Abstract
Objectives
The Mindful Self-Care Scale-Standard (MSCS-Standard) is a 33-item self-report questionnaire that assesses mindfulness practices in six self-care domains: (1) physical care, (2) mindful relaxation, (3) supportive structure, (4) supportive relationships, (5) mindful awareness, and (6) self-compassion and purpose. The study aimed to validate the Polish version of the MSCS-Standard.
Method
The study was performed on a sample of 774 people (646 females, 122 males, and 6 non-binary) aged 18–76 (M = 28.49, SD = 10.81). The factor structure was verified with confirmatory factor analysis. Convergent and divergent validity were assessed based on the relationship between the MSCS-Standard scores and markers of alexithymia, anxiety, depression, stress, and somatic symptoms as well as life satisfaction. We examined discriminant validity by conducting a second-order exploratory factor analysis of MSCS-Standard subscales, alexithymia traits, anxiety, depression, stress, and somatic symptoms.
Results
Our results indicated a good factorial validity, conforming to the intended 6-factor structure (χ2/df = 1352.38/477; CFI = 0.912; RMSEA = 0.051 [90% CI: 0.048; 0.055]; SRMR = 0.064). As expected, all MSCS-Standard subscales correlated in expected directions with markers of alexithymia, anxiety, depression, stress, and somatic symptoms as well as with life satisfaction. The MSCS-Standard showed a good discriminant validity in terms of measuring mindfulness practices construct that was separable from people’s current levels of alexithymia, negative affect and somatic symptoms. Internal consistency reliability was also good.
Conclusions
Overall, the Polish version of the MSCS-Standard appears to have satisfactory psychometric properties.
Preregistration
This study is not preregistered.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
For many years, self-care was a more medically oriented set of behaviors, solely conceptualized as a person’s ability to complete daily life tasks specific to their own basic functioning (e.g., bathing, taking medicines, dressing, and preparing foods (Cook-Cottone & Guyker, 2018). Generally, researchers focused on how well those with medical or developmental challenges were able to engage in relatively basic self-care activities. Aligned with the more medical conceptualization, the World Health Organization (2022) currently defines self-care as “the ability of individuals, families and communities to promote health, prevent disease, maintain health and to cope with illness and disability with or without the support of a health worker”. Accordingly, in medicine self-care has been associated with patient behaviors in nursing care (Denyes et al., 2001), especially in relation to cardiovascular, autoimmune, dermatological chronic diseases (Chen et al., 2022; Ghio et al., 2020; Krzemińska et al., 2021). More recently, theory, research and practice of self-care has focused on a broader definition of the term inclusive of practices beyond the support the maintenance of basic daily-life functioning related to the prevention and treatment of disease. The significance and potential contributions of self-care assessments and interventions are recognized by the World Health Organization (2022), as prevention diseases and promoting health is crucial. Therefore, facilitating research on self-care, its assessment in general populations, and the development of self-care measures are important. This can contribute to providing informing interventions or improving mental health services.
Self-care has conceptually evolved to include behaviors known to contribute to self-regulation and wellbeing, prevention of physical and mental health disease and disorders, as well as prevention of burnout (Cook-Cottone & Guyker, 2018; Loi & Pryce, 2022). In this broader approach to self-care, physical exercise, relaxation, and other self-nurturing practices are emphasized. Ultimately, in many large-scale studies, this self-nurturing approach to self-care was revealed as a protective factor for physical and mental health problems (Gosnell et al., 2021). Cook-Cottone (2015) built on this self-nurturing approach to self-care integrating mindfulness practices as well as an overarching practice of mindful awareness and assessment of one’s own self-care. This type of self-care is referred to as mindful self-care.
We based our study on Cook-Cottone’s (2015) definition of mindful self-care which refers to the daily process of becoming aware of and attending to basic physiological and emotional needs that involve the component of mindful awareness. Mindful self-care is composed of six components, including (1) physical care, (2) mindful relaxation, (3) supportive structure, (4) supportive relationships, (5) mindful awareness, and (6) self-compassion and purpose (Cook-Cottone & Guyker, 2018). For measuring mindful self-care and its components, the original American version of the Mindful Self-Care Scale (MSCS) by Cook-Cottone and Guyker (2018) was developed. There are three versions of the questionnaire, i.e., an 84-item MSCS-Clinical (Cook-Cottone, 2015), a 33-item MSCS-Standard (Cook-Cottone & Guyker, 2018), and a 24-item MSCS-Brief (Hotchkiss & Cook-Cottone, 2019). The 84-item MSCS-Clinical is designed for assessing self-care behaviours in clinical, educational, or self-care settings and can be used for developing a self-care plan (Cook-Cottone, 2015). Thus, this long scale is designed for personalized and more comprehensive assessments. The MSCS-Standard is a 33-item questionnaire to assess the frequency of mindfulness behaviours related to physical and mental health in the six above-described self-care domains. The 24-item MSCS-Brief was developed through analyzing hospice workers and is aimed at people for whom the clinical or standard versions might be too long (Hotchkiss & Cook-Cottone, 2019).
Compared to other self-care measures for professionals (e.g., healthcare workers) and trainers or people with chronic conditions, the MSCS-Standard can be used in both clinical and non-clinical settings (see reviews on self-care questionnaires, e.g., Biagioli et al. (2022), Hudon et al. (2021), Jiang et al. (2021), Luciani et al. (2022). Moreover, the scale is theoretically grounded and psychometrically sound (Jiang et al., 2021). As the 33-item MSCS-Standard provides a good balance of comprehensiveness and brevity that is suitable for most purposes, including assessing mindful self-care in people from a general population in large-scale studies (Cook-Cottone & Guyker, 2018), we aimed to introduce and validate a first Polish version of the MSCS-Standard.
