Abstract
Objectives
Interventions involving kindness- and compassion-based meditation (KCBM) have been shown to have various benefits for adults, and there is growing interest in using KCBMs with children. This systematic review explores the effects of KCBM on wellbeing, prosociality, and cognitive functioning in children and adolescents.
Methods
Studies were eligible if they examined interventions that contained a proportion of KCBM above a set threshold, included child participants only, used any or no control group, and included at least one outcome measure related to wellbeing, prosociality, or cognitive functioning. Studies were assessed for quality using the Quality Assessment Tool for Quantitative Studies, and findings were synthesised narratively.
Results
A systematic literature search of 11 databases up to February 2020 identified 3,073 papers. Ten studies were eligible for inclusion in the review, including 807 children. There was evidence of improvements in wellbeing in 47% of wellbeing outcome measures (including stress, anxiety, depression, negative affect, markers of inflammation, mindfulness, and self-compassion). Prosociality and cognitive functioning (visual perception and motor accuracy) were examined in 1 study each, and there was evidence of improvements in both outcomes. Effect sizes ranged from small to large. There was some evidence that interventions were more effective with younger, non-clinical populations and where intervention teachers were experienced. Study quality was generally weak.
Conclusions
There was no strong evidence base for positive effects of KCBM with children. However, the findings of the review are encouraging given the early stage of development of the field, and further research is warranted. Recommendations for future research include more robust methodological design, improved reporting, and a focus on developmental mechanisms of change.
Systematic Review Registration
PROSPERO CRD42014013065.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Mindfulness meditation and mindfulness-based interventions (MBIs) have been linked to positive mental health outcomes in adults (Goldberg et al., 2022; Khoury et al., 2015) and to improvements in wellbeing and cognition in children (Dunning et al., 2019; Mak et al., 2018), and are increasingly being used to enhance mental health and wellbeing. More recently, research attention has turned to the potential benefits of related meditation practices that aim to cultivate prosocial emotions and behaviours such as empathy (feeling and understanding another’s emotions), kindness (acting out of genuine concern for another), and compassion (being aware of suffering and being motivated to alleviate and prevent it). Two of the most common examples of such practices are Loving-Kindness Meditation (LKM) and Compassion Meditation (CM; a variant of LKM directed towards those who are suffering). In these different but related practices, the practitioner aims to cultivate kindness and compassion by calling to mind various individuals and silently offering phrases of well-wishing to them, for example, “may you be happy” in LKM, or “may you be free from suffering” in CM (Hofmann et al., 2011; Salzberg, 1995).
Kindness- and compassion-based interventions (KCBIs) have been shown to improve adults’ health, psychological wellbeing, and interpersonal relationships (Galante et al., 2014; Shonin et al., 2015) and to impact positively on prosociality in non-clinical adult samples, for example, improving affective empathy, perspective-taking, empathic accuracy, empathic concern, compassion, altruism, and prosocial behaviour (e.g. Böckler et al., 2018; Mascaro et al., 2013). Given the positive effects of MBIs on outcomes in children, and the reported benefits of KCBIs for adults, there may be potential for KCBIs to promote wellbeing in children.
The wellbeing of children is an increasing concern (Greenberg & Harris, 2012; Weare, 2015). Around 10% of children aged 5–16 in the UK meet diagnostic criteria for a mental health problem (Mental Health Foundation, 2020), half of lifetime mental illness is established by age 14 (Kessler et al., 2005), and the number of young people attempting suicide is rising (Weare, 2015). Poor mental health in children has negative implications for both physical health and academic achievement (Burstow et al., 2014; Welford & Langmead, 2015); for example, children with greater wellbeing and better mental health achieve higher exam results (Weare, 2015).
One way to enhance wellbeing is via prosocial behaviour—voluntary behaviour intended to benefit another (Eisenberg, 1986). Prosocial behaviour, as well as having positive effects for the beneficiary, has been shown to produce a range of health and wellbeing benefits for the prosocial actor, in both adults (Curry et al., 2018; Nelson et al., 2016) and children (Aknin, Hamlin, et al., 2012; Schreier et al., 2013). Children who are prosocial are less likely to bully others, are less likely to be bullied themselves, and are more likely to be socially accepted and have more friends, protecting them against mental health problems (Bukowski et al., 2010; Layous et al., 2012). Reducing bullying is an important aim, given that bullying is a major contributor to the risk of mental health problems in childhood, and to poor physical and mental health, and poor social outcomes in adulthood (Lereya et al., 2013; Wolke et al., 2013). Prosocial behaviour has also been shown to predict higher academic achievement at both the individual and classroom level (Bergin, 2015; Layous et al., 2012). Wellbeing, in turn, has been shown to promote prosociality, resulting in a positive feedback loop between wellbeing and prosociality (Aknin, Dunn, et al., 2012; Layous et al., 2012) which, along with the contagious nature of altruism (Fowler & Christakis, 2010), has led to calls to promote prosociality as a public health initiative to enhance societal wellbeing (Galante et al., 2014). Wellbeing, academic achievement, and prosociality, then, are important outcomes in childhood. Given their interrelated nature, interventions aiming to promote any of these outcomes have the potential to impact positively on the others, creating a virtuous circle.
Within developmental psychology, there are compelling reasons to explore the potential beneficial effects of KCBIs for children. Some theorists suggest KCBIs may support the development of cognitive and emotional capacities such as attention, emotional awareness and regulation, affective empathy, and perspective-taking (which are thought to contribute to prosocial behaviour, mental wellbeing, and academic success), and that childhood may offer a valuable window to support development of these processes, given the plasticity of children’s brains in childhood and adolescence (Mind and Life Education Research Network, 2012; Roeser & Pinela, 2014). Research suggests that the neural processes underlying attention and prosociality are malleable and that KCBIs can be effective in producing such changes (Singer & Engert, 2019; Weng et al., 2018).
Recent systematic reviews of research on KCBIs have reported benefits including enhanced emotional wellbeing, mindfulness, compassion, self-compassion, and interpersonal skills, in both clinical and non-clinical populations (Galante et al., 2014; Kirby et al., 2017; Shonin et al., 2015). The reviews by Galante et al. (2014) and Kirby et al. (2017) were limited to adult populations, and although Shonin et al. (2015) included both adults and children in their review, only two of the 20 studies included in their review examined effects on children and the authors did not offer distinct conclusions for adults and children, making it difficult to draw conclusions about the effects of KCBIs on wellbeing in children.
Two recent systematic reviews have explored effects of various forms of meditation on prosociality. Kreplin et al. (2018) found a positive effect on empathy and compassion, but no effect on aggression, prejudice, and connectedness in adults. Luberto et al. (2018) conducted a similar review but included both adults and children. They found positive effects on at least one prosocial outcome in 22 out of 26 studies. However, like Shonin et al. (2015), they did not offer separate conclusions according to whether participants were adults or children. Cheang et al. (2019), in a systematic review of the effects of MBIs (which included LKM and CM) on empathy and compassion in children, found evidence for increases in empathy and self-compassion. Although this review included outcome measures of prosocial behaviour in order to infer empathy, prosocial behaviour was not included in their search strategy, and therefore we cannot draw conclusions about the effects of MBIs on prosocial behaviour from this review, since key studies may not have been included.
Another obstacle to drawing conclusions about the effects of KCBIs on prosociality is that reviews on this topic have included MBIs, KCBIs, and interventions that combined the two, without separating results according to the type of intervention, making it difficult to differentiate the effects of these interventions (Cheang et al., 2019; Kreplin et al., 2018; Luberto et al., 2018). The intentions and instructions for mindfulness meditation and kindness- and compassion-based meditation (KCBM) are distinct, and there is evidence for differential effects, mechanisms, and related physiology and neurophysiology (Lee et al., 2012; Singer & Engert, 2019). If KCBIs have a greater effect on prosociality than MBIs, as some recent research indicates (Böckler et al., 2018; Trautwein et al., 2020), then combining these interventions in review syntheses and meta-analyses could downplay the effects of KCBIs on prosocial behaviour. Indeed, Kreplin et al. (2018) noted in their review that the studies examining effects on compassion (where positive effects were found) tended to use LKM or CM, whereas the studies examining aggression, prejudice, and connectedness (where no positive effects were found) tended to use mindfulness-based meditation. Similarly, Cheang et al. (2019) noted that seven of the 10 studies in their review showing increases in empathy, and four of the five studies showing increases in self-compassion, included a compassion element in the intervention, and suggested that explicit training in compassion, as opposed to mindfulness alone, may be needed to cultivate empathy and compassion.
There were no studies that appeared in all three of the systematic reviews that included children (Cheang et al., 2019; Luberto et al., 2018; Shonin et al., 2015), and only one (Schonert-Reichl et al., 2015) that appeared in two of them (Cheang et al., 2019; Luberto et al., 2018), suggesting that existing reviews have not adequately captured the effects of KCBIs on children’s wellbeing and prosociality.
