Abstract
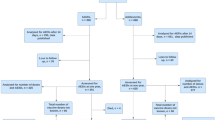
Routine vaccination with three doses of human papillomavirus (HPV) vaccine is recommended for adolescent girls and boys at 11 or 12 years of age; however, vaccine uptake remains suboptimal. To understand the reasons why parents may accept or refuse HPV vaccine for their children at age 11 or 12 years, we conducted a qualitative study. Semi-structured interviews were conducted with parents or guardians (n = 45) whose adolescents receive care at an urban, hospital-based primary care practice. Data were analyzed using an iterative thematic approach. We found that many parents expressed high levels of support for HPV vaccine, including a majority who agreed with vaccination at age 11–12 years. Parents recognized that for prevention of consequences of HPV infection, vaccination of their child early in adolescence was desirable conceptually. However, many parents also expressed that in practice, HPV vaccine should be given to adolescents at the onset of sexual activity, a perception that led to preferences to delay administration of HPV vaccine among certain parents. These apparently contradictory views indicate the need for interventions focused on the benefits of vaccination at the recommended ages. Our findings may be useful in providers’ discussions with parents about the vaccine, as pediatric and adolescent health care providers have the unique opportunity to educate parents and clarify misconceptions about vaccination.
Similar content being viewed by others
References
Centers for Disease Control and Prevention (2010) FDA licensure of bivalent human papillomavirus vaccine (HPV2, Cervarix) for use in females and updated HPV vaccination recommendations from the Advisory Committee on Immunization Practices (ACIP). MMWR 59:626–630
Centers for Disease Control and Prevention (CDC) (2011) Recommendations of the use of quadrivalent human papillomavirus vaccine in males—Advisory Committee of Immunization Practices (ACIP), 2011. MMWR 60(50):1705–1708
American Academy of Pediatrics Committee on Infectious Diseases (2012) HPV vaccine recommendations. Pediatrics 129(3):602–605
Winer RL, Feng Q, Hughes JP et al (2008) Risk of female human papillomavirus associated with first male sex partner. JID 197:279–282
Block SL, Nolan T, Sattler C et al (2006) Comparison of the immunogenicity and reactogenicity of a prophylactic quadrivalent human papillomavirus (types 6, 11, 16, and 18) L1 virus-like particle vaccine in male and female adolescents and young adult women. Pediatrics 118(5):2135–2145
Centers for Disease Control and Prevention (2014) National, regional, state, and selected local area vaccination coverage among adolescents aged 13–17 years, United States, 2013. MMWR 63(29):625–633
Centers for Disease Control and Prevention (2014) Human papillomavirus vaccination coverage among adolescents, 2007–2013, and post licensure vaccine safety monitoring, 2006–2014—United States. MMWR 63(29):620–624
Holman DM, Benard V, Roland KB et al (2014) Barriers to human papillomavirus vaccination among US adolescents: a systematic review of the literature. JAMA Pediatr 168(1):76–82
Kessels SJ, Marshall HS, Watson M et al (2012) Factors associated with HPV vaccine uptake in teenage girls: a systematic review. Vaccine 30(24):3546–3556
Vadaparampil ST, Kahn JA, Salmon D (2011) Missed clinical opportunities: provider recommendations for HPV vaccination for 11–12 year old girls are limited. Vaccine 29(47):8634–8641
Daley MF, Crane LA, Markowitz LE et al (2010) Human papillomavirus vaccination practices: a survey of US physicians 18 months after licensure. Pediatrics 126(3):425–433
Hariri S, Markowitz LE, Dunne ED, Unger ER (2013) Population impact of HPV vaccines: summary of early evidence. J Adolesc Health 53:679–682
Niccolai LM, Julian PJ, Bilinski A et al (2013) Area-based poverty, racial, and ethnic disparities in cervical cancer precursor rates in Connecticut, 2008–2009. Am J Public Health 103:156–163
Centers for Disease Control and Prevention (2014) United States Cancer statistics. http://apps.nccd.cdc.gov/uscs/cancersbyraceandethnicity.aspx. Accessed 14 Feb 2014
Jemal A, Simard EP, Dorell C et al (2013) Annual report to the nation on the status of cancer, 1975–2009, featuring the burden and trends in human papillomavirus (HPV)-associated cancers and HPV vaccination coverage levels. J Nat Cancer Inst 105(3):175–201
Clarke V, Braun V (2013) Successful qualitative research: a practical guide for beginners. Sage Publications, Los Angeles
Guest G, MacQueen KM, Namey EE (2012) Applied thematic analysis. Sage Publications, Los Angeles
Hughes CC, Jones AJ, Feemster KA et al (2011) HPV vaccine decision making in pediatric primary care: a semi-structured interview study. BMC Pediatr 11:74
Perkins RB, Clark JA, Apti G et al. Missed opportunities for HPV vaccination in adolescent girls: a qualitative study. [published online ahead of print August 18, 2014]. Pediatrics. doi:10.1542/peds.2014-0442
President’s Cancer Panel Annual Report 2012–2013. 2014. Accelerating HPV vaccine uptake: urgency for action to prevent cancer. http://deainfo.nci.nih.gov/advisory/pcp/annualReports/HPV/index.htm. Accessed 10 Feb 2014
Darden PM, Thompson DM, Roberts JR et al (2013) Reasons for not vaccinating adolescents: national immunization survey of teens, 2008–2010. Pediatrics 131(4):645–651
Dempsey AF, Abraham LM, Dalton V et al (2009) Understanding the reasons why mothers do or do not have their adolescent daughters vaccinated against human papillomavirus. Ann Epidemiol 19(8):531–538
Liddon N, Michael SM, Dittus P et al (2013) Maternal underestimation of child’s sexual experience: suggested implications for HPV vaccine uptake at recommended ages. J Adolesc Health 53(5):674–676
Kornfeld J, Byrne MM, Vanderpool R et al (2013) HPV knowledge and vaccine acceptability among Hispanic fathers. J Prim Prev 34:59–69
Acknowledgments
This work was supported by National Institutes of Health grants R21 CA163160, P30 MH062294, T32 AI007210, and CTSA grants UL1 TR000142 and KL2 TR000140 from the National Center for Research Resources (NCRR) and the National Center for Advancing Translational Science (NCATS), components of the National Institutes of Health (NIH), and NIH Roadmap for Medical Research. The funders had no role in the design, implementation, or interpretation of this work. Its contents are solely the responsibility of the authors and do not necessarily represent the official view of NIH.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hansen, C.E., Credle, M., Shapiro, E.D. et al. “It All Depends”: A Qualitative Study of Parents’ Views of Human Papillomavirus Vaccine for their Adolescents at Ages 11–12 years. J Canc Educ 31, 147–152 (2016). https://doi.org/10.1007/s13187-014-0788-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13187-014-0788-6