Abstract
Introduction
The acute phase of the COVID-19 pandemic impacted the sexual function and mental health of healthcare workers worldwide. However, the extent to which sexual health, including its relational dimension, was affected among different healthcare services and the protective coping strategies employed at that time is currently unclear. The present study aimed to investigate these two issues, exploring for the first time the role of meaning-centered coping on sexual health.
Method
The sample consisted of 109 healthcare workers divided into two groups: a high-exposure group (Intensive Care Unit service, 63 participants) and a low-exposure group (gynecology, obstetrics, and pediatrics services, 46 participants). One year after the onset of the COVID-19 pandemic, participants completed an online survey comprised of sociodemographic and COVID-19 exposure variables, the Depression Anxiety and Stress Scale, the New Sexual Satisfaction Scale-Short Form, and the Meaning-Centered Coping Scale.
Results
(1) High-exposure participants reported more anxiety and depressive symptoms, (2) anxiety, depression and stress were associated with decreased sexual health after the pandemic, (3) High-exposure participants reported a higher decrease in their sexual health, (4) High-exposure workers reported higher levels of meaning-centered coping, and (5) higher levels of meaning-centered coping predicted higher sexual health in both groups.
Policy Implications
Various healthcare services pose distinct risks regarding the detrimental effects of collective health crises on mental and sexual health, and therefore they should be differently treated. The promotion of meaning-centered coping is a sensible policy to improve preparedness in healthcare contexts, especially in vulnerable services and subpopulations.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The COVID-19 pandemic subjected most of the world’s population to national confinements, health risks, social isolation, and economic decline. This has had a considerable impact on multiple markers of physical and mental health (Cullen et al., 2020; Luo et al., 2020; Serafini et al., 2020; Sher, 2020; Carreno et al., 2021; Eisenbeck et al., 2021, 2022). One of the important aspects of overall well-being is the sexual health of the individual as it is closely related to several parameters of quality of life (Flynn & Gow, 2015; Wright & Jenks, 2016; Ford et al., 2019; Smith et al., 2019, 2020; Jackson et al., 2020), including psychological distress (Dèttore et al., 2013; Montesi et al., 2013; Kalmbach & Pillai, 2014; Leavitt & Willoughby, 2015; Rokach, 2019). The COVID-19 pandemic not only increased stress, anxiety and depression levels (e.g., Sher, 2020) that can directly affect sexual health. It also involved fear of transmission and involuntary social restrictions (like social distancing, home confinement and quarantine), which affected the sexual life of many people (Patrì et al., 2020; Pennanen-Iire et al., 2021) because of its relational nature.
A distinction between sexual functions and sexual health must be noticed. Sexual functions refer to performance in different stages of the sexual response cycle, like sexual desire, erection, orgasm and ejaculation (Rosen et al., 1997, 1999, 2000). Instead, sexual health is a more comprehensive construct that includes a subjective general evaluation of sexual life highlighting its relational dimension (Heiman & LoPicccolo, 1988; Schnarch, 1991; Lawrance & Byers, 1995; Byers et al., 1998; Sprecher, 1998; Ellison, 2001; Bancroft et al., 2003; Byers, 2005; Carpenter et al., 2009; Strizzi et al., 2016). Regarding sexual functions, there is recent evidence showing that they have been affected by the COVID-19 pandemic in the general population. For instance, a recent meta-analysis of 21 studies concluded that COVID-19 related restrictions were associated with higher rates of sexual dysfunction and reduced sexual activity (Masoudi et al., 2022). Another study by Ballester-Arnal et al. (2021) employing a big sample of the general population in Spain found that approximately half of the participants reported that their general sexual health was not affected, while 37.9% and 14.4% reported that it was affected negatively and positively, respectively. Other studies conducted on Spanish women showed that the frequency of sexual activities decreased (Leon-Larios et al., 2022), especially in heterosexual women (Ballester-Arnal et al., 2023). Similarly to the heterogeneous results of the Spanish populations, a study (Panzeri et al., 2020) conducted in Italy showed that, after the onset of the pandemic, 12.1% of men and of 18.7% women saw their sexual desire increased, 18.2% of men and 26.4% of women saw it decreased, while the rest did not notice any change. Sexual arousal and reaching orgasms followed the same trend in this study. In contrast, Coombe et al. (2021) found that the general population in Australia experienced a decline in the sexual activity of 53.5%. In this vein, recent meta-analyses have concluded that both sexual functions and sexual satisfaction of the populations of multiple countries were negatively affected by the pandemic (Qaderi et al., 2023), as well as global sexual health (Jacob et al., 2020; Eleuteri & Terzitta, 2021; Toldam et al., 2022).
Sexual and Mental Health in Healthcare Workers
One of the established potential risk factors for decreased mental health during a health crisis is being a healthcare worker, as evidenced in the previous SARS 2003 epidemic (Maunder, 2003, 2004; Maunder et al., 2004, 2006, 2008; Nickell et al., 2004; Sim & Chua, 2004; Lancee et al., 2008; Thomas & Wai, 2010) and the SARS-COV-2 pandemic (Almaghrabi et al., 2020; Azoulay et al., 2020; Canestrari et al., 2021; Giusti et al., 2020; Lai et al., 2020; Luan et al., 2020; Martínez-López et al., 2020; Pappa et al., 2020; Raudenská et al., 2020, Wang et al., 2020; Wańkowicz et al., 2020; Yıldırım et al., 2020; Lenzo et al., 2021; Yang et al., 2021; Blasco-Belled et al., 2022; Chen et al., 2022; Chutiyami et al., 2022; Shekhar et al., 2022; Daniali et al., 2023).
As for the impact on the sexual health of healthcare workers, only a few studies have been published so far. Two of them (Culha et al., 2021; Güzel & Döndü, 2022) analyzed a sample of healthcare workers in Turkey, finding that the overall sexual desire of the participants was low during the COVID-19 pandemic. Also in Turkey, it was determined that sexual function was negatively affected in both male and female healthcare workers (Eroglu et al., 2022). In Brazil the pandemic led to 37% lower libido and 44.5% lower satisfaction in healthcare workers (Neto et al., 2021), and to decreased sexual function in female doctors (de Souza Ziegler et al., 2023). It has also been shown that the pandemic disrupted Iranian-specific cultural attitudes towards sex (Mohammadkhah et al., 2023).
Despite these findings, there are few data on the characteristics of healthcare workers that are at greater risk of developing psychological and sexual problems. In general, working in an intensive care unit (ICU) is considered a risk factor for anxiety, depression, burnout, distress and PTSD (Greenberg et al., 2021; Wozniak et al., 2021; Hall et al., 2022) but research is lacking on how it affects sexual health. Also, the studies above have mostly employed scales focused on sexual function (e.g. arousal, erections, lubrication, pain, and personal satisfaction), with a lesser focus on the relational aspects of sex; see Abdo, 2007; Rosen et al., 1997; Abdo, 2009; Rosen et al., 2000). Because sexual functions are just a part of overall sexual health (which includes, for instance, relational aspects of sex and being satisfied with one’s sexual life), it is also important to assess sexual health more broadly and comprehensively with a scale devoted to this purpose. For example, it has been argued and shown that the relational aspect of sex contributes to sexual satisfaction (Heiman & LoPicccolo, 1988; Schnarch, 1991; Lawrance & Byers, 1995; Byers et al., 1998; Sprecher, 1998; Ellison, 2001; Bancroft et al., 2003; Byers, 2005; Carpenter et al., 2009; Strizzi et al., 2016).
Taking into account the above-mentioned considerations, the first main aim of this study was to identify the mental and sexual health of healthcare workers as a function of the characteristics of their work related to the exposure of the COVID-19 (working in ICU or not). Findings of this nature could aid in discerning the distinct psychological needs of each healthcare service during health crises like the COVID-19 pandemic. This understanding can inform the development of targeted policies for each group, thereby enhancing effectiveness and optimizing resource utilization.
Meaning-Centered Coping and Health Outcomes
Beyond analyzing the vulnerabilities of healthcare workers, it is also relevant to identify protective factors, such as the coping strategies adopted by people during this crisis that may prevent a deterioration of mental and sexual health. For instance, problem-focused strategies (e.g., Cai et al., 2020; Gerhold, 2020) and emotion-focused strategies (e.g., Huang et al., 2020; Man et al., 2020; Savitsky et al., 2020; Rosa-Alcázar et al., 2021) have been associated with mental health in the context of the COVID-19 pandemic. However, one emerging topic in the coping literature is the importance of maintaining and cultivating meaning in life during hardship. Meaning in life, as a general construct, has been related to well-being, lower psychological distress and aid with psychopathological symptoms (Nakamura & Csikzentmihalyi, 2003; Feldman & Snyder, 2005; Schueller & Seligman, 2010; Kleiman et al., 2013; Maddi, 2013; Van Tongeren et al., 2016; Klein, 2017; Carreno & Pérez-Escobar, 2019; Jans-Beken & Wong, 2021).