In this review, we aimed to provide a summary and critique of current research on KCBM with children. Specifically, we conducted a systematic review of the effects of interventions that use KCBM on the wellbeing, prosociality, and cognitive functioning of children. We chose to examine these outcomes due to existing evidence of the effects of KCBIs on wellbeing and prosociality in adults, evidence of the effects of MBIs on wellbeing and cognitive functioning in children, and the importance of all three outcome categories for children.
Method
We followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines (Moher et al., 2009).
Eligibility Criteria
To be included in the systematic review, studies had to (a) evaluate an intervention that met one of two thresholds for proportion of KCBM (see below); (b) include child participants only (under 18 years, or 18 years in full-time, non-higher education); (c) include at least one outcome measure related to wellbeing, prosociality, or cognitive functioning; (d) be written in English; and (e) have a full text that could be retrieved. The KCBM thresholds for inclusion were that either (1) more than 50% of the intervention sessions included KCBM (i.e. a meditation practice; this threshold is similar to that used in previous reviews, e.g. Galante et al., 2014; Zeng et al., 2017), or (2) more than a third of the intervention sessions were devoted to the topic of kindness or compassion (i.e. didactic instruction, discussion, and activities) and included KCBM (i.e. a meditation practice). MBIs and KCBIs for children and adolescents tend to include less meditation and more didactic and activity-based components than those for adults. We included this second threshold to capture interventions that included a focus on kindness and compassion, but where the meditation component was condensed into a smaller portion of the intervention. If the amount of KCBM was not clear from the full text, then the study was excluded.
We included studies regardless of publication type and study design. Although this approach reduces the overall quality of studies included in the review and therefore limits the strength of the conclusions that can be drawn, it is useful in new areas of research where there may be few high-quality studies, and it enables recommendations to be made for improving the quality of the evidence base (Khan et al., 2011). We included both quantitative and qualitative studies. KCBM for the purpose of this review was taken to mean any meditation that has the explicit aim of cultivating kindness or compassion (e.g. LKM, CM, or self-compassion meditation).
There is some debate about the validity of combining the “three flows of compassion”—compassion for self, receiving compassion, and compassion for others—into a single construct (Shonin et al., 2015; Strauss et al., 2016). Although we do not suggest that these three forms of compassion are the same, they may all impact positively on wellbeing, prosociality, and cognitive functioning, albeit via different pathways. Self-compassion has been shown to have positive effects on wellbeing (MacBeth & Gumley, 2012), and some theorists suggest that it may lead to greater compassion for others (Neff & Pommier, 2013). Studies have found evidence that self-compassion is linked to empathy, compassion for others, and altruism in adults (Neff & Pommier, 2013), and to prosocial behaviour in adolescents (Marshall et al., 2020), and that “self-reassurance” and compassion for others involve similar neuronal activity (Longe et al., 2010), suggesting that the underlying neural basis may be similar for compassion for self and others. It is possible that compassion is a “mode” that can be applied either to oneself or to others, such that having compassion for oneself could make it easier to have compassion for others. Another motivation for including in our definition of KCBM meditations aiming to cultivate any of these three forms of compassion is that the field is in its infancy and we aimed to capture all relevant research.
We excluded interventions where meditation was not the main focus of the intervention, for example, Acceptance and Commitment Therapy and Compassion Focused Therapy (CFT; as in previous similar reviews, e.g. Kreplin et al., 2018; Luberto et al., 2018; Shonin et al., 2015), and mind–body techniques, such as yoga and tai chi, in an attempt to separate the effects of meditation from other intervention components, such as other aspects of therapy or physical exertion.
Information Sources
We searched the databases EMBASE, Ovid MEDLINE, PsycINFO, PsycARTICLES Full Text, Global Health, Social Policy and Practice, ERIC, ASSIA, IBSS, ATLA, and Web of Science on 24 February 2020 using the keywords described in the search strategy below. We searched EThOS and ProQuest Dissertations and Theses Global for theses, Cochrane and PROSPERO for systematic reviews, and Open Grey for grey literature, using the search terms “loving-kindness” and “compassion meditation”. We searched the tables of contents of key journals, publication lists of key academic researchers and institutions (e.g. The Center for Compassion and Altruism Research and Education, The Center for Healthy Minds, The Center for Contemplative Science and Compassion-Based Ethics at Emory University, The Oxford Mindfulness Centre, and The Mindfulness in Schools Project), and the reference lists of other relevant systematic reviews and the studies included in our review.
Search Strategy
We used the following keywords, along with relevant subject headings for each database, and search filters where available (Ovid MEDLINE and EMBASE): (((kindness OR compassion OR altruis*) AND (meditat* OR mindful* OR contemplat* practice* OR sitting practice*)) OR loving-kindness OR metta OR maitri OR mettha OR mudita OR karuna OR upekkha OR upeksa OR sympathetic joy OR equanimity) AND (child* or kid* or adolescen* or youth* or teen* or juvenil* or pupil* or student* or school* or preschool* or classroom or education or young people or young person). See Supplementary Appendix 1 for the full search strategy in Ovid MEDLINE.
Study Selection
The first and second authors independently screened search results against the eligibility criteria using titles and abstracts. Full texts were retrieved for studies that could feasibly meet the eligibility criteria, and were assessed against the eligibility criteria independently by the first two authors. Disagreements were resolved through discussion between the first, second, and third authors, and a consensus was reached in all cases.
Data Extraction
The first and second authors independently extracted data using a data extraction form designed for the review. Disagreements were resolved through discussion and a consensus was reached in all cases. The extracted data consisted of study characteristics (author, year, type of publication, country, study aims, study design, inclusion and exclusion criteria, recruitment procedures, unit of allocation), population (age, sex, ethnicity, socio-economic status, setting, clinical characteristics, universal vs. targeted, sample size, attrition rates), intervention (title, content, type and duration of meditation, frequency and length of sessions, length of intervention, total contact time, mode of delivery, homework, intervention teacher qualifications, whether the intervention teacher was a co-author), control group (type, description), outcome (type, measures, time points), findings (outcomes, attendance, homework adherence), and data on potential mechanisms or mediators. We did not contact authors where information was not reported.
Quality Assessment
The first and second authors independently assessed methodological quality using the Quality Assessment Tool for Quantitative Studies (QATQS). Disagreements were resolved through discussion and a consensus was reached in all cases. The QATQS is a reliable and valid general quality assessment tool that can be used for multiple quantitative study designs, including non-randomised trials and those with no control group (Effective Public Health Practice Project, 2012). It is one of only six of 194 tools deemed suitable for appraising non-randomised studies for systematic reviews (Deeks et al., 2003), and has “excellent” inter-rater agreement for final grades (Armijo-Olivo et al., 2012). It was an appropriate tool for this review since we had deliberately used broad eligibility criteria by including studies with any or no control group in order to capture all relevant studies in this emerging field.
The QATQS assesses methodological quality in the following eight domains: (a) selection bias, (b) study design, (c) confounders, (d) blinding, (e) data collection methods, (f) withdrawals and dropouts, (g) intervention integrity, and (h) analyses, leading to a rating of “strong”, “moderate”, or “weak” for each domain. Studies are given a global rating of “weak” if two or more domains receive a weak rating, “moderate” if one domain receives a weak rating, and “strong” if no domains receive a weak rating. As concerns have been raised about the use of global ratings (CRD, 2008), we report both the global rating and the ratings for each domain. Unfortunately, despite being a recommended tool (Deeks et al., 2003), the QATQS does not give guidance for rating the final two domains (intervention integrity and analyses) and does not include them in the global rating. For this reason, we have provided ratings for the first six domains and narrative feedback on the last two domains.
Summary Measures
Where applicable, significance levels (p), effect sizes (Cohen’s d or Hedges’ g), and other relevant measures of effect or correlation size were extracted. We used the standard interpretation of effect sizes of d and g: 0.20 = small, 0.50 = medium, and 0.80 = large (Cohen, 1988), although effect sizes should be considered in light of the area of inquiry, the outcomes used, and various aspects of individual study design. For example, Cohen’s benchmarks may underestimate the effect sizes of education interventions (Kraft, 2020).
Synthesis of Results
Since we did not restrict our review by study design, we expected a high level of heterogeneity and a low overall level of quality amongst the included studies, and therefore meta-analysis was not appropriate (CRD, 2008; Reeves et al., 2019). We summarised, synthesised, and appraised findings narratively, giving consideration to subgroups of interventions, populations, comparators, and outcomes, and to study quality.
Results
Study Selection
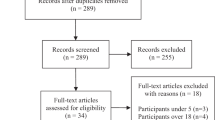
Searches yielded 3,073 records after removal of duplicates. We excluded 2,940 records based on their title and abstract, and retrieved 133 full texts. Of the 133 full texts, 123 were excluded as they did not use a child population (n = 84), were not intervention studies (n = 2), did not meet our KCBM inclusion thresholds (n = 26), did not report sufficient information for evaluation (n = 9), or were not available in full-text format (n = 2). This left 10 studies eligible for inclusion in this review. Of note, six of these 10 studies were not included in previous relevant reviews (Cheang et al., 2019; Luberto et al., 2018; Shonin et al., 2015; Waters et al., 2015). See Fig. 1 for the PRISMA flow diagram of the study selection process. See Supplementary Table 1 for a list of studies that were close to meeting the eligibility criteria but were not included in this review.
