Abstract
Objectives
Attention deficit hyperactivity disorder (ADHD) is associated with increased criticism from others. To date, there is little research considering the consequences of how others respond to people with ADHD. Self-compassion is a positive way of relating to oneself during difficulty. Here, we investigate whether levels of self-compassion differ between people with and without ADHD, and whether perceived criticism mediates any differences in self-compassion between people with and without ADHD.
Methods
A cross-sectional design was used to conduct natural group comparisons. A sample of 1203 adults (46% with a self-reported ADHD diagnosis) recruited via social media, online forums and posters completed online self-report measures of diagnostic status, ADHD traits, self-compassion and perceived criticism. Between-group comparisons of self-compassion and perceived criticism were conducted on participants grouped by diagnosis, then grouped by ADHD trait severity. Perceived criticism was tested as a mediator variable between ADHD diagnosis and self-compassion.
Results
Adults with an ADHD diagnosis showed significantly lower self-compassion and higher perceived criticism than the participants without ADHD. Participants high in ADHD traits but without a diagnosis had significantly similar levels of self-compassion to the diagnosed group. Mediation analysis found that higher perceived criticism partially explained the relationship between ADHD diagnosis and self-compassion, even after accounting for co-occurring mood disorder diagnosis.
Conclusions
Adults with ADHD are less self-compassionate than adults without ADHD. This is partially explained by the higher level of criticism they perceive from others.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
ADHD is a highly prevalent lifelong neurodevelopmental disorder (Polanczyk et al. 2007), which is associated with high levels of criticism, failure, and poor mental health (Kessler et al. 2006). Concurrently, people with ADHD have negative perceptions of themselves (Barber et al. 2005) and low levels of self-compassion (Willoughby and Evans 2019). Self-compassion reflects how people relate to themselves in times of failure or difficulty; either taking a balanced, understanding and non-judgemental stance, or an over identified, non-accepting and judgemental stance towards the self (Neff 2003a). High levels of self-compassion have a positive impact on mental health and well-being (Neff et al. 2007; Raes 2011) and improve resilience in the face of adversity (Neff and McGehee 2010; Wong et al. 2016). In contrast, low self-compassion is associated with higher levels of self-criticism, depression and anxiety and lower levels of well-being (Neff 2003b). Thus, self-compassion is an important trait to explore in populations, such as those with ADHD, who have poor mental health and more frequent negative experiences than typical, which may require higher levels of resilience. Accordingly, interest in self-compassion and ADHD together has started to gain attention—with researchers investigating self-compassion in parents of children with ADHD (Navab et al. 2019), and changes in self-compassion following mindfulness interventions in adults with ADHD (Janssen et al. 2019).
ADHD is recognised, assessed and diagnosed through behavioural differences to typically developing peers (American Psychiatric Association [APA] 2013). These can include behaviours of impulsivity (e.g. interrupting people when talking), inattention (an inability to adequately deploy attention, resulting in either a lack of focus or hyper focus) and/or hyperactivity (e.g. difficulty sitting still for long periods of time). On average, 2.8% of adults across Europe, Asia, the Americas and Middle East (0.6–7.3%) have a diagnosis of ADHD (Fayyad et al. 2017). Nevertheless, symptoms of ADHD are also seen on a continuum within the general population, with some people experiencing little to no symptoms, and others experiencing symptoms to a clinical level without a diagnosis (McLennan 2016). Hence, it is thought that many people who experience ADHD to a clinical level remain undiagnosed, and the prevalence of the disorder is actually much greater than originally suggested (Ginsberg et al. 2014).
Many symptoms of ADHD are typically behaviours that are not desirable in modern societies, and people with ADHD can find it difficult to ‘fit in’. This is exemplified through the reported rejection (Hoza et al. 2005; Lifford et al. 2008), criticism (Psychogiou et al. 2007) and high level of stigma (Law et al. 2007) towards people who display traits of ADHD. In childhood, parents of children with ADHD or ADHD traits may show enhanced hostility and criticism and decreased warmth towards their child compared to parents of typically developing children (Psychogiou et al. 2007). Children with ADHD are also more likely to be bullied and rejected by their peers at school (Hoza et al. 2005). This continues into adulthood, whereby higher levels of hostility and rejection are projected towards people with traits of ADHD compared to the general population (Paulson and Buermeyer 2005). People report that they are less willing to collaborate with, work with, live with, become friends with or get to know individuals with ADHD compared to those with a medical condition (Canu et al. 2008).
It has long been argued that hostility and criticism from others contribute to a person directing negativity towards themselves (e.g. Thompson and Zuroff 1999a, 1999b). It is theorised that people develop interpersonal schemata’s, which are then used to model self-relationships (Baldwin and Dandeneau 2005); thus, if a person is treated negatively and highly criticised, that person may then come to adopt this interpersonal style towards the self. This is evident from the work of Brewin et al. (1996), who found that self-criticism in women was predicted through levels of perceived criticism from their mothers. Furthermore, an interpretive phenomenological analysis on barriers to self-compassion found that a hypercritical home environment led to participants marginalising the compassion they showed towards themselves (Bayir and Lomas 2016). Similarly, there is empirical evidence that children and young adults who report higher levels of criticism and less support from parents show significantly less compassion towards themselves than those who report their parents as warm and supportive (Neff and McGehee 2010). In contrast, Irons et al. (2006) demonstrated that the ability to reassure the self is mediated through memories of parental warmth. Consequently, interactions with others are important to provide a positive model on how to relate towards the self, and subsequently for the development of self-compassion in times of failure or setbacks (Baldwin and Dandeneau 2005; Shaver et al. 2016).
Self-compassion is a positive way to relate to the self, which adds resilience against failure and criticism from others (Neff et al. 2005; Vigna et al. 2018), and protects against negative self-evaluations (Neff and McGehee 2010). Neff’s (2003a, 2003b) model of self-compassion is composed of three interrelated components: (a) self-kindness versus self-judgement—the tendency to be understanding and warm towards the self rather than take a judgemental and hostile attitude towards one’s difficult experience; (b) common humanity versus isolation—the recognition that failure and suffering are all part of the human experience, and not something unique to the individual; (c) mindfulness versus over-identification—the ability to have an awareness of the experience as is, without over identifying and applying it globally. In short, self-compassionate people recognise that all people have negative experiences, fail and make mistakes and are able to acknowledge these experiences and approach them with acceptance and kindness, without becoming over-identified with their negative feelings.
