Abstract
Trimethylamine-n-oxide (TMAO) is a metabolite of intestinal flora following the consumption of phosphatidylcholine-rich foods. Clinical cohort studies have shown that plasma TMAO may be a risk factor for cancer development, including hepatocellular carcinoma (HCC), but fundamental research data supporting this hypothesis are lacking. In this study, HCC cells were treated with TMAO in vivo and in vitro to evaluate the effect on some indicators related to the malignancy degree of HCC, and the relevant molecular mechanisms were explored. In vitro, TMAO promoted the proliferation and migration of HCC cells and significantly upregulated the expression of proteins related to epithelial–mesenchymal transformation (EMT). In vivo, after HCC cells were inoculated subcutaneously in nude mice given water containing TMAO, the tumors grew faster and larger than those in the mice given ordinary water. The immunohistochemistry analysis showed that proliferation, migration and EMT-related proteins in the tumor tissues were significantly upregulated by TMAO. Furthermore, TMAO obviously enhanced the phosphorylation of MAPK signaling molecules in vivo and in vitro. In conclusion, TMAO promotes the proliferation, migration and EMT of HCC cells by activating the MAPK pathway.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Hepatocellular carcinoma (HCC) is one of the most common malignant tumors. Each year HCC leads to more than 900,000 new cases and 830,000 deaths [1], and accounts for 70–85% of the total cancer burden [2]. Major risk factors for HCC include hepatitis B virus (HBV), hepatitis C virus (HCV) and aflatoxin exposure [3]. The incidence of infection-induced HCC is declining due to routine immunization of infants against hepatitis B and improved personal hygiene [4]. However, attention has been paid in recent years to other risk factors for non-infection-associated HCC, such as alcohol abuse, smoking, non-alcoholic fatty liver disease (NAFLD), obesity, and type 2 diabetes; and there is growing evidence that diet plays an important role in the development of HCC [5,6,7].
In recent years, trimethylamine-n-oxide (TMAO), as a metabolite of phosphatidylcholine (lecithin) in the diet, has been found and attracted much attention due to its association with many diseases, including cardiovascular disease [8], type 2 diabetes mellitus [9] and chronic kidney disease [10]. Foods rich in phosphatidylcholine (mainly including eggs and red meat in the diet) are catalyzed by intestinal microbial enzymes to produce trimethylamine, most of which is then absorbed into the bloodstream through the mesentery and transported to the liver where it is rapidly oxidized to trimethylamine oxide by flavin monooxygenase [11].Recent studies have shown that TMAO is involved in the development of various cancers, particularly colorectal cancer (CRC) [12, 13]. Sajin Baeetal et al. were the first to reported the positive association between plasma TMAO and CRC in a nested case–control study including 835 matched pairs [14]. Another study revealed a strong association between CRC and TMAO using genome-wide systems analysis to construct chemical genes, disease genes, and protein–protein interaction datas from multiple large-scale datasets [15]. Since TMAO production needs to be based on the connection between the gut and the liver (dietary choline/betaine/l-carnitine → gut-formed trimethylamine → liver-formed TMAO) [11], the relationship between TMAO and CRC implies that TMAO may also be association with HCC. In addition, a study has shown that there is obvious positive correlation between serum TMAO and NAFLD [16]. Due to the recognized close association between NAFLD and HCC, it is natural to infer a possible relationship between TMAO and HCC. In fact, a recent case–control study showed that raised serum TMAO levels were related to an incremental risk of HCC [17]. Then, a recent study showed that the gut microbial metabolite TMAO promoted the development of inflammatory hepatocellular carcinoma [18].
Therefore, it can be inferred that TMAO is highly likely related to the progression of HCC. Whether TMAO can be used as a molecular marker for predicting HCC needs to be confirmed by additional exploratory studies. In this study, the effect of TMAO on the proliferation, migration and epithelial mesenchymal transformation of HCC cells in vivo and in vitro was analyzed, and the relevant mechanisms were clarified.
2 Materials and methods
2.1 Cell culture and treatment
Human HCC cell lines (HepG2 and Huh-7) were obtained from the Institute of Chemistry and Cell Biology (Shanghai, China). The cells were cultured with DMEM (HyClone, USA) containing 10% fetal bovine serum (FBS, HyClone, USA), 100 U/ml penicillin/streptomycin (Sigma-Aldrich, USA) and cultured at 37 °C in a 5% CO2 incubator. Different concentrations of TMAO (Sigma-Aldrich, USA) were added to the medium, and cells were collected 48 h later for detection.
