Abstract
Objectives
Moderate mental health problems are highly prevalent and increasing in Swedish schoolchildren, elevating risk for future mental and somatic disability. The aim of this study was to determine whether an 8-week mindfulness-based intervention, Training for Mindfulness and Resilience (TMR), mitigates mental health symptoms and increases resilience during a 2-year follow-up.
Methods
Schoolchildren (aged 9–14 years) reporting moderate mental health problems were randomized into either TMR intervention group (N = 22) or control group, receiving best current practice (N = 12). We used validated questionnaires to measure anxiety, depression, anger, disruptive behavior, self-concept, resilience, stress, and mindfulness before treatment with either TMR or control, as well as at 6 months, 1 year, and 2 years follow-up.
Results
We found a statistically significant effect of TMR intervention vs control, on resilience, anxiety, anger, and disruptive behavior. Compared to baseline, TMR increased the level of resilience at 6 months (p < .001); anxiety at 1 (p < = .033) and 2 years (p = .04); anger at 6 months (p = .004) and 2 years (p = .039); disruptive behavior at 6 months (p = .006). In the control group, a decrease in resilience between 6 months and 2 years (p = .05) was observed. No other significant effects were found in the control group.
Conclusions
This study suggested that TMR improved mental health in schoolchildren with effects on anxiety and anger lasting for 2 years, and on resilience and disruptive behavior lasting for 6 months.
Trial Registration Number
NCT04806542, date of registration 18th of March 2021, retrospectively registered.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Psychosocial stress and poor mental health are the leading causes of disability in young people aged 10–24 years worldwide (Kieling et al., 2011; Patton et al., 2016). A Swedish study describing mental health development in youth showed a marked increase in stress, starting at 13 years of age (Friberg et al., 2012). The National Board of Health and Welfare in Sweden recently published a report about the steep and continuous increase in moderate mental health problems, such as anxiety disorders and depression among children and adolescents (Socialstyrelsen, 2019). This report emphasizes that early debut of mental illness is associated with chronic psychiatric disease and disability later in life, possibly leading to an inability to pursue studies and to thrive in adult working life. At worst, this may lead to an elevated risk for suicidal attempts and, finally, even suicide. The current available treatment protocols for children and adolescents focus mainly on pharmacological treatment (Oreland et al., 2016). Thus, there is a need for developing additional psychological methods to address mental health problems before pharmacological treatment is necessary (Socialstyrelsen, 2019).
The concept of resilience can be defined as systems and processes that, over time, give the individual opportunities for successful adaptation despite difficult and threatening circumstances (Masten & Obradovic, 2006; Rutter, 2012). These processes can take place at various levels, including the community level, family level, and the individual level. A longitudinal study concerning children at risk showed that traumatic life events synergistically magnified the negative effects of risk factors from infancy (O'Grady & Metz, 2012). However, the study showed that the social support these children received increased their ability to self-regulate, which was protective against risk and stress. Prior to and during adolescence, developmental effects related to puberty and brain development lead to new sets of behaviors and capacities that facilitate transitions into adulthood (Dey et al., 2015). This is a vulnerable period during which both social and psychological factors can affect the well-being and health of children and adolescents. Self-control is crucial in the development of resilience. Self-control is related to mental health and well-being and is defined as regulation of and control over the expression of emotions, thoughts, and behavioral impulses (Diamond, 2013). The longitudinal Dunedin study from New Zealand shows that self-control in early life was the most distinct predictor for health, economic stability, and cost to society in adulthood (Moffitt et al., 2011). This result remained even when adjusted for cognitive development, IQ, and socioeconomic factors during childhood. Mindfulness-based interventions (MBIs) have shown potential in improving self-control in youths with impulse control problems (Barnert et al., 2014; Bogels et al., 2008; Papies et al., 2012). However, more knowledge regarding the long-term effects of mindfulness on self-control is needed.
MBIs tailored to children and adolescents constitute a fairly novel field of research. Despite this, there is a plethora of studies showing promising results in reducing behavioral, mental, and cognitive symptoms and improving varying dimensions of mental health and well-being in children and adolescents according to a recent overview (Singh & Singh Joy, 2021). There is a rapidly growing body of evidence for the effectiveness of MBIs in treating various mental as well as somatic disorders in youths (Dunning et al., 2019; Perry-Parrish et al., 2016; Tan & Martin, 2014). There is further evidence that MBIs for children and adolescents promote executive functioning, socio-emotional resilience, positive coping strategies, and a reduction of anxiety and depression (Ames et al., 2014; Henje Blom et al., 2014; Mak et al., 2018; Zoogman et al., 2015). MBIs directed to both adolescents and their parents reduce acting-out behavior and bullying in adolescents while increasing capacity to voluntarily focus attention and decrease stress reactivity in their parents (Bogels et al., 2008; Tan, 2015). It is possible that MBIs strengthen both social support, by reducing stress level and promoting compassion in parents, as well as internal self-control through practicing self-regulation and other mindfulness skills (Haydicky et al., 2015; Liu et al., 2018; Tan, 2015). Furthermore, MBIs have been shown to reduce adverse effects of childhood stress and trauma (Ortiz & Sibinga, 2017). MBIs have therefore become a viable option in modern clinical mental and somatic health practices and research. In order to further the field, more randomized controlled trial (RCT) studies that investigate whether the effects of MBIs in children persist longer than 1 year are needed.
Several of the clinical tools used in international MBI studies usually last for 10–12 weeks (Burke, 2010; Lee et al., 2008; Semple et al., 2010). In a Swedish context, both parents usually work fulltime and share childcare duties (Hwang & Broberg, 2013). An 8-week protocol was therefore developed to increase possibilities for attendance. This 8-week Swedish protocol named Training for Mindfulness and Resilience (TMR) was developed by a group of experienced clinical psychologists with inspiration from a US protocol, called Mindfulness-based Cognitive Therapy for Children (MBCT-C) which is a group-based therapeutic intervention for children with anxiety and depressive symptoms (Semple et al., 2010).
The aims of the present study were twofold. First, we explored whether TMR for children and adolescents can mitigate mental health problems and increase resilience. Second, we investigated for how long the potential effects of TMR would persist. Our hypothesis was that TMR would reduce adverse mental health outcomes such as anxiety, depression, anger, and disruptive behavior, and stimulate resilience, self-concept, and mindfulness and that results would persist over a 2-year period.