The MSCS-Standard is a 33-item self-report questionnaire that consists of the following six subscales (with examples of statements): (1) physical care (e.g., “I planned my meals and snacks”), (2) mindful relaxation (e.g., “I did something interpersonal to relax (e.g., connected with friends)”), (3) supportive structure (e.g., “I maintained a manageable schedule”), (4) supportive relationships (e.g., “I felt supported by people in my life”), (5) mindful awareness (e.g., “I had a calm awareness of my body”), and (6) self-compassion and purpose (e.g., “I kindly acknowledged my own challenges and difficulties”). There are also three separate items assessing the individual’s general or more global self-care practices, i.e., (1) “I engaged in a variety of self-care activities”, (2) “I planned my self-care” and (3) “I explored new ways to bring self-care into my life” (Cook-Cottone & Guyker, 2018).
Originally developed in English, the MSCS-Standard has now been translated into several languages, including Chinese (Wong, 2020), Portuguese (Garcia et al., 2022), and Turkish (Aydin Sunbul et al., 2018) versions. In general, these studies indicated that the 6-factor mindful self-care construct was consistently supported empirically in different language versions and the MSCS-Standard, as well as its brief form, appears to have good psychometric properties. The MSCS and its versions are not presently available in Polish, which limits MSCS’s usage in Polish-speaking populations. Therefore, we targeted to validate the Polish version of the MSCS-Standard.
The study aimed to examine the psychometric properties (factor structure, internal consistency reliability, convergent, divergent, and discriminant validity) of the Polish version of the MSCS-Standard. We expected that the 6-factor model would be the most appropriate for the current data. Based on the previous works (Cook-Cottone, 2015; Feng et al., 2019; Preston et al., 2022; Simerly & Blackhart, 2021) indicating that mindful self-care was positively associated with better mental and physical health, we predicted that the MSCS-Standard subscales would be negatively correlated with symptoms of anxiety, depression, stress as well as with somatic symptoms, whereas they would be positively correlated with life satisfaction. As alexithymia is expressed in difficulties identifying and describing one’s own feelings and less attention on one’s own internal emotional states (Preece et al., 2022), we predicted negative correlations between alexithymia traits (especially, externally orientated thinking) and mindful self-care practices. We also expected that the MSCS-Standard subscales would show empirically good discriminant validity against alexithymia traits, mental health symptoms, and somatic complaints (i.e., the MSCS-Standard subscales would be statistically separable from the other variables). The previous studies showed ambiguous results regarding gender differences for MSCS-Standard scores (Archer, 2020; Zeb et al., 2022), therefore we had no specific hypotheses regarding these differences.
Method
Participants
The sample consisted of 774 Polish adults (646 females, 122 males and 6 non-binary) with ages ranging from 18 to 76 (M = 28.49, SD = 10.81) from the general population. Most respondents (45.99%) lived in large cities (above 100,000 inhabitants), 20.80% in towns (from 20,000 to 100,000), 10.08% in small towns (up to 20,000) and 23.13% in villages. Individuals with higher education made up 47.80% of the respondents, with secondary education 49.48%, vocational education 1.16%, and primary education 1.55%. Among the respondents 39.66% were single, 34.24% were living common-law and 26.10% were married.
A sample size of more than 500 participants is generally regarded as very good for factor analytic studies (Mundfrom et al., 2005). Thus, our sample size of 774 people was appropriate for testing of the 33-item MSCS-Standard.
Procedure
The study was conducted in accordance with the Declaration of Helsinki Ethical Principles. The Kazimierz Wielki University Ethics Committee approved the study (No. 1/13.06.2022). It was conducted from June 2022 to November 2022.
Convenience sampling was applied. The participants were recruited via social networks Facebook and Instagram where we had posted links to our online anonymous survey in Google Forms. At the beginning of the survey, a consent form was appended. All participants submitted their written informed consent digitally, and no reimbursement was offered to them for their involvement.
The translation procedure followed the recommendations of the International Test Commission (2017). The English version of the MSCS-Standard was translated into Polish by three independent professional translators and their common Polish translation was developed. Then it was translated back into English, and this back translation was compared with the original version of the MSCS-Standard. Any discrepancies at all stages of translation procedure were discussed with the MSCS-Standard’s developers. The minor discrepancies were verified by bilingual experts, and minor corrections were made appropriately, resulting in the final Polish version administered in this study (see Supplementary Materials). Additionally, two minor corrections for two items of the physical care subscale were made, i.e., adding “per day” in the end of the statements (“I drank at least 6 to 8 cups of water per day”; “I exercised at least 30 to 60 minutes per day”). These corrections were also approved by the developers of the original version of the MSCS-Standard.
Measures
The MSCS-Standard is a 33-item self-report questionnaire designed to measure mindful self-care practices (Cook-Cottone & Guyker, 2018). The scale consists of 6 subscales, i.e., (1) physical care (8 items, e.g., “I planned my meals and snacks”), (2) mindful relaxation (6 items, e.g., “I did something interpersonal to relax (e.g., connected with friends)”), (3) supportive structure (4 items, e.g., “I maintained a manageable schedule”), (4) supportive relationships (5 items, e.g., “I felt supported by people in my life”), (5) mindful awareness (4 items, e.g., “I had a calm awareness of my body”), and (6) self-compassion and purpose (6 items, e.g., “I kindly acknowledged my own challenges and difficulties”). One item is reverse scored. The statements are scored on a 5-point scale ranging from 1 (never (0 days)) to 5 (regularly (6 to 7 days)), with higher scores indicating higher levels of mindful self-care behaviours.
