Abstract
The current study extended previous research on self-compassion and health behaviours by examining the associations of self-compassion to bedtime procrastination, an important sleep-related behaviour. We hypothesized that lower negative affect and adaptive emotion regulation would explain the proposed links between self-compassion and less bedtime procrastination. Two cross-sectional online studies were conducted. Study 1 included 134 healthy individuals from the community (mean age 30.22, 77.4% female). Study 2 included 646 individuals from the community (mean age 30.74, 68.9% female) who were screened for the absence of clinical insomnia. Participants in both studies completed measures of self-compassion, positive and negative affect and bedtime procrastination. Participants in study 2 also completed a measure of cognitive reappraisal. Multiple mediation analysis in study 1 revealed the expected indirect effects of self-compassion on less bedtime procrastination through lower negative affect [b = − .09, 95% CI = (− .20, − .02), but not higher positive affect. Path analysis in study 2 replicated these findings and further demonstrated that cognitive reappraisal explained the lower negative affect linked to self-compassion [b = − .011; 95% CI = (− .025; − .003)]. The direct effect of self-compassion on less bedtime procrastination remained significant. Our novel findings provide preliminary evidence that self-compassionate people are less likely to engage in bedtime procrastination, due in part to their use of healthy emotion regulation strategies that downregulate negative mood.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Whether conceived of as a momentary mindset or as an enduring dispositional tendency, self-compassion involves taking a kind, accepting and non-judgmental stance towards oneself in times of failure or difficulty, responding mindfully to the negative emotions arising from difficulties, and acknowledging that one is not alone in suffering (Neff 2003b). A growing evidence base indicates that being self-compassionate when facing one’s flaws and failures is linked to an array of beneficial health-related outcomes. Self-compassion is associated with fewer physical symptoms (Dunne et al. 2016; Terry et al. 2013), lower perceived stress (Allen and Leary 2010; Homan and Sirois 2017; Sirois et al. 2015b) and attenuated physiological responses to stress (Arch et al. 2014; Breines et al. 2014). Self-compassion has also been identified as an important predictor of a range of different health behaviours, including healthy eating (Adams and Leary 2007; Schoenefeld and Webb 2013), exercise (Magnus et al. 2010), smoking cessation (Kelly et al. 2010), medical adherence (Dowd and Jung 2017; Sirois and Hirsch 2018), seeking medical care (Terry et al. 2013) and general health-promoting behaviours (Dunne et al. 2016; Sirois et al. 2015a). Importantly, there is emerging evidence that the link between self-compassion and better physical health is explained in part by better practice of health behaviours (Dunne et al. 2016; Homan and Sirois 2017). Although self-compassion is often examined as a dispositional quality in relation to health, several studies have now demonstrated that self-compassion levels can be increased and maintained with simple interventions (e.g. Neff and Germer 2013). Understanding the ways in which self-compassion can be beneficial for promoting key health behaviours, as well as the underlying processes involved, is an important aim for promoting health.
Terry and Leary (2011) proposed that self-compassion enhances the self-regulation of health behaviours through its links to adaptive self-regulatory processes, such as setting goals, taking action, monitoring ongoing behaviour and regulating emotions. However, evidence supporting the links between self-compassion and global measures of self-regulation is scant and inconclusive. In one of the few studies that tested self-compassion in relation to self-regulation, self-compassion was positively correlated with six separate self-regulatory processes, but the link between self-compassion and intentions to seek prompt medical care was not explained by the overall self-regulation score (Terry et al. 2013).
Theory and evidence suggests that self-compassion has strong links to one specific aspect of self-regulation, emotion regulation, and that this may be an important explanatory pathway linking self-compassion and health behaviours. The three main components of self-compassion—self-kindness (vs. self-judgment), common humanity (vs. isolation) and mindfulness (vs. over-identification) (Neff 2003b)—each have consequences for emotion regulation, that is the upregulation of positive affect and the downregulation of negative affect (Gross and John 2003). For example, responding self-compassionately to the inevitable failures that occur while trying to stay on track with health behaviour goals means being kind and accepting of one’s failings (self-kindness), acknowledging that making mistakes while trying to get healthier is part of the human condition (common humanity), and not becoming over-identified with feelings of guilt or frustration (mindfulness). In short, having compassion for oneself while struggling to maintain healthy behaviours translates into healthy emotion regulation. Results from a narrative review support this proposition, and specifically suggest that self-compassion is associated with an emotion regulation style that is typified by higher levels of positive affect, faster recovery from and lower reactivity to stress, and the use of adaptive emotion regulation capacities and strategies (Finlay-Jones 2017). For example, research has demonstrated that self-compassion is associated with emotion-focused coping strategies that increase positive affect, such as acceptance and positive reappraisal, and is negatively related to coping strategies that increase negative affect, such as self-blame (Allen and Leary 2010; Sirois et al. 2015a, b). There is also evidence that trait self-compassion is associated with physiological measures of emotion regulation, such as heart rate variability (Svendsen et al. 2016). Cognitive reappraisal, reframing a situation to change the way it is emotionally responded to (Gross 1998), is one emotion regulation strategy that is effective for downregulating negative emotions (Gross and John 2003). Self-compassion has been linked to cognitive reappraisal for decreasing negative mood (Diedrich et al. 2016), suggesting that cognitive reappraisal is an emotion regulation strategy with particular relevance for understanding how self-compassion may be beneficial for regulating emotions.
With respect to health behaviours, a nascent body of research indicates that the adaptive emotional responses associated with self-compassion may account for why self-compassionate people engage in better health behaviours. In one study of emerging adults, the link between self-compassion and intentions to engage in health behaviours was explained in part by low levels of negative affect (Sirois 2015d). There is also evidence that the associations between self-compassion and the practice of a range of health behaviours, including healthy eating, exercise, stress reduction and getting proper sleep, can be explained in part by the healthy affective balance associated with self-compassion. Across eight samples, the indirect effects of self-compassion on health behaviours were significant for both positive and negative affect (Sirois et al. 2015a, b), suggesting that emotion regulation may play a key role in facilitating positive health behaviours for self-compassionate individuals.
This research is consistent with the temporal-affective self-regulation resource (TASRR) model of health behaviours (Sirois 2015b, d, 2017), which highlights the central role of affective and temporal internal resources, and the qualities which deplete these resources, for regulating health behaviour. The TASRR model builds on theory and research indicating that positive affect can be viewed as a self-regulatory resource that bolsters the practice of health behaviours (Pressman and Cohen 2005; Sirois 2015d; Tice et al. 2007), and posits that individual differences characterized by positive affect will therefore be linked to successful self-regulation of health behaviours. In contrast, negative affect can interfere with effective self-regulation (Sirois 2015b; Wagner and Heatherton 2015), and individual differences that are characterized by negative affect will therefore be prone to misregulation of health behaviours. The TASRR model has been previously validated across several individual differences, including self-compassion (Sirois 2015d), perfectionism (Sirois 2015b), procrastination (Sirois 2015c) and the big five traits (Sirois and Hirsch 2015). It is therefore reasonable to expect, as Terry and Leary (2011) proposed, that self-compassion may equip individuals with the necessary (affective) self-regulatory resources to engage in important health behaviours.