In this vein, a novel meaning-centered coping style has been recently proposed by Eisenbeck et al. (2022). This coping style is based on existential positive psychology and the self-transcendental notion of meaning in life (see Frankl, 1969, 1985; Wong, 1993, 2020a, b; Wong et al., 2006). It involves a set of cognitive, emotional, and behavioral strategies aimed to promote and sustain meaning in life, especially in adversity. Among these strategies are positive reframing, existential courage, maintenance of hope, life appreciation, interpersonal closeness, prosociality, and engagement in meaningful activities (Eisenbeck et al., 2022). Meaning-centered coping has emerged as a significant protective factor against the effects of the pandemic on stress, anxiety, and depression in people from 30 countries (Eisenbeck et al., 2021). Furthermore, during the first months of the COVID-19 pandemic, meaning-centered coping has been shown to be a better predictor of mental and physical health than other traditional coping strategies such as problem-focused and emotion-focused coping mechanisms (Eisenbeck et al., 2022; see also Avsec et al., 2022).
However, no study has explored the relationship between meaning-centered coping and sexual health yet. In fact, there is also a lack of studies analyzing the relationship between meaning in life and sexual health in general. The only study in this line has been carried out by Kashdan et al. (2018). These authors found that sexual activity predicts increased global meaning in life in the following days, but not the other way around. Thus, the second main purpose of the current study was to gain additional knowledge on the relationship between sexual health and meaning-centered coping. Insights in this direction could help to orientate policies and interventions that prevent a deterioration of sexual health, which is an important component of quality of life, during stressful situations.
While empirical evidence supporting our hypothesis is currently lacking, we posit that meaning-centered coping may bolster sexual health through at least two plausible mechanisms. Firstly, meaning-centered coping has a positive influence on mental and physical health (Eisenbeck et al., 2021, 2022), factors known to exert a direct influence on sexual health (Dèttore et al., 2013; Montesi et al., 2013; Kalmbach & Pillai, 2014; Leavitt & Willoughby, 2015; Rokach, 2019). Secondly, meaning-centered coping and sexual health share a relational dimension. Strategies involved in meaning-centered coping such as fostering interpersonal closeness and engaging in prosocial behavior may enhance the quality of relationships among partners and, consequently, their sexual life.
The Present Study
Based on the aforementioned considerations, the present study aimed to investigate how the COVID-19 outbreak affected the levels of distress and sexual health (broadly understood, including its relational aspect) of different types of healthcare workers. Additionally, the association of meaning-centered coping with sexual health was examined for the first time in the literature. The study featured two groups: ICU workers as a high-exposure group (HE) and healthcare workers in other departments (gynecology, obstetrics and pediatrics services) as a low-exposure group (LE). Measures of pandemic exposure, psychological distress (depression, anxiety and stress), sexual health (including a retrospective version) and meaning-centered coping were administered. The following hypotheses were tested:
Hypothesis 1
The HE group would suffer from higher levels of distress including stress, anxiety and depression compared to the LE group.
Hypothesis 2
Anxiety, depression and stress levels would correlate with steeper perceived decreases in sexual health and lower sexual health after the pandemic in both groups.
Hypothesis 3
The HE group would show a perceived decrease of their sexual health compared to the LE group.
Hypothesis 4
The HE group, as ICU workers typically exposed to emergency situations, would employ higher levels of meaning-centered coping to face adversity as compared to the LE group.
Hypothesis 5
Meaning-centered coping would show a significant positive association with sexual health, being a protective factor against a decline in sexual health.
Method
Participants
Participants were recruited at a large state hospital in Almeria, Spain. The inclusion criterion was to be healthcare personnel in the intensive care unit (ICU), gynecology and obstetrics, or pediatrics services of the Torrecardenas University Hospital in Almeria, Spain. The ICU staff comprised the high exposure group (HE; high burden of care with respect to COVID-19, high exposure to the pandemic), while the gynecology, obstetrics and pediatrics staff comprised the low exposure group (LE; low burden of care with respect to COVID-19, low exposure to the pandemic). All physicians, nurses and nursing assistants from the three departments who volunteered to participate were included in the study, yielding 63 participants in the first service (HE group) and 46 in the other two services (LE group). For sociodemographic data of the sample, see Table 1.
Measures
Sociodemographic and Pandemic Exposure Data
To gather general sociodemographic and pandemic exposure data, we inquired about age, sex, sexual orientation, suffering or not from a disease, professional category (medical doctor, nurse, assistant), having or not an intimate partner and duration of the relationship, living together with an intimate partner, living together with someone else, living together with a specially vulnerable person, having or not tested positive for COVID-19, last time that they took a COVID-19 test, last time that they worried about exposition to the virus, having lacked personal protective equipment at work, feeling avoided by other people due to their job, fear to spread the virus to close people due to working with infected people, and having been subjected to self-isolation at home.
Depression, Anxiety and Stress
The Depression Anxiety and Stress Scale 21 in Spanish (DASS-21; Daza et al., 2002) was used to measure depression, anxiety and stress. It consists of 21 items, seven for each subscale, the values of which range from 0 (did not apply to me) to 3 (applied to me very much, or most of the time). Higher scores in each subscale indicate higher levels of depression, anxiety and stress.
Sexual Health
Sexual health was measured with the New Sexual Satisfaction Scale-Short Form (NSSS-S) in Spanish (Strizzi et al., 2016). The theoretical foundation of the scale is the comprehensive “three windows” approach (Bancroft et al., 2003), which encompasses (1) personal habits, perceptions and feelings, (2) emotional closeness between partners, and (3) sexual activities. This instrument emphasizes social and relational aspects of sex and evaluates sexual satisfaction globally (Štulhofer et al., 2010). It contains 12 items with five answer options. The score for each option ranged from 1 (not satisfied at all) to 5 (extremely satisfied). This is the only scale for which participants were asked to answer the questions retrospectively (before the pandemic) and presently. The differences between present and past scores were used as a measure of perceived change in sexual health during the pandemic.
Meaning-Centered Coping
The levels of meaning coping were measured with the Spanish version of the Meaning-Centered Coping Scale (MCCS; Eisenbeck et al., 2022). It features nine items that comprise different elements of meaning-centered coping such as positive reframing, hope, existential courage, life appreciation, interpersonal closeness, meaningful activities and prosociality. Each item is rated with a maximum of seven points (I completely agree) and a minimum of 1 (I do not agree at all).
Procedure
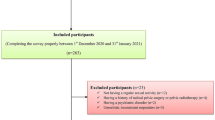
This cross-sectional study was carried out in the ICU, gynecology and obstetrics, and pediatrics services of a university hospital. A link to a form in the Google online office suite was used to fill in the questionnaires. This link was periodically announced in the relevant management Whatsapp groups of each service and professional category by the managers and the researchers. The participants gave their consent to participate without revealing personal data that would lead to their identification at any time, and the data were treated confidentially and exclusively for research purposes. Data were collected between 02/26/2021 and 05/21/2021. No incentives were given to the participants. The only exclusion criterion was not being actively and regularly working at the time of filling out the questionnaire, since this would have prevented the working conditions of the healthcare service in question to be reflected in their mental and sexual health.
Data Analysis
Data were analyzed with SPSS (Version 26). Outliers were identified following the outlier labelling rule of 1.5 (Tukey, 1977). One participant was removed from the study because it was labelled as an outlier according to this rule. Then, data were tested for normality, and a suitable analysis followed accordingly.
Sociodemographic data, pandemic exposure, depression, anxiety and stress levels and meaning-centered coping were compared between the two groups. Due to non-normality of the data, continuous variables were analyzed using Mann–Whitney U and η2 tests, while categorical variables were assessed with Pearson’s chi-squared and Cramer’s V tests (Tables 1, 2 and 3). Spearman’s two-tailed correlation analysis was used to test the correlations between sexual health after COVID-19 and decrease in sexual health, and anxiety, depression and stress levels (Table 4). Finally, to test the relationship between sexual health, group, and meaning-centered coping, a mixed ANOVA was performed: the effect of time between pre and post-pandemic on sexual health was the within-subjects factor and the group (HE or LE) was the between-subjects factor. Professional category (nurse, physician or nursing assistant, as there were differences between the two groups) and MCCS were added covariates (Tables 5 and 6) to test their unique contribution on the dependent variable (sexual health). Mixed ANOVA, involving repeated measures, is adequate for this data because it is robust to non-normality (Berkovits et al., 2000).