Research has shown that people with ADHD tend to be less compassionate and more negative towards themselves. For example, Brod et al. (2012) reported that many of the 108 people they interviewed across seven different countries viewed themselves as ‘not normal’ or ‘wrong’. More recently, a study investigating the language used on social media found that people with ADHD commonly spoke around themes of self-criticism and failure (Guntuku et al. 2019). In addition, undergraduate students with ADHD and learning difficulties (LD) were found to have low levels of compassion towards themselves (Willoughby and Evans 2019). Willoughby and Evans also compared their ADHD/LD sample with samples from other studies, which further demonstrated that the levels of self-compassion in students with ADHD/LD were lower compared to other undergraduate students.
Based on the above research, we propose that the negativity people with ADHD experience from others across their lifetimes is likely to result in them responding towards themselves with negativity. In particular, due to the high degree of emotional suffering and challenges that people with ADHD experience academically and personally (Kessler et al. 2006), we theorise that people with ADHD may relate towards themselves more negatively during times of suffering. As such, this study aimed to expand on Willoughby and Evans (2019) study by directly comparing levels of self-compassion between people with and without a self-reported ADHD diagnosis from the general population and by investigating whether criticism explains any differences in self-compassion between those with and without ADHD. It was hypothesised that adults with a self-reported ADHD diagnosis would have significantly lower levels of self-compassion compared to adults without an ADHD diagnosis and that they would perceive higher levels of criticism compared to participants without ADHD. It was further predicted that the level of perceived criticism would mediate the relationship between a self-reported ADHD diagnosis and levels of self-compassion. The analysis for this study was pre-registered as an additional exploratory analysis of a wider study; thus, the hypotheses were not pre-registered. Nonetheless, the predictions made are in line with the overall hypotheses of the wider study, and with relevant theory.
Method
Participants
Participants with and without a diagnosis of ADHD were recruited to take part in the study between January and March 2019. The study was advertised on social media sites, online forums and posters displayed in shops, university disability services and at ADHD support group venues across the UK. To be included in the study, participants were required to be over the age 18, have English as a language and to complete all questions regarding ADHD diagnosis, self-compassion, ADHD traits and perceived criticism. All participants were invited to enter into a prize draw to win one of two £25 vouchers after completion of the questionnaires.
Of the 1909 participants who followed the link to take part in the study, 1203 participants were included in analysis. A detailed description of participant inclusion/exclusion is presented in Fig. 1. Nearly half of the total sample (45.55%) self-reported having a clinical diagnosis of ADHD. Participants without a diagnosis were aged between 18 and 82 years (M = 33.74, SD = 11.15). This was statistically similar (t (1126.9) = 0.41, p = 0.68) to the participants with a self-reported ADHD diagnosis, whose ages ranged between 18 and 67 years (M = 33.48, SD = 10.49). The average age of receiving a diagnosis was 27.84 years (SD = 12.66) and the length of time since diagnosis varied between 0 and 45 years (M = 5.53, SD = 7.50), but the majority of participants reported that they had only recently received their diagnosis. Table 1 presents the full demographic information of the final analytical sample.
Procedure
Participants completed a series of questionnaires online, hosted on the survey website Qualtrics (https://www.qualtrics.com). Firstly, participants completed demographic questions and questions regarding diagnosis of ADHD and co-occurring mental health conditions. This was followed by measures of ADHD traits and self-compassion. Additional questionnaires measuring well-being, stress, depression and anxiety were completed by participants as part of a wider study but not included in the analysis reported here. Measures of depression and anxiety were always presented last to prevent negative priming, whilst stress and well-being were presented in a random order in the central section of the study along with measures of perceived criticism and an attention check question.
Measures
ADHD Diagnosis
A yes/no style answer was used to assess if participants had a clinical diagnosis of ADHD. Additional questions asked for the age participants were diagnosed, if they had ever taken medication or engaged in psychological interventions to manage their symptoms and what medication and/or interventions had been used to manage their disorder. These were used to provide added confidence in the legitimacy of participants answers. If the age of diagnosis provided was inconsistent with the participant’s country of residence diagnostic guidelines (i.e. > 4 years, USA; > 6 years, UK) AND no legitimate medication or psychological interventions were reported, the self-report was considered unreliable and therefore excluded from further analysis. In addition, participants that reported an ADHD diagnosis but did not score above the clinical ‘cut off’ in the ADHD measurement scale were also excluded from analysis.
ADHD Traits
The Adult ADHD Self-Report Scale (ASRS; Kessler et al. 2005) is a measure created in association with the World Health Organisation (WHO). It includes six items questioning the frequency of ADHD symptoms ranging from 0 (never) to 4 (very often) in accordance with DSM-IV clinical criteria (APA 2013). It is recommended that individuals who report “sometimes”, “often” or “very often” to the first three questions on the ASRS, or “often”/“very often” to the final three questions more than 4 times in the questionnaire, have symptoms highly consistent with ADHD, which provides a categorical classification of ADHD. A total score is obtained by summing the scores, whereby a higher score indicates a greater affiliation with ADHD. The scale has been reported as having moderate sensitivity of 68.7% and high specificity of 99.5% (Kessler et al. 2005). It also has high internal consistency (Cochrane α = .84 ; Adler et al. 2006) and test-retest reliability (r = .86; Matza et al. 2011). In this study, reliability was also good, with a Cronbach α and McDonald’s ω of .85.
Self-compassion
The Self-Compassion Scale (SCS; Neff 2003b) is a 26 item self-report questionnaire that assesses the main components of self-compassion (self-kindness vs self-judgement, common humanity vs. isolation and mindfulness vs. over-identification) using both positively and negatively worded items. Items ask respondents to indicate how often they respond towards themselves for each of the positive and negative dimensions of self-compassion on a 6-point Likert scale (almost never-to-almost always). Global self-compassion scores are attained by reverse coding the negative items, and then averaging across the mean scores of each facet. The scale has been found to have good levels of internal consistency when using a 5-point Likert scale (α = .92; Mantelou and Karakasidou 2017; Neff 2003b), and good test-retest reliability (α = .93; Neff 2003b; Neff et al. 2005; Neff and Pommier 2013). In this study, the measure was also highly reliable (α = .94 and ω = .74).