One important health behaviour that has received little empirical study with respect to self-compassion is sleep behaviour. Sleep deprivation increases people’s risk of getting seriously ill through infectious diseases, cancer, cardiovascular problems or depression (Irwin et al. 2016; Strine and Chapman 2005). Behavioural factors strongly affect people’s sleep quality and quantity (Barber et al. 2013; Brown et al. 2002; Nauts and Kroese 2017), for example, because people unnecessarily go to bed too late, despite expecting to be worse off as a result of doing so (bedtime procrastination; Kroese et al. 2016). Bedtime procrastination is highly prevalent, with 74% of people in a representative Dutch sample reporting that they unnecessarily delay going to bed at least once a week (Kroese et al. 2014b), and moderate levels of bedtime procrastination reported among a sample from the USA (Kroese et al. 2014a). As a result of delaying their bedtime, people feel more fatigued and report shorter sleep times (Kroese et al. 2014b). Not surprisingly, bedtime procrastination is related to general procrastination.
Like other types of procrastination, bedtime procrastination is related to trait self-control (Kroese et al. 2014b), suggesting that people need to exert effort to hit the pillow at a reasonable hour. In line with this view, in a qualitative study, bedtime procrastinators indicated that it often requires effort to quit leisurely, rewarding activities to go to sleep (Nauts et al. Forthcoming). Moreover, many bedtime procrastinators in this study indicated that they delayed their bedtimes after tiring or stressful days to allow themselves time to watch TV or play video games to help them unwind. Thus, bedtime procrastination may serve as a form of short-term mood repair: after a long and stressful day, people want to watch a movie, play video games or engage in other leisure activities because doing so makes them feel good. In this respect, bedtime procrastination may be similar to procrastination in general: rather than working on a potentially stressful task, procrastinators often “give in to feel good”, because doing so provides short-term mood repair (Sirois and Pychyl 2013).
Research into the activities that bedtime procrastinators engage in rather than sleeping reveals a range of different activities. A large majority of participants indicates that they engage in media use: they watch “just one more” episode of their favourite TV show, surf the web for funny videos of cats or play video games until the break of dawn (Kroese et al. 2014a, b; Kroese et al. 2016). Although media use can be replenishing with respect to self-regulation (Reinecke 2009), it can also make people feel worse when used as a means to avoid important tasks (Myrick 2015). When people have little self-regulatory resources at their disposal, they are more likely to feel guilty as a result of using media (Reinecke et al. 2014), which may further increase the need for short-term mood repair.
Accordingly, we propose that bedtime procrastination can function as an inadequate emotion regulation strategy to regulate immediate mood. This view is consistent with theory and research on general procrastination, which posits that affect regulation is a key factor in the maintenance of procrastination (Pychyl and Sirois 2016; Sirois and Pychyl 2013), and that bolstering emotion regulation skills reduces procrastination (Eckert et al. 2016). Procrastination can instigate a vicious cycle in which people procrastinate to regulate mood, but feel bad as a result of doing so, which increases their propensity to procrastinate (Sirois and Giguère 2018; Sirois and Kitner 2015). In the present research, we propose that these findings may extend to bedtime procrastination. Specifically, bedtime procrastinators delay going to bed to help themselves cope with their negative mood. As a result of doing so, they are more likely to become sleep deprived, which further limits their capacity to cope with stress, making them increasingly likely to engage in bedtime procrastination.
Current evidence suggests that self-compassion is associated with the practice of health behaviours, and that adaptive emotional responses to personal flaws and failures that upregulate positive affect and downregulate negative affect might explain this association (Sirois et al. 2015a). Yet to date, there is little (if any) research directly testing whether emotion regulation, and cognitive reappraisal in particular, accounts for the adaptive levels of positive and negative affect associated with self-compassion that are proposed to facilitate health behaviours. In addition, self-compassion has not been examined in relation to bedtime procrastination, an important sleep-related behaviour that has links to poor self-regulation (Kroese et al. 2014b), and possibly poor emotion regulation (Sirois and Pychyl 2013). Consistent with research demonstrating that self-compassion is associated with lower levels of general procrastination (Sirois 2014), we expected that self-compassionate people would engage in less bedtime procrastination. We also hypothesized that the high positive affect and low negative affect associated with being self-compassionate would account for less bedtime procrastination. These hypotheses were tested in two non-clinical samples with respect to sleep disorders. In people with sleep disorders, it is difficult to ascertain whether late bedtimes are a result of a sleep disorder (e.g. because people are unable to sleep at an earlier time) or bedtime procrastination (e.g. because people could have gone to bed earlier, but choose to watch television instead).
Study 1
In study 1, we tested the linkages of dispositional self-compassion to sleep quality and behaviours, with the expectation that self-compassion would be associated with better sleep quality, less difficulty falling asleep and less bedtime procrastination. We also tested the mediating roles of positive and negative affect for linking self-compassion to bedtime procrastination.
Method
Participants
A sample of 134 people (mean age = 30.22, SD = 13.5; 77.4% female) participated in the study. Just over half (52.2%) of the participants were not students, and among those who were students, the majority were undergraduate students (41.0% of the sample).
Procedure
Ethical clearance for the data collection was obtained through the Institutional Review Board prior to recruitment and data collection. A convenience sample of participants was recruited via emails sent to a university student volunteer list, through notices placed on social media, and via online psychology web site ads. Participants completed an online survey after clicking “I agree” to provide consent. Data were collected between December and January.
Measures
Participants completed basic demographic questions (age, gender and student status) and the following measures.
Self-Compassion
Participants completed the 26-item Self-Compassion Scale (SCS; Neff 2003a), which assesses the three main components of self-compassion and their negative counterparts, self-kindness (self-judgment), common humanity (isolation) and Mindfulness (over-identification). The SCS includes equal numbers of items worded positively (“I try to be loving towards myself when I’m feeling emotional pain”) and negatively (“I’m disapproving and judgmental about my own flaws and inadequacies”). The subscales are best explained by a single higher order factor of self-compassion (Neff 2003a). Items prefaced with the statement “How I typically act towards myself during difficult times” are rated on a five-point scale from 1 (almost never) to 5 (almost always), with the average of the items (after reverse coding) yielding a score reflecting higher levels of self-compassion. The SCS demonstrates good validity, both convergent and discriminate, and excellent test-retest reliability in previous research (α = .93) (Neff 2003a; Neff and Pommier 2013). In the current study, the SCS demonstrated very good reliability (see Table 1).