Ethics Statement
This study was approved by the bioethics committee of the Torrecardenas University Hospital in Almeria, Spain (code: TFM-ASSC-2021). As this was a questionnaire-based study, the participants were not exposed to any risk. Both the Declaration of Helsinki (seventh and last revision, 2013) regarding ethical aspects of human research, as well as the Omnibus Law of 2009 and its adaptation of 2018 to the Spanish context with respect to personal data protection were respected.
Results
Sociodemographic Data
The two groups did not significantly differ in eight of the nine parameters, including the age and gender of participants, whether they were vulnerable or suffered from a physical or mental pathology and whether they lived with an intimate partner. The exception was professional category (see Table 1).
Pandemic Exposure
Participants of the HE group reported feeling more isolated and avoided by others, took tests more recently, worried about becoming infected more recently, and more of them had tested positive for COVID-19 at some point than respondents in the LE group. There were no significant differences between the two groups regarding the recency of their last positive test, having been subjected to self-isolation at home or being afraid of infecting others. The two groups differed in the perceived lack of personal protective equipment: more participants in the HE group reported lack of equipment “always” and “never”, while more participants of the LE group reported a lack of equipment “only at the onset of the pandemic” and “never, I do not work with COVID-19 patients” (see Table 2).
Group Comparisons
The HE group reported higher total values of depression, anxiety and stress. Furthermore, the independent analysis of each subscale showed that the HE group reported higher depression and anxiety levels, but not significantly different stress levels. The HE group reported higher levels of meaning-centered coping (see Table 3).
Depression, stress and anxiety levels correlated negatively with sexual health after the onset of the COVID-19 pandemic, and positively with the decrease of sexual health from before to after the onset of the pandemic.
Perceived Change in Sexual Health and the Role of Meaning-Centered Coping
To evaluate the perceived impact of the pandemic on the sexual health of the two groups, a mixed ANOVA was performed. The results indicated a significant interaction between group membership and sexual health (see Table 5; Fig. 1): participants in the HE group reported a significantly steeper decrease in their post-pandemic sexual health than those in the LE group.
The model showed no interactions for meaning-centered coping and professional category, that is, the effect of these variables did not depend on the group (see Table 5). The analysis also indicated significant between-subjects effects of MCCS but not of professional category (Table 6). This means that meaning-centered coping was a predictor of sexual health among participants, independently of the time of assessment (pre or post) or group membership (HE or LE).
Discussion
The purpose of this study was to evaluate the levels of distress and sexual health of different healthcare workers during the COVID-19 outbreak. Additionally, the potential protective role of meaning-centered coping on sexual health was explored. Five hypotheses were tested for this study.
As expected, this study confirmed that ICU workers were more exposed to the effects of the COVID-19 pandemic than other healthcare workers. This was the case in most of the exposure parameters that we explored, namely feeling isolated and avoided by others, lacking personal protective equipment, time since last COVID-19 test, time since last worry about becoming infected, and having ever tested positive. These findings complement other works which claim that ICU workers are especially vulnerable staff in hospitals (Greenberg et al., 2021; Wozniak et al., 2021; Hall et al., 2022). It also raises the need for further studies aiming to assess the impact of pandemics and other types of difficulties than those traditionally assessed in healthcare workers, individually considering different healthcare services.
The data also showed that the high exposure group exhibited higher levels of depression, anxiety and general distress, confirming Hypothesis 1. However, stress was similar in both groups. Previous research has shown that the COVID-19 pandemic increased the stress, anxiety and depression of the general population (e.g., Eisenbeck et al., 2021; Eisenbeck et al., 2022) and healthcare workers (e.g., Lenzo et al., 2021; Yang et al., 2021; Shekhar et al., 2022), but differences among types of healthcare workers have not been studied before. A possible explanation is that ICU workers may be adapted to work under stressful conditions, including the COVID-19 pandemic, since the data were gathered one year after the onset of the pandemic. Healthcare workers in general (Juvet et al., 2021), COVID-19 ward healthcare workers (Irandoost et al., 2022) and ICU staff in particular (Holmberg et al., 2020; Yin et al., 2022) are known to have developed psychological and other types of adaptations during the COVID-19 pandemic. Yet, stress can lead to longer lasting neuroadaptations leading to anxiety and depression (e.g., Pizzagalli, 2016; Kovner, Olen & Kalin, 2019), which persist even in the absence of stress.
In line with Hypothesis 2, the data showed that anxiety, depression and stress levels were related to steeper perceived decreases in sexual health and lower sexual health after the pandemic in the whole sample. This is in line with previous literature showing that anxiety, depression and stress impair sexual health (Dèttore et al., 2013; Montesi et al., 2013; Kalmbach & Pillai, 2014; Leavitt & Willoughby, 2015; Rokach, 2019). Interestingly, the distress factor most associated with lower levels and steeper decreases of sexual health was depression. This can be due to the fact that a key depressive symptom is anhedonia, which prevents enjoying sex, leading to high comorbidity between depression and low sexual health (Field et al., 2016). In this line, it has been argued that depression affects sexual health mainly via decreased libido (Kennedy & Rizvi, 2009).
The results additionally indicated that the high exposure group suffered from a steeper perceived decrease in sexual health due to the COVID-19 pandemic (Hypothesis 3). There are several possible interpretations as for why this is the case. One possible scenario is that fear of spreading the virus to their partners interfered with sexual activity, but this specific parameter did not reach statistical significance compared to low exposure healthcare workers in our study, and there is no other literature assessing differences among types of healthcare workers in this regard. Another possibility is that ICU workers, who often dealt with severe cases of COVID-19 and the death of patients, developed an increased awareness, thus changing relationship habits (Güzel & Döndü, 2022) or acquiring vicarious trauma (Suo et al., 2022) that interfered with sexual activity. A third potential cause is that anxiety and depression impacted sexual health negatively (Dèttore et al., 2013; Montesi et al., 2013; Kalmbach & Pillai, 2014).
Interestingly, ICU workers showed higher levels of meaning-centered coping (Hypothesis 4). It is likely that this is the result of adaptations to the higher exposition to death and trauma that ICU workers suffer compared to other healthcare workers. Meaning-centered coping is particularly adaptive during hardships (Eisenbeck et al., 2022). ICU workers often see how patients, old and young, suffer from serious ailments and die. They also hear their patient’s regrets in life and see the pain of their patient’s close ones. As a result, ICU workers perhaps tend to cultivate a deeper appreciation for life, value more interpersonal relations, and therefore focus more on meaning in life compared to other healthcare workers. A similar phenomenon has been found in people with cancer (Carreno & Eisenbeck, 2022: Carreno et al., 2023).
Finally, the tested model in this study indicated that meaning-centered coping was a positive predictor of sexual health regardless of the moment (pre- or post-pandemic) and the group (high or low exposure), therefore supporting Hypothesis 5. Both meaning in life (Ryff, 1989, 2014; Ryff et al., 2016; Vos, 2016; Vos & Vitali, 2018) and meaning-centered coping (Eisenbeck et al., 2022) relate to general wellbeing, and according to our results, this includes sexual wellbeing. This is one of the only two studies that aim to characterize the relationship between sexual health and meaning in life. In a longitudinal study, Kashdan et al. (2018) found that sexual activity predicts increased meaning in life in the following days, but not the inverse. However, our study is different in various regards. First, our study is concerned with meaning-centered coping, which involves different strategies like interpersonal closeness and prosociality, instead of a global judgment of life as meaningful. Second, Kashdan et al. (2018) used a sample of college students in their daily life, a population which displays particular sexual behaviors (see Garcia et al., 2012), while our study investigated healthcare workers amidst the difficulties of the COVID-19 pandemic. Third, these authors measured sexual activity and meaning in life in the span of three weeks in three-day blocks, while in our study only two measures were taken, one of them concerning the day of measurement and the other retrospective, these two periods of time being separated by several months.