Study Characteristics
Of the 10 studies that met the inclusion criteria, seven were carried out within the last 5 years. Six studies were conducted in the USA, two in Israel, one in the UK, and one in South Africa. Although six studies described themselves as randomised, only one study provided sufficient details of the randomisation process to be classified as a randomised controlled trial (RCT) for the purposes of our review (Berger et al., 2018). One study used an active control group of weekly positive psychology reading materials (Bach & Guse, 2015). However, this activity was not well matched to the intervention group and adherence was not measured, making it questionable whether we can treat this group as an active rather than passive control. Six studies used a passive control of lessons-as-usual or a waitlist and three studies had no control group. There were no qualitative studies that met our inclusion criteria. Outcome measures were taken pre- and post-intervention for all studies. Four studies included a follow-up, which ranged from 5 weeks to 6 months after the intervention. Sample sizes ranged from 11 to 328. The total number of participants across studies was 807. Participant ages ranged from 8 to 18 years old, with the majority of studies carried out with adolescents. Participants’ sex across all studies was 52.8% female, 46.7% male, 0.4% unsure, and 0.1% gender neutral. Ethnicity and socio-economic background varied substantially between studies. Participants were school children and adolescents in four studies, adolescents with histories of trauma who were in the foster care system or living in youth care centres in three studies, adolescents enrolled in a mindful self-compassion course in two studies, and children with elevated anxiety in one study. A summary and further details of the characteristics of included studies is shown in Table 1.
There were eight different interventions examined by the studies included in this review. Six studies used established interventions. These were Cognitively-Based Compassion Training (CBCT) adapted for adolescents (Pace et al., 2013; Reddy et al., 2013), Call to Care-Israel (C2C-I; Berger et al., 2018; Tarrasch et al., 2017), and Making Friends with Yourself: A Mindful Self-Compassion Program for Teens (Bluth & Eisenlohr-Moul, 2017; Bluth et al., 2016). CBCT is based on lojong practices (from the Tibetan Buddhist tradition) that teach analytic methods to challenge one’s assumptions about others, in order to cultivate kindness and compassion towards all people (see Ozawa-de Silva & Dodson-Lavelle, 2011). C2C-I is a mindfulness- and compassion-based social-emotional programme that aims to teach mindfulness skills, cultivate a compassionate school climate, and promote academic achievement, wellbeing, and ethical and prosocial behaviour. C2C-I is based on Sustainable Compassion Training (see Condon & Makransky, 2020). Making Friends with Yourself is a version of the Mindful Self-Compassion course, adapted for adolescents (see Neff & Germer, 2013). The remaining four studies used a Contemplation Meditation, which involved analytic contemplation on the topic of compassion and focusing on the feelings and intentions generated (Bach & Guse, 2015); Group Mindfulness Therapy for anxiety (Crowley et al., 2018); a Positive Psychology Intervention (Teodorczuk et al., 2019); and Breath Counting Training and Self-Compassion Training (Moore, 2017).
The most common KCBM used in interventions was LKM, which was used in five interventions (Berger et al., 2018; Crowley et al., 2018; Moore, 2017; Tarrasch et al., 2017; Teodorczuk et al., 2019). Self-compassion practices were used in three interventions (Bluth & Eisenlohr-Moul, 2017; Bluth et al., 2016; Moore, 2017), caring-figure meditations were used in two interventions (Berger et al., 2018; Tarrasch et al., 2017), lojong compassion practices were used in one intervention that formed two studies (Pace et al., 2013; Reddy et al., 2013), self-nurturing meditation was used in one intervention (Berger et al., 2018), and analytic meditation on compassion was used in one intervention (Bach & Guse, 2015). See Table 2 for details of which KCBM inclusion threshold was met for each study.
The interventions varied in length from 4 to 24 weeks, with sessions lasting between 7 and 90 min. The total contact time of interventions ranged from 64 min (Moore, 2017) to 1,080 min (Berger et al., 2018; Tarrasch et al., 2017). In eight studies, participants were encouraged to meditate at home. See Table 2 for further details of homework. In nine studies, interventions were delivered in a group format by an intervention teacher, and in one study the intervention was delivered via computerised trainings using pre-recorded audio meditation guidance (Moore, 2017). Of the nine studies that used an intervention teacher, three studies reported that teachers had some form of meditation teacher-training (Bach & Guse, 2015; Bluth et al., 2016; Crowley et al., 2018), two reported that teachers had a personal meditation practice and experience in working with children (Berger et al., 2018; Tarrasch et al., 2017), two reported the professional qualifications of teachers (Crowley et al., 2018; Teodorczuk et al., 2019), and three studies did not report teacher background (Bluth & Eisenlohr-Moul, 2017; Pace et al., 2013; Reddy et al., 2013). In two studies, the intervention teacher was an author of the paper (Bluth et al., 2016; Teodorczuk et al., 2019), in one study two group facilitators were authors but it was unclear whether the intervention leader was an author (Crowley et al., 2018), in one study the intervention teachers were supervised by an author of the paper but it was unclear whether they were also authors (Berger et al., 2018), and in five studies it was unclear whether the teacher was an author of the paper (Bach & Guse, 2015; Bluth & Eisenlohr-Moul, 2017; Pace et al., 2013; Reddy et al., 2013; Tarrasch et al., 2017). A summary and further details of intervention characteristics are shown in Table 2. See Supplementary Table 2 for a summary of attrition rates, attendance, and homework adherence for included studies.
Quality Assessment
Overall, we found methodological quality to be weak, with no studies rated as strong in quality, only two studies rated as moderate (Berger et al., 2018; Pace et al., 2013), and the remaining eight studies rated as weak. See Table 3 for details of the quality assessment for each study, and Supplementary Fig. 1 for details of quality ratings by domain. Overall, the design, confounders, and data collection domains of studies were strong, with seven, six, and nine studies respectively receiving strong ratings. Lack of reporting accounted for the only weak scores in these domains. Attrition was mixed, with four studies receiving a strong rating and five receiving a weak rating (all due to lack of reporting). Selection bias and blinding were generally weak, with six studies receiving a weak rating for selection bias (one due to lack of reporting), and nine receiving a weak rating for blinding (eight due to lack of reporting). Overall, then, we found insufficient reporting in the domains of blinding and attrition, and a substantial risk of selection bias. Although all studies included in the review included multiple comparisons, only two studies reported correcting for this, using Bonferroni adjustments and Tukey Honest Significant Difference (Berger et al., 2018; Tarrasch et al., 2017). There is therefore potential for type I error in eight of the included studies. See Supplementary Appendix 2 for a discussion of quality in the domains of intervention integrity and analyses, and a comparison to quality scores of the same studies by Cheang et al. (2019) and Shonin et al. (2015).
Synthesis of Results
Table 3 gives a summary of outcome measures and findings for all studies. The majority of outcome measures were related to wellbeing and were self-report or parent-report, with only one study employing a physiological wellbeing outcome measure (Pace et al., 2013). One study examined outcome measures related to prosociality (Berger et al., 2018), and one study examined outcomes measures related to cognitive functioning (Tarrasch et al., 2017). For significant results, effect sizes ranged from small (d = 0.25) to large (d = 1.34). Effect sizes for non-significant results were mostly negligible to small in three studies, were not reported in five studies, and did not apply in two studies (since all results were significant). There were no adverse effects reported in any of the studies. As it has been suggested that self-compassion and compassion for others may be distinct phenomena (Shonin et al., 2015; Strauss et al., 2016), we examined the findings of studies under two subgroups: (1) interventions that included a substantial amount of meditation involving kindness or compassion for others (n = 7), and (2) interventions that mainly included self-compassion meditation (n = 3). Table 4 provides a summary of study findings by intervention type, outcome type, and sample age group.
Wellbeing outcomes for studies assessing interventions that included kindness or compassion for others meditation were significant in 11 out of 33 measures (33%). Significant improvements were found for some measures of stress, anxiety, internalising, externalising, and attention problems, negative affect, mindfulness, environmental mastery, and personal growth, with effect sizes ranging from medium (d = 0.76) to large (d = 1.34). No differences were found in depression, self-mutilation, callous and unemotional traits, scores on the Childhood Trauma Questionnaire, emotion regulation, mental health, hope, life satisfaction, positive affect, scores on the Self-Other Four Immeasurables scale (which measures loving-kindness, compassion, joy, and equanimity), and salivary C-reactive protein concentration (a biomarker for inflammation). However, Pace et al. (2013) reported a significant correlation between the number of practice sessions completed and salivary C-reactive protein, and concluded that engagement with CBCT may reduce inflammation. Similarly, Reddy et al. (2013) reported a significant correlation between practice frequency in the second half of the intervention and increased hope, and suggested that engagement with practice may have an impact on hopefulness. There were no observable patterns of significant results across studies according to study quality, design, sample size, dose of intervention, attendance and homework adherence, authorship status of the intervention teacher, or outcome measures used. Significant results for wellbeing came from studies using mainly non-clinical samples with a slightly younger age group and intervention teachers who were either very experienced or had some experience and received training.
