwahlen M. Body-mass index and incidence of cancer: a systematic review and meta-analysis of prospective observational studies. Lancet. 2008;371:569–78.
Crosbie EJ, Zwahlen M, Kitchener HC, Egger M, Renehan AG. Body mass index, hormone replacement therapy, and endometrial cancer risk: a meta-analysis. Cancer Epidemiol Biomarkers Prev. 2010;19:3119–30.
Everett E, Tamimi H, Greer B, Swisher E, Paley P, Mandel L, et al. The effect of body mass index on clinical/pathologic features, surgical morbidity, and outcome in patients with endometrial cancer. Gynecol Oncol. 2003;90:150–7.
Martra F, Kunos C, Gibbons H, Zola P, Galletto L, DeBernardo R, von Gruenigen V. (2008) Adjuvant treatment and survival in obese women with endometrial cancer: an international collaborative study. Am J Obstet Gynecol. 198:89. e1–8.
Münstedt K, Wagner M, Kullmer U, Hackethal A, Franke FE. Influence of body mass index on prognosis in gynecological malignancies. Cancer Causes Control. 2008;19:909–16.
Crosbie EJ, Roberts C, Qian W, Swart AM, Kitchener HC, Renehan AG. Body mass index does not influence post-treatment survival in early stage endometrial cancer: results from the MRC ASTEC trial. Eur J Cancer. 2012;48:853–64.
Maxwell GL, Hood BL, Day R, Chandran U, Kirchner D, Kolli VS, et al. Proteomic analysis of stage I endometrial cancer tissue: identification of proteins associated with oxidative processes and inflammation. Gynecol Oncol. 2011;121:586–94.
Ferrandina G, Ranelletti FO, Gallotta V, Martinelli E, Zannoni GF, Gessi M, et al. Expression of cyclooxygenase-2 (COX-2), receptors for estrogen (ER), and progesterone (PR), p53, ki67, and neu protein in endometrial cancer. Gynecol Oncol. 2005;98:383–9.
Fowler JM, Ramirez N, Cohn DE, Kelbick N, Pavelka J, Ben-Shachar I, et al. Correlation of cyclooxygenase-2 (COX-2) and aromatase expression in human endometrial cancer: tissue microarray analysis. Am J Obstet Gynecol. 2005;192:1262–73.
Knapp P, Chabowski A, Błachnio-Zabielska A, Walentowicz-Sadłecka M, Grabiec M, Knapp P. Expression of estrogen receptors (α, β), cyclooxygenase-2 and aromatase in normal endometrium and endometrioid cancer of uterus. Adv Med Sci. 2013;24:1–8.
Jazaeri AA, Nunes KJ, Dalton MS, Xu M, Shupnik MA, Rice LW. Well-differentiated endometrial adenocarcinomas and poorly differentiated mixed mullerian tumors have altered ER and PR isoform expression. Oncogene. 2001;20:6965–9.
Saegusa M, Okayasu I. Changes in expression of estrogen receptors alpha and beta in relation to progesterone receptor and pS2 status in normal and malignant endometrium. Jpn J Cancer Res. 2000;91:510–8.
Kolkova Z, Noskova V, Ehinger A, Hansson S, Casslén B. G protein-coupled estrogen receptor 1 (GPER, GPR 30) in normal human endometrium and early pregnancy decidua. Mol Hum Reprod. 2010;16:743–51.
Krakstad C, Trovik J, Wik E, Engelsen IB, Werner HM, Birkeland E, et al. Loss of GPER identifies new targets for therapy among a subgroup of ERα-positive endometrial cancer patients with poor outcome. Br J Cancer. 2012;106:1682–8.
Acknowledgments
This work was financially supported by the Polish Ministry of Higher Education (KBN grant no. 2 PO5E 06428).
Conflict of interest
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution License which permits any use, distribution, and reproduction in any medium, provided the original author(s) and the source are credited.
About this article
Cite this article
Jarzabek, K., Koda, M., Walentowicz-Sadlecka, M. et al. Altered expression of ERs, aromatase, and COX2 connected to estrogen action in type 1 endometrial cancer biology. Tumor Biol. 34, 4007–4016 (2013). https://doi.org/10.1007/s13277-013-0991-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13277-013-0991-9