Overall, the relationship between sexual health and meaning-related aspects remains almost unexplored. Our study opens the door to further characterizations of the relationship between sexual health and meaning-coping strategies. For instance, it may be that sexual activity improves interpersonal closeness (Rubin & Campbell, 2012), which is one of the components of meaning-centered coping, or that higher meaning-centered coping improves closeness among partners, which has been reported to promote sexual satisfaction (Lawrance & Byers, 1995). An alternative interpretation could be that meaning-centered coping may mitigate psychological distress (Eisenbeck et al., 2021) and improve mental wellbeing (Eisenbeck et al., 2022), both recognized factors influencing sexual heath (Dèttore et al., 2013; Montesi et al., 2013; Kalmbach & Pillai, 2014; Flynn & Gow, 2015; Leavitt & Willoughby, 2015; Wright & Jenks, 2016; Ford et al., 2019; Rokach, 2019; Smith et al., 2019, 2020; Jackson et al., 2020). To determine this potential causal link between meaning-centered coping and sexual health, forthcoming longitudinal and experimental studies are needed.
Limitations and Future Lines of Investigation
There are some limitations to this study worth highlighting. First, its cross-sectional character makes it challenging to make finer interpretations. For instance, tracing the evolution of the different parameters would allow the establishment of more precise causal relationships. Despite this, this study sought to palliate this weakness by incorporating a retrospective measurement, a novelty among studies concerned with sexual health during the COVID-19 pandemic. Of note, retrospective self-reports of well-being and health-related quality of life are generally considered valid (e.g., Lawson et al., 2020; Hudson et al., 2022). Second, there are three sampling suboptimalities: the sample is relatively small (we did not predetermine the sample size, but we included as many participants from relevant healthcare services as was possible to us), the two groups are not equivalent as for professional category and there was an overrepresentation of women. To mitigate possible limitations concerning professional category, this variable was included as a covariate in the analysis. Third, there might be a sampling bias. For instance, perhaps people more uninhibited and less prejudiced about sexuality, or those more resilient to stress and therefore more energetic, were more likely take part in the study.
Conclusions and Policy Implications
This study has extended on the rich and important literature on the effects of the COVID-19 pandemic in healthcare workers by showing mainly that (1) ICU workers were more exposed than other healthcare workers to the contingencies of the pandemic, (2) their mental and broadly conceived sexual health were more affected, (3) they developed more meaning-centered coping adaptations, and (4) meaning-centered coping predicted better sexual health. Various healthcare services carry unique risks concerning the adverse impacts of health crises on mental and sexual health, and thus require distinct targeting strategies. This could make policies more effective and the use of resources more efficient. According to the findings of this study, it seems that an increase of meaning-centered coping is part of the natural repertoire of adaptations of ICU workers. Hence, active promotion of meaning-centered coping may be an effective preventive strategy to improve preparedness for future hardships but also to cope with daily work in normal conditions, especially in vulnerable subtypes of healthcare workers. This can be achieved with interventions fostering meaning coping from the perspectives of positive psychology (e.g., Craske et al., 2019; Carr et al., 2021; Hendriks et al., 2020) and especially existential positive psychology (e.g., Wong, 2010, 2012, 2020a).
Data Availability
The data is freely available in the following repository address: http://hdl.handle.net/10835/14338.
Code Availability
Not applicable.
References
Abdo, C. H. (2007). The male sexual quotient: A brief, self-administered questionnaire to assess male sexual satisfaction. The Journal of Sexual Medicine, 4(2), 382–389. https://doi.org/10.1111/j.1743-6109.2006.00414.x.
Abdo, C. H. N. (2009). Quociente sexual feminino: Um questionário brasileiro para avaliara atividade sexual da mulher. Diagnóstico E Tratamento, 14(2), 89–90.
Almaghrabi, R. H., Alfaradi, H., Hebshi, A., W. A., & Albaadani, M. M. (2020). Healthcare workers experience in dealing with coronavirus (COVID-19) pandemic. Saudi Medical Journal, 41(6), 657. https://doi.org/10.15537/smj.2020.6.25101.
Avsec, A., Eisenbeck, N., Carreno, D. F., Kocjan, G. Z., & Kavčič, T. (2022). Coping styles mediate the association between psychological inflexibility and psychological functioning during the COVID-19 pandemic: A crucial role of meaning-centered coping. Journal of Contextual Behavioral Science, 26, 201–209. https://doi.org/10.1016/j.jcbs.2022.10.001.
Azoulay, E., De Waele, J., Ferrer, R., Staudinger, T., Borkowska, M., Povoa, P., & Cecconi, M. (2020). Symptoms of burnout in intensive care unit specialists facing the COVID-19 outbreak. Annals of Intensive care, 10(1), 1–8. https://doi.org/10.1186/s13613-020-00722-3.
Ballester-Arnal, R., Nebot-Garcia, J. E., Ruiz-Palomino, E., Giménez-García, C., & Gil-Llario, M. D. (2021). INSIDE project on sexual health in Spain: Sexual life during the lockdown caused by COVID-19. Sexuality Research and Social Policy, 18(4), 1023–1041. https://doi.org/10.1007/s13178-020-00506-1.
Ballester-Arnal, R., Nebot-Garcia, J. E., Ruiz-Palomino, E., García-Barba, M., Fernández-García, O., & Gil-Llario, M. D. (2023, May). Sexual life of Spanish women during the lockdown by COVID-19: Differences according to sexual orientation? In Women’s Studies International Forum (Vol. 98, p. 102719). Pergamon. https://doi.org/10.1016/j.wsif.2023.102719.
Bancroft, J., Loftus, J., & Long, J. S. (2003). Distress about sex: A national survey of women in heterosexual relationships. Archives of Sexual Behavior, 32(3), 193–208. https://doi.org/10.1023/a:1023420431760.
Berkovits, I., Hancock, G. R., & Nevitt, J. (2000). Bootstrap resampling approaches for repeated measure designs: Relative robustness to sphericity and normality violations. Educational and Psychological Measurement, 60(6), 877–892. https://doi.org/10.1177/00131640021970961.
Blasco-Belled, A., Tejada-Gallardo, C., Fatsini-Prats, M., & Alsinet, C. (2022). Mental health among the general population and healthcare workers during the COVID-19 pandemic: A meta-analysis of well-being and psychological distress prevalence. Current Psychology, 1–12. https://doi.org/10.1007/s12144-022-02913-6.
Byers, E. S. (2005). Relationship satisfaction and sexual satisfaction: A longitudinal study of individuals in long-term relationships. Journal of Sex Research, 42(2), 113–118. https://doi.org/10.1080/00224490509552264.
Byers, E. S., Demmons, S., & Lawrance, K. (1998). Sexual satisfaction within dating relationships: A test of the interpersonal exchange model of sexual satisfaction. Journal of Social and Personal Relationships, 15(2), 257–267. https://doi.org/10.1177/0265407598152008.
Cai, H., Tu, B., Ma, J., Chen, L., Fu, L., Jiang, Y., & Zhuang, Q. (2020). Psychological impact and coping strategies of frontline medical staff in Hunan between January and March 2020 during the outbreak of coronavirus disease 2019 (COVID-19) in Hubei, China. Medical Science Monitor: International Medical Journal of Experimental and Clinical Research, 26, e924171–e924171. https://doi.org/10.12659/msm.924171.
Canestrari, C., Bongelli, R., Fermani, A., Riccioni, I., Bertolazzi, A., Muzi, M., & Burro, R. (2021). Coronavirus disease stress among Italian healthcare workers: The role of coping humor. Frontiers in Psychology, 11, 601574. https://doi.org/10.3389/fpsyg.2020.601574.
Carpenter, L. M., Nathanson, C. A., & Kim, Y. J. (2009). Physical women, emotional men: Gender and sexual satisfaction in midlife. Archives of Sexual Behavior, 38, 87–107. https://doi.org/10.1007/s10508-007-9215-y.
Carr, A., Cullen, K., Keeney, C., Canning, C., Mooney, O., Chinseallaigh, E., & O’Dowd, A. (2021). Effectiveness of positive psychology interventions: A systematic review and meta-analysis. The Journal of Positive Psychology, 16(6), 749–769. https://doi.org/10.1080/17439760.2020.1818807.
Carreno, D. F., & Eisenbeck, N. (2022). Existential insights in Cancer: Meaning in Life Adaptability. Medicina, 58(4), 461. https://doi.org/10.3390/medicina58040461.
Carreno, D. F., Eisenbeck, N., Pérez-Escobar, J. A., & García-Montes, J. M. (2021). Inner harmony as an essential facet of well-being: A multinational study during the COVID-19 pandemic. Frontiers in Psychology, 12, 648280. https://doi.org/10.3389/fpsyg.2021.648280.
Carreno, D. F., Eisenbeck, N., Uclés-Juárez, R., & García-Montes, J. M. (2023). Reapprasing personal values in cancer: Meaning-in-life adaptation, meaningfulness, and quality of life. Psycho-Oncology, 32(12), 1905–1917. https://doi.org/10.1002/pon.6244.
