Abstract
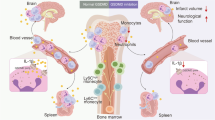
Accumulation of neutrophils in the brain is a hallmark of cerebral ischemia and considered central in exacerbating tissue injury. Intercellular adhesion molecule (ICAM)-1 is upregulated on brain endothelial cells after ischemic stroke and considered pivotal in neutrophil recruitment as ICAM-1-deficient mouse lines were found protected from experimental stroke. Translation of therapeutic inhibition of ICAM-1 into the clinic however failed. This prompted us to investigate stroke pathogenesis in Icam1tm1Alb C57BL/6 mutants, a true ICAM-1null mouse line. Performing transient middle cerebral artery occlusion, we found that absence of ICAM-1 did not ameliorate stroke pathology at acute time points after reperfusion. Near-infrared imaging showed comparable accumulation of neutrophils in the ischemic hemispheres of ICAM-1null and wild type C57BL/6 mice. We also isolated equal numbers of neutrophils from the ischemic brains of ICAM-1null and wild type C57BL/6 mice. Immunostaining of the brains showed neutrophils to equally accumulate in the leptomeninges and brain parenchymal vessels of ICAM-1null and wild type C57BL/6 mice. In addition, the lesion size was comparable in ICAM-1null and wild type mice. Our study demonstrates that absence of ICAM-1 neither inhibits cerebral ischemia-induced accumulation of neutrophils in the brain nor provides protection from ischemic stroke.







Similar content being viewed by others
References
Neuwelt EA, Bauer B, Fahlke C, Fricker G, Iadecola C, Janigro D, et al. Engaging neuroscience to advance translational research in brain barrier biology. Nat Rev Neurosci. 2011;12(3):169–82. https://doi.org/10.1038/nrn2995.
Engelhardt B, Carare RO, Bechmann I, Flugel A, Laman JD, Weller RO. Vascular, glial, and lymphatic immune gateways of the central nervous system. Acta Neuropathol. 2016;132(3):317–38. https://doi.org/10.1007/s00401-016-1606-5.
Stanimirovic DB, Friedman A. Pathophysiology of the neurovascular unit: disease cause or consequence? JCBFM. 2012;32:1207–21.
Engelhardt B, Ransohoff RM. Capture, crawl, cross: the T cell code to breach the blood-brain barriers. Trends Immunol. 2012;33(12):579–89. https://doi.org/10.1016/j.it.2012.07.004.
Owens T, Bechmann I, Engelhardt B. Perivascular spaces and the two steps to neuroinflammation. J Neuropath Exp Neurol. 2008;67(12):1113–21. https://doi.org/10.1097/NEN.0b013e31818f9ca8.
Gelderblom M, Sobey CG, Kleinschnitz C, Magnus T. Danger signals in stroke. Ageing Res Rev. 2015;24(Pt A):77–82. https://doi.org/10.1016/j.arr.2015.07.004.
Barone FC, Feuerstein GZ. Inflammatory mediators and stroke: new opportunities for novel therapeutics. JCBFM. 1999;19:819–34.
Okada Y, Copeland BR, Mori E, Tung MM, Thomas WS, del Zoppo GJ. P-selectin and intercellular adhesion molecule-1 expression after focal brain ischemia and reperfusion. Stroke. 1994;25(1):202–11. https://doi.org/10.1161/01.STR.25.1.202.
Enzmann G, Mysiorek C, Gorina R, Cheng YJ, Ghavampour S, Hannocks MJ, et al. The neurovascular unit as a selective barrier to polymorphonuclear granulocyte (PMN) infiltration into the brain after ischemic injury. Acta Neuropathol. 2013;125(3):395–412. https://doi.org/10.1007/s00401-012-1076-3.
Jander S, Kraemer M, Schroeter M, Witte OW, Stoll G. Lymphocytic infiltration and expression of intercellular adhesion molecule-1 in photochemically induced ischemia of the rat cortex. JCBFM. 1995;15:42–51.
Garcia JH, Liu KF, Yoshida Y, Lian J, Chen S, del Zoppo GJ. Influx of leukocytes and platelets in an evolving brain infarct (Wistar rat). Am J Pathol. 1994;144(1):188–99.