The Patient Health Questionnaire–4 (PHQ–4) by Kroenke et al. (2009) in its Polish version by Larionow and Mudło-Głagolska (2023) is a 4-item questionnaire for measuring anxiety and depressive symptoms in the previous 2 weeks. The PHQ–4 has 2 subscales: anxiety (2 items, e.g., “Not being able to stop or control worrying”) and depression (2 items, e.g., “Little interest or pleasure in doing things”). The total PHQ–4 score can be calculated. The PHQ–4 uses a 4-point Likert scale from 0 (not at all) to 3 (nearly every day), with higher scores indicating higher levels of the symptoms. The Polish version of the PHQ–4 has demonstrated strong psychometric properties, i.e., an intended factor structure, convergent validity, and internal consistency reliability (Larionow & Mudło-Głagolska, 2023).
The Perceived Stress Scale–4 (PSS–4) developed by Cohen et al. (1983) in its Polish version by Kleszczewska et al. (2018) was used for measuring the level of perceived stress during the previous month. The PSS–4 has four statements (e.g., “In the last month, how often have you felt that you were unable to control the important things in your life?”) with 2 reverse scored items. The statements are evaluated on a 4-point Likert scale from 0 (never) to 4 (very often), with higher scores indicating higher levels of stress. The Polish version of the PSS–4 has demonstrated strong psychometric properties (Kleszczewska et al., 2018).
The Perth Alexithymia Questionnaire (PAQ) by Preece at al. (2018) in its Polish version by Larionow, Preece et al. (2022) is a 24-item self-report measure of alexithymia. The PAQ consists of 5 subscales, i.e., (1) Negative-Difficulty identifying feelings (N-DIF; 4 items, e.g., “When I’m feeling bad, I’m puzzled by those feelings”), (2) Positive-Difficulty identifying feelings (P-DIF; 4 items, e.g., “When I’m feeling good, I can’t make sense of those feelings”), (3) Negative-Difficulty describing feelings (N-DDF; 4 items, e.g., “When I’m feeling bad, if I try to describe how I’m feeling I don’t know what to say”), (4) Positive-Difficulty describing feelings (P-DDF; 4 items, e.g., “When something good happens, it’s hard for me to put into words how I’m feeling”) and (5) General-Externally orientated thinking (G-EOT; 8 items, e.g., “I tend to ignore how I feel”) and several composite scores, including a total scale score. Items are scored on a 7-point scale ranging from 1 (strongly disagree) to 7 (strongly agree), with higher scores indicating higher levels of alexithymic traits. The Polish version of the PAQ has demonstrated strong psychometric properties, i.e., factor structure, convergent, divergent and discriminant validity as well as internal consistency and test-retest reliabilities (Larionow, Preece et al., 2022).
The Giessen Subjective Complaints List (GBB–8; Kliem et al., 2017; Petrowski et al., 2022) in its Polish version by Larionow, Mudło-Głagolska et al. (2022) is an 8-item questionnaire for measuring somatic symptoms. The GBB–8 has four 2-item subscales, namely, exhaustion (e.g., being easily exhausted), gastrointestinal (e.g., feeling bloated or distended), musculoskeletal (e.g., backache), and cardiovascular (palpitations or heart pounding). A total score can also be calculated. The GBB–8 uses a 5-point Likert scale from 0 (not at all) to 4 (very much), with higher scores indicating higher levels of somatic symptoms. The Polish version of the GBB–8 has demonstrated strong psychometric properties, i.e., factor structure, convergent and discriminant validity as well as internal consistency and test-retest reliabilities (Larionow, Mudło-Głagolska et al., 2022).
The Cantril ladder approach (Cantril, 1965) was used to assess life satisfaction. The measure in its in Polish version by Kleszczewska et al. (2018) presents a unidimensional scale where respondents rated their current level of life satisfaction. The respondents indicated their position on the ladder from 0 (being the worst possible life satisfaction) to 10 (being the best).
In order to avoid common method bias and fatigue while filling out the questionnaires, not all respondents completed every measure. All participants completed the MSCS-Standard, PHQ–4, PSS–4 and the life satisfaction scale (n = 774). Among respondents, 321 additionally fulfilled the PAQ, and among them 99 respondents also completed the GBB–8. In this study, internal consistency reliability coefficients (i.e., McDonald’s omega reliability estimates) for each psychometric scale and their subscales are displayed in Table 1.
Data Analyses
Statistical analysis was carried out using Statistica version 13.3 and the EFAtools and lavaan statistical packages in R version 4.2.1. The data were screened for accuracy (min. and max. range of each variable). There were no missing data. In order to present precise fit indices and factor loadings in confirmatory and exploratory factor analyses, we used three decimal places, while all other results were reported with two decimal places.
Gender Differences
Due to an unequal sample size of the female and male groups, MSCS-Standard scores gained by females and males were compared by the Mann–Whitney U test and the effect size (η² with the following interpretation: negligible < 0.01 < small < 0.06 < medium < 0.14 < large) was calculated by Psychometrica calculator (Lenhard & Lenhard, 2016).
Factor Structure
We examined a 6-factor correlated model comprised of 6 intended subscales using confirmatory factor analysis with maximum likelihood estimation with robust standard errors and a Satorra-Bentler scaled test statistic. We evaluated the fit based on the following fit index values: root mean square error of approximation (RMSEA), standardized root mean square residual (SRMR), and comparative fit index (CFI). RMSEA and SRMR values below 0.08, and CFI values greater than 0.90 indicate acceptable fit (Hu & Bentler, 1999).
Internal Consistency Reliability
McDonald’s omega (ω) values with 95% confidence intervals were calculated for assessing an internal consistency reliability. Reliability coefficients > 0.70 were considered acceptable, > 0.80 good, and > 0.90 excellent (Groth-Marnat, 2009).
Convergent and Divergent Validity
Pearson correlations between MSCS-Standard scores and PHQ–4 (anxiety and depression), PSS–4 (stress), PAQ (alexithymia), GBB–8 (somatic symptoms) and life satisfaction scores were examined to assess convergent and divergent validity.