Methods
Participants
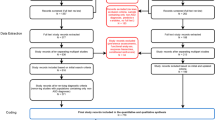
In total, 43 participants with one parent each signed up for the study and were thereafter randomized into either a TMR group or a control group. During the study, three participants were excluded due to psychiatric episodes, according to our criteria for exclusion. Another three participants dropped out of the study. Since we used repeated measures in analyzing our data, we had to leave out the participants who missed one of the follow-up measures from the analysis in the current study. This further excluded three participants from the study (Fig. 1). Finally, a total of 34 participants, aged 9–14 years, were included (Table 1).
We conducted the power analysis based on a study of MBI for children and adolescents (Lagor et al., 2013). This study showed that a 6-week MBI mitigated anxiety measured by Beck Youth Inventories from 58.7 ± 11.1 before MBI to 52.0 ± 10.0 after MBI. The levels of anxiety were presented as t-scores converted according to an appendix in the BYI II manual (Beck et al., 2005). To achieve this change in anxiety with an alpha value of 0.05, power of 80%, and a non-response/dropout of 20% in a parallel group study, 102 participants were required assuming equal randomization. Due to a lack of participants that fulfilled the inclusion and were exempted by the exclusion criteria, we were not able to recruit the 102 participants that we originally aimed for.
Procedures
Recruitment for the study was performed at an Educational Mental Health Care Clinic in Gothenburg, Sweden, where parents seek assistance for their children with mild to moderate mental health problems. In order to strengthen the external validity of the study, we chose recruiting from the Educational Health Care Services, as it is a common clinical setting for all Swedish schoolchildren with mild to moderate mental health symptoms. The staff leading the TMR intervention were all licensed child psychologists who were educated in how to lead mindfulness-based programs for the purpose of this study. The Clinic psychologists were informed about the current study and the possibility to include patients. The project leader and/or research assistant were alerted when patients that could fit the criteria for the study were identified. If a patient was suitable, a thorough clinical interview took place by one of the clinical psychologists in our study. After considering the inclusion and exclusion criteria, the patient was recruited to the study. A flowchart of activities is presented in Fig. 2.
All participants were asked to fill out the questionnaires administered in a paper–pencil format, just prior to the TMR intervention and directly after the TMR intervention at the Clinic where the TMR intervention took place. The follow-up measurements occurred at 6 months, 1 year, and 2 years post TMR intervention and took place before booster sessions (Fig. 2). Where possible, the questionnaires were filled out at the Clinic or else they were posted to participants with a stamped envelope.
Inclusion and Exclusion Criteria
The diagnostic criteria for inclusion and exclusion were based on the ICD-10 manual with updated diagnostics for mental health disorders (WHO, 1992) and for inclusion the following diagnoses were used: F32.0 Mild depressive episode; F32.1 Moderate depressive episode; F41 Anxiety disorders; F43 Reactions to stress; F51 Nonorganic sleep disorders; F93 Emotional disorders with onset specific to childhood; F94.8 Other childhood disorders of social functioning; F94.9 Other childhood disorder of social functioning, unspecified.
The criteria for exclusion from the study were general, rather than diagnose specific: ongoing treatment for severe psychiatric disorders (F20–29, F31–F33.3); cognitive disorders; difficulties in understanding Swedish; neuropsychiatric considerations and diagnosis; learning disabilities with difficulties in verbal understanding; ongoing parental conflict in conjunction with separation or divorce, since this was deemed to risk an escalation of mental health problems and additionally add practical problems that might reduce the child’s possibilities to attend the sessions; attending less than 5 of the 8 sessions of the TMR program. The criteria for inclusion and exclusion were held as close to the clinic’s general criteria as possible to improve external validity.
Randomization
This study was designed as a randomized controlled trial (RCT). In order to fulfil treatment requirements for a group intervention, we deemed the TMR group needed to have, at least, six participants per treatment group. This number of participants created a safety buffer in the case of participants dropping out, falling sick, or reaching the criteria for exclusion during the intervention. The flow of patients in the Mental Health Clinic matching our criteria for inclusion was insufficient to keep the numbers of patients equal in both TMR group and control group. We were therefore compelled to prioritize the number of participants in the TMR group in order to be able to carry out the study. We used an unequal randomization process where non-identifiable codes were assigned to either TMR group or control group by the Clinic Manager, who was not part of the research team. The unequal randomization means that we allocated more participants to the TMR group as compared with the control group in order to reach a minimum of 6 participants for the TMR group. The randomization ratio (TMR vs. control group) was 1.4:1. According to Pocock (1979), randomization in a ratio of 2:1 or 3:2 does not greatly alter the statistical properties of a trial.
TMR Intervention
The TMR intervention consisted of weekly sessions, each lasting for 2 h, in groups of 6–8 participants, for a total of 8 weeks. Each weekly lesson contained an essential theme with a purpose to further mindful awareness in the participants. The themes were ordered in the following sequence: the first week dealt with the automatic pilot reactions and simple exercises to address those reactions; the second week addressed the hindrances for practice with awareness exercises to discover those hindrances and make more conscious choices; the theme of the third week explored non-judgmental awareness with focus on describing rather than judging inner and outer phenomena; the fourth week dealt with the themes of stress and coping; the fifth week focused on acceptance in order to help the participants to remain in the present moment, rather than ruminating over the past or worrying about the possible future catastrophes; the theme of the sixth week was compassion training directed to self and others; the seventh week was devoted to gathering material for a maintenance plan to be used after the intervention and setting a future intention for the continued practice and the final theme of week 8 was to reflect over the plans made during week for future practice and evaluate the skills acquired. The TMR intervention combined practical mindfulness exercises with theoretical sessions in order to embody the message of the intervention by experience-based learning and illuminate the theoretical aspects by reflection. The content of the 8-week program was structured and presented in the order shown in Table 2.
Parents/caregivers were invited to attend two separate adult sessions to gain information about the program, the progress of the group and the individual child and to experience some of the exercises in the protocol. The agency of the child was underlined as a benchmark for whether the parents ought to practice together with the child or not.