Bedtime Procrastination
Bedtime procrastination was measured using a nine-item Bedtime Procrastination Scale (BPS; Kroese et al. 2014a, b), which assesses participants’ propensity to unnecessarily delay their bedtimes. The BPS contains four positively worded items (“I go to bed later than I intended”) and five negatively worded items (“I can easily stop with my activities when it is time to go to bed”), that are rated on a five-point scale (almost never-almost always). The average of these items (after the negatively worded items have been reverse coded) reflects the extent to which people engage in bedtime procrastination, with higher scores reflecting more procrastination. The BPS has good internal and external validity and acceptable test-retest reliability (r = .79; Kroese et al. 2014a, b). In the current study, reliability for the BPS was very good (see Table 1).
Sleep Behaviour
Sleep behaviour was assessed with two questions adapted from the Pittsburg Sleep Quality Index (PSQI; Buysse et al. 1989), a widely used and well-validated measure of seven different aspects of sleep quality. For the purposes of this study, and as a descriptive assessment of participants’ sleep behaviours, only the PSQI global sleep quality and the sleep difficulty items were used. Participants rated their sleep quality by responding to the question “During the past week, how would you rate your sleep quality overall?” on scale from 1 (very good) to 4 (very bad), with higher scores reflecting poor sleep quality. How often they had difficulty getting to sleep within 30 min within the past week was rated on a scale from 1 (not during the past week) to 4 (three or more times a week), with higher scores reflecting more frequent sleep difficulties.
Positive and Negative Affect
The positive and negative affect subscales of the Positive and Negative Affect Schedule (PANAS; Watson et al. 1988) consists of 20 items consisting of words describing different affective states (e.g. happy, upset), with 10 items for each of the positive and negative affect scales. Respondents rated the extent to which they are currently experiencing each of these affect states on a five-point Likert scale ranging from 1 (very slightly or not at all) to 5 (extremely). The PANAS has demonstrated good psychometric properties, including good discriminant validity compared to measures of anxiety and depression, and good internal reliability (α = .88) (Crawford and Henry 2004). In the current study, reliabilities for the PANAS subscales were very good (see Table 1).
Data Availability Statement
All data are available upon request from the authors.
Results
The results of the correlation analysis among the study variables are presented in Table 1. Consistent with our hypotheses, self-compassion was negatively associated with bedtime procrastination, trouble falling asleep within 30 min, poor sleep quality and negative affect and positively associated with positive affect. However, only negative affect (but not positive affect) was significantly associated with bedtime procrastination.
Given that positive affect was not related to bedtime procrastination, the planned multiple mediation model was abandoned and simple mediation model with negative affect was tested. The significance of the indirect effects (mediation) of self-compassion on bedtime procrastination through negative affect was evaluated using the SPSS macro PROCESS (Hayes 2013), which employs a bootstrapping resampling procedure that draws k-bootstrapped samples from the data to estimate the indirect effect and its confidence interval (CI). The current analyses used 5000 bootstrapping resamples and bias corrected 95% confidence intervals. The extent to which negative affect explained the variance in the relationship between self-compassion and bedtime procrastination was estimated with the kappa2 statistic (k2). This statistic is independent of sample size and provides an estimate of the proportion of the maximum indirect effect available for explanation by indirect effects, that is explained by a mediator (Preacher and Kelley 2011).
The analyses revealed the expected significant indirect effects of self-compassion on bedtime procrastination through negative affect, with the overall model explaining 8% of the variance in bedtime procrastination (see Table 2). Of the variance in bedtime procrastination that was explainable by self-compassion, 6% was explained by negative affect (k2 = .06).
Study 2
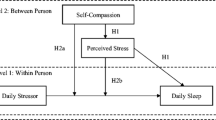
In study 2, we expanded this model to include cognitive reappraisal as a precursor of positive and negative affect, to directly test the proposition that healthy emotion regulation explains why self-compassionate people engage in less bedtime procrastination (see Fig. 1). We chose cognitive reappraisal as the emotion regulation strategy given evidence that cognitive reappraisal effectively downregulates negative affect and, to a lesser extent, upregulates positive affect (Engen and Singer 2015), and that self-compassion is linked to cognitive reappraisal for decreasing negative mood (Diedrich et al. 2016).
Method
Participants
A sample of 810 people completed an online survey. Of this sample, 103 participants who met clinical criteria for insomnia and 61 participants with missing responses on the measure of insomnia were removed, leaving a final sample of 646 (mean age = 30.74, SD = 12.2; 68.9% female) that was analysed for this study.
Procedure
Ethical clearance for the data collection was obtained from the Institutional Review Boards prior to recruitment and data collection. Participants were recruited via a notice sent out to a university volunteer list, through noticed placed on social media, and via online psychology web site ads. All participants were offered a chance to win a gift voucher worth £25. Data were collected between January and March.
Measures
Participants completed demographic questions (age and gender), and the Bedtime Procrastination Scale (Kroese et al. 2014a, b) that was completed in study 1, along with the following measures.
Self-Compassion and Affect
Participants completed the short 12-item version of the self-compassion scale (SCS-12; Raes et al. 2011), and short 10-item version of the PANAS-X (Watson et al. 1988) presented as a visual analogue scale with six negative affect (distressed, upset, guilty, angry, dissatisfied with self, ashamed) and four positive affect (inspired, proud, thankful, hopeful) adjectives scored on an eight-point rating scale (1 = not at all to 8 = extremely). For negative affect, items were chosen from the PANAS-X to reflect distress and guilt, two affective states known to be linked to procrastination (Blunt and Pychyl 2005; Flett et al. 2012). For positive affect, items were chosen to reflect positive self-conscious (pride) and future oriented (inspired, proud) affective states, as these have been linked to lower procrastination behaviour (Blouin-Hudon and Pychyl 2015; Giguère et al. 2016). An additional item was chosen to reflect gratitude, a positive affective state associated with healthy sleep behaviour (Wood et al. 2009).
Participants additionally completed the following new measures for this study. Scale descriptives are presented in Table 3.
Insomnia
The insomnia severity index (ISI; Bastien et al. 2001) is a seven-item measure for screening insomnia and evaluating sleep difficulties. Items are rated on a five-point scale ranging from 0 to 4, in two sets. The first set of three questions asks about the severity of insomnia symptoms (none to very severe), and the next four questions focus on perceptions of sleep problems, including dissatisfaction with, noticeability, distress and the interference of sleep problems. The ISI has demonstrated excellent psychometric properties in previous research (Morin et al. 2011). In the current study, the ISI was used for the purpose of screening out participants meeting clinical criteria for insomnia, as indicated by scores above the recommended subclinical cut-off score of 14 (Morin et al. 2011).