2.2 Cell proliferation assay
The cell growth index was automatically recorded using a label free real-time cell analysis system (RTCA, xCELLigenceRTCADP, Afghanistan) with a cell inoculation density of 3 × 103 cells/well. Also, cell proliferation was assessed using the BeyoClick™5-ethynyl-2′-deoxyuridine (EdU) Cell Proliferation Kit with 3,3ʹ,5,5ʹ-Tetramethylbenzidine(TMB), which could directly measureactive DNA synthesis or S-phase synthesis of a cell cycle via reaction with fluorescent azides in a Cu(I)-catalyzed [3 + 2] cycloaddition. The absorbance was measured at 630 nm and calculated as a ratio against untreated cells.
2.3 Colony formation assay
The cells were dispersed with trypsin and collected, they were then re-suspended with medium containing different concentrations of TMAO. 500 cells/well were inoculated in 6-well plate with triplicate per concentration. Cells were incubated for 8 days, the medium was changed every 3 days. After 8 days, the medium was discarded, the cells were washed twice with PBS and fixed with 4% paraformaldehyde for 20 min. The paraformaldehyde was then discarded, the cells were washed twice with PBS and stained with 0.1% crystal violet (Beyotime Biotechnology, China) 500 μL per well for 10 min. The dye was discarded and the cells were gently rinsed with PBS until the color became clear. Finally, a digital camera was used to take pictures of the colony cells.
2.4 Cell migration assay
Wound healing assay was used to evaluate the migration ability of HepG2 and Huh-7 cells. 6-well plates were used in this experimental. HepG2 and Huh-7 cells were respectively seeded in 6-well plates (3 × 104 cells/well) in triplicate. After 90% confluence of cells on the plates, the wells were scratched with a 200 μL pipette tip across the center of the well. The medium in the wells was removed and gently washed with PBS to remove floating cells. Then the medium without serum including different concentrations of TMAO were added. ImageJ software 1.49 was used for measuring the wound gaps.
Transwell assay was used to measurethe migration ability of cells. In brief, the cells were re-suspended with serum-free medium (2 × 105/mL) and inoculated into the upper chamber of transwell (Corning, NY, USA). 600 μL medium containing 10% fetal bovine serum were added to the lower chamber. After 24 h, the chamber was removed and gently cleaned with PBS. The bottom of chamber was soaked with 4% paraformaldehyde solution to fix the migrated cells for 20 min. Then the cells on the membrane were stained with 0.1% crystal violet for 15 min. After staining, the chamber were washed with water, and the number of migrated cells was counted under the microscope (Olympus Corp. Tokyo, Japan).
2.5 Tumorigenicity assay
For the tumorigenicity assay, 1 × 106 HepG2 cells in 100 mL PBS were resuspended and injected subcutaneously into the flanks of nude mice (Beijing Vital River Laboratory Animal Technology Co., Ltd.) 0.8 female nude mice, 4 weeks old with an average body weight of 15 g, were randomly divided into 2 groups and anesthetized with 0.8% pentobarbital sodium (40 mg/kg) before transplantation. One group of mice was fed normal drinking water, while the other group was fed drinking water containing 8 mg/mL of TMAO. Tumor size was measured using calipers at 5-day intervals. After 25 days, the subcutaneous tumors of the mice were removed and weighed (mean ± SD). The maximal tumor size/burden was not exceeded the rules of Ethics Committee. A portion of the tumor tissue was clipped and treated with cell lysate to extract the protein for Western blot assay. Another part of the tumor tissue was embedded with paraffin and then detected by immunohistochemistry. All animal work was approved by the Ethics Committee for Animal Experiments of the Hubei University of Medicine (No. 00201033).
2.6 IHC staining and immunofluorescence
Tumor tissues of nude mice were taken, fixed with 4% paraformaldehyde for 48 h, dehydrated, embedded in paraffin, and sectioned with a thickness of 3 µm for immunohistochemical studies. Slides were incubated overnight in 4℃ with primary antibodies (rabbit anti-human polyclonal antibody PCNA, Vimentin, MMP9and VEGF, diluted at 1:100, Proteintech, China). Horseradish peroxidase-conjugated goat anti-rabbit secondary antibody (diluted at 1:500, Proteintech, China) was added and treated at 37 ℃ for 1 h. The expression level of 3,3ʹ-diaminobenzidine was detected under an inverted microscope (Olympus IX73). For immunofluorescence, the HepG2 cell treated with different concentrations of TMAO were fixed in 4% paraformaldehyde and incubated overnight in 4 ℃ with primary antibodies (rabbit anti-human polyclonal antibody VEGF, MMP9, and vimentin, diluted at 1:200, Proteintech, China). The second antibody with fluorescent was added to interact with the primary antibodies at room temperature for 2 h in dark. The fluorescence intensity was observed under the fluorescence microscope.
