Abstract
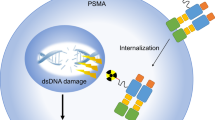
Prostate-specific membrane antigen (PSMA) is an attractive target for both diagnosis and therapy because of its high expression in the vast majority of prostate cancers. Development of small molecules for targeting PSMA is important for molecular imaging and radionuclide therapy of prostate cancer. Recent evidence implies that androgen-deprivation therapy increase PSMA-ligand uptake in some cases. The reported upregulations in PSMA-ligand uptake after exposure to second-generation antiandrogens such as enzalutamide and abiraterone might disturb PSMA-targeted imaging for staging and response monitoring of patients undergoing treatment with antiandrogen-based drugs. On the other hand, second-generation antiandrogens are emerging as potential endoradio-/chemosensitizers. Therefore, the enhancement of the therapeutic efficiency of PSMA-targeted theranostic methods can be listed as a new capability of antiandrogens. In this manuscript, we will present what is currently known about the mechanism of increasing PSMA uptake following exposure to antiandrogens. In addition, we will discuss whether these above-mentioned antiandrogens could play the role of endoradio-/chemosensitizers in combination with the well-established PSMA-targeted methods for pre-targeting of prostate cancer.




Similar content being viewed by others
References
Haas GP, Delongchamps N, Brawley OW, Wang CY, de la Roza G. The worldwide epidemiology of prostate cancer: perspectives from autopsy studies. Can J Urol. 2008;15:3866–71.
Perner S, Cronauer MV, Schrader AJ, Klocker H, Culig Z, Baniahmad A. Adaptive responses of androgen receptor signaling in castration-resistant prostate cancer. Oncotarget. 2015;29:35542–55.
Chandrasekar T, Yang JC, Gao AC, Evans CP. Targeting molecular resistance in castration-resistant prostate cancer. BMC Med. 2015. doi:10.1186/s12916-015-0457-6.
Heidenreich A, Bastian PJ, Bellmunt J, Bolla M, Joniau S, van der Kwast T, et al. EAU guidelines on prostate cancer. Part II: Treatment of advanced, relapsing, and castration-resistant prostate cancer. Eur Urol. 2014;65:467–79.
Kiess AP, Banerjee SR, Mease RC, Rowe SP, Rao A, Foss CA, et al. Prostate-specific membrane antigen as a target for cancer imaging and therapy. Q J Nucl Med Mol Imaging. 2015;59:241–68.
Rai BP, Baum R, Patel A, Hughes R, Alonzi R, Lane T, et al. The role PET with 68Gallium (Ga)-labelled prostate-specific membrane antigen (PSMA) in the management of patient with organ confined and locally advanced prostate cancer prior to radical treatment and after radical prostatectomy. Urology. 2016. doi:10.1016/j.urology.2015.12.048.
Ananias HJ, van den Heuvel MC, Helfrich W, de Jong IJ. Expression of the gastrin‐releasing peptide receptor, the prostate stem cell antigen and the prostate‐specific membrane antigen in lymph node and bone metastases of prostate cancer. Prostate. 2009;69:1101–8.
Minner S, Wittmer C, Graefen M, Salomon G, Steuber T, Haese A, et al. High level PSMA expression is associated with early PSA recurrence in surgically treated prostate cancer. Prostate. 2011;71:281–8.
Rybalov M, Ananias HJ, Hoving HD, van der Poel HG, Rosati S, de Jong IJ. PSMA, EpCAM, VEGF and GRPR as imaging targets in locally recurrent prostate cancer after radiotherapy. Int J Mol Sci. 2014;15:6046–61.
Akhtar NH, Pail O, Saran A, Tyrell L, Tagawa ST. Prostate-specific membrane antigen-based therapeutics. Adv Urol. 2011. doi:10.1155/2012/973820als/au/2012/973820.