Wellbeing outcomes for studies assessing interventions that mainly included self-compassion meditation were significant in 15 out of 22 measures (68%). Significant improvements were found for some measures of stress, anxiety, depression, negative affect, mindfulness, self-compassion, life satisfaction, resilience, gratitude, and “curiosity and exploration”, with effect sizes ranging from small (d = 0.25) to medium (d = 0.72). No differences were found in positive affect or social connectedness. The two studies that produced most of the significant results (Bluth & Eisenlohr-Moul, 2017; Bluth et al., 2016) included a slightly younger age group and used an established intervention, a higher dose, and an in-person teacher as opposed to e-learning audio. The findings of the studies examining self-compassion interventions should be interpreted with caution, as all three studies were graded as weak in quality, had relatively low sample sizes, and lacked adequate control groups—many significant effects were for pre- post-intervention only, rather than compared to controls.
Prosociality was examined in one kindness or compassion for others intervention study (Berger et al., 2018). The authors examined readiness for social contact, affective prejudice, and negative stereotyping using 5-point Likert-type scales designed for the context of conflict within which the study took place. Some examples of items from these measures (completed by Israeli-Jewish pupils) are rating willingness to play with Israeli-Palestinian pupils (readiness for social contact); rating how relaxed pupils felt towards Israeli-Palestinian pupils (affective prejudice); and rating traits of Israeli-Palestinian pupils, for example, from “very smart” to “very stupid” (negative stereotyping). The authors found an increase in readiness for social contact, and a decrease in affective prejudice and negative stereotyping following the intervention, gains which were maintained at a 6-month follow-up, with large effect sizes at both post-intervention and follow-up (d = 0.84–1.28). This study was the only one to qualify as an RCT in this review, and one of only two studies that received a moderate quality rating. Although only a passive control was used, the sample size was the largest in this review, at 328 children. The intervention was an established one (C2C-I), and one of the highest-dose interventions included in this review. In keeping with the pattern of wellbeing findings, the sample was non-clinical and used the youngest age group of any study in this review, with children aged 8 to 11 years old, and the intervention teachers had relevant experience, received training, and were supervised.
Cognitive functioning was examined in one kindness or compassion for others intervention study (Tarrasch et al., 2017). The authors measured visual perception and motor accuracy using the Beery-Buktenica Developmental Test of Visual-Motor Integration and found an increase in both outcomes following the intervention, as compared to a control group, with medium (ηp2 = 0.083) to large (ηp2 = 0.193) effect sizes. Although this study received a weak quality rating, it benefitted from a large sample size of 216 children, making it one of only two studies included in the review with a sample size over 100. This study used the same established intervention as Berger et al. (2018), and so was one of the highest-dose interventions included. Again, the sample was non-clinical and was one of the youngest in this review, with children aged 9 to 11 years old, and the intervention teachers had relevant experience and received training.
Potential predictors of outcomes were examined in two of the 10 studies included in this review. Both of these were studies assessing interventions that mainly included self-compassion meditation. Bluth et al. (2016) performed hierarchical regressions and reported that increases in mindfulness predicted decreases in depression and anxiety, and that increases in self-compassion predicted decreases in anxiety and stress and increases in life satisfaction. Bluth & Eisenlohr-Moul (2017) used multilevel growth models and reported that increases in mindfulness were associated with lower depression, anxiety, and stress, and that increases in self-compassion were associated with lower depression and stress, greater resilience, and greater “curiosity and exploration”.
Three kindness or compassion for others intervention studies reported correlational data. Tarrasch et al. (2017) reported that increases in mindfulness and reductions in anxiety correlated with improvements in motor accuracy, but not with improvements in visual perception. The authors suggested that mindfulness may be a mechanism by which children improved their motor accuracy, and that it is unclear whether children improved their motor accuracy because they were less anxious, or whether they were less anxious because of their improved performance. As this data is correlational, it is not possible to infer causation, and therefore this hypothesis would need further testing. Both Pace et al. (2013) and Reddy et al. (2013) found that greater practice frequency was correlated with some aspects of wellbeing. Although this leaves open the question of psychological mechanisms, it suggests that the amount of meditation practice completed has an important impact on outcome measures, as opposed to outcomes being solely affected by, for example, didactic teaching or meeting as a group.
Discussion
We conducted a systematic review of effects of KCBM on wellbeing, prosociality, and cognitive functioning in children and adolescents. Ten studies were eligible for inclusion in our review, with publication dates ranging from 2012 to 2019. We found some evidence of improvements in wellbeing following interventions, including reductions in stress, anxiety, depression, negative affect, and markers of inflammation, and increases in mindfulness and self-compassion, with changes on 26 out of 55 (47%) outcome measures across studies reaching significance and effect sizes ranging from small to large. Despite non-significant results for wellbeing in three studies (Pace et al., 2013; Reddy et al., 2013; Teodorczuk et al., 2019), all three reported that the intervention was evaluated positively by participants, with qualitative feedback that the techniques learnt had been helpful, suggesting that the outcome measures used in these studies may not have been adequate to detect the effects of interventions. It is also possible that some wellbeing outcomes take longer to emerge due to being more distal (e.g. psychological outcomes such as depression and anxiety may take longer to emerge than physiological outcomes; Pace et al., 2013), that some people can feel worse before they feel better in response to meditation (Boellinghaus et al., 2014; Davidson & Kaszniak, 2015), and that individuals have different emotional responses to different meditations (Boellinghaus et al., 2013; Weng et al., 2017), particularly a more variable response to KCBM than MBIs (Singer & Engert, 2019), with the consequence that a range of responses across individuals can result in no overall effect and mask effects within subgroups.
We found encouraging results for improvements in prosociality, with large effect sizes, and for improvements in cognitive functioning (specifically, visual perception and motor accuracy), with medium to large effect sizes and all outcome measures reaching significance. Although only one study measured prosociality and only one measured visual perception and motor accuracy, these two studies had the largest sample sizes, and the study measuring prosociality was one of the more methodologically robust.
Overall, we found the quality of studies to be weak, with only two out of 10 studies being rated as moderate in quality (Berger et al., 2018; Pace et al., 2013). However, most low ratings were due to non-reporting, rather than clear methodological failings. Overall, these are promising results, but they should be interpreted with caution given both the low methodological quality and the small number of studies included in the review.
We did not find evidence for variation of results dependent on study quality, design, sample size, dose of intervention, or authorship status of the intervention teacher. We did, however, find a larger number of significant results in studies that used non-clinical samples (in line with findings for KCBIs by Kirby et al., 2017), younger age groups, established interventions, and experienced intervention teachers. However, these suggested patterns should be viewed in the context of the heterogeneity between studies and the very low number of studies informing these comparisons. Many outcomes were measured by only one study, and many factors varied between studies, making it difficult to determine conclusively which factors impacted the results. For example, it may be that KCBMs are more effective with younger children (8–11 years) than with older children (11–18 years), or it could be that the two studies involving younger children produced significant results because the sample was non-clinical, the intervention was an established one, or the intervention teachers had relevant experience and training. Without a larger number of studies where all but one of these factors remain consistent, it is difficult to draw conclusions.
When interpreting our results, it should also be taken into account that the majority of included studies used adolescent samples as opposed to younger children. Adolescence is a formative period in which there are opportunities for flourishing but also increased risk of mental health difficulties (Roeser & Pinela, 2014). Given that strong emotions can be evoked by KCBMs, they may be more challenging for an adolescent sample, who may also be dealing with issues such as depression or anxiety. Adolescence is also a key period for social development, marked by a developing sense of self, higher-level prosocial reasoning, and an increased focus on social relations (Crone & Achterberg, 2022; Eisenberg et al., 1991). These factors mean that peers become particularly important in motivating prosocial behaviour, and that prosocial behaviour becomes critical to the development of reciprocal social relationships (Wentzel, 2015). KCBMs may therefore have a different impact on prosocial behaviour in this age group compared to in younger children or adults. It is key to the development of the field to establish the differing impacts of KCBMs on different age groups.
The three studies with the most null findings all involved adolescents in care settings—it is possible that this group may find it particularly difficult to engage with KCBM. KCBM has been shown to be a challenging practice (Bibeau et al., 2020; Boellinghaus et al., 2013), to be more effortful than breathing meditation (Singer & Engert, 2019), and to have the potential to be counter-productive in those with a history of trauma and insecure attachment, since attempts to evoke feelings of kindness and compassion can trigger sadness and grief at having not received similar care in childhood (Gilbert, 2009). However, some research shows that those who are most in need tend to benefit most from such interventions (e.g. Flook et al., 2015). It may be that longer interventions are needed for significant changes in outcome measures for this population. This suggestion is supported by the findings of Pace et al. (2013) and Reddy et al. (2013) that engagement in the latter half of the course correlated with reductions in inflammation markers and increases in hope. It may be that group interventions containing KCBMs are appropriate as preventative and mental health promotion tools, rather than as treatment interventions targeting, for example, individuals with complex histories of trauma. In these cases, a more individualised approach such as a one-to-one therapy may be needed. For example, CFT can help children and adolescents to navigate the potential difficulties of engaging with KCBM by first addressing the fears, blocks, and resistances that they may have to receiving and giving compassion (Gilbert, 2009).