Carreno, D. F., & Pérez-Escobar, J. A. (2019) Addiction in existential positive psychology (EPP PP2.0): from a critique of the brain disease model towards a meaning-centered approach. Counselling Psychology Quarterly, 32(3–4) 415–435. https://doi.org/10.1080/09515070.2019.1604494.
Chen, X., Chen, J., Zhang, M., Dong, R. K., Li, J., Dong, Z., & Zhang, S. X. (2022). Meta-regression on the heterogenous factors contributing to the prevalence of mental health symptoms during the COVID-19 crisis among healthcare workers. Frontiers in Psychiatry, 13, 833865. https://doi.org/10.3389/fpsyt.2022.833865.
Chutiyami, M., Cheong, A. M., Salihu, D., Bello, U. M., Ndwiga, D., Maharaj, R., & Kannan, P. (2022). COVID-19 pandemic and overall mental health of healthcare professionals globally: A meta-review of systematic reviews. Frontiers in Psychiatry, 12, 2600. https://doi.org/10.3389/fpsyt.2021.804525.
Coombe, J., Kong, F. Y. S., Bittleston, H., Williams, H., Tomnay, J., Vaisey, A., & Hocking, J. S. (2021). Love during lockdown: Findings from an online survey examining the impact of COVID-19 on the sexual health of people living in Australia. Sexually Transmitted Infections, 97(5), 357–362. https://doi.org/10.1136/sextrans-2020-054688.
Craske, M. G., Meuret, A. E., Ritz, T., Treanor, M., Dour, H., & Rosenfield, D. (2019). Positive affect treatment for depression and anxiety: A randomized clinical trial for a core feature of anhedonia. Journal of Consulting and Clinical Psychology, 87(5), 457. https://doi.org/10.1037/ccp0000396.
Culha, M. G., Demir, O., Sahin, O., & Altunrende, F. (2021). Sexual attitudes of healthcare professionals during the COVID-19 outbreak. International Journal of Impotence Research, 33(1), 102–109. https://doi.org/10.1038/s41443-020-00381-9.
Cullen, W., Gulati, G., & Kelly, B. D. (2020). Mental health in the COVID-19 pandemic. QJM: An International Journal of Medicine, 113(5), 311–312. https://doi.org/10.1093/qjmed/hcaa110.
Daniali, H., Martinussen, M., & Flaten, M. A. (2023). A global meta-analysis of depression, anxiety, and stress before and during COVID-19. Health Psychology, 42(2), 124–138. https://doi.org/10.1037/hea0001259.
Daza, P., Novy, D. M., Stanley, M. A., & Averill, P. (2002). The depression anxiety stress scale-21: Spanish translation and validation with a hispanic sample. Journal of Psychopathology and Behavioral Assessment, 24(3), 195–205. https://doi.org/10.1023/A:1016014818163.
de Souza Ziegler, N., Muller, G. C., Grossi, F. S., Pacagnella, R. D. C., Hermel, J. S., & Vettorazzi, J. (2023). Impact of the covid-19 pandemic on mental health and sexuality of female doctors. Plos One, 18(7), e0281321. https://doi.org/10.1371/journal.pone.0281321.
Dèttore, D., Pucciarelli, M., & Santarnecchi, E. (2013). Anxiety and female sexual functioning: An empirical study. Journal of Sex & Marital Therapy, 39(3), 216–240. https://doi.org/10.1080/0092623x.2011.606879.
Eisenbeck, N., Carreno, D. F., & Pérez-Escobar, J. A. (2021). Meaning-centered coping in the era of COVID-19: Direct and moderating effects on depression, anxiety, and stress. Frontiers in Psychology, 12, 648383. https://doi.org/10.3389/fpsyg.2021.648383.
Eisenbeck, N., Carreno, D. F., Wong, P. T., Hicks, J. A., María, R. R. G., Puga, J. L., & García-Montes, J. M. (2022). An international study on psychological coping during COVID-19: Towards a meaning-centered coping style. International Journal of Clinical and Health Psychology, 22(1), 100256. https://doi.org/10.1016/j.ijchp.2021.100256.
Eleuteri, S., & Terzitta, G. (2021). Sexuality during the COVID-19 pandemic: The importance of internet. Sexologies, 30(1), e55–e60. https://doi.org/10.1016%2Fj.sexol.2020.12.008.
Ellison, C. R. (2001). Intimacy-based sex therapy: Sexual choreography. In P. J. Kleinplatz (Ed.), New directions in sex therapy: Innovations and alternatives (pp. 163–184). Brunner-Routledge.
Eroglu, U., Balci, M., Coser, S., Basboga, S., Ozercan, A. Y., Kizilkan, Y., & Tuncel, A. (2022). Impact of the COVID-19 pandemic on the psychosexual functions of healthcare workers. The Journal of Sexual Medicine, 19(2), 182–187. https://doi.org/10.1016/j.jsxm.2021.11.013.
Feldman, D. B., & Snyder, C. R. (2005). Hope and the meaningful life: Theoretical and empirical associations between goal–directed thinking and life meaning. Journal of Social and Clinical Psychology, 24(3), 401–421. https://doi.org/10.1521/jscp.24.3.401.65616.
Field, N., Prah, P., Mercer, C. H., Rait, G., King, M., Cassell, J. A., & Sonnenberg, P. (2016). Are depression and poor sexual health neglected comorbidities? Evidence from a population sample. BMJ open, 6(3), e010521. https://doi.org/10.1136/bmjopen-2015-010521.
Flynn, T. J., & Gow, A. J. (2015). Examining associations between sexual behaviours and quality of life in older adults. Age and Ageing, 44(5), 823–828. https://doi.org/10.1093/ageing/afv083.
Ford, J. V., Vargas, C., Finotelli Jr, E., Fortenberry, I., Kismödi, J. D., Philpott, E., & Coleman, A., E (2019). Why pleasure matters: Its global relevance for sexual health, sexual rights and wellbeing. International Journal of Sexual Health, 31(3), 217–230. https://doi.org/10.1080/19317611.2019.1654587.
Frankl, V. E. (1969). The will to meaning: Foundations and applications of Logotherapy. World Publishing Company.
Frankl, V. E. (1985). Man’s search for meaning. Simon and Schuster.
Garcia, J. R., Reiber, C., Massey, S. G., & Merriwether, A. M. (2012). Sexual hookup culture: A review. Review of General Psychology, 16(2), 161–176. https://doi.org/10.1037/a0027911.
Gerhold, L. (2020). COVID-19: Risk perception and coping strategies. PsyArXiv. https://doi.org/10.31234/osf.io/xmpk4.
Giusti, E. M., Pedroli, E., D’Aniello, G. E., Badiale, S., Pietrabissa, C., Manna, G., C., …, & Molinari, E. (2020). The psychological impact of the COVID-19 outbreak on health professionals: A cross-sectional study. Frontiers in Psychology, 11, 1684. https://doi.org/10.3389/fpsyg.2020.01684.
Greenberg, N., Weston, D., Hall, C., Caulfield, T., Williamson, V., & Fong, K. (2021). Mental health of staff working in intensive care during Covid-19. Occupational Medicine, 71(2), 62–67. https://doi.org/10.1093/occmed/kqaa220.
Güzel, A., & Döndü, A. (2022). Changes in sexual functions and habits of healthcare workers during the ongoing COVID-19 outbreak: A cross-sectional survey study. Irish Journal of Medical Science (1971-), 191(3), 1013–1021. https://doi.org/10.1007/s11845-021-02691-3.
Hall, C. E., Milward, J., Spoiala, C., Bhogal, J. K., Weston, D., Potts, H. W., & Greenberg, N. (2022). The mental health of staff working on intensive care units over the COVID-19 winter surge of 2020 in England: A cross sectional survey. British Journal of Anaesthesia, 128(6), 971–979. https://doi.org/10.1016/j.bja.2022.03.016.
Heiman, J., & LoPiccolo, J. (1988). Becoming orgasmic: A sexual and personal growth program for women. Prentice Hall.
Hendriks, T., Schotanus-Dijkstra, M., Hassankhan, A., De Jong, J., & Bohlmeijer, E. (2020). The efficacy of multi-component positive psychology interventions: A systematic review and meta-analysis of randomized controlled trials. Journal of Happiness Studies, 21, 357–390. https://doi.org/10.1007/s10902-019-00082-1.
Holmberg, J., Kemani, M. K., Holmström, L., Öst, L. G., & Wicksell, R. K. (2020). Psychological flexibility and its relationship to distress and work engagement among intensive care medical staff. Frontiers in Psychology, 11, 603986. https://doi.org/10.3389/fpsyg.2020.603986.