2.7 Western blot
Proteins samples were collected and quivalent aliquots of protein were electrophoresed on a 10% sodium dodecylsulfate/polyacrylamide gel, in 1 × Tris–glycine buffer, followed by transfer to nitrocellulose membranes, and incubated with primary antibodies (PCNA, MMP9, VEGF, Ki67, Vimentin, Snail, Slug, E-cadherin, P38, P-P38, ERK, P-ERK, JNK, P-JNK, diluted at 1:500, Proteintech, China), over night at 4 °C. Thereafter, the nitrocellulose membranes were incubated with secondary antibody (Goat anti-Rabbit IgG-HRP, diluted at 1:10,000, Proteintech, China) for 1 h, at room temperature. The immunoreactive proteins were detected by enhanced chemiluminescence substrate and the blot was scanned, and densitometric analysis with the Image J software was performed.
2.8 Statistical analysis
All results that are expressed as the mean ± SEM were obtained from more than three samples per experiment, and significant differences between different groups were calculated using a Dunnett-t test. A value of P < 0.05 was considered statistically significant.
All methods were carried out in accordance with relevant guidelines and regulations of Hubei Key Laboratory of Embryonic Stem Cell Research.
3 Results
3.1 TMAO promoted the proliferation of HCC cells
We cultured HepG2 and Huh-7 human HCC cells in vitro and treated these two cell lines with different concentrations of TMAO. The EdU experiment showed that the promoting effect of TMAO on the proliferation of Huh-7 cells was gradually obvious with the extension of culture days. At day 3, the OD value of Huh-7 cells treated with 100 μM TMAO (1.25 ± 0.43) was significantly higher than that of the control group (0 μM TMAO, OD: 0.72 ± 0.21) (Fig. 1A-a). With the increase of TMAO concentration, the OD value of Huh-7 cells was always significantly higher than that of control (Fig. 1A-a). Meanwhile, EdU experiment showed that OD values of HepG2 cells rised significantly with the increase of TMAO concentration (Fig. 1B-a). RTCA showed that TMAO significantly increased the cell index of Huh-7 cells with the prolongation of culture time; at 50 h, the cell indexes of the 600 μM, 200 μM and 0 μM TMAO treatment groups were 7.05 ± 0.23, 7.14 ± 0.52 and 6.11 ± 0.33 respectively (Fig. 1A-b). Also, RTCA showed a similar trend in HepG2 cells (Fig. 1B-b). Colony formation assay displayed that the numbers of colonies formed by the 600 μM TMAO treated HepG2 (395 ± 27) and Huh-7 cells (482 ± 49) were significantly higher than 0 μM TMAO treated HepG2 (196 ± 22) and Huh-7 cells(283 ± 9) (Fig. 1C).These results show that TMAO significantly promotes the proliferation of HCC cells.
TMAO promotes human hepatocellular carcinoma (HCC) cell growth and colony formation. A Huh-7 cells were treated with different concentrations of TMAO, and cell proliferation was measured with EdU assays (a) and RTCA assays (b). B The proliferation of HepG2 cells treated with TMAO was measured with an EdU assay (a) and RTCA (b). C Colony formation assay of HepG2 and Huh-7. All experiments were performed in triplicate. TMAO-treated vs. PBS-treated; *P < 0.05, **P < 0.01
3.2 TMAO promoted the migration of HCC cells
When different concentrations of TMAO were added to the culture medium, the migration distances of Huh-7 (Fig. 2A-a, b) and HepG2 (Fig. 2B-a, b) cells were detected by a wound healing assay, and the results showed that the migration ability of HCC cells was enhanced by increasing TMAO concentrations. The Transwell experiments showed that the number of Huh-7 (Fig. 2A-c, d) and HepG2 (Fig. 2B-c, d) cells that crossed the Transwell chambers significantly increased as the TMAO concentration increased. These results show that TMAO significantly promotes the migration of HCC cells.
TMAO promotes HCC cell migration. A Detection of Huh-7 migration speed by a scratch assay (a), quantitative analysis of migration speed by migration index (b); detection of the migration ability of Huh-7 cells by a Transwell assay (c), statistical analysis of the number of Huh-7 cells passing through the chambers (d). B The migration ability of HepG2 cells was detected by a scratch assay (a), the migration index was quantitatively analyzed (b), the migration ability of HepG2 cells was detected with a Transwell assay (c), and the number of HepG2 cells passing through the chambers was quantitatively analyzed (d). All experiments were performed in triplicate. TMAO-treated vs. PBS-treated; *P < 0.05, **P < 0.01
3.3 TMAO promoted the expression of proteins related to the proliferation and migration of HCC cells
Immunofluorescence was used to detect the expression of the migration-related proteins MMP9 and VEGF in HepG2 cells treated with 400 μM TMAO for 48 h, and the results showed that the fluorescence intensity of the HepG2 cells treated with TMAO was significantly increased compared with that of the control group (Fig. 3A). The Western blot analysis showed that the expression of proliferation- and migration-related proteins in the Huh-7 cells (Fig. 3B) and HepG2 cells (Fig. 3C) was significantly upregulated as the TMAO concentration increased.