In addition to the 8-week intervention, the participants were offered 3 booster sessions; the first booster session was given 6 months after the TMR intervention, the second booster was given after 1 year, and the third booster was given 2 years after the intervention (Fig. 2). The booster sessions were designed to reiterate important points from the program, stimulate to further practice, and refresh the skills and insights targeted during the 8-week TMR.
Best Current Practice
The control group received best current practice as intervention. This consisted of individual counselling sessions offered by a school counsellor or a child psychologist. The number of sessions was based on the need of the patient and varied between 1 and 15 sessions. The school counsellor was either a school nurse with experience of mental health problems in schoolchildren or a social worker. The second option was a child psychologist at the Mental Health Clinic, where the study took place. The way that counselling is carried out in Educational Mental Health Care in Sweden is not uniform.
Measures
Beck Youth Inventories
Primary outcomes mental health was measured using Beck Youth Inventories (BYI). BYI encompasses 100 items, divided into 5 subscales that measure anxiety, depression, anger, disruptive behavior, and self-concept respectively. Each subscale consists of 20 statements. Each statement is rated on a 4-point Likert scale ranging from never (0 points) to always (3 points). The scores were calculated separately for each subscale and the total sum of each subscale can range between 0 and 60 points. A maximum of two missing items in each subscale was accepted and missing items were replaced by intrapersonal means of each subscale before a total score was calculated. Higher scores on the anxiety, depression, anger, and disruptive behavior inventories indicate a higher symptom load and hence a more negative outcome, while a higher score on the Self-Concept Inventory indicates a positive outcome (Beck et al., 2005). BYI has been translated from English to Swedish, and has been studied extensively on 2000 Swedish youths, from standardized samples drawn from different Swedish regions and from various clinical and school settings, producing normative data showing good psychometric characteristics (Tideman, 2004). The BYI subscales have norm group mean and clinical mean values; Anxiety: 10.3 and 16.6; Depression: 10.5 and 20.2; Anger: 9.7 and 20.5; Disruptive behavior: 5.4 and 15.3; Self-concept: 40.8 and 22.6. Cronbach’s alpha coefficients based on baseline data of our sample were 0.906 for anxiety, 0.924 for depression, 0.939 for anger, 0.813 for disruptive behavior, and 0.937 for self-concept.
Resilience Scale 10
Resilience scale 10 (RS10) is a 10-item shortened version of the well-validated 25-item Resilience scale, which has been widely used in international studies on psychological resilience since 1994 (Wagnild & Young, 1993). RS10 measures individual resilience through five underlying dimensions: sense of purpose and meaning, authenticity, equanimity, self-reliance, and perseverance (Wagnild, 2012). Each statement is rated on a 4-point Likert scale ranging from “not at all like me” (1 point) to “very much like me” (4 points) with a maximum of 40 points. The RS10 scale is not developed for clinical use, rather it is a strengths-based tool that measures a child’s capacity to respond in a positive way to challenges. Hence, a higher score only points towards a more favorable outcome with regard to psychological resilience. Cronbach’s alpha coefficient based on baseline data of our sample was 0.833.
Stress in Children Questionnaire
The Stress in Children (SiC) questionnaire was used to measure the level of stress in the participants. The 21-item SiC measures three dimensions of subjective stress, namely lack of well-being, distress, and lack of social support (Osika et al., 2007). Each item is scored on a 4-point Likert scale ranging from none (0 points) to always (3 points). A maximum of two missing items was accepted and a mean score, i.e., SiC Global Mean Score (GMS), was calculated for each participant. Although SiC is not a clinical scale, the following cutoffs have been used: the score < 2 indicates a lack of stress, and the scores 2–2.49 are norm group scores, while score > 2.5 indicates stressed states. The SiC has been validated against BYI (Osika et al., 2007). Cronbach’s alpha coefficient based on baseline data of our sample was 0.824.
Child and Adolescent Mindfulness Measure
The 10-item Child and Adolescent Mindfulness Measure (CAMM) measures the capacity for mindfulness in children and adolescents aged 10–17 years (Greco et al., 2011). The participants were asked to rate how true each item reflected their experience, using a 5-point Likert scale ranging from never true (0 points) to always true (4 points). A total mindfulness score was generated by reversely scoring negatively worded items and thereafter summing all items, ranging from 0 to 40 points. A maximum of one missing item was accepted and missing item was replaced by intrapersonal means before a total score was calculated. Higher score indicates a higher level of mindfulness. The CAMM scale is not developed for clinical use, rather it assesses present-moment awareness and non-judgmental, non-avoidant responses to thoughts and feelings in children and adolescents. Hence, a higher score only points towards a more favorable outcome with regard to present moment awareness. The Cronbach alpha coefficient based on baseline data of our sample was 0.801.
Data Analyses
To compare baseline variables across the two groups, we used an independent t-test for normally distributed variables, Wilcoxon signed rank test for variables with skewed distribution, and Chi-square test for gender. To explore whether the effects of the TMR over the 2-year period may differ from the effects of the best current practice, we performed analysis on data collected at baseline and the follow-ups at 6 months, 1 year, and 2 years using a general linear model for repeated measures. The data collected directly after the intervention were not included in the analysis due to a lack of data for three participants. When there was a statistically significant difference between the two groups, we further examined the effects within subjects in the TMR and control groups separately, using ANOVA with Bonferroni correction for multiple comparisons. To examine effect size, partial eta squared ŋp2 for time × group interaction and Hedges’ g (a correction for Cohen’s d given small sample size in this study) for pairwise comparisons were reported. All statistical analyses were performed with IBM SPSS 26. A two-sided p ≤ 0.05 was considered as statistically significant.
Results
There were no statistically significant differences in age and gender distribution between the TMR group and the control group (Table 1), neither in baseline measures of stress, resilience, mindfulness, anxiety, depression, anger, disruptive behavior, nor self-concept between the two groups (Table 3).