Discriminant Validity
Discriminant validity was evaluated by conducting a second-order exploratory factor analysis (based on Pearson correlations with principal axis factoring with direct oblimin rotation) of the 6 MSCS-Standard subscales, the 5 PAQ subscales, the 2 PHQ–4 subscales, the PSS–4 score and the 4 GBB–8 subscales. Before conducting this second-order exploratory factor analysis, the results of Bartlett’s test of sphericity and Kaiser–Meyer–Olkin (KMO) criterion (with acceptable cut-off value > 0.70) were assessed. Parallel analysis based on squared multiple correlations was used to determine the appropriate number of factors to retain (Lim & Jahng, 2019; Watkins, 2018). We expect that the MSCS-Standard subscales would load on a mindful self-care factor, the PAQ subscales on alexithymia factor, and the PHQ–4 and PSS–4 subscales on a separate negative affect factor, and the 4 GBB–8 subscales on a separate somatic symptoms factor, thus supporting discriminant validity.
Results
Table 1 presents descriptive statistics for all the study variables. All 36 MSCS-Standard items (the reverse scored item was recoded) and subscales scores were reasonably normally distributed (skewness values ranged from − 1.22 to 2.01, whereas kurtosis ones ranged from − 1.27 to 3.47).
Gender Differences
There were no differences between females and males in mindful relaxation, physical care and supportive structure scores (all p > 0.05). Self-compassion and purpose (p = 0.012, η² < 0.01) and supportive relationships (p = 0.040, η² < 0.01) were higher in females than in males, whereas mindful awareness was higher in males (p = 0.029, η² < 0.01).
Factor Structure
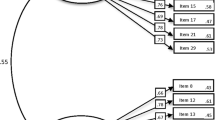
Multivariate normality was assessed by the Henze-Zirkler’s multivariate normality test (HZ = 1.00, p < 0.001), which indicated a lack of multivariate normality of 33 MSCS-Standard items. The 6-factor model fit was satisfactory (χ2/df = 1613.99/480; CFI = 0.885; RMSEA = 0.058 [90% CI: 0.055; 0.061]; SRMR = 0.061), but CFI was unacceptable, because it was lower than 0.90 (Hu & Bentler, 1999). We analysed the modification indices, and added three correlated error terms into the 6-factor model between MSCS-Standard items 19 and 20, between 8 and 9, between 21 and 22. Bollen and Lennox (1991) suggested that errors were typically independent, though the possibility of correlation existed among statements (items) with similar wording or those in close proximity on the questionnaire. In line with this rationale, we found it theoretically reasonable to include these error terms, because of conceptual (Items 8 and 9; Items 21 and 22) and wording similarities (Items 19 and 20) between those statements (Table 2) as well as because these pairs of items appear near to each other on the scale, and these pairs of items are referred to their intended subscales. The addition of these three error terms improved fit index values (χ2/df = 1352.38/477; CFI = 0.912; RMSEA = 0.051 [90% CI: 0.048; 0.055]; SRMR = 0.064). Factor loadings ranged from 0.405 (for Item 7) to 0.904 (for Item 31), except for Item 14 (“I practiced yoga or another mind/body practice (e.g., Tae Kwon Do, Tai Chi)”), which had low loading (0.375) on the intended factor. As descriptive statistics evidenced (Table 2), people’s activity described by Item 14 occurred rarely in the Polish sample. Due to this fact, and due to the loading of Item 14 being slightly lower than the considered meaningful loading of 0.40 or greater (Pituch & Stevens, 2016), we decided to keep Item 14 to maintain the MSCS-Standard integrity for cross-cultural research. The results indicated that the 6-factor model with three error terms was an acceptable fit.
The estimated correlations between MSCS-Standard subscales of the 6-factor model are shown in Table 3. In general, the 5 MSCS-Standard subscales are highly correlated (r from 0.52 to 0.79, all p < 0.001) with each other. The physical care subscale was moderately correlated with the other ones (r from 0.25 to 0.47, all p < 0.001). In sum, confirmatory factor analysis showed the 6-factor model with three error terms presents an intended factor structure of the MSCS-Standard and demonstrates the utility of separating six mindful self-care domains.
Internal Consistency Reliability
The internal consistency reliability of 5 MSCS-Standard subscales was good (ω ≥ 0.79). However, the mindful relaxation subscale had moderate reliability (ω = 0.66; Table 1).
Convergent and Divergent Validity
Pearson correlations between the MSCS-Standard scores and symptoms of anxiety, depression and stress, alexithymia traits, somatic symptoms and life satisfaction were calculated (Table 4). All MSCS-Standard subscales were slightly or moderately negatively correlated with symptoms of anxiety, depression and stress as well as alexithymia traits. The supportive relationships, supportive structure and mindful awareness were moderately correlated with these mental health symptoms and alexithymia. In general, five MSCS subscales were slightly negatively correlated with individual somatic symptoms. All MSCS-Standard subscales were positively correlated with life satisfaction. In sum, these results support good convergent and divergent validity of the questionnaire.
Discriminant Validity
The Bartlett’s test of sphericity was significant (χ²(153) = 1148.51, p < 0.001), and the overall KMO value for our data was meritorious (0.83), indicating that the data were suitable for factor analysis. Parallel analysis, which was performed using 1000 simulated random data sets, revealed that 4 factors should be retained. Therefore, we evaluated a 4-factor solution by applying a second-order exploratory factor analysis of the 6 MSCS-Standard subscales, anxiety, and depressive symptoms (the 2 PHQ–4 subscales), stress (the PSS–4 score), alexithymia traits (the 5 PAQ subscales) and four somatic symptoms (the 4 GBB–8 subscales). All these scores were reasonably normally distributed (skewness from − 0.59 to 0.82, kurtosis from − 1.27 to 0.20).