Although we found a larger number of significant results in studies where intervention teachers were experienced, it is difficult to draw definitive conclusions from our review regarding the impact of teacher qualifications due to the non-reporting of intervention teacher background in 40% of the included studies. Unlike Kreplin et al. (2018), we did not find a difference in the number of significant results according to whether the intervention teacher was a co-author on the paper. However, this finding is limited by the lack of reporting of the authorship status of the intervention teacher in 50% of studies and unclear reporting in a further 20%. To fully address the question of whether authorship status of the intervention teacher affects outcomes, reporting of teacher background must be improved, stating clearly who the intervention teacher was and their link to both the authors and the developers of the intervention (another possible source of allegiance bias).
Two studies included in our review identified increases in mindfulness and self-compassion as predictors of improved wellbeing (Bluth & Eisenlohr-Moul, 2017; Bluth et al., 2016), and one study found that increases in mindfulness correlated with improved motor accuracy (Tarrasch et al., 2017), suggesting that mindfulness and self-compassion may be mechanisms through which outcomes improved. This is consistent with existing literature that links mindfulness and self-compassion to wellbeing outcomes (Dunning et al., 2019; MacBeth & Gumley, 2012). Looking across the other studies in our review, there was no clear evidence to support these hypotheses, as studies either did not measure these potential mechanisms, did not find significant results, or did not measure comparable outcomes. Some studies speculated on mechanisms but did not include outcome measures that could support their hypotheses. For example, Bach and Guse (2015) speculated that their compassion intervention may have impacted wellbeing by increasing compassion for others, causing participants to focus on others rather than themselves, consequently giving them more energy and ease in mastering their own daily activities. However, compassion was not measured in their study. Berger et al. (2018) suggested that mindfulness, compassion, and perspective-taking may be mechanisms by which prosociality was impacted but did not include these as outcome measures. Pace et al. (2013) suggested that CBCT may reduce inflammation by reducing interpersonal conflict, social isolation, and stress. However, none of these outcomes were measured in their study.
Limitations and Future Research
Our review is limited by the weak quality of included studies (including potential for type I error due to multiple comparisons); the lack of RCT design amongst the majority of included studies; small sample sizes; the risk of selection bias in 50% of included studies (although see Rosenkranz et al. (2019) for a discussion of the impact of participant choice on outcome effects and the generalisability of random samples in meditation research); the lack of adequate control groups that control for non-specific factors of interventions, such as meeting as a supportive group; possible expectation bias due to the potential lack of blinding of participants, intervention teachers, and outcome assessors in 90% of included studies; and over-reliance on self-report, particularly given that children may have difficulty understanding questionnaire items and have been shown to respond in an extreme manner to self-report questionnaires (Chambers & Johnston, 2002), and given that the increase in awareness caused by interventions designed to increase meta-cognitive awareness can itself confound pre-/post-differences (e.g. one may be more aware of one’s depressive thoughts following an intervention; Davidson & Kaszniak, 2015). The lack of active control groups, potential lack of blinding, and reliance on self-report combined mean that expectation bias could be responsible for the observed effects in the studies.
We restricted our review to English language articles, which may have excluded relevant non-English language articles. We did not contact authors where study information was not reported (for example, the amount of KCBM in the intervention), which may have excluded relevant studies. We did not include as search terms “visualisation” and “imagery”, practices that are used extensively in CFT, but these may be comparable to meditation. We included studies based on an arbitrary threshold for the amount of KCBM within the intervention, which meant that we excluded studies of interventions that are similar to those included in the review but contain slightly less KCBM. Deciding on an appropriate threshold of the amount of meditation within an intervention is particularly difficult in research with children, where meditations tend to be shorter and interventions tend to contain more didactic and activity-based components. Our KCBM inclusion thresholds meant that studies involving interventions that included up to two thirds of other activities were included in the review. This makes it difficult to attribute the effects reported in the studies to KCBM, as, for example, an intervention could, as well as KCBM, include mindfulness meditation in up to two thirds of the sessions. This is a problem that similar reviews faced, given that interventions tend to include multiple components.
In an attempt to give a comprehensive summary of the research in this area to date, we included all types of study design in our review. Although the weak quality of included studies is to be expected given this decision, it nevertheless limits the conclusions that can be drawn from the review. Despite including all types of study design, only 10 studies met our inclusion criteria, which suggests that the trade-off of quality against comprehensiveness was worthwhile, provided the results of our review are interpreted with its limitations in mind. Our review is also limited by the small number of studies included, and their high clinical and methodological heterogeneity, an issue which has been problematic for similar reviews (e.g. Cheang et al., 2019; Shonin et al., 2015). This makes it very difficult to draw firm conclusions about the contributions of different aspects of the interventions, populations, or other potential moderators and mediators to study findings (Reeves et al., 2019). Finally, we did not formally check for publication bias. However, this bias has not been found in similar reviews (Kirby et al., 2017; Kreplin et al., 2018; Luberto et al., 2018; Zeng et al., 2015).
There is evidence that KCBM may be an effective method for improving wellbeing, prosociality, and cognitive functioning in non-clinical child populations, and could therefore be a useful alternative to existing school programmes such as MBIs and social-emotional learning programmes. Consideration should be given to the age group of children and the experience of the teacher, given that KCBIs may be more effective when implemented with younger age groups and when intervention teachers have meditation experience. If KCBIs are used with clinical populations, they may need careful tailoring, for example, by being longer in order to give these populations time to engage with the practices and see beneficial effects, and by including exercises and discussions about fears, blocks, and resistances to compassion, as well as how to work with any difficult emotions that may be evoked. However, our findings should be treated as preliminary given the limitations discussed above. Schools and intervention providers should bear in mind that although there is evidence of the benefits of KCBM for wellbeing and prosociality in adults (Galante et al., 2014; Luberto et al., 2018; Shonin et al., 2015), and initial findings with children are promising, there is not yet a strong evidence base for beneficial effects of KCBM with children and adolescents.
Following a similar trajectory to mindfulness research with children (Dunning et al., 2019; Weare, 2019) and compassion research with adults (Galante et al., 2014; Kirby et al., 2017), research on KCBIs with children is very much in its infancy, with most studies either uncontrolled, using passive controls, or statistically underpowered. The findings of the current review should be seen as preparation for further research, highlighting areas where research methodology needs to be improved as well as avenues for further research. Here, we offer seven recommendations for future research.
There is a need for larger-scale, fully powered RCTs with pre-registered protocols, and evaluation conducted by a different team than that which developed and delivered the intervention. Although double-blinded RCTs are preferable in medical research, they may be less feasible within psychological research. Cluster randomisation may be more realistic for group intervention research within schools. Double-blinding can be particularly challenging in meditation research, where the aims of the intervention are often intentionally explicit in the meditation instructions. Some studies have managed to achieve this; for example, Ashar and colleagues compared charitable donations from participants in a CM condition with those from participants in a placebo oxytocin condition, where participants falsely believed they were inhaling oxytocin that would enhance compassion (Ashar et al., 2016, 2019; see also Davidson & Kaszniak, 2015). The field would benefit from comparable active control interventions (to control for non-specific effects of the intervention), in which children believe they will benefit in the same way as the experimental intervention and intervention teachers are fully trained on the control intervention and believe in its efficacy (to control for expectation effects; Davidson & Kaszniak, 2015). However, the time and cost of developing convincing active controls may preclude this for most research.
We found a need for improved reporting of: details of the randomisation process; blinding of participants, intervention teachers, and outcome assessors; details of who developed, delivered, and evaluated the intervention, including the authorship status and experience of the intervention teacher; the exact dose of KCBM within the intervention, including the length and frequency of meditations; attrition rates and the reasons for drop-out; and adherence to homework. Future research would benefit from use of the meditation-based intervention design reporting checklist by Pilla et al. (2020).
There is a need for more research with younger children to identify optimum periods in which to introduce KCBM, particularly given the early onset of many mental health issues (Kessler et al., 2005), the significant changes in prosociality and the cognitive capacities that impact on it during early childhood (Laible & Karahuta, 2015; Spinrad & Eisenberg, 2017), the plasticity associated with early childhood (Flook et al., 2015), and the finding that interventions targeting empathy-related constructs produce larger effects when implemented earlier in development (Malti et al., 2016). The optimum periods may depend on the type of outcome and may be different from the optimum periods in which to introduce MBIs (Dunning et al., 2019; Malti et al., 2016).
The field would benefit from research using standardised interventions, to enable robust comparisons to be made between studies so that conclusions can be drawn about their relative effectiveness and findings can be replicated.
In respect of outcome measures, there is a need for standardised measures to enable comparisons between studies; more behavioural, physiological, and neurological measures to overcome the limitations of over-reliance on self-report; and more research on prosocial and cognitive outcomes, for example, by using behavioural measures of prosociality that have been tried and tested in the developmental literature.