Perceived Criticism
An adapted version of the Perceived Criticism Scale (Hooley and Teasdale 1989) was used. A single question: “How critical do you think people in your nearest environment—such as family, friends…—are of you?” was rated on a scale between 0 (not at all critical) and 10 (very critical). The adapted question accounts for criticism from multiple others, whereas the original accounts for criticism from one single relative. The adapted measure has also been used by Baeken et al. (2018). The perceived criticism scale has good criterion validity, as the responses are strongly associated with measures of expressed emotion (r = .51) and the item also has good test-retest reliability (r = .75; Hooley and Parker 2006).
Attention Check
An attention check question was included to reduce biases from primacy effects: “People vary in the amount they pay attention to these kinds of surveys. Some take them seriously and read each question, whereas others go very quickly, and barely read the questions at all. If you have read this question carefully, please write the word yes in the blank box below labelled “other”. There is no need for you to respond to the scale below.”
This was followed by a 7-point Likert scale (strongly disagree–strongly agree), and an empty text box labelled ‘Other’. If participants did not respond in the text box or did not put ‘yes’ in the text box, they were considered as failing the attention check and were excluded from data analysis.
Data Analyses
The analysis reported here is part of a wider study that was pre-registered on the Open Science Framework (https://osf.io/uwekq). Additional analyses that provide an important additional insight into the findings have also been conducted that were not originally included on the pre-registration form.
The data was coded, cleaned and analysed using Excel and ‘R’ (Development Core Team 2013). Data was rounded to two decimal places, and confidence intervals are to 95%. To investigate between group differences in self-compassion, independent t tests were used, whilst Mann-Whitney U tests were used to investigate group differences in perceived criticism due to the ordinal nature of the data. Mediation modelling was conducted using ‘Lavaan’ (Rosseell 2012). ADHD diagnosis was entered as the independent variable, the mediator was perceived criticism dummy coded (0 = ratings < 5, 1 = ratings > 5), and self-compassion was entered as the dependent variable. This was also conducted controlling for self-reported mood diagnosis.
Unexpectedly, 52.06% of the participants without a diagnosis of ADHD scored above the cut off on the ASRS (Table 2). Thus, we ran additional analyses investigating whether self-compassion differs between people with similar levels of ADHD traits who either have or do not have a diagnosis of ADHD. For this, participants were assigned to groups depending on whether participants had a self-reported ADHD diagnosis (ADHD), high ASRS scores but no self-reported diagnosis (ADHD traits+) or low ASRS scores and no self-reported diagnosis (ADHD traits−). Secondly, a large proportion of the ADHD sample self-reported that they also had a clinical mood disorder. Further statistical exploration was conducted to ascertain that differences in self-compassion were a consequence of the ADHD diagnosis, and not the self-reported mood diagnosis. For this analysis, the sample was subdivided into (a) participants with self-reported ADHD but not a self-reported mood disorder (ADHD+MD−), (b) participants who self-reported both ADHD and a mood disorder (ADHD+MD+), (c) participants with a self-reported mood disorder but not self-reported ADHD (ADHD-MD+) and finally participants who reported neither a mood disorder or ADHD diagnosis (ADHD−MD−). Exploratory analysis used one-way ANOVAs to investigate differences in self-compassion and a Kruskal-Wallis rank test to assess differences in perceived criticism. A binary logistic regression was also conducted as an exploratory analysis to evaluate the probability that participants had high ADHD traits (with or without a diagnosis) based on levels of self-compassion, and perceived criticism, controlling for co-occurring self-reported mood disorder.
Assumptions of normality were assessed using density plot histograms and QQ-plots, and homogeneity of variance was checked using Levene’s test. Data points were considered as outliers if they were 1.5 times greater than the interquartile range (IQR). It was specified during pre-registration that outliers would only be excluded from analysis if (a) there are no changes in the model relationship or results but did impact the assumptions; (b) there are no changes in assumptions, but the model relationship change.
Results
Assumption Checks
Assumptions of normality and equal variances were met. No outliers were detected for perceived criticism. Ten data points were identified as outliers in the self-compassion measure, but the outliers did not significantly change the model relationships nor the assumptions to a significant level, and therefore were not removed from the data for analysis.
ADHD Diagnosis and Self-Compassion
Participants with self-reported ADHD had a significantly lower mean self-compassion score (M = 2.57, SD = .76) compared to the no ADHD group (M = 2.94, SD = .81), t(1201) = 7.57, p < .001, d = .44, CI [.32, .56]. As can be seen in Table 3, participants in the ADHD group scored lower on questions regarding self-kindness, mindfulness and common humanity, with a low-to-medium sized effect, and scored much higher on the questions regarding self-judgement, over-identification and isolation with a larger sized effect.
Significant differences in self-compassion were also observed between ADHD/Mood disorder groups (F (3, 1141) = 59.6, p < .001, η2 = .14, CI[.10, .17]). Tukey HSD post hoc analysis revealed that self-compassion scores in the ADHD+MD+ group were significantly lower than the ADHD+MD− group (diff = − .39, p < .001, CI [− .58, − .21). However, both ADHD+ MD− participants (diff = 0.36, p < .001, CI [− .53, .19]) and ADHD+ MD+ (diff = 0.39, p < .001, CI [− .57, − .21]) had significantly lower self-compassion than participants with neither diagnosis. Finally, self-compassion was significantly lower in the ADHD-MD+ group compared to the ADHD+ MD− (diff = − 0.27, p < .01, CI [− .48, − .07]) and ADHD-MD− groups (diff = − 0.64, p < .001, CI [− .82, − .46). Levels of self-compassion did not differ between ADHD-MD+ and ADHD+MD+ groups (diff = 0.11, p = .40, CI [− 08, .31]). Fig .2 demonstrates these relationships visually and reports the mean scores and standard deviations for each group.