Our second-order exploratory factor analysis extracted four factors (i.e., Factor 1 “alexithymia”, Factor 2 “mindful self-care”, Factor 3 “negative affect” and Factor 4 “somatic symptoms”; Table 5). As expected, all MSCS-Standard subscales loaded precisely on the “mindful self-care” factor and did not load on the “alexithymia”, “negative affect” and “somatic symptoms” factors, thus supporting good discriminant validity of the MSCS-Standard.
Discussion
The study aimed to validate the MSCS-Standard in Polish and to demonstrate its psychometric properties. As anticipated, our findings revealed that the Polish version of the MSCS-Standard was characterized by an intended 6-factor structure. It is in line with the previous studies on the MSCS-Standard conducted in other cultures, e.g., in the original study (Cook-Cottone & Guyker, 2018) or Turkish sample (Aydin Sunbul et al., 2018). We indicated that Item 14 (“I practiced yoga or another mind/body practice (e.g., Tae Kwon Do, Tai Chi)”) had relatively low loading (0.375) on the intended factor, which may be explained by several reasons. Firstly, in our sample, people’s activity described by this item occurred rarely (see Table 2 with descriptive statistics), which may be considered as a potential cultural factor impacting the cross-cultural validation of the scale. Secondly, as indicated by Archer (2020), this activity seems to be more closely associated with mindful engagement when compared to physical activity, therefore, conceptual inconsistency may be considered as a reason of this low factor loading. In the studies by Archer (2020) and Cabral et al. (2021), Item 14 was recommended for deletion, because of its low factor loading on an intended factor. In contrast, in the original (Cook-Cottone & Guyker, 2018), Turkish (Aydin Sunbul et al., 2018), and the Brazilian-Portuguese versions (Garcia et al., 2022), Item 14 had a considerable factor loading. Due to these mixed results and considering increasing spreading of mindful practices among general populations, we decided to keep Item 14 to maintain the MSCS-Standard integrity for cross-cultural research.
In general, the internal consistency reliability of the MSCS-Standard and its 5 subscales was good, and only the mindful relaxation subscale had moderately lower yet satisfactory reliability (ω = 0.66). The 6-factor model of the Polish MSCS-Standard is an intended and theoretically grounded solution, which demonstrates the utility of separating six mindful self-care domains. This aligns with the findings observed in other cultural samples across five continents (Hotchkiss et al., 2023).
The results of the MSCS-Standard convergent and divergent validity were in line with the expectations. All MSCS-Standard subscales were negatively correlated with anxiety, depression, and stress symptoms as well as with alexithymia, and were positively correlated with life satisfaction. All MSCS-Standard subscales (except mindful relaxation) were negatively correlated with individual somatic symptoms. These results indicate that higher levels of mindful self-care practices are related to experiencing fewer mental health and somatic symptoms and to a greater life satisfaction. Our results are in line with the previous studies on the MSCS (Archer, 2020; Aydin Sunbul et al., 2018; Chatterjee & Jethwani, 2020; Hotchkiss, 2018; Hotchkiss & Cook-Cottone, 2019; Simerly & Blackhart, 2021). We also examined the relationship between mindful self-care and alexithymia as a relatively stable trait which is characterized by difficulty appraising feelings and by externally orientated thinking. As expected, alexithymia was negatively correlated with all MSCS-Standard subscales, especially supportive structure, and mindful awareness. Being a transdiagnostic factor of psychopathology, alexithymia may lead to mental health problems through emotion regulation difficulties (Preece et al., 2022). Our results showed that this trait is related to the decrease in mindful self-care practices, probably, through a reduced ability to focus on one’s own emotional states (in terms of mindful self-care construct through low levels of mindful awareness), which makes it difficult to understand and meet one’s needs. This relationship might also help explain, in part the mechanism involved in the MSCS’s negative correlations with eating disorder measures (Cook-Cottone & Guyker, 2018). Given these findings, alexithymia may be considered a negative predictor of mindful self-care practices. Nevertheless, future studies are requested to examine this mechanism empirically.
Our second-order exploratory factor analysis showed that the six MSCS-Standard subscales were statistically separable from the level of negative affect (anxiety, depression and stress symptoms), alexithymia traits and somatic symptoms, supporting good discriminant validity, which was examined empirically in this study for the first time. Therefore, we could not make comparisons with other findings.
In our study, we also examined gender differences. To the best of our knowledge, there are two reports which used the MSCS-Standard and provided gender differences (Archer, 2020; Zeb et al., 2022). Archer (2020) reported that males had higher physical care and mindful awareness scores, but they reported lower engagement in mindful relaxation than females. In contrast, Zeb et al. (2022) showed that female nurses had higher levels of mindful self-care than male ones. Our results indicated some gender differences in MSCS-Standard scores (higher levels of self-compassion and purpose and supportive relationships in females, and higher levels of mindful awareness in males), but they are characterized by negligible effect sizes. Based on different self-care studies and questionnaires, females tend to care more about their health than males (Ragonese et al., 2019; Senay et al., 2010). For example, the mean of specific self-care behaviours for common colds by primary care patients (Hoffman et al., 2021) or heart failure patients (Abe et al., 2019) was higher in females than in males. In contrast, numerous medical studies showed no gender differences in self-care in several diseases (Heo et al., 2008; Lee et al., 2009; Lerma et al., 2021; Riegel et al., 2010). To sum up, although there were some gender differences in mindful self-care in our study, the effect sizes of these differences were negligible.