Effects of TMAO on the expression of proliferation- and migration-related proteins in hepatocellular carcinoma cells. A The expression of VEGF and MMP9 in HepG2 cells after TMAO treatment was detected by immunofluorescence. B Western blot analysis of PCNA, MMP9 and VEGF expression in Huh-7 cells treated with TMAO. C Western blot analysis was used to detect the expression of PCNA, Ki67 and VEGF in HepG2 cells treated with TMAO. A few strips were clipped before color development because ladder staining strongly affected the display of target proteins. All experiments were performed in triplicate. TMAO-treated vs. PBS-treated; *P < 0.05, **P < 0.01
3.4 TMAO promoted epithelial mesenchymal transformation EMT in HCC cells
During the treatment of HCC cells with TMAO, the morphology of the HCC cells became more elongated, the connections between the cells became looser (Fig. 4A), and the cells showed a trend of EMT The immunofluorescence analysis showed that when treated with 800 μM TMAO, the fluorescence intensity of vimentin expression in the HepG2 cells was significantly higher than that in the control group (Fig. 4B). The Western blot analysis showed that as the TMAO concentration increased, the expression of EMT-related proteins in the Huh-7 cells (Fig. 4C) and HepG2 cells (Fig. 4D) was significantly upregulated. When Huh-7 cells (Fig. 4E) and HepG2 cells (Fig. 4F) were treated with 600 μM and 800 μM TMAO, respectively, the expression intensity of EMT-related proteins significantly increased as the treatment time increased. These results showthat TMAO promots EMT in HCC cells.
Effects of TMAO on the epithelial mesenchymal transformation of hepatocellular carcinoma cells. A Observation of the morphology of HCC cells after treatment with TMAO. B Immunofluorescence detection of vimentin expression in HepG2 cells treated with TMAO. C Western blot analysis was used to detect the expression of EMT-related proteins in Huh-7 cells treated with different concentrations of TMAO. D Western blot analysis of EMT-related protein expression in HepG2 cells treated with different concentrations of TMAO. E Western blot analysis of EMT-related protein expression in Huh-7 cells treated with 600 μmol/L TMAO over time. F Western blot analysis of EMT-related protein expression in HepG2 cells treated with 800 μmol/L TMAO over time. A few strips were clipped before color development because ladder staining strongly affected the display of target proteins. All experiments were performed in triplicate. TMAO-treated vs. PBS-treated; *P < 0.05, **P < 0.01
3.5 TMAO promoted the tumorigenesis and growth of HCC cells in mice
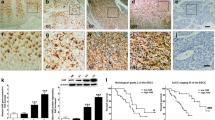
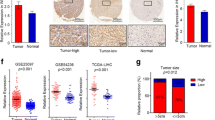
HepG2 cells were inoculated subcutaneously into nude mice given drinking water containing 8 mg/mL TMAO. The subcutaneous tumors were detected every 10 days, indicating that the tumors in the mice given TMAO were significantly larger than those in the control mice (Fig. 5A-b). After 30 days of treatment, the mice were sacrificed, and the subcutaneous tumors were removed. The subcutaneous tumors in the mice given TMAO were significantly larger than those in the control group (Fig. 5A-a). The tumor mass in the mice drinking water with TMAO was significantly heavier than that in the mice drinking normal water (Fig. 5A-c). The immunohistochemical detection showed that the expression of proliferation-, migration- and EMT-related proteins in the tumor tissues of the mice given TMAO was significantly higher than that in the control group (Fig. 5B). The Western blot analysis also showed similar results (Fig. 5C). These results show that TMAO could promote the proliferation, migration and EMT of HCC cells in vivo.
TMAO promotes tumor growth in xenograft mice. A Twenty-five days after HCC cell injection, the mice were euthanized, and the xenograft tumors were collected. The image shows the tumors generated in two different treatment groups (a). Xenograft volumes were monitored at the indicated time (b). Tumor weight was analyzed (c). B PCNA, vimentin, MMP9, VEGF and E-cadherin expression in subcutaneous tumors detected by IHC. C PCNA and EMT-related protein expression in subcutaneous tumors detected by a Western blot analysis. *P < 0.05, **P < 0.01, compared with control
3.6 TMAO activated the mitogen-activated protein kinase (MAPK) pathway in HCC cells
The MAPK signal transduction pathway plays a very important role in mediating cell responses and widely participates in cell growth, migration, division and death and changes in various biochemical reaction signals in cells. The MAPK signaling pathway is mainly composed of the p38 MAPK, c-Jun N-terminal kinase (JNK) and extracellular regulated protein kinases 1/2 (ERK1/2) signaling pathways. In this study, we examined the effect of TMAO on the MAPK signaling pathway in HCC cells to explore the relevant molecular mechanisms. HCC cells were treated with different concentrations of TMAO for 48 h, and proteins were extracted for a Western blot analysis. The results showed that the expression of phosphorylated p38, JNK and ERK in the HepG2 (Fig. 6A) and Huh-7 cells (Fig. 6B) increased with the TMAO concentrations. Additionally, the Western blot assays showed that the expression levels of MAPK pathway proteins in the tumor tissues of the mice given TMAO were significantly higher than those in the control mice (Fig. 6C).