A violin plot demonstrating the variance, mean, and 95% confidence intervals for self-compassion scores across ADHD/mood groupings. Note: The mean and standard deviation are reported for each group. Error bars represent the 95% confidence intervals, and the dot represents the group mean. Groups are divided based on participants self-reported ADHD diagnosis and/or self-reported diagnosis of a mood disorder. ADHD-MD−: participants reported no ADHD or mood disorder. ADHD+MD−: participants reported having a diagnosis of ADHD but no mood disorder. ADHD+MD+: participants reported both ADHD and a mood disorder. ADHD-MD+: participants reported a diagnosed mood disorder but no ADHD diagnosis
A one-way ANOVA revealed a significant effect of group, signifying differences in self-compassion scores between participants with a self-reported ADHD diagnosis, ADHD traits+ and ADHD traits−, even when controlling for self-reported mood disorders (F(2, 1200) = 127.6, p < .000, η2 = .17, CI [.13, .21]). The mood disorder had a significant, but smaller effect on self-compassion (F(1, 1200) = 85.86, p < .000, η2 = .06, CI [.03, .08]). Tukey HSD revealed that the ADHD trait− (M = 3.36, SD = .76) group had significantly higher levels of self-compassion than both the ADHD group (M = 2.57, SD = .76; diff = .79, CI [.66, .92]) and the ADHD traits+ group (M = 2.55, SD = .55; diff = .81, CI [.66, .95]). However, self-compassion levels did not differ significantly between the ADHD traits+ and ADHD group; self-compassion scores differed by only − .02 (CI [− .14, .11], p = .95).
ADHD Diagnosis and Perceived Criticism
On average, participants perceived significantly higher levels of criticism from others if they had a self-reported ADHD diagnosis (M = 6.00, SD = 2.33) compared to participants who did not report an ADHD diagnosis (M = 5.23, SD = 2.53; W = 148,230, p < .001).
Perceived criticism also differed significantly between ADHD+ (M = 6.00, SD = 2.33), ADHD traits+ (M = 5.83, SD = 2.48) and ADHD traits− groups (M = 4.58, SD = 2.42; X2(2) = 69.21, p < .000). Wilcoxon rank sum test demonstrated that the ADHD traits− group had significantly lower ratings of perceived criticism compared to both ADHD traits+ (W = 38,304, p < .000) and ADHD groups (W = 57,327, p < .000). The ADHD and ADHD traits+ groups did not differ in perceived criticism (W = 97,058, p = .41).
Self-compassion and Perceived Criticism as Predictors of ADHD
A binary logistic regression was used to predict the probability that participants had high ADHD traits based on levels of self-compassion and perceived criticism whilst controlling for co-occurring self-reported mood disorders. The full model was statistically significant (χ2 (3) = 239.75, p < .001) and correctly classified 78% of participants. For self-compassion, the odds ratio of .37 [.31, .45] revealed that for every 1-unit increase in self-compassion, the odds of being in the group with high ADHD traits was lowered by 63% when perceived criticism and mood disorders were held constant. For perceived criticism, the odds ratio of 1.87 [1.39, 2.53] suggests that if participants reported high levels of perceived criticism, the odds of having high ADHD traits increased by 87%.
Perceived Criticism as a Mediator Between ADHD Diagnosis and Self-compassion
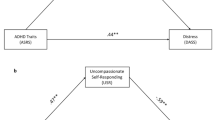
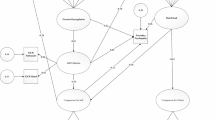
The mediation analysis revealed a significant partial indirect effect of perceived criticism on self-compassion through differences in diagnosis group, indirect(a*b) = − .06, CI [− .09, − .03], p < .000. Perceived criticism accounted for approximately 2.2% of the total effect PM = − .37, CI [− .46, − .27], p < .000. However, ADHD diagnosis was still directly associated with lower levels of self-compassion to a significant degree (Fig. 3a). Thus, having a diagnosis of ADHD was associated with high levels of perceived criticism, which was associated with lower levels of self-compassion. This in turn partially explained the negative association between having an ADHD diagnosis and levels of self-compassion.
The mediating effects of perceived criticism between ADHD and self-compassion both independent of co-occurring mood disorder, and when co-occurring mood disorders are controlled for. Note a the relationships between ADHD, perceived criticism and self-compassion when not controlling for co-occurring mood diagnosis; b the relationships between ADHD, perceived criticism and self-compassion when controlling for co-occurring mood diagnosis. *p < .000
Similar results were found when controlling for co-occurring mood disorders. A significant partial indirect effect of perceived criticism was still observed, indirect(a*b) = − .04, CI [− .07, − .19], p < .000. Perceived criticism accounted for approximately 3.7% of the total effect (PM = − .25, CI [− .34, − .16], p < .000), but ADHD was still directly associated with self-compassion to a significant degree (see Fig. 3b).
Discussion
This study aimed to examine group differences in self-compassion and perceived criticism between adults with and without ADHD and to investigate the potential mediating effect that perceived criticism may have on the relationship between ADHD and self-compassion. Additional analysis explored the potential confounding effect of having a mood disorder, and whether self-compassion differed between participants with a diagnosis of ADHD and participants with high and low traits of ADHD. Due to the externalised nature of many ADHD behaviours, the presence of the symptoms is not only experienced by the person internally but also accompanied by the reactions and feedback of others. This study exemplifies the necessity to consider social-emotional factors in ADHD and to think about how these factors may influence how people with ADHD subsequently treat themselves.
In accordance with the first hypothesis, we found that adults with an ADHD diagnosis were less self-compassionate than those without ADHD. This extends the findings that Willoughby and Evans (2019) obtained with a mixed ADHD/LD sample of undergraduate students, by demonstrating that self-compassion is significantly lower in adults with ADHD from a variety of backgrounds and ages. We also demonstrated that lower levels of self-compassion are not isolated to people with an ADHD diagnosis but extend to those with high traits of ADHD, which suggests that self-compassion is a correlate of ADHD symptoms, not of the diagnosis. What is more, we found that the odds of having high ADHD traits (with or without a diagnosis) decreased by 63% for each 1-unit of increase in self-compassion. This strengthens the argument that people with high traits of ADHD are significantly less self-compassionate, irrespective of whether they have a diagnosis of the disorder or not.
We also identified differences in the individual facets of self-compassion, providing a deeper insight into what specific attributes contribute to low self-compassion in people with ADHD. Similar to Willoughby and Evans (2019), self-kindness had the lowest average score of the positive components of self-compassion, followed by common humanity, whilst mindfulness scores were moderate. Over-identification had the highest average score of the negative components of self-compassion followed by isolation, and then self-judgement. Between-group comparisons revealed that although there were significant differences in levels of self-kindness and mindfulness, the largest differences were found for isolation, over-identification, self-judgement, and common humanity.
High scores on isolation and low scores on common humanity indicate that people with ADHD feel more withdrawn from humanity compared to people without ADHD. During difficult times people with ADHD may be less likely to believe that their inadequacies and suffering is part of being human and subsequently shared by others. Instead, they may be more likely to feel alone in their negative experiences—believing that other people have happier, easier lives. This is consistent with qualitative studies that have previously reported that people with ADHD feel different from others in a negative way (Brod et al. 2012; Kendall et al. 2003). Taken together, this evidence suggests that people with ADHD are aware of how their behaviour differs from others, and that this extends to how they relate towards the self by showing themselves less compassion during difficult times.