Huang, L., Lei, W., Xu, F., Liu, H., & Yu, L. (2020). Emotional responses and coping strategies in nurses and nursing students during Covid-19 outbreak: A comparative study. PloS One, 15(8), e0237303. https://doi.org/10.1371/journal.pone.0237303.
Hudson, N. W., Lucas, R. E., & Donnellan, M. B. (2022). A direct comparison of the temporal stability and criterion validities of experiential and retrospective global measures of subjective well-being. Journal of Research in Personality, 98, 104230. https://doi.org/10.1016/j.jrp.2022.104230.
Irandoost, S. F., Lebni, Y., Safari, J., Khorami, H., Ahmadi, F., Soofizad, S., G., & Azar, E. F., F (2022). Explaining the challenges and adaptation strategies of nurses in caring for patients with COVID-19: A qualitative study in Iran. BMC Nursing, 21(1), 1–16. https://doi.org/10.1186/s12912-022-00937-8.
Jackson, S. E., Yang, L., Koyanagi, A., Stubbs, B., Veronese, N., & Smith, L. (2020). Declines in sexual activity and function predict incident health problems in older adults: Prospective findings from the English longitudinal study of ageing. Archives of Sexual Behavior, 49(3), 929–940. https://doi.org/10.1007/s10508-019-1443-4.
Jacob, L., Smith, L., Butler, L., Barnett, Y., Grabovac, I., McDermott, D., & Tully, M. A. (2020). Challenges in the practice of sexual medicine in the time of COVID-19 in the United Kingdom. The Journal of Sexual Medicine, 17(7), 1229–1236. https://doi.org/10.1016/j.jsxm.2020.05.001.
Jans-Beken, L., & Wong, P. T. (2021). Development and preliminary validation of the Existential Gratitude Scale (EGS). Counselling Psychology Quarterly, 34(1), 72–86. https://doi.org/10.1080/09515070.2019.1656054.
Juvet, T. M., Corbaz-Kurth, S., Roos, P., Benzakour, L., Cereghetti, S., Moullec, G., & Weissbrodt, R. (2021). Adapting to the unexpected: Problematic work situations and resilience strategies in healthcare institutions during the COVID-19 pandemic’s first wave. Safety Science, 139, 105277. https://doi.org/10.1016/j.ssci.2021.105277.
Kalmbach, D. A., & Pillai, V. (2014). Daily affect and female sexual function. The Journal of Sexual Medicine, 11(12), 2938–2954. https://doi.org/10.1111/jsm.12712.
Kashdan, T. B., Goodman, F. R., Stiksma, M., Milius, C. R., & McKnight, P. E. (2018). Sexuality leads to boosts in mood and meaning in life with no evidence for the reverse direction: A daily diary investigation. Emotion, 18(4), 563. https://doi.org/10.1037/emo0000324.
Kennedy, S. H., & Rizvi, S. (2009). Sexual dysfunction, depression, and the impact of antidepressants. Journal of Clinical Psychopharmacology, 29(2), 157–164. https://doi.org/10.1097/jcp.0b013e31819c76e9.
Kleiman, E. M., Adams, L. M., Kashdan, T. B., & Riskind, J. H. (2013). Gratitude and grit indirectly reduce risk of suicidal ideations by enhancing meaning in life: Evidence for a mediated moderation model. Journal of Research in Personality, 47(5), 539–546. https://doi.org/10.1016/j.jrp.2013.04.007.
Klein, N. (2017). Prosocial behavior increases perceptions of meaning in life. The Journal of Positive Psychology, 12(4), 354–361. https://doi.org/10.1080/17439760.2016.1209541.
Kovner, R., Oler, J. A., & Kalin, N. H. (2019). Cortico-limbic interactions mediate adaptive and maladaptive responses relevant to psychopathology. American Journal of Psychiatry, 176(12), 987–999. https://doi.org/10.1176/appi.ajp.2019.19101064.
Lai, J., Ma, S., Wang, Y., Cai, Z., Hu, J., Wei, N., & Hu, S. (2020). Factors associated with mental health outcomes among health care workers exposed to coronavirus disease 2019. JAMA Network open, 3(3), e203976. https://doi.org/10.1001/jamanetworkopen.2020.3976.
Lancee, W. J., Maunder, R. G., & Goldbloom, D. S. (2008). Prevalence of psychiatric disorders among Toronto hospital workers one to two years after the SARS outbreak. Psychiatric Services, 59(1), 91–95. https://doi.org/10.1176/ps.2008.59.1.91.
Lawrance, K., & Byers, E. S. (1995). Sexual satisfaction in long-term heterosexual relationships: The interpersonal exchange model of sexual satisfaction. Personal Relationships, 2, 267–285. https://doi.org/10.1111/j.1475-6811.1995.tb00092.x.
Lawson, A., Tan, A. C., Naylor, J., & Harris, I. A. (2020). Is retrospective assessment of health-related quality of life valid? BMC Musculoskeletal Disorders, 21(1), 1–10. https://doi.org/10.1186/s12891-020-03434-8.
Leavitt, C. E., & Willoughby, B. J. (2015). Associations between attempts at physical intimacy and relational outcomes among cohabiting and married couples. Journal of Social and Personal Relationships, 32(2), 241–262. https://doi.org/10.1177/0265407514529067.
Lenzo, V., Quattropani, M. C., Sardella, A., Martino, G., & Bonanno, G. A. (2021). Depression, anxiety, and stress among healthcare workers during the COVID-19 outbreak and relationships with expressive flexibility and context sensitivity. Frontiers in Psychology, 12, 623033. https://doi.org/10.3389/fpsyg.2021.623033.
Leon-Larios, F., Silva Reus, I., Lahoz Pascual, I., Quílez Conde, J. C., Martínez, P., Gutiérrez, M. J., Ales, J., & Rancel, C., M (2022). Women’s access to sexual and reproductive health services during confinement due to the COVID-19 pandemic in Spain. Journal of Clinical Medicine, 11(14), 4074. https://doi.org/10.3390%2Fjcm11144074.
Luan, R., Pu, W., Dai, L., Yang, R., & Wang, P. (2020). Comparison of psychological stress levels and associated factors among healthcare workers, frontline workers, and the general public during the novel coronavirus pandemic. Frontiers in Psychiatry, 11, 583971. https://doi.org/10.3389/fpsyt.2020.583971.
Luo, M., Guo, L., Yu, M., Jiang, W., & Wang, H. (2020). The psychological and mental impact of coronavirus disease 2019 (COVID-19) on medical staff and general public–A systematic review and meta-analysis. Psychiatry Research, 291, 113190. https://doi.org/10.1016/j.psychres.2020.113190.
Maddi, S. R. (2013). Hardiness as the existential courage to grow through searching for meaning. In J. Hicks & C. Routledge (Eds.), The experience of meaning in life (pp. 227–239). Springer. https://doi.org/10.1007/978-94-007-6527-6_18.
Man, M. A., Toma, C., Motoc, N. S., Necrelescu, O. L., Bondor, C. I., Chis, A. F., & Rajnoveanu, R. M. (2020). Disease perception and coping with emotional distress during COVID-19 pandemic: A survey among medical staff. International Journal of Environmental Research and Public Health, 17(13), 4899. https://doi.org/10.3390/ijerph17134899.
Martínez-López, J. Á., Lázaro-Pérez, C., Gómez-Galán, J., & Fernández-Martínez, M. D. M. (2020). Psychological impact of COVID-19 emergency on health professionals: Burnout incidence at the most critical period in Spain. Journal of Clinical Medicine, 9(9), 3029. https://doi.org/10.3390/jcm9093029.
Masoudi, M., Maasoumi, R., & Bragazzi, N. L. (2022). Effects of the COVID-19 pandemic on sexual functioning and activity: A systematic review and meta-analysis. BMC Public Health, 22(1), 1–18. https://doi.org/10.1186/s12889-021-12390-4.
Maunder, R. (2003). Stress, coping and lessons learned from the SARS outbreak. Hospital Quarterly, 6(4), 49–50. https://doi.org/10.12927/hcq.16480.
Maunder, R. (2004). The experience of the 2003 SARS outbreak as a traumatic stress among frontline healthcare workers in Toronto: Lessons learned. Philosophical Transactions of the Royal Society of London Series B: Biological Sciences, 359(1447), 1117–1125. https://doi.org/10.1098/rstb.2004.1483.