All participants in the TMR group participated in at least 5 of the 8 sessions of the TMR program, which was a criterion we had set up as an acceptable rate of attendance. Firstly, we explored whether TMR for children and adolescents can mitigate symptoms of mental health and increase resilience in comparison with the control group by examining the interaction terms between time and group in the general linear model analysis. We found a statistically significant time × group interaction in resilience (F(3, 96) = 3.505, p=0.018, partial eta squared ŋp2 = 0.099), anxiety (F(3, 93) = 2.980, p=0.046, ŋp2 = 0.088), anger (F(3, 93) = 4.399, p=0.013, ŋp2 = 0.124), and disruptive behavior (F(3, 93) = 2.696, p = 0.05, ŋp2 = 0.08), as shown in Table 3. Thus, in comparison with the control group, the 8-week TMR intervention reduced the levels of anxiety, anger, and disruptive behavior and increased resilience. The ŋp2 ranged from 0.08 to 0.124, indicating medium effects according to Cohen’s benchmarks to define small (ŋp2 = 0.01), medium (ŋp2 = 0.06), and large (ŋp2 = 0.14) effects (Cohen, 1988).
There was no significant time × group interaction in depression (F(3, 93) = 0.441, p = 0.725), self-concept (F(3, 93) = 2.232, p = 0.090), mindfulness (F (3, 96) = 0.702, p = 0.553), stress global scale (F(3, 96) = 1.240, p = 0.300), distress (F(3, 96) = 0.330, p = 0.803), lack of well-being (F(3, 96) = 2.139, p = 0.100), and lack of social support (F(3, 96) = 1.622, p = 0.189).
Having found group differences in anxiety, anger, disruptive behavior, and resilience, we examined the changes over time in the TMR group and control group separately to see how long the effects of TMR would persist. We observed statistically significant changes over time in the TMR group (Anxiety: F(3, 63) = 4.417, p = 0.007); Anger: F(3, 63) = 5.574, p = 009; Disruptive behavior: F(3, 63) = 4.282, p = 0.008), but not in the control (Anxiety: F(3, 30) = 0.967, p = 0.421; Anger: F(3, 30) = 1.517, p = 0.241; Disruptive behavior: F(3, 30) = 2.675, p = 0.065).
Pairwise comparisons using ANOVA with Bonferroni correction showed that the TMR group exhibited a statistically significant decrease in the level of anxiety at 1 year (p = 0.033, Hedges’ g = 0.70) and 2 years (p = 0.04, Hedges’ g = 0.59) after intervention when compared with the baseline. For the level of anger, the TMR group exhibited a statistically significant decrease at 6 months (p = 0.004, Hedges’ g = 0.47) and 2 years (p = 0.039, Hedges’ g = 0.57) after intervention when compared with the baseline. For the level of disruptive behavior, the TMR group exhibited a significant decrease at 6 months after intervention as compared with the baseline (p = 0.006, Hedges’ g = 0.52).
Regarding the level of resilience, we observed statistically significant changes over time in both the TMR group (F(3, 63) = 4.342, p = 0.008) and the control group (F(3, 33) = 3.512, p = 0.026). Pairwise comparisons revealed that the level of resilience increased in the TMR group at 6 months after the intervention when compared with the baseline (p < 0.001, Hedges’ g = 0.79). In the control group, however, we observed a statistically significant decrease in resilience at follow-up 4 when compared to follow-up 2 (p = 0.05, Hedges’ g = 0.59). For pairwise comparisons, Hedges’ g ranged from 0.5 to 0.8, indicating medium to large effects according to Cohen’s benchmarks to define small (d = 0.2), medium (d = 0.5), and large (d = 0.8) effects (Cohen, 1988).
To evaluate the clinical consequences of these effects, we examined the variables that were significantly changed by TMR in relation to available clinical means. For anxiety, the percentages of participants who scored above the clinical mean were 59.1%, 18.2%, 27.3%, and 27.3% in the TMR group at baseline, 6 months, 1 year, and 2 years after intervention, respectively, while the corresponding percentages were 41.7%, 54.5%, 58.3%, and 50.0% in the control group. For anger, the percentages of participants who scored above the clinical mean were 18.2%, 13.6%, 9.1%, and 18.2% in the TMR group at baseline, 6 months, 1 year, and 2 years after intervention, respectively, while the corresponding percentages were 33.3%, 36.4%, 25.0%, and 50.0% in the control group. For disruptive behavior, majority of the participants in both groups scored under the clinical mean. The RS-10 scale does not have any known clinical cutoff; hence, it is difficult to comment on clinical significance for this measure.
Discussion
In the present study, we found that an 8-week TMR intervention appeared to increase the level of resilience and decreased the levels of anxiety, anger, and disruptive behavior in children and adolescents with moderate mental health problems. The effects of TMR intervention on anxiety and anger seem to persist over the 2-year follow-up period. No improvement was seen in the control group that received the best current practice. Instead, a decrease in resilience between 6 months and 2 years was observed.
We hypothesized that TMR would be more effective than the best current practice in mitigating moderate mental health symptoms and increasing resilience and that the effects would be sustained over a 2-year period. Our hypothesis was partly verified by the results, which suggested that TMR alleviated some symptoms of moderate mental health problems and increased resilience as compared to the control group. Benefits such as reduced anxiety and anger seemed to persist over 2 years. Increased resilience and disruptive behavior probably persisted over 6 months.
Mindfulness-based interventions have demonstrated efficacy in treating a variety of mental health problems, such as anxiety, depression, problems with attention, and somatization, and improving resilience (Blom et al., 2017; Perry-Parrish et al., 2016). Our data regarding resilience, anxiety, anger, and disruptive behavior are to a large extent in line with these studies. In addition, our results suggested that the improvements may have persisted during a 2-year period.
Although at the follow-ups after 1 and 2 years, there was a statistically significant decrease in anxiety, no significant improvement was observed at 6 months. Since the majority of the participants were under the age of 12, with median age of 11.5 for TMR group and 11 years for the control group, they were still at an age before the common major onset of the serious increase in mental health problems, at age 14 (Kessler et al., 2007). A plausible hypothesis may be that problems with anxiety were not fully developed in the participants of either TMR group or control group at baseline. However, as time went on, it seemed that the TMR group acquired tools to handle the onset of anxiety in a more effective way than the control group.
We found statistically significant decrease in the level of anger at the 6-month and 2-year follow-ups but not at the 1-year follow-up. Externalizing behaviors, being the second leading cause of disease burden in young adolescents, tend to peak at 10–14 years according to a current international factsheet (WHO, 2020). Interestingly, the TMR group did not show the expected peak in anger, which was seen in the control group. The significant decrease in the level of disruptive behavior at 6-month follow-up in the TMR group was not followed by further decrease at the 1- and 2-year follow-ups. In the control group, there was a slight, although non-significant, increase in the level of disruptive behavior towards the end of the study period. The TMR intervention might have been protective against symptoms of disruptive behavior.