Emotion Regulation
Individual differences in the use of emotion regulation strategies were assessed with the Emotion Regulation Questionnaire (ERQ; Gross and John 2003), a 10-item measure of two strategies: cognitive reappraisal (6 items) and expressive suppression (4 items). Items are rated on a scale ranging from 1 (strongly disagree) to 7 (strongly agree), and subscale scores are averaged with higher sores indicating greater use of the emotion regulation strategy. The subscales of the ERQ have demonstrated good psychometric properties in previous research including good predictive validity and internal consistency (Gross and John 2003). For the current study, only the cognitive reappraisal subscale was analysed, as previous research indicates that it has associations with self-compassion, and both positive and negative affect (Diedrich et al. 2016; Engen and Singer 2015).
Data Analyses
Correlation analyses tested the proposed links between self-compassion, reappraisal, positive and negative affect and bedtime procrastination. In multivariate analyses, we tested the hypothesis that self-compassion was associated with greater reappraisal, and in turn, to greater positive and less negative affect, and then to less bedtime procrastination (see Fig. 1), using path analysis via Mplus 7.4 (Muthen and Muthen 2013). Age and respondents’ sex were statistically accounted for in the model (see Fig. 1). Full-information maximum likelihood (FIML; Arbuckle 1996) estimation procedures were employed. The total, direct and indirect effects of self-compassion on bedtime procrastination were estimated, along with direct effects of self-compassion on reappraisal and on positive and negative affect, and direct effects of each of these latter variables on bedtime procrastination. Since the path model was fully saturated (i.e. df = 0), fit indices were uninformative. Consequently, our primary interest was decomposition of the total predictive effects of self-compassion on bedtime procrastination into direct and indirect effects (see MacKinnon et al. 2004). Indirect effects were tested using the biased-corrected bootstrap method with 10,000 resamples and the 95% bias-corrected confidence intervals (CIs). This method provides a more accurate balance between type 1 and type 2 errors compared to other methods used to test indirect effects (MacKinnon et al. 2004).
Results
All variables were normally distributed (i.e. skewness and kurtosis values all between − 1 and + 1). Four outliers were identified for negative affect, and four outliers were identified for reappraisal. To minimize the influence of these cases on analyses, we replaced any values larger than 3 SDs above the group mean with the value equal to the group mean plus 3 SDs. Descriptive information along with correlations between all study variables is presented in Table 3. Results indicated that self-compassion was positively associated with positive affect, reappraisal and age; self-compassion was negatively associated with negative affect and bedtime procrastination. Reappraisal was positively associated with positive affect and negatively associated with negative affect and bedtime procrastination. Positive affect was related to less negative affect and bedtime procrastination and greater age, whereas negative affect was associated with greater bedtime procrastination along with being younger. Finally, bedtime procrastination was negatively associated with age.
As can be seen in Table 4, the overall model accounted for 17% of the variance in bedtime procrastination. Examination of the correlations revealed that self-compassion accounted for 9.61% of the variance in bedtime procrastination, which was consistent with the findings from study 1. Cognitive reappraisal and negative affect accounted for 24.01 and 23.04% of the variance in bedtime procrastination, respectively, whereas positive affect accounted for 19.36% of the variance in bedtime procrastination.
The results from the path analyses are presented in Table 4. As expected, after accounting for the effects of age and respondents’ sex, self-compassion shared a direct and positive relationship with reappraisal and was also linked with higher levels of positive affect and lower levels of negative affect. Self-compassion was also directly and negatively associated with bedtime procrastination. Reappraisal was associated with higher levels of positive affect and with lower levels of negative affect. Positive affect was not associated with bedtime procrastination, whereas negative affect was associated with greater bedtime procrastination. With respect to indirect effects, self-compassion shared significant and negative indirect associations with bedtime procrastination via reappraisal and negative affect [b = − .011; 95% CI = (− .025; − .003)] and through negative affect [b = − .062; 95% CI = (− .112; − .020)]. Following recommendations made by Simmons et al. (2011), we also conducted the path analyses without any covariates in the model and there were no meaningful differences in the results.
Discussion
Across two studies, individuals high in self-compassion reported high levels of positive affect and low levels of negative affect, and engaged in less bedtime procrastination. Overall, the findings were somewhat consistent with our proposed emotion regulation perspective: low negative affect, but not high positive affect, explained why self-compassionate people reported less bedtime procrastination. Importantly, the path analysis from study 2 indicated that the effects of self-compassion on bedtime procrastination operate partly through the use of cognitive reappraisal, an adaptive emotion regulation strategy (Gross and John 2003), which was in turn linked to low negative affect. However, the indirect effects solely through negative affect, and the direct effect on bedtime procrastination, were also significant, suggesting that there are other reasons, beyond having an effective emotion regulation style (Finlay-Jones 2017), why self-compassionate people tend to not stay up later than they intended.
Our findings confirm and extend theory and research on self-compassion and health behaviours in several important ways. This research tested and found that self-compassion is related to less bedtime procrastination, an important sleep-related behaviour. In doing so, the current research adds to a growing body of literature indicating that being self-compassionate can not only have benefits for the practice of important health behaviours (Dunne et al. 2016; Sirois et al. 2015a; Terry et al. 2013) but can also be beneficial for reducing health-compromising behaviours (e.g. Kelly et al. 2010). If we consider the consequences of bedtime procrastination for sleep duration and daily fatigue (Kroese et al. 2014a, b), and the consequences of poor sleep for health (e.g. Irwin et al. 2016), then bedtime procrastination can be viewed as a sleep behaviour that may compromise health.
The current study suggests that low negative affect rather than high positive affect is implicated in the association between self-compassion and bedtime procrastination. Recent controversy regarding the factor structure of the self-compassion construct suggests one possible explanation for this finding. Some researchers have contended that self-compassion as measured by the self-compassion scale (Neff 2003a) reflects positive (self-compassion) and negative (self-criticism) poles that should be assessed separately rather than as whole (Costa et al. 2015; Montero-Marín et al. 2016). For example, a meta-analysis of 18 studies found that the negatively scored items on the self-compassion scale (self-criticism, isolation and over-identification) were more strongly related to psychopathology than the positive items (self-kindness, common humanity and mindfulness), prompting the researchers to conclude that using a total scale score will inflate the links of self-compassion to negative affective states (Muris and Petrocchi 2017). However, a recent test of the factor structure of the self-compassions scale across 20 diverse samples comparing six-factor, one-factor and bifactor models found that a bifactor model reflecting compassionate and reduced uncompassionate self-responding had poor fit in all samples, whereas a single-factor model had the best fit, explaining 95% of the item variance (Neff et al. 2018). Accordingly, conceptual reasons related to emotion regulation rather than methodological reasons related to scale validity may explain why negative but not positive affect explains the link between self-compassion and bedtime procrastination.