Maunder, R. G., Lancee, W. J., Rourke, S., Hunter, J. J., Goldbloom, D., Balderson, K., & Fones, C. S. (2004). Factors associated with the psychological impact of severe acute respiratory syndrome on nurses and other hospital workers in Toronto. Psychosomatic Medicine, 66(6), 938–942. https://doi.org/10.1097/01.psy.0000145673.84698.18.
Maunder, R. G., Lancee, W. J., Balderson, K. E., Bennett, J. P., Borgundvaag, B., Evans, S., & Wasylenki, D. A. (2006). Long-term psychological and occupational effects of providing hospital healthcare during SARS outbreak. Emerging infectious diseases, 12(12), 1924. https://doi.org/10.3201/eid1212.060584.
Maunder, R. G., Leszcz, M., Savage, D., Adam, M. A., Peladeau, N., Romano, D., & Schulman, R. B. (2008). Applying the lessons of SARS to pandemic influenza. Canadian Journal of Public Health, 99(6), 486–488. https://doi.org/10.1007/bf03403782.
Mohammadkhah, F., Chaboksavar, F., Alhani, F., Mahmoudian, A., Ziapour, A., Sigaroudi, A. E., & Alipour, Z. J. (2023). Lived sexual experience of health workers on the Iranian frontline of the fight against the COVID-19 pandemic: A qualitative content analysis. Heliyon, 9(8). https://doi.org/10.1016/j.heliyon.2023.e18584.
Montesi, J. L., Conner, B. T., Gordon, E. A., Fauber, R. L., Kim, K. H., & Heimberg, R. G. (2013). On the relationship among social anxiety, intimacy, sexual communication, and sexual satisfaction in young couples. Archives of Sexual Behavior, 42(1), 81–91. https://doi.org/10.1007/s10508-012-9929-3.
Nakamura, J., & Csikzentmihalyi, M. (2003). The construction of meaning through vital engagement. In C. L. M. Keyes & J. Haidt (Eds.), Flourishing: Positive Psychology and the Life Well-Lived (pp. 83–104). American Psychological Association Books. https://doi.org/10.1037/10594-004.
Neto, R. P., Nascimento, B. C., dos Anjos Silva, G. C., Barbosa, J. A. B. A., de Bessa Júnior, J., Teixeira, T. A., & Cury, J. (2021). Impact of COVID-19 pandemic on the sexual function of health professionals from an epicenter in Brazil. Sexual Medicine, 9(5), 100408. https://doi.org/10.1016/j.esxm.2021.100408.
Nickell, L. A., Crighton, E. J., Tracy, C. S., Al-Enazy, H., Bolaji, Y., Hanjrah, S., & Upshur, R. E. (2004). Psychosocial effects of SARS on hospital staff: Survey of a large tertiary care institution. Cmaj, 170(5), 793–798. https://doi.org/10.1503%2Fcmaj.1031077.
Panzeri, M., Ferrucci, R., Cozza, A., & Fontanesi, L. (2020). Changes in sexuality and quality of couple relationship during the COVID-19 lockdown. Frontiers in Psychology, 11, 565823. https://doi.org/10.3389/fpsyg.2020.565823.
Pappa, S., Ntella, V., Giannakas, T., Giannakoulis, V. G., Papoutsi, E., & Katsaounou, P. (2020). Prevalence of depression, anxiety, and insomnia among healthcare workers during the COVID-19 pandemic: A systematic review and meta-analysis. Brain Behavior and Immunity, 88, 901–907. https://doi.org/10.1016/j.bbi.2020.05.026.
Patrì, A., Gallo, L., Guarino, M., & Fabbrocini, G. (2020). Sexual transmission of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2): A new possible route of infection? Journal of the American Academy of Dermatology, 82(6), e227. https://doi.org/10.1016%2Fj.jaad.2020.03.098.
Pennanen-Iire, C., Prereira-Lourenço, M., Padoa, A., Ribeirinho, A., Samico, A., Gressler, M., Jatoi, N. A., Mehrad, M., & Girard, A. (2021). Sexual Health implications of COVID-19 pandemic. Sexual Medicine Reviews, 9(1), 3–14. https://doi.org/10.1016/j.sxmr.2020.10.004.
Pizzagalli, D. A. (2016). Psychobiology of the intersection and divergence of depression and anxiety. Depression and Anxiety, 33(10), 891. https://doi.org/10.1002%2Fda.22550.
Qaderi, K., Yazdkhasti, M., Zangeneh, S., Behbahani, B. M., Kalhor, M., Shamsabadi, A., & Rasoal, D. (2023). Changes in sexual activities, function, and satisfaction during the COVID-19 pandemic era: A systematic review and meta-analysis. Sexual Medicine, 11(2), qfad005. https://doi.org/10.1093/sexmed/qfad005.
Raudenská, J., Steinerová, V., Javůrková, A., Urits, I., Kaye, A. D., Viswanath, O., & Varrassi, G. (2020). Occupational burnout syndrome and post-traumatic stress among healthcare professionals during the novel coronavirus disease 2019 (COVID-19) pandemic. Best Practice & Research Clinical Anaesthesiology, 34(3), 553–560. https://doi.org/10.1016/j.bpa.2020.07.008.
Rokach, A. (2019). The psychological journey to and from loneliness: Development, causes, and effects of social and emotional isolation. Academic Press. https://doi.org/10.1016/C2017-0-03510-3.
Rosa-Alcázar, Á., García-Hernández, M. D., Parada-Navas, J. L., Olivares-Olivares, P. J., Martínez-Murillo, S., & Rosa-Alcázar, A. I. (2021). Coping strategies in obsessive-compulsive patients during Covid-19 lockdown. International Journal of Clinical and Health Psychology, 21(2), 100223. https://doi.org/10.1016/j.ijchp.2021.100223.
Rosen, R. C., Riley, A., Wagner, G., Osterloh, I. H., Kirkpatrick, J., & Mishra, A. (1997). The international index of erectile function (IIEF): A multidimensional scale for assessment of erectile dysfunction. Urology, 49(6), 822–830. https://doi.org/10.1016/s0090-4295(97)00238-0.
Rosen, R. C., Cappelleri, J. C., Smith, M. D., Lipsky, J., & Pena, B. M. (1999). Development and evaluation of an abridged, 5-item version of the International Index of Erectile function (IIEF-5) as a diagnostic tool for erectile dysfunction. International Journal of Impotence Research, 11(6), 319–326. https://doi.org/10.1038/sj.ijir.3900472.
Rosen, R. C., Brown, C., Heiman, J., Leiblum, S., Meston, C. M., Shabsigh, R., Ferguson, D., & D’Agostino, R. (2000). The female sexual function index (FSFI): A multidimensional self-report instrument for the assessment of female sexual function. Journal of Sex & Marital Therapy, 26(2), 191–208. https://doi.org/10.1080/009262300278597.
Rubin, H., & Campbell, L. (2012). Day-to-day changes in intimacy predict heightened relationship passion, sexual occurrence, and sexual satisfaction: A dyadic diary analysis. Social Psychological and Personality Science, 3(2), 224–231. https://doi.org/10.1177/194855061141652.
Ryff, C. D. (1989). Happiness is everything, or is it? Explorations on the meaning of psychological well-being. Journal of Personality and Social Psychology, 57(6), 1069–1081. https://doi.org/10.1037/0022-3514.57.6.1069.
Ryff, C. D. (2014). Psychological well-being revisited: Advances in the science and practice of eudaimonia. Psychotherapy and Psychosomatics, 83(1), 10–28. https://doi.org/10.1159/000353263.
Ryff, C. D., Heller, A. S., Schaefer, S. M., Van Reekum, C., & Davidson, R. J. (2016). Purposeful engagement, healthy aging, and the brain. Current Behavioral Neuroscience Reports, 3(4), 318–327. https://doi.org/10.1007/s40473-016-0096-z.
Savitsky, B., Findling, Y., Ereli, A., & Hendel, T. (2020). Anxiety and coping strategies among nursing students during the covid-19 pandemic. Nurse Education in Practice, 46, 102809. https://doi.org/10.1016/j.nepr.2020.102809.
Schnarch, D. (1991). Constructing the sexual crucible: An integration of sexual and marital therapy. W.W. Norton and Company.
Schueller, S. M., & Seligman, M. E. (2010). Pursuit of pleasure, engagement, and meaning: Relationships to subjective and objective measures of well-being. The Journal of Positive Psychology, 5(4), 253–263. https://doi.org/10.1080/17439761003794130.
Serafini, G., Parmigiani, B., Amerio, A., Aguglia, A., Sher, L., & Amore, M. (2020). The psychological impact of COVID-19 on the mental health in the general population. Qjm, 113(8), 531–537. https://doi.org/10.1093/qjmed/hcaa201.