MAPK pathway was activated by TMAO in HCC cells. A The protein levels of p-p38, p38, p-ERK, ERK, p-JNK, and JNK were detected by a Western blot analysis after Huh-7 cells were exposed to 0, 200, 400 and 600 μmol/L TMAO for 48 h. B The protein levels of the MAPK pathway were detected by a Western blot analysis after HepG2 cells were exposed to 0, 200, 400 and 800 μmol/L TMAO for 48 h. C Western blot analysis of MAPK pathway protein expression in subcutaneous tumors from xenograft mice. All experiments were performed in triplicate. *P < 0.05, **P < 0.01, compared with control
4 Discussion
In the past decade, studies have increasingly suggested that the intestinal microbiota is involved in carcinogenesis, and previous studies have also shown the role of diet in regulating the composition of intestinal microbiota [19, 20]. However, the molecular mechanisms by which diet-induced changes in the intestinal microbiota are associated with cancer are still not fully understood. TMAO, an metabolite of the gut flora produced after eating a cholinine-rich diet, may be a potential candidate to explain this relationship. In the first study to explore this association published in 2014, Bae et al. [14] showed that plasma TMAO levels were positively associated with colorectal cancer risk in women in the United States. Except for colorectal cancer, some studies have suggested that TMAO may be related to an incremental risk of other cancers. A cohort study using metabolomics in prostate cancer patients and healthy controls by Mondul et al. in Finland showed that elevated plasma TMAO levels were positively related to the risk of aggressive prostate cancer [21]. In addition, proton nuclear magnetic resonance spectroscopic data demonstrated that plasma TMAO levels in patients with oral squamous cell carcinoma were distinctly higher than those in healthy controls [22]. Furthermore, a recent case–control study showed that elevated serum TMAO levels were related to an incremental risk of HCC [17]. Thus, these studies suggest that the plasma TMAO levels may alter the risk of not only CRC but also other types of cancer. However, these studies are limited to clinical investigations. In this study, we used HCC as an example to study the effects and preliminatively explore mechanisms of TMAO on the proliferation, migration and EMT of hepatoma carcinoma cells in vivo and in vitro.
Although the effects of TMAO on cancer cells are still unknown, TMAO has affected the proliferation and migration of various other cells. In a recent study, TMAO-mediated y-box binding protein-1 nuclear translocation accelerated cell expansion in a cell model of chronic kidney disease by directly downregulating Gadd45a expression to promote cell cycle progression [23]. TMAO promoted macrophage migration and the expression of inflammatory factors [24]. TMAO treatment leaded to proliferation and migration changes in human umbilical vein endothelial cells [25]. Consistent with these studies, in our study, TMAO promoted the proliferation and migration of HCC cells in vitro. After HCC cells were treated with different concentrations of TMAO, experiments (EdU, RTCA and the clonogenesis) showed that the growth rate of HCC cells increased as the TMAO concentration increased. And in fact, the latest research showed that TMAO displayed oncogenic effects by accelerating cell proliferation and angiogenesis in colorectal cancer [26]. Furthermore, in this study, drinking water containing TMAO made subcutaneous tumors grow larger and faster in nude mice. However, the immune system of nude mice is not robust, and recent studies have shown that TMAO promotes antitumor immunity in triple-negative breast cancer and pancreatic cancer [27, 28], so it is necessary to consider various factors in vivo. However, from the in vivo and in vitro experimental results of this study, TMAO can promote the proliferation of simple HCC cells without considering the complex immune environment.
Subsequently, the wound healing and transwell assays demonstrated that the migration ability of HCC cells increased as the TMAO concentration increased. Accordingly, immunofluorescence and Western blot analysis showed that TMAO promoted the expression of proteins related to proliferation and migration in HCC cells. In the experiments, the effects of TMAO on HepG2 and Huh-7 cells were observed when the concentration of TMAO reached 400 μM and 200 μM, respectively, indicating that Huh-7 cells were more sensitive to the action of TMAO.