We did not find statistically significant effect of TMR on the level of self-assessed mindfulness. Problems associated with measuring mindfulness by self-report are not unknown (Goodman et al., 2017). One such challenge in measurement can be that those with less mindfulness training may have less insight into the nature of their own minds and hence be less likely to report the level of mindfulness accurately. The more experienced practitioners may see their thoughts and behaviors with more insight and clarity and subsequently self-report lesser levels of mindfulness (Grossman, 2011). Furthermore, we compared the CAMM values in our participants with data from a population of healthy children (Greco et al., 2011) and found them to be similar. Hence, it is plausible to assume that the group of children in our study were not specifically low in the level of mindfulness at baseline, measured by the CAMM, and therefore there was not much room for further progress during the 8-week TMR intervention. Finally, it is noteworthy that some studies show that the CAMM may not be a sensitive enough instrument to measure mindfulness developed in meditation or yoga practice in children (de Bruin et al., 2011, 2014).
We did not find any effect of the TMR intervention on self-assessed stress as measured by the SiC questionnaire. A Swedish research team found in a study of a MBI for pupils in grades 5, 7, and 8 significant improvement in pupils’ capacity for effortful control, feelings of well-being at school, and perceived peer relations (Terjestam et al., 2016). They showed that the positive effects increased with the number of times the participants took part in the MBI training, for all but one of the measures, which was “general stress” measured by the SiC questionnaire. Also, a team who studied the effect of yoga using the SiC questionnaire found no significant differences in self-perceived stress levels between the control group and the treatment groups (Smith-Vogtmann, 2009). We speculate that TMR may have changed the way children and adolescents coped with stressors (Tabibnia, 2020; Ursin & Eriksen, 2004, 2010). This is in line with our data that the TMR intervention may increase resilience, defined as successful adaptation despite difficult and threatening circumstances (Rutter, 2012). In a review by Tabibnia (2020), the three general routes to resilience are identified: (1) downregulating the negative, (2) upregulating the positive, and (3) transcending the self. The author concludes that some strategies, including social support and mindfulness, can boost resilience via more than one route. Furthermore, the stress levels in both the TMR group and control group were all within a normal span; hence, there was not much room for improvement for our study participants.
In the control group, however, there was a statistically significant decrease in resilience during the entire study period. Keeping in mind that our study participants are children and adolescents with moderate mental health problems, the decrease in resilience may have impact on their future mental health. The effect of TMR on resilience is encouraging as a contrast to the decreasing tendency in resilience seen in the control group. Hence, our data suggested that the TMR intervention helped children and adolescents cope with stress through increasing resilience.
Self-control is of utmost importance for resilience in particular and adequate human development in general (Moffitt et al., 2011). It consists of, among other skills, the ability to regulate emotions and impulsive and inattentive behavior. The significant decreases in anxiety, anger, and disruptive behavior in the TMR group suggest that the TMR intervention may increase self-control. Apart from the decrease in symptoms, which benefit mental health and well-being in the short-term, the possible consequences of the TMR on self-control may still be more valuable in the long term.
Limitations and Future Research
One major limitation of our study is the small sample size, which was mainly due to the limited flow of patients in our clinic who met our criteria of inclusion and exclusion. Our small sample size has decreased the power of this study. Thus, the findings are only tentative and should be interpreted with caution. Another limitation is multiple testing that may have increased type I error. The main purpose of this study was to evaluate whether an 8-week TMR intervention would improve mental health measured by the Beck Youth Inventory. We measured other variables such as mindfulness, stress, and resilience to help us to understand the effect of the TMR; thus, these variables are more of an exploratory nature and considered secondary outcomes. Since the secondary outcomes were mainly hypothesis-generating and not so much hypothesis-controlling, we believe that findings worthy of further research might be missed by applying a too rigid p-value adjustment. Furthermore, as pointed out by Bender and Lange (2001), methods to adjust for multiple testing in studies collecting repeated measurements are rare. Third, even though we used an active control group, it differed from the TMR group in some characteristics, such as the children allotted to the TMR group having a possibility to practice mindfulness exercises at home with their parents. Fourth, there were almost twice as many females as males in both the TMR group and the control group. The unequal gender ratio in our study mirrors rather correctly the gender distribution of children and adolescents who seek help from the student mental health clinic where the study took place and the gender ratio in several longitudinal studies of mental health problems in youth, both Swedish and international (Chen et al., 2012; Dey et al., 2015; Potrebny et al., 2017). Given the small sample size, this uneven gender ratio made it impossible to compare effects between males and females.
Most participants attended 7–8 sessions and very few of them missed 2–3 sessions. Regrettably, since some of the lists of attendance disappeared, we were unable to analyze the number of sessions per participant. Thus, we were not able to analyze whether missing a specific session may have influenced the effects reported. We discussed whether the 8 sessions could be shortened into 6 sessions in a clinical setting. Participants may miss one or more sessions because they get sick, need to attend other activities, or if their parents are unable to take them to the session. We considered that shortening the program to 6 sessions may risk lessening the effects of the intervention should the participants who missed a session not be given the opportunity to catch up. Having discussed this with the clinicians, we conclude it is valuable for the children missing some sessions to be given an opportunity to catch up with the group and the practice.
As none of the children from the TMR-group wished to attend the third booster session, we inquired about the reasons for their absence. One of the objections given by the participants was that they had overcome their difficulties and did not want to be reminded of them by visiting the clinic. Some of the older participants had, by the time of the third booster session, reached well into their teens (15–16 years of age) and they found the TMR program somewhat infantile for the age they had now reached. The latter objective may be resolved by changing the booster protocol with new material adapted to a teen population, both in layout of the visual materials as well as the language used. It could also be reasonable to assume that 2 booster sessions are enough for this protocol and age group.