All in all, our study supports the results on the six-factor mindful self-care construct and cross-cultural validity of the MSCS-Standard conducted in other cultures (Aydin Sunbul et al., 2018; Chatterjee & Jethwani, 2020; Garcia et al., 2022; Hotchkiss & Cook-Cottone, 2019; Simerly & Blackhart, 2021; Wong, 2020). Overall, the Polish version of the MSCS-Standard appears to be useful tool for comprehensively measuring the multidimensional mindful self-care construct. The scale has a theoretically congruent factor structure, has a high internal consistency reliability, and shows good convergent, divergent and discriminant validity. Our findings add to the growing body of literature supporting the multidimensional structure of the mindful self-care construct and the validity of the MSCS-Standard.
Limitations and Future Research
Several limitations should be noted. Our study took place in a broad general sample of adults with a wide range of ages; however, females and in general younger people were predominated in our sample. As our sample consisted of people aged from 18 to 76 years, and only small percentage of people were older adults, we were unable to examine psychometrics of the scale in older adults’ population. Hence, future research is required to assess the universality of our findings. We did not test the MSCS-Standard in clinical or professional (i.e., healthcare workers) samples, and did not provide the test–retest reliability of the questionnaire. We also did not examine concurrent validity, due to the absence of other Polish-language versions of established self-care measures used for non-clinical research. This is a cross-sectional study; therefore, no conclusions can be drawn regarding the temporal order of mindful self-care practices and their correlates. In general, our results reflected the strengths of the Polish version of the MSCS-Standard and presented a good support for conducting the studies in diverse settings.
Data Availability
All data are available at the Open Science Framework (osf.io/xkje9).
References
Abe, R., Sakata, Y., Nochioka, K., Miura, M., Oikawa, T., Kasahara, S., Sato, M., Aoyanagi, H., Shiroto, T., Sugimura, K., Takahashi, J., Miyata, S., & Shimokawa, H. (2019). Gender differences in prognostic relevance of self-care behaviors on mortality and hospitalization in patients with heart failure - A report from the CHART-2 study. Journal of Cardiology, 73(5), 370–378. https://doi.org/10.1016/j.jjcc.2018.11.006
Archer, C. (2020). A further validation of the mindful self-care scale in emerging adults. Electronic Theses and Dissertations. 2425. https://digitalcommons.memphis.edu/etd/2425
Aydin Sunbul, Z., Malkoc, A., Aslan Gordesli, M., Arslan, R., & Cekici, F. (2018). Mindful self-care scale (MSCS): Adaptation and validation in a normative Turkish sample. European Journal of Educational Research, 7(4), 887–892. https://doi.org/10.12973/eu-jer.7.4.887
Biagioli, V., Spitaletta, G., Kania, V., Mascolo, R., Gawronski, O., Liburdi, A., Manzi, G., Salata, M., Vellone, E., Tiozzo, E., & Dall’Oglio, I. (2022). Instruments measuring self-care in children and young adults with chronic conditions: A systematic review. Frontiers in Pediatrics, 10, 832453. https://doi.org/10.3389/fped.2022.832453
Bollen, K., & Lennox, R. (1991). Conventional wisdom on measurement: A structural equation perspective. Psychological Bulletin, 110(2), 305–314. https://doi.org/10.1037/0033-2909.110.2.305
Cabral, J., Barreto Carvalho, C., da Motta, C., Rodrigues, J. P., Pato, C., & Castilho, P. (2021). Mindful Self-Care Scale (MSCS): Psychometric study in a Portuguese sample. SelfCare Journal, 12(2), 1–11.
Cantril, H. (1965). The pattern of human concerns. Rutgers University Press.
Chatterjee, S., & Jethwani, J. (2020). A study of the relationship between mindful self-care and subjective well-being among college students and working professionals. International Journal of Innovative Research in Technology, 7(2), 417–425.
Chen, T., Kao, C., Cheng, S., & Chang, Y. (2022). A web-based self‐care program to promote healthy lifestyles and control blood pressure in patients with primary hypertension: A randomized controlled trial. Journal of Nursing Scholarship, 54(6), 678–691. https://doi.org/10.1111/jnu.12792
Cohen, S., Kamarck, T., & Mermelstein, R. (1983). A Global measure of perceived stress. Journal of Health and Social Behavior, 24(4), 385–396. https://doi.org/10.2307/2136404
Cook-Cottone, C. P. (2015). Mindfulness and yoga for self-regulation: A primer for mental health professionals. Springer.
Cook-Cottone, C. P., & Guyker, W. M. (2018). The development and validation of the mindful self-care scale (MSCS): An assessment of practices that support positive embodiment. Mindfulness, 9(1), 161–175. https://doi.org/10.1007/s12671-017-0759-1
Denyes, M. J., Orem, D. E., & Bekel, G. (2001). Self-Care: A foundational science. Nursing Science Quarterly, 14(1), 48–54. https://doi.org/10.1177/089431840101400113
Feng, X., Mosimah, C. I., Sizemore, G., Goyat, R., & Dwibedi, N. (2019). Impact of mindful self-care and perceived stress on the health related quality of life among young-adult students in West Virginia. Journal of Human Behavior in the Social Environment, 29(1), 26–36. https://doi.org/10.1080/10911359.2018.1470953
Garcia, A., Silva, L., Ferreira, A., Conceição, V., Meireles, E., & Mills, J. (2022). Translation, cultural adaptation, and validation of the mindful self-care scale among Brazilian palliative care providers. Palliative and Supportive Care, 20(6), 839–845. https://doi.org/10.1017/S1478951521001802
Ghio, D., Muller, I., Greenwell, K., Roberts, A., McNiven, A., Langan, S. M., & Santer, M. (2020). It’s like the bad guy in a movie who just doesn’t die: A qualitative exploration of young people’s adaptation to eczema and implications for self-care. The British Journal of Dermatology, 182(1), 112–118. https://doi.org/10.1111/bjd.18046
Gosnell, N. M., O’Neal, C. R., & Atapattu, R. (2021). Stress, mental health, and self-care among refugee teachers in Malaysia. Asian American Journal of Psychology, 12(3), 176–192. https://doi.org/10.1037/aap0000249
Groth-Marnat, G. (2009). Handbook of psychological assessment (5th ed.). Wiley.