EMT is a highly conserved cellular process in which epithelial cells lose their polarized organization and attain the ability to migrate and invade [29]. Solid tumor cells lose intercellular adhesion and gain motility through EMT, thus invading adjacent cell layers. Thus, EMT is considered to be a premetastatic cellular event that leads to tumor cell invasion and malignant tumor progression [30]. Epidemiological survey studies offered strong evidence supporting our assumption that TMAO may be related to CRC and HCC pathogenesis [15, 17]. In this study, we further confirmed this hypothesis by analysing the effect of TMAO on EMT in HCC cells in vitro and in vivo. The TMAO-treated HCC cells showed an altered morphology and upregulated Vimentin, Snail and Slug but decreased E-cadherin expression. Additionally, these EMT-related proteins in HCC cells transplanted subcutaneously into nude mice were accordingly regulated by water containing TMAO.
A genome-wide analysis demonstrated that TMAO exhibited to be involved in many genetic pathways obviously implicated in cancer [15]. The MAPK signaling pathway was included in the top ten ranked genetic pathways shared between TMAO and cancer. MAPK is a serine/threonine kinase in cells, and its major members include ERK, p38 MAPK, and JNK [31]. An abnormally activated MAPK signaling pathway is strongly associated with the occurrence, development, invasion and metastasis of HCC [32,33,34]. In this study, to explore the role of TMAO in the MAPK signaling pathway in HCC cells, the protein and phosphorylation levels of key molecules (ERK, p38 and JNK) of the MAPK signaling pathway were determined in HCC cells treated with increasing concentrations of TMAO. Therefore, the observed promoting effect of TMAO on the proliferation, migration and EMT of HCC cells may occur through the activation of the MAPK pathway. The molecular mechanisms involved need to be further explored.
In summary, our study shows that TMAO promotes the proliferation and migration of HCC cells through the activation of the MAPK pathway. This finding suggests that patients with intestinal flora dysregulation or immunosuppression should be more cautious when choosing foods rich in phosphatidylcholine in their diet. Nevertheless, the internal environment is complex, choline-rich foods produce TMAO, but they also provide a wealth of nutrients. TMAO may act as a double-edged sword on tumors in immunocompetent individuals, and the exact mechanism needs to be further studied.
Data availability
All datasets for the analysis in the present study are available upon reasonable request to the corresponding author.
Abbreviations
- HCC:
-
Hepatocellular carcinoma
- HBV:
-
Hepatitis B virus
- HCV:
-
Hepatitis C virus
- NAFLD:
-
Non-alcoholic fatty liver disease
- TMAO:
-
Trimethylamine-n-oxide
- CRC:
-
Colorectal cancer
- RTCA:
-
Real-time cell analysis
- EdU:
-
5-Ethynyl-2ʹ-deoxyuridine
- TMB:
-
3,3ʹ,5,5ʹ-Tetramethylbenzidine
- PCNA:
-
Proliferating cell nuclear antigen
- MMP9:
-
Matrix metalloproteinase-9
- VEGF:
-
Vascular endothlial growth factor
- ERK:
-
Extracellular regulated protein kinases
- JNK:
-
C-Jun N-terminal kinase
- EMT:
-
Epithelial mesenchymal tranformation
References
Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global Cancer Statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71(3):209–49. https://doi.org/10.3322/caac.21660.
Sayiner M, Golabi P, Younossi ZM. Disease burden of hepatocellular carcinoma: a global perspective. Dig Dis Sci. 2019;64(4):910–7. https://doi.org/10.1007/s10620-019-05537-2.
Gnyawali B, Pusateri A, Nickerson A, Jalil S, Mumtaz K. Epidemiologic and socioeconomic factors impacting hepatitis B virus and related hepatocellular carcinoma. World J Gastroenterol. 2022;28(29):3793–802. https://doi.org/10.3748/wjg.v28.i29.3793.
Vogel A, Meyer T, Sapisochin G, Salem R, Saborowski A. Hepatocellular carcinoma. Lancet (London, England). 2022;400(10360):1345–62. https://doi.org/10.1016/S0140-6736(22)01200-4.
Ayares G, Idalsoaga F, Díaz LA, Arnold J, Arab JP. Current medical treatment for alcohol-associated liver disease. J Clin Exp Hepatol. 2022;12(5):1333–48. https://doi.org/10.1016/j.jceh.2022.02.001.
Huang DQ, El-Serag HB, Loomba R. Global epidemiology of NAFLD-related HCC: trends, predictions, risk factors and prevention. Nat Rev Gastroenterol Hepatol. 2021;18(4):223–38. https://doi.org/10.1038/s41575-020-00381-6.
Kim H, Lee DS, An TH, Park HJ, Kim WK, Bae KH, et al. Spectrum of liver failure in type 2 diabetes and obesity: from NAFLD to NASH to HCC. Int J Mol Sci. 2021;22(9):4495. https://doi.org/10.3390/ijms22094495.