Akopov SE, Simonian NA, Grigorian GS. Dynamics of polymorphonuclear leukocyte accumulation in acute cerebral infarction and their correlation with brain tissue damage. Stroke. 1996;27(10):1739–43. https://doi.org/10.1161/01.STR.27.10.1739.
Barone FC, Schmidt DB, Hillegass LM, Price WJ, White RF, Feuerstein GZ, et al. Reperfusion increases neutrophils and leukotriene B4 receptor binding in rat focal ischemia. Stroke. 1992;23(9):1337–47; discussion 47-8. https://doi.org/10.1161/01.STR.23.9.1337.
Perez-de-Puig I, Miro-Mur F, Ferrer-Ferrer M, Gelpi E, Pedragosa J, Justicia C, et al. Neutrophil recruitment to the brain in mouse and human ischemic stroke. Acta Neuropathol. 2015;129(2):239–57. https://doi.org/10.1007/s00401-014-1381-0.
Connolly ES Jr, Winfree CJ, Springer TA, Naka Y, Liao H, Yan SD, et al. Cerebral protection in homozygous null ICAM-1 mice after middle cerebral artery occlusion. Role of neutrophil adhesion in the pathogenesis of stroke. J Clin Invest. 1996;97(1):209–16. https://doi.org/10.1172/JCI118392.
Soriano SG, Lipton SA, Wang YF, Xiao M, Springer TA, Gutierrez-Ramos JC, et al. Intercellular adhesion molecule-1-deficient mice are less susceptible to cerebral ischemia-reperfusion injury. Ann Neurol. 1996;39(5):618–24. https://doi.org/10.1002/ana.410390511.
Investigators. Use of anti-ICAM-1 therapy in ischemic stroke: results of the Enlimomab Acute Stroke Trial. Neurol. 2001;57:1428–34.
Becker KJ. Anti-leukocyte antibodies: LeukArrest (Hu23F2G) and Enlimomab (R6.5) in acute stroke. Curr Med Res Opin. 2002;18(Suppl 2):s18–22. https://doi.org/10.1185/030079902125000688.
Xu H, Gonzalo JA, St Pierre Y, Williams IR, Kupper TS, Cotran RS, et al. Leukocytosis and resistance to septic shock in intercellular adhesion molecule 1-deficient mice. J Exp Med. 1994;180(1):95–109. https://doi.org/10.1084/jem.180.1.95.
Sligh JE Jr, Ballantyne CM, Rich SS, Hawkins HK, Smith CW, Bradley A, et al. Inflammatory and immune responses are impaired in mice deficient in intercellular adhesion molecule 1. Proc Nat Acad Sci USA. 1993;90(18):8529–33. https://doi.org/10.1073/pnas.90.18.8529.
van Den Engel NK, Heidenthal E, Vinke A, Kolb H, Martin S. Circulating forms of intercellular adhesion molecule (ICAM)-1 in mice lacking membranous ICAM-1. Blood. 2000;95:1350–5.
Rieckmann P, Michel U, Albrecht M, Bruck W, Wockel L, Felgenhauer K. Soluble forms of intercellular adhesion molecule-1 (ICAM-1) block lymphocyte attachment to cerebral endothelial cells. J Neuroimmunol. 1995;60(1-2):9–15. https://doi.org/10.1016/0165-5728(95)00047-6.
Hu X, Wohler JE, Dugger KJ, Barnum SR. Beta2-integrins in demyelinating disease: not adhering to the paradigm. J Leuk Biol. 2010;87(3):397–403. https://doi.org/10.1189/jlb.1009654.
Ramos TN, Bullard DC, Barnum SR. ICAM-1: isoforms and phenotypes. J Immunol. 2014;192(10):4469–74. https://doi.org/10.4049/jimmunol.1400135.
Dunne JL, Collins RG, Beaudet AL, Ballantyne CM, Ley K. Mac-1, but not LFA-1, uses intercellular adhesion molecule-1 to mediate slow leukocyte rolling in TNF-alpha-induced inflammation. J Immunol. 2003;171(11):6105–11. https://doi.org/10.4049/jimmunol.171.11.6105.