Shekhar, S., Ahmad, S., Ranjan, A., Pandey, S., Ayub, A., & Kumar, P. (2022). Assessment of depression, anxiety and stress experienced by health care and allied workers involved in SARS-CoV2 pandemic. Journal of Family Medicine and Primary Care, 11(2), 466–471. https://doi.org/10.4103/jfmpc.jfmpc_2518_20.
Sher, L. (2020). The impact of the COVID-19 pandemic on suicide rates. QJM: An International Journal of Medicine, 113(10), 707–712. https://doi.org/10.1093/qjmed/hcaa202.
Sim, K., & Chua, H. C. (2004). The psychological impact of SARS: A matter of heart and mind. Cmaj, 170(5), 811–812. https://doi.org/10.1503%2Fcmaj.1032003.
Smith, L., Yang, L., Veronese, N., Soysal, P., Stubbs, B., & Jackson, S. E. (2019). Sexual activity is associated with greater enjoyment of life in older adults. Sexual Medicine, 7(1), 11–18. https://doi.org/10.1016/j.esxm.2018.11.001.
Smith, L., Grabovac, I., Yang, L., López-Sánchez, G. F., Firth, J., Pizzol, D., & Jackson, S. E. (2020). Sexual activity and cognitive decline in older age: A prospective cohort study. Aging Clinical and Experimental Research, 32(1), 85–91. https://doi.org/10.1007/s40520-019-01334-z.
Sprecher, S. (1998). Social exchange theories and sexuality. Journal of Sex Research, 35(1), 32–43. https://doi.org/10.1080/00224499809551915.
Strizzi, J., Fernández-Agis, I., Alarcón-Rodríguez, R., & Parrón-Carreño, T. (2016). Adaptation of the new sexual satisfaction scale-short form into Spanish. Journal of sex & Marital Therapy, 42(7), 579–588. https://doi.org/10.1080/0092623x.2015.1113580.
Štulhofer, A., Buško, V., & Brouillard, P. (2010). Development and bicultural validation of the new sexual satisfaction scale. Journal of sex Research, 47(4), 257–268. https://doi.org/10.1080/00224490903100561.
Suo, X., Zuo, C., Lan, H., Pan, N., Zhang, X., Kemp, G. J., & Gong, Q. (2022). COVID-19 vicarious traumatization links functional connectome to general distress. Neuroimage, 255, 119185. https://doi.org/10.1016/j.neuroimage.2022.119185.
Thomas, S. T. L., & Wai, C. Y. (2010). The lessons of SARS in Hong Kong. Clinical Medicine, 10(1), 50–53. https://doi.org/10.7861/clinmedicine.10-1-50.
Toldam, N. E., Graugaard, C., Meyer, R., Thomsen, L., Dreier, S., Jannini, E. A., & Giraldi, A. (2022). Sexual health during COVID-19: A scoping review. Sexual Medicine Reviews, 10(4), 714–753. https://doi.org/10.1016/j.sxmr.2022.06.005.
Tukey, J. W. (1977). Exploratory data analysis. Addison-Wesley.
Van Tongeren, D. R., Green, J. D., Davis, D. E., Hook, J. N., & Hulsey, T. L. (2016). Prosociality enhances meaning in life. The Journal of Positive Psychology, 11(3), 225–236. https://doi.org/10.1080/17439760.2015.1048814.
Vos, J. (2016). Working with meaning in life in mental health care: A systematic literature review of the practices and effectiveness of meaning-centred therapies. In P. Russo-Netzer, S. E. Schulenberg & A. Batthyany (Eds.), Clinical Perspectives on Meaning (pp. 59–87). Springer. https://doi.org/10.1007/978-3-319-41397-6_4.
Vos, J., & Vitali, D. (2018). The effects of psychological meaning-centered therapies on quality of life and psychological stress: A metaanalysis. Palliative & Supportive care, 16(5), 608–632. https://doi.org/10.1017/s1478951517000931.
Wang, Y., Zhao, X., Feng, Q., Liu, L., Yao, Y., & Shi, J. (2020). Psychological assistance during the coronavirus disease 2019 outbreak in China. Journal of Health Psychology, 25(6), 733–737. https://doi.org/10.1177/1359105320919177.
Wańkowicz, P., Szylińska, A., & Rotter, I. (2020). Assessment of mental health factors among health professionals depending on their contact with COVID-19 patients. International Journal of Environmental Research and Public Health, 17(16), 5849. https://doi.org/10.3390/ijerph17165849.
Wong, P. T. P. (1993). Effective management of life stress: The resource–congruence model. Stress Medicine, 9(1), 51–60. https://doi.org/10.1002/smi.2460090110.
Wong, P. T. P. (2010). Meaning therapy: An integrative and positive existential psychotherapy. Journal of Contemporary Psychotherapy, 40(2), 85–93. https://doi.org/10.1007/s10879-009-9132-6.
Wong, P. T. P. (2012). The Human Quest for meaning: Theories, Research, and applications. Routledge.
Wong, P. T. P. (2020a). Existential positive psychology and integrative meaning therapy. International Review of Psychiatry, 32(7–8), 565–578. https://doi.org/10.1080/09540261.2020.1814703.
Wong, P. T. P. (2020b). Made for resilience and happiness: Effective coping with Covid-19 according to Viktor E. Frankly and Paul TP Wong. INPM.
Wong, P. T. P., Reker, G. T., & Peacock, E. J. (2006). A resource-congruence model of coping and the development of the coping schema inventory. In P. T. P. Wong & L. C. J. Wong (Eds.), Handbook of multicultural perspectives on stress and coping (pp. 223–283). Spring Publications. https://doi.org/10.1007/0-387-26238-5_11.
Wozniak, H., Benzakour, L., Moullec, G., Buetti, N., Nguyen, A., Corbaz, S., & Cereghetti, S. (2021). Mental health outcomes of ICU and non-ICU healthcare workers during the COVID-19 outbreak: A cross-sectional study. Annals of Intensive Care, 11(1), 1–10. https://doi.org/10.1186/s13613-021-00900-x.
Wright, H., & Jenks, R. A. (2016). Sex on the brain! Associations between sexual activity and cognitive function in older age. Age and Ageing, 45(2), 313–317. https://doi.org/10.1093/ageing/afv197.
Yang, Y., Lu, L., Chen, T., Ye, S., Kelifa, M. O., Cao, N., & Wang, W. (2021). Healthcare worker’s mental health and their associated predictors during the epidemic peak of COVID-19. Psychology Research and Behavior Management, 14, 221–231. https://doi.org/10.2147/prbm.s290931.
Yin, Z., Zhang, W., Jia, X., Wang, X., Hao, J., Yang, Y., & Yue, X. (2022). Psychological distress of frontline healthcare workers in the intensive care unit during the early stage of the COVID-19 pandemic: A qualitative study from China. BMJ open, 12(2), e049627. https://doi.org/10.1136/bmjopen-2021-049627.
Yıldırım, M., Arslan, G., & Özaslan, A. (2020). Perceived risk and mental health problems among healthcare professionals during COVID-19 pandemic: Exploring the mediating effects of resilience and coronavirus fear. International Journal of Mental Healthand Addiction, 10, 1035–1045. https://doi.org/10.1007/s11469-020-00424-8.
Acknowledgements
The authors are grateful to Inmaculada Fernández-Agis for her help in designing the questionnaire, to Pedro La Calle Marcos for his help in finding participants, and to the participants of this study.
Funding
Not applicable.
Funding for open access publishing: Universidad de Sevilla/CBUA
Author information
Authors and Affiliations
Contributions
JAP-E: data collection, theoretical framing, writing of the manuscript, and data analysis. DC: theoretical framing and revision of the manuscript. RP-E: data collection and data analysis. NE: data analysis and revision of the manuscript. All authors contributed to the article and approved the submitted version.
Corresponding author
Ethics declarations
Ethical Approval
The study was approved by the Ethical Committee of the Servicio Andaluz de Salud (SAS) in the Almeria province, Spain.
Informed Consent
The participants gave their consent to participation and publication. The data were treated confidentially and exclusively for research purposes without revealing personal data that would lead to the identification of participants at any time.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Pérez-Escobar, J.A., Carreno, D.F., Pérez-Escobar, R. et al. Sexual and Mental Health in Healthcare Workers during the COVID-19 Outbreak: Exploring the Role of Meaning-Centered Coping. Sex Res Soc Policy (2024). https://doi.org/10.1007/s13178-024-00963-y
Accepted:
Published:
DOI: https://doi.org/10.1007/s13178-024-00963-y