Heo, S., Moser, D. K., Lennie, T. A., Riegel, B., & Chung, M. L. (2008). Gender differences in and factors related to self-care behaviors: A cross-sectional, correlational study of patients with heart failure. International Journal of Nursing Studies, 45(12), 1807–1815. https://doi.org/10.1016/j.ijnurstu.2008.05.008
Hoffman, R. D., Thielmann, A., Buczkowski, K., Edirne, T., Hoffmann, K., Koskela, T., Lingner, H., Mevsim, V., Tekiner, S., Zielinski, A., Hoffman Cicurel, N., Petrazzuoli, F., Thulesius, H., Gerasimovska Kitanovska, B., & Weltermann, B. (2021). Gender differences in self-care for common colds by primary care patients: A European multicenter survey on the prevalence and patterns of practices (the COCO study). Journal of Gender Studies, 30(7), 756–771. https://doi.org/10.1080/09589236.2020.1843010
Hotchkiss, J. T. (2018). Mindful self-care and secondary traumatic stress mediate a relationship between compassion satisfaction and burnout risk among hospice care professionals. The American Journal of Hospice & Palliative Care, 35(8), 1099–1108. https://doi.org/10.1177/1049909118756657
Hotchkiss, J. T., & Cook-Cottone, C. P. (2019). Validation of the mindful self-care scale (MSCS) and development of the Brief-MSCS among hospice and healthcare professionals: A confirmatory factor analysis approach to validation. Palliative & Supportive Care, 17(6), 628–636. https://doi.org/10.1017/S1478951519000269
Hotchkiss, J. T., Cook-Cottone, C. P., Wong, M. Y. C., Guyker, W., & Garcia, A. C. M. (2023). Intercultural validation of the mindful self-care scale—Rasch and factor analysis of 16 studies representing five continents. Mindfulness, 14(8), 2055–2072. https://doi.org/10.1007/s12671-023-02196-3
Hu, L. T., & Bentler, P. M. (1999). Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Structural Equation Modeling, 6, 1–55. https://doi.org/10.1080/10705519909540118
Hudon, É., Hudon, C., Lambert, M., Bisson, M., & Chouinard, M. C. (2021). Generic self-reported questionnaires measuring self-management: A scoping review. Clinical Nursing Research, 30(6), 855–865. https://doi.org/10.1177/1054773820974149
International Test Commission (2017). The ITC guidelines for translating and adapting tests (2nd ed.). https://www.intestcom.org/
Jiang, X., Topps, A. K., & Suzuki, R. (2021). A systematic review of self-care measures for professionals and trainees. Training and Education in Professional Psychology, 15(2), 126–139. https://doi.org/10.1037/tep0000318
Kleszczewska, D., Mazur, J., Dzielska, A., Michalska, A., Gaspar de Matos, M., Santos, T., Gaspar, T., Branquinho, C., Inês Antão, M., & Guedes, F. (2018). Improve the youth. Zdrowie psychiczne młodzieży. Raport z badań [Improve the youth. Mental health of adolescents. Research report]. Instytut Matki i Dziecka.
Kliem, S., Lohmann, A., Klatt, T., Mößle, T., Rehbein, F., Hinz, A., Beutel, M., & Brähler, E. (2017). Brief assessment of subjective health complaints: Development, validation and population norms of a brief form of the Giessen subjective complaints list (GBB-8). Journal of Psychosomatic Research, 95, 33–43. https://doi.org/10.1016/j.jpsychores.2017.02.003
Kroenke, K., Spitzer, R. L., Williams, J. B., & Löwe, B. (2009). An ultra-brief screening scale for anxiety and depression: the PHQ-4. Psychosomatics, 50, 613–621. https://doi.org/10.1176/appi.psy.50.6.613
Krzemińska, S., Lomper, K., Chudiak, A., Ausili, D., & Uchmanowicz, I. (2021). The association of the level of self-care on adherence to treatment in patients diagnosed with type 2 diabetes. Acta Diabetologica, 58(4), 437–445. https://doi.org/10.1007/s00592-020-01628-z
Larionow, P., & Mudło-Głagolska, K. (2023). The Patient Health Questionnaire-4: Factor structure, measurement invariance, latent profile analysis of anxiety and depressive symptoms and screening results in Polish adults. Advances in Cognitive Psychology, 19(2), 123–137. https://doi.org/10.5709/acp-0391-2
Larionow, P., Mudło-Głagolska, K., & Michalak, M. (2022). Towards psychosomatic medicine: Psychometric properties of the Polish version of the Giessen subjective complaints list (GBB-8) and the prevalence of somatic symptoms in a Polish community sample. Annales Universitatis Mariae Curie-Skłodowska Sectio J Paedagogia-Psychologia, 35(4), 117–138. https://doi.org/10.17951/j.2022.35.4.117-138
Larionow, P., Preece, D. A., & Mudło-Głagolska, K. (2022). Assessing alexithymia across negative and positive emotions: Psychometric properties of the Polish version of the Perth Alexithymia questionnaire. Frontiers in Psychiatry, 13, 1047191. https://doi.org/10.3389/fpsyt.2022.1047191
Lee, C. S., Riegel, B., Driscoll, A., Suwanno, J., Moser, D. K., Lennie, T. A., Dickson, V. V., Cameron, J., & Worrall-Carter, L. (2009). Gender differences in heart failure self-care: A multinational cross-sectional study. International Journal of Nursing Studies, 46(11), 1485–1495. https://doi.org/10.1016/j.ijnurstu.2009.04.004
Lenhard, W., & Lenhard, A. (2016). Computation of effect sizes. https://doi.org/10.13140/RG.2.2.17823.92329
Lerma, C., Lima-Zapata, L. I., Amaya-Aguilar, J. A., Leonardo-Cruz, I., Lazo-Sánchez, M., Bermúdez, L. A., Pérez-Grovas, H., Lerma, A., & Cadena-Estrada, J. C. (2021). Gender-specific differences in self-care, treatment-related symptoms, and quality of life in hemodialysis patients. International Journal of Environmental Research and Public Health, 18(24), 13022. https://doi.org/10.3390/ijerph182413022