Using the TMR protocol as with all MBIs requires prior knowledge in mindfulness, which means it cannot be implemented without investing in education in mindfulness for clinical staff. However, this is common practice during implementation of new methods and accounted for by clinical managers in primary healthcare. Mindfulness also contributes to the well-being of the staff, making it a sustainable method within the healthcare organization (Boellinghaus et al., 2014; Shapiro & Carlson, 2009; Verweij et al., 2018). Mindfulness as a method is gaining ground in research as well as in clinical care both in Sweden and internationally. To strengthen external validity, studies evaluating the efficacy of the TMR protocol within other levels of Mental Health Care for children and adolescents are important.
In order to further develop this field of research, longitudinal RCT studies with more participants are needed. In particular, a larger number of participants would open the possibility to replicate our results that TMR mitigates mental health symptoms and increases resilience over time. Furthermore, a larger number of participants would enable studying whether gender, age, and/or family socioeconomic status may influence the effects of MBIs.
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Ames, C. S., Richardson, J., Payne, S., Smith, P., & Leigh, E. (2014). Innovations in practice: Mindfulness-based cognitive therapy for depression in adolescents. Child and Adolescent Mental Health, 19(1), 74–78. https://doi.org/10.1111/camh.12034
Barnert, E. S., Himelstein, S., Herbert, S., Garcia-Romeu, A., & Chamberlain, L. J. (2014). Innovations in practice: Exploring an intensive meditation intervention for incarcerated youth. Child and Adolescent Mental Health, 19(1), 69–73. https://doi.org/10.1111/camh.12019
Beck, J. S., Beck, A. T., Jolly, J. B., & Steer, R. A. (2005). Beck Youth Inventories (2nd ed.). The Psychological Corporation.
Bender, R., & Lange, S. (2001). Adjusting for multiple testing - when and how? Journal of Clinical Epidemiology, 54(2001), 343–349. https://doi.org/10.1016/S0895-4356(00)00314-0
Blom, E. H., Tymofiyeva, O., Chesney, M. A., Ho, T. C., Moran, P., Connolly, C. G., Duncan, L. G., Baldini, L., Weng, H. Y., Acree, M., Goldman, V., Hecht, F. M., & Yang, T. T. (2017). Feasibility and preliminary efficacy of a novel RDoC-based treatment program for adolescent depression: “Training for Awareness Resilience and Action” (TARA) - a pilot study. Frontiers in Psychiatry, 7, 208. https://doi.org/10.3389/fpsyt.2016.00208
Boellinghaus, I., Jones, F., & Hutton, J. (2014). The role of mindfulness and loving-kindness meditation in cultivating self-compassion and other-focused concern in health care professionals. Mindfulness, 5(2), 129–138. https://doi.org/10.1007/s12671-012-0158-6
Bogels, S., Hoogstad, B., van Dun, L., De Shutter, S., & Restifo, K. (2008). Mindfulness training for adolescents with externalising disorders and their parents. Behavioural and Cognitive Psychotherapy, 36(2), 193–209. https://doi.org/10.1017/S1352465808004190
Burke, C. (2010). Mindfulness-based approaches with children and adolescents: A preliminary review in an emergent field. Journal of Child and Family Studies, 19(2), 133–144. https://doi.org/10.1007/s10826-009-9282-x
Chen, Y., Dangardt, F., Osika, W., Berggren, K., Gronowitz, E., & Friberg, P. (2012). Age- and sex-related differences in vascular function and vascular response to mental stress. Longitudinal and cross-sectional studies in a cohort of healthy children and adolescents. Atherosclerosis, 220(1), 269–274. https://doi.org/10.1016/j.atherosclerosis.2011.10.030
Cohen, J. (1988). Statistical power analysis for the behavioral sciences (2nd ed.). Hillsdale, NJ: Lawrence Erlbaum Associates, Publishers.
de Bruin, E. I., Zijlstra, B. J., van de Weijer-Bergsma, E., & Bögels, S. M. (2011). The Mindful Attention Awareness Scale for Adolescents (MAAS-A): Psychometric properties in a Dutch sample. Mindfulness, 2(3), 201–211. https://doi.org/10.1007/s12671-011-0061-6
de Bruin, E. I., Zijlstra, B. J. H., & Bögels, S. M. (2014). The meaning of mindfulness in children and adolescents: Further validation of the Child and Adolescent Mindfulness Measure (CAMM) in two independent samples from the Netherlands. Mindfulness, 5, 422–430. https://doi.org/10.1007/s12671-013-0196-8
Dey, M., Jorm, A. F., & Mackinnon, A. J. (2015). Cross-sectional time trends in psychological and somatic health complaints among adolescents: A structural equation modelling analysis of “health Behaviour in School-Aged Children” data from Switzerland. Social Psychiatry and Psychiatric Epidemiology, 50(8), 1189–1198. https://doi.org/10.1007/s00127-015-1040-3
Diamond, A. (2013). Executive functions. Annual Review of Psychology, 64, 135–168. https://doi.org/10.1146/annurev-psych-113011-143750
Dunning, D. L., Griffiths, K., Kuyken, W., Crane, C., Foulkes, L., Parker, J., & Dalgleish, T. (2019). Research review: The effects of mindfulness-based interventions on cognition and mental health in children and adolescents–a meta-analysis of randomized controlled trials. Journal of Child Psychology and Psychiatry, 60(3), 244–258. https://doi.org/10.1111/jcpp.12980
Friberg, P., Hagquist, C., & Osika, W. (2012). Self-perceived psychosomatic health in Swedish children, adolescents and young adults: An Internet-based survey over time. British Medical Journal Open, 2(4), e000681. https://www.ncbi.nlm.nih.gov/pubmed/22855621
Goodman, M. S., Madni, L. A., & Semple, R. J. (2017). Measuring mindfulness in youth: Review of current assessments, challenges, and future directions. Mindfulness, 8(6), 1409–1420. https://doi.org/10.1007/s12671-017-0719-9
Greco, L. A., Baer, R. A., & Smith, G. T. (2011). Assessing mindfulness in children and adolescents: Development and validation of the Child and Adolescent Mindfulness Measure (CAMM). Psychological Assessment, 23(3), 606–614. https://doi.org/10.1037/a0022819
Grossman, P. (2011). Defining mindfulness by how poorly I think I pay attention during everyday awareness and other intractable problems for psychology’s (re)invention of mindfulness: Comment on Brown et al. Psychological Assessment, 23(4), 1041–1046. https://doi.org/10.1037/a0022713
Haydicky, J., Shecter, C., Wiener, J., & Ducharme, J. M. (2015). Evaluation of MBCT for adolescents with ADHD and their parents: Impact on individual and family functioning. Journal of Child and Family Studies, 24(1), 76–94. https://doi.org/10.1007/s10826-013-9815-1
Henje Blom, E., Duncan, L. G., Ho, T. C., Connolly, C. G., LeWinn, K. Z., Chesney, M., Hecht, F. M., & Yang, T. T. (2014). The development of an RDoC-based treatment program for adolescent depression: “Training for Awareness, Resilience, and Action” (TARA). Frontiers in Human Neuroscience, 8, 630. https://doi.org/10.3389/fnhum.2014.00630
Hwang, C. P., & Broberg, A. G. (2013). The historical and social context of child care in Sweden. In M. E. Lamb, K. J. Sternberg, C. P. Hwang, & A. G. E. Broberg (Eds.), Child care in context: Cross-cultural perspectives (1st ed., pp. 28). Psychology Press. https://doi.org/10.4324/9781315799612
Kessler, R. C., Angermeyer, M., C. A. J., DE Graaf, R., Demyttenaere, K., Gasquet, I., DE Girolamo, G., Gluzman, S., Gureje, O., Haro, J. M., Kawakami, N., Karam, A., Levinson, D., Medina Mora, M. E., Oakley Browne, M. A., Posada-Villa, J., Stein, D. J., Adley Tsang, C. H., Aguilar-Gaxiola, S., Alonso, J., …, & Ustün, T. B. (2007). Lifetime prevalence and age-of-onset distributions of mental disorders in the World Health Organization’s world mental health survey initiative. World Psychiatry: Official Journal of the World Psychiatric Association (WPA), 6(3), 168-176.