Lutje S, Heskamp S, Cornelissen AS, Poeppel TD, van den Broek SA, Rosenbaum-Krumme S, et al. PSMA ligands for radionuclide imaging and therapy of prostate cancer: clinical status. Theranostics. 2015;5:1388–401.
Vargas H, Grimm J, Donati FO, Sala E, Hricak H. Molecular imaging of prostate cancer: translating molecular biology approaches into the clinical realm. Eur Radiol. 2015;25:1294–302.
Vallabhajosula S, Jhanwar Y, Tagawa S, Epstein J, Babich J, Youn T, et al. 99m Tc-MIP-1404 Planar and SPECT scan: Imaging biomarker of androgen receptor (AR) signaling and prostate specific membrane antigen (PSMA) expression. J Nucl Med 2016:57:1541–1.
Giesel FL, Fiedler H, Stefanova M, Sterzing F, Rius M, Kopka K, et al. PSMA PET/CT with Glu-urea-Lys-(Ahx)-[68Ga(HBED-CC)] versus 3D CT volumetric lymph node assessment in recurrent prostate cancer. Eur J Nucl Med Mol Imaging. 2015;42:1794–800.
Afshar-Oromieh A, Avtzi E, Giesel FL, Holland-Letz T, Linhart HG, Eder M, et al. The diagnostic value of PET/CT imaging with the (68)Ga-labelled PSMA ligand HBED-CC in the diagnosis of recurrent prostate cancer. Eur J Nucl Med Mol Imaging. 2015;42:197–209.
Ebenhan T, Vorster M, Marjanovic-Painter B, Wagener J, Suthiram J, Modiselle M, et al. Development of a single vial kit solution for radiolabeling of 68Ga-DKFZ-PSMA-11 and its performance in prostate cancer patients. Molecules. 2015;20:14860–78.
Sterzing F, Kratochwil C, Fiedler H, Katayama S, Habl G, Kopka K, et al. (68)Ga-PSMA-11 PET/CT: a new technique with high potential for the radiotherapeutic management of prostate cancer patients. Eur J Nucl Med Mol Imaging. 2016;43:34–41.
Kratochwil C, Giesel FL, Eder M, Afshar-Oromieh A, Benešová M, Mier W, et al. [177Lu] Lutetium-labelled PSMA ligand-induced remission in a patient with metastatic prostate cancer. Eur J Nucl Med Mol Imaging. 2015;42(6):987–8.
Afshar-Oromieh A, Hetzheim H, Kratochwil C, Benesova M, Eder M, Neels OC, et al. The theranostic PSMA ligand PSMA-617 in the diagnosis of prostate cancer by PET/CT: biodistribution in humans, radiation dosimetry, and first evaluation of tumor lesions. J Nucl Med. 2015;56:1697–705.
Delker A, Fendler WP, Kratochwil C, Brunegraf A, Gosewisch A, Gildehaus FJ, et al. Dosimetry for 177Lu-DKFZ-PSMA-617: a new radiopharmaceutical for the treatment of metastatic prostate cancer. Eur J Nucl Med Mol Imaging. 2016;43:42–51.
Szabo Z, Mena E, Rowe SP, Plyku D, Nidal R, Eisenberger MA, et al. Initial evaluation of [(18)F]DCFPyL for prostate-specific membrane antigen (PSMA)-targeted PET imaging of prostate cancer. Mol Imaging Biol. 2015;17:565–74.
Herrmann K, Bluemel C, Weineisen M, Schottelius M, Wester HJ, Czernin J, et al. Biodistribution and radiation dosimetry for a novel probe targeting prostate specific membrane antigen for Imaging and Therapy (68Ga-PSMA I&T). J Nucl Med. 2015;56:855–61.
Freitag MT, Radtke JP, Hadaschik BA, Kopp-Schneider A, Eder M, Kopka K, et al. Comparison of hybrid 68Ga-PSMA PET/MRI and 68Ga-PSMA PET/CT in the evaluation of lymph node and bone metastases of prostate cancer. Eur J Nucl Med Mol Imaging. 2016;43:70–83.
