Abstract
Purpose
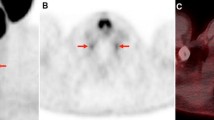
To determine the frequency of seemingly pathological retroperitoneal uptake in the location of the coeliac ganglia in patients undergoing [68Ga]PSMA-HBED PET/CT.
Methods
The study included 85 men with prostate cancer referred for [68Ga]PSMA-HBED PET/CT. The PET/CT scans were evaluated for the local finding in the prostate and the presence of lymph node metastases, distant metastases and coeliac ganglia. The corresponding standardized uptake values (SUV) were determined. SUVmax to background uptake (gluteal muscle SUVmean) ratios were calculated for the ganglia and lymph node metastases. Immunohistochemistry was performed on the ganglia.
Results
In 76 of the 85 patients (89.4 %) at least one ganglion with tracer uptake was found. For the ganglia, SUVmax and SUVmax to background SUVmean ratios were 2.97 ± 0.88 and 7.98 ± 2.84 (range 1.57–6.38 and 2.83–30.6), respectively, and 82.8 % of all ganglia showed an uptake ratio of >5.0. For lymph node metastases, SUVmax and SUVmax to background SUVmean ratios were 8.5 ± 7.0 and 23.31 ± 22.23 (range 2.06–35.9 and 5.25–115.8), respectively. In 35 patients (41.2 %), no lymph node metastases were found but tracer uptake was seen in the ganglia. Immunohistochemistry confirmed strong PSMA expression in the ganglia.
Conclusion
Coeliac ganglia show a relevant [68Ga]PSMA-HBED uptake in most patients and may mimic lymph node metastases.



Similar content being viewed by others
References
Afshar-Oromieh A, Haberkorn U, Eder M, Eisenhut M, Zechmann CM. [68Ga]Gallium-labelled PSMA ligand as superior PET tracer for the diagnosis of prostate cancer: comparison with 18F-FECH. Eur J Nucl Med Mol Imaging. 2012;39:1085–6. doi:10.1007/s00259-012-2069-0.
Afshar-Oromieh A, Haberkorn U, Schlemmer HP, Fenchel M, Eder M, Eisenhut M, et al. Comparison of PET/CT and PET/MRI hybrid systems using a 68Ga-labelled PSMA ligand for the diagnosis of recurrent prostate cancer: initial experience. Eur J Nucl Med Mol Imaging. 2014;41:887–97. doi:10.1007/s00259-013-2660-z.
Afshar-Oromieh A, Zechmann CM, Malcher A, Eder M, Eisenhut M, Linhart HG, et al. Comparison of PET imaging with a (68)Ga-labelled PSMA ligand and (18)F-choline-based PET/CT for the diagnosis of recurrent prostate cancer. Eur J Nucl Med Mol Imaging. 2014;41:11–20. doi:10.1007/s00259-013-2525-5.
Afshar-Oromieh A, Malcher A, Eder M, Eisenhut M, Linhart HG, Hadaschik BA, et al. PET imaging with a [68Ga]gallium-labelled PSMA ligand for the diagnosis of prostate cancer: biodistribution in humans and first evaluation of tumour lesions. Eur J Nucl Med Mol Imaging. 2013;40:486–95. doi:10.1007/s00259-012-2298-2.
Ha TI, Kim GH, Kang DH, Song GA, Kim S, Lee JW. Detection of celiac ganglia with radial scanning endoscopic ultrasonography. Korean J Intern Med. 2008;23:5–8.
Wang ZJ, Webb EM, Westphalen AC, Coakley FV, Yeh BM. Multi-detector row computed tomographic appearance of celiac ganglia. J Comput Assist Tomogr. 2010;34:343–7. doi:10.1097/RCT.0b013e3181d26ddd.
Paz Z, Rosen A. The human celiac ganglion and its splanchnic nerves. Acta Anat (Basel). 1989;136:129–33.
Levy M, Rajan E, Keeney G, Fletcher JG, Topazian M. Neural ganglia visualized by endoscopic ultrasound. Am J Gastroenterol. 2006;101:1787–91. doi:10.1111/j.1572-0241.2006.00685.x.
Abtahi SM, Elmi A, Hedgire SS, Ho YC, Pourjabbar S, Singh S, et al. Depiction of celiac ganglia on positron emission tomography and computed tomography in patients with lung cancer. Clin Imaging. 2014;38:292–5. doi:10.1016/j.clinimag.2013.12.017.
Chang SS, Reuter VE, Heston WD, Bander NH, Grauer LS, Gaudin PB. Five different anti-prostate-specific membrane antigen (PSMA) antibodies confirm PSMA expression in tumor-associated neovasculature. Cancer Res. 1999;59:3192–8.
Eder M, Schafer M, Bauder-Wust U, Hull WE, Wangler C, Mier W, et al. 68Ga-complex lipophilicity and the targeting property of a urea-based PSMA inhibitor for PET imaging. Bioconjug Chem. 2012;23:688–97. doi:10.1021/bc200279b.
Acknowledgments
We thank Nina Koch for technical support with the immunohistochemical examinations.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Krohn, T., Verburg, F.A., Pufe, T. et al. [68Ga]PSMA-HBED uptake mimicking lymph node metastasis in coeliac ganglia: an important pitfall in clinical practice. Eur J Nucl Med Mol Imaging 42, 210–214 (2015). https://doi.org/10.1007/s00259-014-2915-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-014-2915-3