Bullard DC, Hu X, Schoeb TR, Collins RG, Beaudet AL, Barnum SR. Intercellular adhesion molecule-1 expression is required on multiple cell types for the development of experimental autoimmune encephalomyelitis. J Immunol. 2007;178(2):851–7. https://doi.org/10.4049/jimmunol.178.2.851.
Endres M, Fink K, Zhu J, Stagliano NE, Bondada V, Geddes JW, et al. Neuroprotective effects of gelsolin during murine stroke. J Clin Invest. 1999;103(3):347–54. https://doi.org/10.1172/JCI4953.
Bederson JB, Pitts LH, Tsuji M, Nishimura MC, Davis RL, Bartkowski H. Rat middle cerebral artery occlusion: evaluation of the model and development of a neurologic examination. Stroke. 1986;17(3):472–6. https://doi.org/10.1161/01.STR.17.3.472.
Gorina R, Lyck R, Vestweber D, Engelhardt B. Beta2 integrin-mediated crawling on endothelial ICAM-1 and ICAM-2 is a prerequisite for transcellular neutrophil diapedesis across the inflamed blood-brain barrier. J Immunol. 2014;192:324–37.
Vaas M, Enzmann G, Perinat T, Siler U, Reichenbach J, Licha K, et al. Non-invasive near-infrared fluorescence imaging of the neutrophil response in a mouse model of transient cerebral ischemia. JCBFM. 2017;37(8):2833–2847.
Reiss Y, Hoch G, Deutsch U, Engelhardt B. T cell interaction with ICAM-1-deficient endothelium in vitro: essential role for ICAM-1 and ICAM-2 in transendothelial migration of T cells. Eur J Immunol. 1998;28(10):3086–99. https://doi.org/10.1002/(SICI)1521-4141(199810)28:10<3086::AID-IMMU3086>3.0.CO;2-Z.
Engelhardt B, Laschinger M, Schulz M, Samulowitz U, Vestweber D, Hoch G. The development of experimental autoimmune encephalomyelitis in the mouse requires alpha4-integrin but not alpha4beta7-integrin. J Clin Invest. 1998;102(12):2096–105. https://doi.org/10.1172/JCI4271.
Borges E, Tietz W, Steegmaier M, Moll T, Hallmann R, Hamann A, et al. P-selectin glycoprotein ligand-1 (PSGL-1) on T helper 1 but not on T helper 2 cells binds to P-selectin and supports migration into inflamed skin. J Exp Med. 1997;185(3):573–8. https://doi.org/10.1084/jem.185.3.573.
Daley JM, Thomay AA, Connolly MD, Reichner JS, Albina JE. Use of Ly6G-specific monoclonal antibody to deplete neutrophils in mice. J Leuk Biol. 2008;83(1):64–70. https://doi.org/10.1189/jlb.0407247.
Doring A, Wild M, Vestweber D, Deutsch U, Engelhardt B. E- and P-selectin are not required for the development of experimental autoimmune encephalomyelitis in C57BL/6 and SJL mice. J Immunol. 2007;179(12):8470–9. https://doi.org/10.4049/jimmunol.179.12.8470.
Jalkanen S, Saari S, Kalimo H, Lammintausta K, Vainio E, Leino R, et al. Lymphocyte migration into the skin: the role of lymphocyte homing receptor (CD44) and endothelial cell antigen (HECA-452). J Invest Dermatol. 1990;94(6):786–92. https://doi.org/10.1111/1523-1747.ep12874646.
Engelhardt B, Conley FK, Kilshaw PJ, Butcher EC. Lymphocytes infiltrating the CNS during inflammation display a distinctive phenotype and bind to VCAM-1 but not to MAdCAM-1. Int Immunol. 1995;7(3):481–91. https://doi.org/10.1093/intimm/7.3.481.
Neumann J, Riek-Burchardt M, Herz J, Doeppner TR, Konig R, Hutten H, et al. Very-late-antigen-4 (VLA-4)-mediated brain invasion by neutrophils leads to interactions with microglia, increased ischemic injury and impaired behavior in experimental stroke. Acta Neuropathol. 2015;129(2):259–77. https://doi.org/10.1007/s00401-014-1355-2.