Ploussard G, Almeras C, Briganti A, Giannarini G, Hennequin C, Ost P, et al. Management of node only recurrence after primary local treatment for prostate cancer: a systematic review of the literature. J Urol. 2015;194:983–8.
Dost RJ, Glaudemans AW, Breeuwsma AJ, de Jong IJ. Influence of androgen deprivation therapy on choline PET/CT in recurrent prostate cancer. Eur J Nucl Med Mol Imaging. 2013;40:41–7.
Evans MJ, Smith-Jones PM, Wongvipat J, Navarro V, Kim S, Bander NH, et al. Noninvasive measurement of androgen receptor signaling with a positron-emitting radiopharmaceutical that targets prostate-specific membrane antigen. Proc Natl Acad Sci U S A. 2011;108:9578–82.
Murga JD, Moorji SM, Han AQ, Magargal WW, DiPippo VA, Olson WC. Synergistic co-targeting of prostate-specific membrane antigen and androgen receptor in prostate cancer. Prostate. 2015;75:242–54.
DiPippo VA, Nguyen HM, Brown LG, Olson WC, Vessella RL, Corey E. Addition of PSMA ADC to enzalutamide therapy significantly improves survival in in vivo model of castration resistant prostate cancer. Prostate. 2016;76:325–34.
Meller B, Bremmer F, Sahlmann C, Hijazi S, Bouter C, Trojan L, et al. Alterations in androgen deprivation enhanced prostate-specific membrane antigen (PSMA) expression in prostate cancer cells as a target for diagnostics and therapy. EJNMMI Res. 2015;5:1–11.
O’Keefe DS, Su SL, Bacich DJ, Horiguchi Y, Luo Y, Powell CT, et al. Mapping, genomic organization and promoter analysis of the human prostate-specific membrane antigen gene. Biochim Biophys Acta. 1998;1443:113–27.
Chang SS. Overview of prostate-specific membrane antigen. Rev Urol. 2004;6:S13–8.
Israeli RS, Powell CT, Corr JG, Fair WR, Heston WD. Expression of the prostate-specific membrane antigen. Cancer Res. 1994;54:1807–11.
Wright GL, Grob BM, Haley C, Grossman K, Newhall K, Petrylak D, et al. Upregulation of prostate-specific membrane antigen after androgen-deprivation therapy. Urol. 1996;48:326–34.
Good D, Schwarzenberger P, Eastham JA, Rhoads RE, Hunt JD, Collins M, et al. Cloning and characterization of the prostate-specific membrane antigen promoter. J Cell Biochem. 1999;74:395–405.
Watt F, Martorana A, Brookes DE, Ho T, Kingsley E, O’Keefe DS, et al. A tissue-specific enhancer of the prostate-specific membrane antigen gene, FOLH1. Genomics. 2001;73:243–54.
Noss KR, Wolfe SA, Grimes SR. Upregulation of prostate specific membrane antigen/folate hydrolase transcription by an enhancer. Gene. 2002;285:247–56.
Yu J, Yu J, Mani RS, Cao Q, Brenner CJ, Cao X, et al. An integrated network of androgen receptor, polycomb, and TMPRSS2-ERG gene fusions in prostate cancer progression. Cancer Cell. 2010;17:443–54.
DiPippo VA, Nguyen HM, Brown LG, Olson WC, Vessella RL, Corey E. In vivo efficacy of PSMA ADC in combination with enzalutamide in castration-resistant prostate cancer. Cancer Res. 2015;75:1685.
Haile S, Sadar MD. Androgen receptor and its splice variants in prostate cancer. Cell Mol Life Sci. 2011;68:3971–81.
Ammannagari N, George S. Anti-androgen therapies for prostate cancer: a focused review. Am J Hema Oncl. 2015;11:15–9.
Antonarakis ES, Lu C, Wang H, Luber B, Nakazawa M, Roeser JC, et al. AR-V7 and resistance to enzalutamide and abiraterone in prostate cancer. N Engl J Med. 2014;371:1028–38.