Future research should identify and systematically test proposed mechanisms of change, based on existing psychological and neurobiological models of the mechanisms of KCBM (e.g. Ash et al., 2019; Carona et al., 2017; Weng et al., 2017), and taking a developmental perspective (Malti et al., 2016; Roeser & Eccles, 2015). Research should take into account how potential mechanisms unfold over time, so that relevant outcomes can be measured at the relevant time-points, including at follow-up (Rosenkranz et al., 2019), and should investigate the links and direction of causality between wellbeing, prosociality, and cognitive functioning. Investigating moderators of outcomes would help to identify young people for whom KCBM may be most helpful.
Researchers should conduct dismantling studies to identify active ingredients of interventions and compare differential effects of mindfulness and different types of KCBM. Whilst we attempted to focus on KCBM by only including interventions that met set thresholds of KCBM, many of the interventions included in our review also included mindfulness. A useful approach would be to have several arms within a research design that compares mindfulness, LKM, CM, an active matched control (to control for non-specific factors), and a passive control (to examine intentional expectation effects). Such a design would also have the advantage that intervention teachers could be experienced meditators and yet be unaware of research hypotheses and which condition they were in, which would help to prevent expectation bias.
References
* Indicates included in the systematic review
Aknin, L. B., Dunn, E. W., & Norton, M. I. (2012). Happiness runs in a circular motion: Evidence for a positive feedback loop between prosocial spending and happiness. Journal of Happiness Studies, 13(2), 347–355. https://doi.org/10.1007/s10902-011-9267-5
Aknin, L. B., Hamlin, J. K., & Dunn, E. W. (2012). Giving leads to happiness in young children. PLoS ONE, 7(6), e39211. https://doi.org/10.1371/journal.pone.0039211
Armijo-Olivo, S., Stiles, C. R., Hagen, N. A., Biondo, P. D., & Cummings, G. G. (2012). Assessment of study quality for systematic reviews: A comparison of the Cochrane Collaboration Risk of Bias Tool and the Effective Public Health Practice Project Quality Assessment Tool: Methodological research. Journal of Evaluation in Clinical Practice, 18(1), 12–18. https://doi.org/10.1111/j.1365-2753.2010.01516.x
Ash, M., Harrison, T., Pinto, M., DiClemente, R., & Negi, L. T. (2019). A model for cognitively-based compassion training: Theoretical underpinnings and proposed mechanisms. Social Theory & Health, 1-25.https://doi.org/10.1057/s41285-019-00124-x
Ashar, Y. K., Andrews-Hanna, J. R., Yarkoni, T., Sills, J., Halifax, J., Dimidjian, S., & Wager, T. D. (2016). Effects of compassion meditation on a psychological model of charitable donation. Emotion, 16(5), 691–705. https://doi.org/10.1037/emo0000119
Ashar, Y. K., Andrews-Hanna, J. R., Halifax, J., Dimidjian, S., & Wager, T. D. (2019). Effects of compassion training on brain responses to suffering others. BioRxiv, 616029.https://doi.org/10.1093/scan/nsab068
*Bach, J. M., & Guse, T. (2015). The effect of contemplation and meditation on ‘great compassion’ on the psychological well-being of adolescents. The Journal of Positive Psychology, 10(4), 359-369.https://doi.org/10.1080/17439760.2014.965268
*Berger, R., Brenick, A., & Tarrasch, R. (2018). Reducing Israeli-Jewish pupils’ outgroup prejudice with a mindfulness and compassion-based social-emotional program. Mindfulness, 9(6), 1768-1779.https://doi.org/10.1007/s12671-018-0919-y
Bergin, C. (2015). Educating students to be prosocial at school. In L. M. Padilla-Walker & G. Carlo (Eds.), Prosocial development: A multidimensional approach (pp. 279–301). Oxford University Press.
Bibeau, M., Dionne, F., Riera, A., & Leblanc, J. (2020). The influence of compassion meditation on the psychotherapist’s empathy and clinical practice: A phenomenological analysis. Journal of Humanistic Psychology, 0022167820953258.https://doi.org/10.1177/0022167820953258
*Bluth, K., & Eisenlohr-Moul, T. A. (2017). Response to a mindful self-compassion intervention in teens: A within-person association of mindfulness, self-compassion, and emotional well-being outcomes. Journal of Adolescence, 57, 108-118.https://doi.org/10.1016/j.adolescence.2017.04.001
*Bluth, K., Gaylord, S. A., Campo, R. A., Mullarkey, M. C., & Hobbs, L. (2016). Making friends with yourself: A mixed methods pilot study of a mindful self-compassion program for adolescents. Mindfulness, 7(2), 479-492.https://doi.org/10.1007/s12671-015-0476-6
Böckler, A., Tusche, A., Schmidt, P., & Singer, T. (2018). Distinct mental trainings differentially affect altruistically motivated, norm motivated, and self-reported prosocial behaviour. Scientific Reports, 8(1), 13560. https://doi.org/10.1038/s41598-018-31813-8
Boellinghaus, I., Jones, F. W., & Hutton, J. (2013). Cultivating self-care and compassion in psychological therapists in training: The experience of practicing loving-kindness meditation. Training and Education in Professional Psychology, 7(4), 267–277. https://doi.org/10.1037/a0033092
Boellinghaus, I., Jones, F. W., & Hutton, J. (2014). The role of mindfulness and loving-kindness meditation in cultivating self-compassion and other-focused concern in health care professionals. Mindfulness, 5(2), 129–138. https://doi.org/10.1007/s12671-012-0158-6
Bukowski, W. M., Laursen, B., & Hoza, B. (2010). The snowball effect: Friendship moderates escalations in depressed affect among avoidant and excluded children. Development and Psychopathology, 22(4), 749–757. https://doi.org/10.1017/S095457941000043X
Burstow, P., Jenkins, P., Adebowale, V., Bailey, S., Farmer, P., Greatley, A., & Rose-Quirie, A. (2014). The pursuit of happiness: A new ambition for our mental health. A CentreForum Commission. http://www.centreforum.org/assets/pubs/the-pursuit-of-happiness.pdf. Accessed 19 September 2017.
Carona, C., Rijo, D., Salvador, C., Castilho, P., & Gilbert, P. (2017). Compassion-focused therapy with children and adolescents. Bjpsych Advances, 23(4), 240–252. https://doi.org/10.1192/apt.bp.115.015420
Chambers, C. T., & Johnston, C. (2002). Developmental differences in children’s use of rating scales. Journal of Pediatric Psychology, 27(1), 27–36. https://doi.org/10.1093/jpepsy/27.1.27
Cheang, R., Gillions, A., & Sparkes, E. (2019). Do mindfulness-based interventions increase empathy and compassion in children and adolescents: A systematic review. Journal of Child and Family Studies, 28(7), 1765–1779. https://doi.org/10.1007/s10826-019-01413-9
Cohen, J. (1988). Statistical power analysis for the behavioral sciences (2nd ed.). Routledge. https://doi.org/10.4324/9780203771587
Condon, P., & Makransky, J. (2020). Sustainable compassion training: Integrating meditation theory with psychological science. Frontiers in Psychology, 11, 2249. https://doi.org/10.3389/fpsyg.2020.02249
CRD. (2008). Systematic Reviews: CRD’s guidance for undertaking reviews in healthcare. Centre for Reviews and Dissemination (3rd ed.). York Publishing Services.
Crone, E. A., & Achterberg, M. (2022). Prosocial development in adolescence. Current Opinion in Psychology, 44, 220–225. https://doi.org/10.1016/j.copsyc.2021.09.020
*Crowley, M. J., Nicholls, S. S., McCarthy, D., Greatorex, K., Wu, J., & Mayes, L. C. (2018). Innovations in practice: Group mindfulness for adolescent anxiety - Results of an open trial. Child and Adolescent Mental Health, 23(2), 130-133.https://doi.org/10.1111/camh.12214
Curry, O. S., Rowland, L. A., Van Lissa, C. J., Zlotowitz, S., McAlaney, J., & Whitehouse, H. (2018). Happy to help? A systematic review and meta-analysis of the effects of performing acts of kindness on the well-being of the actor. Journal of Experimental Social Psychology, 76, 320–329. https://doi.org/10.1016/j.jesp.2018.02.014
Davidson, R. J., & Kaszniak, A. W. (2015). Conceptual and methodological issues in research on mindfulness and meditation. American Psychologist, 70(7), 581–592. https://doi.org/10.1037/a0039512
Deeks, J. J., Dinnes, J., D’Amico, R., Sowden, A. J., Sakarovitch, C., Song, F., Petticrew, M., & Altman, D. G. (2003). Evaluating non-randomised intervention studies. Health Technology Assessment, 7(27), 1–173. https://doi.org/10.3310/hta7270
Dunning, D. L., Griffiths, K., Kuyken, W., Crane, C., Foulkes, L., Parker, J., & Dalgleish, T. (2019). Research review: The effects of mindfulness-based interventions on cognition and mental health in children and adolescents - a meta-analysis of randomized controlled trials. Journal of Child Psychology and Psychiatry, 60(3), 244–258. https://doi.org/10.1111/jcpp.12980
Effective Public Health Practice Project. (2012). Quality assessment tool for quantitative studies. https://merst.ca/ephpp/. Accessed 1 February 2020.