Barkalow FJ, Goodman MJ, Gerritsen ME, Mayadas TN. Brain endothelium lack one of two pathways of P-selectin-mediated neutrophil adhesion. Blood. 1996;88(12):4585–93.
Krams M, Lees KR, Hacke W, Grieve AP, Orgogozo JM, Ford GA. Acute stroke therapy by inhibition of neutrophils (ASTIN): an adaptive dose-response study of UK-279,276 in acute ischemic stroke. Stroke. 2003;34(11):2543–8. https://doi.org/10.1161/01.STR.0000092527.33910.89.
Deddens LH, van Tilborg GAF, van der Marel K, Hunt H, van der Toorn A, Viergever MA, et al. In vivo molecular MRI of ICAM-1 expression on endothelium and leukocytes from subacute to chronic stages after experimental stroke. Transl Stroke Res. 2017;8(5):440–8. https://doi.org/10.1007/s12975-017-0536-4.
Fan Z, McArdle S, Marki A, Mikulski Z, Gutierrez E, Engelhardt B, et al. Neutrophil recruitment limited by high-affinity bent beta2 integrin binding ligand in cis. Nat Commun. 2016;7:12658. https://doi.org/10.1038/ncomms12658.
Hu X, Barnum SR, Wohler JE, Schoeb TR, Bullard DC. Differential ICAM-1 isoform expression regulates the development and progression of experimental autoimmune encephalomyelitis. Mol Immunol. 2010;47(9):1692–700. https://doi.org/10.1016/j.molimm.2010.03.005.
Carrano A, Hoozemans JJ, van der Vies SM, van Horssen J, de Vries HE, Rozemuller AJ. Neuroinflammation and blood-brain barrier changes in capillary amyloid angiopathy. Neurodegener Dis. 2012;10(1-4):329–31. https://doi.org/10.1159/000334916.
Tyagi N, Roberts AM, Dean WL, Tyagi SC, Lominadze D. Fibrinogen induces endothelial cell permeability. Mol Cell Biochem. 2008;307(1-2):13–22. https://doi.org/10.1007/s11010-007-9579-2.
Tailor A, Cooper D, Granger DN. Platelet-vessel wall interactions in the microcirculation. Microcirculation. 2005;12(3):275–85. https://doi.org/10.1080/10739680590925691.
Chaichana KL, Pradilla G, Huang J, Tamargo RJ. Role of inflammation (leukocyte-endothelial cell interactions) in vasospasm after subarachnoid hemorrhage. World Neurosurg. 2010;73(1):22–41. https://doi.org/10.1016/j.surneu.2009.05.027.
Provencio JJ, Fu X, Siu A, Rasmussen PA, Hazen SL, Ransohoff RM. CSF neutrophils are implicated in the development of vasospasm in subarachnoid hemorrhage. Neurocrit Care. 2010;12(2):244–51. https://doi.org/10.1007/s12028-009-9308-7.
Provencio JJ, Altay T, Smithason S, Moore SK, Ransohoff RM. Depletion of Ly6G/C(+) cells ameliorates delayed cerebral vasospasm in subarachnoid hemorrhage. J Neuroimmunol. 2011;232(1-2):94–100. https://doi.org/10.1016/j.jneuroim.2010.10.016.
Hall CN, Reynell C, Gesslein B, Hamilton NB, Mishra A, Sutherland BA, et al. Capillary pericytes regulate cerebral blood flow in health and disease. Nature. 2014;508(7494):55–60. https://doi.org/10.1038/nature13165.
Acknowledgements
We would like to thank the Microscopy Imaging Center (MIC) of the University of Bern, especially Dr. Roch-Philippe Charles (IBMM), for support in image analysis. We express our sincere thanks to Claudia Blatti, Therese Périnat, and Albert Witt for technical help in this study. We thank Dr. Urban Deutsch for help with the mouse breeding and genotyping logistics. Additional thanks go to Katrin Bissegger, Isabelle Wymann, and Svetlozar Tsonev for professional caretaking of the mice.