Afshar-Oromieh A, Malcher A, Eder M, Eisenhut M, Linhart H, Hadaschik B, et al. PET imaging with a [68Ga] gallium-labelled PSMA ligand for the diagnosis of prostate cancer: biodistribution in humans and first evaluation of tumour lesions. Eur J Nucl Med Mol Imaging. 2013;40:486–95.
Chakraborty PS, Tripathi M, Agarwal KK, Kumar R, Vijay MK, Bal C. Metastatic poorly differentiated prostatic carcinoma with neuroendocrine differentiation: negative on 68Ga-PSMA PET/CT. Clin Nucl Med. 2015;40:163–6.
Jadvar H. PSMA PET, in prostate cancer. J Nucl Med. 2015;56:1131–2.
Krohn T, Verburg FA, Pufe T, Neuhuber W, Vogg A, Heinzel A, et al. [68Ga] PSMA-HBED uptake mimicking lymph node metastasis in coeliac ganglia: an important pitfall in clinical practice. Eur J Nucl Med Mol Imaging. 2015;42:210–4.
Weineisen M, Schottelius M, Simecek J, Baum RP, Yildiz A, Beykan S, et al. 68Ga-and 177Lu-labeled PSMA I&T: optimization of a PSMA-targeted theranostic concept and first proof-of-concept human studies. J Nucl Med. 2015;56:1169–76.
Kratochwil C, Giesel FL, Leotta K, Eder M, Hoppe-Tich T, Youssoufian H, et al. PMPA for nephroprotection in PSMA-targeted radionuclide therapy of prostate cancer. J Nucl Med. 2015;56:293–8.
Wilbur DS, Chyan M-K, Hamlin D, Balkin E. In vivo comparison of two anti-PSMA mAb Fab’ conjugates containing branched-chain PEG derivatives with Fab’ and F(ab’)2. J Nucl Med. 2012;53:1545.
Behnam Azad B, Banerjee SR, Pullambhatla M, Lacerda S, Foss CA, Wang Y, et al. Evaluation of a PSMA-targeted BNF nanoparticle construct. Nanoscale. 2015;7:4432–42.
Moon S-H, Yang BY, Kim YJ, Hong MK, Lee Y-S, Lee DS, et al. Development of a complementary PET/MR dual-modal imaging probe for targeting prostate-specific membrane antigen (PSMA). Nanomed Nanotech Biol Med. 2016;12:871–9.
DiPippo VA, Olson WC, Nguyen HM, Brown LG, Vessella RL, Corey E. Efficacy studies of an antibody‐drug conjugate PSMA‐ADC in patient‐derived prostate cancer xenografts. Prostate. 2015;75:303–13.
Paximadis P, Najy AJ, Snyder M, Kim HR. The interaction between androgen receptor and PDGF-D in the radiation response of prostate carcinoma. Prostate. 2016;76:534–43.
Scher HI, Beer TM, Higano CS, Anand A, Taplin ME, Efstathiou E, et al. Antitumour activity of MDV3100 in castration-resistant prostate cancer: a phase 1–2 study. Lancet. 2010;375:1437–46.
Caffo O, Maines F, Donner D, Veccia A, Chierichetti F, Galligioni E. Impact of enzalutamide administration on primary prostate cancer volume: a metabolic evaluation by choline positron emission tomography in castration-resistant prostate cancer patients. Clin Genitourin Cancer. 2014;12:312–6.
De Giorgi U, Caroli P, Scarpi E, Conteduca V, Burgio S, Menna C, et al. 18F-Fluorocholine PET/CT for early response assessment in patients with metastatic castration-resistant prostate cancer treated with enzalutamide. Eur J Nucl Med Mol Imaging. 2015;42:1276–83.
Evans MJ. Measuring oncogenic signaling pathways in cancer with PET: an emerging paradigm from studies in castration-resistant prostate cancer. Cancer Discov. 2012;2:985–4.