Kieling, C., Baker-Henningham, H., Belfer, M., Conti, G., Ertem, I., Omigbodun, O., Rohde, L. A., Srinath, S., Ulkuer, N., & Rahman, A. (2011). Child and adolescent mental health worldwide: Evidence for action. Lancet, 378(9801), 1515–1525. https://doi.org/10.1016/S0140-6736(11)60827-1
Lagor, A. F., Williams, D. J., Lerner, J. B., & McClure, K. S. (2013). Lessons learned from a mindfulness-based intervention with chronically ill youth. Clinical Practice in Pediatric Psychology, 1(2), 146–158. https://doi.org/10.1037/cpp0000015
Lee, J., Semple, R. J., Rosa, D., & Miller, L. (2008). Mindfulness-based cognitive therapy for children: Results of a pilot study. Journal of Cognitive Psychotherapy, 22(1), 15–28. https://doi.org/10.1891/0889.8391.22.1.15
Liu, Q.-Q., Zhou, Z.-K., Yang, X.-J., Kong, F.-C., Sun, X.-J., & Fan, C.-Y. (2018). Mindfulness and sleep quality in adolescents: Analysis of rumination as a mediator and self-control as a moderator. Personality and Individual Differences, 122, 171–176. https://doi.org/10.1016/j.paid.2017.10.031
Mak, C., Whittingham, K., Cunnington, R., & Boyd, R. N. (2018). Efficacy of mindfulness-based interventions for attention and executive function in children and adolescents—a systematic review. Mindfulness, 9(1), 59–78. https://doi.org/10.1007/s12671-017-0770-6
Masten, A. S., & Obradovic, J. (2006). Competence and resilience in development. Annals of the New York Academy of Sciences, 1094(1), 13–27. https://doi.org/10.1196/annals.1376.003
Moffitt, T. E., Arseneault, L., Belsky, D., Dickson, N., Hancox, R. J., Harrington, H., Houts, R., Poulton, R., Roberts, B. W., Ross, S., Sears, M. R., Thomson, W. M., & Caspi, A. (2011). A gradient of childhood self-control predicts health, wealth, and public safety. Proceedings of the National Academy of Sciences of the United States of America, 108(7), 2693–2698. https://doi.org/10.1073/pnas.1010076108
O’Grady, D., & Metz, J. R. (2012). Resilience in children at high risk for psychological disorders. Journal of Pediatric Psychology, 12(1), 3–23. https://doi.org/10.1093/jpepsy/12.1.3
Oreland, L., Jarbin, H., Ivarsson, T., Wallin, L., Westholm, C. W., Adler, M., von Knorring, L., Djurfeldt, D. R., Rück, C., Magnusson, Å., Bendix, M., Blomdal, M., Tham, A., & Wahlström, L. (2016). Depression, ångestsyndrom och tvångssyndrom hos barn och vuxna-behandlingsrekommendation. Information Från Läkemedelsverket, 27(6), 26–59.
Ortiz, R., & Sibinga, E. M. (2017). The role of mindfulness in reducing the adverse effects of childhood stress and trauma. Children (basel), 4(3), 16. https://doi.org/10.3390/children4030016
Osika, W., Friberg, P., & Wahrborg, P. (2007). A new short self-rating questionnaire to assess stress in children. International Journal of Behavioral Medicine, 14(2), 108–117. https://doi.org/10.1007/BF03004176
Papies, E. K., Barsalou, L. W., & Custers, R. (2012). Mindful attention prevents mindless impulses. Social Psychological and Personality Science, 3(3), 291–299. https://doi.org/10.1177/1948550611419031
Patton, G. C., Sawyer, S. M., Santelli, J. S., Ross, D. A., Afifi, R., Allen, N. B., Arora, M., Azzopardi, P., Baldwin, W., Bonell, C., Kakuma, R., Kennedy, E., Mahon, J., McGovern, T., Mokdad, A. H., Patel, V., Petroni, S., Reavley, N., Taiwo, K., & Viner, R. M. (2016). Our future: A Lancet commission on adolescent health and wellbeing. Lancet, 387(10036), 2423–2478. https://doi.org/10.1016/S0140-6736(16)00579-1
Perry-Parrish, C., Copeland-Linder, N., Webb, L., & Sibinga, E. M. (2016). Mindfulness-based approaches for children and youth. Current Problems in Pediatric and Adolescent Health Care, 46(6), 172–178. https://doi.org/10.1016/j.cppeds.2015.12.006
Pocock, S. J. (1979). Allocation of patients to treatment in clinical trials. Biometrics, 35(1), 183–197. https://doi.org/10.2307/2529944
Potrebny, T., Wiium, N., & Lundegård, M. M. (2017). Temporal trends in adolescents’ self-reported psychosomatic health complaints from 1980–2016: A systematic review and meta-analysis. Public Library of Science ONE, 12(11), e0188374.