The high scores in over-identification and self-judgement found in the current study highlight that people with ADHD are more negative towards themselves. This suggests a greater likelihood to be consumed by, and fixate on, negative thoughts, emotions and experiences and to be less tolerant and more judgemental towards their own flaws and failures. This may be a consequence of the higher frequency at which people with ADHD typically experience difficulties or failures in day to day life (Kessler et al. 2006), and the increased criticism that people with ADHD tend to experience ( Brooks 2002; Psychogiou et al. 2007).
In accordance with our hypotheses, people with ADHD reported that they observed high levels of criticism from others, which was significantly higher than the level of criticism that people without ADHD perceived from others. Exploratory results strengthened this finding further, by finding that the odds of having high ADHD traits (with or without a diagnosis) increased by 87% if participants reported high levels of perceived criticism compared to low levels of criticism. These findings are consistent with qualitative research and anecdotal accounts of the experiences of criticism in adults and children with ADHD (Brooks 2002; Singh et al. 2010). It also extends on existing quantitative research that used vignettes and expressed emotion to capture criticism from others (Musser et al. 2016; Psychogiou et al. 2007), by demonstrating that people with ADHD also perceive the criticism from others. Consequently, the current findings provide further evidence, from the perspective of those with ADHD, that people with ADHD have more experiences of criticism.
Importantly, we found that the high levels of criticism perceived by people with ADHD contributed to lower self-compassion, even when concurrent self-reported mood disorders were taken into account. The results of the mediation analysis provide support for the proposition that the way others treat people with ADHD, influences how people with ADHD treat themselves. Interactions with others are important for the development of coping strategies in times of failure or setbacks, providing memories of others being helpful, warm and soothing to use as a model of appropriate behaviours towards ourselves (Baldwin and Dandeneau 2005; Shaver et al. 2016). Individuals with ADHD are more prone to making mistakes, such as being late, forgetful or clumsy and are typically more emotionally reactive to situations (Asherson et al. 2018). If caregivers or peers frequently react to these mistakes and emotional reactions with judgement, criticism and hostility rather than understanding and acceptance, then people with ADHD may be more likely to relate towards themselves in the same way when they make mistakes or are emotional.
Criticism from others may also influence levels of self-compassion in people with ADHD by contributing a fear of compassion. Although traditionally discussed under Paul Gilberts conceptualisation of self-compassion, which views self-compassion as part of the broader concept of compassion (Gilbert 2014), there is evidence that fear of compassion acts as an inhibitor that prevents people engaging in compassionate behaviours towards the self and others (Naismith et al. 2019). Fears of compassion have been argued to manifest from developing an insecure relationship with caregivers following the lack of supportive and affectionate parental behaviours and/or from classical conditioning of negative outcomes to positive emotions (Gilbert 2014). Individuals consequently perceive kindness and compassion from others or the self as a potential threat that prevents people from engaging in self-compassion (Naismith et al. 2019). This offers a further potential explanation for the reduced self-compassion in people with ADHD, as experiences of hostility towards symptoms of ADHD, such as being loud, excitable or emotionally reactive, may subsequently be associated with caregivers, which in turn may result in care being associated with punishment and subsequently lead to fear of care or compassion (Kirby 2020).
Alternatively, people with ADHD may internalise the criticism that they receive, making them more self-critical. Self-judgement has been suggested as representative of self-criticism (Rose and Rimes 2018), and our findings suggest that people with ADHD were significantly more self-judgemental. In research investigating perfectionism, perceived criticism has been associated with higher self-criticism in undergraduate students, indicating that perceived criticism may have a direct relationship with self-criticism (Dunkley et al. 2003). Research has demonstrated that people with ADHD perceive their ADHD symptoms as part of them and their personality (Kendall et al. 2003). Thus, receiving negativity towards failure, or rejection as a consequence of these ADHD behaviours, may condition people to view themselves as ‘bad’ (Kendall et al. 2003). A negative internalised view of the self may then act as a barrier towards being self-compassionate, as people have reported that feelings of inadequacy inhibit them from being compassionate towards themselves (Bayir and Lomas 2016). Moreover, it is more comfortable and less threatening to see the self in the same way as others, so people with ADHD may also react to themselves in the same way that others react towards them in order to prevent rejection from others (Powers and Zuroff 1988). Nevertheless, self-judgement is not a direct measure of self-criticism, and so, these suggestions are speculative and require further investigation.
Additionally, the results of the mediation analysis may also be an indicator that people with ADHD may benefit from developing greater resilience to the high levels of criticism they receive. Self-compassion has been found to serve as a coping strategy in the face of rejection, providing enhanced resilience to criticism and rejection from others (Neff et al. 2005; Neff and McGehee 2010; Vigna et al. 2018; Wong et al. 2016). Consequently, as people with ADHD experience more hardship and criticism than the average person (Kessler et al. 2006; Paulson and Buermeyer 2005), they may profit more than those without ADHD from developing higher levels of self-compassion to cope with these challenges.
Finally, this study highlighted relationships between ADHD, mood disorders and self-compassion. Individuals with ADHD, either with or without a co-occurring mood disorder, were less self-compassionate than participants that reported having neither ADHD nor a mood disorder. This suggests that having an ADHD diagnosis is specifically associated with lower self-compassion independent of co-occurring mood disorders. Nevertheless, the results also determined that adults with diagnosed or undiagnosed ADHD and a co-occurring mood disorder, were the most likely to have low self-compassion, suggesting that co-occurring mood disorders has an additive effect on ADHD, leading to even lower levels of self-compassion. However, it is unclear whether self-compassion levels may predict the presence of mood disorders, or if the mood disorder results in lower self-compassion. In previous research, self-compassion has been shown to be negatively associated with low mood (MacBeth and Gumley 2012) and fears of compassion have been demonstrated to be significantly associated with increased depression, anxiety and stress (Kirby et al. 2019). In accordance with this research, it could be posited that low self-compassion contributes towards the symptoms of the mood disorders; however, further research is necessary to determine the direction of these relationships.