Author Contribution Statement
G.E. and M.V. performed experiments including surgeries and data analysis, and G.E. wrote the manuscript. S.P. performed the experiments, analyzed the data, and prepared some figures. B.E. and J.K. outlined and supervised the project, evaluated data, and edited the manuscript.
Funding
This study was funded by the EU FP7 European Stroke Network (grant nos. 201024 and 202213 to BE), the Swiss Heart Foundation (to BE and GE), and the Swiss National Science Foundation (grant PZ00P3_136822), and Hartmann-Müller Foundation (to JK).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
All applicable international, national, and institutional guidelines for the care and use of animals were followed. In detail, in vivo experiments were approved by the Veterinary Office of the Canton of Bern (Switzerland) (licenses BE79/11, BE127/14). Animal research was performed in accordance to the Swiss legislation on the protection of animals and in compliance with the ARRIVE guidelines for reporting animal research (https://www.nc3rs.org.uk/arrive-guidelines).
Conflict of Interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Suppl. Fig. 1
Absence of ICAM-1 does not induce compensatory upregulation of endothelial cell adhesion molecules in the ischemic hemisphere following 60-min ischemia and 24-h reperfusion. ICAM-1null and wild type (WT) C57BL/6 mice displayed numerous VCAM-1 positive blood vessels both in the ipsilateral cortex (Fig. 1(a’, d’)) and in the meningeal compartment (Fig. 1(c’, f’)). In relation to ICAM-1-positive blood vessels in WT C57BL/6 mice (Fig. 1(a–c)), VCAM-1-positive vessels outnumbered the former and were distributed rather evenly throughout the lesioned hemisphere. Lack of ICAM-1 immunoreactivity in ICAM-1null C57BL/6 mice confirmed the complete absence of ICAM-1 isoforms (Fig. 1(d–f)). We observed de novo synthesis of P-selectin in parenchymal microvessels (Fig. 1(a”–b”, e”–f”)) in C57BL/6 mice of either genotype. The scale bar equals 50 μm and applies to all images (GIF 689 kb)
Suppl. Fig. 2
ICAM-1 is dispensable for neutrophil accumulation in blood vessels following stroke and reperfusion. Double immunofluorescence staining of neutrophils (Ly6G, green) and ICAM-1 (red) revealed that ICAM-1 is not required for localization of neutrophils to microvessels in the ischemic hemisphere. Both ICAM-1-positive brain microvessels (wild type (WT) mouse, left column, arrow) and blood vessels deficient of ICAM-1 (ICAM-1null, right column, arrowheads) permitted neutrophil adhesion. The scale bar equals 50 μm (GIF 40 kb)
Suppl. Fig. 3
VCAM-1 does not exclusively mediate neutrophil adhesion to brain microvessels after stroke. Double immunofluorescence staining of neutrophils (Ly6G, green) and VCAM-1 (red) confirmed neutrophil endothelial interaction in both the presence (arrow) and absence (arrowhead) of VCAM-1 following transient ischemia and reperfusion in wild type (WT) (a–d) and ICAM-1null (a’–d’) C57BL/6 mice. The scale bar equals 50 μm (GIF 54 kb)
Suppl. Fig. 4
Expression of P-selectin does not favor neutrophil localization to brain microvessels after stroke. Double immunofluorescence staining of neutrophils (Ly6G, green) and P-selectin (red) demonstrated no preferential localization of neutrophils to P-selectin positive microvessels in the ischemic cortex of wild type (WT) (left column) and ICAM-1null (right column) C57BL/6 mice. Neutrophils localized to the perivascular compartment in both the presence (white arrow) and absence (white arrowhead) of P-selectin. Occasionally, neutrophils were observed adjacent to platelets, which express P-selectin as well (yellow arrow). Irrespective of the expression of P-selectin, neutrophils were also detected in the leptomeningeal compartment (yellow arrowhead). The scale bar equals 50 μm (GIF 84 kb)
Rights and permissions
About this article
Cite this article
Enzmann, G.U., Pavlidou, S., Vaas, M. et al. ICAM-1null C57BL/6 Mice Are Not Protected from Experimental Ischemic Stroke. Transl. Stroke Res. 9, 608–621 (2018). https://doi.org/10.1007/s12975-018-0612-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12975-018-0612-4