Rutter, M. (2012). Resilience as a dynamic concept. Developemental Psychopathology, 24(2), 335–344. https://doi.org/10.1017/S0954579412000028
Semple, R. J., Lee, J., Rosa, D., & Miller, L. F. (2010). A randomized trial of mindfulness-based cognitive therapy for children - promoting mindful attention to social-emotional resiliency in children. Journal of Child and Family Studies, 19(2), 218–229. https://doi.org/10.1007/s10826-009-9301-y
Shapiro, S. L., & Carlson, L. E. (2009). The art and science of mindfulness: Integrating mindfulness into psychology and the helping professions. American Psychological Association. https://doi.org/10.1037/11885-000
Singh, N. N., & Singh Joy, S. D. (2021). Mindfulness-based interventions with children and adolescents. Routledge.
Smith-Vogtmann, H. (2009). The effects of yoga on children’s self-perceived stress and coping abilities. [Master's Theses and Doctoral Dissertations., Eastern Michigan University]. https://commons.emich.edu/theses/246
Socialstyrelsen. (2019). Psykiatrisk vård och behandling till barn och unga - Öppna jämförelser 2019. https://www.socialstyrelsen.se/globalassets/sharepoint-dokument/artikelkatalog/oppna-jamforelser/2019-12-6475.pdf
Tabibnia, G. (2020). An affective neuroscience model of boosting resilience in adults. Neuroscience and Biobehavioral Reviews, 115(9), 321–350. https://doi.org/10.1016/j.neubiorev.2020.05.005
Tan, L. B. G. (2015). A critical review of adolescent mindfulness-based programmes. Journal of Child Psychology and Psychiatry, 21(2), 49–55. https://doi.org/10.1177/1359104515577486
Tan, L. B. G., & Martin, G. (2014). Taming the adolescent mind: A randomised controlled trial examining clinical efficacy of an adolescent mindfulness-based group programme. Child and Adolescent Mental Health, 20(1), 49–55. https://doi.org/10.1111/camh.12057
Terjestam, Y., Bengtsson, H., & Jansson, A. (2016). Cultivating awareness at school. Effects on effortful control, peer relations and well-being at school in grades 5, 7, and 8. School Psychology International, 37(5), 456–469. https://doi.org/10.1177/0143034316658321
Tideman, E. (2004). Manual of the Swedish version of the Beck Youth Inventories. The Psychological Corporation.
Ursin, H., & Eriksen, H. R. (2004). The cognitive activation theory of stress. Psychoneuroendocrinology, 29(5), 567–592. https://doi.org/10.1016/S0306-4530(03)00091-X
Ursin, H., & Eriksen, H. R. (2010). Cognitive activation theory of stress (CATS). Neuroscience and Biobehavioral Reviews, 34(6), 877–881. https://doi.org/10.1016/j.neubiorev.2009.03.001
Verweij, H., van Ravesteijn, H., van Hooff, M. L. M., Lagro-Janssen, A. L. M., & Speckens, A. E. M. (2018). Mindfulness-based stress reduction for residents: A randomized controlled trial. Journal of General Internal Medicine, 33(4), 429–436. https://doi.org/10.1007/s11606-017-4249-x
Wagnild, G. (2012). The Resilience Scale. Resilience in children, adolescents, and adults. Springer Publishing Company.
Wagnild, G., & Young, H. M. (1993). Development and psychometric evaluation of the Resilience Scale. Journal of Nursing Measurement, 1(2), 165–178.
WHO. (1992). International Statistical Classification of Diseases and Related Health Problems, 10th Revision (ICD-10). Geneva: WHO.
WHO. (2020). Adolescent mental health. WHO. https://www.who.int/news-room/fact-sheets/detail/adolescent-mental-health
Zoogman, S., Goldberg, S. B., Hoyt, W. T., & Miller, L. (2015). Mindfulness interventions with youth: A meta-analysis. Mindfulness, 6, 290–302. https://doi.org/10.1007/s12671-013-0260-4
Acknowledgements
We thank the West City of Gothenburg for providing assistance with recruitment, data collection, and support with materials and clinic space. Specifically, we thank lic. psychologists Charlotte Ericsson and Hanna Ricksten for helping with booking up study participants for survey, data collection, and data entry. Maria Hägg, the Clinic Manager, had a crucial role in all the necessary steps in providing a participant base for the study and bridging the practicalities between the City of Gothenburg and the study.
Funding
This study was funded by Göteborgs Stad (City Council, West), Sahlgrenska Academy, Kempe-Carlgrenska Foundation, and the Västra Götalandsregionen, West Sweden. The funders had no role in study design, data collection, analysis, interpretation, or preparation of this article.
Author information
Authors and Affiliations
Contributions
KL: contributed to study design, managed the design and preparation of TMR intervention materials, educated and supervised the psychologist who led the TMR intervention. KL and YC: analyzed the data. KL: wrote the first version of the paper. PF, WO, and YC: designed and developed the study, participated in discussions around the study, and contributed the writing of the paper.
Corresponding author
Ethics declarations
Ethics Approval
The ethics application was submitted to the Ethics Review Board in Gothenburg, Sweden in 2015 and granted in January 2016 with file number Dnr_718-15.
Consent to Participate and Publish
The participants and their parents were informed of the purpose of the study, both in conjunction with signing the informed consent forms as well as verbally during the assessment session for the study. All participants and their parents were informed that they would be filling out measures before and after the intervention and additionally at 6 months, 1 year, and 2 years and that they would be offered 3 booster sessions in this period. Informed consent was obtained from all participants and their parents. Data in the study was treated according to GDPR. All participants and their parents gave their consent for their anonymized data to be published in a research article.
Conflict of Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Laundy, K., Friberg, P., Osika, W. et al. Mindfulness-Based Intervention for Children with Mental Health Problems: a 2-Year Follow-up Randomized Controlled Study. Mindfulness 12, 3073–3085 (2021). https://doi.org/10.1007/s12671-021-01771-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12671-021-01771-w