Organ CL, Li Z, Sharp TE 3rd, Polhemus DJ, Gupta N, Goodchild TT, et al. Nonlethal inhibition of gut microbial trimethylamine N-oxide production improves cardiac function and remodeling in a murine model of heart failure. J Am Heart Assoc. 2020;9(10): e016223. https://doi.org/10.1161/JAHA.119.016223.
Tanase DM, Gosav EM, Neculae E, Costea CF, Ciocoiu M, Hurjui LL, et al. Role of gut microbiota on onset and progression of microvascular complications of type 2 diabetes (T2DM). Nutrients. 2020;12(12):3719. https://doi.org/10.3390/nu12123719.
Lim YJ, Sidor NA, Tonial NC, Che A, Urquhart BL. Uremic toxins in the progression of chronic kidney disease and cardiovascular disease: mechanisms and therapeutic targets. Toxins (Basel). 2021;13(2):142. https://doi.org/10.3390/toxins13020142.
Coutinho-Wolino KS, de Cardozo LFM, de Oliveira Leal V, Mafra D, Stockler-Pinto MB. Can diet modulate trimethylamine N-oxide (TMAO) production? What do we know so far? Eur J Nutr. 2021;60(7):3567–84. https://doi.org/10.1007/s00394-021-02491-6.
Jalandra R, Dalal N, Yadav AK, Verma D, Sharma M, Singh R, et al. Emerging role of trimethylamine-N-oxide (TMAO) in colorectal cancer. Appl Microbiol Biotechnol. 2021;105(20):7651–60. https://doi.org/10.1007/s00253-021-11582-7.
Chan CWH, Law BMH, Waye MMY, Chan JYW, So WKW, Chow KM. Trimethylamine-N-oxide as one hypothetical link for the relationship between intestinal microbiota and cancer—where we are and where shall we go? J Cancer. 2019;23:5874–82. https://doi.org/10.7150/jca.31737.PMID:31737123;PMCID:PMC6843879.
Bae S, Ulrich CM, Neuhouser ML, Malysheva O, Bailey LB, Xiao L, et al. Plasma choline metabolites and colorectal cancer risk in the Women’s Health Initiative Observational Study. Cancer Res. 2014;74(24):7442–52. https://doi.org/10.1158/0008-5472.CAN-14-1835.
Xu R, Wang Q, Li L. A genome-wide systems analysis reveals strong link between colorectal cancer and trimethylamine N-oxide (TMAO), a gut microbial metabolite of dietary meat and fat. BMC Genomics. 2015;16(Suppl 7):S4. https://doi.org/10.1186/1471-2164-16-S7-S4.
Nian F, Zhu C, Jin N, Xia Q, Wu L, Lu X. Gut microbiota metabolite TMAO promoted lipid deposition and fibrosis process via KRT17 in fatty liver cells in vitro. Biochem Biophys Res Commun. 2023;669:134–42. https://doi.org/10.1016/j.bbrc.2023.05.041.
Liu ZY, Tan XY, Li QJ, Liao GC, Fang AP, Zhang DM, et al. Trimethylamine N-oxide, a gut microbiota-dependent metabolite of choline, is positively associated with the risk of primary liver cancer: a case–control study. Nutr Metab (Lond). 2018;15:81. https://doi.org/10.1186/s12986-018-0319-2.
Wu Y, Rong X, Pan M, Wang T, Yang H, Chen X, et al. Integrated analysis reveals the gut microbial metabolite TMAO promotes inflammatory hepatocellular carcinoma by upregulating POSTN. Front Cell Dev Biol. 2022;10:840171. https://doi.org/10.3389/fcell.2022.840171.
Yu Q, Newsome RC, Beveridge M, Hernandez MC, Gharaibeh RZ, Jobin C, et al. Intestinal microbiota modulates pancreatic carcinogenesis through intratumoral natural killer cells. Gut Microbes. 2022;14(1):2112881. https://doi.org/10.1080/19490976.2022.2112881.
Hullar MA, Burnett-Hartman AN, Lampe JW. Gut microbes, diet, and cancer. Cancer Treat Res. 2014;159:377–99. https://doi.org/10.1007/978-3-642-38007-5_22.
Mondul AM, Moore SC, Weinstein SJ, Karoly ED, Sampson JN, et al. Metabolomic analysis of prostate cancer risk in a prospective cohort: the alpha-tocolpherol, beta-carotene cancer prevention (ATBC) study. Int J Cancer. 2015;137(9):2124–32. https://doi.org/10.1002/ijc.29576.