Limitations and Future Research
The three main limitations of this study are the cross-sectional nature of the design, which prevents any causal conclusions being made, the use of self-report measures, and the use of a 6-point rather than 5-point scale in the SCS. Although efforts were made to assess the reliability of self-reported diagnosis, we cannot be certain of the truthfulness of participant’s reports. Moreover, as multiple constructs were measured using self-report questionnaires, the study may be open to common method bias. Providing responses to multiple constructs in the same survey may lead to spurious correlations between items that are independent from ‘true’ effects due to similarity in response style, social desirability and priming effects (Podsakoff et al. 2003). Although the addition of the sixth point increased the variance in the SCS and it has been debated that six points has better discrimination and reliability than five point scales (Chomeya 2010), we cannot compare the self-compassion values across studies to ascertain whether this population group have lower levels of self-compassion to other minority groups researched.
A strength of this study is the large sample size, which allowed us to conduct additional exploratory analysis to expand our understanding and interpretation of the results. A small proportion of participants were recruited via posters distributed in public spaces and university student disability meeting rooms across the UK; however, the majority of the participants were recruited online via multiple different social media platforms and online forums. The audience for these online support forums will likely attract people with a diagnosis, people awaiting a diagnosis, or people who have self-diagnosed. This resulted in a sample with an over-representative number of participants without a diagnosis, but with higher traits of ADHD than is usually reported in the general population (Lundin et al. 2019) which allowed us to account for people with a diagnosis, people with symptoms but without a diagnosis and people with low levels of symptoms in the analyses. This enables us to generalise our findings to both people with a diagnosis, and people with traits of ADHD. In addition, the large sample size allowed us to take into consideration the high proportion of participants in the ADHD diagnostic group who also had a mood disorder diagnosis, which added novel and important findings but also highlighted areas for future research.
Overall, the study supports and extends upon previous research into self-compassion and ADHD. It highlights the potential importance of including people with traits of ADHD in future research investigating self-compassion in ADHD and has demonstrated that co-occurring mood disorders have an independent relationship with levels of self-compassion in ADHD. The study underscores the need to understand whether self-compassion is predictive of mood in people with ADHD or vice versa, whether criticism from others impacts levels of self-criticism in people with ADHD and whether levels of self-compassion provide protection and resilience against criticism and the frequent challenges that people with ADHD endure. This research would be well-placed to understand the potential utility of self-compassion in an ADHD population.
References
Adler, L. A., Spencer, T., Faraone, S. V., Kessler, R. C., Howes, M. J., Biederman, J., & Secnik, K. (2006). Validity of pilot adult ADHD self-report scale (ASRS) to rate adult ADHD symptoms. Annals of Clinical Psychiatry, 18(3), 145–148. https://doi.org/10.1080/10401230600801077.
American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (DSM-5®). American Psychiatric Publishing.
Asherson, P., Ramos-Quiroga, J. A., & Young, S. (2018). Adult ADHD clinical presentation and assessment. In Banaschewski, T., Coghill, D., & Zuddas, A. (Ed.), Oxford textbook of Attention Deficit Hyperactivity Disorder (pp. 179–189). Oxford University Press.
Baeken, C., Dedoncker, J., Remue, J., Wu, G.-R., Vanderhasselt, M., De Witte, S., Poppa, T., Hooley, J., & De Raedt, R. (2018). One MRI-compatible tDCS session attenuates ventromedial cortical perfusion when exposed to verbal criticism: the role of perceived criticism. Human Brain Mapping, 39(11), 4462–4470. https://doi.org/10.1002/hbm.24285.
Baldwin, M. W., & Dandeneau, S. (2005). Understanding and modifying the relational schemas underlying insecurity. In Baldwin, M. W. (Ed.), Interpersonal cognition (pp. 33–61). Guilford Press.
Barber, S., Grubbs, L., & Cottrell, B. (2005). Self-perception in children with attention deficit/hyperactivity disorder. Journal of Pediatric Nursing, 20(4), 235–245. https://doi.org/10.1016/j.pedn.2005.02.012.
Bayir, A., & Lomas, T. (2016). Difficulties generating self-compassion: an interpretative phenomenological analysis. The Journal of Happiness & Well-Being, 4(1), 15–33.
Brewin, C. R., Andrews, B., & Furnham, A. (1996). Self-critical attitudes and parental criticism in young women. British Journal of Medical Psychology, 69(1), 69–78. https://doi.org/10.1111/j.2044-8341.1996.tb01851.x.
Brod, M., Pohlman, B., Lasser, R., & Hodgkins, P. (2012). Comparison of the burden of illness for adults with ADHD across seven countries: a qualitative study. Health and Quality of Life Outcomes, 10(1), 47. https://doi.org/10.1186/1477-7525-10-47.
Brooks, R. (2002). Changing the mindset of adults with ADHD: strategies for fostering hope, optimism, and resilience. In Goldstein, S. & Teeter Ellison, A. (Eds.), Clinicians guide to adult ADHD: Assessment and intervention (pp. 127–146). Academic Press. https://doi.org/10.1016/B978-012287049-1/50009-8.
Canu, W. H., Newman, M. L., Morrow, T. L., & Pope, D. L. W. (2008). Social appraisal of adult ADHD: stigma and influences of the beholder’s big five personality traits. Journal of Attention Disorders, 11(6), 700–710. https://doi.org/10.1177/1087054707305090.
Chomeya, R. (2010). Quality of psychology test between Likert scale 5 and 6 points. Journal of Social Sciences, 6(3), 399–403.
Dunkley, D. M., Zuroff, D. C., & Blankstein, K. R. (2003). Self-critical perfectionism and daily affect: dispositional and situational influences on stress and coping. Journal of Personality and Social Psychology, 84(1), 234–252.
Fayyad, J., Sampson, N. A., Hwang, I., Adamowski, T., Aguilar-Gaxiola, S., Al-Hamzawi, A., Andrade, L. H. S. G., Borges, G., de Girolamo, G., Florescu, S., Gureje, O., Haro, J. M., Hu, C., Karam, E. G., Lee, S., Navarro-Mateu, F., O’Neill, S., Pennell, B. E., Piazza, M., … Wojtyniak, B. (2017). The descriptive epidemiology of DSM-IV adult ADHD in the World Health Organization World Mental Health Surveys. Attention Deficit and Hyperactivity Disorders, 9(1), 47–65. https://doi.org/10.1007/s12402-016-0208-3.