The current research extends previous findings suggesting that self-compassion may promote healthy behaviours due in part to its links to adaptive emotions, which can serve as a self-regulation resource that facilitates the practice of health behaviours (Sirois 2015d; Sirois et al. 2015a). Whereas previous research has examined the levels of positive and negative affect associated with self-compassion in relation to health behaviours, which are suggestive of healthy emotion regulation, this is an initial study to test whether emotion regulation, and specifically cognitive reappraisal, explains the healthy affective states linking self-compassion to health behaviours. Cognitive reappraisal involves “construing a potentially emotion eliciting situation in a way that changes its emotional impact” (Gross and John 2003, p. 349). When viewed from an emotion regulation perspective, the current findings are consistent with the notion that self-compassionate people cognitively reappraise challenges and potential stressors as less stressful and upsetting, and in this respect downregulate their negative emotions (Finlay-Jones 2017). This in turn may reduce the need to engage in bedtime procrastination as a means to repair negative mood.
The current research also extends our understanding of bedtime procrastination by situating it within the context of emotion regulation, and in relation to one particular emotion regulation strategy, cognitive reappraisal. Viewing our findings from the reverse—that people low in self-compassion tend to use less cognitive reappraisal, and experience higher levels of negative mood, and engage in more bedtime procrastination—provides some support for the proposition that bedtime procrastination can serve a mood regulating function. Research has found that engaging in pleasurable activities, such as watching funny kitten videos, can serve a hedonic function, by replenishing positive emotions and providing stress relief (e.g. Myrick 2015). But when the motivation for doing so is to avoid important tasks, such as going to bed on time, then feelings of guilt are likely to replace those of enjoyment (Myrick 2015). In this respect, bedtime procrastination can be viewed as a short-term mood regulation strategy that, similar to general procrastination, comes with a cost to health (Sirois 2015a; Sirois et al. 2003; Sirois and Pychyl 2013).
Given that the direct effects of self-compassion remained significant, our findings also indicate that self-compassionate people are less likely to procrastinate on their bedtime for reasons outside of affective states and emotion regulation. For example, it is possible that going to bed on time could simply be a demonstration of self-kindness and making sure that one gets enough sleep at night. Research on mindfulness, a component of self-compassion, further suggests that effective sleep regulation may account for the direct effects. In a study of undergraduate students, mindfulness was associated with a range of healthy sleep-regulating behaviours and indicators, including less pre-sleep arousal (Howell et al. 2010). Similarly, self-compassionate people may simply be better at preparing themselves to get a good night sleep, which would include avoiding interacting with potential distractors such as technology, engaging books and other tasks that might promote bedtime procrastination. Further research into these and other possible alternative explanations for the direct effects noted in the current study is needed to gain a more complete understanding of the reasons why self-compassionate people tend to not engage in bedtime procrastination.
Limitations and Future Directions
Though novel, our current findings need to be considered in light of several limitations. In the current study, only cognitive reappraisal was tested. Given the cross-sectional data in both studies, it is not possible to confirm the proposed directionality of the relations among self-compassion, cognitive reappraisal, affect and bedtime procrastination. However, our model follows the recommendations of Kline (2010) and is thus predicated on previous theory on self-compassion and the role of affect in the self-regulation of health behaviours (Sirois 2015d; Sirois et al. 2015a). The results are consistent with our model and with a systematic review which found that self-compassion interventions were as effective as other health behaviour change approaches (Biber and Ellis 2017). Nonetheless, given the limitations of our study design, it is also possible that people who are sleep deprived may have difficulty being self-compassionate, and may default to being self-critical instead (Campion and Glover 2016). In addition, the links between emotion regulation and sleep-related behaviours can be reciprocal and mutually reinforcing (Gruber and Cassoff 2014; Palmer and Alfano 2017), suggesting the possibility of more complex relations between emotion regulation and bedtime procrastination than those proposed in the current study. Given the limitations of our research design, we encourage future research to rigorously test our model with longitudinal and/or experimental data to establish temporal precedence suggested by our model.
Other issues arising from the cross-sectional design of our studies involves the retrospective reporting of bedtime procrastination and the assessment of affect at a single static time point and not directly before prior to bedtime procrastination behaviour. This approach could be viewed as less than ideal for assessing the proposed roles of affect and emotion regulation in the linkages of self-compassion to bedtime procrastination. However, an underlying assumption of both our analyses and the TASRR model (Sirois 2015b, d) is that affective states associated with personality traits and dispositional qualities, such as self-compassion, are a relatively stable resource that creates risk or resilience for the self-regulation of health behaviours. Accordingly, it could be reasoned that the one-time measure of affect in each study was generally reflective of more enduring affective states associated with self-compassion. Recent evidence demonstrating that daily affect is surprisingly stable over time, and that up to half the variance in daily affect can be attributed to trait level qualities (Hudson et al. 2016), provides support for this proposition. Further research using a daily diary approach would nonetheless provide a more fine-grained perspective on the role of self-compassion in response to daily challenges and the role of affective responses for attenuating a propensity to engage in bedtime procrastination.
Although further research is needed, our findings provide preliminary evidence that self-compassion may be protective against bedtime procrastination. A growing evidence base indicates that self-compassion can be enhanced through training and interventions (e.g. Neff and Germer 2013), and that such methods can be effective for reducing health risk behaviours such as overeating (Adams and Leary 2007), smoking (Kelly et al. 2010), alcohol misuse (Brooks et al. 2012) and other unhealthy behaviours (Biber and Ellis 2017). Although the amount of variance in bedtime procrastination explained by self-compassion in study 1 (6%) and study 2 (9%) may seem negligible, it is nonetheless comparable to other research that found that self-compassion explained on average 6% of the variance in a measure of multiple health behaviours, which included sleep behaviour, across 15 samples (Sirois et al. 2015a). In terms of clinical significance, previous research has found that even small changes in self-compassion were effective for reducing other harmful health behaviours such as alcohol use (Brooks et al. 2012) and smoking (Kelly et al. 2010). Given this, the current findings provide preliminary evidence to suggest that cultivating self-compassion in response to the daily stresses and failures that can compromise mood and contribute to bedtime procrastination could therefore be one way to reduce this unhealthy sleep-related behaviour.
Our findings provide novel evidence suggesting that self-compassionate people are less likely to engage in bedtime procrastination, due in part to their use of cognitive reappraisal, a healthy emotion regulation strategy that downregulates negative mood. This mood regulation perspective of bedtime procrastination also provides new possibilities for understanding and addressing the harmful health effects of bedtime procrastination, as research to date on the causes of bedtime procrastination has been mainly descriptive rather than explanatory. Further longitudinal and intervention-based research is necessary to provide additional insights into how responding with self-kindness and mindful acceptance to daily challenges can make it easier for people to resist engaging in pleasurable activities, such as watching funny kitten videos and playing video games into the night, and get to bed on time.