Eisenberg, N. (1986). Altruistic emotion, cognition and behavior. Erlbaum.
Eisenberg, N., Miller, P. A., Shell, R., McNalley, S., & Shea, C. (1991). Prosocial development in adolescence: A longitudinal study. Developmental Psychology, 27(5), 849–857. https://doi.org/10.1037/0012-1649.27.5.849
Flook, L., Goldberg, S. B., Pinger, L., & Davidson, R. J. (2015). Promoting prosocial behavior and self-regulatory skills in preschool children through a mindfulness-based kindness curriculum. Developmental Psychology, 51(1), 44–51. https://doi.org/10.1037/a0038256
Fowler, J. H., & Christakis, N. A. (2010). Cooperative behavior cascades in human social networks. Proceedings of the National Academy of Sciences, 107(12), 5334–5338. https://doi.org/10.1073/pnas.0913149107
Galante, J., Galante, I., Bekkers, M. J., & Gallacher, J. (2014). Effect of kindness-based meditation on health and well-being: A systematic review and meta-analysis. Journal of Consulting and Clinical Psychology, 82(6), 1101–1114. https://doi.org/10.1037/a0037249
Gilbert, P. (2009). Introducing compassion-focused therapy. Advances in Psychiatric Treatment, 15(3), 199–208. https://doi.org/10.1192/apt.bp.107.005264
Goldberg, S. B., Riordan, K. M., Sun, S., & Davidson, R. J. (2022). The empirical status of mindfulness-based interventions: A systematic review of 44 meta-analyses of randomized controlled trials. Perspectives on Psychological Science, 17(1), 108–130. https://doi.org/10.1177/1745691620968771
Greenberg, M. T., & Harris, A. R. (2012). Nurturing mindfulness in children and youth: Current state of research. Child Development Perspectives, 6(2), 161–166. https://doi.org/10.1111/j.1750-8606.2011.00215.x
Hofmann, S. G., Grossman, P., & Hinton, D. E. (2011). Loving-kindness and compassion meditation: Potential for psychological interventions. Clinical Psychology Review, 31(7), 1126–1132. https://doi.org/10.1016/j.cpr.2011.07.003
Kessler, R. C., Berglund, P., Demler, O., Jin, R., Merikangas, K. R., & Walters, E. E. (2005). Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Archives of General Psychiatry, 62(6), 593–602. https://doi.org/10.1001/archpsyc.62.6.593
Khan, K., Kunz, R., Kleijnen, J., & Antes, G. (2011). Systematic reviews to support evidence-based medicine (2nd ed.). Hodder Arnold.
Khoury, B., Sharma, M., Rush, S. E., & Fournier, C. (2015). Mindfulness-based stress reduction for healthy individuals: A meta-analysis. Journal of Psychosomatic Research, 78(6), 519–528. https://doi.org/10.1016/j.jpsychores.2015.03.009
Kirby, J. N., Tellegen, C. L., & Steindl, S. R. (2017). A meta-analysis of compassion-based interventions: Current state of knowledge and future directions. Behavior Therapy, 48(6), 778–792. https://doi.org/10.1016/j.beth.2017.06.003
Kraft, M. A. (2020). Interpreting effect sizes of education interventions. Educational Researcher, 49(4), 241–253. https://doi.org/10.3102/0013189X20912798
Kreplin, U., Farias, M., & Brazil, I. A. (2018). The limited prosocial effects of meditation: A systematic review and meta-analysis. Scientific Reports, 8(1), 1–10. https://doi.org/10.1038/s41598-018-20299-z
Laible, D., & Karahuta, E. (2015). Prosocial behaviours in early childhood: Helping others, responding to the distress of others, and working with others. In L. M. Padilla-Walker & G. Carlo (Eds.), Prosocial development: A multidimensional approach (pp. 350–373). Oxford University Press.
Layous, K., Nelson, S. K., Oberle, E., Schonert-Reichl, K. A., & Lyubomirsky, S. (2012). Kindness counts: Prompting prosocial behavior in preadolescents boosts peer acceptance and well-being. PLoS ONE, 7(12), e51380. https://doi.org/10.1371/journal.pone.0051380
Lee, T. M., Leung, M.-K., Hou, W.-K., Tang, J. C., Yin, J., So, K.-F., Lee, C.-F., & Chan, C. C. H. (2012). Distinct neural activity associated with focused-attention meditation and loving-kindness meditation. PLoS ONE, 7(8), e40054. https://doi.org/10.1371/journal.pone.0040054
Lereya, S. T., Winsper, C., Heron, J., Lewis, G., Gunnell, D., Fisher, H. L., & Wolke, D. (2013). Being bullied during childhood and the prospective pathways to self-harm in late adolescence. Journal of the American Academy of Child & Adolescent Psychiatry, 52(6), 608–618. https://doi.org/10.1016/j.jaac.2013.03.012
Longe, O., Maratos, F. A., Gilbert, P., Evans, G., Volker, F., Rockliff, H., & Rippon, G. (2010). Having a word with yourself: Neural correlates of self-criticism and self-reassurance. NeuroImage, 49(2), 1849–1856. https://doi.org/10.1016/j.neuroimage.2009.09.019
Luberto, C. M., Shinday, N., Song, R., Philpotts, L. L., Park, E. R., Fricchione, G. L., & Yeh, G. Y. (2018). A systematic review and meta-analysis of the effects of meditation on empathy, compassion, and prosocial behaviors. Mindfulness, 9(3), 708–724. https://doi.org/10.1007/s12671-017-0841-8
MacBeth, A., & Gumley, A. (2012). Exploring compassion: A meta-analysis of the association between self-compassion and psychopathology. Clinical Psychology Review, 32(6), 545–552. https://doi.org/10.1016/j.cpr.2012.06.003
Mak, C., Whittingham, K., Cunnington, R., & Boyd, R. N. (2018). Efficacy of mindfulness-based interventions for attention and executive function in children and adolescents - A systematic review. Mindfulness, 9(1), 59–78. https://doi.org/10.1007/s12671-017-0770-6
Malti, T., Chaparro, M. P., Zuffianò, A., & Colasante, T. (2016). School-based interventions to promote empathy-related responding in children and adolescents: A developmental analysis. Journal of Clinical Child & Adolescent Psychology, 45(6), 718–731. https://doi.org/10.1080/15374416.2015.1121822
Marshall, S. L., Ciarrochi, J., Parker, P. D., & Sahdra, B. K. (2020). Is self-compassion selfish? The development of self-compassion, empathy, and prosocial behavior in adolescence. Journal of Research on Adolescence, 30, 472–484. https://doi.org/10.1111/jora.12492
Mascaro, J. S., Rilling, J. K., Tenzin Negi, L., & Raison, C. L. (2013). Compassion meditation enhances empathic accuracy and related neural activity. Social Cognitive and Affective Neuroscience, 8(1), 48–55. https://doi.org/10.1093/scan/nss095
Mental Health Foundation (2020). Mental health statistics: Children and young people. https://www.mentalhealth.org.uk/statistics/mental-health-statistics-children-and-young-people.
Mind and Life Education Research Network (MLERN), Davidson, R. J., Dunne, J., Eccles, J. S., Engle, A., Greenberg, M., Jennings, P., Jha, A., Jinpa, T., Lantieri, L., Meyer, D., Roeser, R., & Vago, D. (2012). Contemplative practices and mental training: Prospects for American education. Child Development Perspectives, 6(2), 146–153. https://doi.org/10.1111/j.1750-8606.2012.00240.x
Moher, D., Liberati, A., Tetzlaff, J., Altman, D. G., The PRISMA Group. (2009). Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. PLoS Medicine, 6(7), e1000097. https://doi.org/10.7326/0003-4819-151-4-200908180-00135
*Moore, J. A. (2017). Examination of the effects of computer assisted mindfulness strategies with adolescents in an alternative high school setting (Doctoral dissertation). Retrieved from https://scholarworks.wmich.edu/dissertations/3166/
Neff, K. D., & Germer, C. K. (2013). A pilot study and randomized controlled trial of the mindful self-compassion program. Journal of Clinical Psychology, 69, 28–44. https://doi.org/10.1002/jclp.21923
Neff, K. D., & Pommier, E. (2013). The relationship between self-compassion and other-focused concern among college undergraduates, community adults, and practicing meditators. Self and Identity, 12(2), 160–176. https://doi.org/10.1080/15298868.2011.649546
Nelson, S. K., Layous, K., Cole, S. W., & Lyubomirsky, S. (2016). Do unto others or treat yourself? The effects of prosocial and self-focused behavior on psychological flourishing. Emotion, 16(6), 850–861. https://doi.org/10.1037/emo0000178
Ozawa-de Silva, B., & Dodson-Lavelle, B. (2011). An education of heart and mind: Practical and theoretical issues in teaching cognitive-based compassion training to children. Practical Matters, 4, 1–28.