Gilbert, P. (2014). The origins and nature of compassion focused therapy. British Journal of Clinical Psychology, 53(1), 6–41. https://doi.org/10.1111/bjc.12043.
Ginsberg, Y., Quintero, J., Anand, E., Casillas, M., & Upadhyaya, H. P. (2014). Underdiagnosis of attention-deficit/hyperactivity disorder in adult patients: a review of the literature. Primary Care Companion for CNS Disorders, 16(3), PCC.13r01600. https://doi.org/10.4088/PCC.13r01600.
Guntuku, S. C., Ramsay, J. R., Merchant, R. M., & Ungar, L. H. (2019). Language of ADHD in adults on social media. Journal of Attention Disorders, 23(12), 1475–1485. https://doi.org/10.1177/1087054717738083.
Hooley, J. M., & Parker, H. A. (2006). Measuring expressed emotion: an evaluation of the shortcuts. Journal of Family Psychology, 20(3), 386–396. https://doi.org/10.1037/0893-3200.20.3.386.
Hooley, J. M., & Teasdale, J. D. (1989). Predictors of relapse in unipolar depressives: expressed emotion, marital distress, and perceived criticism. Journal of Abnormal Psychology, 98(3), 229–235.
Hoza, B., Mrug, S., Gerdes, A. C., Hinshaw, S. P., Bukowski, W. M., Gold, J. A., Kraemer, H. C., Pelham, W. E., Wigal, T., & Arnold, L. E. (2005). What aspects of peer relationships are impaired in children with attention-deficit/hyperactivity disorder? Journal of Consulting and Clinical Psychology, 73(3), 411–423. https://doi.org/10.1037/0022-006X.73.3.411.
Irons, C., Gilbert, P., Baldwin, M. W., Baccus, J. R., & Palmer, M. (2006). Parental recall, attachment relating and self-attacking/self-reassurance: their relationship with depression. British Journal of Clinical Psychology, 45(3), 297–308. https://doi.org/10.1348/014466505X68230.
Janssen, L., Kan, C. C., Carpentier, P. J., Sizoo, B., Hepark, S., Schellekens, M. P. J., Donders, A. R. T., Buitelaar, J. K., & Speckens, A. E. M. (2019). Mindfulness-based cognitive therapy v. treatment as usual in adults with ADHD: a multicentre, single-blind, randomised controlled trial. Psychological Medicine, 49(01), 55–65. https://doi.org/10.1017/S0033291718000429.
Kendall, J. R. N., Hatton, D. R. N., Beckett, A. R. N., & Leo, M. M. S. (2003). Children’s accounts of attention-deficit/hyperactivity disorder. Advances in Nursing Science Childhood Health and Illness, 26(2), 114–130.
Kessler, R. C., Adler, L., Ames, M., Demler, O., Faraone, S., Hiripi, E., Howes, M. J., Jin, R., Secnik, K., Spencer, T., Ustun, T. B., & Walters, E. E. (2005). The World Health Organization adult ADHD self-report scale (ASRS): a short screening scale for use in the general population. Psychological Medicine, 35(2), 245–256. https://doi.org/10.1017/S0033291704002892.
Kessler, R. C., Adler, L., Barkley, R., Biederman, J., Conners, C. K., Demler, O., Faraone, S. V., Greenhill, L. L., Howes, M. J., Secnik, K., Spencer, T., Ustun, T. B., Walters, E. E., & Zaslavsky, A. M. (2006). The prevalence and correlates of adult ADHD in the United States: results from the National Comorbidity Survey Replication. The American Journal of Psychiatry, 163(4), 716–723. https://doi.org/10.1176/appi.ajp.163.4.716.
Kirby, J. N. (2020). Nurturing family environments for children: compassion-focused parenting as a form of parenting intervention. Education in Science, 10(1), 3. https://doi.org/10.3390/educsci10010003.
Kirby, J. N., Day, J., & Sagar, V. (2019). The ‘flow’ of compassion: a meta-analysis of the fears of compassion scales and psychological functioning. Clinical Psychology Review, 70, 26–39. https://doi.org/10.1016/j.cpr.2019.03.001.
Law, G. U., Sinclair, S., & Fraser, N. (2007). Children’s attitudes and behavioural intentions towards a peer with symptoms of ADHD: Does the addition of a diagnostic label make a difference? Journal of Child Health Care, 11(2), 98–111. https://doi.org/10.1177/1367493507076061.
Lifford, K. J., Harold, G. T., & Thapar, A. (2008). Parent-child relationships and ADHD symptoms: a longitudinal analysis. Journal of Abnormal Child Psychology, 36(2), 285–296. https://doi.org/10.1007/s10802-007-9177-5.
Lundin, A., Kosidou, K., & Dalman, C. (2019). Testing the discriminant and convergent validity of the World Health Organization six-item adult ADHD self-report scale screener using the Stockholm Public Health cohort. Journal of Attention Disorders, 23(10), 1170–1177 1087054717735381.
MacBeth, A., & Gumley, A. (2012). Exploring compassion: a meta-analysis of the association between self-compassion and psychopathology. Clinical Psychology Review, 32(6), 545–552. https://doi.org/10.1016/j.cpr.2012.06.003.
Mantelou, A., & Karakasidou, E. (2017). The effectiveness of a brief self-compassion intervention program on self-compassion, positive and negative affect and life satisfaction. Psychology, 08(04), 590–610. https://doi.org/10.4236/psych.2017.84038.
Matza, L. S., Van Brunt, D. L., Cates, C., & Murray, L. T. (2011). Test-retest reliability of two patient-report measures for use in adults with ADHD. Journal of Attention Disorders, 15(7), 557–563. https://doi.org/10.1177/1087054710372488.
McLennan, J. D. (2016). Understanding attention deficit hyperactivity disorder as a continuum. Canadian Family Physician, 62(12), 979–982.
Musser, E. D., Karalunas, S. L., Dieckmann, N., Peris, T. S., & Nigg, J. T. (2016). Attention-deficit/hyperactivity disorder developmental trajectories related to parental expressed emotion. Journal of Abnormal Psychology, 125(2), 182–195. https://doi.org/10.1037/abn0000097.
Naismith, I., Zarate Guerrero, S., & Feigenbaum, J. (2019). Abuse, invalidation, and lack of early warmth show distinct relationships with self-criticism, self-compassion, and fear of self-compassion in personality disorder. Clinical Psychology & Psychotherapy, 26(3), 350–361. https://doi.org/10.1002/cpp.2357.