References
Adams, C. E., & Leary, M. R. (2007). Promoting self-compassionate attitudes toward eating among restrictive and guilty eaters. Journal of Social & Clinical Psychology, 26(10), 1120–1144. https://doi.org/10.1521/jscp.2007.26.10.1120.
Allen, A. B., & Leary, M. R. (2010). Self-compassion, stress, and coping. Social and Personality Psychology Compass, 4(2), 107–118. https://doi.org/10.1111/j.1751-9004.2009.00246.x.
Arbuckle, J. L. (1996). Full information estimation in the presence of incomplete data. In G. A. Marcoulides & R. E. Schumacker (Eds.), Advanced structural equation modeling: Issues and techniques (Vol. 243–277). Mahwah: Lawrence Erlbaum Associates..
Arch, J. J., Brown, K. W., Dean, D. J., Landy, L. N., Brown, K. D., & Laudenslager, M. L. (2014). Self-compassion training modulates alpha-amylase, heart rate variability, and subjective responses to social evaluative threat in women. Psychoneuroendocrinology, 42(0), 49–58. https://doi.org/10.1016/j.psyneuen.2013.12.018.
Barber, L., Grawitch, M. J., & Munz, D. C. (2013). Are better sleepers more engaged workers? A self-regulatory approach to sleep hygiene and work engagement. Stress and Health, 29(4), 307–316. https://doi.org/10.1002/smi.2468.
Bastien, C. H., Vallières, A., & Morin, C. M. (2001). Validation of the insomnia severity index as an outcome measure for insomnia research. Sleep Medicine, 2(4), 297–307. https://doi.org/10.1016/S1389-9457(00)00065-4.
Biber, D. D., & Ellis, R. (2017). The effect of self-compassion on the self-regulation of health behaviors: a systematic review. Journal of Health Psychology, 1359105317713361. https://doi.org/10.1177/1359105317713361.
Blouin-Hudon, E.-M. C., & Pychyl, T. A. (2015). Experiencing the temporally extended self: initial support for the role of affective states, vivid mental imagery, and future self-continuity in the prediction of academic procrastination. Personality and Individual Differences, 86, 50–56. https://doi.org/10.1016/j.paid.2015.06.003.
Blunt, A., & Pychyl, T. A. (2005). Project systems of procrastinators: a personal project-analytic and action control perspective. Personality and Individual Differences, 38(8), 1771–1780. https://doi.org/10.1016/j.paid.2004.11.019.
Breines, J. G., Thoma, M. V., Gianferante, D., Hanlin, L., Chen, X., & Rohleder, N. (2014). Self-compassion as a predictor of interleukin-6 response to acute psychosocial stress. Brain, Behavior, and Immunity, 37(0), 109–114. https://doi.org/10.1016/j.bbi.2013.11.006.
Brooks, M., Kay-Lambkin, F., Bowman, J., & Childs, S. (2012). Self-compassion amongst clients with problematic alcohol use. Mindfulness, 3(4), 308–317. https://doi.org/10.1007/s12671-012-0106-5.
Brown, F. C., Buboltz, W. C., & Soper, B. (2002). Relationship of sleep hygiene awareness, sleep hygiene practices, and sleep quality in university students. Behavioral Medicine, 28(1), 33–38. https://doi.org/10.1080/08964280209596396.
Buysse, D. J., Reynolds, C. F. r., Monk, T. H., Berman, S. R., & Kupfer, D. J. (1989). The Pittsburgh sleep quality index: a new instrument for psychiatric practice and research. Psychiatry Research, 28(2), 193–213.
Campion, M., & Glover, L. (2017). A qualitative exploration of responses to self-compassion in a non-clinical sample. Health & Social Care in the Community, 25, 1100-1108. https://doi.org/10.1111/hsc.12408
Costa, J., Marôco, J., Pinto-Gouveia, J., Ferreira, C., & Castilho, P. (2015). Validation of the psychometric properties of the self-compassion scale. Clinical Psychology & Psychotherapy, 23, 460–468. https://doi.org/10.1002/cpp.1974.
Crawford, J. R., & Henry, J. D. (2004). The Positive and Negative Affect Schedule (PANAS): construct validity, measurement properties and normative data in a large non-clinical sample. British Journal of Clinical Psychology, 43(3), 245–265. https://doi.org/10.1348/0144665031752934.
Diedrich, A., Hofmann, S. G., Cuijpers, P., & Berking, M. (2016). Self-compassion enhances the efficacy of explicit cognitive reappraisal as an emotion regulation strategy in individuals with major depressive disorder. Behaviour Research and Therapy, 82, 1–10. https://doi.org/10.1016/j.brat.2016.04.003.
Dowd, A. J., & Jung, M. E. (2017). Self-compassion directly and indirectly predicts dietary adherence and quality of life among adults with celiac disease. Appetite. https://doi.org/10.1016/j.appet.2017.02.023.
Dunne, S., Sheffield, D., & Chilcot, J. (2016). Brief report: self-compassion, physical health and the mediating role of health-promoting behaviours. Journal of Health Psychology. https://doi.org/10.1177/1359105316643377.
Eckert, M., Ebert, D. D., Lehr, D., Sieland, B., & Berking, M. (2016). Overcome procrastination: enhancing emotion regulation skills reduce procrastination. Learning and Individual Differences, 52, 10–18. https://doi.org/10.1016/j.lindif.2016.10.001.
Engen, H. G., & Singer, T. (2015). Compassion-based emotion regulation up-regulates experienced positive affect and associated neural networks. Social Cognitive and Affective Neuroscience, 10(9), 1291–1301. https://doi.org/10.1093/scan/nsv008.
Finlay-Jones, A. L. (2017). The relevance of self-compassion as an intervention target in mood and anxiety disorders: a narrative review based on an emotion regulation framework. Clinical Psychologist, 21(2), 90–103. https://doi.org/10.1111/cp.12131.
Flett, G. L., Stainton, M., Hewitt, P., Sherry, S., & Lay, C. (2012). Procrastination automatic thoughts as a personality construct: an analysis of the procrastinatory cognitions inventory. Journal of Rational-Emotive & Cognitive-Behavior Therapy, 4, 1–14. https://doi.org/10.1007/s10942-012-0150-z.
Giguère, B., Sirois, F. M., & Vaswani, M. (2016). Delaying things and feeling bad about it? A norm-based approach to procrastination. In Procrastination, health, and well-being (pp. 189–212). San Diego: Academic Press.
Gross, J. J. (1998). Antecedent- and response-focused emotion regulation: divergent consequences for experience, expression, and physiology. Journal of Personality and Social Psychology, 74, 224–237.
Gross, J. J., & John, O. P. (2003). Individual differences in two emotion regulation processes: implications for affect, relationships, and well-being. Journal of Personality and Social Psychology, 85, 348–362. https://doi.org/10.1037/0022-3514.85.2.348.