*Pace, T. W., Negi, L. T., Dodson-Lavelle, B., Ozawa-de Silva, B., Reddy, S. D., Cole, S. P., Danese, A., Craighead, L. W., & Raison, C. L. (2013). Engagement with cognitively-based compassion training is associated with reduced salivary C-reactive protein from before to after training in foster care program adolescents. Psychoneuroendocrinology, 38(2), 294-299.https://doi.org/10.1016/j.psyneuen.2012.05.019
Pilla, D., Qina’au, J., Patel, A., Meddaoui, B., Watson, N., Dugad, S., & Saskin, M. (2020). Toward a framework for reporting and differentiating key features of meditation- and mindfulness-based interventions. Mindfulness, 11, 2613–2628. https://doi.org/10.1007/s12671-020-01475-7
*Reddy, S. D., Negi, L. T., Dodson-Lavelle, B., Ozawa-de Silva, B., Pace, T. W., Cole, S. P., Raison, C. L., & Craighead, L. W. (2013). Cognitive-based compassion training: A promising prevention strategy for at-risk adolescents. Journal of Child and Family Studies, 22, 219-230.https://doi.org/10.1007/s10826-012-9571-7
Reeves, B. C., Deeks, J. J., Higgins, J. P. T., Shea, B., Tugwell, P., & Wells, G. A. (2019). Chapter 24: Including non-randomized studies on intervention effects. In J. P. T. Higgins, J. Thomas, J. Chandler, M. Cumpston, T. Li, M. J. Page, & V. A. Welch (Eds.), Cochrane handbook for systematic reviews of interventions (version 6.0) (pp. 595-620). www.training.cochrane.org/handbook
Roeser, R. W., & Eccles, J. S. (2015). Mindfulness and compassion in human development: Introduction to the special section. Developmental Psychology, 51(1), 1–6. https://doi.org/10.1037/a0038453
Roeser, R. W., & Pinela, C. (2014). Mindfulness and compassion training in adolescence: A developmental contemplative science perspective. New Directions for Youth Development, 2014(142), 9–30. https://doi.org/10.1002/yd.20094
Rosenkranz, M. A., Dunne, J. D., & Davidson, R. J. (2019). The next generation of mindfulness-based intervention research: What have we learned and where are we headed? Current Opinion in Psychology, 28, 179–183. https://doi.org/10.1016/j.copsyc.2018.12.022
Salzberg, S. (1995). Lovingkindness: The revolutionary art of happiness. Shambhala.
Schonert-Reichl, K. A., Oberle, E., Lawlor, M. S., Abbott, D., Thomson, K., Oberlander, T. F., & Diamond, A. (2015). Enhancing cognitive and social-emotional development through a simple-to-administer mindfulness-based school program for elementary school children: A randomized controlled trial. Developmental Psychology, 51(1), 52–66. https://doi.org/10.1037/a0038454
Schreier, H. M., Schonert-Reichl, K. A., & Chen, E. (2013). Effect of volunteering on risk factors for cardiovascular disease in adolescents: A randomized controlled trial. JAMA Pediatrics, 167(4), 327–332. https://doi.org/10.1001/jamapediatrics.2013.1100
Shonin, E., Van Gordon, W., Compare, A., Zangeneh, M., & Griffiths, M. D. (2015). Buddhist-derived loving-kindness and compassion meditation for the treatment of psychopathology: A systematic review. Mindfulness, 6(5), 1161–1180. https://doi.org/10.1007/s12671-014-0368-1
Singer, T., & Engert, V. (2019). It matters what you practice: Differential training effects on subjective experience, behavior, brain and body in the ReSource Project. Current Opinion in Psychology, 28, 151–158. https://doi.org/10.1016/j.copsyc.2018.12.005
Spinrad, T. L., & Eisenberg, N. (2017). Compassion in children. In E. M. Seppälä, E. Simon-Thomas, S. L. Brown, C. M. Worline, C. D. Cameron, & J. R. Doty (Eds.), The Oxford handbook of compassion science (pp. 53–63). Oxford University Press.
Strauss, C., Taylor, B. L., Gu, J., Kuyken, W., Baer, R., Jones, F., & Cavanagh, K. (2016). What is compassion and how can we measure it? A review of definitions and measures. Clinical Psychology Review, 47, 15–27. https://doi.org/10.1016/j.cpr.2016.05.004
*Tarrasch, R., Margalit-Shalom, L., & Berger, R. (2017). Enhancing visual perception and motor accuracy among school children through a mindfulness and compassion program. Frontiers in Psychology, 8, 281.https://doi.org/10.3389/fpsyg.2017.00281
*Teodorczuk, K., Guse, T., & du Plessis, G. A. (2019). The effect of positive psychology interventions on hope and well-being of adolescents living in a child and youth care centre. British Journal of Guidance & Counselling, 47(2), 234–245.https://doi.org/10.1080/03069885.2018.1504880
Trautwein, F. M., Kanske, P., Böckler, A., & Singer, T. (2020). Differential benefits of mental training types for attention, compassion, and theory of mind. Cognition, 194, 104039. https://doi.org/10.1016/j.cognition.2019.104039
Waters, L., Barsky, A., Ridd, A., & Allen, K. (2015). Contemplative education: A systematic, evidence-based review of the effect of meditation interventions in schools. Educational Psychology Review, 27(1), 103–134. https://doi.org/10.1007/s10648-014-9258-2
Weare, K. (2019). Mindfulness and contemplative approaches in education. Current Opinion in Psychology, 28, 321–326. https://doi.org/10.1016/j.copsyc.2019.06.001
Weare, K. (2015). What works in promoting social and emotional well-being and responding to mental health problems in schools. National Children’s Bureau. https://www.ncb.org.uk/sites/default/files/uploads/documents/Health_wellbeing_docs/ncb_framework_for_promoting_well-being_and_responding_to_mental_health_in_schools.pdf Accessed 17 July 2017.
Welford, M., & Langmead, K. (2015). Compassion-based initiatives in educational settings. Educational and Child Psychology, 32(1), 71–80.
Weng, H. Y., Fox, A. S., Shackman, A. J., Stodola, D. E., Caldwell, J. Z., Olson, M. C., Rogers, G. M., & Davidson, R. J. (2013). Compassion training alters altruism and neural responses to suffering. Psychological Science, 24(7), 1171–1180. https://doi.org/10.1177/0956797612469537
Weng, H. Y., Schuyler, B., & Davidson, R. J. (2017). The impact of compassion meditation training on the brain and prosocial behavior. In E. M. Seppälä, E. Simon-Thomas, S. L. Brown, C. M. Worline, C. D. Cameron, & J. R. Doty (Eds.), The Oxford handbook of compassion science (pp. 133–146). Oxford University Press.
Weng, H. Y., Lapate, R. C., Stodola, D. E., Rogers, G. M., & Davidson, R. J. (2018). Visual attention to suffering after compassion training is associated with decreased amygdala responses. Frontiers in Psychology, 9, 771. https://doi.org/10.3389/fpsyg.2018.00771
Wentzel, K. R. (2015). Prosocial behavior and peer relations in adolescence. In L. M. Padilla-Walker & G. Carlo (Eds.), Prosocial development: A multidimensional approach (pp. 178–200). Oxford University Press.
Wolke, D., Copeland, W. E., Angold, A., & Costello, E. J. (2013). Impact of bullying in childhood on adult health, wealth, crime, and social outcomes. Psychological Science, 24(10), 1958–1970. https://doi.org/10.1177/0956797613481608
Zeng, X., Chiu, C. P., Wang, R., Oei, T. P., & Leung, F. Y. (2015). The effect of loving-kindness meditation on positive emotions: A meta-analytic review. Frontiers in Psychology, 6, 1693. https://doi.org/10.3389/fpsyg.2015.01693
Zeng, X., Chio, F. H., Oei, T. P., Leung, F. Y., & Liu, X. (2017). A systematic review of associations between amount of meditation practice and outcomes in interventions using the four immeasurables meditations. Frontiers in Psychology, 8, 141. https://doi.org/10.3389/fpsyg.2017.00141
Acknowledgements
We are grateful to Dr. Jo Temple for her assistance with scoping searches and refining the review protocol, and to the three anonymous reviewers for their invaluable feedback.
Funding
This work was supported by the Economic and Social Research Council (grant number ES/J500057/1).
Author information
Authors and Affiliations
Contributions
NP designed the review; conducted the literature search, study selection, data extraction, quality assessment, and data synthesis; and wrote the manuscript. TS conducted the study selection, data extraction, and quality assessment. PS collaborated with the design of the review and resolved disagreements during study selection. All authors commented on previous versions of the manuscript and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical Standards
The manuscript does not contain clinical studies or patient data.
Conflict of Interest
Financial interests: Nicole Perkins teaches mindfulness- and compassion-based interventions for both adults and children in a freelance capacity. Patrick Smith is a co-investigator on a UK NIHR award (NIHR201024): A combined mindfulness-based approach for adolescent non-responders to first-line treatments of depression or anxiety and their carers: Establishing feasibility of implementation and delivery.
Non-financial interests: None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Perkins, N., Sehmbi, T. & Smith, P. Effects of Kindness- and Compassion-Based Meditation on Wellbeing, Prosociality, and Cognitive Functioning in Children and Adolescents: a Systematic Review. Mindfulness 13, 2103–2127 (2022). https://doi.org/10.1007/s12671-022-01925-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12671-022-01925-4