Navab, M., Dehghani, A., & Salehi, M. (2019). Effect of compassion-focused group therapy on psychological symptoms in mothers of attention-deficit hyperactivity disorder children: a pilot study. Counselling and Psychotherapy Research, 19(2), 149–157. https://doi.org/10.1002/capr.12212.
Neff, K. (2003a). The development and validation of a scale to measure self-compassion. Self and Identity, 2(3), 223–250.
Neff, K. (2003b). Self-compassion: an alternative conceptualization of a healthy attitude toward oneself. Self and Identity, 2(2), 85–101. https://doi.org/10.1080/15298860309032.
Neff, K. D., Hsieh, Y., & Dejitterat, K. (2005). Self-compassion, achievement goals, and coping with academic failure. Self and Identity, 4, 263–287. https://doi.org/10.1080/13576500444000317.
Neff, K. D., Kirkpatrick, K. L., & Rude, S. S. (2007). Self-compassion and adaptive psychological functioning. Journal of Research in Personality, 41(1), 139–154. https://doi.org/10.1016/j.jrp.2006.03.004.
Neff, K. D., & McGehee, P. (2010). Self-compassion and psychological resilience among adolescents and young adults. Self and Identity, 9(3), 225–240. https://doi.org/10.1080/15298860902979307.
Neff, K. D., & Pommier, E. (2013). The relationship between self-compassion and other-focused concern among college undergraduates, community adults, and practicing meditators. Self and Identity, 12(2), 160–176. https://doi.org/10.1080/15298868.2011.649546.
Paulson, J. F., & Buermeyer, C. (2005). Social rejection and ADHD in young adults: an analogue experiment. Journal of Attention Disorders, 8(3), 127–135. https://doi.org/10.1177/1087054705277203.
Podsakoff, P. M., MacKenzie, S. B., Lee, J. Y., & Podsakoff, N. P. (2003). Common method biases in behavioral research: a critical review of the literature and recommended remedies. Journal of Applied Psychology, 88(5), 879–903. https://doi.org/10.1037/0021-9010.88.5.879.
Polanczyk, G., De Lima, M. S., Horta, B. L., Biederman, J., & Rohde, L. A. (2007). The worldwide prevalence of ADHD: a systematic review and metaregression analysis. American Journal of Psychiatry, 164(6), 942–948. https://doi.org/10.1176/ajp.2007.164.6.942.
Powers, T. A., & Zuroff, D. C. (1988). Interpersonal consequences of overt self-criticism: a comparison with neutral and self-enhancing presentations of self. Journal of Personality and Social Psychology, 54(6), 1054–1062. https://doi.org/10.1037/0022-3514.54.6.1054.
Psychogiou, L., Daley, D. M., Thompson, M. J., & Sonuga-Barke, E. J. S. (2007). Mothers’ expressed emotion toward their school-aged sons: associations with child and maternal symptoms of psychopathology. European Child and Adolescent Psychiatry, 16(7), 458–464. https://doi.org/10.1007/s00787-007-0619-y.
R Development Core Team. (2013). R: A language and environment for statistical computing. R Foundation for Statistical Computing.
Raes, F. (2011). The effect of self-compassion on the development of depression symptoms in a non-clinical sample. Mindfulness, 2(1), 33–36. https://doi.org/10.1007/s12671-011-0040-y.
Rose, A. V., & Rimes, K. A. (2018). Self-criticism self-report measures: systematic review. Psychology and Psychotherapy: Theory, Research and Practice, 91(4), 450–489. https://doi.org/10.1111/papt.12171.
Rosseell, Y. (2012). Lavaan: An R package for structural equation modeling. Journal of Statistical Software, 48(2), 1–36.
Shaver, P. R., Mikulincer, M., Sahdra, B., & Gross, J. (2016). Attachment security as a foundation for kindness toward self and others. In K. W. Brown & M. R. Leary (Eds.), The oxford handbook of hypo-egoic phenomena (Vol. 1). Oxford University Press..
Singh, I., Kendall, T., Taylor, C., Mears, A., Hollis, C., Batty, M., & Keenan, S. (2010). Young people’s experience of ADHD and stimulant medication: a qualitative study for the NICE guideline. Child and Adolescent Mental Health, 15(4), 186–192. https://doi.org/10.1111/j.1475-3588.2010.00565.x.
Thompson, R., & Zuroff, D. C. (1999a). Dependency, self-criticism, and mothers’ responses to adolescent sons’ autonomy and competence. Journal of Youth and Adolescence, 28(3), 365–384.
Thompson, R., & Zuroff, D. C. (1999b). Development of self-criticism in adolescent girls: Roles of maternal dissatisfaction, maternal coldness, and insecure attachment. Journal of Youth and Adolescence, 28(2), 197–210.
Vigna, A. J., Poehlmann-Tynan, J., & Koenig, B. W. (2018). Does self-compassion facilitate resilience to stigma? A school-based study of sexual and gender minority youth. Mindfulness, 9(3), 914–924. https://doi.org/10.1007/s12671-017-0831-x.
Willoughby, D., & Evans, M. A. (2019). Self-processes of acceptance, compassion, and regulation of learning in university students with learning disabilities and/or ADHD. Learning Disabilities Research & Practice, 34(4), 175–184. https://doi.org/10.1111/ldrp.12209.
Wong, C. C. Y., Mak, W. W. S., & Liao, K. Y. H. (2016). Self-compassion: a potential buffer against affiliate stigma experienced by parents of children with autism spectrum disorders. Mindfulness, 7(6), 1385–1395. https://doi.org/10.1007/s12671-016-0580-2.
Author information
Authors and Affiliations
Contributions
DMB: designed and executed the study, conducted statistical analysis and wrote the paper. FS: collaborated with the design and editing of the manuscript. EM: collaborated with the design and editing of the manuscript.
Corresponding author
Ethics declarations
All procedures were performed in accordance with the ethical standards of the Research Ethics Board of the University of Sheffield (reference: 024076) and with the 1964 Helsinki declaration its later amendments or comparable ethical standards.
Conflict of Interest
The authors declare that they have no conflict of interest.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Beaton, D.M., Sirois, F. & Milne, E. Self-compassion and Perceived Criticism in Adults with Attention Deficit Hyperactivity Disorder (ADHD). Mindfulness 11, 2506–2518 (2020). https://doi.org/10.1007/s12671-020-01464-w
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12671-020-01464-w