Gruber, R., & Cassoff, J. (2014). The interplay between sleep and emotion regulation: conceptual framework empirical evidence and future directions. Current Psychiatry Reports, 16(11), 500. https://doi.org/10.1007/s11920-014-0500-x.
Hayes, A. F. (2013). An introduction to mediation, moderation, and conditional process analysis: a regression-based approach. New York: Guilford Press.
Homan, K. J., & Sirois, F. M. (2017). Self-compassion and physical health: exploring the roles of perceived stress and health-promoting behaviors. Health Psychology Open, 4(2), 2055102917729542. https://doi.org/10.1177/2055102917729542.
Howell, A. J., Digdon, N. L., & Buro, K. (2010). Mindfulness predicts sleep-related self-regulation and well-being. Personality and Individual Differences, 48(4), 419–424. https://doi.org/10.1016/j.paid.2009.11.009.
Hudson, N. W., Lucas, R. E., & Donnellan, M. B. (2016). Day-to-day affect is surprisingly stable: a 2-year longitudinal study of well-being. Social Psychological and Personality Science. https://doi.org/10.1177/1948550616662129.
Irwin, M. R., Olmstead, R., & Carroll, J. E. (2016). Sleep disturbance, sleep duration, and inflammation: a systematic review and meta-analysis of cohort studies and experimental sleep deprivation. Biological Psychiatry, 80(1), 40–52. https://doi.org/10.1016/j.biopsych.2015.05.014.
Kelly, A. C., Zuroff, D. C., Foa, C. L., & Gilbert, P. (2010). Who benefits from training in self-compassionate self-regulation? A study of smoking reduction. Journal of Social and Clinical Psychology, 29(7), 727–755. https://doi.org/10.1521/jscp.2010.29.7.727.
Kline, R. B. (2010). Principles and practices of structural equation modeling. New York: Guilford Press.
Kroese, F. M., De Ridder, D. T. D., Evers, C., & Adriaanse, M. A. (2014a). Bedtime procrastination: introducing a new area of procrastination. Frontiers in Psychology, 5. https://doi.org/10.3389/fpsyg.2014.00611.
Kroese, F. M., Evers, C., Adriaanse, M. A., & de Ridder, D. T. D. (2014b). Bedtime procrastination: a self-regulation perspective on sleep insufficiency in the general population. Journal of Health Psychology, 21, 853-862. https://doi.org/10.1177/1359105314540014.
Kroese, F. M., Nauts, S., Kamphorst, B. A., Anderson, J. H., & de Ridder, D. T. D. (2016). Bedtime procrastination: a behavioral perspective on sleep insufficiency. In F. M. Sirois & T. A. Pychyl (Eds.), Procrastination, health, and well-being (pp. 93–119). San Diego: Academic Press.
MacKinnon, D. P., Lockwood, C. M., & Williams, J. (2004). Confidence limits for the indirect effect: distribution of the product and resampling methods. Multivariate Behavioral Research, 39(1), 99–128.
Magnus, C. M. R., Kowalski, K. C., & McHugh, T.-L. F. (2010). The role of self-compassion in women’s self-determined motives to exercise and exercise-related outcomes. Self and Identity, 9(4), 363–382. https://doi.org/10.1080/15298860903135073.
Montero-Marín, J., Gaete, J., Demarzo, M., Rodero, B., Lopez, L. C. S., & García-Campayo, J. (2016). Self-criticism: a measure of uncompassionate behaviors toward the self, based on the negative components of the self-compassion scale. Frontiers in Psychology, 7, 1281. https://doi.org/10.3389/fpsyg.2016.01281.
Morin, C. M., Belleville, G., Bélanger, L., & Ivers, H. (2011). The insomnia severity index: psychometric indicators to detect insomnia cases and evaluate treatment response. Sleep, 34(5), 601–608.
Muris, P., & Petrocchi, N. (2017). Protection or vulnerability? A meta-analysis of the relations between the positive and negative components of self-compassion and psychopathology. Clinical Psychology & Psychotherapy, 24(2), 373–383. https://doi.org/10.1002/cpp.2005.
Muthen, L. K., & Muthen, B. O. (2013). Mplus user’s guide. Los Angeles: Muthen & Muthen.
Myrick, J. G. (2015). Emotion regulation, procrastination, and watching cat videos online: who watches internet cats, why, and to what effect? Computers in Human Behavior, 52, 168–176. https://doi.org/10.1016/j.chb.2015.06.001.
Nauts, S., & Kroese, F. M. (2017). Self-control in sleep behavior. In D. T. D. de Ridder, M. A. Adriaanse, & K. Fujita (Eds.), Handbook of self-control in health and well-being. New York: Routledge.
Nauts, S., Kamphorst, B. A., Stut, W., de Ridder, D. T. D., & Anderson, J. H. (Forthcoming). The reasons people give for going to bed late: a qualitative study of the varieties of bedtime procrastination.
Neff, K. D. (2003a). Development and validation of a scale to measure self-compassion. Self and Identity, 2, 223–250. https://doi.org/10.1080/15298860309027.
Neff, K. D. (2003b). Self-compassion: an alternative conceptualization of a healthy attitude toward oneself. Self and Identity, 2(2), 85–101. https://doi.org/10.1080/15298860390129863.
Neff, K. D., & Germer, C. K. (2013). A pilot study and randomized controlled trial of the mindful self-compassion program. Journal of Clinical Psychology, 69(1), 28–44. https://doi.org/10.1002/jclp.21923.
Neff, K. D., & Pommier, E. (2013). The relationship between self-compassion and other-focused concern among college undergraduates, community adults, and practicing meditators. Self and Identity, 12(2), 160–176. https://doi.org/10.1080/15298868.2011.649546.
Neff, K. D., Tóth-Király, I., Yarnell, L. M., Arimitsu, K., Castilho, P., Ghorbani, N., ... Mantzios, M. (2018). Examining the factor structure of the self-compassion scale in 20 samples with bifactor ESEM: support for use of a total score and six subscale scores. Psychological Assessment. (in press).
Palmer, C. A., & Alfano, C. A. (2017). Sleep and emotion regulation: an organizing, integrative review. Sleep Medicine Reviews, 31(Supplement C), 6–16. https://doi.org/10.1016/j.smrv.2015.12.006.
Preacher, K. J., & Kelley, K. (2011). Effect size measures for mediation models: quantitative strategies for communicating indirect effects. Psychological Methods, 16, 93–115.
Pressman, S. D., & Cohen, S. (2005). Does positive affect influence health? Psychological Bulletin, 131(6), 925–971. https://doi.org/10.1037/0033-2909.131.6.925.
Pychyl, T. A., & Sirois, F. M. (2016). Procrastination, emotion regulation and well-being. In F. M. Sirois & T. Pychyl (Eds.), Procrastination, health, and well-being: (pp. 163–188). San Diego: Academic Press.