Jadvar H. Imaging evaluation of prostate cancer with 18F-fluorodeoxyglucose PET/CT: utility and limitations. Eur J Nucl Med Mol Imaging. 2013;40:5–10.
Tolmachev V, Malmberg J, Estrada S, Eriksson O, Orlova A. Development of a 124I-labeled version of the anti-PSMA monoclonal antibody capromab for immunoPET staging of prostate cancer: Aspects of labeling chemistry and biodistribution. Int J Oncol. 2014;44:1998–2008.
Chatalic KL, Veldhoven-Zweistra J, Bolkestein M, Hoeben S, Koning GA, Boerman OC, et al. A Novel 111In-Labeled Anti–Prostate-Specific Membrane Antigen Nanobody for Targeted SPECT/CT Imaging of Prostate Cancer. J Nucl Med. 2015;56:1094–9.
Hillier SM, Kern AM, Maresca KP, Marquis JC, Eckelman WC, Joyal JL, et al. 123I-MIP-1072, a small-molecule inhibitor of prostate-specific membrane antigen, is effective at monitoring tumor response to taxane therapy. J Nucl Med. 2011;52:1087–93.
Chatalic KS, Heskamp S, Konijnenberg M, Molkenboer-Kuenen JM, Franssen GM, Clahsen-van Groningen MC, et al. Towards personalized treatment of prostate cancer: PSMA I&T, a promising prostate-specific membrane antigen-targeted theranostic agent. Theranostics. 2016;6:849–61.
Lee SJ, Zhang Y, Lee SD, Jung C, Li X, Kim HS, et al. Targeting prostate cancer with conditionally replicative adenovirus using PSMA enhancer. Mol Ther. 2004;10:1051–8.
Cheng WS, Kraaij R, Nilsson B, van der Weel L, de Ridder CM, Tötterman TH, et al. A novel TARP-promoter-based adenovirus against hormone-dependent and hormone-refractory prostate cancer. Mol Ther. 2004;10:355–64.
Ikegami S, Tadakuma T, Suzuki S, Yoshimura I, Asano T, Hayakawa M. Development of gene therapy using prostate‐specific membrane antigen promoter/enhancer with Cre recombinase/LoxP system for prostate cancer cells under androgen ablation condition. Jap J Cancer Res. 2002;93:1154–63.
Zhao W, Xu Y, Kong D, Liu R, Zhang Z, Jin C, et al. Tissue-selective RNA interference in prostate cancer cell using prostate specific membrane antigen promoter/enhancer. Urol Oncol. 2009;27:539–66.
Zhao FJ, Zhang S, Yu ZM, Xia SJ, Li H. Specific targeting of prostate cancer cells in vitro by the suicide gene/prodrug system, uracil phosphoribosylltransferase/5-fluorouracil, under the control of prostate-specific membrane antigen promoter/enhancer. Prostate Cancer Prostatic Dis. 2009;12:166–71.
Zeng H, Wei Q, Huang R, Chen N, Dong Q, Yang Y, et al. Recombinant adenovirus mediated prostate‐specific enzyme pro‐drug gene therapy regulated by prostate‐specific membrane antigen (PSMA) enhancer/promoter. J Androl. 2007;28:827–35.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Martin K. Bakht, So Won Oh, Hyewon Youn, Gi jeong Cheon, Cheol Kwak and Keon Wook Kang declare that they have no conflict of interest.
Ethical Statement
This article does not contain any studies with human participants or animals performed by any of the authors. The manuscript has not been published before, is not under consideration for publication anywhere else and has been approved by all co-authors.
Rights and permissions
About this article
Cite this article
Bakht, M.K., Oh, S.W., Youn, H. et al. Influence of Androgen Deprivation Therapy on the Uptake of PSMA-Targeted Agents: Emerging Opportunities and Challenges. Nucl Med Mol Imaging 51, 202–211 (2017). https://doi.org/10.1007/s13139-016-0439-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13139-016-0439-4