Lim, S., & Jahng, S. (2019). Determining the number of factors using parallel analysis and its recent variants. Psychological Methods, 24(4), 452–467. https://doi.org/10.1037/met0000230
Loi, N. M., & Pryce, N. (2022). The role of mindful self-care in the relationship between emotional intelligence and burnout in university students. The Journal of Psychology, 156(4), 295–309. https://doi.org/10.1080/00223980.2022.2045887
Luciani, M., De Maria, M., Page, S. D., Barbaranelli, C., Ausili, D., & Riegel, B. (2022). Measuring self-care in the general adult population: Development and psychometric testing of the self-care inventory. BMC Public Health, 22(1), 598. https://doi.org/10.1186/s12889-022-12913-7
Mundfrom, D. J., Shaw, D. G., & Ke, T. L. (2005). Minimum sample size recommendations for conducting factor analyses. International Journal of Testing, 5(2), 159–168. https://doi.org/10.1207/s15327574ijt0502_4
Petrowski, K., Zenger, M., Schmalbach, B., Bastianon, C. D., & Strauss, B. (2022). Psychometric properties and validation of the English version Giessen subjective complaints list (GBB-8). BMC Psychology, 10, 60. https://doi.org/10.1186/s40359-022-00741-8
Pituch, K. A., & Stevens, P. (2016). Applied multivariate statistics for the social sciences (6th ed.). Routledge.
Preece, D., Becerra, R., Robinson, K., Dandy, J., & Allan, A. (2018). The psychometric assessment of alexithymia: Development and validation of the Perth Alexithymia questionnaire. Personality and Individual Differences, 132, 32–44. https://doi.org/10.1016/j.paid.2018.05.011
Preece, D. A., Mehta, A., Becerra, R., Chen, W., Allan, A., Robinson, K., Boyes, M., Hasking, P., & Gross, J. J. (2022). Why is alexithymia a risk factor for affective disorder symptoms? The role of emotion regulation. Journal of Affective Disorders, 296, 337–341. https://doi.org/10.1016/j.jad.2021.09.085
Preston, P. J., Sanchez, D., & Preston, K. S. J. (2022). Exploring mindful self-care as a potential mediator between compassion satisfaction and compassion fatigue among student services professionals. Trauma Care, 2(4), 535–549. https://doi.org/10.3390/traumacare2040044
Ragonese, C., Shand, T., & Barker, G. (2019). Masculine norms and men’s Health. Making the Connections. Promundo-US.
Riegel, B., Dickson, V. V., Kuhn, L., Page, K., & Worrall-Carter, L. (2010). Gender-specific barriers and facilitators to heart failure self-care: A mixed methods study. International Journal of Nursing Studies, 47(7), 888–895. https://doi.org/10.1016/j.ijnurstu.2009.12.011
Senay, E., & Waters, R. (2010). From boys to men: A woman’s guide to the health of husbands, partner. Simon and Schuster.
Simerly, G., & Blackhart, G. (2021). Effects of self-care on undergraduate stress. Undergraduate Journal of Psychology, 32(1), 20–30.
Watkins, M. W. (2018). Exploratory factor analysis: A guide to best practice. Journal of Black Psychology, 44(3), 219–246. https://doi.org/10.1177/0095798418771807
Wong, M. Y. C. (2020). Translation and validation of the mindful self-care scale—Chinese version: A pilot study. Psych, 2(4), 338–346. https://doi.org/10.3390/psych2040025
World Health Organization. (2022). WHO guideline on self-care interventions for health and well-being, 2022 revision. World Health Organization.
Zeb, H., Arif, I., & Younas, A. (2022). Mindful self-care practice of nurses in acute care: A multisite cross-sectional survey. Western Journal of Nursing Research, 44(6), 540–547. https://doi.org/10.1177/01939459211004591
Acknowledgements
The authors would like to thank the editors and reviewers of this paper for their recommendations, and the participants of this study for their effort.
Funding
No funds, grants, or other support was received.
Author information
Authors and Affiliations
Contributions
PL: designed and executed the study, collected and analyzed the data, wrote, reviewed, and edited the manuscript, as well as administered the research project. CC-C: collaborated with the writing and editing of the final manuscript. NP: designed and executed the study, collected the data and assisted with the data analyses, as well as wrote the manuscript. All author approved the final version of the manuscript for submission.
Corresponding author
Ethics declarations
Conflict of Interest
The authors have no relevant financial or non-financial interests to disclose.
Ethics Statement
The study was conducted in accordance with the Declaration of Helsinki Ethical Principles. The Kazimierz Wielki University Ethics Committee approved the study (No. 1/13.06.2022).
Informed Consent
All respondents provided their written informed consent digitally before they answered the questions. There was no reimbursement for the participants.
Use of Artificial Intelligence
AI was not used.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Larionow, P., Cook-Cottone, C. & Pilarska, N. Psychometric Properties of the Polish Version of the Mindful Self-Care Scale-Standard. Mindfulness 15, 435–446 (2024). https://doi.org/10.1007/s12671-023-02282-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12671-023-02282-6