Raes, F., Pommier, E., Neff, K. D., & Van Gucht, D. (2011). Construction and factorial validation of a short form of the self-compassion scale. Clinical Psychology & Psychotherapy, 18(3), 250–255. https://doi.org/10.1002/cpp.702.
Reinecke, L. (2009). Games and recovery. Journal of Media Psychology, 21(3), 126–142. https://doi.org/10.1027/1864-1105.21.3.126.
Reinecke, L., Hartmann, T., & Eden, A. (2014). The guilty couch potato: the role of ego depletion in reducing recovery through media use. Journal of Communication, 64(4), 569–589. https://doi.org/10.1111/jcom.12107.
Schoenefeld, S. J., & Webb, J. B. (2013). Self-compassion and intuitive eating in college women: examining the contributions of distress tolerance and body image acceptance and action. Eating Behaviors, 14(4), 493–496. https://doi.org/10.1016/j.eatbeh.2013.09.001.
Simmons, J. P., Nelson, L. D., & Simonsohn, U. (2011). False-positive psychology. Psychological Science, 22(11), 1359–1366.
Sirois, F. M. (2014). Procrastination and stress: exploring the role of self-compassion. Self and Identity, 13(2), 128–145.
Sirois, F. M. (2015a). Is procrastination a vulnerability factor for hypertension and cardiovascular disease? Testing an extension of the procrastination-health model. Journal of Behavioral Medicine, 38, 578–589. https://doi.org/10.1007/s10865-015-9629-2.
Sirois, F. M. (2015b). Perfectionism and health behaviors: a self-regulation resource perspective. In F. M. Sirois & D. S. Molnar (Eds.), Perfectionism, health and well-being (pp. 45–68). Cham: Springer.
Sirois, F. M. (2015c). A self-regulation resource model of procrastination and health behaviors. Paper presented at the 9th Biennial Procrastination Research Conference, Bielefeld.
Sirois, F. M. (2015d). A self-regulation resource model of self-compassion and health behavior intentions in emerging adults. Preventive Medicine Reports, 2, 218–222. https://doi.org/10.1016/j.pmedr.2015.03.006.
Sirois, F. M. (2017). Procrastination as vulnerability for poor health: a temporal-affective self-regulation resource perspective. Paper presented at the University of Zurich Department of Psychology Seminar Series, Zurich.
Sirois, F. M., & Giguère, B. (2018). Giving in when feeling less good: procrastination, action control, and social temptations. British Journal of Social Psychology, 57(2), 404–427. https://doi.org/10.1111/bjso.12243.
Sirois, F. M., & Hirsch, J. K. (2015). Big five traits, affect balance and health behaviors: a self-regulation resource perspective. Personality and Individual Differences, 87, 59–64. https://doi.org/10.1016/j.paid.2015.07.031.
Sirois, F. M., & Hirsch, J. K. (2018). Self-compassion and adherence in five medical samples: the role of stress. Mindfulness. https://doi.org/10.1007/s12671-018-0945-9.
Sirois, F. M., & Kitner, R. (2015). Less adaptive or more maladaptive? A meta-analytic investigation of procrastination and coping. European Journal of Personality, 29, 433–444.
Sirois, F. M., & Pychyl, T. (2013). Procrastination and the priority of short-term mood regulation: consequences for future self. Social and Personality Psychology Compass, 7(2), 115–127. https://doi.org/10.1111/spc3.12011.
Sirois, F. M., Melia-Gordon, M. L., & Pychyl, T. A. (2003). “I’ll look after my health, later”: an investigation of procrastination and health. Personality and Individual Differences, 35(5), 1167–1184.
Sirois, F. M., Kitner, R., & Hirsch, J. K. (2015a). Self-compassion, affect, and health behaviors. Health Psychology, 34, 661–669. https://doi.org/10.1037/hea0000158.
Sirois, F. M., Molnar, D. S., & Hirsch, J. K. (2015b). Self-compassion, stress, and coping in the context of chronic illness. Self and Identity, 14,334-347. https://doi.org/10.1080/15298868.2014.996249.
Strine, T. W., & Chapman, D. P. (2005). Associations of frequent sleep insufficiency with health-related quality of life and health behaviors. Sleep Medicine, 6(1), 23–27. https://doi.org/10.1016/j.sleep.2004.06.003.
Svendsen, J. L., Osnes, B., Binder, P.-E., Dundas, I., Visted, E., Nordby, H., et al. (2016). Trait self-compassion reflects emotional flexibility through an association with high vagally mediated heart rate variability. Mindfulness, 7(5), 1103–1113. https://doi.org/10.1007/s12671-016-0549-1.
Terry, M. L., & Leary, M. R. (2011). Self-compassion, self-regulation, and health. Self and Identity, 10(3), 352–362. https://doi.org/10.1080/15298868.2011.558404.
Terry, M. L., Leary, M. R., Mehta, S., & Henderson, K. (2013). Self-compassionate reactions to health threats. Personality and Social Psychology Bulletin, 39(7), 911–926. https://doi.org/10.1177/0146167213488213.
Tice, D. M., Baumeister, R. F., Shmueli, D., & Muraven, M. (2007). Restoring the self: positive affect helps improve self-regulation following ego depletion. Journal of Experimental Social Psychology, 43(3), 379–384. https://doi.org/10.1016/j.jesp.2006.05.007.
Wagner, D. D., & Heatherton, T. F. (2015). Self-regulation and its failure: the seven deadly threats to self-regulation. In M. Mikulincer, P. R. Shaver, E. Borgida, & J. A. Bargh (Eds.), APA handbook of personality and social psychology, volume 1: Attitudes and social cognition (pp. 805–842). Washington: American Psychological Association..
Watson, D., Clark, L. A., & Tellegen, A. (1988). Development and validation of brief measures of positive and negative affect: the PANAS scales. Journal of Personality and Social Psychology, 54, 1063–1070. https://doi.org/10.1037/0022-3514.54.6.1063.
Wood, A. M., Joseph, S., Lloyd, J., & Atkins, S. (2009). Gratitude influences sleep through the mechanism of pre-sleep cognitions. Journal of Psychosomatic Research, 66(1), 43–48.
Author information
Authors and Affiliations
Contributions
FS: designed and executed the studies, ran the data analyses for study 1 and wrote the majority of the paper. SN: collaborated with the design, analysis and writing of the study. DM: analysed the data and wrote the results for study 2 and collaborated in the editing of the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the Research Ethics Board of the University of Sheffield and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Sirois, F.M., Nauts, S. & Molnar, D.S. Self-Compassion and Bedtime Procrastination: an Emotion Regulation Perspective. Mindfulness 10, 434–445 (2019). https://doi.org/10.1007/s12671-018-0983-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12671-018-0983-3