Bag S, Banerjee DR, Basak A, Das AK, Pal M, Banerjee R, et al. NMR ((1)H and (13)C) based signatures of abnormal choline metabolism in oral squamous cell carcinoma with no prominent Warburg effect. Biochem Biophys Res Commun. 2015;459(4):574–8. https://doi.org/10.1016/j.bbrc.2015.02.149.
Wang L, Zhu N, Jia J, Gu L, Du Y, Tang G, et al. Trimethylamine N-oxide mediated Y-box binding protein-1 nuclear translocation promotes cell cycle progression by directly downregulating Gadd45a expression in a cellular model of chronic kidney disease. Life Sci. 2021;271: 119173. https://doi.org/10.1016/j.lfs.2021.119173.
Geng J, Yang C, Wang B, Zhang X, Hu T, Gu Y, et al. Trimethylamine N-oxide promotes atherosclerosis via CD36-dependent MAPK/JNK pathway. Biomed Pharmacother. 2018;97:941–7. https://doi.org/10.1016/j.biopha.2017.11.016.
Ke Y, Li D, Zhao M, Liu C, Liu J, Zeng A, et al. Gut flora-dependent metabolite Trimethylamine-N-oxide accelerates endothelial cell senescence and vascular aging through oxidative stress. Free Radic Biol Med. 2018;116:88–100. https://doi.org/10.1016/j.freeradbiomed.2018.01.007.
Yang S, Dai H, Lu Y, Li R, Gao C, Pan S. Trimethylamine N-oxide promotes cell proliferation and angiogenesis in colorectal cancer. J Immunol Res. 2022;2022:7043856. https://doi.org/10.1155/2022/7043856.
Mirji G, Worth A, Bhat SA, El Sayed M, Kannan T, Goldman AR, et al. The microbiome-derived metabolite TMAO drives immune activation and boosts responses to immune checkpoint blockade in pancreatic cancer. Sci Immunol. 2022;7(75):eabn0704. https://doi.org/10.1126/sciimmunol.abn0704.
Wang H, Rong X, Zhao G, Zhou Y, Xiao Y, Ma DJ, et al. The microbial metabolite trimethylamine N-oxide promotes antitumor immunity in triple-negative breast cancer. Cell Metab. 2022;34(4):581–5948. https://doi.org/10.1016/j.cmet.2022.02.010.
Diepenbruck M, Christofori G. Epithelial–mesenchymal transition (EMT) and metastasis: yes, no, maybe? Curr Opin Cell Biol. 2016;43:7–13. https://doi.org/10.1016/j.ceb.2016.06.002.
Dong G, Chen P, Xu Y, Liu T, Yin R. Cancer-associated fibroblasts: key criminals of tumor pre-metastatic niche. Cancer Lett. 2023;566: 216234. https://doi.org/10.1016/j.canlet.2023.216234.
Kim EK, Choi EJ. Compromised MAPK signaling in human diseases: an update. Arch Toxicol. 2015;89(6):867–82. https://doi.org/10.1007/s00204-015-1472-2.
Chen L, Guo P, He Y, Chen Z, Chen L, Luo Y, et al. HCC-derived exosomes elicit HCC progression and recurrence by epithelial-mesenchymal transition through MAPK/ERK signalling pathway. Cell Death Dis. 2018;9(5):513. https://doi.org/10.1038/s41419-018-0534-9.
Moon H, Ro SW. MAPK/ERK signaling pathway in hepatocellular carcinoma. Cancers (Basel). 2021;13(12):3026. https://doi.org/10.3390/cancers13123026.
Pang Y, Liu Z, Han H, Wang B, Li W, Mao C, et al. Peptide SMIM30 promotes HCC development by inducing SRC/YES1 membrane anchoring and MAPK pathway activation. J Hepatol. 2020;73(5):1155–69. https://doi.org/10.1016/j.jhep.2020.05.028.
Acknowledgements
We thank members of Hubei Key Laboratory of Embryonic Stem Cell Research for effective discussion, providing significant insights and technical support.
Funding
This work was supported by Natural Science Foundation of Hubei Provincial Department of Education with grant number B2022135, and two National Innovative Training Program with grant number 202110929009 and 201910929018.
Author information
Authors and Affiliations
Contributions
C.F.Z. and R.B. wrote the main text; C.X.Z. and S.N.M. prepared Figs. 1, 2, 4, 5 and 6; X.R.G edited the manuscript; Z.X.W. and Y.H.Y. funding acquisition and supervision. All authors reviewed the manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
The study was approved by the Ethics Committee of Hubei University of Medicine.
Patient consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Zhou, C., Basnet, R., Zhen, C. et al. Trimethylamine N-oxide promotes the proliferation and migration of hepatocellular carcinoma cell through the MAPK pathway. Discov Onc 15, 346 (2024). https://doi.org/10.1007/s12672-024-01178-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12672-024-01178-8